Final pathway of lymphatics The Thoracic Duct Introduction
























- Slides: 30

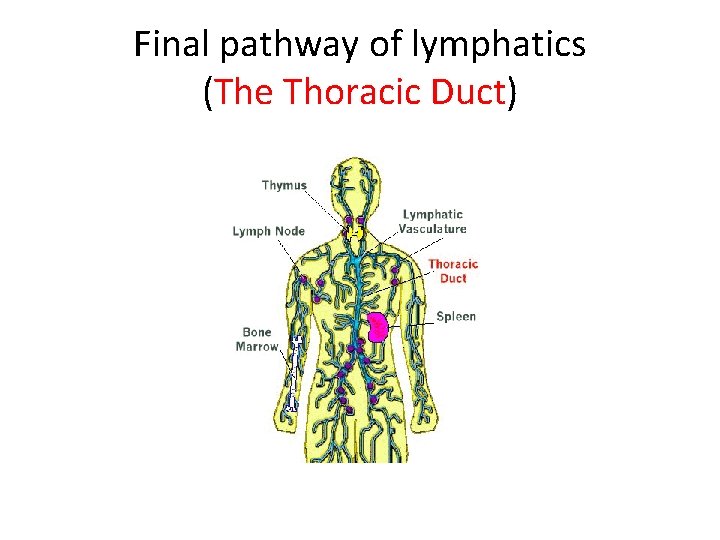
Final pathway of lymphatics (The Thoracic Duct)

Introduction • The lymphatic system serves as a slow flowing, low pressure drainage system • That collects a small portion of the interstitial fluid (ISF, lymph) from throughout the body • Returns it to the bloodstream.

What actually is the lymph? • Lymph is the fluid that circulates throughout the lymphatic system. • The lymph is formed when the interstitial fluid (the fluid which lies in the interstices of all body tissues) is collected through lymph capillaries. • It is then transported through lymph vessels to lymph nodes • Before emptying ultimately into the right or the left subclavian vein, where it mixes back with blood.

Composition of lymph • Since the lymph is derived from the interstitial fluid, its composition continually changes as the blood and the surrounding cells continually exchange substances with the interstitial fluid. • It is generally similar to blood plasma except that it also contains white blood cells. • Lymph returns proteins and excess interstitial fluid to the bloodstream. • Lymph may pick up bacteria and bring them to lymph nodes where they are destroyed. • Metastatic cancer cells can also be transported via lymph. Lymph also transports fats from the digestive system.

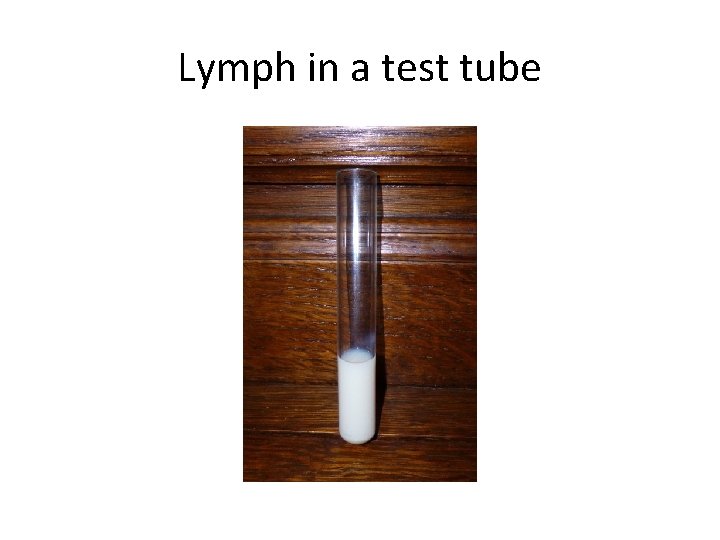
Composition contd. • Lymph has a composition comparable to that of blood plasma, but it may differ slightly. • Lymph contains white blood cells. • In particular the lymph that leaves a lymph node is richer in lymphocytes. • Likewise, the lymph formed in the human digestive system called chyle is rich in triglycerides (fat), and looks milky white.

Composition contd. • Another useful way to view the composition of lymph is that it is similar to blood without the red blood cells. • That is not a technically precise definition, but it is a good first-order approximation.

Lymph in a test tube

Formation of lymph • Blood supplies nutrients and important metabolites to the cells of a tissue • It collects back the waste products they produce, which requires exchange of respective constituents between the blood and tissue cells. • However, this exchange is not direct but instead is effected through an intermediary called interstitial fluid or tissue fluid that the blood forms. • Interstitial fluid is the fluid that occupies the spaces between the cells and constitutes their immediate environment.

Formation of lymph contd. • Interstitial fluid forms at the arterial (coming from the heart) end of capillaries because of the higher pressure of blood compared to veins, • and most of it returns to its venous ends and venules • the rest (up to 10%) enters the lymph capillaries as lymph. • Thus, lymph when formed is a watery clear liquid with the same composition as the interstitial fluid. • However, as it flows through the lymph nodes it comes in contact with blood, and tends to accumulate more cells (particularly, lymphocytes) and proteins.

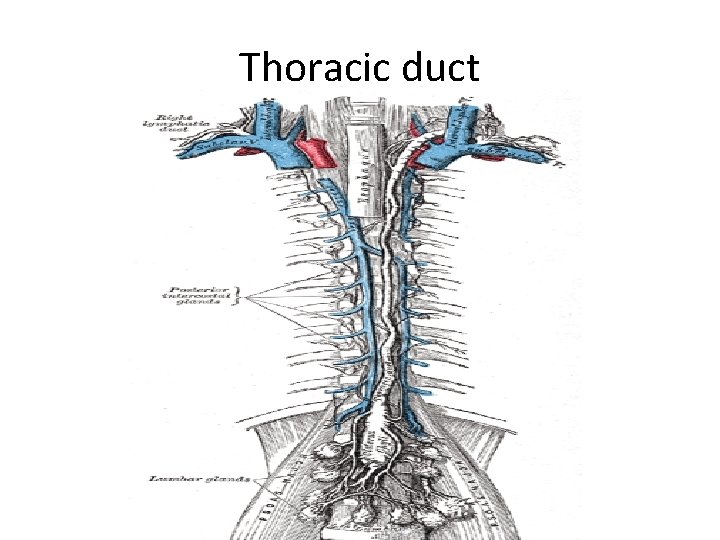
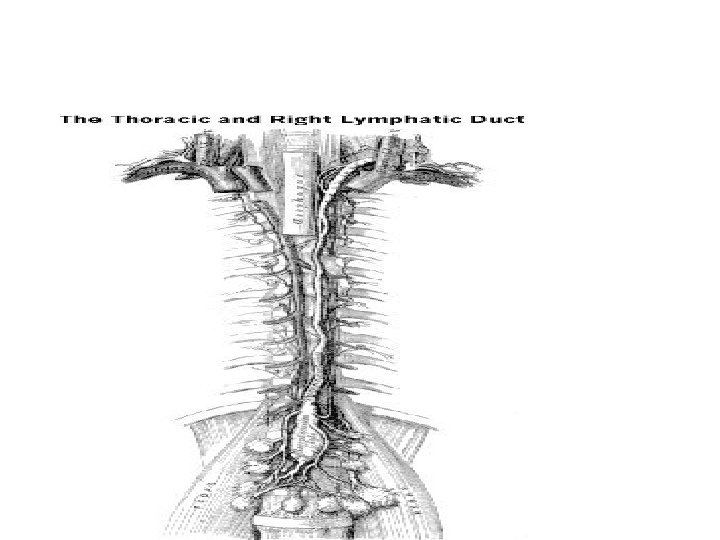
The thoracic duct • Lymph flows slowly along the primary lymphatics, • the lymph empties into progressively larger lymphatic vessels • which ultimately converge as the Thoracic Duct • The thoracic duct finally empties its contents into the right and left subclavian veins in the thorax.

Formation of the thoracic duct • At the level the 2 nd lumber vertebra anteriorly, an enlarged sac is formed by unification of small lymphatics. • This enlarged sac is called Cistern Chyli • The Thoracic Duct arises anterior to the second lumbar vertebra from this enlarged sac, the cistern chyli.

cisterna chyli • The thoracic duct beginning as the cisterna chyli. • This sac like lymphatic mass collects lymph from – lower limbs of the body – as well as the digestive system.

Thoracic duct

Features of lymphatic system • Unlike the circulatory systems, the lymphatic system lacks any central "heart“- like organ to pump lymph throughout the lymph vessels. • Instead, the lymphatic system depends on – muscular movement, – breathing, and – simple gravity • to move lymph fluid throughout the body.

Features of lymphatic system contd. • The Thoracic Duct contains smooth muscle. • The muscle is the same type that exists in the lower digestive system and the arterial system • This is necessary in order to aid lymph flow. • Thus, frequent movement is critical for humans to properly move lymph and prevent lymph fluid build-up in certain areas of the body. (lymph-oedema)


Eponyms of thoracic duct • In human anatomy, the thoracic duct is the largest lymphatic vessel of the lymphatic system. • It is also known as the – – left lymphatic duct, alimentary duct, chyliferous duct, and Van Hoorne's canal. • It carries chyle, a liquid containing both lymph and emulsified fats, rather than pure lymph. • Thus when it ruptures, the resulting flood of liquid into the pleural cavity is known as chylothorax.

Volume / size • In adults, the thoracic duct is typically 38– 45 cm in length • Has an average diameter of about 5 mm. • The vessel usually starts from the level of the twelfth thoracic vertebrae (T 12) and extends to the root of the neck. • It drains into the systemic (blood) circulation at the left subclavian vein. • It also collects most of the lymph in the body other than from the right thorax, arm, head and neck which are drained by the right lymphatic duct. [1]

Course of Thoracic duct • The lymph duct originates in the abdomen from the confluence of – the right and left lumbar trunks and – the intestinal trunk, forming a significant pathway upward called the cisterna chyli. • It traverses the diaphragm at the aortic aperture • It ascends the superior and posterior mediastinum between – the descending thoracic aorta (to its left) and – the azygos vein (to its right).

Termination of the thoracic duct • The duct extends vertically in the chest • Curves posteriorly to the left carotid artery and left internal jugular vein at the T 5 vertebral level to • It empty into the junction of the left subclavian vein and left jugular vein, below the clavicle, near the shoulders.

Special features / transport mechanism • The lymph transport, in the thoracic duct, is mainly caused by the action – of breathing, – aided by the duct's smooth muscle and – by internal valves which prevent the lymph from flowing back down again. • There also two valves at the junction of the duct with the left subclavian vein, • This is to prevent the flow of venous blood into the duct. • In adults, the thoracic duct transports up to 4 L of lymph per day.

Clinical importance (Index of Malignancy) • The first sign of a malignancy, especially an intraabdominal one, may be an enlarged Supraclavicular lymph node. • This is known as Virchow's node, a lymph node in the left supra-clavicular area, • This is found in the vicinity where thoracic duct empties into the left innominate vein, • This is between where the left subclavian vein and left internal jugular join. • This junction is known as the left Pirogoff angle.

chylothorax • When the thoracic duct is blocked or damaged • A large amount of lymph can quickly accumulate in the pleural cavity, • This situation is called chylothorax


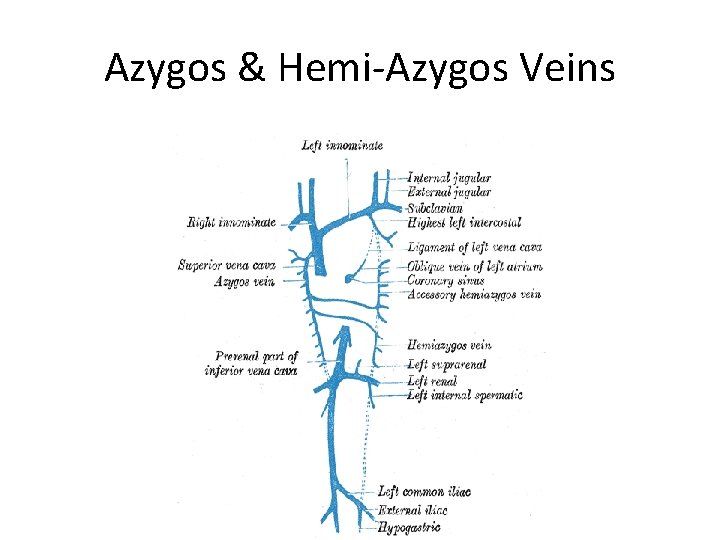
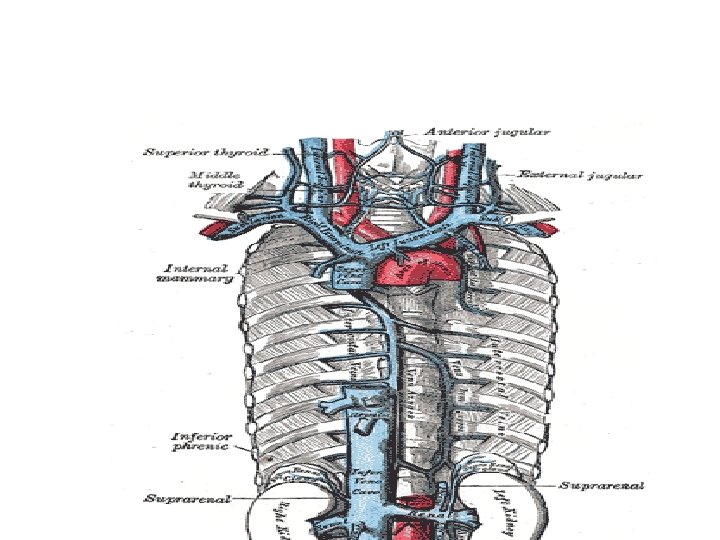
Azygos &Hemi Azygos vein • Azygos means 'unpaired', and hemi means half • The name for hemi-azygos vein is derived from that of the azygos vein. . • This vein mirrors the bottom half the Azygos vein.

Azygos & Hemi-Azygos Veins

Azygos and Hemi Azygos veins • The hemiazygos vein and the accessory hemiazygos vein, when taken together, essentially serve as the leftsided equivalent of the azygos vein. • That is, the azygos vein serves to drain most of the posterior intercostal veins on the right side of the body, • While the hemiazygos vein and the accessory hemiazygos vein drain most of the posterior intercostal veins on the left side of the body. • Specifically, the hemiazygos vein is a mirror image of the bottom part of the Azygos vein.

Variation in formation • The structure of the hemiazygos vein is often variable. • It usually begins in the left ascending lumbar vein or renal vein, • and passes upward through the left crus of the diaphragm to enter the thorax. • It continues ascending on the left side of the vertebral column, • and around the level of the ninth thoracic vertebra, • it passes rightward across the column, behind the aorta, esophagus, and thoracic duct, to end in the azygos vein.

Variation in formation contd. • The hemiazygos may or may not be continuous superiorly with the accessory hemiazygos vein. • It receives the 9 th, 10 th, and 11 th posterior intercostal veins and the subcostal vein of the left side, and some esophageal and mediastinal veins.
