Fluids Nutrition in SCN By Nicole Stevens Types

Fluids & Nutrition in SCN By: Nicole Stevens

Types of Fluids & additives § § § Breast milk Term Formula 10% dextrose with additives Parenteral nutrition (including a glucose solution with electrolytes and amino acids and a fats/vitamins solution) § Breast milk fortification and Preterm formulas § Thickener
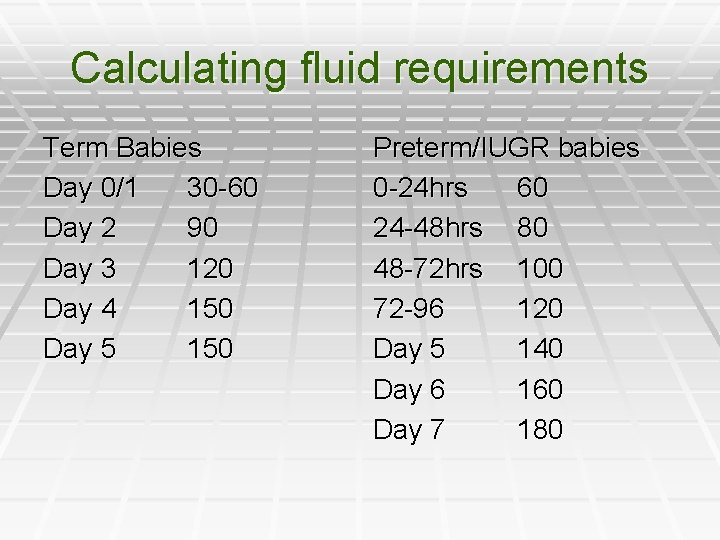
Calculating fluid requirements Term Babies Day 0/1 30 -60 Day 2 90 Day 3 120 Day 4 150 Day 5 150 Preterm/IUGR babies 0 -24 hrs 60 24 -48 hrs 80 48 -72 hrs 100 72 -96 120 Day 5 140 Day 6 160 Day 7 180

Who has what when? ? § In the newborn baby maintenance of normoglycaemia is the priority in all babies § In the well baby, without risk factors, on postnatal ward we won’t even monitor for hypoglycaemia (we will just assume it will be OK), and the focus will on the establishment of suck feeding and adequate intake, assessed by watching feeds, talking with mums, assessing supply and assessing the baby (behaviour, output)

Who has what when? In SCN it’s not so simple (it’s a game of numbers, so get out your calculators!) NBM? § IV access, and commence 10% dextrose. In NICU’s with significantly preterm babies parenteral nutrition may be commenced as soon as line (central) placement is confirmed. This will not apply for the >32 wk infants we care for in SCN’s § If unable to feed at all, or much, after 48 hrs add Sodium and Potassium to the 10%dextrose (eg. In a 500 m. L bag of 10% dextrose add 10 mmol of KCL and 22 mmol of Sodium Chloride)

Who has what when? NBM cont. . § If due to feed intolerance, or ongoing respiratory issues (significant enough to contraindicate feeding), adequate feeds are not able to be achieved after several days there needs to be consideration for transfer to a centre that can provide parenteral nutrition. § The more preterm the baby, the earlier this decision needs to be made. Dextrose is hydrating and maintains normoglycaemia, but it is not nutrition, and babies need nutrition in the form of milk or PN.

Who has what when? Mother chooses to breastfeed? § Introduce milk feeds as soon as medically indicated § For the preterm baby receiving gastric tube feeds commence with small volumes as available and gradually work up as tolerated § If supply of EBM does not meet babies requirements over first few days may be preferable to maintain IV fluids to make up the difference, rather than introduce formula. The more preterm and/or growth restriced the baby is, the more important it is to wait for supply to improve. § Obviously, can’t wait for ever so need to assess on an individual basis.

Grading up feeds (IV to oral) § Calculate hrly rate § Determine frequency of feeds (2, 3 or 4 hrly) § Titrate IV down and oral up to maintain TFI, speed at which we grade up depends on milk availability and babies tolerance of increased volumes § Watch for abdo distention and bilious vomits, especially in the LBW and IUGR infants § Check IV site, rate of infusion, TFI and feed volumes at the start of your shift – you can’t rely on the shift before having it correct.

Fortification of Breast milk § Depends on hospital policy. At BHS we use fortification § § § for babies born <2 kgs, and it will be ceased once they are gaining adequate weight and are over 2 kgs Fortification is added to breast milk only. If using FM 85 (nestle), 1 stick (20 g) is added to 20 m. L of EBM – this is described as ‘full fortification’, in some cases babies may be on ‘ 1/2’ fortification (1 stick to 40 m. Ls EBM) Fortification adds extra calories to the milk and provides additional vitamins and electrolytes Should not be introduced until babies have proven tolerance to milk at volumes of at least 120 m. L/kg/day.

Establishing lactation For mothers who are separated from their babies, unable to breastfeed, needing to hand express & pump. As a guide only: § Express 8 – 10 times a day (2 -3 hrly during the day and 4 hrly overnight) § Night expressing very important (prolactin surge) § Rest, healthy diet, drink lots of water § Skin to skin if well enough § Breast contact when baby well enough (even if quite premature – great for learning, bonding and prolactin levels)

Formula fed § If a mother chooses to formula feed they will supply their § § own on most maternity units. If admitted to SCN it will depend on the hospital as to what the process is. Best practice would indicate that in the SCN environment we should be using sterilised, ready to feed options. At BHS we offer Nan, Aptamil and S 26 options These also have preterm equivalents Pre. Nan, Aptamil preterm and LBWS 26 – these would be introduced at the same time we would introduce fortification in babies receiving breastmilk. So they would start on a ‘term’ formula and transition over days down the track to ‘preterm’

Supplements and testing for deficiencies § Don’t test Vit D levels in newborns, just give if indicated by gestational age (<37 wks), or maternal Vit D status (low) § For babies born <32 wks gestation it is common to begin doing ‘premature’ bone bloods at 3 weeks of age to monitor levels of electrolytes, haemoglobin and reticulocytes. These would be repeated fortnightly during inpatient stay, and then followed up in paediatric outpt. clinics § Most babies do not need electrolyte supplements post discharge, but if Vit D and iron commenced they will go home on these.

Supplements § Vit D (500 iu daily, oral) – given to all babies born <37 wks § § § and/or if the mother is Vit D deficient (commence day 5) – continue for 12 months Iron (dosing will vary from hospital to hospital, but for eg. May be given 0. 5 m. L/kg, daily dose, oral), given to babies <34 wks or <2 kgs at birth, commenced on day 14 (BHS practice, other hospitals differ) – continue for 6 months Na. Cl supplements (the more preterm the baby at birth the more likely they will need some Na. Cl supplementation during inpatient stay), dose varies KCl, Ca. Cl supplements (premature bone disease, need to replace these if depleted).
- Slides: 13