FINANCIAL DISCLOSURES The authors do not have any




- Slides: 7

FINANCIAL DISCLOSURES The authors do not have any financial disclosure

BILATERAL POSTOPERATIVE POSTERIOR ISCHEMIC OPTIC NEUROPATHY AFTER LOW RISK SURGERIES Paulo Silva Guerra MD, Manuela Novais MD, Ivone Cravo MD, Fátima Campos MD, Ana Fonseca MD, Walter Rodrigues MD, Manuel Monteiro-Grillo MD Neurophthalmology Department. Hospital de Santa Maria. Lisbon/Portugal Director: Prof. Dr. M. Monteiro Grillo

Introduction • Posterior Ischemic Optic Neuropathy (PION) predominates in patients who have had spine and neck procedures. 8 • Risk factors for visual loss include hypotension, anemia, prone position, increased surgical time and increased venous pressure, among others. 6, 9 • There is no proven effective treatment. Perioperative correction of hemodynamic abnormalities may be beneficial. 4 Purpose: ü To report 2 cases of bilateral postoperative posterior ischemic optic neuropathy after gynecological surgery.

Material & Methods ü Retrospective analysis of 2 patients with 44 and 31 years, who experienced bilateral and painless sudden visual loss in the immediate postoperative period after tubal ligation and complicated distocic delivery.

Case 1 • ♀, 44 years, painless visual loss upon awakening from anesthesia after tubal ligation • Visual Acuity at presentation: RE-0, 5 LE-0, 5 • Normal optic discs • MRI Brain/Orbit - Normal • Reduced color vision (red-green axis) • Bilateral visual field loss • pattern VEP - amplitudes ↓, normal latency • Blood transfusion, correction of hypotension • After 8 weeks: BILATERAL OPTIC ATROPHY (documented by OCT) • Final VA: 0, 6

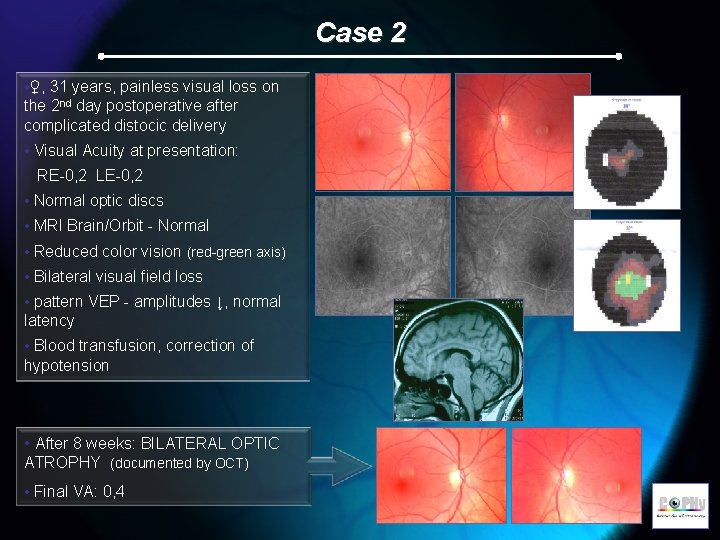
Case 2 • ♀, 31 years, painless visual loss on the 2 nd day postoperative after complicated distocic delivery • Visual Acuity at presentation: RE-0, 2 LE-0, 2 • Normal optic discs • MRI Brain/Orbit - Normal • Reduced color vision (red-green axis) • Bilateral visual field loss • pattern VEP - amplitudes ↓, normal latency • Blood transfusion, correction of hypotension • After 8 weeks: BILATERAL OPTIC ATROPHY (documented by OCT) • Final VA: 0, 4

Conclusions ü The postoperative PION is a diagnosis of exclusion. ü Young patients without atherosclerotic risk factors may develop postoperative posterior ION after low risk surgeries. ü In patients complaining of visual loss in the postoperative period who have a normal fundus and normal neuroimaging, a diagnosis of PION should be suspected. References: 1. Hayreh SS. Posterior ischaemic optic neuropathy: clinical features, pathogenesis, and management. Eye. 2004 Nov; 18(11)1188 -206. 2. Moster ML. Visual loss after coronary artery bypass surgery. Surv Ophthalmol. 1998 Mar. Apr; 42(5): 453 -7. 3. Sweeney PJ, Breuer AC, Selhorst JB, Waybright EA, Furlan AJ, Lederman RJ, et al. Ischemic optic neuropathy: a complication of cardiopulmonary bypass surgery. Neurology. 1982 May; 32 (5): 560 -2. 4. Newman NJ. Perioperative visual loss after nonocular surgeries. Am J Ophthalmol 2008; 145: 604 -610. 5. Weber ED, Colyer MH, Lesser RL, Subramanian PS. Posterior ischemic optic neuropathy after minimally invasive prostatectomy. J Neuro. Ophthalmol 2007; 27: 285 -287. 6. Murphy MA. Bilateral posterior ischemic optic neuropathy after lumbar spine surgery. Ophthalmol 2003; 110: 1454 -1457. 7. Ho VTG, Newman NJ, Song S, Ksiazek S, Roth S. Ischemic optic neuropathy following spine surgery. J Neurosurg Anesthesiol 2005; 17: 38 -44. 8. Buono LM, Foroozan R. Perioperative posterior ischemic optic neuropathy: review of the literature. Surv Ophthalmol 2005; 50: 15 -26. 9. Sadda SR, Nee M, Miller NR, et al. Clinical spectrum of posterior ischemic optic neuropathy. Am J Ophthalmol. 2001; 132: 743 -750. 10. Lee LA, Roth S, Posner KL, et al. The American Society of Anesthesiologists postoperative visual loss registry. Anesthesiology 2006; 105: 652 - 659. 12. Myers MA, Hamilton SR, Bogosian AJ, et al. Visual loss as a complication of spine surgery: a review of 37 cases. Spine 1997; 22: 1325 -1329. 13. Kim JW, Hills WL, Rizzo JF, et al. Ischemic optic neuropathy following spine surgery in a 16 -year old patient and a 10 -year-old patient. J Neuro Ophthalmol 2006; 26: 30 -33