Fluid Therapy in the Surgical Patient CTVT pgs
































- Slides: 38

Fluid Therapy in the Surgical Patient CTVT pgs. 883 -894 A&A pgs. 27 -39 (Anesthetist) *Step-by-step fluid calculation on my website

Indications for Fluid Administration �Dehydration �Hypovolemia �Disease that depletes the normal fluid and electrolyte balance (polyuria, decreased intake of fluids, diarrhea) �Surgery �Potential of fluid loss or excessive blood loss �Maintenance of blood pressure and organ perfusion

Normal Fluid Balance �The body is made up of approximately 60% water �This is divided into intracellular (2/3 of body fluid) and extracellular fluids (1/3 of body fluid) �Extracellular fluid is further divided into �Interstitial- fluid in your body’s tissues �Intravascular- fluid in the vessels �The body maintains fluid balance (homeostasis) on a constant basis �Works via osmotic pressure

Normal Fluid Balance �Osmotic pressure �Number of positive and negative charges in an area must be equal: �Water- moves freely, follows Na+ �Electrolytes- rely on positive and negative charges to maintain balance � ICF- Potassium(+) and Magnesium (+) Phosphate (-) � ECF- Sodium (+) and Chloride (-) Normal plasma osmolarity is 300 m. Osm/L

Fluid Treatment Questions �How much fluid will be needed to rehydrate the patient, right now? �How much fluid will be needed to compensate for ongoing losses? �How much fluid will be needed to maintain the animal’s daily necessary requirements? �What is the animal’s surgical fluid rate? Total circulating blood volume: Dog = 85 ml/kg Cat = 55 ml/kg

Daily Maintenance Requirements Sensible losses (measurable losses) �Urine output � 1 -2 ml/kg/hr = normal Insensible losses �Feces �Respiration

Unexpected Fluid Loss Ongoing Losses �Vomiting �Diarrhea �Polyuria �Pleural effusion �Blood loss �Add to rehydration calculation Every 1 ml lost = 2 mls of replacement fluid needed

Assessing Dehydration 1. Skin turgor test � � What about obese animals? Emaciated animals? 2. Mucous membranes (MM) � Moist/tacky/dry? 3. Eye position 4. Serial body weights *Loss of 1 kg during a 24 hour period is about equal to loss of 1 L of water.

Assessing Perfusion 1. Capillary refill time (CRT) � Normal value? 2. Heart rate & pulse 3. Blood pressure 4. Cool extremities

Routes of Fluid Administration Oral: minimal loss, normal intake Subcutaneous: mild-moderate dehydration � Given on dorsal midline/flank Intravenous: moderate-severe dehydration; perioperative precaution Intraperitoneal: mild to moderately dehydrated; large volumes � This method is not commonly used in cats and dogs Intraosseous: head of the femur/humerus of small animals � Neonates or animals with poor venous access; birds and reptiles

Intravenous Catheterization Why is this important? �Provide fluid therapy �Administer emergency drugs quickly �Name two (NAVEL) �Leave in until patient is fully recovered! �CRI of analgesics or anesthetics �Calculations to follow… �Induce anesthesia �Can easily titrate IV medications on a sedated animal �Safely administer vesicants

Anesthetic fluid therapy �Requires IV catheter placement �What vein? �What size? �Prep site- what technique? �Considerations/Risks �Transfer of patient- disconnecting from P or air introduced �Injection port- drugs must be injected slowly! �Limb ties �Non-aseptic technique �Hypervolemia

Purpose of Anesthetic Fluid Therapy �To maintain blood volume AND pressure �Be prepared for expected OR unexpected blood loss � What’s an example of a bloody surgery? �Combat bradycardia & vasodilation due to anesthetic drugs � Your anesthetized patient WILL have hypotension � Especially long surgeries �Correct known dehydration or electrolyte abnormalities � How do we know this? ?

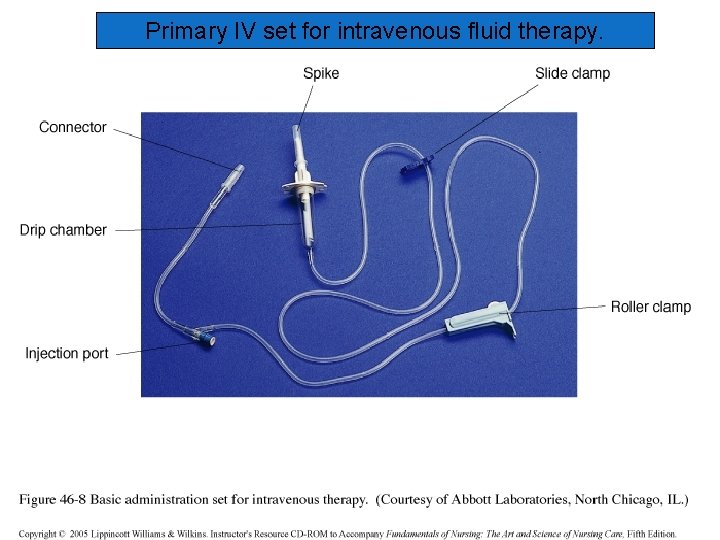
Primary IV set for intravenous fluid therapy.

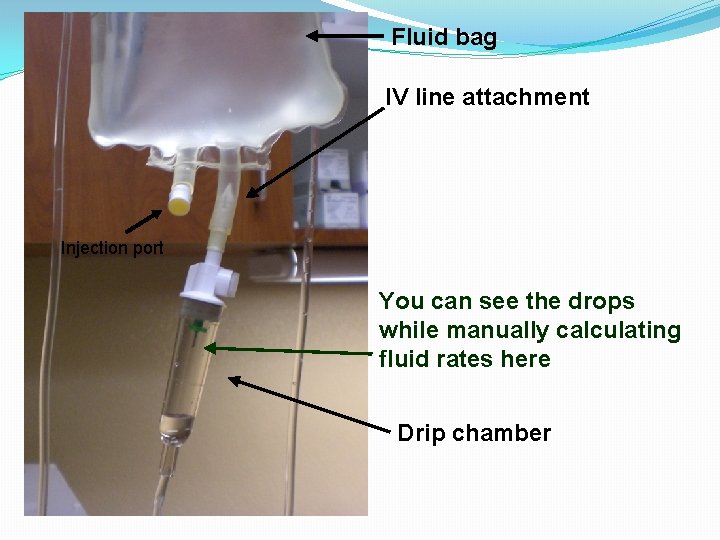
Fluid bag IV line attachment Injection port You can see the drops while manually calculating fluid rates here Drip chamber

IV pumps come in many brands and sizes. BAXTER 6300 DOUBLE PUMP IV Pump/ Fluid Stand

HESKA VET IV infusion pump

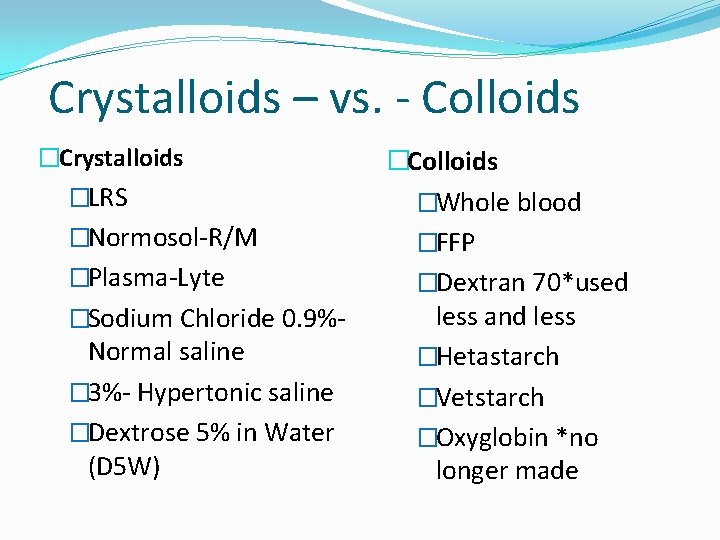
Crystalloids –vs- Colloids �Crystalloids are solutions of salts and water with variable electrolyte composition and contain no protein or colloids �Are in intravascular compartment for less than an hour �Rapidly excreted in urine (if renal function is normal) �Classified by their osmolarity: Isotonic, hypertonic, or hypotonic �Colloids contain larger insoluble molecules, which act to retain existing fluid and promote movement of fluid into intravascular spaces �Remain within the circulation (cannot freely cross vascular endothelium)

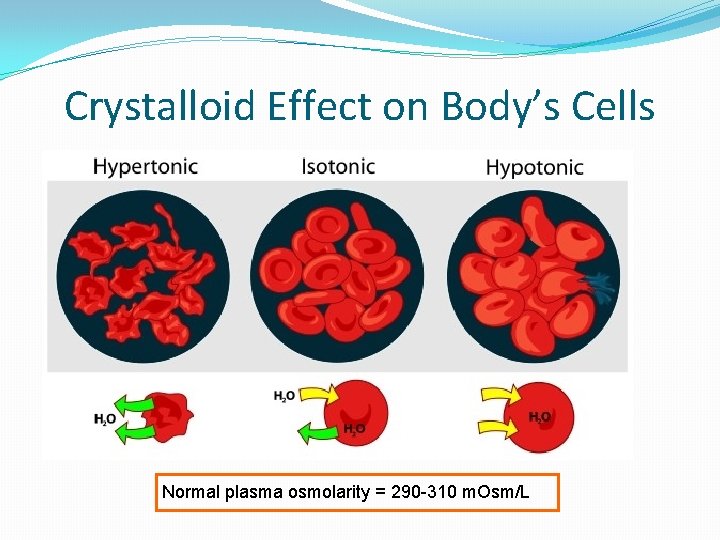
Crystalloid Effect on Body’s Cells Normal plasma osmolarity = 290 -310 m. Osm/L

Hypotonic Crystalloids �Lower osmotic pressure (osmolarity) than blood – thereby encouraging movement of fluids into interstitial fluid and then into cells �Contain low amounts of Na+ and Cl�Indicated for maintenance of cardiac patients or hypernatremic patients �Examples: � 5% Dextrose in water (D 5 W) � 0. 45% Saline (Na. Cl) �Normasol-M; Plasmalyte 56 *Provide more water than electrolytes*

Isotonic Crystalloids �Most common type of fluids used to replace body fluids; osmolarity = to blood �Rehydration, maintenance, and anesthesia � 0. 9% saline, BES, or Dextrose solutions Note: dextrose solutions are used for specific purposes, not for maintenance or shock �For each 1 ml increase in vasculature fluid, you need to give 3 -4 mls of isotonic fluid

Isotonic Crystalloids �Normal Saline (0. 9% Na. Cl) -slightly acidifying effect due to high Cl� Used for irrigation, lavage, flush �Balanced electrolyte solutions Contain other electrolytes in addition to Na+ and Cl� Such as? � Buffered alkalinizing affects due to bicarbonate precursors (lactate) Examples: Normasol-R, LRS, Plasmalyte 148

Hypertonic Crystalloids �Saline greater than 0. 9% (ex. 3% Na. Cl, 7% Na. Cl) �Administered for resuscitation or shock �Greater osmotic pressure than blood -encouraging movement of fluid from the interstitial space into circulation (vasculature) �Why is this a “quick fix”? �Quickly increases blood volume and pressure �For each 1 ml given, increases vasculature volume by 5 -10 mls NOTE: If given too quickly, can cause interstitial or ICF dehydration *Provides more electrolytes than it provides water*

Colloids �Contains large molecules suspended in an isotonic crystalloid �Used for resuscitation –hypoproteinemia, acute blood loss, clotting disorders �Natural or synthetic �Whole blood and plasma transfusions � Increase IVF and perfusion when RBCs are abnormal � Anaphylaxis �Hetastarch and Vetstarch � Increase IVF and perfusion when RBCs are normal

Crystalloids – vs. - Colloids �Crystalloids �LRS �Normosol-R/M �Plasma-Lyte �Sodium Chloride 0. 9%- Normal saline � 3%- Hypertonic saline �Dextrose 5% in Water (D 5 W) �Colloids �Whole blood �FFP �Dextran 70*used less and less �Hetastarch �Vetstarch �Oxyglobin *no longer made

General Rule of thumb �Know drug compatibilities! �It can be undesirable to mix multiple drugs in a syringe or intravenous fluids- sometimes drug interactions are visible, other times they are not �Physical incompatibilities include: precipitation and chemical inactivation �Fluids should be warmed before being given �Fluid incubator, line warmer, “warmies” � What colors should NOT be added to warmies?

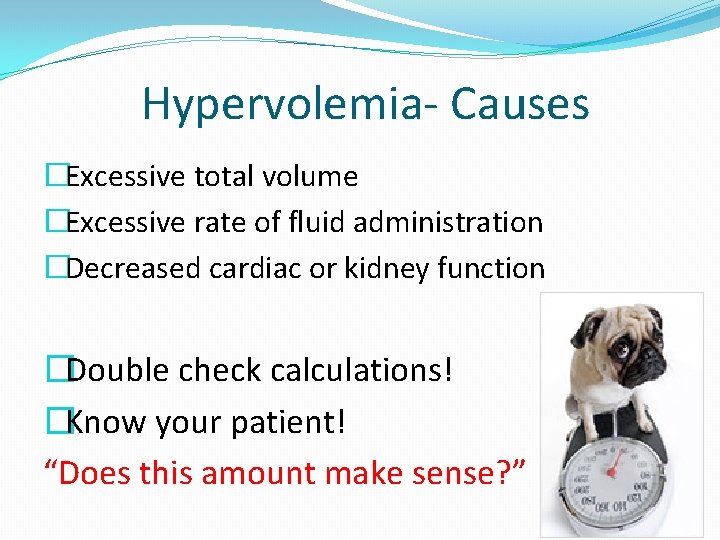
Hypervolemia- Causes �Excessive total volume �Excessive rate of fluid administration �Decreased cardiac or kidney function �Double check calculations! �Know your patient! “Does this amount make sense? ”

Hypervolemia- Clinical Signs �Serous nasal discharge �Chemosis- edema of the ocular conjunctiva �Pitting edema –skin remaining indented for a prolonged amount of time after removal of firm finger pressure (Over saturation of the cells) �Restlessness and coughing- during recovery �Hyperpnea- abnormal increase in depth and rate of respiration but not to the point of labored

Fluid Protocols and Rates �Maintenance �Rehydration �Anesthesia �Resuscitation/Shock Calculation examples on page 38 of A&A

Maintenance Rate �Maintenance volume is the amount of fluid and electrolytes needed on a daily basis to keep the volume of water and electrolyte content normal in a well-hydrated patient �Animals that refuse or cannot eat, recently dehydrated �Remember insensible and sensible losses? 40 -60 ml/kg/24 h �Usually isotonic crystalloids

Maintenance Problem �A 10 lb 4 year old s/F DSH named Arlene has recovered from anesthesia for major dental surgery and will probably not be eating or drinking. Your vet would like her to be on IV fluids overnight from 6 pm-7 am. 1. What type of fluids would you prepare? 2. How many milliliters per hour will you set your pump to? 3. What’s the minimum amount of fluid you should ensure is in the fluid bag before clocking out? 4. How many gtt/sec will Arlene receive if your pump breaks? (Your infusion set is 60 gtt/ml)

Rehydration Formula % dehydrated x body weight (kg) x 1000 ml/kg = ml of fluid needed for replacement �This formula is used for patients who are dehydrated and may or may not have ongoing losses (i. e. vomiting / diarrhea) �To be given over a specified period of time �We also have to account for ongoing losses Ex: 20 ml excessive urine = 40 ml fluid

Rehydration Problem �A 5 yr old, 11 lb Pomeranian is 6% dehydrated and has vomited about 25 mls since he was admitted to your clinic for surgery today. Your vet asks to correct his fluid status over the next 3 hours with IV LRS. 1. What vein would you most likely place an IV catheter in? 2. What gauge would you choose? 3. How many mls/hr will you set your fluid pump to? 4. gtt/sec?

Anesthetic Protocol �To compensate for losses during surgery �To sustain oxygen saturation and tissue perfusion �Common rate is 10 ml/kg/hr (old school) CATS: 3 ml/kg/hr DOGS: 5 ml/kg/hr �Hypotension? *Can increase to 20 ml/kg/hr (cats) and 40 ml/kg/hr (dogs)

Anesthetic Protocol Calculation �Your next surgical patient is a 28 lb spaniel mix OHE. Her blood work was WNL and she has no known disease. 1. What fluid type will your vet most likely choose? 2. What will the rate of fluid administration be per hour? 3. How many gtt/sec using a 15 gtt/ml set?

Resuscitation/Shock Protocol �Patient: �Is experiencing hypovolemia or shock state �Has lost significant amount of total blood volume If a 20 lb dog lost 10% of its blood volume, how many mls of blood would this be? �Goal is to replace fluid in the vasculature AND increase perfusion Dogs Cats Isotonic fluids: 80 -90 ml/kg 55 ml/kg Hypertonic crystalloids: 3 -4 ml/kg 2 -3 ml/kg Colloids: 10 -20 ml/kg 5 -10 ml/kg

Resuscitation/Shock �Give ¼ of total dose as a bolus �Check parameters and reassess �By using crystalloids and colloids together, you can increase benefits and decrease side effects. �Calculate half the shock dose of each, still only give ¼ of that

Resuscitation Problem �A 3 year old 50 lb Labrador retriever is in hypovolemic shock and needs IV Hetastach per Dr. Dev. 1. What is the total dose of Hetastarch in mls? 2. How much Hetastarch will you give initially?