Fighting the Beast of Opiate Use Disorders with

Fighting the Beast of Opiate Use Disorders with Medication Assisted Treatment Martina Moore, Ph. D. , LPCC, LICDC-CS, CEAP, SAP John Carroll University

Opiates: A Natural Pain Remedy • Opiates are alkaloids derived from the opium poppy. Opium is a strong pain relieving medication, and a number of drugs are also made from this source. • Types Of Opiates • • Morphine Codeine Heroin Opium Poppy

• Opioids: Synthetic Pain Medications • Opioids are synthetic or partly-synthetic drugs that are manufactured to work in a similar way to opiates. Their active ingredients are made via chemical synthesis. Opioids may act like opiates when taken for pain because they have similar molecules. Opioids Types Of Opioids • Methadone • Percocet, Percodan, Oxy. Contin (oxycodone) • Vicodin, Lorcet, Lortab (hydrocodone) • Demerol (pethidine) • Dilaudid (hydromorphone) • Duragesic (fentanyl)

Most Commonly Used Opioids & Opiates • Heroin Hydrocodone • Codeine Oxycodone • Demerol Levorphanol • Morphine Vicodin • Darvocet Oxy. Contin • Fentanyl Tylenol 3 • Dilaudid Tylox • Methadone Percocet • Opium Percodan

Both of these types of drugs alter the way that pain is perceived, as opposed to making the pain go away. Opiates & Opioids They attach onto molecules that protrude from certain nerve cells in the brain called opioid receptors. Once they are attached, the nerve cells send messages to the brain that are not accurate measures of the severity of the pain that the body is experiencing. Thus, the person who has taken the drug experience less pain. However, overtime once tolerance develops the experience changes.

Prescription Drug Abuse • Nearly 50% of teens abusing prescription opioids find them in their own homes, in the homes of family members, or at a friend’s house. • Some teens are legitimately being prescribed opioids “medications” by licensed physicians. Many due to injuries while playing sports. • Others buy them off the street or at school. These types of drugs are highly addictive and as the demand grows so does the price. • Some of the higher milligram doses are selling for as much as $60 to $80 per pill.

The fifth vital sign Pain control Pain Relief Mind shift (Physicians and Patients) Physicians trained to manage pain The answer prescription opioids
Opioids can relieve moderate to severe pain. If taking opioids 8 days or longer on a regular basis, withdrawal symptoms may occur, one may need to be weaned off medications slowly. After 8 days there is a 13. 5 % chance of becoming addicted. After 30 days there is a 29. 9% chance of developing addiction. When people use pain medications only to treat pain as directed and for a short time, they are less likely to become addicted. Prescription drug addiction occurs when patients develop a tolerance for the level of medication they have been described and no longer get the same level of relief. Pain Relief

Patients may not have the same expectations for relief as their physicians and may equate the term “painkillers” with the medication being able to take away all of their pain, while their doctor may be thinking in terms of pain management, which means bringing the pain to a level where they can function at a reasonable manner. Pain Management When expectations do not match, patients may take more of the pain medication than prescribed to get a higher level of relief and in turn develop a drug addiction issue.

Addiction is defined as a chronic, relapsing brain disease that is characterized by compulsive drug seeking and use, despite harmful consequences. Addiction It is considered a brain disease because drugs change the brain; they change its structure and how it works. These brain changes can be long lasting and can lead to many harmful, often self-destructive, behaviors. National Institute on Drug Abuse, 2007

Substance use disorders are brain diseases mostly characterized by a person’s inability to control his or her thoughts or intake of a substance. Substance Use Disorders are Diseases A substance use disorder develops after a substance is repetitively consumed and the brain readjusts to its consistent presence. Research shows that adaptations in neuronal functioning occur regardless of whether a person is taking legitimate medication for pain relief, consuming five beers as a first time drinker or injecting heroin on the streets.

Tolerance “When drugs such as heroin or other opiates are used repeatedly over time, tolerance may develop. Tolerance occurs when the person no longer responds to the drug in the way that person initially responded. Stated another way, it takes a higher dose of the drug to achieve the same level of response achieved initially. ” -National Institute on Drug Abuse, 2007

Heroin and other Opiates causes severe physical and psychological symptoms 6 to 8 hours after the last dosage. Painful withdrawal gets worse as time passes. Withdrawal Symptoms Include: • Runny nose, muscle and bone pain • Emotional distress and restlessness • Diarrhea • Vomiting • Hot flashes and heavy sweating • Cold flashes with goose bumps • Insomnia • An overwhelming need for more heroin or opiates • Hence the cycle to avoid the painful withdrawal
Predisposition for Addiction Genetic Factors- Account for about half of the likelihood that an individual will develop addiction. Environmental factors interact with the person’s biology and affect the extent to which genetic factors exert their influence. Resiliencies the individual acquires (through parenting or later life experiences) can affect the extent to which genetic predispositions lead to the behavioral and other manifestations of addiction. American Society of Addiction Medicine, 2011
Culture also plays a role in how addiction becomes actualized in persons with biological vulnerabilities to the development of addiction. Other Factors- Stress, trauma, lack of healthy support etc. No single factor will determine whether a person will become addicted to drugs or not. American Society of Addiction Medicine, 2011 Predisposition for Addiction

So What’s the Problem? • 1 of 5 patients without non-cancer pain or pain related diagnoses are prescribed opioid pain medications. • Nearly 2 million Americans abused or were dependent on prescription opioids in 2014. • From 1999 -2015 more than 180, 000 people died from an overdose related to prescription opioids. • As many as 1 in 4 patients prescribed opioids for chronic pain develops a opioid use disorder.

Prescription Opioid Abuse Often Leads to Heroin Abuse 4 out of 5 new heroin users started misusing prescription opioids 1 1 Hedegaard MD MSPH, Chen MS Ph. D, Warner Ph. D. Drug-Poisoning Deaths Involving Heroin: United States, 2000 -2013. National Center for Health Statistics Data Brief. 2015: 190: 1 -8.

The Shift From Pills to Heroin

Figure 09. UN 06: Crude heroin is dark, whereas purified heroin is a white powder. Courtesy of DEA.




Figure 09. UN 07: Heroin paraphernalia is usually simple and crude but effective: a spoon and a makeshift syringe. © Feng Yu/Dreamstime. com
Figure 09. UN 08: A heroin addict "mainlining" his drug. © Oscar Knott/Fog. Stock/Alamy Images

WHAT WE’RE SEEING IN OHIO
TODAY IN OHIO OVER 4, 000 OVERDOSE DEATHS IN OHIO PER YEAR THAT’S ABOUT 11 OVERDOSE DEATHS PER DAY, EVERY DAY OF THE YEAR

2016 Statistics from CDC According to the CDC there were 4, 050 reported unintentional overdose deaths in Ohio.

Fentanyl Statewide Statistics ODH 2016 Fentanyl and related drugs were involved in 58. 2 percent (2, 357) of all unintentional drug overdose deaths in 2016. In 2015, fentanyl was involved in 37. 9 percent (1, 155). In 2014, fentanyl was involved in 19. 9 percent (503).
Ohio and Opioids To understand how heroin took hold in rural America, you need to go back two decades and look at the surge of prescription drug use in Portsmouth, Ohio. Portsmouth was the pill mill capital of America. They had more pill mills per capita in that town than anywhere else in the country. Pill mills are where a doctor prescribes pills for cash without almost any diagnosis of any pain problems. Portsmouth had a dozen of these, and they prescribed millions of pills a year and was one of the main reasons why so many people got addicted there. (Quinones, 2015)

Ohio and Opioids In the early 2000’s the state of Ohio cracked down on the pill mills closing many of them, thus leaving patients without away to get their prescription. As a result, many of those who originally became addicted to pills eventually wound up on heroin. Mexican drug cartels then stepped in, providing reliable home delivery for the addicts in a model similar to the pizza delivery business, and replicating it far beyond Portsmouth. Selling black tar heroin which is cheaper and more potent. (Quinones, 2015) Heroin became the “fallback drug".
Fentanyl Crisis Fentanyl Synthetic and shortacting opioid analgesic 100 X more potent than Morphine 50 X more potent than Heroin Primary use is for managing acute or chronic pain associated with advanced cancer
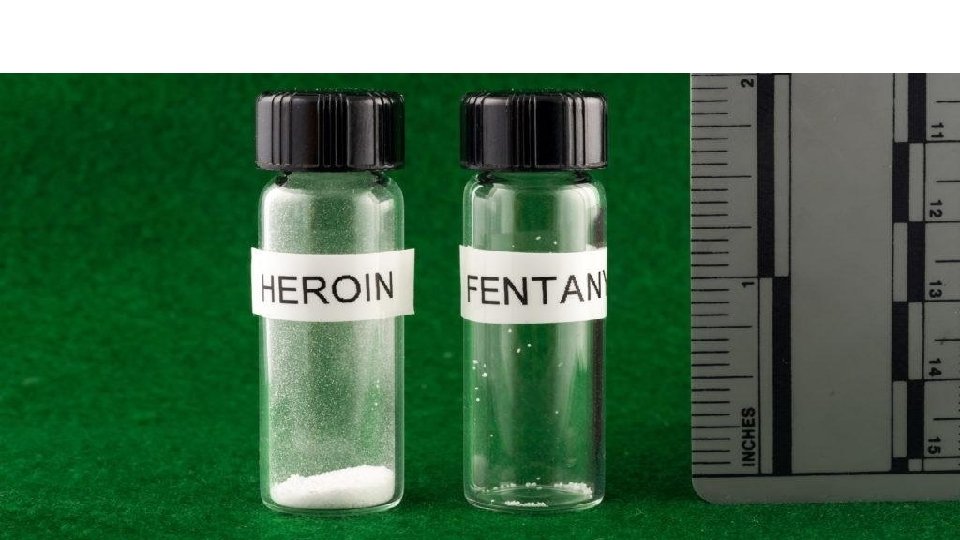
LETHAL DOSE
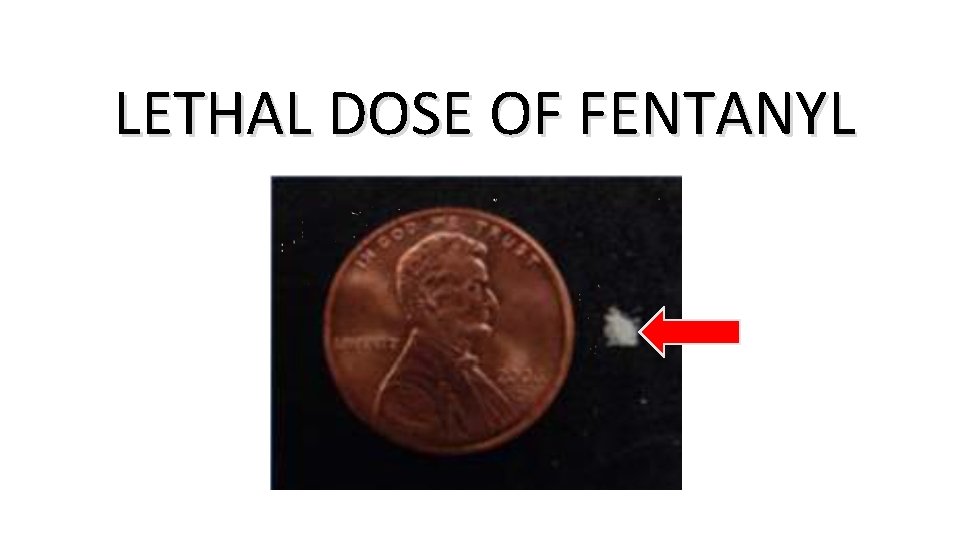
LETHAL DOSE OF FENTANYL

Carfentanil An synthetic opioid used by veterinarians to sedate large animals such as elephants. NOT intended for human consumption Up to 2, 500 times stronger than heroin Emerged recently in Ohio in areas such as Cuyahoga, Hamilton and Summit counties and others EXTREMELY LETHAL Immediate death for many

The Washington Post, reported that Ohio is “ground zero” for the drug Carfentanil in the United States. A tiny dose, a fraction of the weight of a paper clip could send 500 people to the morgue.

LETHAL DOSE CARFENTANIL IS 100 TIMES MORE POWERFUL THAN FENTANYL
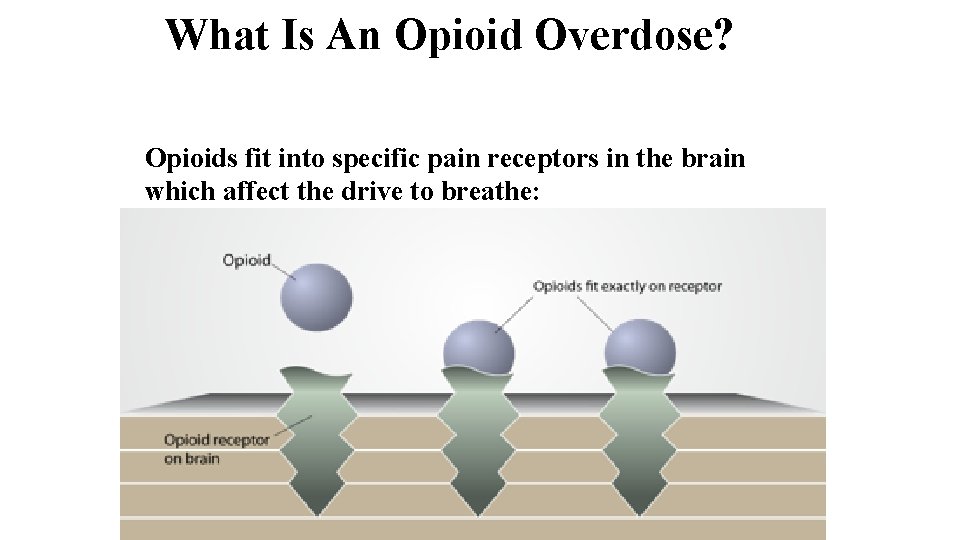
What Is An Opioid Overdose? Opioids fit into specific pain receptors in the brain which affect the drive to breathe:
Overdose can occur immediately after drug ingestion OR could happen hours after drug ingestion Opioid Overdose Fentanyl related overdoses tend to: • Happen instantaneously • Narrow window of time available to rescue the victim • Require additional doses of naloxone to reverse effects of opioids • Victims die from suffocation not the drug Overdose can last up to a couple of hours where the overdose victim experience respiratory depression
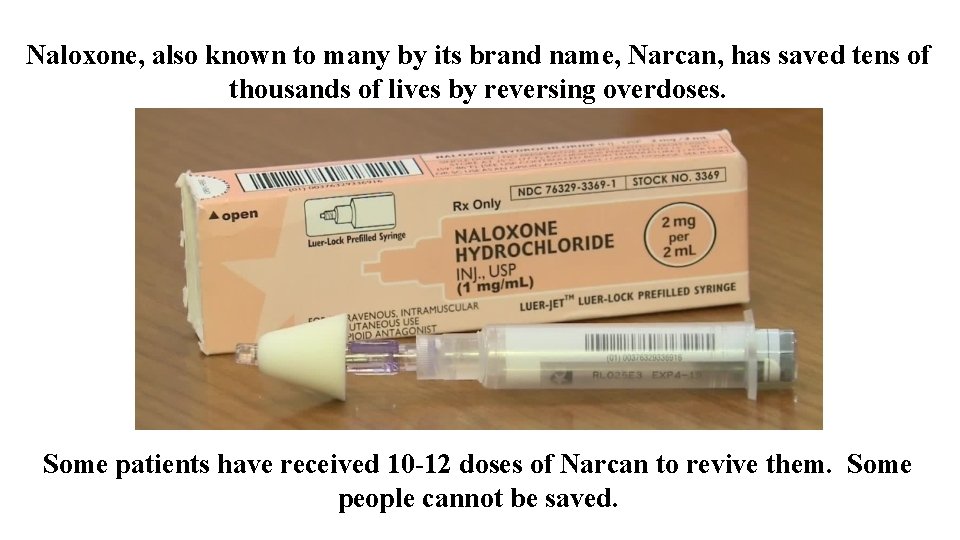
Naloxone, also known to many by its brand name, Narcan, has saved tens of thousands of lives by reversing overdoses. Some patients have received 10 -12 doses of Narcan to revive them. Some people cannot be saved.

Naloxone/Narcan Naloxone (also known as Narcan) is a medication that can reverse an overdose caused by an opioid drug (heroin or prescription pain medications). When administered during an overdose, naloxone blocks the effects of opioids on the brain and quickly restores breathing. Naloxone has been used safely by emergency medical professionals for more than 40 years and has only this one critical function: to reverse the effects of opioids in order to prevent overdose death. Naloxone has no potential for abuse. 41
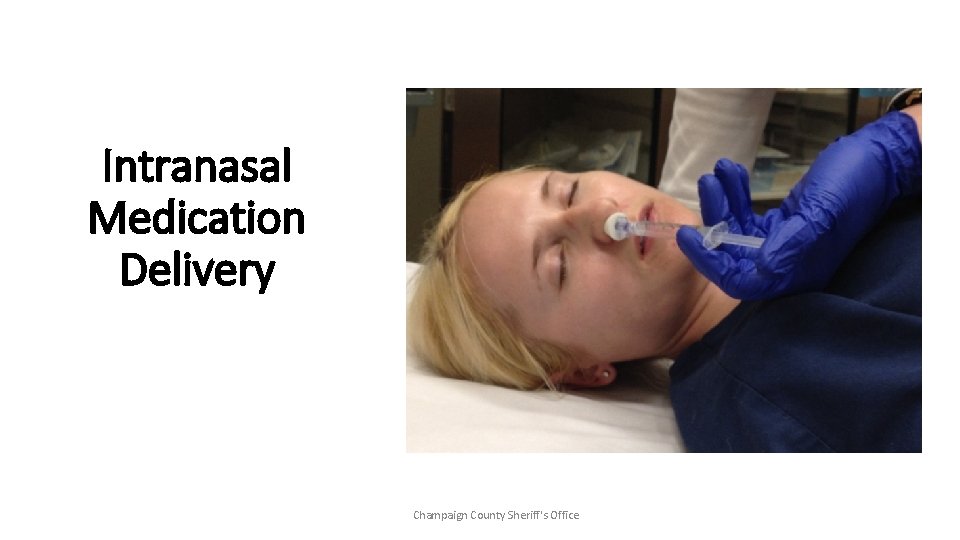
Intranasal Medication Delivery Champaign County Sheriff's Office
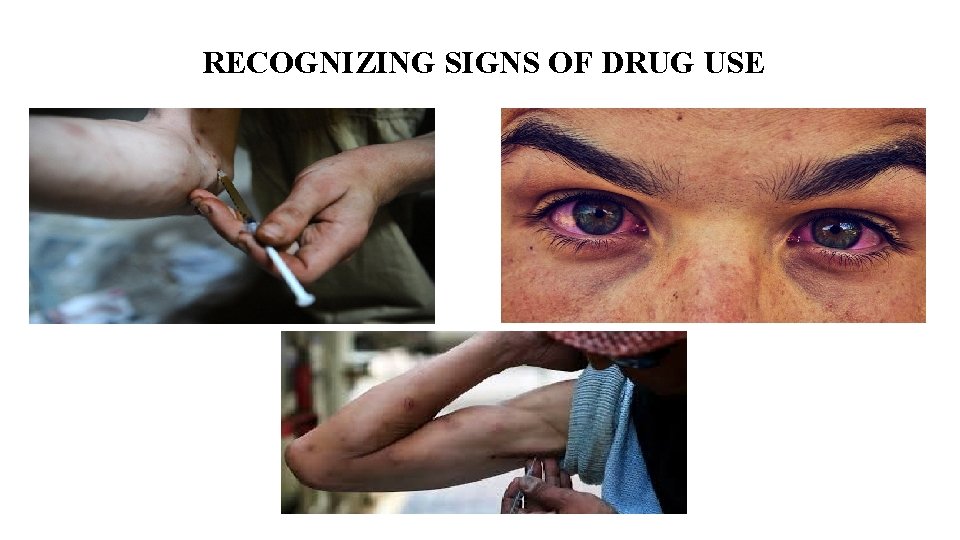
RECOGNIZING SIGNS OF DRUG USE
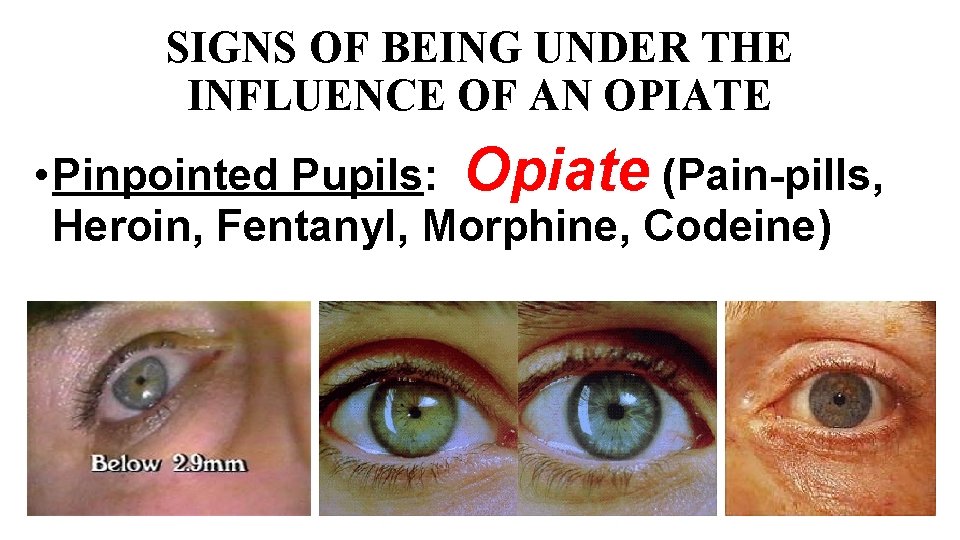
SIGNS OF BEING UNDER THE INFLUENCE OF AN OPIATE • Pinpointed Pupils: Opiate (Pain-pills, Heroin, Fentanyl, Morphine, Codeine)
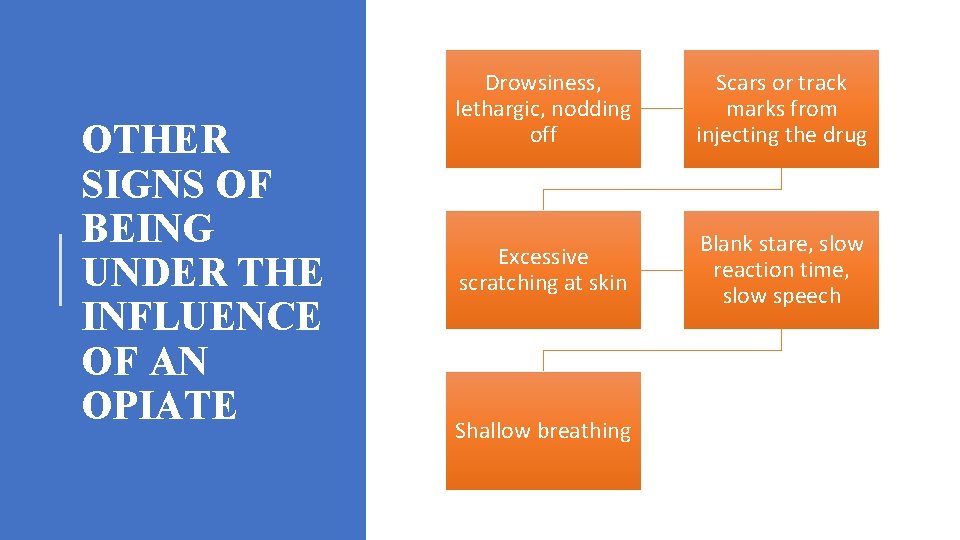
OTHER SIGNS OF BEING UNDER THE INFLUENCE OF AN OPIATE Drowsiness, lethargic, nodding off Scars or track marks from injecting the drug Excessive scratching at skin Blank stare, slow reaction time, slow speech Shallow breathing

The goal of addiction treatment is always to assist a client in stopping the compulsive use of drugs or alcohol and progress to living a normal, functional life. Treatment Addiction creates a host of negative effects to the dependent client, his or her family and friends and society as a whole. Research has shown that the most effective treatment regimen for opioid use disorders is a combination of medication assisted treatment, with cognitive behavioral therapy, and person centered therapy.

Medication Assisted Treatment (MAT) • The medication is only one aspect of treatment. • The medication is intended to help prevent relapse while the addicted individual works to make lasting behavioral changes. • A full treatment continuum should take place along with MAT; counseling and meetings are necessary for lasting recovery.
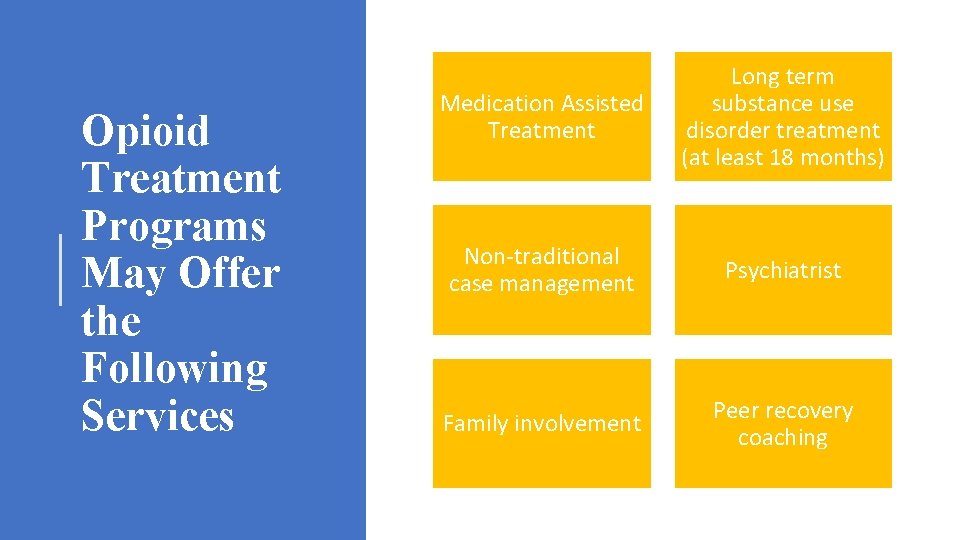
Opioid Treatment Programs May Offer the Following Services Medication Assisted Treatment Long term substance use disorder treatment (at least 18 months) Non-traditional case management Psychiatrist Family involvement Peer recovery coaching
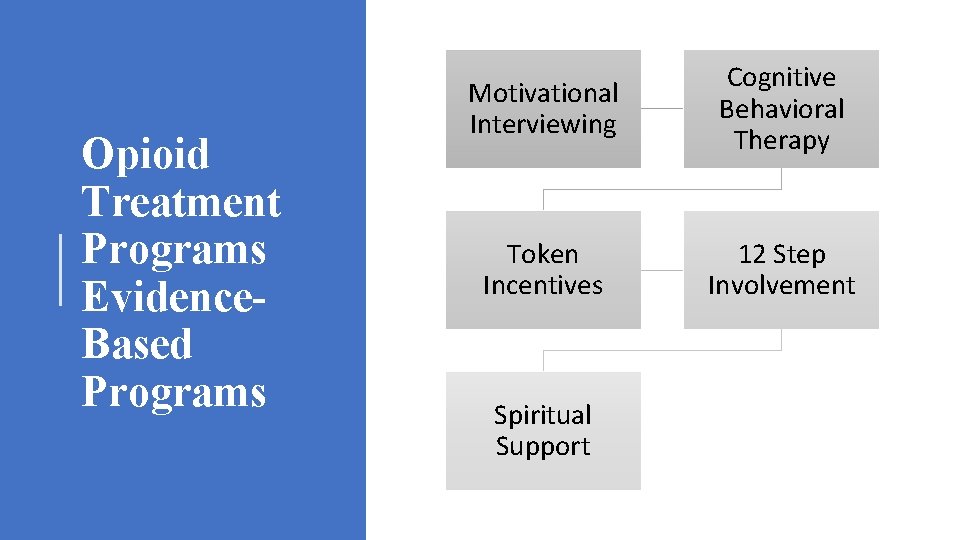
Opioid Treatment Programs Evidence. Based Programs Motivational Interviewing Cognitive Behavioral Therapy Token Incentives 12 Step Involvement Spiritual Support
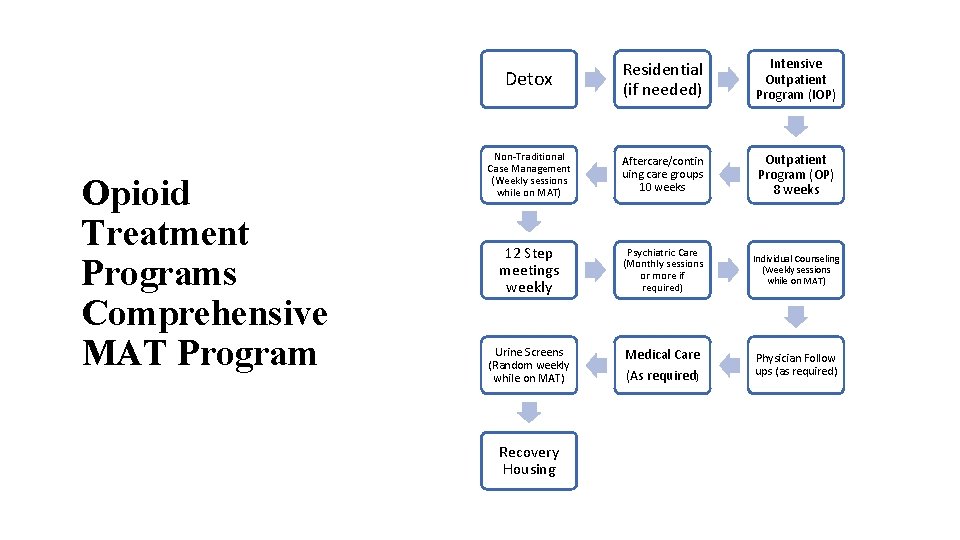
Opioid Treatment Programs Comprehensive MAT Program Detox Residential (if needed) Intensive Outpatient Program (IOP) Non-Traditional Case Management (Weekly sessions while on MAT) Aftercare/contin uing care groups 10 weeks Outpatient Program (OP) 8 weeks 12 Step meetings weekly Psychiatric Care (Monthly sessions or more if required) Individual Counseling (Weekly sessions while on MAT) Urine Screens (Random weekly while on MAT) Medical Care (As required) Physician Follow ups (as required) Recovery Housing
Assessing Readiness to Change When an addiction professional first interacts with a substance dependent client, the client may not be ready to stop using illicit drugs and/or alcohol. In order for clients to experience sustained behavior change, they must voluntarily desire for their lives to be different. Even clients expressing the desire to stop using will have ambivalent feelings about the change process.
Assessing Readiness to Change However, clients enter treatment at varying stages of readiness for treatment and openness to counseling. And experience has shown that some treatment interventions are better suited for particular types of clients, while others are best used at specific time periods during the treatment process. Some are eager, and some are looking for the door as soon as they sign in.

Stages of Change Model • The Stages of Change Model identifies six independent stages of behavior and thinking that clients can experience during the treatment process. • By identifying which stage of change a client is currently in, addiction professionals can better understand the treatment needs of that client and which treatment options are most appropriate.

Medication. Assisted Treatment The single most accurate predictor of successful treatment outcome is the length of time in treatment. Pharmacotherapies can: • help clients remain in treatment longer • achieve complete abstinence • help prevent relapse • reduce frequency and amount of consumption • help them continue to stay committed to meeting their treatment goals and maintain long-term recovery. Pharmacotherapies are effective. Clinical data suggest that clients perform better in treatment when psycho-social-educationalspiritual therapy is combined with appropriate pharmacotherapies. • Medications can serve as a tool to initiate treatment.

MAT of Decreases in the number of opioid overdoses from heroin abuse. addiction is associated Increases retention of patients with: Benefits of MAT in treatment. Decreases drug use, infectious disease transmission. Decreases in criminal activity. (SAMHSA, 2014)

7 MYTHS About MAT

MYTH #1: MAT Trades One Addiction For Another MYTHS About MAT • FACT: MAT bridges the biological and behavioral components of addiction. Research indicates that a combination of medication and behavioral therapies can successfully treat SUDs and help sustain recovery. -National Council for Behavioral Health

MYTH #2: MAT Is Only For The Short Term MYTHS About MAT • FACT: Research shows that patients on MAT for at least 1 -2 years have the greatest rates of long-term success. There is currently no evidence to support benefits from cessation. • FACT: Patients with long-term abstinence can follow a slow taper schedule under a physician’s direction, when free of stressors, to attempt dose reduction or total cessation. -National Council for Behavioral Health

MYTH #3: Many Patients’ Addiction Conditions Are Not Severe Enough to Require MAT MYTHS About MAT • FACT: MAT utilizes a multitude of different medication options (agonists, partial agonists and antagonists) that can be tailored to fit the unique needs of the patient. -National Council for Behavioral Health

MYTH #4: MAT Increases The Risk For Overdose In Patients MYTHS About MAT • FACT: MAT helps to prevent overdoses from occurring. Even a single use of opioids after detoxification can result in a life-threatening or fatal overdose. Following detoxification, tolerance to the euphoria brought on by opioid use remains higher than tolerance to respiratory depression. -National Council for Behavioral Health

MYTH #5: Providing MAT Will Only Disrupt and Hinder a Patient’s Recovery Process MYTHS About MAT • FACT: MAT has been shown to assist patients in recovery by improving quality of life, level of functioning and the ability to handle stress. Above all, MAT helps reduce mortality while patients begin recovery. -National Council for Behavioral Health

MYTH #6: There Isn’t Any Proof That MAT Is Better Than Abstinence MYTHS About MAT • FACT: MAT is evidence-based and is the recommended course of treatment for opioid addiction. The National Institute on Drug Abuse, Substance Abuse and Mental Health Services Administration, National Institute on Alcohol Abuse and Alcoholism, Centers for Disease Control and Prevention, and other agencies emphasize MAT as first line treatment. -National Council for Behavioral Health

MYTH #7: Most Insurance Plans Don’t Cover MAT MYTHS About MAT • FACT: As of May 2013, 31 state Medicaid FFS programs covered methadone maintenance treatment provided in outpatient programs. • State Medicaid agencies vary as to whether buprenorphine is listed on the Preferred Drug List (PDL), and whether prior authorization is required (a distinction often made based on the specific buprenorphine medication type). Extended-release naltrexone is listed on the Medicaid PDL in over 60 percent of states. -National Council for Behavioral Health

TREATING OPIOID DEPENDENCE WITH MEDICATIONS There are 3 medication options for treating opioid dependence ➔Full agonist ➔Partial agonist ➔Antagonist 64

TREATING OPIOID DEPENDENCE WITH A FULL AGONIST Full opioid agonists attach to opioid receptors in a similar manner as opioid drugs like heroin or Oxy. Contin Methadone is a full agonist: ➔ One does not have to withdraw before starting a full agonist ➔ One will experience withdrawal when they stop taking a full agonist ➔ Full agonists prolong dependence on opioids ➔ Full agonists prevents withdrawal symptoms 65

TREATING OPIOID DEPENDENCE WITH A PARTIAL AGONIST Partial opioid agonists attach to opioid receptors and partially activate them SUBOXONE® (buprenorphine) is a partial agonist: ➔ Partial agonists still stimulate the brain’s opioid receptors, but not as much as full agonists ➔ One does not have to withdraw before starting a partial agonist ➔ If one stops a partial agonist abruptly, they will experience withdrawal ➔ Partial agonists prolong physical dependence on opioids 66

TREATING OPIOID DEPENDENCE WITH AN ANTAGONIST OR BLOCKING MEDICATION Opioid antagonists attach to opioid receptors but don’t trigger them Naltrexone/Vivitrol is an Antagonist: ➔ One must withdraw before starting an antagonist ➔ Antagonists are non-addictive and won’t lead to physical dependence ➔ One will not experience withdrawal when stopping an antagonist 67

• The medication is only 1 aspect of treatment. Medication Assisted Treatment • The medication is intended to help prevent relapse while the individual works to make lasting behavioral changes. • A full treatment continuum should take place along with MAT, (counseling/meetings) are necessary for lasting recovery.

QUESTIONS?

Substance Abuse and Mental Health Services Administration. (2014). Results from the 2013 National Survey on Drug Use and Health: Summary of National Findings. NSDUH Series H-48, HHS Publication No. (SMA) 14 -4863. References Centers for Disease Control and Prevention. (2014). Web-based Injury Statistics Query and Reporting System (WISQARS) [online]. http: //www. cdc. gov/injury/wisqars/fatal. html. Birnbaum HG, White AG, Schiller M, Waldman T, Cleveland JM, Roland CL. (2011). Societal costs of prescription opioid abuse, dependence, and misuse in the United States. Pain Medicine, 12: 657 -667. Degenhardt L, Randall D, Hall W. (2009). Mortality among clients of a statewide opioid pharmacotherapy program over 20 years: risk factors and lives saved. Drug Alcohol Depend, 105: 9 -15.

Centers for Disease Control and Prevention. (2015). National Vital Statistics System mortality data. http: //www. cdc. gov/nchs/deaths. htm. References National Institute on Drug Abuse. (2014). Why does heroin use create special risk for contracting HIV/AIDS and hepatitis B and C? https: //www. drugabuse. gov/publications/research-reports/heroin/why-are-heroin-usersspecial-risk-contracting-hivaids-hepatitis-b-c 8. Knudsen HK, Abraham AJ, Roman PM. (2011). Adoption and implementation of medications in addiction treatment programs. Journal of Addiction Medicine, 5: UNODC, World Drug Report 2012. http: //www. unodc. org/unodc/en/data-and-analysis/WDR-2012. html. External link. Pradip et al. Associations of Nonmedical Pain Reliever Use and Initiation of Heroin Use in the US. Center for behavioral Health Statistics and Quality. Data Review. SAMHSA (2013) http: //www. samhsa. gov/data/2 k 13/Data. Review/DR 006/nonmedical-pain-reliever-use 2013. htm. International Narcotics Control Board Report 2008. External link, please review our disclaimer. United Nations Pubns. 2009. p. 20.

Treatment Episode Data Set (TEDS) Highlights – 2007. National Admissions to Substance Abuse Treatment Services. SAMHSA. Paulozzi et al. Increasing deaths from opioid analgesics in the United States Pharmacoepidemiol. Drug Saf. , 15 (2006), pp. 618– 627. References Relieving Pain in America External link, please review our disclaimer. : A Blueprint for Transforming Prevention, Care, Education, and Research. REPORT BRIEF JUNE 2011; Johannes et al. The prevalence of chronic pain in United States adults: results of an Internet-based survey. J Pain. 11(11): 1230 -9. (2010); Gallup-Healthways Well-Being Index. De Leon Casada. Opioids for Chronic Pain: New Evidence, New Strategies, Safe Prescribing The American Journal of Medicine, 126(3 s 1): S 3–S 11. (2013).

American Academy of Pain Medicine; American Pain Society; American Society of Addiction Medicine. Definitions Related to the Use of Opioids for the Treatment of Pain. Glenview, IL, and Chevy Chase, MD: American Academy of Pain Medicine, American Pain Society, American Society of Addiction Medicine; 2001. References Assessment of Analgesic Treatment of Chronic Pain: A Scientific Workshop, linked to 4 -24 -2014 available at http: //www. fda. gov/downloads/Drugs/News. Events/UCM 308363. pdf. SAMHSA: Results from the 2012 National Survey on Drug Use and Health: Summary of National Findings and Detailed Tables. CDC. Vital signs. http: //www. cdc. gov/vitalsigns/Prescription. Painkiller. Overdoses/index. html. Extended-Release Naltrexone to Prevent Opioid Relapse in Criminal Justice Offenders, Joshua D. Lee, et al. , N Engl J Med 2016; 374: 1232 -1242; March 31, 2016 DOI: 10. 1056/NEJMoa 1505409.

www. hhs. gov/opioids/about-the-epidemic/index. html www. odh. ohio. gov//media/ODH/ASSETS/Files/health/injury-prevention/2016 Ohio-Drug-Overdose-Report-FINAL. pdf? la=en References www. thenationalcouncil. org/wpcontent/uploads/2016/12/Myths-vs-Facts-edited_1215. pdf Quinones, S. (2015). Dreamland: The true tale of America's opiate epidemic. New York, NY: Bloomsbury Press.
- Slides: 74