Fluid is a Drug Late Conservative Fluid Management




![Percent Fluid Overload (%FO) %FO = Σ [FLUID IN – FLUID OUT] x 100 Percent Fluid Overload (%FO) %FO = Σ [FLUID IN – FLUID OUT] x 100](https://slidetodoc.com/presentation_image_h/19de90ae5ba50b159708f769c3252e4b/image-8.jpg)










- Slides: 34

Fluid is a Drug: Late Conservative Fluid Management Sean M Bagshaw, MD, MSc Division of Critical Care Medicine Faculty of Medicine and Dentistry, University of Alberta 1 st International Symposium on AKI in Children Cincinnati, Ohio September 28, 2012

Disclosure Summary • Sean M Bagshaw, MD, MSc – Consultancy: Gambro Inc. – Speaking: Gambro Inc. , Alere Inc.

Learning Objectives • Review and Discuss: – Fluid Overload – Fluid Management – Concept of “De-Resuscitation”

‘The dose makes the poison’ Paracelus

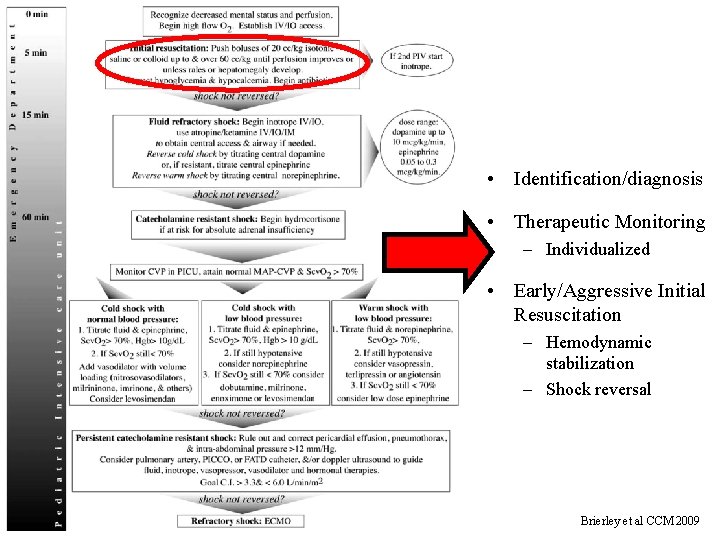
• Identification/diagnosis • Therapeutic Monitoring – Individualized • Early/Aggressive Initial Resuscitation – Hemodynamic stabilization – Shock reversal Brierley et al CCM 2009

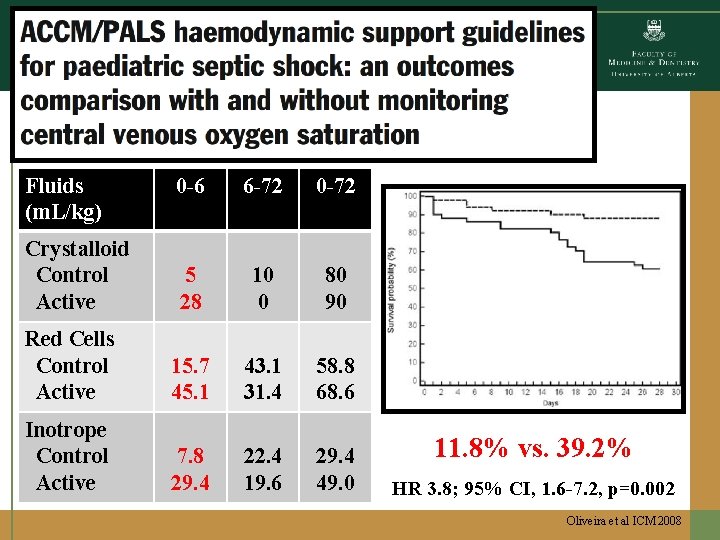
Fluids (m. L/kg) 0 -6 6 -72 0 -72 5 28 10 0 80 90 Red Cells Control Active 15. 7 45. 1 43. 1 31. 4 58. 8 68. 6 Inotrope Control Active 7. 8 29. 4 22. 4 19. 6 29. 4 49. 0 Crystalloid Control Active 11. 8% vs. 39. 2% HR 3. 8; 95% CI, 1. 6 -7. 2, p=0. 002 Oliveira et al ICM 2008

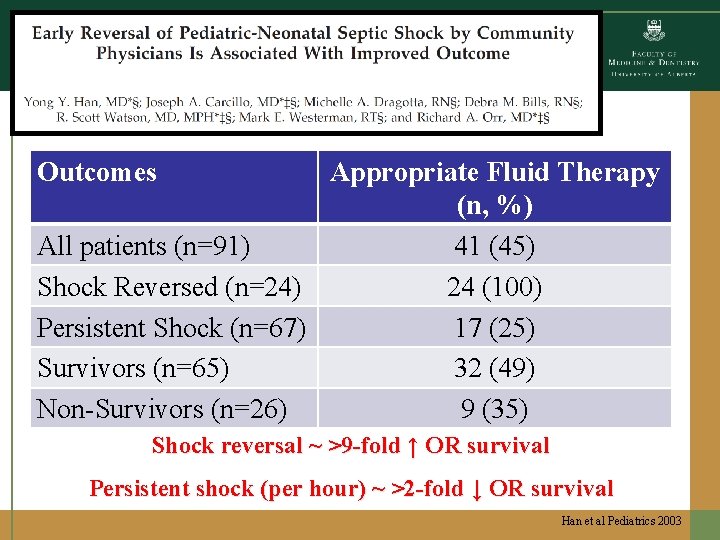
Outcomes Appropriate Fluid Therapy (n, %) All patients (n=91) 41 (45) Shock Reversed (n=24) 24 (100) Persistent Shock (n=67) 17 (25) Survivors (n=65) 32 (49) Non-Survivors (n=26) 9 (35) Shock reversal ~ >9 -fold ↑ OR survival Persistent shock (per hour) ~ >2 -fold ↓ OR survival Han et al Pediatrics 2003
![Percent Fluid Overload FO FO Σ FLUID IN FLUID OUT x 100 Percent Fluid Overload (%FO) %FO = Σ [FLUID IN – FLUID OUT] x 100](https://slidetodoc.com/presentation_image_h/19de90ae5ba50b159708f769c3252e4b/image-8.jpg)
Percent Fluid Overload (%FO) %FO = Σ [FLUID IN – FLUID OUT] x 100 [Admission Weight (kg)] Goldstein et al Pediatrics 2001

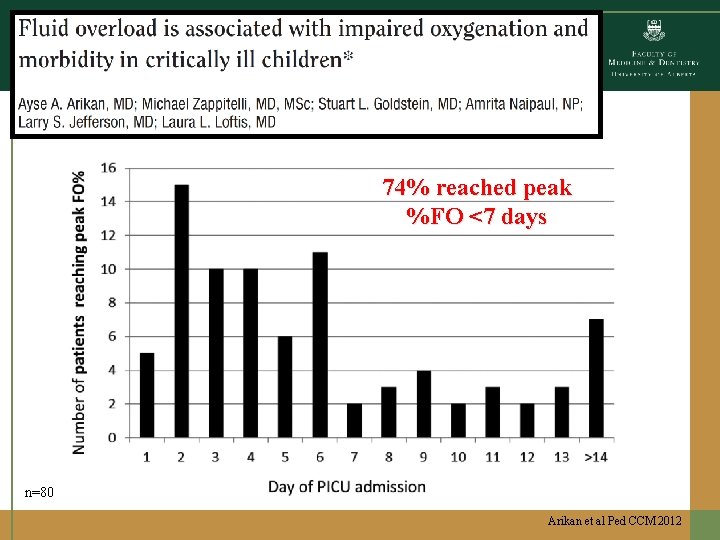
74% reached peak %FO <7 days n=80 Arikan et al Ped CCM 2012

Goldstein et al Pediatrics 2001

• “It is possible that in some cases CVVH/D may be a prevention, rather than a treatment, for worsening degrees of fluid overload. ” • “Early initiation of CVVH to allow for sufficient blood product and nutrition administration, while preventing fluid overload may improve patient survival…” Goldstein et al Pediatrics 2001

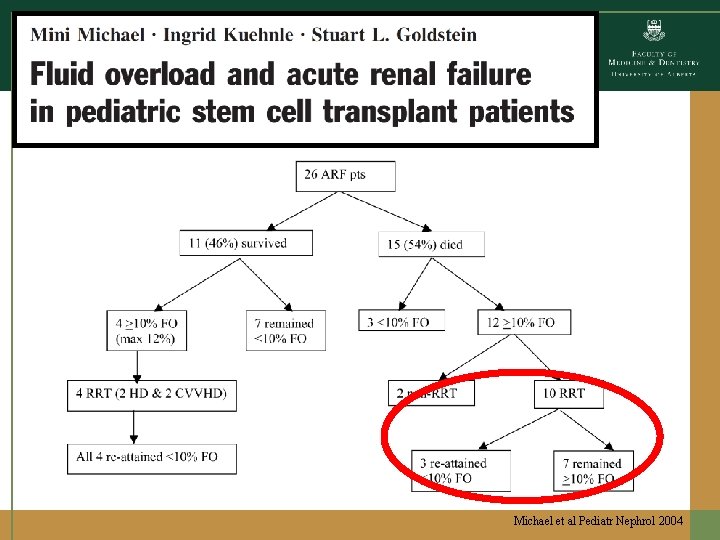
Michael et al Pediatr Nephrol 2004

%FO>10% for PICU Admission: 68. 4% vs. 22. 1%, p<0. 001 Risk factors for %FO>10% ~ smaller children; AKI Indications for CRRT Initiation ~ FO in 39% %FO at CRRT Initiation ~ 10. 6% vs. 13. 9% (p=NS) Benoit et al Pediatr Nephrol 2007; Flores et al Pediatr Nephrol 2008

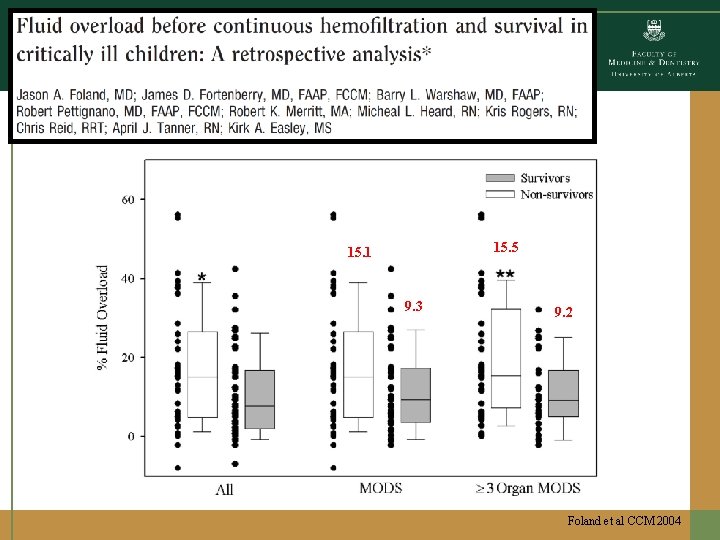
15. 5 15. 1 9. 3 9. 2 Foland et al CCM 2004

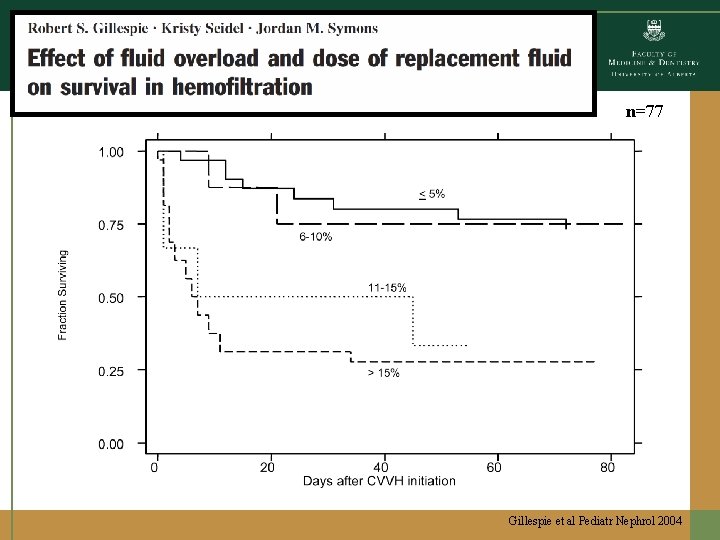
n=77 Gillespie et al Pediatr Nephrol 2004

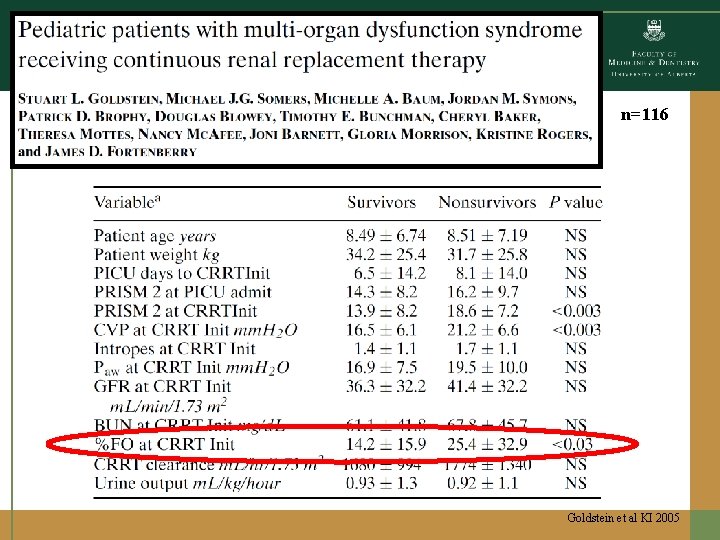
n=116 Goldstein et al KI 2005

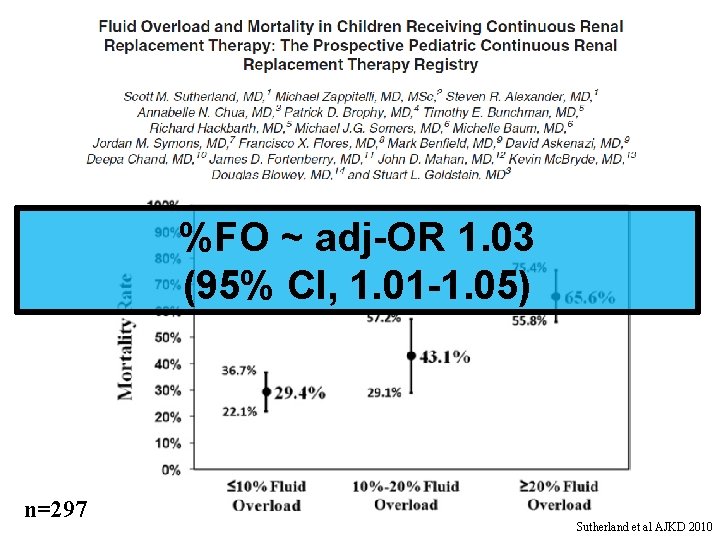
%FO ~ adj-OR 1. 03 (95% CI, 1. 01 -1. 05) n=297 Sutherland et al AJKD 2010

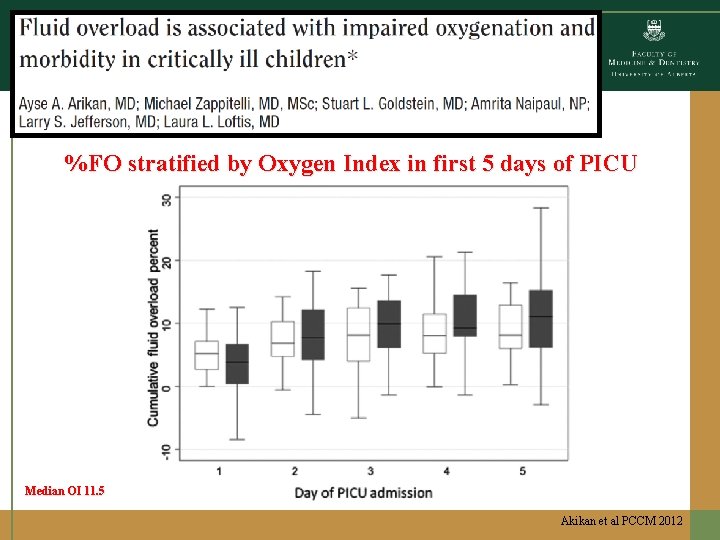
%FO stratified by Oxygen Index in first 5 days of PICU Median OI 11. 5 Akikan et al PCCM 2012

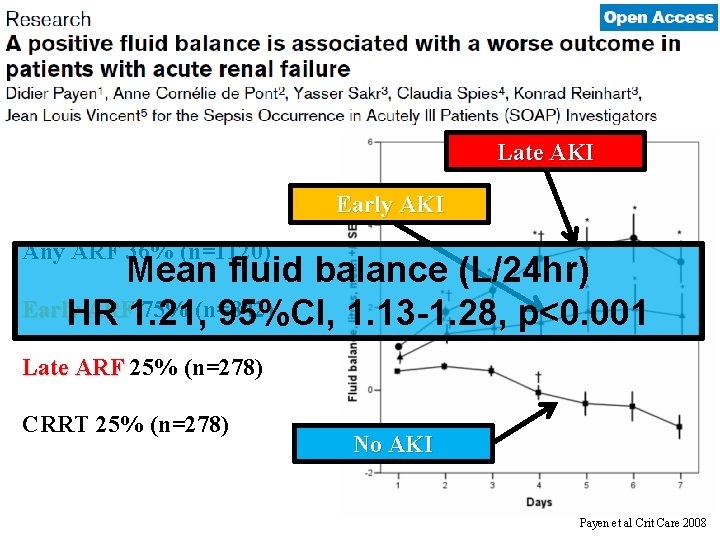
Late AKI Early AKI Any ARF 36% (n=1120) Mean fluid balance (L/24 hr) Early ARF 1. 21, 75% (n=842) HR 95%CI, 1. 13 -1. 28, p<0. 001 Late ARF 25% (n=278) CRRT 25% (n=278) No AKI Payen et al Crit Care 2008

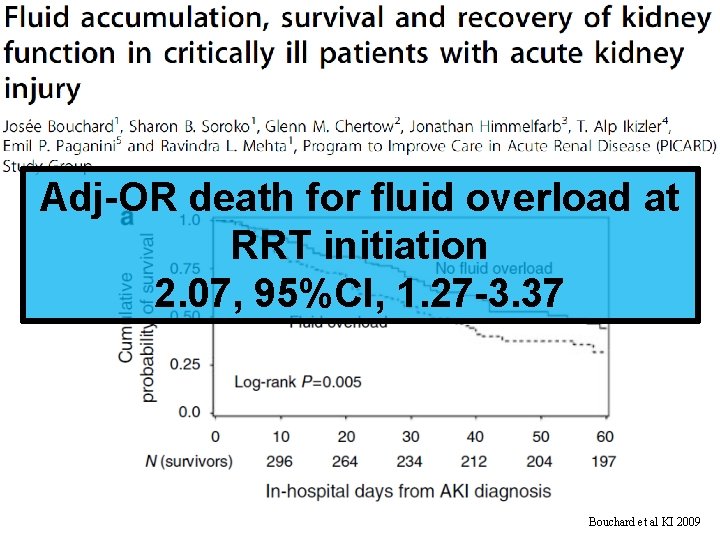
Fluid Overload at RRT Initiation Adj-OR death for fluid overload at RRT initiation 2. 07, 95%CI, 1. 27 -3. 37 Bouchard et al KI 2009

Prowle et al NRN 2010

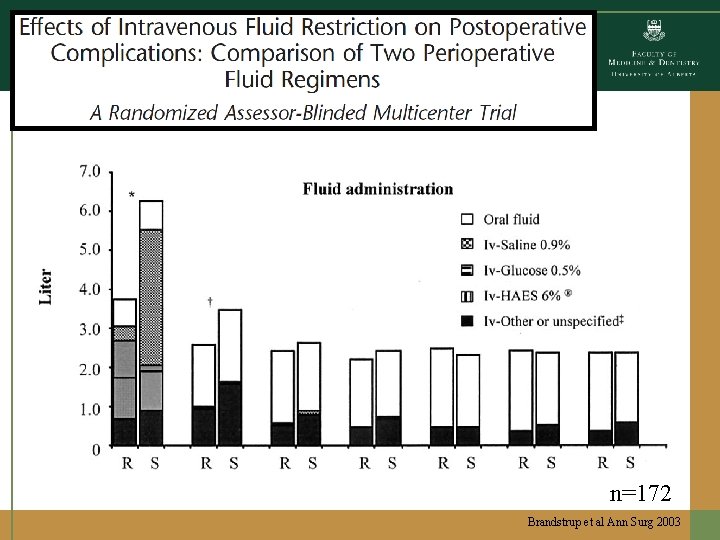
Challenges… • Available literature: – Small sample size – Retrospective or Registry data • Few data from INTERVENTIONAL trials: – Focused specifically on children! – Fluid management AFTER initial resuscitation – Focused on strategies for fluid management: • Volume: “Conservative” vs. “Liberal” (standard) • Type: Crystalloid or Colloid; Isotonic or Balanced

n=172 Brandstrup et al Ann Surg 2003

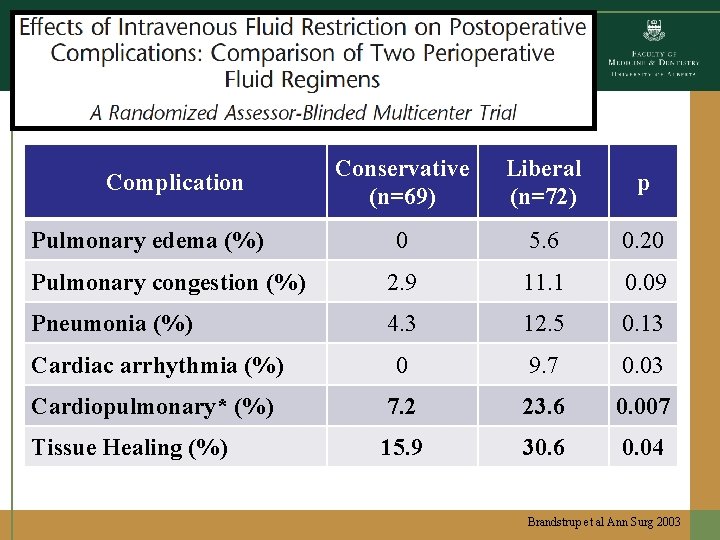
Conservative (n=69) Liberal (n=72) p 0 5. 6 0. 20 Pulmonary congestion (%) 2. 9 11. 1 0. 09 Pneumonia (%) 4. 3 12. 5 0. 13 Cardiac arrhythmia (%) 0 9. 7 0. 03 Cardiopulmonary* (%) 7. 2 23. 6 0. 007 Tissue Healing (%) 15. 9 30. 6 0. 04 Complication Pulmonary edema (%) Brandstrup et al Ann Surg 2003

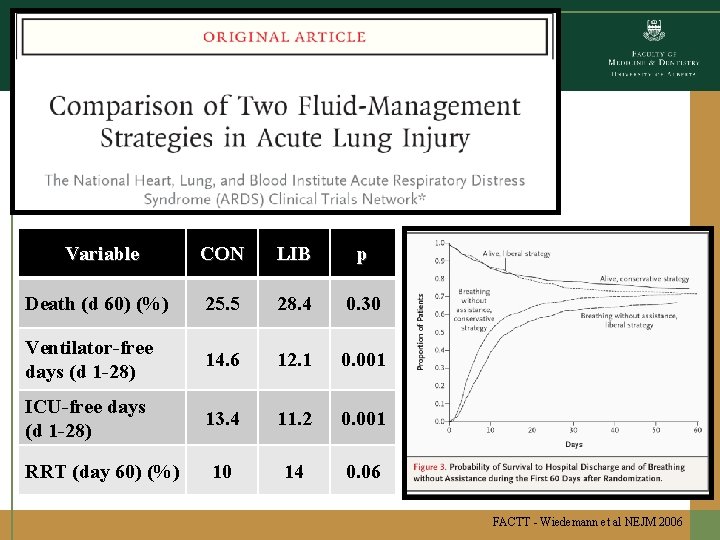
Variable CON LIB p Death (d 60) (%) 25. 5 28. 4 0. 30 Ventilator-free days (d 1 -28) 14. 6 12. 1 0. 001 ICU-free days (d 1 -28) 13. 4 11. 2 0. 001 10 14 0. 06 RRT (day 60) (%) FACTT - Wiedemann et al NEJM 2006

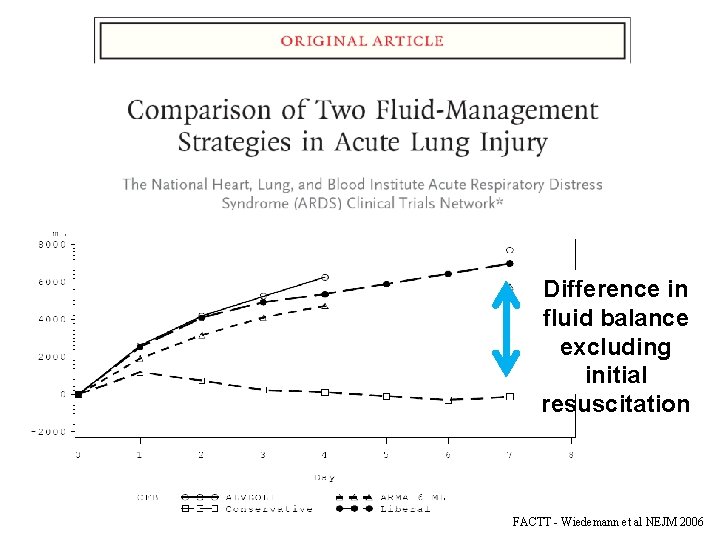
Difference in fluid balance excluding initial resuscitation FACTT - Wiedemann et al NEJM 2006

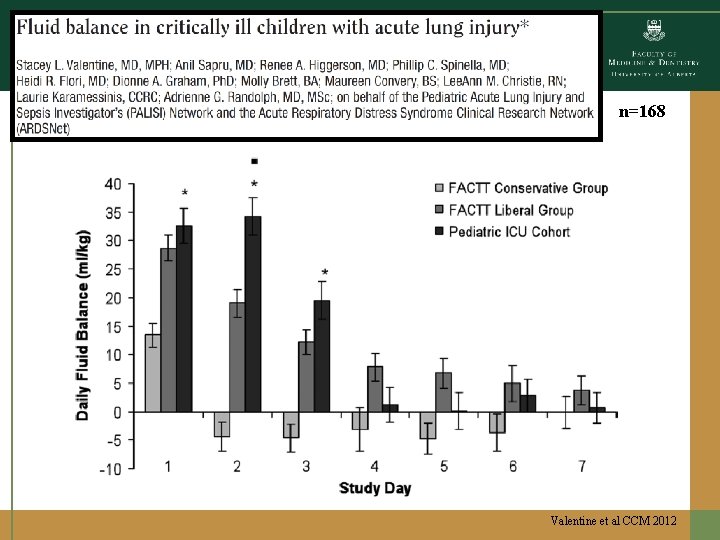
n=168 Valentine et al CCM 2012

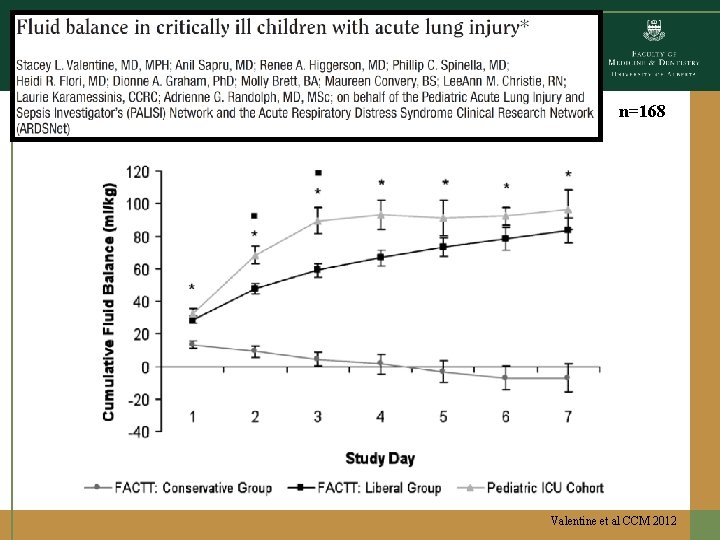
n=168 Valentine et al CCM 2012

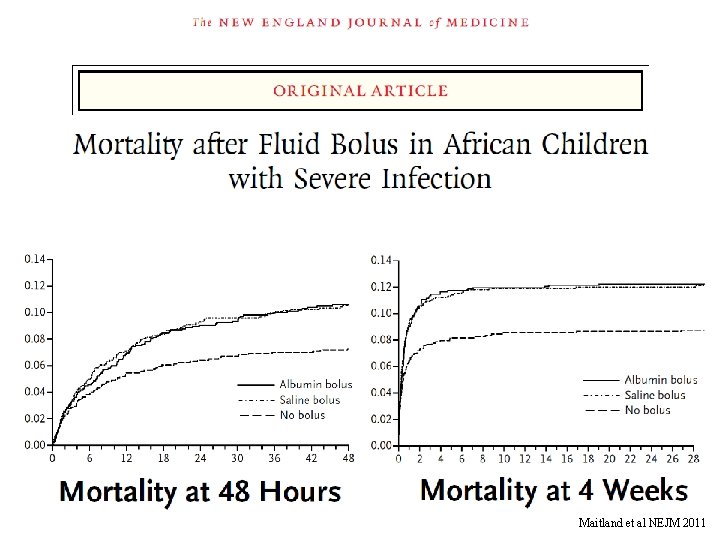
Maitland et al NEJM 2011

24 bags ≈ 9000 mg Na. Cl ≈

Next Steps… • Body has not evolved a natural mechanism to remove excess ↑ Na+ and water • “De-resuscitation” in MODS/AKI? – When can fluid be ideally removed? Triggers? – How much fluid should/must be removed?

NGAL-Directed RRT Initiation Use of Neutrophil Gelatinase-Associated Lipocalin (NGAL) to Optimize Fluid Dosing, Continuous Renal Replacement Therapy (CRRT) Initiation and Discontinuation in Critically Ill Children With Acute Kidney Injury (AKI) Clinical. Trials. gov Identifier: NCT 01416298 Available at: http: //www. clinicaltrials. gov/ct 2/show/NCT 01416298? term=NCT 01416298&rank=1

Summary • (Excessive) fluid accumulation is bad • Contribute to and/or worsen AKI/MODS • Short/longer term injury to non-renal organs • ↑ Risk morbidity/poor outcomes • Need to better understand ideal strategies to (safely) mitigate and/or remove excess extravascular fluid

Thank You For Your Attention! Questions? bagshaw@ualberta. ca