Focused Abdominal Sonography for Trauma Samuel Kingsley Advocate

+ Focused Abdominal Sonography for Trauma Samuel Kingsley Advocate Illinois Masonic Hospital

+ Abdominal Ultrasonography An important diagnostic modality within the trauma population Originally reported in this context by German and Japanese physicians in the 1970 s US implementation and publications began in the 1980 s Rozycki (1995) formalized the abdominal assessment describing four windows: RUQ, LUQ, Pelvis, Pericardium Shackford (1996) introduced the acronym FAST

+ Pros & Cons Benefits: Drawbacks: n Rapid assessment n False negative n Non invasive n n No radiation Misses injuries not associated with large extravasation n Possible false positives n User dependent n Skills decay over time n n n Requires no drugs/toxins Serial assessments Rapid learning curve

+ Accuracy FAST exam requires ~200 cc of fluid to be positive (reports of 100 cc) Sensitivity of FAST 73 -88% Specificity of FAST 98 -100%

+ Indications n Blunt abdominal trauma n n n In unstable patient, can help determine source: peritoneal bleed vs. pericardial effusion vs. BCI In stable patient, presence of fluid helps to determine need for CT imaging Penetrating trauma n n Unstable patient – no indication to perform FAST; patient should be taken immediately to OR Stable patient – assess for automatic operative indications (stability), trajectory, evisceration, hematemsis, BPR; if negative… n A positive FAST will rule in operative intervention n a negative FAST does not rule out operative intervention (sensitivity< 50%)
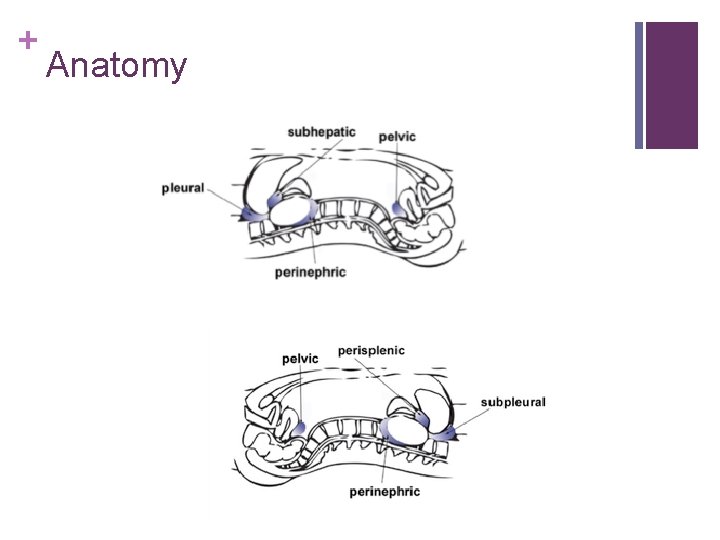
+ Anatomy
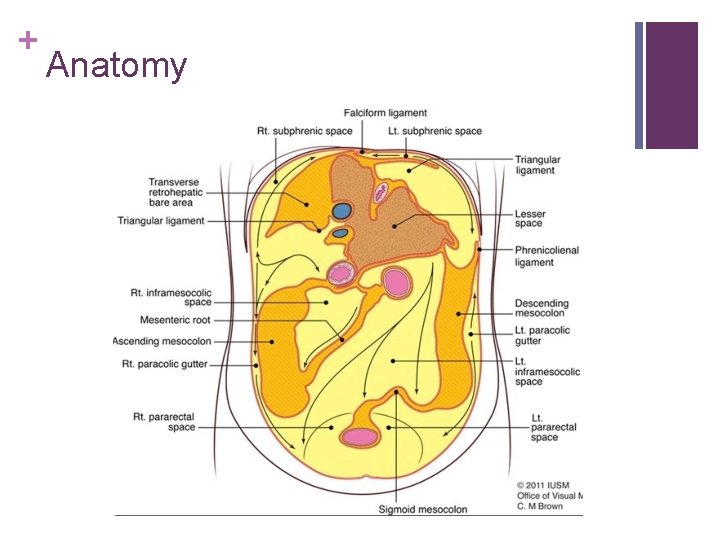
+ Anatomy
+ Equipment

+ Probe Types
+ Orientation

+ Probe Types

+ Probe Types
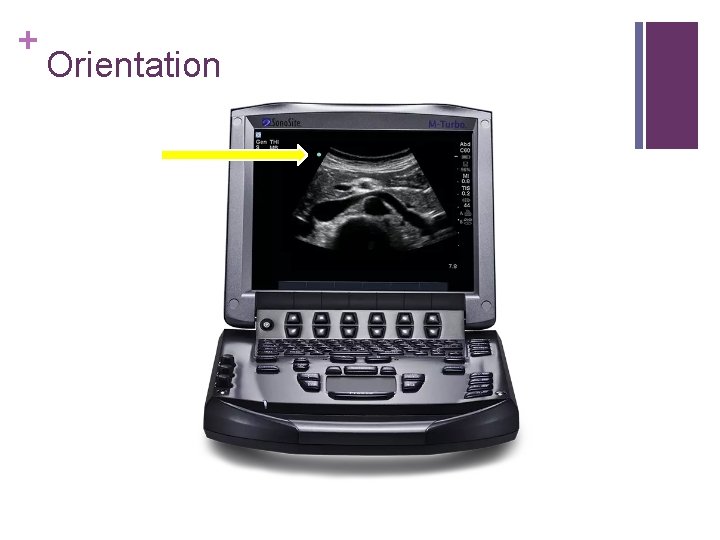
+ Orientation

+ Sonosite M Turbo

+ Sonosite M Turbo

+ Sonosite M Turbo

+ Sonosite M Turbo

+ Sonosite M Turbo

+ Sonosite M Turbo

+ FAST Exam Technique n Pelvic n Right Upper Quadrant n Left Upper Quadrant n Cardiac
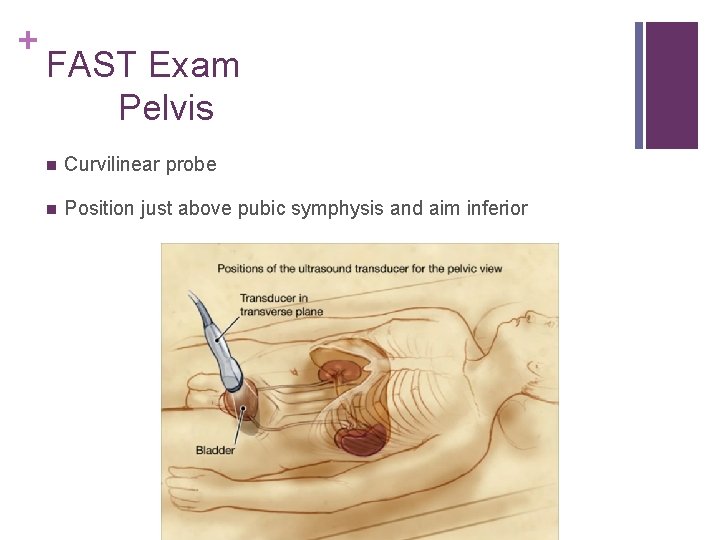
+ FAST Exam Pelvis n Curvilinear probe n Position just above pubic symphysis and aim inferior
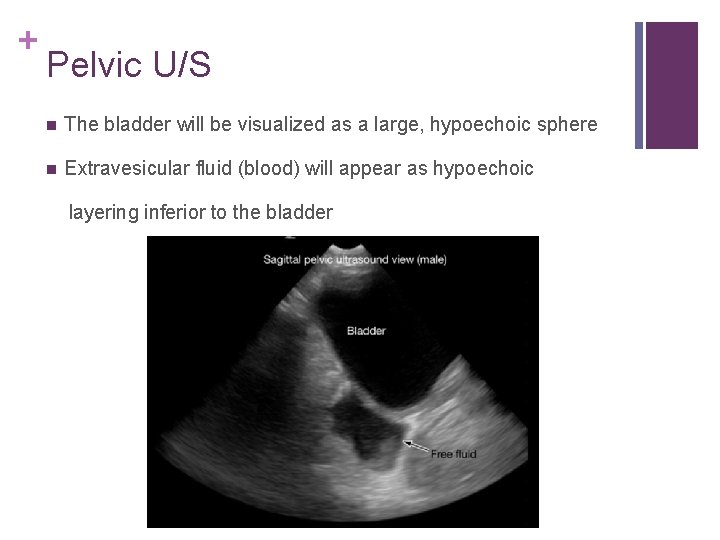
+ Pelvic U/S n The bladder will be visualized as a large, hypoechoic sphere n Extravesicular fluid (blood) will appear as hypoechoic layering inferior to the bladder
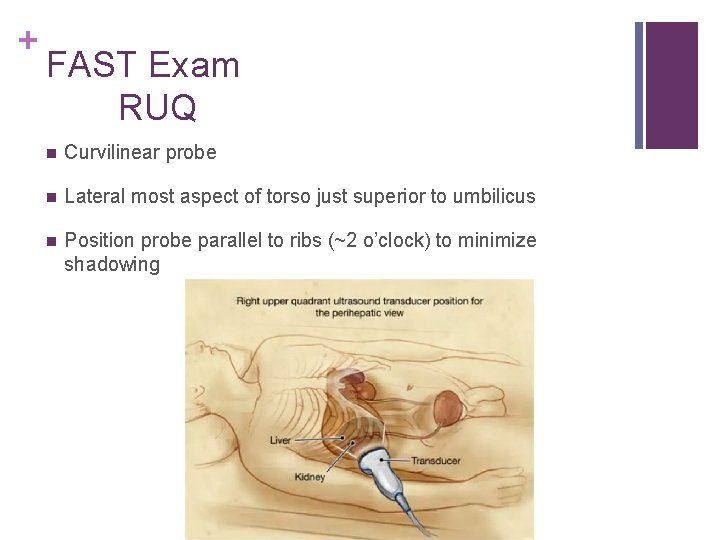
+ FAST Exam RUQ n Curvilinear probe n Lateral most aspect of torso just superior to umbilicus n Position probe parallel to ribs (~2 o’clock) to minimize shadowing
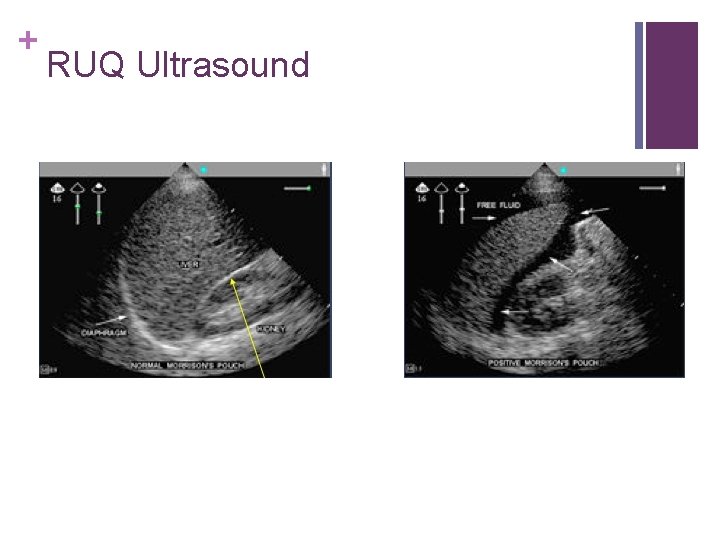
+ RUQ Ultrasound
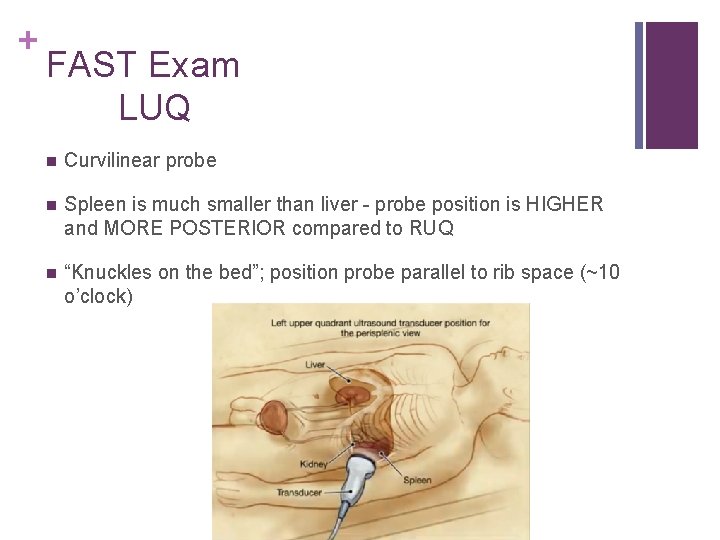
+ FAST Exam LUQ n Curvilinear probe n Spleen is much smaller than liver - probe position is HIGHER and MORE POSTERIOR compared to RUQ n “Knuckles on the bed”; position probe parallel to rib space (~10 o’clock)
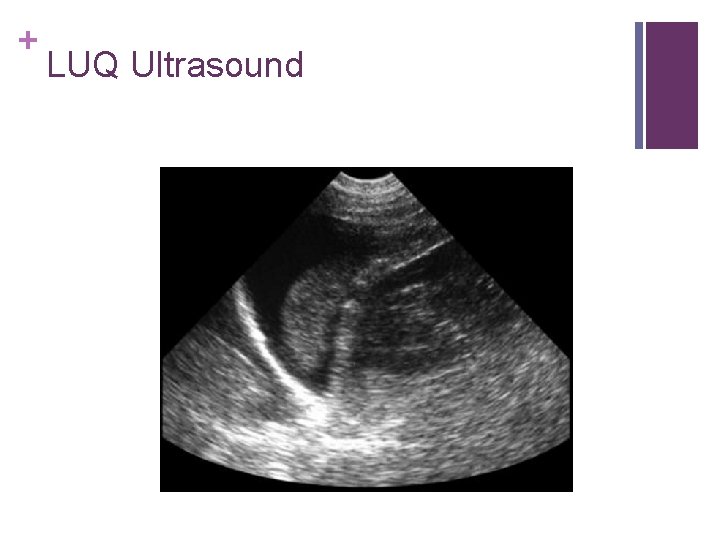
+ LUQ Ultrasound
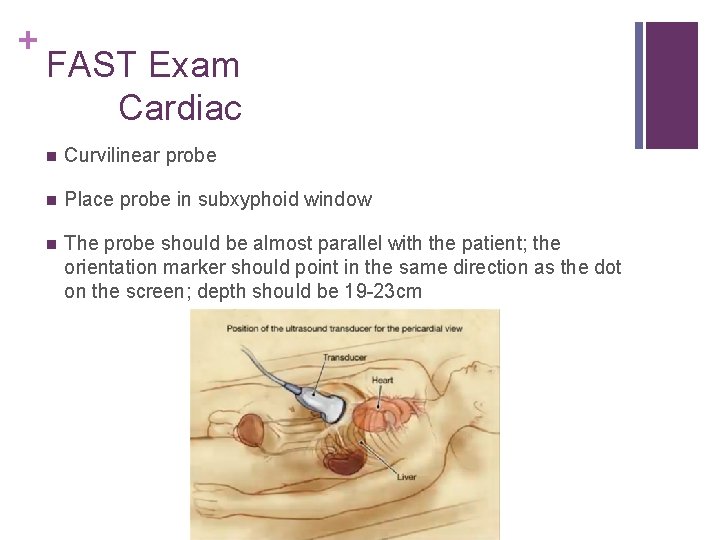
+ FAST Exam Cardiac n Curvilinear probe n Place probe in subxyphoid window n The probe should be almost parallel with the patient; the orientation marker should point in the same direction as the dot on the screen; depth should be 19 -23 cm
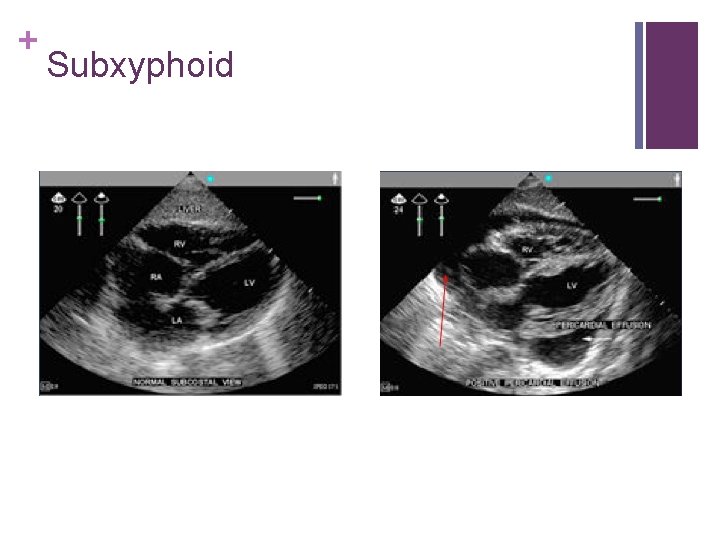
+ Subxyphoid

+ IVC assessment n Once the subxyphoid view is established, the IVC can be assessed by rotating the probe 90° so the marker is pointing upwards n IVC diameter (3 cm from RA) <1 cm correlates with hypovolemia; >2 cm correlates with euvolemia or hypervolemia n Collapse is important as well
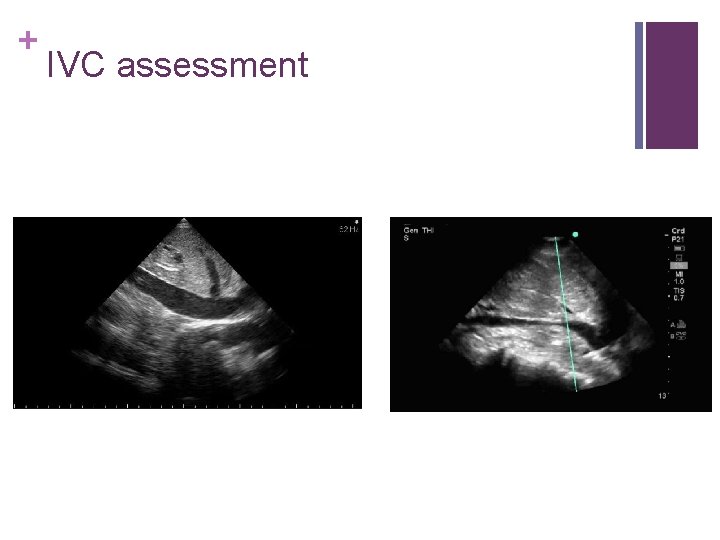
+ IVC assessment

+ Questions?
- Slides: 31