Fluids and Electrolytes Objectives To discuss fluid and

Fluids and Electrolytes

Objectives • To discuss fluid and electrolyte changes: • How to assess fluid patterns and changes in electrolytes • To focus on hypo and hypernatremia, hypo and hyperkalemia, hypo and hypercalcemia and hypophosphatemia

Most common fluid disorder deficits • Excessive loss / inadequate intake • G. I. losses from vomiting, nasogastric suction, diarrhea, and fistula drainage • Fluid sequestration • Pre and postoperative deficits • • • NPO Bowel prep Vomiting, NGT losses Ileus, obstruction Peritonitis
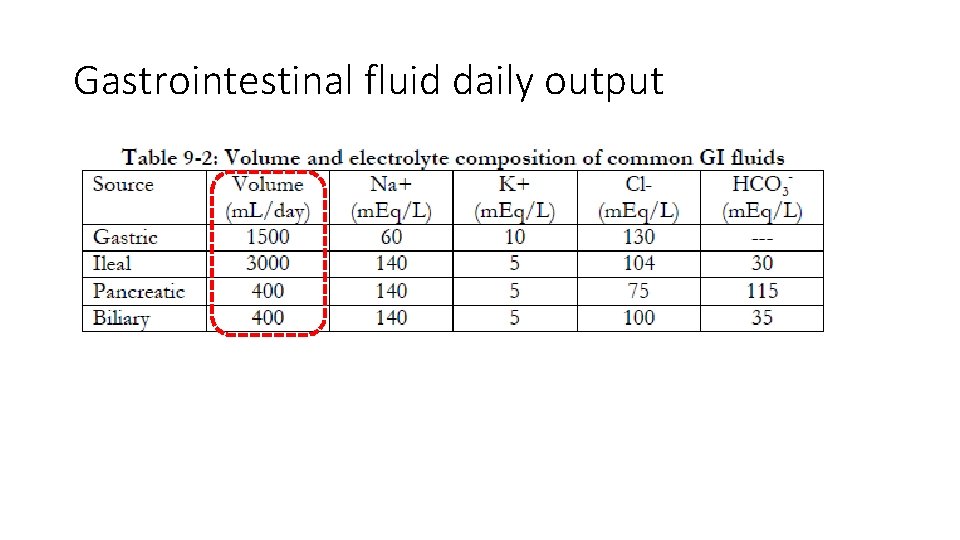
Gastrointestinal fluid daily output

How to assess and manage fluid status • Is the patient in need of fluid? How much? Plasma volume • If you know the amount of losses – replace them and deliver rapidly • Example: hypotensive patient given a 2 liter bolus as initial treatment Total Blood Volume 2 liters • If not: replace losses as they occur • Fluid given based on composition, tonicity of fluid lost • Example: ileostomy losses replaced volume per volume every 4 hrs with lactated Ringer’s solution (better with sterofundin) IVBV 5. 6 L ICF = 28 L IVFV 5%, plasma volume = 3. 5 L ECF = 14 L Resurreccion R. PCS Committee on Critical Care. Handbook of Critical Care and Surgical Nutrition First Ed, 2015. Philippine College of Surgeons • 70 kg male 8. 4 L = interstitial fluid

How to assess and manage fluid status • Is the patient in need of fluid? How much? • If you know the amount of losses – replace them and deliver rapidly RESUSCITATION • Example: hypotensive patient given a 2 liter bolus as initial treatment • If not: replace losses as they occur REPLACEMENT • Fluid given based on composition, tonicity of fluid lost • Example: ileostomy losses replaced volume per volume every 4 hrs with lactated Ringer’s solution (better with sterofundin) Plasma volume Total Blood Volume 2 liters IVBV 5. 6 L ICF = 28 L IVFV 5%, plasma volume = 3. 5 L ECF = 14 L Resurreccion R. PCS Committee on Critical Care. Handbook of Critical Care and Surgical Nutrition First Ed, 2015. Philippine College of Surgeons • 70 kg male 8. 4 L = interstitial fluid

How to assess and manage fluid status Maintenance requirements: after resuscitation and replacement MAINTENANCE Based on normal physiologic requirements Get the accurate weight Get the 5% plasma volume (70 kg x 5% = 3. 5 liters) Get 1/2 of the plasma volume = 3. 5 liters divided by ½ = 1. 75 liters Add the “insensible loss” of 70 kg x 0. 05 ml/kg/day = 300 + 1. 75 liters = 2. 05 liters/day or 2 liters/day • Similar to daily fluid requirement = kg BW x 30 cc/kg/day or 70 kg x 30 ml/kg/day = 2. 1 liters/day or 2 liters/day • • •

Fluid overload and mortality • Overload criteria: > 10% weight gain from pre-admission weight • Weight gain and mortality: • 5% weight gain -> 10% mortality • 15% weight gain -> 20% mortality • 32% weight gain -> 100% mortality Lowell JA, Schifferdecker C, Driscoll DF et al. Postoperative fluid overload: Not a benign problem. Crit Care Med 1990; 18: 728 -33.
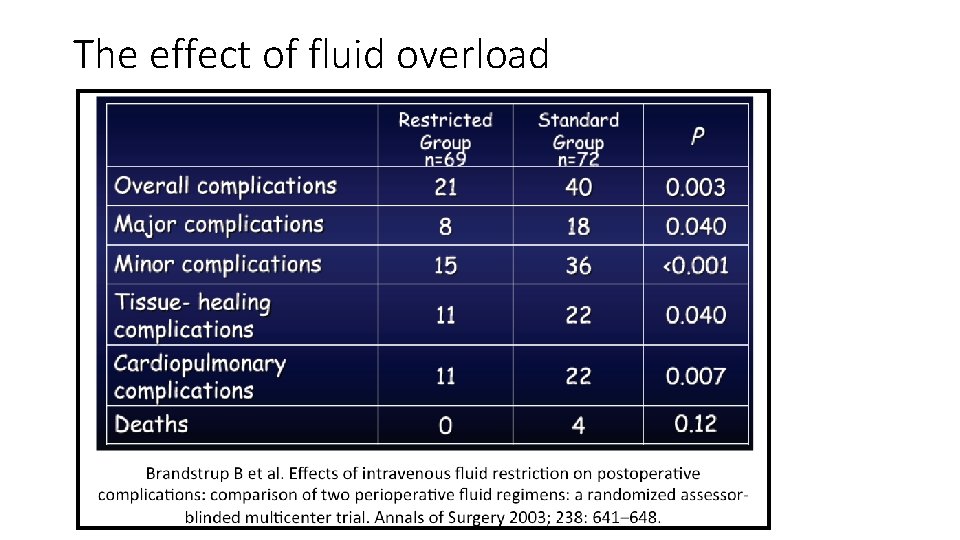
The effect of fluid overload

In the resuscitation phase what to do? • BLS and ATLS protocols • Not ABC, but CAB (=establish perfusion first to reach the microcirculation then oxygenation and the rest follows) • Ventilation: bag > mask > intubate • Establish intravenous line when possible (large bore needle) > central line is ideal if possible • Crystalloids: first line > give as much as 2 -3 liters fast (500 ml bolus every 15 -20 minutes) • Colloids: given as blood volume deficits • Medications: inotropes • Blood: Hb? Hct? what level? Aquino ML, Resurreccion R. PCS Committee on Critical Care. Handbook of Critical Care and Surgical Nutrition First Ed, 2015. Philippine College of Surgeons

Plasma and crystalloids given * Ringer’s Lactate Sterofundin* • Balanced electrolyte solution When you add dextrose to all of the above > HYPO-OSMOLAR
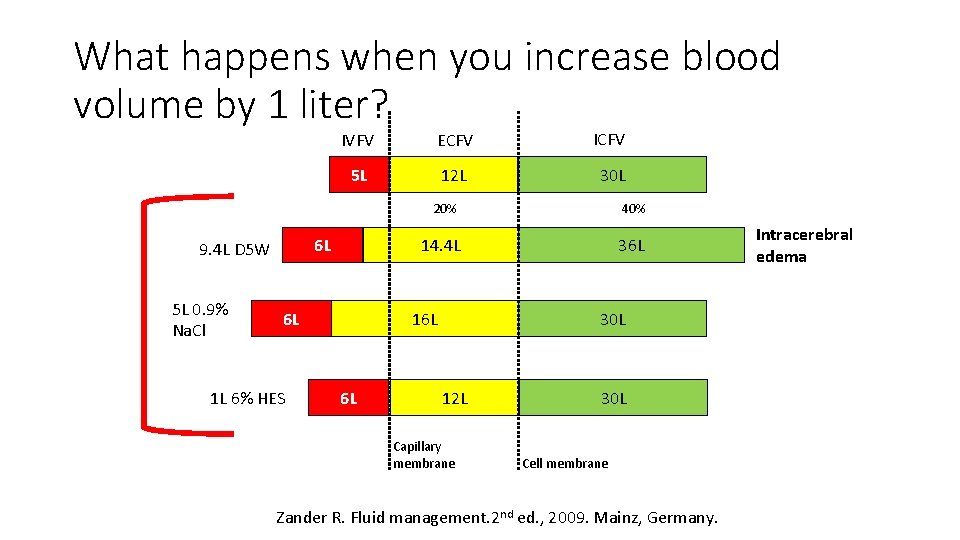
What happens when you increase blood volume by 1 liter? ECFV ICFV 5 L 12 L 30 L 6 L 9. 4 L D 5 W 5 L 0. 9% Na. Cl IVFV 6 L 1 L 6% HES 20% 40% 14. 4 L 36 L 16 L 6 L 30 L 12 L Capillary membrane 30 L Cell membrane Zander R. Fluid management. 2 nd ed. , 2009. Mainz, Germany. Intracerebral edema

Specific electrolyte management

Hyponatremia <135 • Determine volume status Hypovolemia • Give 0. 9 Na. Cl solution • Causes: • GI losses • Renal losses • Primary renal disease Principles of Surgery 10 th ed; G. Tom Shires III Euvolemia • Correct using hypertonic 3% Na. Cl (513 m. Eq/L) • Calculate for total sodium deficit in m. Eq = (135 – serum Na) x 0. 6 x kg body weight • Ex: (135 -130) x 0. 6 x 70 kg = 5 x 0. 6 x 70 = 210 m. Eq to add • Rate of correction should follow the following: • Risk of demyelinating encephalopathy with rapid correction of hyponatremia • Maximum rate of correction is 0. 5 m. Eq/L/hr Normovolemia • Water restriction (0. 5 – 1. 5 liter per day) (evidence of peripheral edema, ascites, pleural effusion • Avoid diuretics to lessen urinary Na+ losses • Correct hyperglycemia • Monitor and decrease increased plasma lipids or proteins • SIDH Resurreccion R. PCS Committee on Critical Care. Handbook of Critical Care and Surgical Nutrition First Ed, 2015. Philippine College of Surgeons

Hypernatremia > 140 • Determine volume status Hypovolemia • Non-renal water losses • Skin and GI losses • Renal water losses as in renal tubule disease • Osmotic diuresis • Diabetes insipidus • Adrenal failure Principles of Surgery 10 th ed; G. Tom Shires III Euvolemia • Non-renal water losses • Skin and GI losses • Renal water losses as in renal tubule disease • Osmotic diuresis • Diabetes insipidus • Adrenal failure Hypervolemia • Iatrogenic sodium administration • Mineralocorticoid excess • Aldosteronism • Cushing’s disease • Congenital adrenal hyperplasia Treatment for hypernatremia, regardless of its cause, is free water replacement. • For a 70 kg man with hypernatremia of 10, needs 3 liters of free water replacement

Hypernatremia correction • How to give free water replacement • H 2 O deficit (liters) = 0. 60 x weight (kg) x (serum Na – 140) ÷ 140 • Water deficit (L) = [0. 6 x 70 kg x (150 -140)] / 140 = 3 liters • One half of the water deficit should be given over the first 24 hours, with the remainder given over the next 24 to 48 hours • 3 liters – 24 hrs = 1. 5 liters in 24 hours • The rest in the next 24 to 48 hours (e. g. 1. 5 liters in 48 hours or 31 ml/hr for 48 hours) • If diabetes insipidus: • give DDAVP (Desmopressin), an ADH analogue • Minirin 100 mcg tablet every 12 hrs • DDAVP nasal spray 1μg/spray, 2 -4 μg BID Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS.

Hypokalemia < 3 • Serum potassium less than 3 m. Eq/L • Common problem in the surgical patient • Caveats • Measured extracellular potassium represents only a small proportion of total body potassium • Small changes in serum concentrations correspond to significant alterations in total body potassium • No reliable equation to compute for K deficit Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS.

Hypokalemia correction • Estimate of K+ deficit: • If serum K+: 3. 0 to 4. 0 m. Eq/L → total deficit: 100 to 200 m. Eq • If serum K+: 2. 0 to 3. 0 m. Eq/L → total deficit: 200 to 400 m. Eq • Management: • Intravenous: • Maximum rate of KCl infusion 10 m. Eq/hr (in the floors) to 20 m. Eq/hour (ICU under cardiac monitor) • Use central vein for KCl incorporation >40 m. Eq/L • • Oral: Kalium durule 0. 75 mg (10 m. Eq), 3 durules q 4 hrs NGT: do not crush Kalium! Use oral KCl solution (1 m. Eq/cc) Total max dose: 3 m. Eq/kg/day If persistently low K+ despite correction, check Mg levels for concurrent hypomagnesemia Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS.

Hyperkalemia > 5. 5 • Serum K+ greater than 5. 5 m. Eq/L • Management: • • • Cardiac monitoring indicated Renal excretion can be enhanced by the administration of loop diuretics K+ binding resins: ex. Kalimate 5 g/sachet 3 sachets in 1/2 glass of water BID Hemodialysis in renal failure Immediate treatment required if: • K+ > 6. 0 mmol/L with ECG changes or • K+ > 6. 5 mmol/L with or without ECG changes Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS.

Hyperkalemia correction • Management • Calcium gluconate 10% soln, 10 m. L IV over 2 to 5 minutes: to decrease myocardial excitability. Does not decrease K levels • Na. HCO 3 44 to 132 m. Eq (1 to 3 amps of 7. 5%) IV over 5 min, given after calcium in a separate line, repeat in 10 to 15 minutes, ff by infusion of 2 to 3 amps in D 5 W titrated over 2 to 4 hours • Insulin 10 to 20 U regular in D 10 W 500 m. L over 1 hour, or 10 U IV push with 1 amp 50% glucose (25 gm) over 5 mins. Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS.

Hypocalcemia < 2. 2 • Serum Ca < 2. 2 mmol/L • Artifact of hypoalbuminemia: serum calcium predominantly bound to albumin. • For every 1 g /L decrease in albumin, serum Ca decreases by 0. 02 mmol/L. • Symptoms: Chvostek’s sign, Trousseau’s sign • Management: • Calcium gluconate 10% soln, 10 – 20 m. L IV bolus over 10 to 15 minutes. Followed by 6 -8 10 m. L ampoules of 10% calcium gluconate in 1 L D 5 W • Maintenance: Calcium carbonate 1 -2 g P. O. TID with Vitamin D 3 (Calcitriol; brand name: Rolcaltrol) 0. 25 mcg capsule/day Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS.

Hypercalcemia > 3 • Serum Ca > 3. 0 mmol/L • Causes: • Hyperparathyroidism • Bone metastases (breast, lung, thyroid, colon, multiple myeloma) • Vitamin D intoxication • Management: • Hydration with normal saline • Diuretics (except thiazide diuretics) • Chronic therapy for: • Bone metastases: biphosphonate therapy • Paresthesias Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS.

Hypophosphatemia < 2. 5 • Serum phosphate < 2. 5 mg/dl • Normal levels: 2. 5 -4. 5 mg/dl or - 0. 801. 45 mmol/L • Classified as • Moderate: 0. 32 – 0. 65 mmol/L • Severe: < 0. 32 mmol/L • Causes • Transcellular shift (Refeeding syndrome; Phil incidence = 9%) • Diminished intake (long-term TPN, alcoholism) • Renal replacement therapy (deficiency of trace elements) Stanga R. Refeeding syndrome in ESPEN basic clinical nutrition manual. Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS. Mustofa N. Refeeding syndrome. Phils. PEN online j paren ent nutr. POJ_0097. html

Hypophosphatemia • Manifestations: • Muscle dysfunction: respiratory failure, myocardial dysfunction, skeletal muscle weakness, rhabdomyolysis • Altered mental status, seizures, encephalopathy • Arrhythmia: ventricular tachycardia, supraventricular tachycardia • Hemolysis • • • Jeejeebhoy. Malnutrition, , starvation and Refeeding Syndrome. Stanga R. Refeeding syndrome in ESPEN basic clinical nutrition manual. Resurreccion R. Fluids, electrolytes and acid base management in Handbook of Surgical Critical Care and Surgical Nutrition 1 st ed. PCS.

Thank You
- Slides: 25