First Responder Overdose Response Training In collaboration with

First Responder Overdose Response Training In collaboration with the Massachusetts Department of Public Health, Bureau of Substance Abuse Services and Office of HIV/AIDS

Go to getnaloxonenow. org for an online module for first responders (EMTs, firefighters, and law enforcement officers) with post‐test

The Overdose Problem
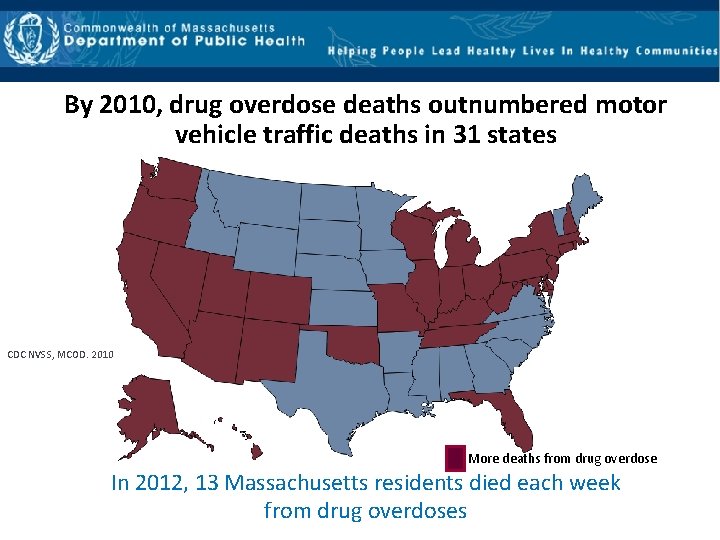
By 2010, drug overdose deaths outnumbered motor vehicle traffic deaths in 31 states CDC NVSS, MCOD. 2010 More deaths from drug overdose In 2012, 13 Massachusetts residents died each week from drug overdoses 4
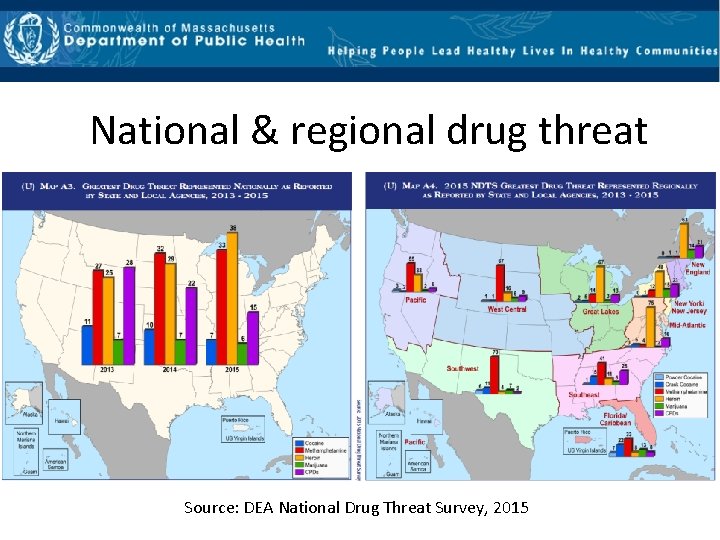
National & regional drug threat Source: DEA National Drug Threat Survey, 2015
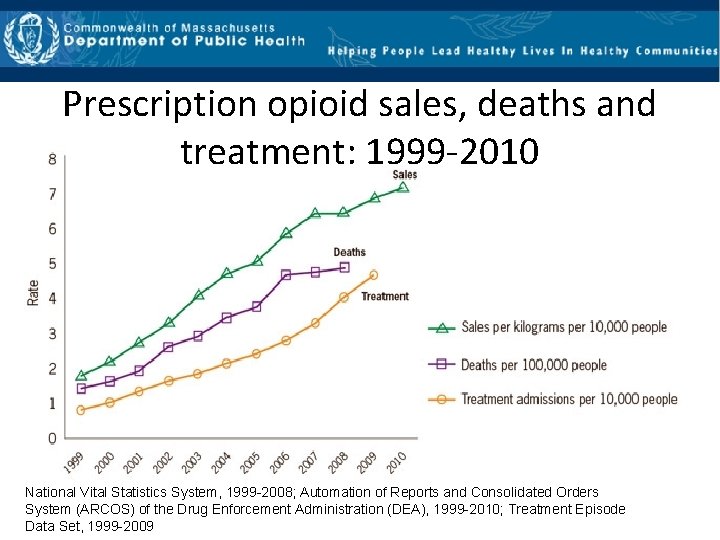
Prescription opioid sales, deaths and treatment: 1999‐ 2010 National Vital Statistics System, 1999 -2008; Automation of Reports and Consolidated Orders System (ARCOS) of the Drug Enforcement Administration (DEA), 1999 -2010; Treatment Episode Data Set, 1999 -2009

Fentanyl: a synthetic short‐acting opioid 40 -50 x more potent than pure heroin Illicitly manufactured fentanyl is sold in the illicit market often mixed with heroin and/or cocaine as a combination product — with or without the user’s knowledge — to increase its euphoric effects Fentanyl‐related overdoses can be reversed with naloxone, however a higher dose or multiple number of doses per overdose event may be required due to its high potency http: //emergency. cdc. gov/han 00384. asp
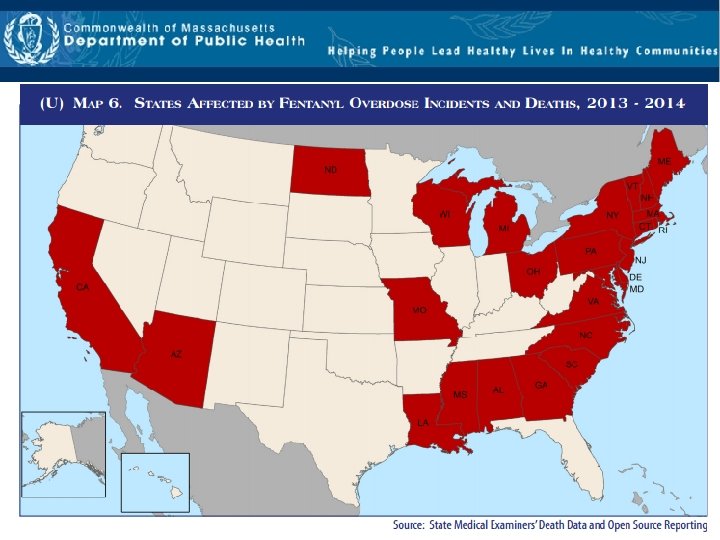
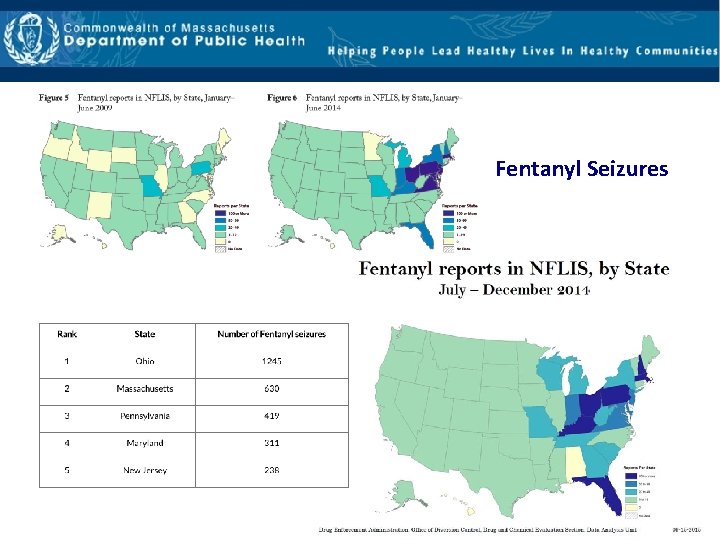
Fentanyl Seizures
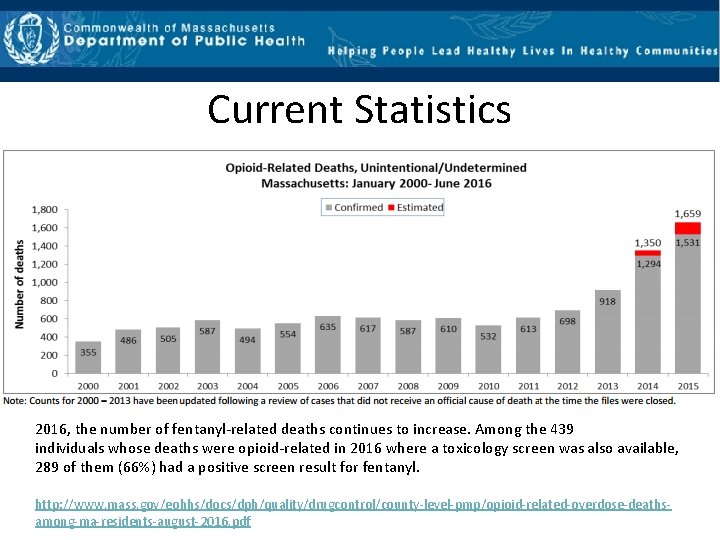
Current Statistics 2016, the number of fentanyl‐related deaths continues to increase. Among the 439 individuals whose deaths were opioid‐related in 2016 where a toxicology screen was also available, 289 of them (66%) had a positive screen result for fentanyl. http: //www. mass. gov/eohhs/docs/dph/quality/drugcontrol/county‐level‐pmp/opioid‐related‐overdose‐deaths‐ among‐ma‐residents‐august‐ 2016. pdf

Learning Objectives 1. Understand the overdose crisis 2. Know how opioids work and overdose risk factors 3. Recognize an opioid overdose 4. Respond to opioid overdose 5. Review Good Samaritan/Naloxone Law § Passed August 2012 6. Comply with the emergency regulations § Passed March 2014

13

https: //www. whitehouse. gov/ondcp/national‐drug‐control‐strategy
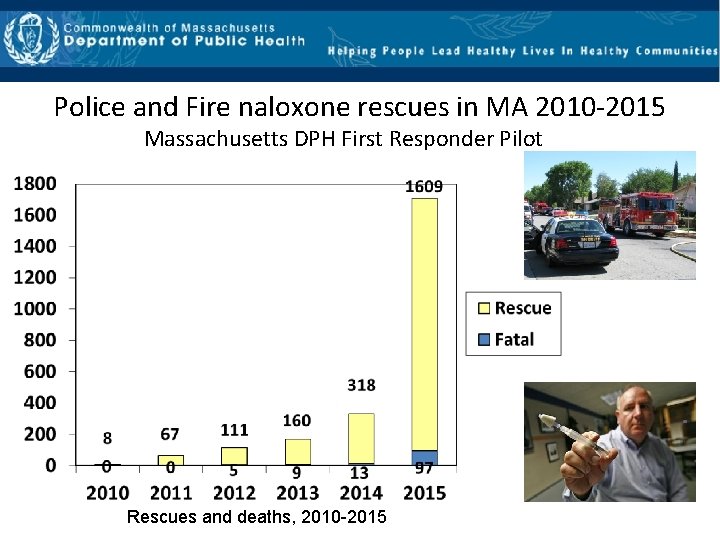
Police and Fire naloxone rescues in MA 2010‐ 2015 Massachusetts DPH First Responder Pilot Rescues and deaths, 2010 -2015

Why Police Officers? • First to the scene of an overdose • Frequent interaction with high risk populations • With the right tools, police can make a public health impact • Builds bridges to active users and their social networks • Overdose is a true crisis and police can help

How Opioids Work and Overdose Risk Factors

• There were ads in papers and journals for Bayer’s many products, including aspirin and 18

What are opioids/opiates? • Medications that relieve pain • Attach to the opioid receptors in the brain and reduce the intensity of pain signals reaching the brain.

Opioids Natural Opiates Semi-Synthetic Opiates Fully Synthetic Opioids opium morphine codeine heroin hydromorphone hydrocodone oxycodone fentanyl methadone The term opiate is often used as a synonym for opioid, however the term opiate refers to just those opioids derived from the poppy plant either natural or semi‐ synthetic All categories have overdose risk
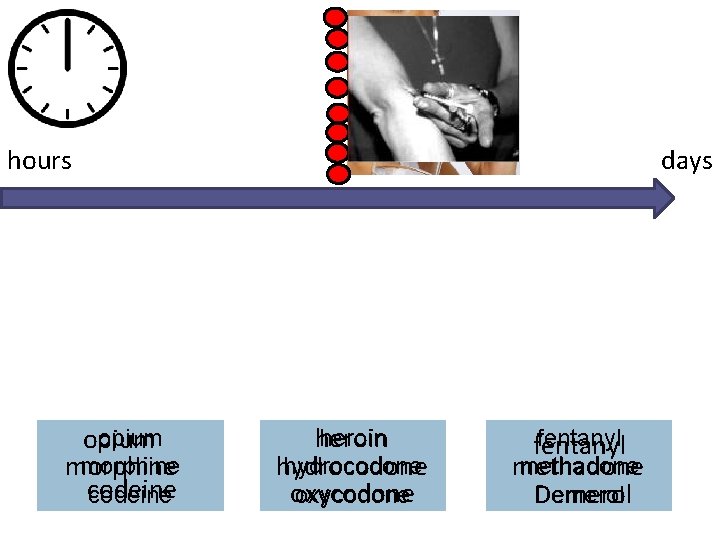
hours opium morphine codeine days heroin hydrocodone oxycodone fentanyl methadone Demerol

How do opioids affect breathing? Opioid Receptors

How Overdose Occurs • Slow Breathing • Breathing Stops • Lack of oxygen may cause brain damage • Heart Stops • Death

What is Narcan® (naloxone)? Narcan knocks the opioid off the opioid receptor, blocking opioid receptors from the opioid Temporarily takes away the “high, ” giving the person the chance to breathe Narcan works in 1 to 3 minutes and lasts 30 to 90 minutes Narcan neither be abused nor cause overdose only contraindication is known sensitivity, which is very rare Too much Narcan cause withdrawal symptoms such as: • • • nausea/vomiting diarrhea chills • • • muscle discomfort disorientation combativeness

How does Narcan affect overdose?
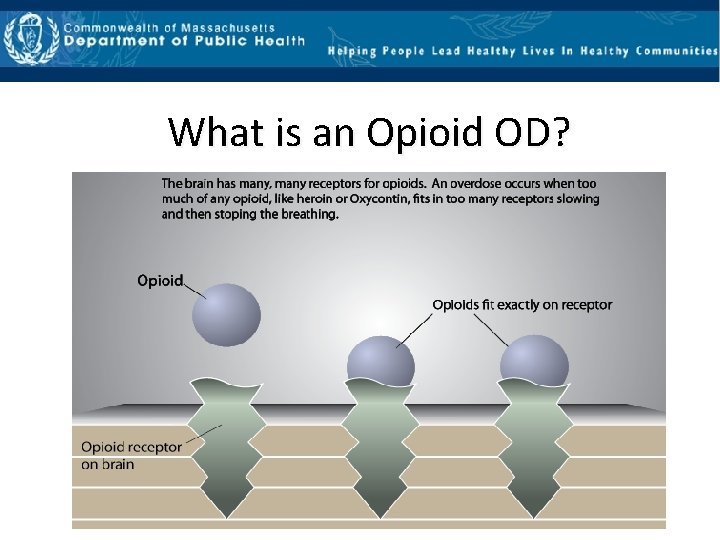
What is an Opioid OD?

Naloxone Reversing Overdose


Mixing Opioids with Benzos • • • Combining opioids with benzodiazepines or alcohol leads to a worse outcome Benzos are psychoactive drugs prescribed for sedation, anxiety, sleep and seizures The most commonly used benzos are: Klonopin, Valium, Ativan, Librium, and Xanax

Medications for Opioid Overdose and Treatment • Narcan® = naloxone • Reverses opioid overdose • Short and fast‐acting opioid blocker No street value because they cause • Vivitrol® = naltrexone • Treatment for opioid and alcohol addiction withdrawal symptoms • Long‐acting opioid blocker • Suboxone® = buprenorphine + naloxone • Treatment for opioid addiction Streetor value • The naloxone is added to discourage injecting sniffing because • Subutex® = buprenorphine only they can relieve withdrawal symptoms • Treatment for opioid addiction in pregnant women • Methadone aka dolophine and methadose • Treatment for opioid addiction or pain

Revolving door? ? ? • As it is for tobacco and weight loss, it takes multiple attempts before achieving success – By definition, addiction is a chronic condition where people make risky choices despite negative consequences • With time, treatment works ‐ people get better • With treatment, crime is less common and therefore they interact with police less often – Law enforcement because its law enforcement is more likely to see the relapses than recovery

Administering Naloxone

Reminder • Naloxone is not a controlled substance but is a regulated substance (a prescription medication) that requires a licensed prescriber

Office of Emergency Medical Services Pre-Hospital Statewide Treatment Protocols Currently includes only Multi‐Step and Auto‐Injector http: //www. mass. gov/eohhs/docs/dph/emergency‐services/treatment‐protocols‐ 2015‐ 1. pdf


Scene Safety and Potential Hazards Oncoming traffic Unstable surfaces Leaking gasoline Downed electrical lines • Potential for violence • Fire or smoke • • • Hazardous materials • Other dangers at crash or rescue scenes • Crime scenes • NEEDLES • PEOPLE WEAR GLOVES: Assume all body fluids present a possible risk for infection

Recognize Overdose • If a person is not breathing or is struggling to breath: call out name and rub knuckles of a closed fist over the sternum (Sternum Rub) • Signs of drug use? – Pills, drugs, needles, cookers • Look for overdose – Slow or absent breathing • Gasping for breath or a snoring sound – Pinpoint pupils – Blue/gray lips and nails • Ensure EMS is activated

Just high/overmedicated vs. overdose Just high/overmedicated • Small pupils • Drowsy, but arousable – Responds to sternal rub Overdose • Small pupils • Not arousable – No response to sternal rub • Not speaking • Speech is slurred • Breathing slow or stopped • Drowsy, but breathing – < 8 times per minute – 8 or more times per minute – May hear choking sounds or a gurgling/snoring noise – Blue/gray lips and fingertips >> Stimulate and observe >> Rescue breathe + give naloxone
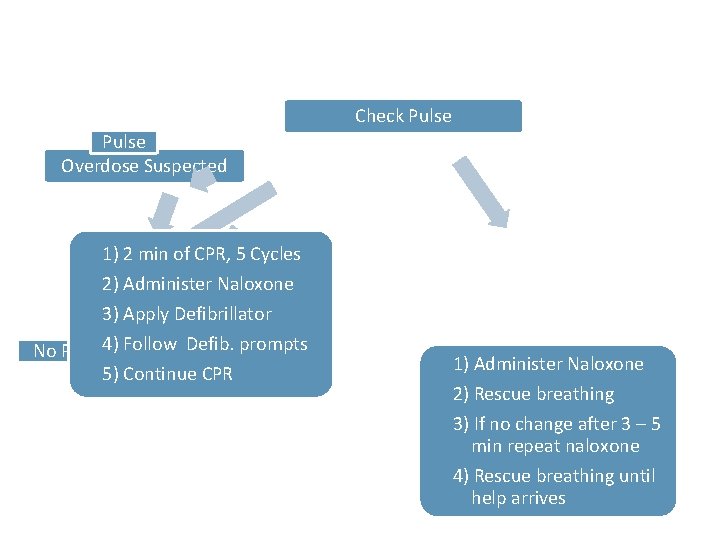
Check Pulse Overdose Suspected 1) 2 min of CPR, 5 Cycles 2) Administer Naloxone 3) Apply Defibrillator No Pulse 4) Follow Defib. prompts 5) Continue CPR 1) Administer Naloxone 2) Rescue breathing 3) If no change after 3 – 5 min repeat naloxone 4) Rescue breathing until help arrives
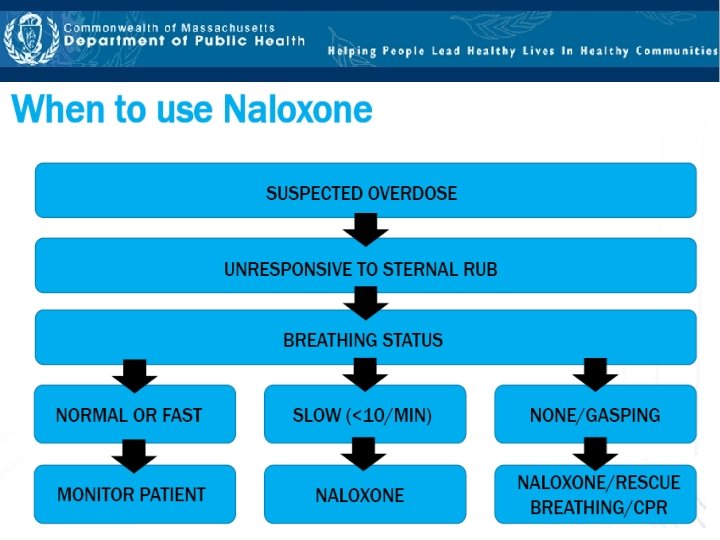
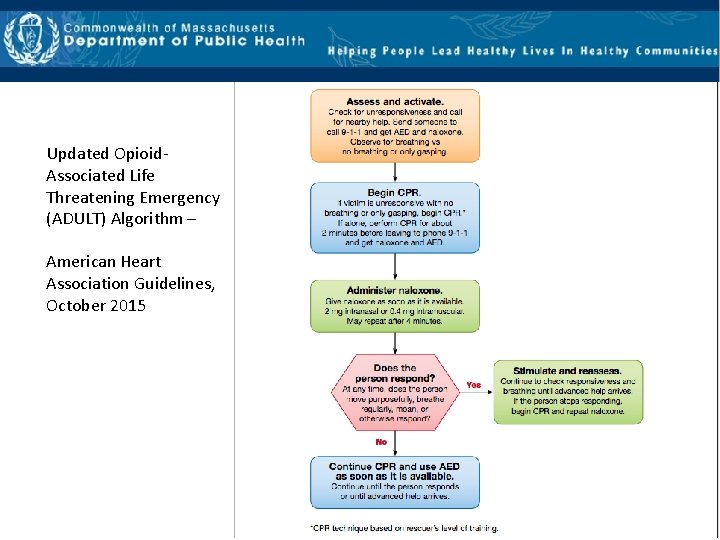
Updated Opioid‐ Associated Life Threatening Emergency (ADULT) Algorithm – American Heart Association Guidelines, October 2015

Remember “Four Rights” for medication administration Massachusetts Office of Emergency Medical Services Minimum Standards for First Responder Training in First Aid, Epinephrine Auto‐Injector and Naloxone Use AR‐ 2‐ 100 • Right Patient (opioid overdose) • Right Medication (Naloxone‐check for clarity) • Right Date (check expiration) • Right Dose (spray half (1 ml) in each nostril)

Naloxone formulations Nasal with separate atomizer “Multi‐step”* NEW: Nasal Spray “Single‐Step” Auto‐injector* Intramuscular Injection * In OEMS Clinical Protocols for First Responders

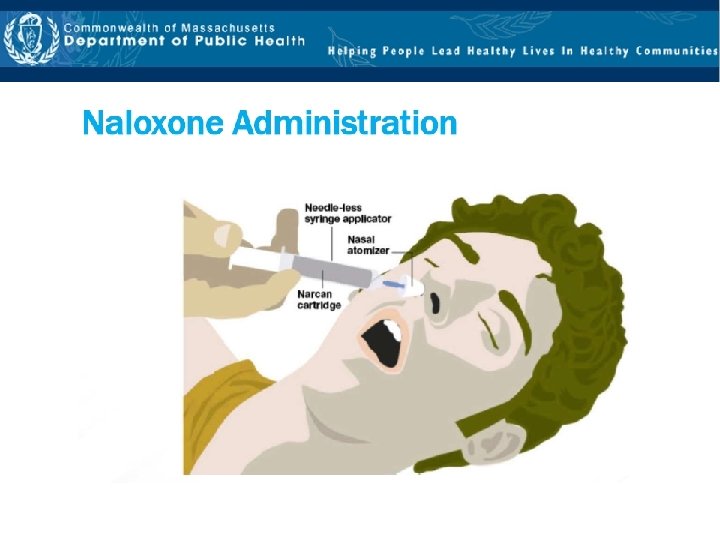
Nasal Naloxone with atomizer – Multi‐step • Intranasal naloxone needs to be dispensed with the mucosal atomization device • If there is nasal trauma or bleeding, do not administer naloxone Benefits of Intranasal Naloxone • Nose is an easy access point • Painless • Eliminates risk of contaminated needle sticks and needle dispensing

Give Naloxone: Nasal with atomizer 1. 2. 3. 4. Remove both yellow caps from the ends of the syringe Twist the nasal atomizer onto the tip of the syringe Remove the purple cap from the naloxone Twist the naloxone on the other side of the syringe

Give Naloxone: Nasal with atomizer • Push 1 ml (1 mg) of naloxone into each nostril • Administer the entire contents of the 2 ml syringe with approximately one half (1 ml) administered in each nostril • Administering one half in each nostril maximizes absorption

NEW: Nasal Spray
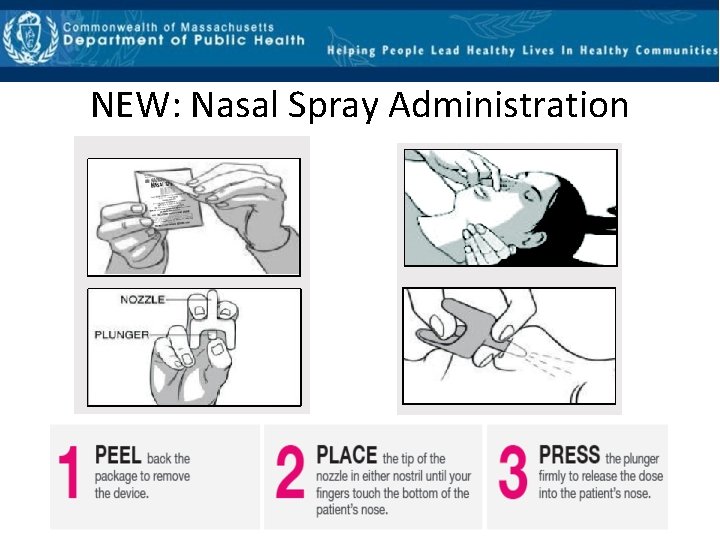
NEW: Nasal Spray Administration

Four important points for the New Nasal Spray Single Step • Do not prime the spray – you will end up wasting it • Insert the tip until your fingers are against the nose • One dose is one nostril • Nasal trauma will reduce the effectiveness

Auto‐injector Naloxone Each auto‐injector contains only 1 dose Inject into muscle or skin of the outer thigh Can be injected through clothing if needed Device injects intramuscularly or subcutaneously, delivers the naloxone, and retracts the needle fully into its housing • Needle not visible before, during, or after • •

Auto‐injector Naloxone • Practice with the Trainer to make sure you are able to safely use the auto‐injector in an emergency • The Trainer does not contain a needle or medicine • It can be reused to practice your injection • The red safety guard can be removed and replaced on the Trainer

Give Naloxone: Auto‐injector

Give Naloxone: Auto‐injector

Give Naloxone: Auto‐injector

Give Naloxone: Auto‐injector

How does a person respond to Naloxone? Range of responses: 1. Gradually improves breathing and becomes responsive within 3 – 5 minutes 2. Immediately improves breathing, responsive, and is in withdrawal 3. Starts breathing within 3 – 5 minutes but remains unresponsive 4. Does not respond to first dose and naloxone must be repeated in 3 – 5 minutes (keep rescue breathing) 5. No response to multiple doses of naloxone
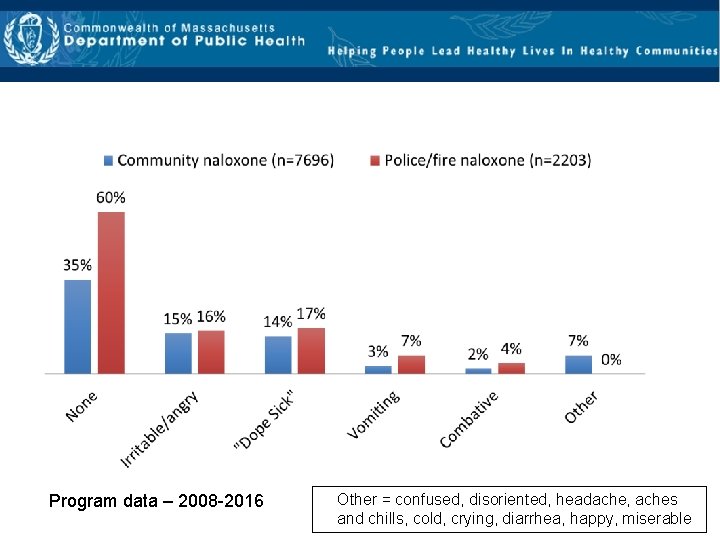
Withdrawal symptoms after naloxone rescue (2010 -2014) Program data – 2008 -2016 Other = confused, disoriented, headache, aches and chills, cold, crying, diarrhea, happy, miserable

After Administering Naloxone • Continue rescue breathing with 1 ventilation every 5 seconds until EMS arrives • After 3‐ 5 minutes, if the patient is still unresponsive with slow or no breathing, administer another dose of naloxone
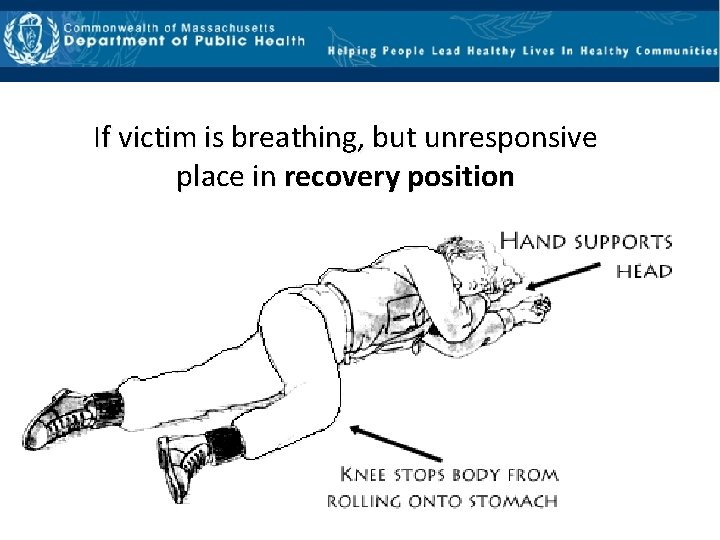
If victim is breathing, but unresponsive place in recovery position

Naloxone Storage • Nasal with separate atomizer: Storage between 59°F to 86°F – Avoid extremes in temperatures for long periods of time – Replace every 6‐ 12 months, before expiration date • New Narcan Nasal Spray: 59°F to 77°F – Replace before expiration • Auto-injector: 59°F to 77°F – – Temperature excursions are permitted between 39°F and 104°F Keep in outer case until needed If solution through viewing window is discolored, cloudy, then replace Replace before expiration date

Naloxone Deployment Options • • Vehicles, front desk, booking area, holding area Vehicle glove compartment Vehicle pelican case Attached to AED case in passenger compartment First in bag Issued per shift Issued per officer

Questions and Answers • Will Naloxone work on an alcohol overdose? – No. Naloxone only works on opioids • What if it is a crack/cocaine or speed/methamphetamine overdose? – No. Naloxone only works on opioids • What is the risk period for an overdose to reoccur after giving Naloxone? – Depends on how long acting the opioid is and how much they took • If the person isn’t overdosing and I give them Naloxone will it hurt them? – No. If in doubt give naloxone.

What if a person refuses care and transport after Naloxone is administered? • Inform the person of the risk of re‐overdosing • Inform the person naloxone is only temporary • If person still refuses consider the mechanism of injury or Illness • Do you believe he/she can refuse treatment with a sound mind and clear understanding of the circumstances? Remember they just overdosed! • If no, the person can not refuse treatment

Good Samaritan & Naloxone Law Passed August 2012

OEND program rescues: 2006‐ 2016 Active use, in treatment, in recovery N=4, 854 Non‐User (family, friend, staff) N=551 911 called or public safety present 40% 68% Stayed until alert or help arrived 91% 95% Program data
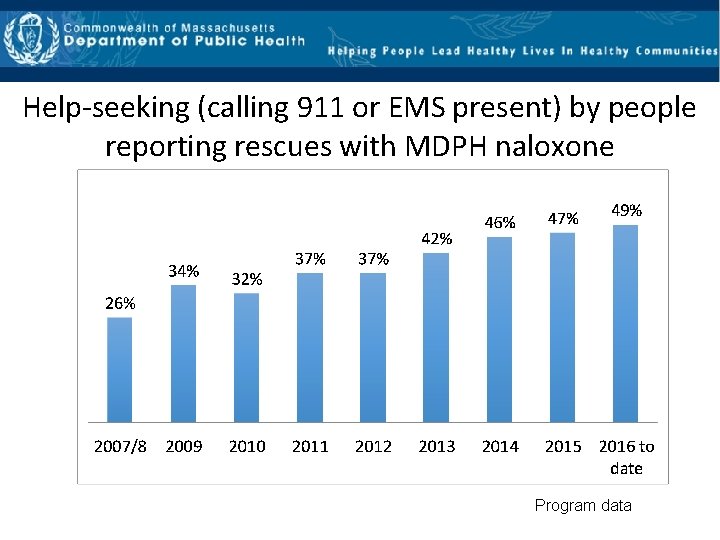
Help‐seeking (calling 911 or EMS present) by people reporting rescues with MDPH naloxone Program data

911 Good Samaritan Campaign “Make the Right Call” Collaboration between DPH and the Office of the Attorney General. Campaign includes a Roll‐Call video done in collaboration with the Mass Chiefs of Police Association. https: //youtu. be/o. NFns. Pygjx 8 www. mass. gov/maketherightcall

Encouraging people to call for help • First responders play a key role • Bystanders not calling is one of the reasons people are dying – Fear of public safety reduces 911 call rates • Interactions at overdose scenes with people who use drugs can reduce fear of public safety
Acts of 2012, Chapter 192, Sections 11 & 32

Good Samaritan Law Policy

Example of incorporating MGL c. 94 C s 34 A into Department Policy

Bulk Purchasing Program • As a First Responder department, you may purchase naloxone directly from the State Office of Pharmacy Services (SOPS) • The legislation establishing the trust fund authorizes DPH to reduce the cost of naloxone for municipal first responder agencies below the negotiated SOPS purchase price • Contact: Edward Cavallari – Edward. Cavallari@massmail. state. ma. us – 978‐ 858‐ 2153

Technical Assistance Online Resources: Mass. TAPP Page: http: //masstapp. edc. org/first‐responder‐naloxone‐ narcan‐technical‐assistance DPH-BSAS Page: http: //www. mass. gov/eohhs/gov/departments/dph/pr ograms/substance‐abuse/prevention/naloxone‐ access. html

Thank You
- Slides: 75