FIRST STAGE OF LABOUR LABOUR n Labour is

FIRST STAGE OF LABOUR

LABOUR n Labour is described as a process by which the fetus placenta and membranes are expelled through the birth canal

NORMAL LABOUR n Occurs at term n Spontaneous in onset n Fetus presenting by the vertex n Process completed within 18 hours n No complications arise

STAGES OF LABOUR n FIRST STAGE ( 12 hr primi, 6 hr multi) n SECONT STAGE (2 hr primi, 30 mins multi) n THIRD STAGE (15 mins in both primi and multi) n FOURTH STAGE ( 1 hour)
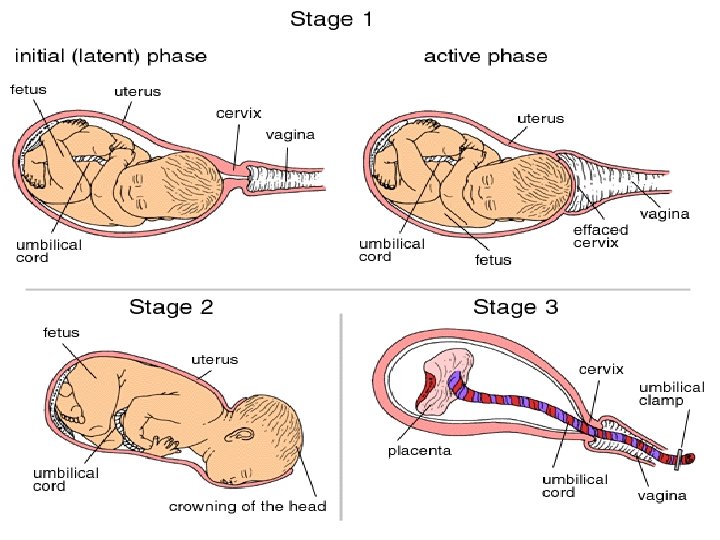

FIRST STAGE OF LABOUR q ü ü ü q ü ü Latent phase Mild, short contractions Cervix 0 -3 cms 6 – 8 hrs Active phase Moderate to strong contraction Cervix 4 -7 cms 4. 6 h for nullipara and 2. 4 h for multipara Transition Strong contraction Cervix 7 -10 cms
FIRST STAGE

SIGNS AND SYMPTOMS OF IMPENTING LABOUR n n n n Lightening Frequency of micturition Spurious labour Cervical changes Premature rupture of membrane Bloody show Energy spurt Gastrointestinal upset
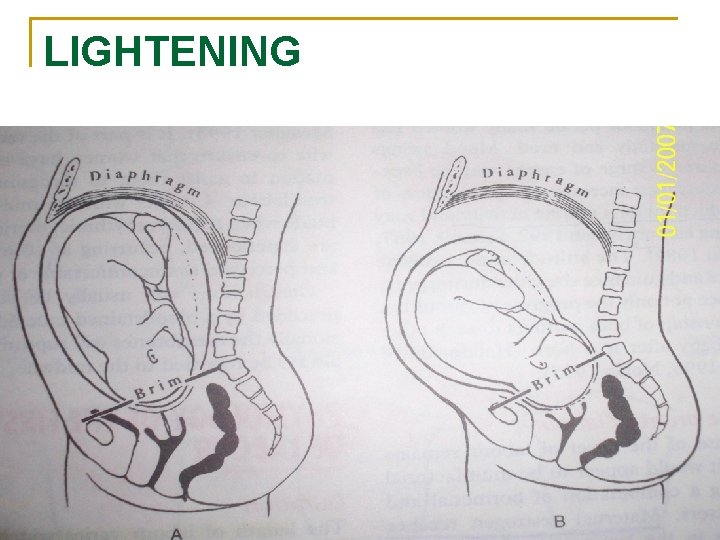
LIGHTENING
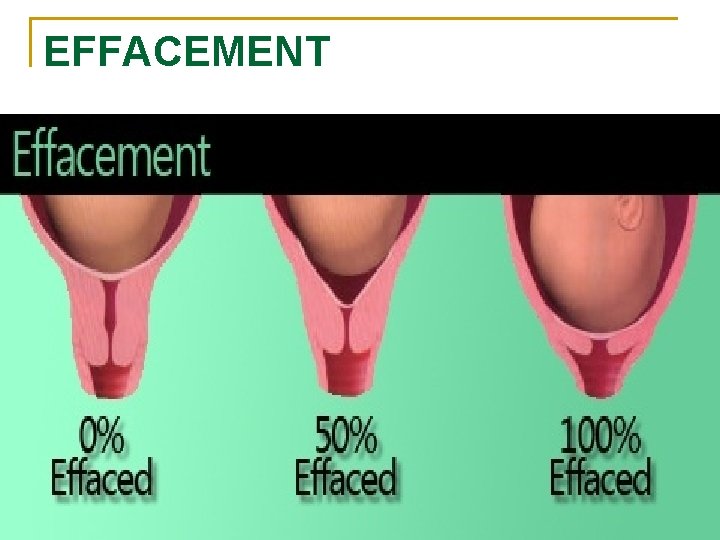
EFFACEMENT
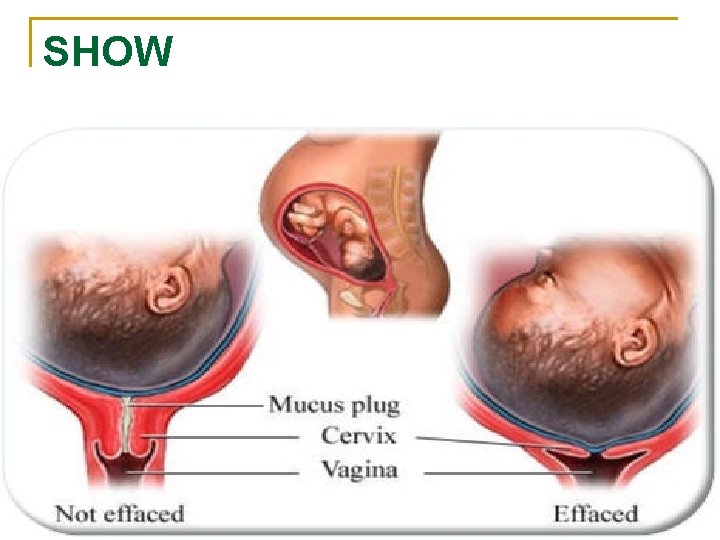
SHOW
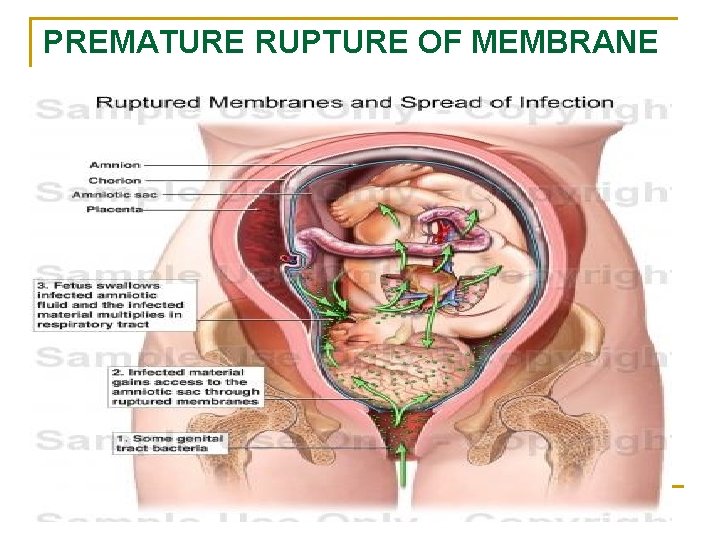
PREMATURE RUPTURE OF MEMBRANE

CAUSES OF ONSET OF LABOUR q q Uterine distension theory Oxytocin stimulation theory q Prostaglandin stimulation theory q Progesterone withdrawal theory q Estrogen stimulation theory q Fetal cortisol theory

CAUSES OF ONSET OF LABOUR q Uterine distension (Optimal distension theory) ü Overstretching promotes muscle excitability q ü Oxytocin stimulation theory Oxytocin inhibit calcium binding to sacroplasmic reticulum Increasing the intracellular calcium level Promotes myometrial contraction ü Sensitivity of oxytocin to myometrium increases in the late pregnancy due to increase in the number of oxytocin receptors ü Oxytocin promotes release of prostaglandins from the decidua

Contd…. q ü Prostaglandin stimulation theory Prostaglandin may diffuse to myometrium and initiate labour Progesterone withdrawal theory Progesterone binds Calcium to the sacroplasmic reticulum Decrease intracellular calcium level q Estrogen stimulation theory ü Increases the release of oxytocin from the maternal pituitary ü Promotes synthesis of receptors for oxytocin

Contd…. ü Feto placental contribution Activation of hypothalamo pituitary axis CRH Increase release of ACTH Fetal adrenals Increased cortisol secretion Accelerated production oestrogen and prostaglandins from the placenta q Contractile system of myometrium

PHYSIOLOGICAL PROCESS IN THE FIRST STAGE OF LABOUR n Ø Ø Ø Ø UTERINE ACTION Fundal Dominance Polarity Contraction and Retraction Formation of Upper and Lower Uterine Segment Retraction Ring Cervical Effacement Cervical Dialation Ripening of the cervix
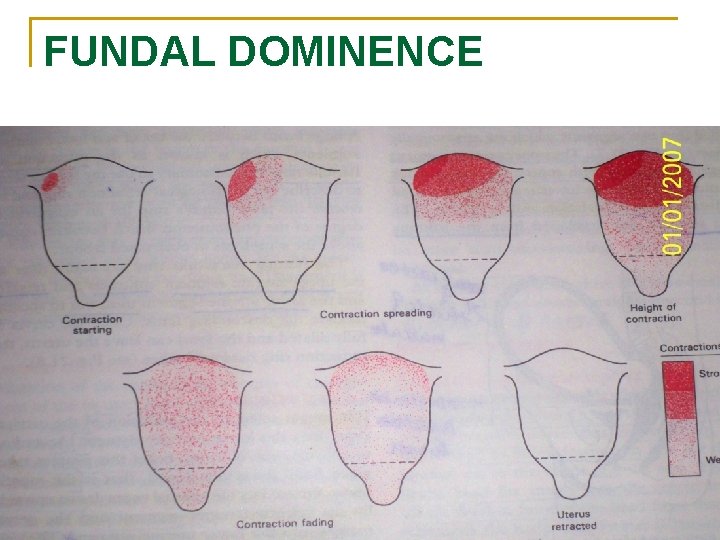
FUNDAL DOMINENCE
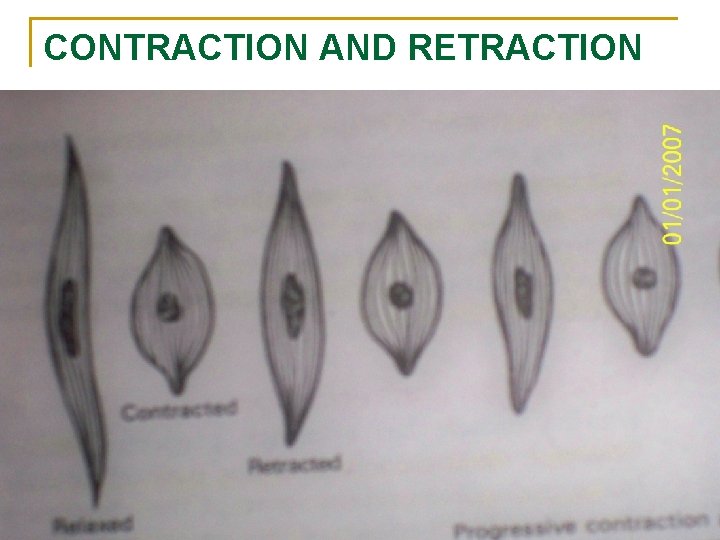
CONTRACTION AND RETRACTION
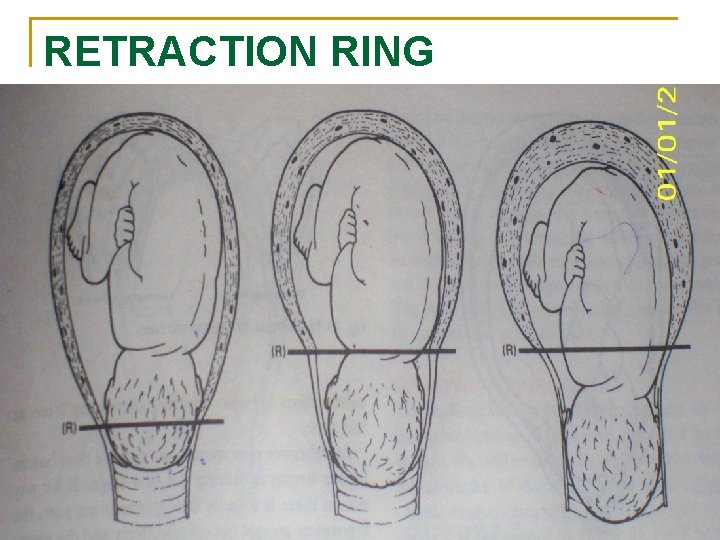
RETRACTION RING
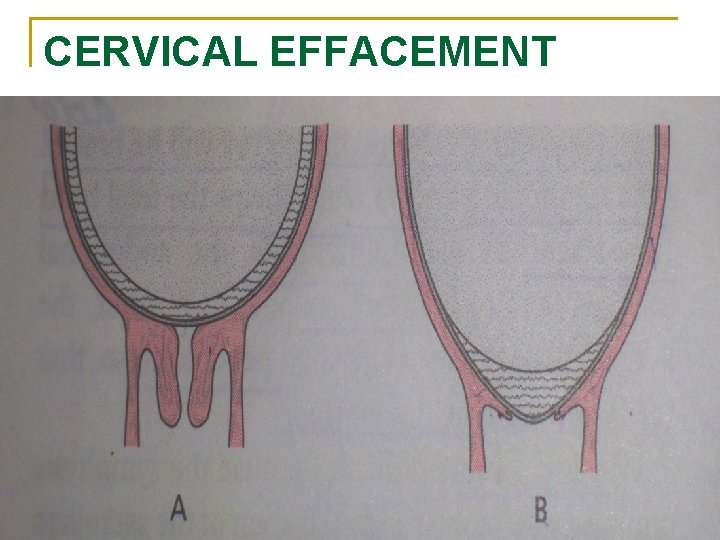
CERVICAL EFFACEMENT
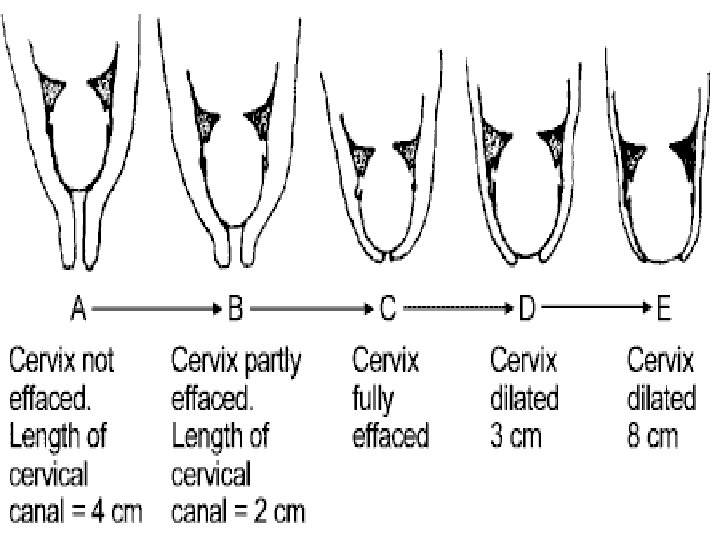

n MECHANICAL FACTORS Ø Formation of the forewaters Ø General fluid pressure Ø Rupture of the membranes Ø Fetal axis pressure Ø Descend of presenting part
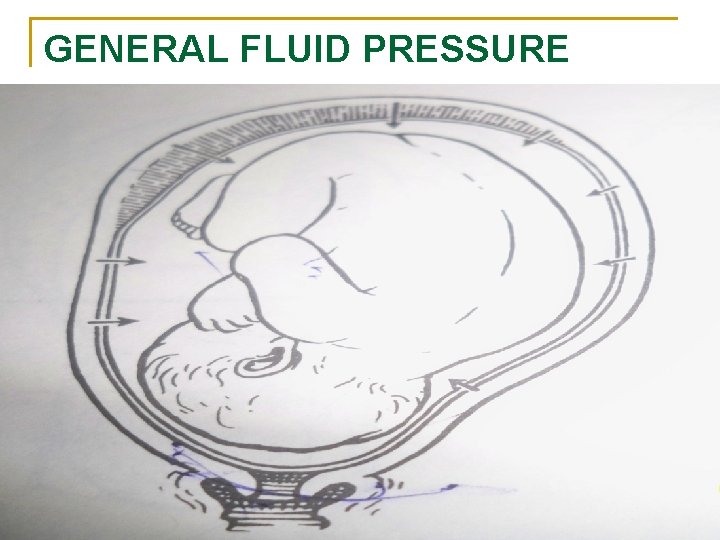
GENERAL FLUID PRESSURE
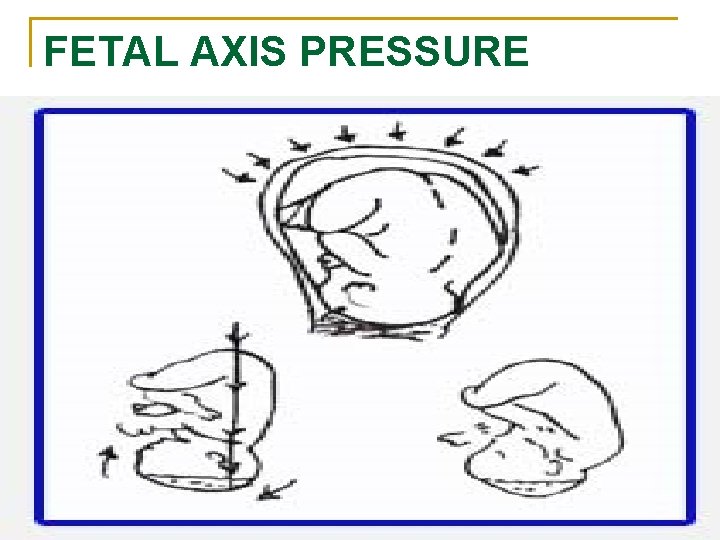
FETAL AXIS PRESSURE
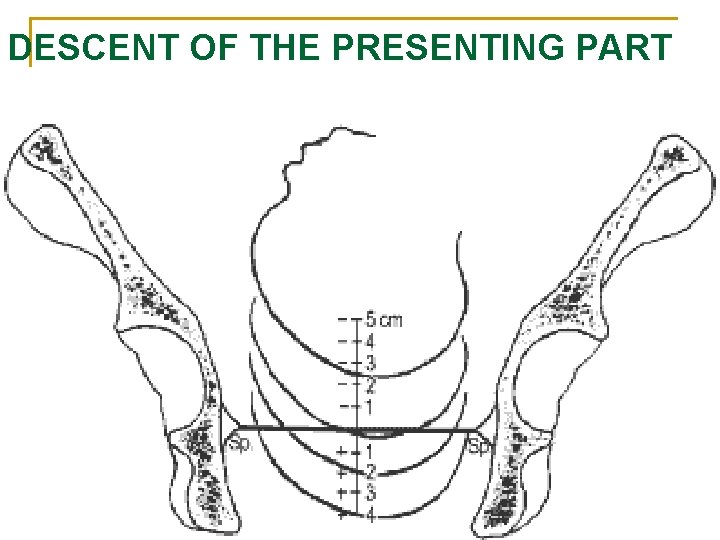
DESCENT OF THE PRESENTING PART

FACTORS INFLUENCING LABOUR q PASSAGE WAY q PASSENGER(FOETUS AND PLACENTA) q POWERS q POSITION OF MOTHER q PSYCHOLOGIC RESPONCE

INITIAL ASSESSMENT AND DIAGNOSIS n n n n Age Gravida and para Time of onset of uterine contractions Duration of contractions Intensity of contraction (when lying down contrasted to when walking around) Location of discomfort or pain Length of labour Number of years since the last baby

Contd…. n n n n Method of previous delivery Size of largest and smallest previous babies Expected date of delivery and present weeks of gestation Absence, presence or increase in bloody show Presence of vaginal bleeding Membranes ruptured or not Any prenatal problem

PHYSICAL EXAMINATION q VITAL SIGNS Ø Elevated temperature – Infectious process Ø Elevated pulse – Infection, Shock or Anxiety Ø Elevated respiration – Shock and anxiety Ø Elevated or lowered Bp – Hypertensive disorders or shock Ø Elevated systolic or normal diastolic Bp - Anxiety

PHYSICAL EXAMINATION – CONTD…. q Ø Ø ü ü PHYSICAL MEASUREMENTS Height and weight Fetal heart tone Normal – 120 -160 beats per minute Heart rate below 120 or above 160 – Fetal distress

PHYSICAL EXAMINATION – CONTD…. Ø ü ü ü Ø ü Contraction pattern Frequency Duration Intensity Engagement Unengaged or unfixed head in primigravid in labour indicate CPD

PHYSICAL EXAMINATION – CONTD…. Ø ü Estimated fetal weight and fundal height Smaller than expected fundal height and fetal weight – incorrect date or small for date baby ü Larger than EFW and fundal height - incorrect date or large baby ü Large baby – uterine atony, shoulder dystocia

PHYSICAL EXAMINATION – CONTD…. Ø ü ü Lie, Presentation, Position and Variety Abnormal lie , presentation, or position Edema of extremities One of the classical sign of preeclampsia Physiological edema is normal Pelvic examination and vaginal examination Effacement Confirm abdominal diagnosis

PHYSICAL EXAMINATION – CONTD…. Ø ü Ø ü ü ü Position of the cervix Anterior cervix indicates readiness for labour Station To determine station of the fetal head Whether or not the membranes have ruptured Amniotic fluid escaping from the cervical os Amniotic fluid pooled in the vagina Membranes are not felt over the presenting part

NURSING MANAGEMENT q ü ü ENVIORMENT Feel comfortable in their own surroundings Facilities for prompt and efficient action ü Reduce anxiety ü Labour women should be welcomed and encouraged in their own surrounding

Contd…. q ü EMOTIONAL SUPPORT Should display a tolerant and non judgemental attitude 1. Companion in labour 2. Explanation 3. Privacy

Contd…. q 1. 2. Ø Ø Ø 3. 4. 5. PREVENTION OF INFECTION Mothers wellbeing during pregnancy Factors affecting resistance The blood Nutritional status The skin and the membranes Hygiene Rest General hygiene and care of the environment Asepsis and antisepsis Restriction of invasive techniques

Contd…. q POSITION AND MOBILITY Ø Upright position – facilitate efficient contraction - shorten latent phase - reduce the need for analgesia Ø She may rock, walk, kneel or squat (effective in OP position) Ø Recumbent position cause compression of the inferior vena cava and supine hypotension Ø Lateral position is preferable if wishes to lie down

OTHER FACTORS GOVERNING CHOICE OF POSITION q ü ü ü q ü q q ü Analgesia Unable to walk if narcotic analgesia is requested Lateral position or supported sitting is suitable Epidural analgesia demands women should be in bed either sitting up or lying on her side Monitoring Cardiotocograph limit the choice of position Fetal condition Supine hypotension reduces fetal oxygenation Intravenous infusion Complication APH, ROM When the head is high

q 1. Ø Ø Ø 2. Ø 3. 4. Ø NUTRITION Advice prior to admission Women need energy – CHO Foods – Toast, breakfast cereal, yogurt, fruit juice, tea, plain biscuit, clear broth Fluids taken freely Intake in early labour Depending upon hospital policy Glycogenic and fluid requirement Comfort Drink, brushing, mouth wash.

q BLADDER CARE Ø Empty bladder every 1. 5 to 2 hours Ø Full bladder inhibit descend of the fetal head and effective uterine contraction Ø Uterine retension cause hypotonic uterine action

n BOWEL ü Soap and water enema or glycerine suppository ü Emptying the bowel prevents the soiling of the rectum in the second stage of labour

OBSERVATIONS MOTHER q REACTION TO LABOUR q VITAL SIGNS q URINALYSIS q FLUID BALANCE q PROGRESS Ø Ø Abdominal Examination Vaginal Examination

q ü REACTION TO LABOUR Some women experience contractions as positive, motivating, life giving force ü Others feel them as pain and resist them ü As labour progress she may feel less confident

q VITAL SIGNS TEMPERATURE ü Pulse rate should be steady ü More than 100 – infection, ketosis, haemorrhage ü Rising pulse rate – rupture of uterus ü Record 1 -2 hr in early labour ü Record every 15 -30 minutes when labour is more advanced PULSE ü Pyrexia – infection, ketosis ü Record every 4 hours BLOOD PRESSURE ü Every 4 hours unless it is abnormal ü Hypotension – supine position, shock, epidural anaesthesia

q URINALYSIS ü Test urine for glucose, ketones and protein ü Ketones – starvation or maternal distress ü Trace of protein – Rupture of membrane ü Significant proteinuria – Worsening pre eclampsia q FLUID BALANCE ü Record of intake and output must be recorded

PROGRESS q ABDOMINAL EXAMINATION Ø Regular abdominal examination throughout labour Ø Nature of contractions like intensity, frequency and duration are assessed clinically Ø No of contractions should be assessed in 10 minutes Ø Duration of contraction should be assessed in seconds Ø Pelvic grip – gradual disappearance of the poles of the head Shifting the maximal impulse of the FHS downward and medially Ø

OBSERVATIONS THE FETUS q THE FETAL HEART q FETAL BLOOD SAMPLING q AMNIOTIC FLUID q FETAL DISTRESS

The fetal heart TYPES q INTERMITTENT RECORDING q CONTINUOUS RECORDING

INTERMITTENT FETAL HEART RATE MONITORING Ø This term is used when the fetal heart rate is auscultated at interval using a Pinard’s fetoscope or a Doppler ultrasound apparatus Ø Rate should be counted over a minute Ø Normal rate is between 120 and 160 beats per minute Ø Rhythm should remain steady Ø FHR should be monitored immediately following uterine contraction

CONTINUOUS FETAL HEART RATE MONITORING Ø Continuous recording usually involves fetal cardiograph and maternal tocograph in a cardiotocograph apparutus Ø Observes the response of the fetal heart to uterine activity as well as rate and rhythm Ø Usually applied for 20 min or be used for whole labour

Fetal blood sampling Ø Normal p. H of fetal blood is 7. 33 or above Ø Fetus who become hypoxic will also become acidotic

Amniotic fluid Ø Amniotic fluid normally clear Ø Amniotic fluid provides information about the condition of the fetus q Green – Meconium staining q Muddy yellow colour or slightly green – Previous distress q Golden yellow – Rhesus iso-immunisation q Bleeding – May be rupture of vasa previa

Fetal Distress Signs of fetal distress Ø Fetal tachycardia R/T oxygen deprivation Ø Fetal bradycardia R/T uterine contraction Ø Passage of meconium stained amniotic fluid Management Ø Call a doctor Ø Syntocin must be stopped Ø Place mother in left lateral position Ø Administer oxygen Ø First stage prepare for LSCS Ø Second stage liberal episiotomy fails ventouse or forceps

ACTIVE MANAGEMENT OF FIRST STAGE OF LABOUR Definition Ø Describe a range of policies which helps to achieve efficient uterine action, thereby preventing prolonged labour in primigravidae Aim Ø Not to expose anyone with the stress of labour for more than 12 hours

Components of active management of labour q ü ü ü q Accurate diagnosis of labour Regular rhythmic contraction Accompanied by show, ROM or complete effacement Early rupture of the membrane 1 hr after labour is diagnosed Not the colour of the liquor Monitoring cervical dialation PV hourly for the first 3 hrs then at 2 hrs interval Chart observations in a partogram Cervical dialation 1 cm per hour is acceptable Continuous professional support for the mother

NOW THE ACTIVE MANAGEMENT OF LABOUR INCLUDE q Rupture of membrane q Followed by oxytocin infusion
- Slides: 58