Fishers change curve Changes to WPBA proposals RCGP

Fisher’s change curve

Changes to WPBA proposals RCGP WPBA group May 2019

WPBA evaluates the trainee's progress in areas of professional practice best tested in the workplace and: Looks at trainees performance in their day to day practice provides evidence for learning and reflection on performance Supports and drives learning in important areas of competence with an underlying theme of patient safety provides constructive feedback on areas of strength and developmental needs, identifying trainees who may be in difficulty evaluates aspects of professional behaviour that are difficult to assess in traditional examinations determines fitness to progress to the next stage of training WPBA assessments take place throughout GP Specialty Training

GMC 2017 – Improving assessment guidelines GMC Mandatory assessments for all trainees CSR with every post, including GP placements in ST 1/2 Multi-source feedback in every training year At least Annual Educational Supervisors reviews and Assessments to comply with Generic Professional Competencies
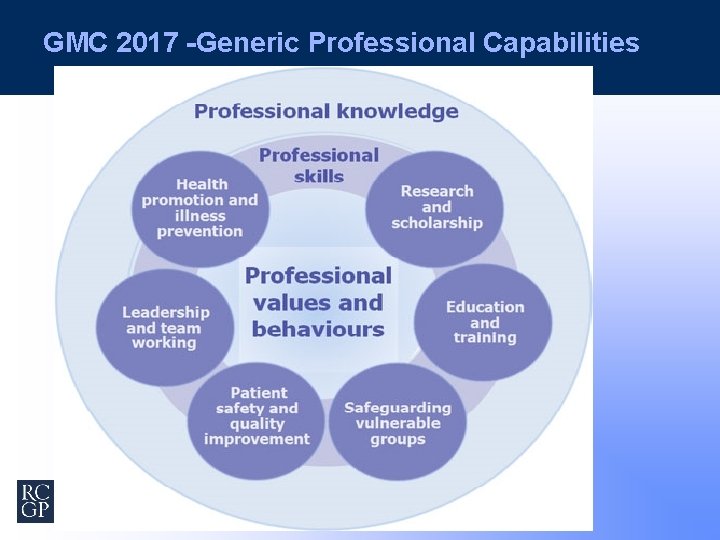
GMC 2017 -Generic Professional Capabilities

6 Domains on Critical Professional Capabilities Health promotion and illness prevention Leadership and team working Patient Safety and Quality Improvement Safeguarding vulnerable groups Education and training Research and Scholarship Assessment -to avoid tick box assessments in favour of qualitative methods i. e. reflective portfolios, structured trainers report and 360 degree appraisal Opportunity to improve WPBA within the MRCGP

Known Issues • • • Assessments / CSRs, particularly in the hospital setting are not always done well Assessments / CSRs can be seen as long box ticking forms with little written feedback + hard to link to competences Evidence that assessments do not identify trainees failing to progress early, especially Cb. Ds / PSQ Log entries seen as a chore Deaneries /LETBs inconsistent in their requirements for WPBA at ARCP Assessment requirements unchanged from start of WPBA and need to change to reflect both GMC requirements, curriculum and future needs of GP

Proposals All assessments to have 4 point scale (so that the low borderline are separated from the worryingly poor) Include entrustable questions (e. g. comparison of levels of supervision needed rather than global judgements) Change of comparison groups in ST 1/2 (in GP and non GP will be compared to peers)

Proposals 2 Stop trainee links to curriculum in log Create trainee suggestions to population groups Trainee makes suggestions on links to capabilities New areas covered as required by GMC (prescribing (ST 3), leadership (ST 3), quality improvement ST 1/2) Improve all LLE formats

Proposals 3 Reduce workload for ES and trainee One ESR annually and shorter interim mid year review* Reduce number of Cb. Ds and introduce CATs in ST 3 Reduce number of required COTs Reduce number of learning logs and shorten log entries Stop PSQ in ST 1/2 and rewrite PSQ for ST 3 Rewrite CSR, Cb. D, COT and Mini. CEX forms


GMC Prescribing proficiencies Assess the risks and benefits including that posed by other medications and medical conditions. Identify when prescribing unlicensed medicines and informs patients appropriately. Adhere to local guidelines and evidence based medicine. Use antimicrobials appropriately. Counsel patients appropriately including instructions for taking medicines safety in line with up to date literature. Review and monitor effects including blood testing at appropriate intervals

Prescribing assessment -1 st half ST 3 Trainee searches /downloads 60 retrospective scripts they have initiated Trainee reviews 60 against prescribing errors manual – right drug, dose, dosage frequency, documentation, follow up. Trainee reflection on the assessment via log entry Completes table mapping their prescribing to errors Supervisor, (possibly pharmacist if available), samples 20 of the scripts, to include any with identified errors Completes assessment form Formative process; but if any significant errors, learning plans to review and address any prescribing proficiencies not covered

Learning logs: new population groups Linked to clinical experience groups not specific curriculum areas 1. Infants, children and young people 2. People with mental health needs 3. People with long-term conditions and disability 4. Frail and elderly people (including multiple morbidity and care of the dying) 5. Gender health (Women’s, Men’s and LGBTQ health) 6. People requiring urgent and unscheduled care 7. People with vulnerabilities (for example veterans, addictions, mental capacity difficulties, safeguarding issues, and those with communication difficulties) 8. Health promotion and people with non-acute and/or non-chronic health problems

Case Assessment Tools Replace Cb. Ds in ST 3 Opportunity to be assessed on other areas within workplace Suggested types of CATs Case based discussion Random case review Leadership activities Prescribing assessment follow up Consultation assessments- which are not COTs Referrals review Other e. g. debriefs, review of investigation or imaging use, follow up of QIP etc
- Slides: 15