FOOD BORNE DISEASES Dr Gaurij Hood Food borne

FOOD BORNE DISEASES Dr Gaurij Hood

Food borne Diseases 1. Introduction-Global and Indian Scenario Food borne infections vs Food Intoxications 2. Pathogenesis and Transmission 3. Some important foodborne pathogens/toxins/chemicals 4. Investigations and Lab diagnosis 5. Treatment

1. Introduction • • • Food borne diseases-(intoxications and infections) covers illnesses acquired through consumption of contaminated food-i. e food poisoning Food borne disease outbreaks-occurrence of 2 or more cases of similar illness resulting from ingestion of common food OR when observed number of paticular disease exceeds expected number Most cases-sporadic but need investigations for control

1. Introduction –Burden • Global burden-high morbidity and mortality • Infectious diarrhoea-3 to 5 billion cases and 1. 8 million deaths annually • CDC-76 million cases of food borne diseases in US annually with appx. 5000 deaths • In India-Integrated disease surveillance Project(IDSP)-Food poisoning outbreak reporting increased to more than double in 2009 from 2008(120 in 2009 and 50 in 2008)

Food borne infections vs intoxication • Infections. Bacterial/Viral/parasite • Invade and or multiply in lining of intestine • Incubation period-hours to days • s/sdiarrhoea, nausea, vomitting, ab dominal cramps, fever • Transmission-spreads from person to person • Factors-inadequate cooking, cross contamination, poor personal hygiene, bare hand contact • Intoxications-toxins (natural/preformed bacterial/chemical) • No invasion or multiplication • Incubation period-minutes to hours • s/svomitting, nausea, diarrhea, dipl opia, weaakness, resp. failure, nu mbness, sensory/motor dysfunction • Not communicable • Factors-inadequate cooking, improper handling temperatures

Some important food-borne pathogens, toxins and chemicals • 1. Bacteria-Bacillus cereus, brucella, campylobacter, clostridium sp, e. coli, Salmonella sp, listeria, staph aureus, , vibrio cholera and parahemolyticus • 2. viruses-hepatitis a and e, rotavirus, norvovirus, • 3. protozoacryptosporidium, cyclospora, entamoeba, giardia, t gondii • 4. trematodes, cestodes and nematodes

Food borne pathogens-toxins and chemicals • Toxins-marine biotoxins, tetrodotoxin(pufferfish), pyrrolizidine alka, mushroom toxins, shellfish toxins, mycotoxins, plant toxicants • Chemicalspesticides(opp, sb), radionuclides, nitrites(food preservatives), toxic metalscd, cu, hg, pb, sn, fluoride, MSG

Pathogenesis and Transmission • Infectious agent or contaminant • Inoculum/size of infective dose-can be as small as 10 -100 bacterial cysts for shigella, EHEC, giardia, E. histolytica or 10^ 5 -10^ 8 for vibrio cholera, variable for salmonella • Animals or humans harbouring infection shed in feces contaminate water, fruits, vegetables inadequate cooking/improper storage infection • Warm temperature(10 -50 degree cent. )multiplication of pathogens
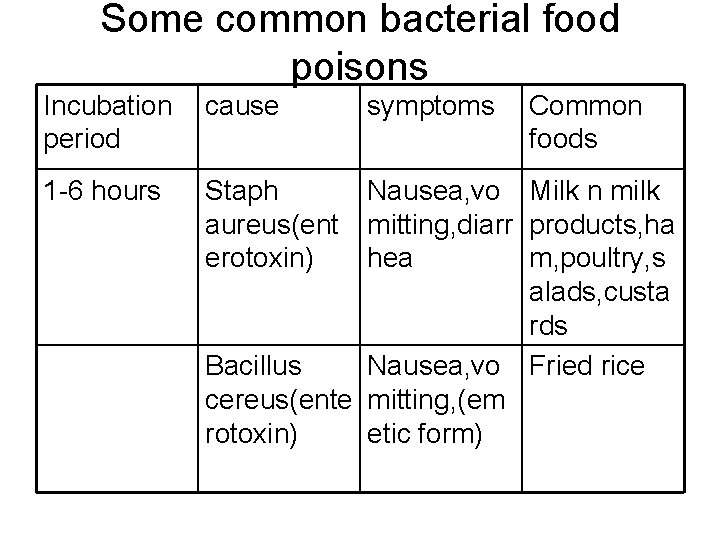
Some common bacterial food poisons Incubation period cause 1 -6 hours Staph aureus(ent erotoxin) symptoms Common foods Nausea, vo Milk n milk mitting, diarr products, ha hea m, poultry, s alads, custa rds Bacillus Nausea, vo Fried rice cereus(ente mitting, (em rotoxin) etic form)
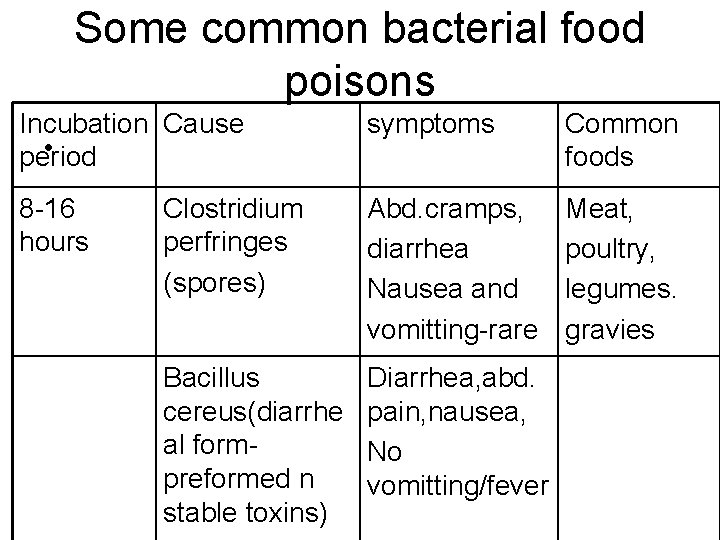
Some common bacterial food poisons Incubation Cause • period symptoms Common foods 8 -16 hours Clostridium perfringes (spores) Abd. cramps, diarrhea Nausea and vomitting-rare Meat, poultry, legumes. gravies Bacillus cereus(diarrhe al formpreformed n stable toxins) Diarrhea, abd. pain, nausea, No vomitting/fever

Some common bacterial food poisons Incubation cause period >16 hours Vibrio cholera Salmonella spp Shigella sp symptoms Common foods Rice watery Water and stools ice creams, sea food Inflammator Meat, milk n y diarrhea milk products, po ultry dysentry Potato/raw eggs-salad

Early diagnosis and investigations • 1. Initial assessment of cases-Detailed clinical history including time of onset, duration of illness, symptoms, h/o travel, recent meals, cooking and refrigeration, details of others with similar complaints • 2. Detailed clinical examination-vitals and degree of dehydration, systemic signs

Lab diagnosis • Main objectives • a)To confirm clinical diagnosis by isolation of causative agent from proper samples, egstool, vomitus/gastric aspirate, food specimens • b)Ensure proper identification of disease • c)Determine causative agent if present in food sources with relevant epidemiological markerseg Biotyping, serotyping, pcr, phage typing etc

Steps of outbreak investigation • Establishing existence of outbreak(detailed baseline epidemiological information) Co-ordination with key personnel Collection and transport of clinical specimens and food samples for lab testing Implementation of control and preventive measures definition of cases, population at risk and finding cases Description of epidemiology Development of possible hypotheses Epidemiological study to evaluate hypotheses Analysis of data and interpretation Reporting findings of outbreak investigation

Prevention in community • Proper handwashing and personal hygiene • Proper storage(refrigeration) • Food saftey education –community and food handlers • Environmental measures-discourage sewage farming for growing fruits and vegetables

Prevention • Hazard Analysis and Critical Control Point(HACCP) • Systematic preventive approach to food saftey • Addresses physical, chemical and biological hazards as means of prevention rather than finished product inspection • Food industry-food saftey hazards identified at all stages of food production and preparation processes key action taken at Critical Control Points(CCPs)

Principles of Hazard Analysis and Critical Control Point(HACCP) • Analyse hazards Identify critical control points Establish preventive measures with critical limits for each CCP Establish procedures to monitor CCPS Establish corrective actions when monitoring shows that critical limit has not met Establish procedures to verify that system is working properly Establish effective record keeping for documentation

Treatment • 1. Initial t/t-Assessment and reversal of dehydration(ORT/IV Fluids) • 2. Cause specific treatment if anyeg. chelating agents in case of pesticide poisoning • 3. Use of antibiotics can be considered if bacterial cause is identified

Collection of food samples • Using aseptic technique n appropriate containers samples be refrigerated during storage and transport must arrive lab within 3 days of collection • Adequate sample-minimum 100 grams • Containers-not to be filled >75% of capacity • Proper labelling is utmost important labelled specimen be placed in zip lock bag and sealed • Vaccine carrier with ice packs for transport and cold chain maintenance(avoid freezing)

• The mainstay of treatment is adequate rehydration. • The treatment of cholera and other dehydrating diarrheal diseases promotion of oral rehydration solutions, efficacy of which depends on the fact that glucose-facilitated absorption of sodium and water in the small intestine remains intact in the presence of cholera toxin. • The use of oral rehydration solutions has reduced mortality due to cholera from >50% (in untreated cases) to <1%. • The World Health Organization recommends a solution containing 3. 5 g sodium chloride, 2. 5 g sodium bicarbonate, 1. 5 g potassium chloride, and 20 g glucose (or 40 g sucrose) per liter of water. • Oral rehydration solutions containing rice or cereal as the carbohydrate source may be even more effective than glucose-based solutions, and the addition of L-histidine may reduce the frequency and volume of stool output. • Patients who are severely dehydrated or in whom vomiting precludes the use of oral therapy should receive IV solutions such as Ringer's lactate.

Five keys to Safer food • 1. Keep Clean-Wash hands before handling food and often during preparation • Wash hands after going to toilet • Wash n sanitise all surfaces n equipment for food preparation-protect kitchen from insects, pets • 2. Separate raw and cooked food-Separate raw meat, poultry n seafood from other foods • Use separate utensils for handling raw foods • Store food in containers to avoid contact between raw and cooked foods

Five Keys to Safer Food • 3. Cook Thoroughly-esp. Meat, poultry, eggs and Seafood • Bring soups n stews to boiling(ensure>70 degree temp) • Reheat cooked food thoroughly • 4. Keep food at safe temperature • Dont leave cooked food at room temp. >2 hours • Prompt refrigeration of cooked n perishable food • Keep cooked food piping hot(>60 de. )prior serving • Don’t store food too long even in refrigerator • Don’t thaw frozen food at room temperature

Five keys to safer food • 5. Use safe water and raw materials • Use safe water or treat to make it safe • Select fresh and wholesome fruits • Choose foods processed for safety-pasteurised milk • Wash fruits n vegetables if eaten raw • Don’t use food beyond expiry date
- Slides: 23