Food Trauma Nourishment Adrienne Markworth Leahs Pantry May






























- Slides: 37

Food, Trauma & Nourishment Adrienne Markworth Leah’s Pantry May 22, 2019

WE ENVISION nourished communities and a healthy, equitable food system. OUR MISSION is to improve the health, wellness, and resilience of communities through traumainformed nutrition security.

… because everyone deserves nourishing meals every day.

STRATEGIES Implement innovative programs that explore our relationship with food, support health, and build resilience. Build capacity of partner organizations to best serve their communities. Start conversations to expand the frame and include impacts of trauma on our nutritional health.

Products and Programs

Outline ● ● ● Explore our own relationship to food Presentation: Food, trauma, and nourishment Table Talk Discussion Flowers and Apples Mindful eating exercise (during lunch)

Meaning of Food in Life Questionnaire

Meaning of Food in Life Domains – Health, Spiritual, Moral, Social, and Aesthetic Have you considered your relationship with food in this way? What was surprising to you? Were there high or lows in particular domains? Do you live with people who might have different priorities? Alignment & My Needs Are there areas where you feel some discomfort or a difference between your values and your practice? Are there domains where you would like to increase your numbers? What do you need to do this? Other Considerations Are these statements relevant for everyone? Clients? How do power and privilege affect whether our relationship to food can be fully realized?

What is nourishment?


Pillars Of Food Security (WHO & FAO) Food Resources Sufficient quantities of food available on consistent basis. Food Access Sufficient resources to obtain appropriate foods for a culturally appropriate diet. Food Use A healthy environment and adequate knowledge to prepare foods that meet nutritional needs. Stability of resources, access, and use over time.

Pillars Of Food Nutrition Security Food Resources Sufficient quantities of nutritious food available on consistent basis. Food Access Sufficient resources to obtain appropriate foods for a culturally appropriate and nourishing diet. Food Use A healthy environment and adequate knowledge to prepare foods that meet nutritional needs. Stability and Self-Sufficiency Stability of resources, access, and use over time.

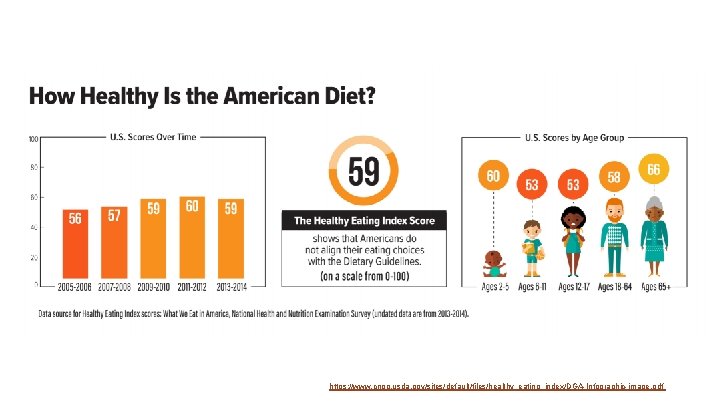
https: //www. cnpp. usda. gov/sites/default/files/healthy_eating_index/DGA-Infographic-image. pdf

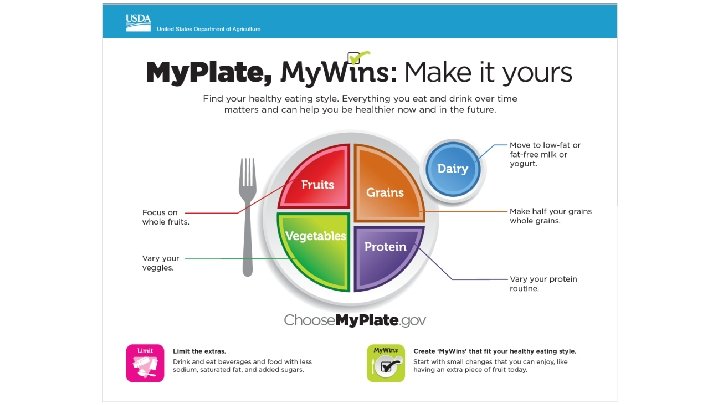
2015 -2020 DGA


Is healthy eating equivalent to nourishment?

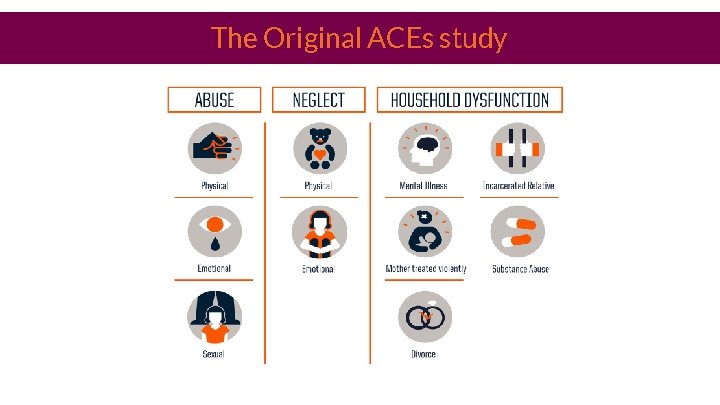
The Original ACEs study

Community ACES 1. Witness Violence 2. Felt Discrimination 3. Adverse Neighborhood experience 4. Bullied 5. Lived in foster care 6. Food Insecurity

Vicarious Trauma Also: compassion fatigue, secondary trauma stress, secondary victimization Different from: burnout Definition: a state of tension and preoccupation of the stories/trauma experiences described by clients Symptoms Directly Tied to Dietary Health Overeating/undereating Related Diminished joy to things once enjoyed; Difficulty sleeping; Exhaustion; Rejecting physical/emotional closeness; apathy; disruption in self-capacity; disruption in needs/beliefs/relationships Adapted from the American Counseling Association Fact Sheet #9

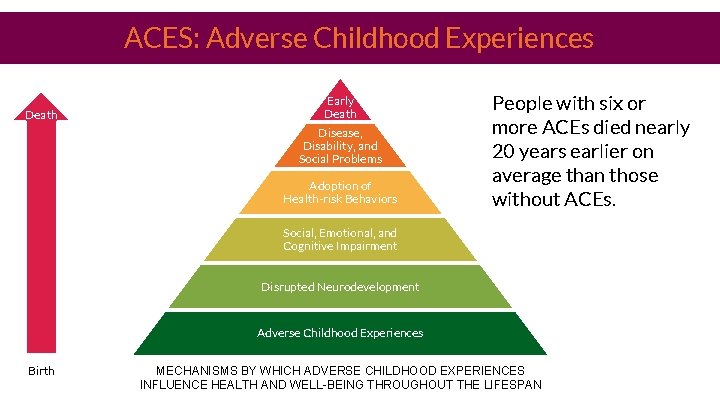
ACES: Adverse Childhood Experiences Death Early Death Disease, Disability, and Social Problems Adoption of Health-risk Behaviors People with six or more ACEs died nearly 20 years earlier on average than those without ACEs. Social, Emotional, and Cognitive Impairment Disrupted Neurodevelopment Adverse Childhood Experiences Birth MECHANISMS BY WHICH ADVERSE CHILDHOOD EXPERIENCES INFLUENCE HEALTH AND WELL-BEING THROUGHOUT THE LIFESPAN

What are “unhealthy” food behaviors? ● Binging ● Lack of physical activity ● Overeating ● Improper decision making ● High fat, sugar, salt intake ● Eating disorders ● Food “addiction” ● Reliance on convenience foods ● Hoarding ● Not exercising will power ● Failed planning and budgeting

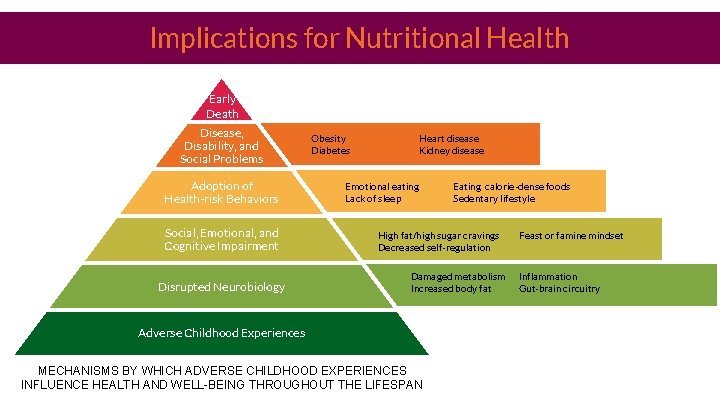
Implications for Nutritional Health Early Death Disease, Disability, and Social Problems Adoption of Health-risk Behaviors Social, Emotional, and Cognitive Impairment Disrupted Neurobiology Obesity Diabetes Heart disease Kidney disease Emotional eating Lack of sleep Eating calorie-dense foods Sedentary lifestyle High fat/high sugar cravings Decreased self-regulation Damaged metabolism Increased body fat Adverse Childhood Experiences MECHANISMS BY WHICH ADVERSE CHILDHOOD EXPERIENCES INFLUENCE HEALTH AND WELL-BEING THROUGHOUT THE LIFESPAN Feast or famine mindset Inflammation Gut-brain circuitry

Reframing ● overfeeding ● overeating ● hoarding ● food addiction ● poor “will power” ● eating disorders ● weight gain ● high salt, fat, sugar intake ● Caregiving/Giving Love ● Feeling Loved ● Seeking protection and safety ● Predictability and security ● Asserting Autonomy ● Dysregulated hunger and satiety signals ● Altered neurochemical and metabolic pathways

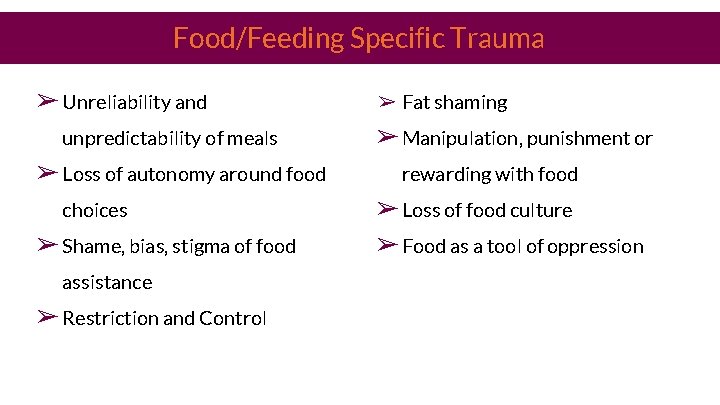
Food/Feeding Specific Trauma ➢ Unreliability and unpredictability of meals ➢ Loss of autonomy around food choices ➢ Shame, bias, stigma of food assistance ➢ Restriction and Control ➢ Fat shaming ➢ Manipulation, punishment or rewarding with food ➢ Loss of food culture ➢ Food as a tool of oppression

Two Perspectives ➢ Trauma of any kind can cause disruption in a healthy relationship with food ➢ Food itself can be a source of trauma, which begins or exacerbates an unhealthy relationship with food ➢ Therefore, the relationship between food, individuals, families, and communities must be treated with care and a holistic perspective

Discussion Questions ➢ How do we move towards a more inclusive concept of nourishment? ➢ How can we work to define this for ourselves and our clients? ➢ What evidence do you see in yourself or your colleagues that points to either burnout or vicarious trauma in the realm of nutritional health?

Trauma-informed organizations provide trauma-informed services

➢ Organizational culture ➢ Staff burnout/turnover ➢ Volunteer burnout ➢ Secondary trauma/compassion fatigue/vicarious trauma ➢ Lack of calendar control, always putting out fires ➢ Food trauma

Resisting Retraumatization

Implications to Programs Does the program or initiative: – reduce shame, anxiety, confusion and tension? – promote safety, dignity, joy? – inspire healing and a healthy relationship to food?

Barriers to Trauma-Informed Nourishment ➢ Focus on obesity and BMI ➢ Rules, restriction, deprivation or scarcity mindset ➢ Disregard of client readiness ➢ Lack of cultural humility ➢ Bureaucratic and non-transparent processes ➢ Over focus on personal behavior change ➢ “Donation dumping”; poor quality resources

Prioritize ➢ Client dignity, voice and needs ➢ Stress reduction ➢ Choice and autonomy ➢ Food in support of mental and physical health ➢ Culturally-relevant and accessible resources ➢ Leveling of power dynamics in interactions (adapted from SAMHSA’s Principles of Trauma Informed Care)

Tensions Caused by Good Intentions ➢ Efficient use of resources ➢ Accountability to funders ➢ Client health ➢ Evaluation and data collection (macro vs. micro) ➢ Meaning of service, charity ➢ Equality and equity

A Model for Trauma-Informed Nutrition Security

Apples and Flowers ➢ What is one personal or organizational practice you’d like to let go of? (These are your apples) ➢ What is a personal or organizational practice you would like to nurture and see blossom? – Who can keep you accountable? – Whose buy-in do you need? – What resources do you need?

Get Started: ACES study and questionnaire www. cdc. gov/violenceprevention/ acestudy/ Principles of Trauma-Informed Care https: //store. samhsa. gov/shin/conten t/SMA 14 -4884. pdf Join the ACES and Nourishment Community www. acesconnection. com/g/acesand-nourishment

Contact Us Adrienne Markworth adrienne@leahspantry. org 415 -710 -2729