Focus on AcidBase Balance and Arterial Blood Gases

Focus on Acid-Base Balance and Arterial Blood Gases Nancy Lin, RN, MS

SLO’s • Analyze and compare normal and abnormal blood gases for pediatric and adult clients. • Examine medications and treatments used to correct acid base imbalances for pediatric and adult clients. • Propose a plan of care for pediatric and adult clients experiencing acid base imbalances.

Purpose of Acid-Base • Maintain a steady balance between acids and bases to achieve homeostasis • Health problems leading to imbalance: ______

Overview of Acid-Base Physiology • Nature of acids & bases – Acid • releases a H+ ion when dissolved in water – Base • bind to a H+ ion when dissolved in water
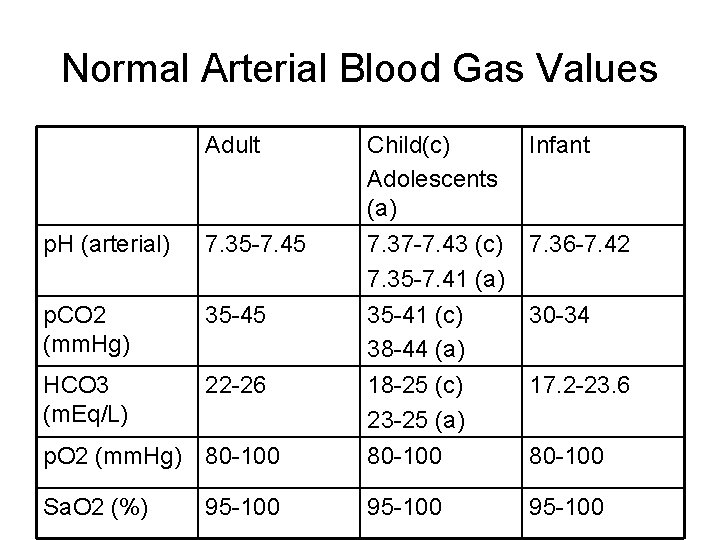
Normal Arterial Blood Gas Values Adult Child(c) Adolescents (a) Infant p. H (arterial) 7. 35 -7. 45 7. 36 -7. 42 p. CO 2 (mm. Hg) 35 -45 HCO 3 (m. Eq/L) 22 -26 p. O 2 (mm. Hg) 80 -100 7. 37 -7. 43 (c) 7. 35 -7. 41 (a) 35 -41 (c) 38 -44 (a) 18 -25 (c) 23 -25 (a) 80 -100 Sa. O 2 (%) 95 -100 30 -34 17. 2 -23. 6 80 -100
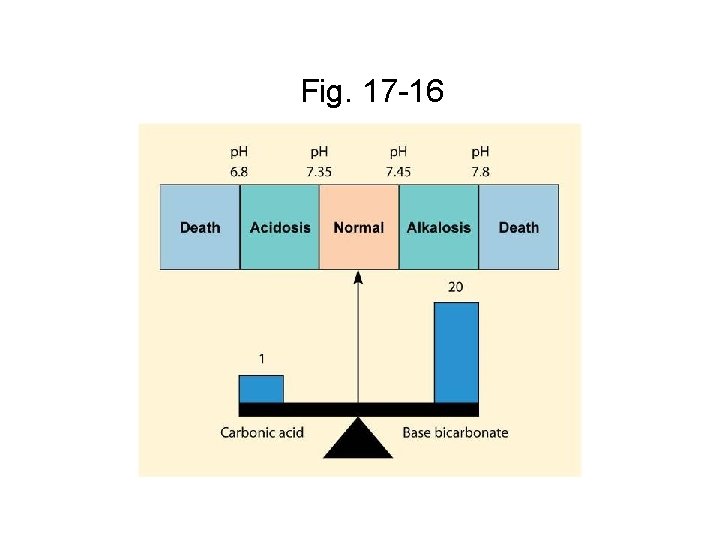
Fig. 17 -16

Alterations in Acid-Base Balance • Respiratory or Metabolic • Respiratory imbalances – affect carbonic acid concentrations • Metabolic imbalances – affect base bicarbonate
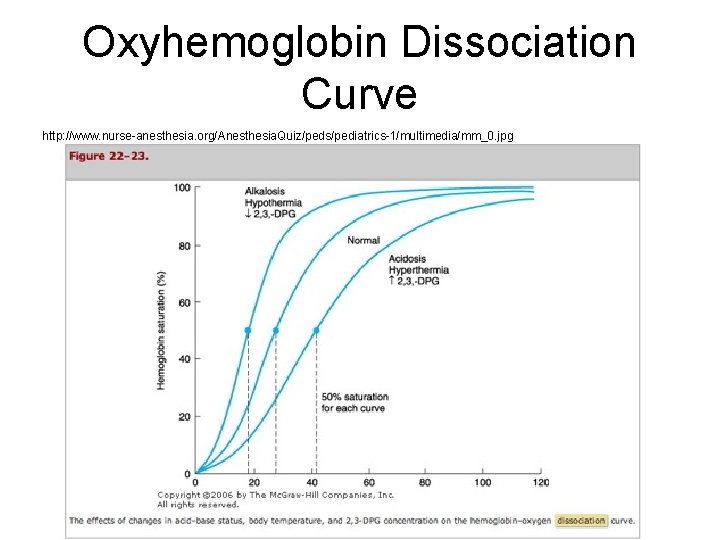
Oxyhemoglobin Dissociation Curve http: //www. nurse-anesthesia. org/Anesthesia. Quiz/peds/pediatrics-1/multimedia/mm_0. jpg

Acid-Base Regulation • Three mechanisms to regulate acid-base balance – Buffer systems – Respiratory system – Renal system

Regulators of Acid/Base: Buffers • Neutralize acids or change strong acids to weak acids – Primary regulators – React immediately – Cannot maintain p. H without adequate respiratory and renal function

Regulators of Acid/Base Respiratory System • Respiratory system: eliminates CO 2 – Respiratory center in medulla controls breathing – Responds within minutes/hours • Inc. respirations → more CO 2 expelled & less remains in blood • Dec. respirations → more CO 2 remains in blood

Regulators of Acid/Base: Renal System • Kidneys: essential buffer system for acids • Renal system: eliminate H+ and reabsorb HCO 3 • Responds within hours to days • Elderly clients – acid-base imbalances more difficult to correct

Compensation • Body uses regulatory mechanism to return p. H to it’s normal level • Complete compensation • Partial compensation • Uncompensated • Decompensation

Acid-Base Imbalances (cont'd) • Imbalances occur when compensatory mechanisms fail • Classification of imbalances – Respiratory – Metabolic • Alterations in acid-base balance – – – Respiratory acidosis Respiratory alkalosis Metabolic acidosis Metabolic alkalosis Mixed acid-base disorders

Blood Gas Values • Arterial blood gas (ABG) values provide information about – Acid-base status – Underlying cause of imbalance – Body’s ability to regulate p. H – Overall oxygen status

Interpretation of ABGs • Diagnosis in six steps – Evaluate p. H – Analyze Pa. CO 2 – Analyze HCO 3– Determine if CO 2 or HCO 3 - matches the alteration – Decide if body attempting to compensate

Acid-Base Mnemonic—ROME • Respiratory • Opposite – p. H ↑ Pa. CO 2 ↓ Alkalosis – p. H ↓ Pa. CO 2 ↑ Acidosis • Metabolic • Equal – p. H ↑ HCO 3 – p. H ↓ HCO 3 ↑ ↓ Alkalosis Acidosis

Respiratory Acidosis • Carbonic acid excess caused by – Hypoventilation – Respiratory failure

Respiratory Acidosis • Clinical presentation – Cardiovascular • • • Hypotension Delayed cardiac conduction → heart block, ECG changes Peripheral vasodilation w/thready, weak pulse Tachycardia Warm, flushed skin – Respiratory • Dysnpnea • Hypoventilation with hypoxia – CNS • • • HA SZ Altered LOC Papilledema Muscle twitching Drowsiness → coma
![Hyperkalemia in Acidosis • As blood [H+] rises in cases of acidosis, more H+ Hyperkalemia in Acidosis • As blood [H+] rises in cases of acidosis, more H+](http://slidetodoc.com/presentation_image_h/dc3136d60746a4e2fc96bc291c22e9ea/image-20.jpg)
Hyperkalemia in Acidosis • As blood [H+] rises in cases of acidosis, more H+ ions are pumped intracellularly in exchange for K+ ions that are pumped extracellularly to maintain electrical neutrality.

Respiratory Acidosis • Compensation – Kidneys conserve HCO 3 - and secrete H+ into urine

Therapeutic Management: Respiratory Acidosis • Correct underlying cause • Improve ventilation – Pulmonary hygiene measures • Adequate fluid intake • Supplemental oxygen • Mechanical ventilation

Respiratory Alkalosis • Carbonic acid deficit caused by – Hyperventilation • Primary cause • Other causes:
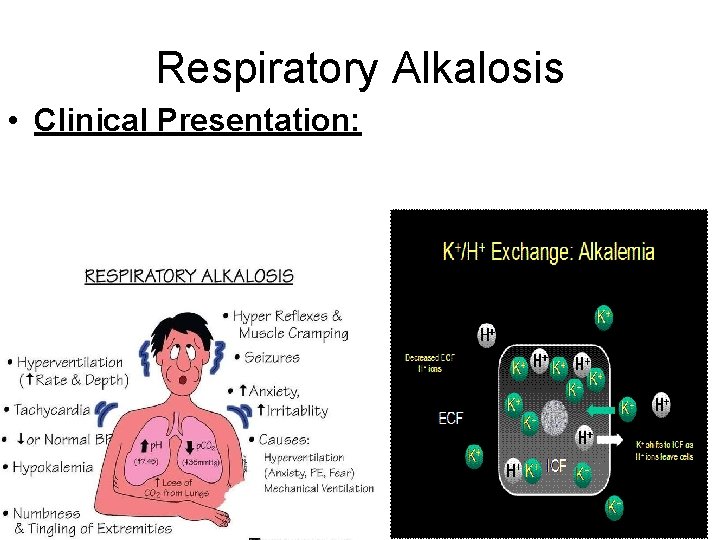
Respiratory Alkalosis • Clinical Presentation:

Respiratory Alkalosis • Compensation – Rarely occurs due to aggressive treatment of causes of hypoxemia

Therapeutic Management: Respiratory Alkalosis • Treat underlying cause • Have pt breathe CO 2 by using rebreather mask or paper bag • Give O 2 therapy if pt is hypoxic • Med as needed with antianxiety drugs

Metabolic Acidosis ● An imbalance in which p. H decreases & HCO 3 decreases • Causes:

Metabolic Acidosis ● Clinical Presentation:

Metabolic Acidosis • Compensatory mechanisms – Increased CO 2 excretion by lungs • Kussmaul respiration • Kidneys excrete acid

Therapeutic Management: Metabolic Acidosis • Correct underlying problem • Provide hydration • Admin alkalotic IV solution – Na Bicarb or Na Lactate • Mechanical ventilation

Metabolic Alkalosis • Base bicarbonate excess caused by – Prolonged vomiting – Gain of HCO 3 -

Metabolic Alkalosis • Clinical Presentation:

Metabolic Alkalosis • Compensatory mechanisms – Decreased respiratory rate to increase plasma CO 2 – Renal excretion of HCO 3 -

Metabolic Alkalosis • Priority nursing diagnoses: • Therapeutic Management:

Interpretation of ABGs • Respiratory – ↑ p. H, ↓ Pa. CO 2 – ↓ p. H, ↑ Pa. CO 2 • Metabolic – ↑ p. H, ↑ HCO 3 – ↓ p. H, ↓ HCO 3

Interpretation of ABGs • • • p. H 7. 36 Pa. CO 2 67 mm Hg Pa. O 2 47 mm Hg HCO 3 37 m. Eq/L What is this?

Interpretation of ABGs • • • p. H 7. 18 Pa. CO 2 38 mm Hg Pa. O 2 70 mm Hg HCO 3 - 15 m. Eq/L What is this?

Interpretation of ABGs • • • p. H 7. 60 Pa. CO 2 30 mm Hg Pa. O 2 60 mm Hg HCO 3 - 22 m. Eq/L What is this?

Interpretation of ABGs • • • p. H 7. 58 Pa. CO 2 35 mm Hg Pa. O 2 75 mm Hg HCO 3 - 50 m. Eq/L What is this?

Interpretation of ABGs • • • p. H 7. 28 Pa. CO 2 28 mm Hg Pa. O 2 70 mm Hg HCO 3 - 18 m. Eq/L What is this ?

Case Study 1: Jeri • • • 1. 2. Jeri’s been on a 3 -day party binge Friends are unable to awaken her Assessment reveals level of consciousness difficult to arouse Respiratory rate 8 Shallow breathing pattern Diminished breath sounds What ABGs do you expect? What is your treatment?

Case Study 2: Mayna • • • Presented to the ER after a sexual assault Physical examination reveals hysterical emotional distress Respiratory rate 38 Lungs clear O 2 sat 96% • • What ABGs do you expect? What is your treatment?

Case Study 3: Glen • • • History of fever, aches, and chills Generally feeling ill Cough productive of yellow, thick sputum for the past 4 days Examination reveals temp 38. 4° C Respiratory rate 20 Lungs with crackles in left lower lobes 1. 2. What ABGs do you expect? What is your treatment?

Case Study 4: Alan • • 17 years old History of – – Feeling bad Fatigue Constant thirst Frequent urination • • Blood sugar is 484 mg/dl Respirations are 28 and deep Breath has a fruity odor His lungs are clear 1. 2. What ABGs do you expect? What is your treatment?

Case Study 5: Anthony • • History of nausea and vomiting for the past week Has been self-medicating himself with baking soda to control his abdominal discomfort 1. What ABGs do you expect? 2. What is your treatment?

Case Study 6: Susan • ABG results are: – – p. H 7. 20 Pa. CO 2 58 mm Hg Pa. O 2 59 mm Hg HCO 3 - 24 m. Eq/L 1. Describe a patient who would have these ABGs, including history and assessment. 2. What is the treatment?

Case Study 7: Fernando • ABG results are: – – p. H 7. 39 Pa. CO 2 38 mm Hg Pa. O 2 44 mm Hg HCO 3 - 24 m. Eq/L 1. Describe a patient who would have these ABGs, including history and assessment. 2. What is the treatment?

Case Study 8: Brianna • ABG results are: – – p. H 7. 36 Pa. CO 2 58 mm Hg Pa. O 2 50 mm Hg HCO 3 - 33 m. Eq/L 1. Describe a patient who would have these ABGs, including history and assessment. 2. What is the treatment?

Case Study 9: Monica • ABG results are: – – p. H 7. 50 Pa. CO 2 28 mm Hg Pa. O 2 85 mm Hg HCO 3 - 24 m. Eq/L 1. Describe a patient who would have these ABGs, including history and assessment. 2. What is the treatment?

Case Study 10: Mike • ABG results are: – – p. H 7. 20 Pa. CO 2 28 mm Hg Pa. O 2 81 mm Hg HCO 3 - 18 m. Eq/L 1. Describe a patient who would have these ABGs, including history and assessment. 2. What is the treatment?

Case Study 11: Jeremy • ABG results are: – – p. H 7. 57 Pa. CO 2 46 mm Hg Pa. O 2 87 mm Hg HCO 3 - 38 m. Eq/L 1. Describe a patient who would have these ABGs, including history and assessment. 2. What is the treatment?

References Hockenberry, M. J. & Wilson, D. (2015). Wong’s Nursing care of infants and children (10 th ed. ). St. Louis, MO: Mosby. Lewis, S. , Heitkemper, M. & Dirksen, S. (2014). Medical Surgical Nursing: Assessment and Management of Clinical Problems (9 th ed. ). St. Louis, MO: Mosby
- Slides: 52