Firstcase on Time Starts and Professionalism Meghan Poe
- Slides: 1

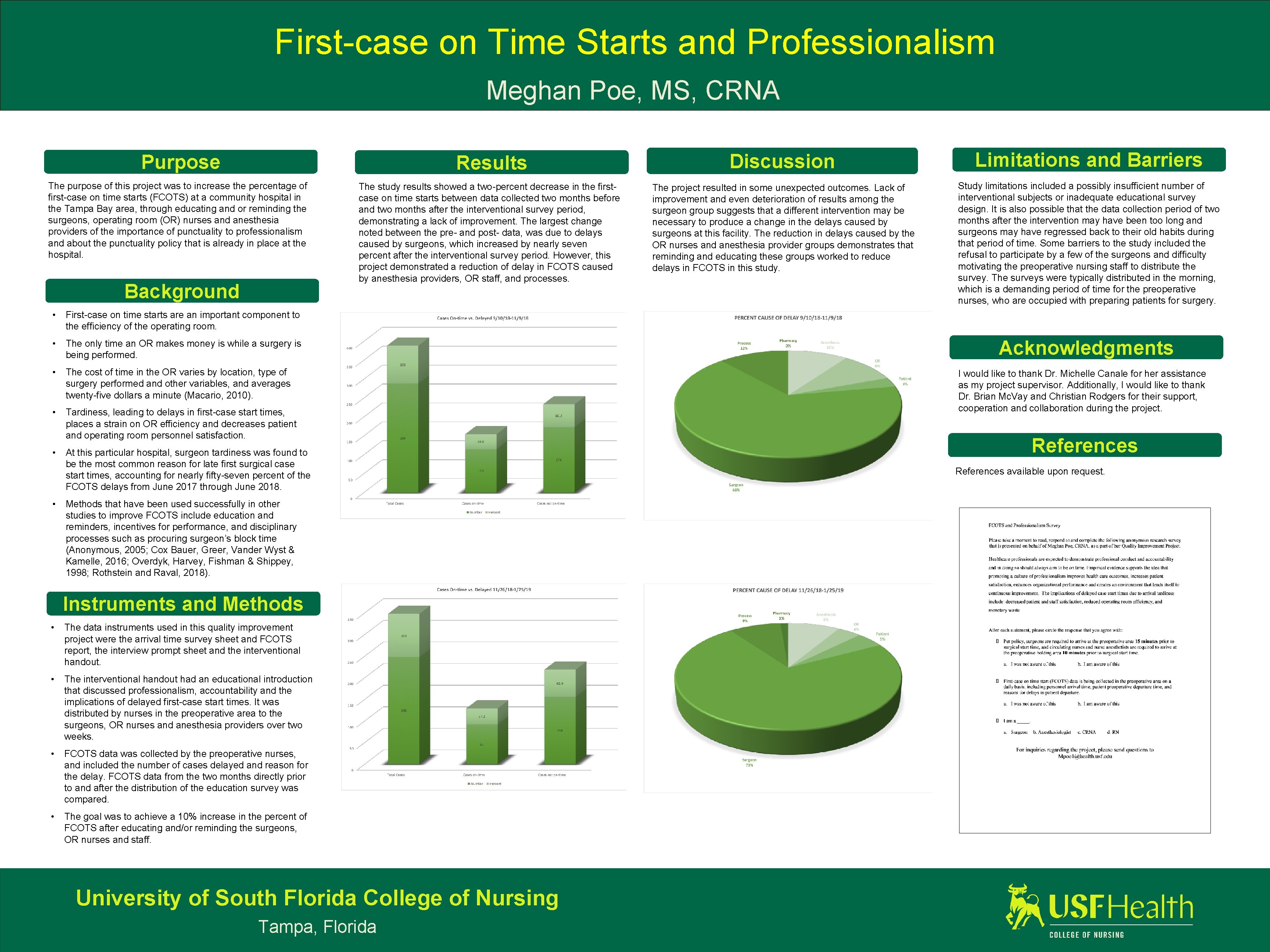
First-case on Time Starts and Professionalism Meghan Poe, MS, CRNA Results Discussion Limitations and Barriers The study results showed a two-percent decrease in the firstcase on time starts between data collected two months before and two months after the interventional survey period, demonstrating a lack of improvement. The largest change noted between the pre- and post- data, was due to delays caused by surgeons, which increased by nearly seven percent after the interventional survey period. However, this project demonstrated a reduction of delay in FCOTS caused by anesthesia providers, OR staff, and processes. The project resulted in some unexpected outcomes. Lack of improvement and even deterioration of results among the surgeon group suggests that a different intervention may be necessary to produce a change in the delays caused by surgeons at this facility. The reduction in delays caused by the OR nurses and anesthesia provider groups demonstrates that reminding and educating these groups worked to reduce delays in FCOTS in this study. Study limitations included a possibly insufficient number of interventional subjects or inadequate educational survey design. It is also possible that the data collection period of two months after the intervention may have been too long and surgeons may have regressed back to their old habits during that period of time. Some barriers to the study included the refusal to participate by a few of the surgeons and difficulty motivating the preoperative nursing staff to distribute the survey. The surveys were typically distributed in the morning, which is a demanding period of time for the preoperative nurses, who are occupied with preparing patients for surgery. Purpose The purpose of this project was to increase the percentage of first-case on time starts (FCOTS) at a community hospital in the Tampa Bay area, through educating and or reminding the surgeons, operating room (OR) nurses and anesthesia providers of the importance of punctuality to professionalism and about the punctuality policy that is already in place at the hospital. Background • First-case on time starts are an important component to the efficiency of the operating room. • The only time an OR makes money is while a surgery is being performed. • The cost of time in the OR varies by location, type of surgery performed and other variables, and averages twenty-five dollars a minute (Macario, 2010). • Tardiness, leading to delays in first-case start times, places a strain on OR efficiency and decreases patient and operating room personnel satisfaction. • At this particular hospital, surgeon tardiness was found to be the most common reason for late first surgical case start times, accounting for nearly fifty-seven percent of the FCOTS delays from June 2017 through June 2018. • Methods that have been used successfully in other studies to improve FCOTS include education and reminders, incentives for performance, and disciplinary processes such as procuring surgeon’s block time (Anonymous, 2005; Cox Bauer, Greer, Vander Wyst & Kamelle, 2016; Overdyk, Harvey, Fishman & Shippey, 1998; Rothstein and Raval, 2018). Instruments and Methods • The data instruments used in this quality improvement project were the arrival time survey sheet and FCOTS report, the interview prompt sheet and the interventional handout. • The interventional handout had an educational introduction that discussed professionalism, accountability and the implications of delayed first-case start times. It was distributed by nurses in the preoperative area to the surgeons, OR nurses and anesthesia providers over two weeks. • FCOTS data was collected by the preoperative nurses, and included the number of cases delayed and reason for the delay. FCOTS data from the two months directly prior to and after the distribution of the education survey was compared. • The goal was to achieve a 10% increase in the percent of FCOTS after educating and/or reminding the surgeons, OR nurses and staff. University of South Florida College of Nursing Tampa, Florida Acknowledgments I would like to thank Dr. Michelle Canale for her assistance as my project supervisor. Additionally, I would like to thank Dr. Brian Mc. Vay and Christian Rodgers for their support, cooperation and collaboration during the project. References available upon request.