Fluid and Electrolyte Imbalance Chapter 13 Fluid and

Fluid and Electrolyte Imbalance Chapter 13

Fluid and Electrolytes • • • Necessary for life, homeostasis Nursing role: help prevent; treat fluid, electrolyte disturbances Know the normal values Understand hypo and hyper Use SBAR and report changes Monitor all labs and medications

Regulation of Fluid • Osmosis: area of low solute concentration to area of high solute concentration • Diffusion: solutes move from area of higher concentration to one of lower concentration • Filtration: movement of water, solutes occurs from area of high hydrostatic pressure to area of low hydrostatic pressure • Active transport: physiologic pump that moves fluid from area of lower concentration of one of higher concentration
Fluid and Electrolyte Imbalance
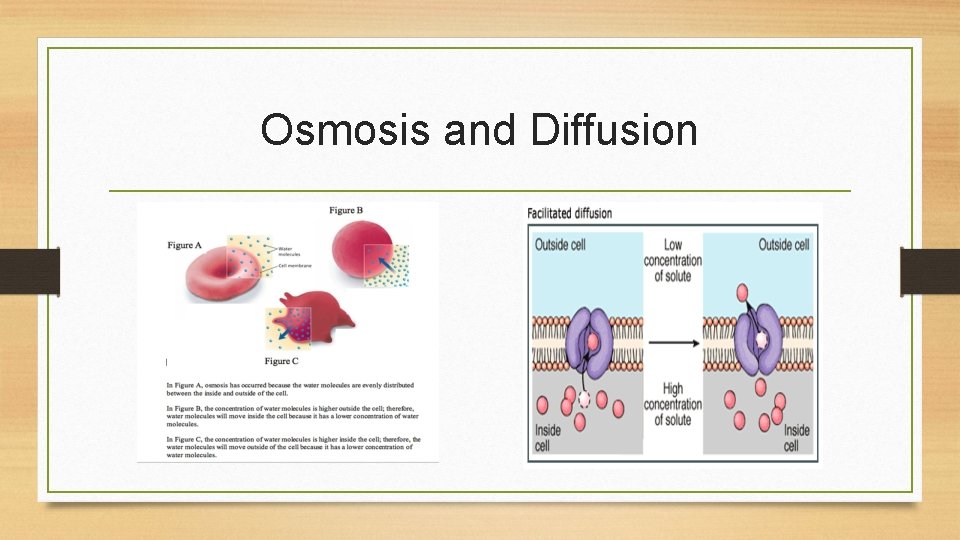
Osmosis and Diffusion
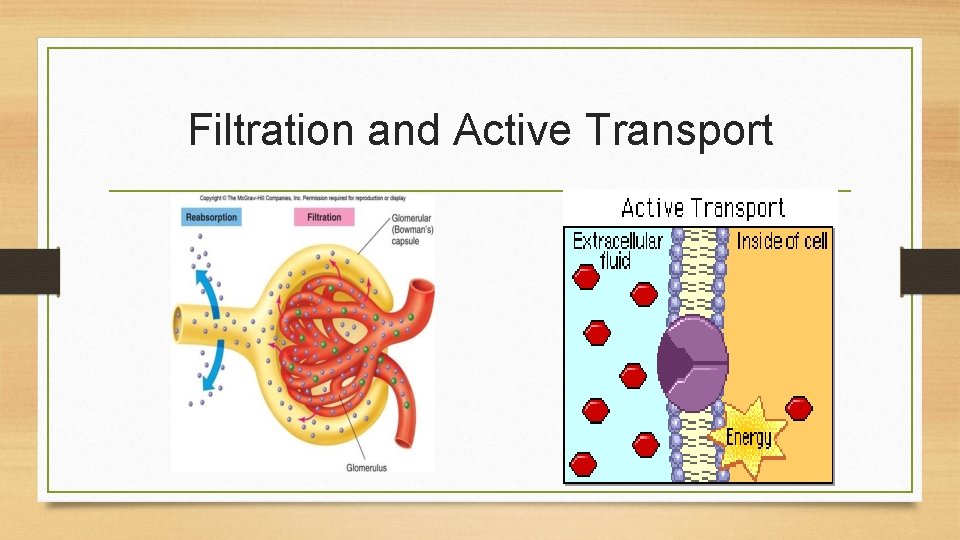
Filtration and Active Transport

Active Transport • Physiologic pump that moves fluid from area of lower concentration to one of higher concentration • Movement against concentration gradient • Sodium–potassium pump: maintains higher concentration of extracellular sodium, intracellular potassium • Requires adenosine (ATP) for energy

Baroreceptors Respond to changes in circulating blood volume
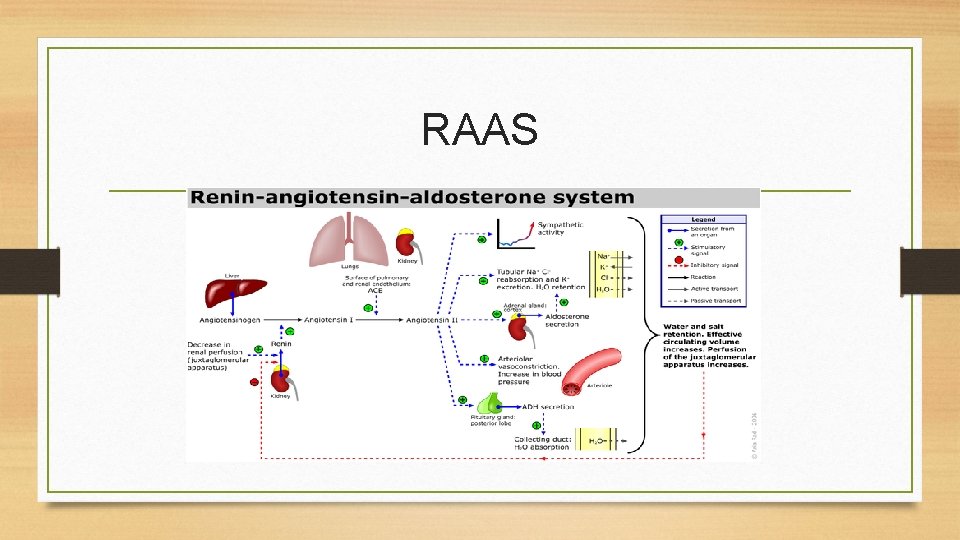
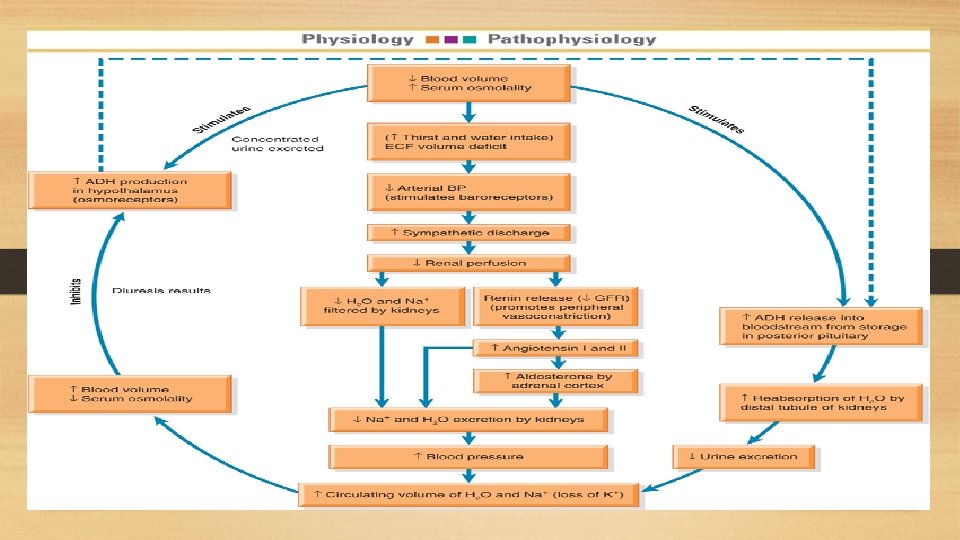
RAAS
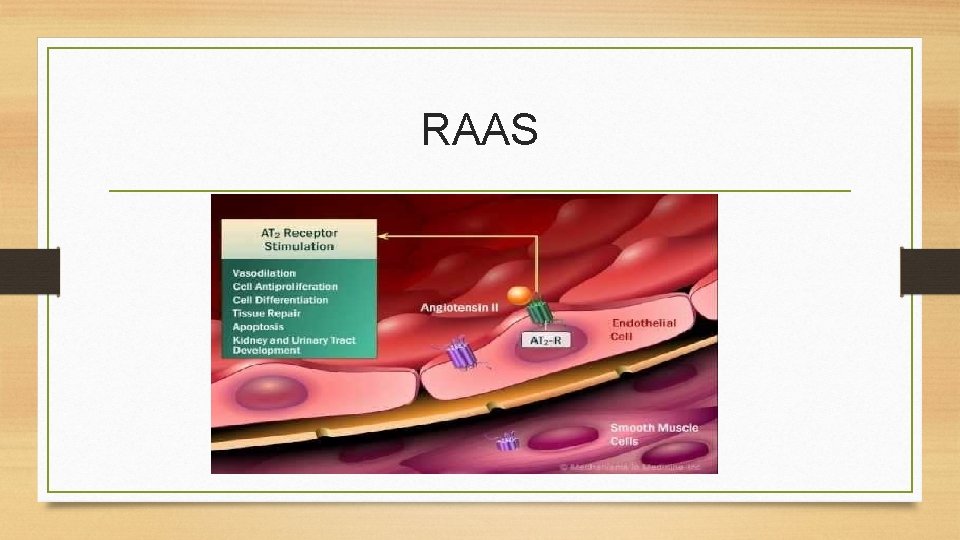
RAAS
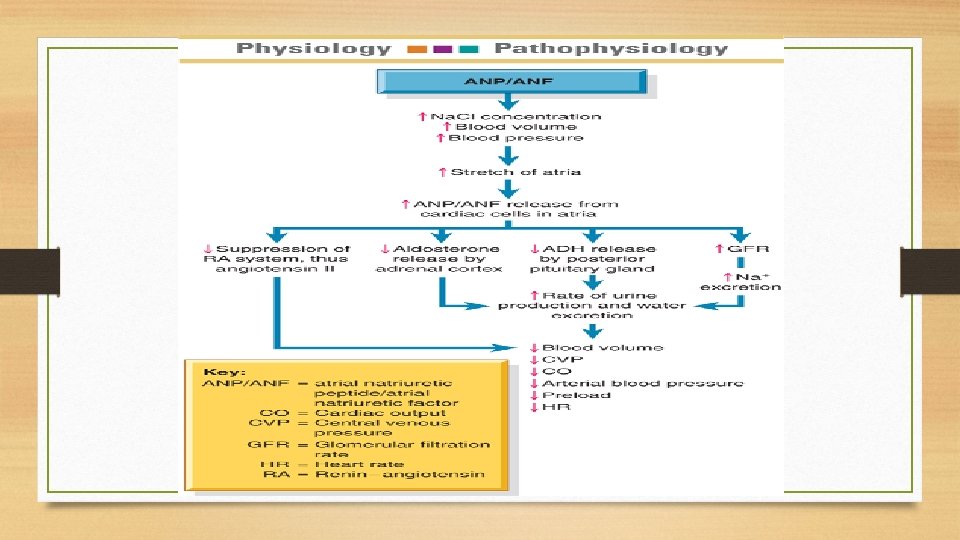

Gerontologic Considerations • Reduced homeostatic mechanisms: cardiac, renal, respiratory function • Decreased body fluid percentage • Medication use • Presence of concomitant conditions

Fluid Volume Imbalances • • Fluid volume deficit (FVD): hypovolemia Fluid volume excess (FVE): hypervolemia Think of causes of hypovolemia and hypervolemia Medications for example, Lasix can cause hypovolemia in a patient with poor PO intake.

Fluid Volume Deficit • Loss of extracellular fluid exceeds intake ratio of water • Electrolytes lost in same proportion as they exist in normal body fluids • Dehydration: loss of water along with increased serum sodium level • May occur in combination with other imbalances • Dehydration • Causes: fluid loss from vomiting, diarrhea, GI suctioning, sweating, decreased intake, inability to gain access to fluid • Risk factors: diabetes insipidus, adrenal insufficiency, osmotic diuresis, hemorrhage, coma, third-space shifts

Fluid Volume Deficit (cont’d) • Manifestations: rapid weight loss, decreased skin turgor, oliguria, concentrated urine, postural hypotension, rapid weak pulse, increased temperature, cool clammy skin due to vasoconstriction, lassitude, thirst, nausea, muscle weakness, cramps • Laboratory data: elevated BUN in relation to serum creatinine, increased hematocrit • Serum electrolyte changes may occur

Fluid Volume Deficit (cont’d) • Medical management: provide fluids to meet body needs • • • Oral fluids (water, Gatorade, pedilyte) IV solutions Hypertonic solution e. g. . 3% Na. Cl Hypotonic solution e. g. . 0. 45% Na. Cl, 5% Dextrose Isotonic solution e. g. 0. 9 % Na. Cl, Lactated Ringers Colloid Solution e. g. . Dextran.

Fluid Volume Deficit—Nursing Management • I&O, daily weight, vital signs • Monitor for symptoms: skin and tongue turgor, mucosa, urine output, mental status • Measures to minimize fluid loss • Oral care • Administration of oral fluids • Administration of parenteral fluids • Monitor lab work • Monitor patient medication list

Fluid Volume Excess • Due to fluid overload or diminished homeostatic mechanisms • Risk factors: heart failure, renal failure, cirrhosis of liver • Contributing factors: excessive dietary sodium or sodium-containing IV solutions • Manifestations: edema, distended neck veins, abnormal lung sounds (crackles), tachycardia, increased blood pressure, pulse pressure and CVP, increased weight, increased urine output, shortness of breath and wheezing • Medical management: directed at cause, restriction of fluids and sodium, administration of diuretics

Fluid Volume Excess—Nursing Management • I&O and daily weights; assess lung sounds, edema, other symptoms • Monitor responses to medications—diuretics • Promote adherence to fluid restrictions, patient teaching related to sodium • • and fluid restrictions Monitor, avoid sources of excessive sodium, including medications Promote rest Semi-Fowler’s position for orthopnea Skin care, positioning/turning
Electrolyte Imbalances Sodium Potassium Calcium Magnesiu m Phosphor us Chloride
Sodium: hyponatremia • Serum sodium less than 135 m. Eq/L • Causes: adrenal insufficiency, water intoxication, SIADH or losses by vomiting, diarrhea, sweating, diuretics • Manifestations: poor skin turgor, dry mucosa, headache, decreased salivation, decreased blood pressure, nausea, abdominal cramping, neurologic changes • Medical management: water restriction, sodium replacement • Nursing management: assessment and prevention, dietary sodium and fluid intake, identify and monitor at-risk patients, effects of medications (diuretics, lithium) • If replacing with 3% Na. Cl administer slowly if 3% given too quickly can kill brain cells.

Hypernatremia Serum sodium greater than 145 m. Eq/L Causes: excess water loss, excess sodium administration, diabetes insipidus, heat stroke, hypertonic IV solutions Manifestations: thirst; elevated temperature; dry, swollen tongue; sticky mucosa; neurologic symptoms; restlessness; weakness Note: thirst may be impaired in elderly or the ill Medical management: hypotonic electrolyte solution or D 5 W Nursing management: assessment and prevention, assess for OTC sources of sodium, offer and encourage fluids to meet patient needs, provide sufficient water with tube feedings
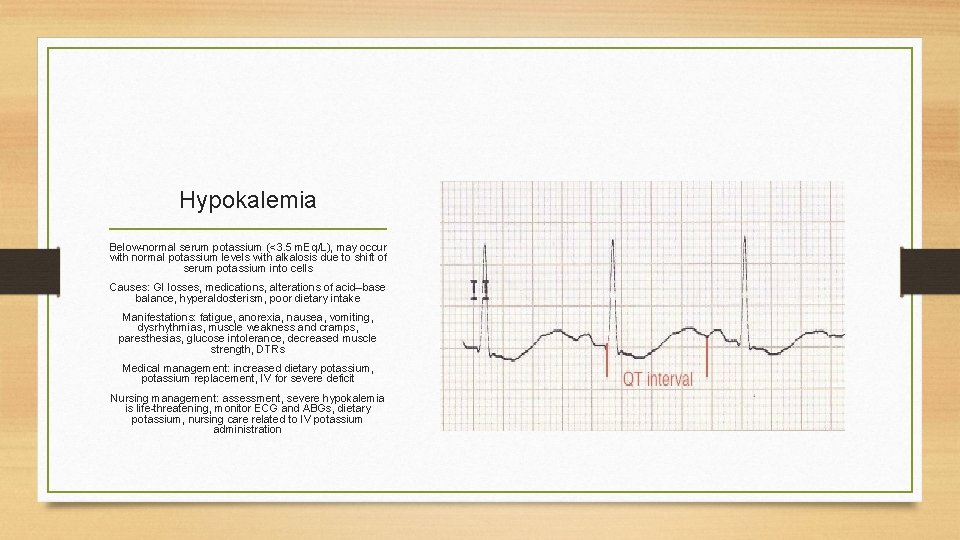
Hypokalemia Below-normal serum potassium (<3. 5 m. Eq/L), may occur with normal potassium levels with alkalosis due to shift of serum potassium into cells Causes: GI losses, medications, alterations of acid–base balance, hyperaldosterism, poor dietary intake Manifestations: fatigue, anorexia, nausea, vomiting, dysrhythmias, muscle weakness and cramps, paresthesias, glucose intolerance, decreased muscle strength, DTRs Medical management: increased dietary potassium, potassium replacement, IV for severe deficit Nursing management: assessment, severe hypokalemia is life-threatening, monitor ECG and ABGs, dietary potassium, nursing care related to IV potassium administration
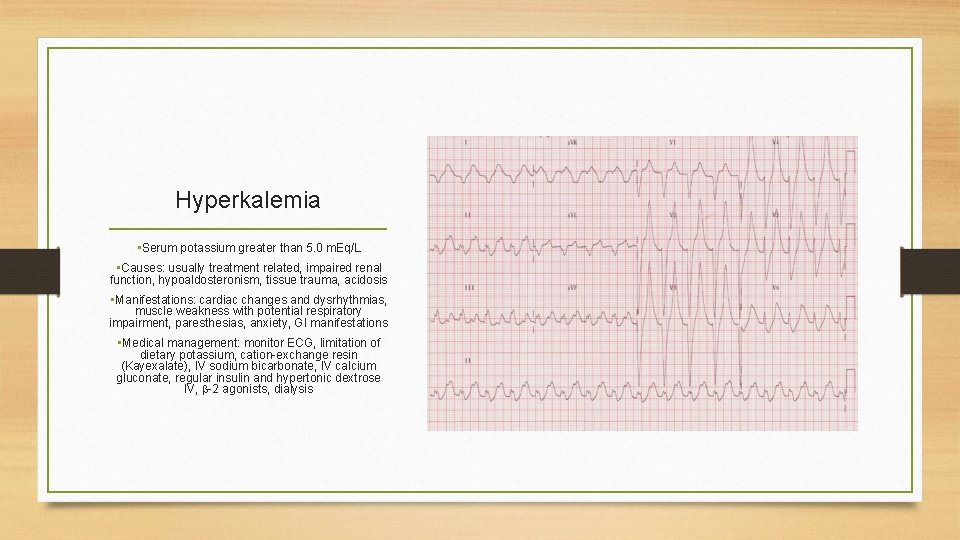
Hyperkalemia • Serum potassium greater than 5. 0 m. Eq/L • Causes: usually treatment related, impaired renal function, hypoaldosteronism, tissue trauma, acidosis • Manifestations: cardiac changes and dysrhythmias, muscle weakness with potential respiratory impairment, paresthesias, anxiety, GI manifestations • Medical management: monitor ECG, limitation of dietary potassium, cation-exchange resin (Kayexalate), IV sodium bicarbonate, IV calcium gluconate, regular insulin and hypertonic dextrose IV, -2 agonists, dialysis

Hyperkalemia (cont’d) • Nursing management: assessment of serum potassium levels, mix IVs containing K+ well, monitor medication affects, dietary potassium restriction/dietary teaching for patients at risk • Hemolysis of blood specimen or drawing of blood above IV site may result in false laboratory result • Salt substitutes, medications may contain potassium • Potassium-sparing diuretics may cause elevation of potassium • Should not be used in patients with renal dysfunction
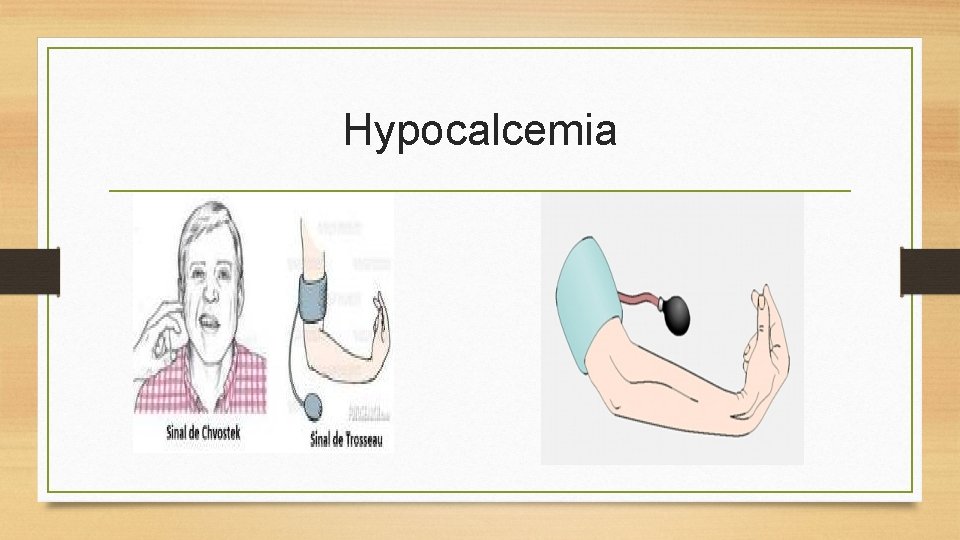
Hypocalcemia

Hypocalcemia • Serum level less than 8. 6 mg/d. L, must be considered in conjunction with serum albumin level • Causes: hypoparathyroidism, malabsorption, pancreatitis, alkalosis, massive transfusion of citrated blood, renal failure, medications, other • Manifestations: tetany, circumoral numbness, paresthesias, hyperactive DTRs, Trousseau’s sign, Chovstek's sign, seizures, respiratory symptoms of dyspnea and laryngospasm, abnormal clotting, anxiety

Hypocalcemia (cont’d) • Medical management: IV of calcium gluconate, calcium and vitamin D supplements; diet • Nursing management: assessment, severe hypocalcemia is lifethreatening, weight-bearing exercises to decrease bone calcium loss, patient teaching related to diet and medications, and nursing care related to IV calcium administration

Hypercalcemia • Serum level greater than 10. 2 mg/d. L • Causes: malignancy and hyperparathyroidism, bone loss related to immobility • Manifestations: muscle weakness, incoordination, anorexia, constipation, nausea and vomiting, abdominal and bone pain, polyuria, thirst, ECG changes, dysrhythmias • Medical management: treat underlying cause, fluids, furosemide, phosphates, calcitonin, biphosphonates • Nursing management: assessment, hypercalcemic crisis has high mortality, encourage ambulation, fluids of 3 to 4 L/d, provide fluids containing sodium unless contraindicated, fiber for constipation, ensure safety

Hypomagnesemia • Serum level less than 1. 3 mg/d. L, evaluate in conjunction with serum albumin • Causes: alcoholism, GI losses, enteral or parenteral feeding deficient in magnesium, medications, rapid administration of citrated blood; contributing causes include diabetic ketoacidosis, sepsis, burns, hypothermia • Manifestations: neuromuscular irritability, muscle weakness, tremors, athetoid movements, ECG changes and dysrhythmias, alterations in mood and level of consciousness • Medical management: diet, oral magnesium, magnesium sulfate IV
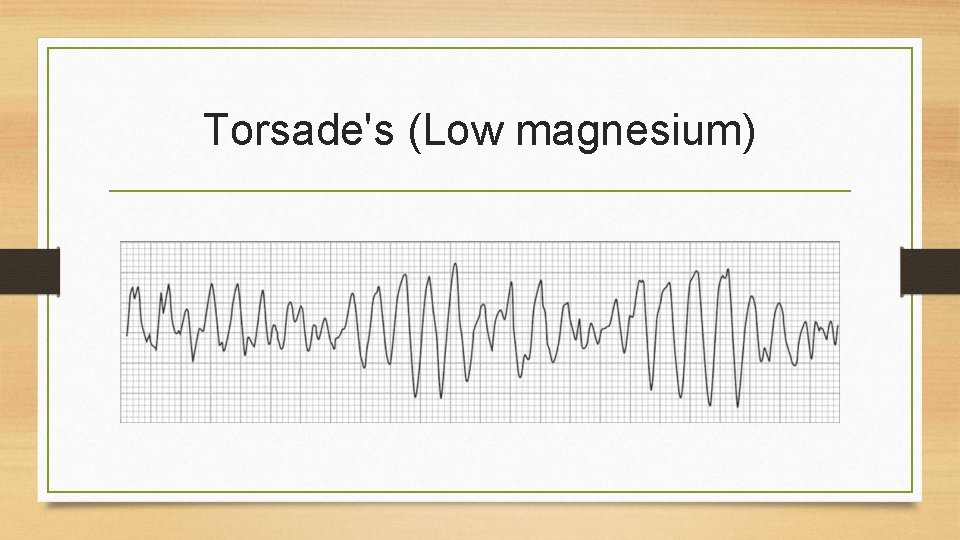
Torsade's (Low magnesium)

Hypomagnesemia (cont’d) • Nursing management: assessment, ensure safety, patient teaching related to diet, medications, alcohol use, and nursing care related to IV magnesium sulfate • Hypomagnesemia often accompanied by hypocalcemia • Need to monitor, treat potential hypocalcemia • Dysphasia common in magnesium-depleted patients • Assess ability to swallow with water before administering food or medications

Hypermagnesemia • Serum level greater than 2. 3 mg/d. L • Causes: renal failure, diabetic ketoacidosis, excessive administration of magnesium • Manifestations: flushing, lowered BP, nausea, vomiting, hypoactive reflexes, drowsiness, muscle weakness, depressed respirations, ECG changes, dysrhythmias • Medical management: IV calcium gluconate, loop diuretics, IV NS of RL, hemodialysis • Nursing management: assessment, do not administer medications containing magnesium, patient teaching regarding magnesium-containing OTC medications

Hypochloremia • Serum level less than 97 m. Eq/L • Causes: Addison’s disease, reduced chloride intake, GI loss, diabetic • • ketoacidosis, excessive sweating, fever, burns, medications, metabolic alkalosis Loss of chloride occurs with loss of other electrolytes, potassium, sodium Manifestations: agitation, irritability, weakness, hyperexcitability of muscles, dysrhythmias, seizures, coma Medical management: replace chloride-IV NS or 0. 45% NS Nursing management: assessment, avoid free water, encourage highchloride foods, patient teaching related to high-chloride foods

Hyperchloremia • Serum level more than 107 m. Eq/L • Causes: excess sodium chloride infusions with water loss, head injury, hypernatremia, dehydration, severe diarrhea, respiratory alkalosis, metabolic acidosis, hyperparathyroidism, medications • Manifestations: tachypnea, lethargy, weakness, rapid, deep respirations, hypertension, cognitive changes • Normal serum anion gap • Medical management: restore electrolyte and fluid balance, LR, sodium bicarbonate, diuretics • Nursing management: assessment, patient teaching related to diet and hydration

Medications That Cause Electrolyte Imbalance • Chemotherapy drugs (cisplatin) can cause hypokalemia, hypocalcemia • Diuretics: Furosemide(Lasix) or Bumetanide(Bumex) Hypokalemia • Antibiotics (amphotericin B) (anti-fungal) decrease sodium, potassium, calcium, and magnesium. • Corticosteroids (hydrocortisone) can cause hypokalemia, hypocalcemia • Digitalis toxicity keeps company with hypokalemia and hypomagnesium

Nursing Considerations • • Keep in mind the patient’s medications and lab values Patient signs and symptoms e. g. : low BP, poor skin turgor, sunken eyes When calling results to MD remember SBAR Rapid infusion of hypertonic solutions can cause (Central pontine myelinolysis) Situation Background Assessment Recommendation
Remember Brain, Heart, and the Relationship to Electrolytes The Brain Loves Sodium The Heart Loves Magnesium, Calcium and Potassium

Reference Hinkle, J. L. , & Cheever, K. H. (2014). Brunner & Suddarth's textbook of medical-surgical nursing. Bethlehem, Pennsylvania: Wolters Kluwer/Lippincott Williams & Wilkins.
- Slides: 40