Fibromyalgia Information Foundation Fall Conference 2008 www myalgia

Fibromyalgia Information Foundation Fall Conference 2008 www. myalgia. com

New developments in fibromyalgia research and treatment Robert Bennett MD, FRCP, FACP, MACR FIF

Some of the FM drug studies that are underway or completed ACTIVE STUDIES COMPLETED STUDIES Ultracet * Eszoplicone Calcitonin Reboxetine * Quetiapine Xyrem * Etoricoxib Rotigitone * Armodafinil Nabilone Neurotropin Fluoxetine Naltrexone Amitryptiline Duloxetine Milnacipran Desvenlafaxine Pregabalin * Gabapentin D-ribose MK-677 * Ropinirole Pyridostigmine * Pramipexole * Hydrocortisone * Levitiracetam Lacosamide Casopitant

Two drugs currently FDA approved for fibromyalgia 1. June 21, 2007 - Lyrica (pregabalin) FDA approved indications: Partial onset seizures Post herpetic neuralgia Fibromyalgia 2. June 16, 2008 - Cymbalta (duloxetine) FDA approved indications: Depression Diabetic neuropathy Generalized anxiety disorder Fibromyalgia
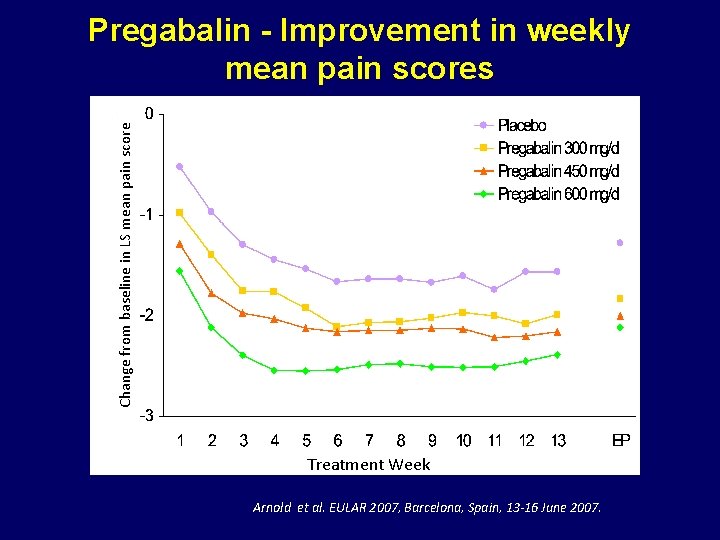
Change from baseline in LS mean pain score Pregabalin - Improvement in weekly mean pain scores Treatment Week Arnold et al. EULAR 2007, Barcelona, Spain, 13 -16 June 2007.
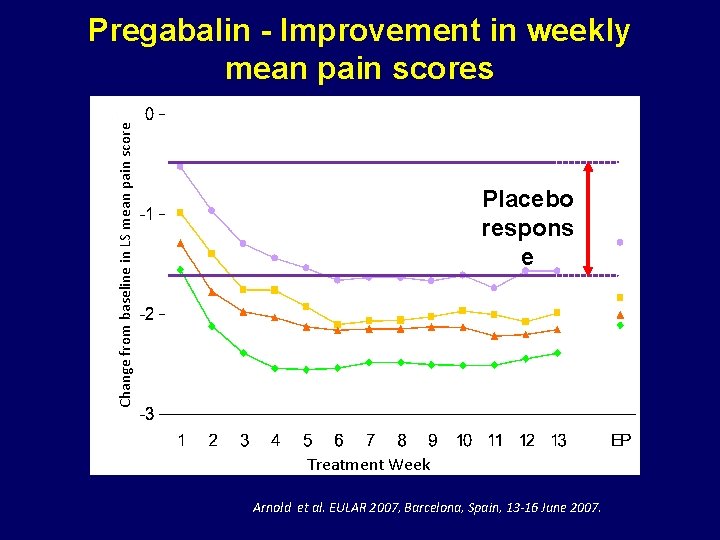
Change from baseline in LS mean pain score Pregabalin - Improvement in weekly mean pain scores Placebo respons e Treatment Week Arnold et al. EULAR 2007, Barcelona, Spain, 13 -16 June 2007.
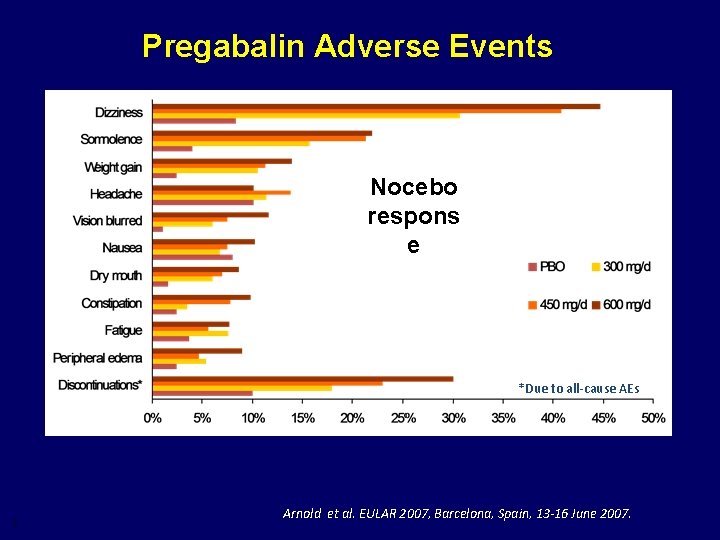
Pregabalin Adverse Events Nocebo respons e *Due to all-cause AEs 7 Arnold et al. EULAR 2007, Barcelona, Spain, 13 -16 June 2007.
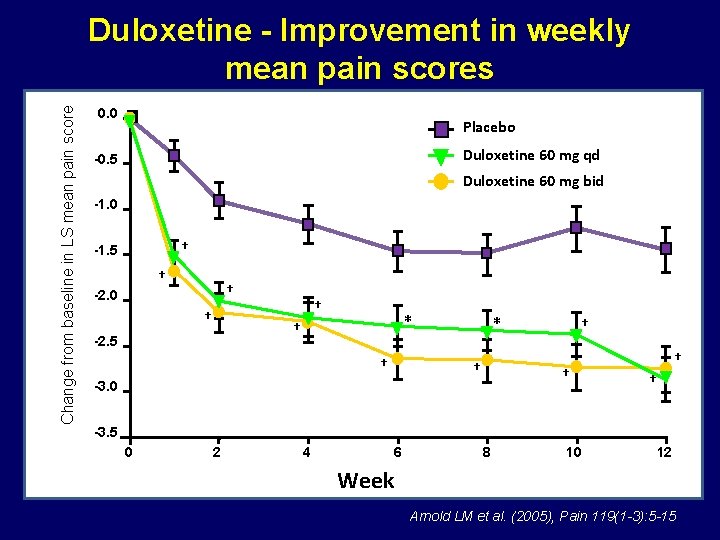
Change from baseline in LS mean pain score Duloxetine - Improvement in weekly mean pain scores 0. 0 Placebo Duloxetine 60 mg qd -0. 5 Duloxetine 60 mg bid -1. 0 † -1. 5 † † -2. 0 † † * † -2. 5 † * † † -3. 0 † -3. 5 0 2 4 6 8 10 12 Week Arnold LM et al. (2005), Pain 119(1 -3): 5 -15
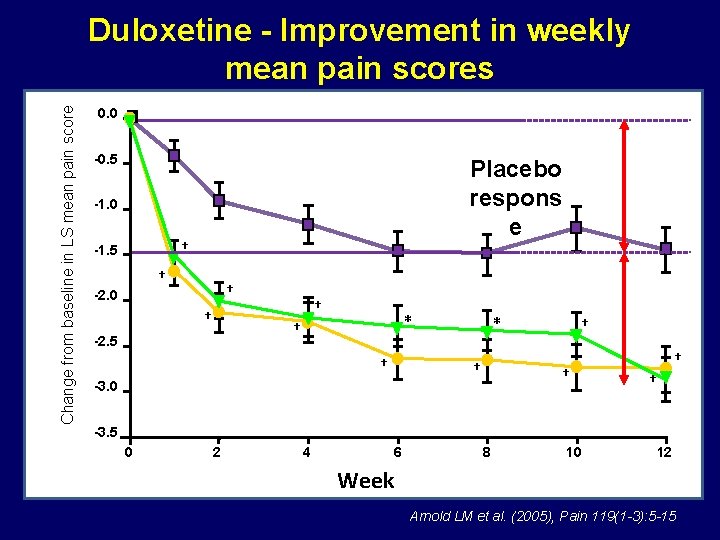
Change from baseline in LS mean pain score Duloxetine - Improvement in weekly mean pain scores 0. 0 -0. 5 Placebo respons e -1. 0 † -1. 5 † † -2. 0 † † * † -2. 5 † * † † -3. 0 † -3. 5 0 2 4 6 8 10 12 Week Arnold LM et al. (2005), Pain 119(1 -3): 5 -15
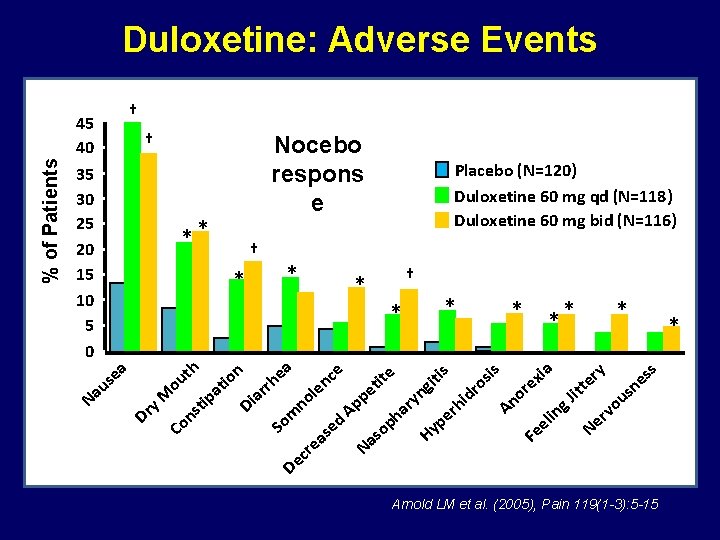
% of Patients Duloxetine: Adverse Events † 45 40 35 30 25 20 15 10 5 0 † Nocebo respons e ** † * Na e us a Placebo (N=120) Duloxetine 60 mg qd (N=118) Duloxetine 60 mg bid (N=116) * * † * ** * s y e n ia is e th is s ea r c t s t x o u i e i i e h t t o g re en ro t rr e at l sn i n o d a J M p p o i u i y i n r p n h o t g y D A r a r s v A n m i r e h n D e p p el ed So y o N Co e s H F as ea N r c De Arnold LM et al. (2005), Pain 119(1 -3): 5 -15 *

Are the placeobo and nocebo response for real? Yes they are for real
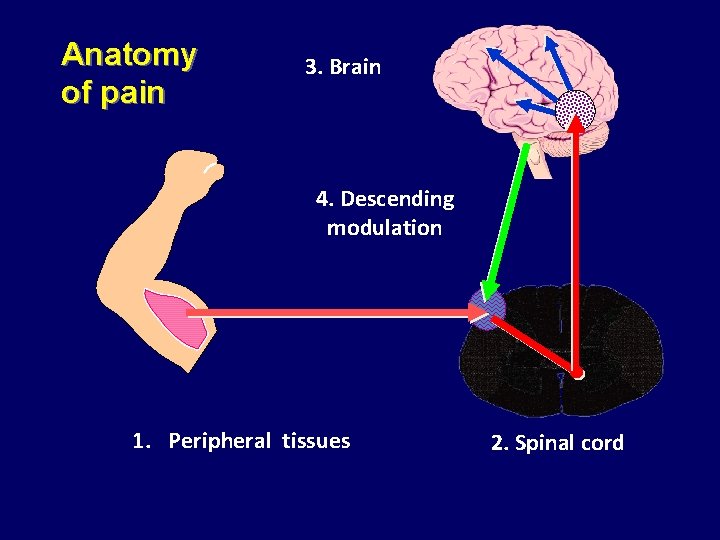
Anatomy of pain 3. Brain 4. Descending modulation 1. Peripheral tissues 2. Spinal cord

What treatments do FM patients really use?
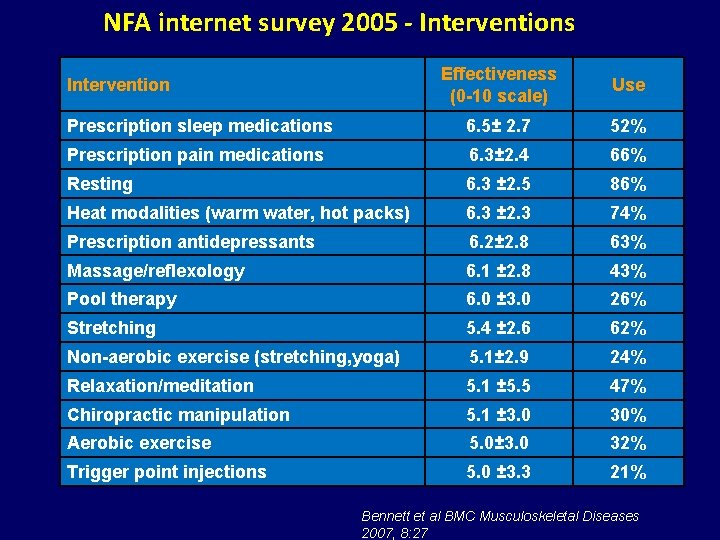
NFA internet survey 2005 - Interventions Effectiveness (0 -10 scale) Use Prescription sleep medications 6. 5± 2. 7 52% Prescription pain medications 6. 3± 2. 4 66% Resting 6. 3 ± 2. 5 86% Heat modalities (warm water, hot packs) 6. 3 ± 2. 3 74% Prescription antidepressants 6. 2± 2. 8 63% Massage/reflexology 6. 1 ± 2. 8 43% Pool therapy 6. 0 ± 3. 0 26% Stretching 5. 4 ± 2. 6 62% Non-aerobic exercise (stretching, yoga) 5. 1± 2. 9 24% Relaxation/meditation 5. 1 ± 5. 5 47% Chiropractic manipulation 5. 1 ± 3. 0 30% Aerobic exercise 5. 0± 3. 0 32% Trigger point injections 5. 0 ± 3. 3 21% Intervention Bennett et al BMC Musculoskeletal Diseases 2007, 8: 27
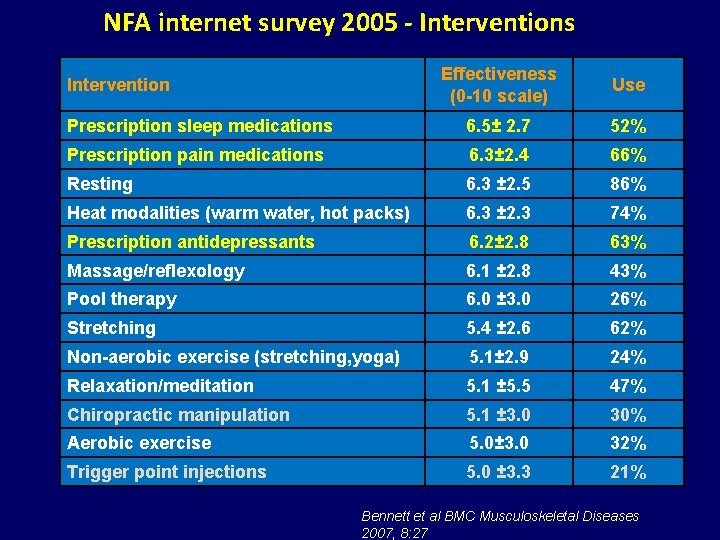
NFA internet survey 2005 - Interventions Effectiveness (0 -10 scale) Use Prescription sleep medications 6. 5± 2. 7 52% Prescription pain medications 6. 3± 2. 4 66% Resting 6. 3 ± 2. 5 86% Heat modalities (warm water, hot packs) 6. 3 ± 2. 3 74% Prescription antidepressants 6. 2± 2. 8 63% Massage/reflexology 6. 1 ± 2. 8 43% Pool therapy 6. 0 ± 3. 0 26% Stretching 5. 4 ± 2. 6 62% Non-aerobic exercise (stretching, yoga) 5. 1± 2. 9 24% Relaxation/meditation 5. 1 ± 5. 5 47% Chiropractic manipulation 5. 1 ± 3. 0 30% Aerobic exercise 5. 0± 3. 0 32% Trigger point injections 5. 0 ± 3. 3 21% Intervention Bennett et al BMC Musculoskeletal Diseases 2007, 8: 27
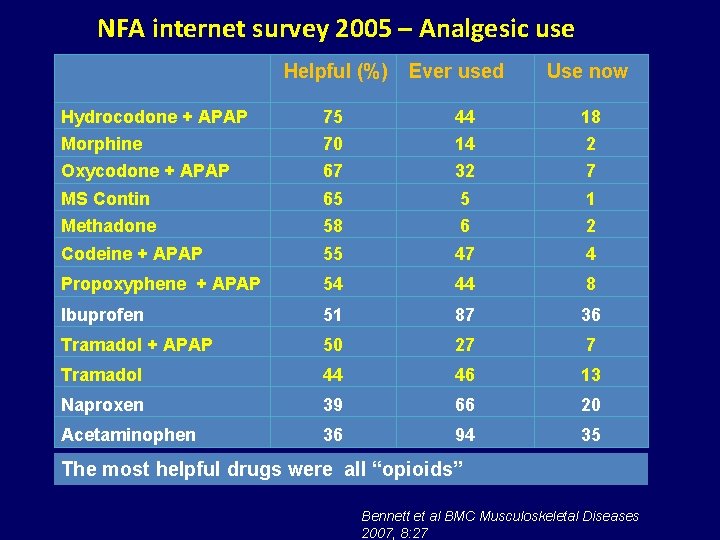
NFA internet survey 2005 – Analgesic use Helpful (%) Ever used Use now Hydrocodone + APAP 75 44 18 Morphine 70 14 2 Oxycodone + APAP 67 32 7 MS Contin 65 5 1 Methadone 58 6 2 Codeine + APAP 55 47 4 Propoxyphene + APAP 54 44 8 Ibuprofen 51 87 36 Tramadol + APAP 50 27 7 Tramadol 44 46 13 Naproxen 39 66 20 Acetaminophen 36 94 35 The most helpful drugs were all “opioids” Bennett et al BMC Musculoskeletal Diseases 2007, 8: 27

PET Scanning The Journal of Neuroscience, September 12, 2007 • 27(37): 10000 – 10006 Neurobiology of Disease Decreased Central-Opioid Receptor Availability in Fibromyalgia Richard E. Harris, Daniel J. Clauw, David J. Scott, Samuel A. Mc. Lean, Richard H. Gracely, and Jon-Kar Zubieta
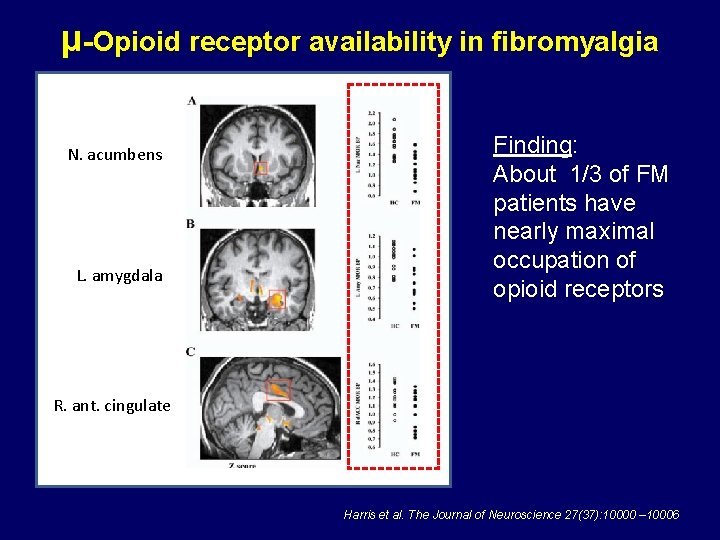
μ-Opioid receptor availability in fibromyalgia N. acumbens L. amygdala Finding: About 1/3 of FM patients have nearly maximal occupation of opioid receptors R. ant. cingulate Harris et al. The Journal of Neuroscience 27(37): 10000 – 10006

What does this stuff really mean? FINDING: Some FM patients have more endorphins than healthy individuals and their endorphin receptors are full CONSEQUENCE: These same patients will be relatively resistant to medications containing opioids

Why do doctors prescribe antidepressants, even when you’re not depressed?
Linking depression and pain Depression is associated with low brain levels of monoamines Serotonin, nor-epinephrine and dopamine
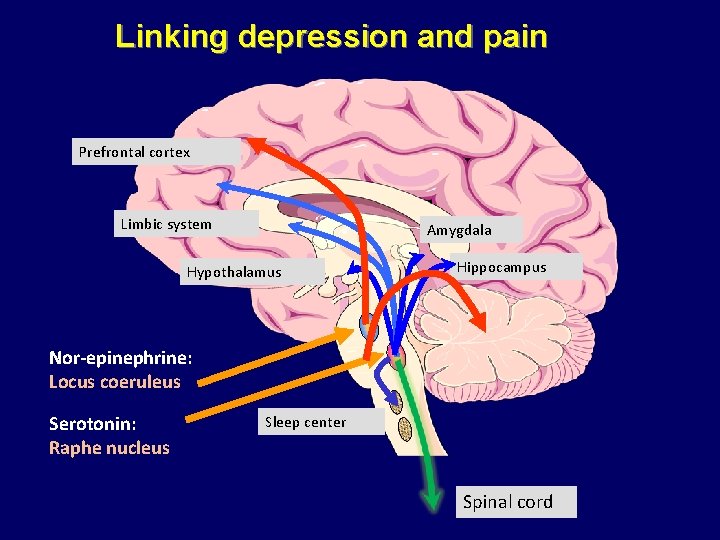
Linking depression and pain Prefrontal cortex Limbic system Amygdala Hypothalamus Hippocampus Nor-epinephrine: Locus coeruleus Serotonin: Raphe nucleus Sleep center Spinal cord
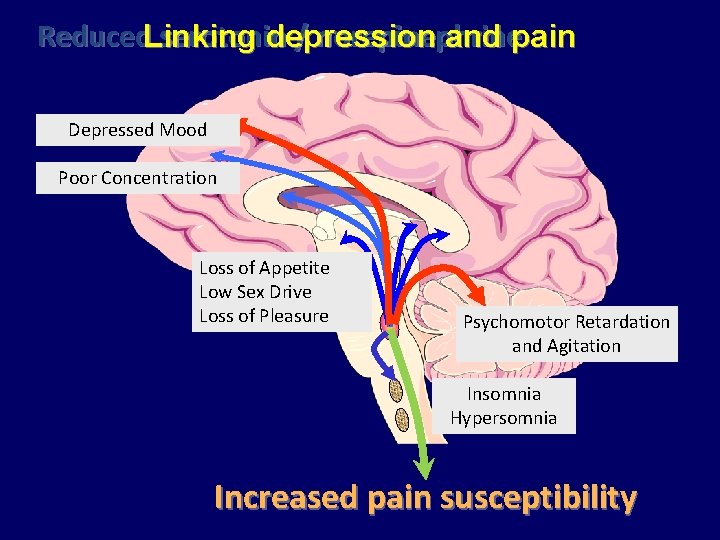
Reduced. Linking serotonin / norepinephrine depression and pain Depressed Mood Poor Concentration Loss of Appetite Low Sex Drive Loss of Pleasure Psychomotor Retardation and Agitation Insomnia Hypersomnia Increased pain susceptibility
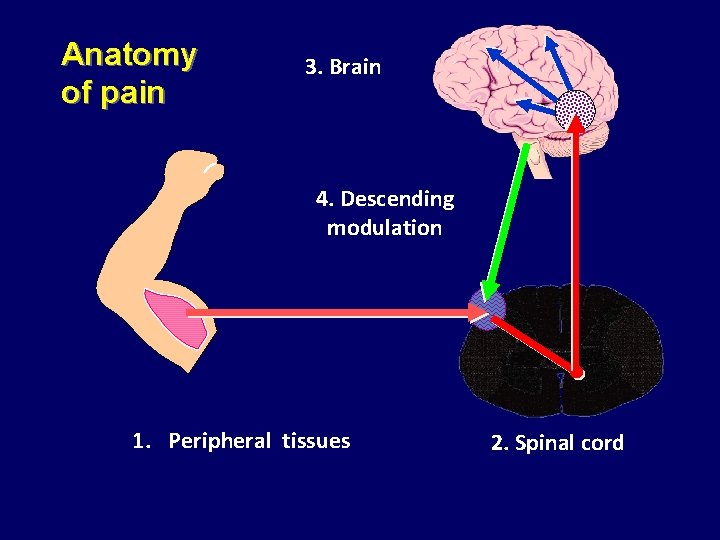
Anatomy of pain 3. Brain 4. Descending modulation 1. Peripheral tissues 2. Spinal cord

N Engl J Med 2005; 352: 1112 -20. The serotonin syndrome is an adverse drug reaction that results from therapeutic drug use or inadvertent interactions between drugs

Serotonin syndrome Cause: excessive stimulation of serotonin receptors Presentation: Agitation or restlessness Nausea, vomiting and diarrhea Confusion , hallucinations Poor coordination Tachycardia Rapid changes in blood pressure Sweating Hyper-reactive reflexes Fever Seizures Coma

Serotonin syndrome – implicated drugs In some patients combinations of the following drugs can lead to a serotonin syndrome: SSRIs: citalopram (Celexa), fluoxetine (Prozac) SNRIs: duloxetine (Cymbalta), venlafaxine (Effexor) NDRIs: buproprion (Wellbutrin) MAOIs: isocarboxazid (Marplan) and phenelzine (Nardil) Analgesics: tramadol (Ultram), fentanyl (Sublimaze) Anti-migraine: sumatriptan (Imitrex) and zolmitriptan (Zomig) Anti-nausea: metoclopramide (Reglan) and ondansetron (Zofran) Bipolar: lithium (Lithobid) Cough: dextromethorphan (Robitussin DM) Herbal supplements: St. John's wort and ginseng This risk depends on genetic make-up (CYP 450 genes)

What you have always wanted to know about Cytochrome P 450 18 families and 43 variants Variant Activity CYP 2 D 6*1 normal CYP 2 D 6*4 absent CYP 2 D 6*5 absent CYP 2 D 6*9 low Nomenclature: CYP 1 A 1, CYP 2 D 6, CYP 3 A 4, etc. CYP 2 D 6*3 absent Function: drug metabolism Relevance: drug interactions Variants are genetically determined CYP 2 D 6*10 low CYP 2 D 6*17 low About 10% of Caucasians have low CYP 2 D 6 activity

Individualize drug dosing based on metabolic profiling of CYP variants 2005 - The FDA-approved Ampli. Chip for analysis of CYP 2 D 6 and CYP 2 C 19, variants of CYP 450 1. Extensive metabolizers. Can be administered drug in "standard“ dosages 2. Intermediate metabolizers. Multiple drug therapy can turn in people into poor metabolizers. 3. Poor metabolizers. May develop drug accumulation and adverse reactions 4. Ultrarapid metabolizers. May experience either no effect or less-thanexpected effectiveness from their drug therapy

You don’t have to wait 5 years Learn about fibromyalgia and help fellow sufferers Adopt a positive attitude, newer treatments are on the way Maintain a regimen of gentle stretching and exercise Learn to be kind to your body Maximize your “sleep hygiene” Give medications a chance (many need 3 -4 weeks to work)

The “New Normal”: Thriving in the here and now! Rebecca Ross RN, Ph. D Psychiatric Mental Health Nurse Practitioner FIF

Identifying YOUR “New Normal” • Fibromyalgia-related changes occur in many spheres of life: – – – Physical Ability, Energy Level, Cognitive Ability, Social Function, Financial Stability, Role Expectations (spouse, parent, employee, etc). “If you cry because the sun has gone out of your life, your tears will prevent you from seeing the stars. ” -William Shakespeare

Accepting “The New Normal” “The secret of health for both mind and body is not to mourn for the past, worry about the future or anticipate troubles, but to live in the present moment wisely and earnestly. ” -- Buddha How to shift “paradigms”: • Identifying negative thoughts/beliefs about your health. • Challenging those thoughts/beliefs. • Adapting thought patterns and behaviors to more effective ways of thinking / behaving.

Mastering “The New Normal” Tasks to Master: • Setting realistic expectations for self and others. • Learning to set healthy boundaries for self and others. • Learning to communicate with difficult friends & family (and acquaintances who think they are “helping”). • Finding and using resources that will help in the journey ahead.

Mastering “The New Normal”: Realistic Expectations • Set realistic expectations with self: – – Let go of what you use to be able to do. Set priorities- Self, family, exercise, friends, work, etc. Educate family/friends about current energy limits. Enlist them is helping you set realistic goals. • Set realistic expectations with others: – You can not be the “fixer” for everyone. – Discuss priorities with important people and ask them to help with communicating their expectations. – Sometimes, you have to JUST SAY NO!

Mastering “The New Normal”: Setting Healthy Boundaries • Energy: 100 units of energy for a 1000 unit day! – Break tasks down. Complete over a few days if necessary. – Six 15 -minute blocks of time, which limits ante-grade pain, is better than an hour at a time and pain for the next two days. – Ask for help AND THEN LET PEOPLE HELP! • Pacing: Time-limited versus task completion. – Let go of perfectionism and unhealthy expectations. – Stop the “I USE to be able to …” statements.

When flares happen, relax & nurture yourself. DON’T PUSH THROUGH THE PAIN!

Mastering “The New Normal”: Communication Techniques • How to communicate with difficult friends/family/acquaintances (who think they are “helping”). – Keep an open mind- it may actually be good advice. – If appropriate, let them know you already have a treatment plan developed with your health care team. – If they are overly persistent, be gentle yet firm with your decline of their “advice”.

Distraction works

Mastering “The New Normal”: Communication Techniques (cont. ) – For those who just don’t know when to stop: • Express your feelings- “I feel frustrated/ invalidated/irritated when you…” • Be patient if possible. Don’t argue, but redirect the conversation- “Be that as it may, I feel…” • Use an easy manner. Manners and humor can sometimes diffuse tense issues- “Interesting, I will ask my health care team about that. ” Optional: “NOT!” (and don’t forget to flash that charm school smile!) – If all else fails, end the conversation • “While I thank you for your concern, my health care team and I have discussed the best treatment options for me and we are doing them. ” –then firmly change the subject or walk away.

Mastering “The New Normal”: Resource List • Resources that may help in the journey ahead: – Websites: • The Fibromyalgia Information Foundation: ww. myalgia. com • The National Fibromyalgia Association: www. fmaware. org – Books: “The ”Complete” Idiots Guide to Fibromyalgia- Lynne Matallana – Magazines: FM AWARE – FM Support Groups- see flyer – FM-friendly exercise group

Thank you for your attention!

What is Wrong With My Exercise Program? Kim Dupree Jones Ph. D, FNP FIF

Ten Things You Should Never Say to Someone with Fibromyalgia 1. 2. "Well, hey, look on the bright side… At least you don't have cancer!" “We all start to ache when we get older. Cardio-combat classes would rev you back up. " 3. “You wouldn't have this if you just lost a few pounds. " 4. "Is fibromyalgia a real disease? Maybe if you relaxed more…" 5. “You just need some vitamins. " 6. "You should probably leave your husband see if your fibromyalgia goes away. " 7. "May I have some of your Vicodin? I could really use one right now for my headache. " 8. "You should move. There must be toxins in your house making you sick. " 9. "My neighbor has fibromyalgia and she works everyday. She says it takes her mind off the pain…“ 10. “But you look OK”
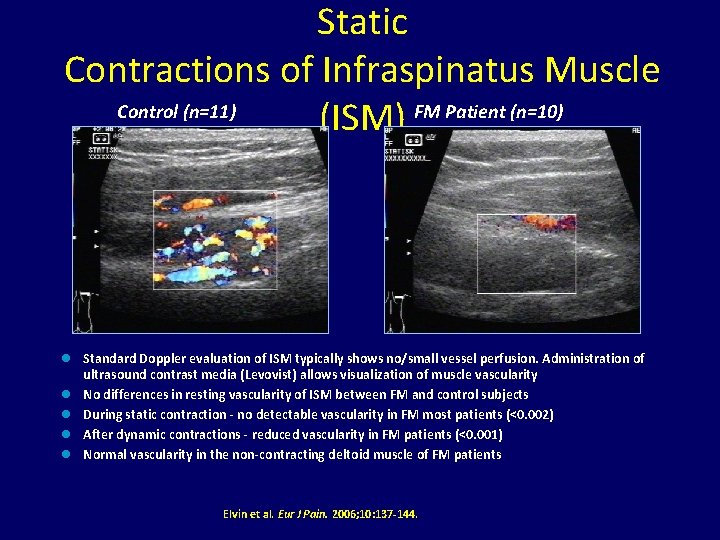
Static Contractions of Infraspinatus Muscle Control (n=11) (ISM) FM Patient (n=10) n n n Standard Doppler evaluation of ISM typically shows no/small vessel perfusion. Administration of ultrasound contrast media (Levovist) allows visualization of muscle vascularity No differences in resting vascularity of ISM between FM and control subjects During static contraction - no detectable vascularity in FM most patients (<0. 002) After dynamic contractions - reduced vascularity in FM patients (<0. 001) Normal vascularity in the non-contracting deltoid muscle of FM patients Elvin et al. Eur J Pain. 2006; 10: 137 -144.

Exercise in FM Can Either Help or Hurt • At least 59 FM intervention studies to date have used aerobics, strength and flexibility training, balneotherapy, most recently balance training • Earlier studies used higher doses of exercise and resulted in greater fitness improvements but worsening symptom scores • Physical functioning, fitness, fatigue, mood, stiffness, sleep and selfefficacy generally improve more than pain • Exercise maintenance may improve with social support and supervision • FM symptom relief may precede fitness improvement • As of last month, we have our 1 st exercise intervention in children with FM Jones 2007, Health Care & QOL: Busch 2008, Cochrane Database Reviews

How to Overcome Postures that Worsen Pain • • Evaluate your posture in a mirror Where are your hands when standing? Are your shoulders pulled up and forward? Is your head pulled forward?
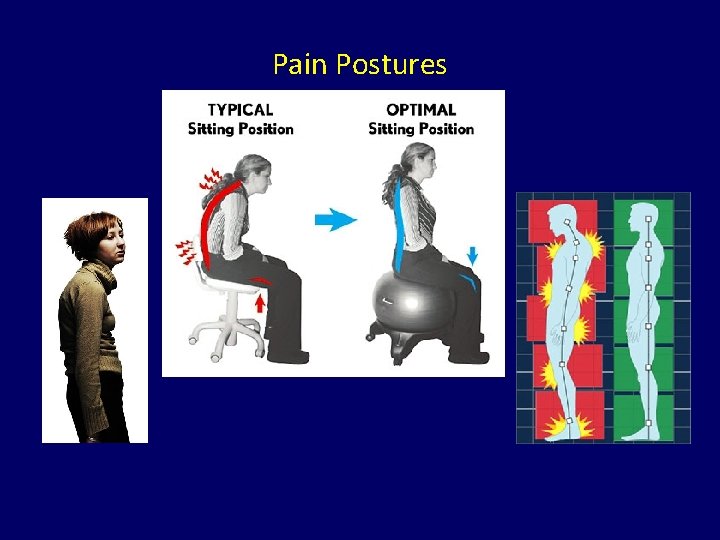
Pain Postures

Exercises to Overcome Pain Postures Stretch Your Anterior Chest

Exercises to Overcome Pain Postures Strengthen Your Upper Back

Am I Afraid I Will Fall While Exercising? • This is a realistic fear. People with FM fall 6 x more than people without FM, and balance is challenged. • However, deconditioning will further your fall risk. • A new OHSU balance study will be enrolling shortly.
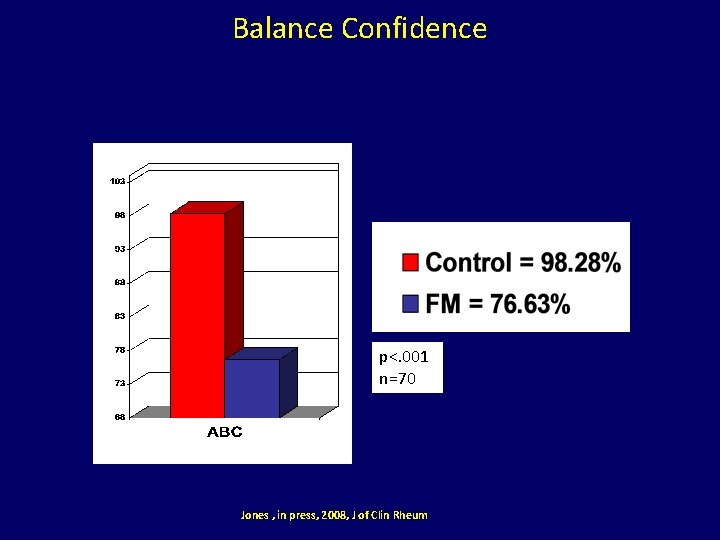
Balance Confidence p<. 001 n=70 Jones , in press, 2008, J of Clin Rheum

How to Minimize Your Risk of Falling During Exercise • Learn what ‘well balanced’ feels like. FM gives your body inaccurate information about the location of your center of gravity. • Exercise from a chair • Transition slowly between positions (for example, lift your neck up last, to minimize dizziness and reduce neck pain) • Avoid prolonged motionless standing • Avoid pivot turns • Stretch your heel cords • Gain muscle strength, especially in your hips and knees • Balance and strength DVD from myalgia. com

What is Your Current Activity Level? • Think of exercise like a medication. If the dose is too low, you will get little or no benefit. If it is too high, you’ll get side effects. • A guiding principle for both medication AND exercise: START LOW, GO SLOW • To determine your “activity level”, keep a diary for 24 hours. How much are you seated or in bed? How much are you standing or moving? • Try a 30 second chair stand test at home

What is Your Activity Dose is too High? • Use fatigue management techniques • Conserve energy in activities of daily living to save your energy for exercise (sit while showering or brushing your teeth, use timebased pacing, park near entrances) • Consider a hairstyle that doesn’t require a daily shower, or prolonged styling time with your arms lifted overhead) • Stretching and relaxation DVD from myalgia. com • Rest in neutral postures several times daily

Example of a Neutral Posture

Balancing Activity with Rest Time-Based Pacing Activity –> Rest –> Activity –> Rest Gil et al. In Chronic Pain (France et al. Eds). 1988. American Psychiatric Press

Is Your Activity Dose Too Low? Why? Do you need: • Access to better medications to control your symptoms? • Access to a bathroom during exercise due to irritable bowel or irritable bladder? • Access to an exercise class that is free from fragrance due to multiple chemical sensitivity or simply enhanced awareness of smells? • Access to an exercise program that understands your current limitation, despite how healthy you look? • In the past have you been more likely to exercise with a group, or individually? In the water, or on land? • Gentle aerobics DVD from myalgia. com

Exercisers In Research Classes at OHSU: Minimize Eccentric Work and Repetition

Is Your Weight Making it Difficult for you to Exercise? • FM symptom severity is not clearly correlated with baseline weight/BMI in multiple studies. • Still, symptoms do improve with weight loss • There is no single fibromyalgia diet yet • Look for a dietary intervention, designed for you individually, to help treat the following: obesity, celiac disease, IBS, constipation, GERD, and food allergies • Consider limiting unbound glutamate and food additives in your diet Kindler, Holmes & Jones, in press, 2008, NA Rheum Clinics

Living Foods / Raw Food Diet

Resources Books: • Yoga for Fibromyalgia: Move, Breathe, and Relax to Improve Your Quality of Life, Shoosh Lettick Crotzer, Rodmell Press Yoga Shorts, 2008 • Fibromyalgia: Simple Relief Through Movement, Stacie L. Bigelow, Wiley, 2000 • Fallproof: A Comprehensive Balance and Mobility Training Program, Debra J. Rose, Human Kinetics Publishers, 2003 • The Pain Survival Guide: How to Reclaim Your Life, Dennis C. Turk, APA Lifetools, 2005 • Healing Fibromyalgia, David H. Trock, Wiley, 2007 • The Complete Idiot’s Guide to Fibromyalgia, Lynne Matallana, Alpha, 2009 • The New Rules of Posture: How to Sit, Stand, and Move in the Modern World, Mary Bond, Healing Arts Press, 2007

More Resources Video/DVD: • Balance & Strength - www. myalgia. com • Stretching & Relaxation - www. myalgia. com • Gentle Aerobic Exercise - www. myalgia. com • Yoga Back Care Basics, Rodney Ye - www. amazon. com Web Resources: • A Fibromyalgia Patients Guide to Exercise - www. myalgia. com/exercise • Everyday Flexibility Moves - www. myalgia. com/exercise • Functional Fitness - www. myalgia. com/excercise • NFA - www. fmaware. org (type exercise in the search engine) • Fibromyalgia Network - www. fmnetnews. com/resources-daily-exercise • Pain Free Radio with host Pete Egoscue - http: //talkradio 1370 am. com/Pain-Free -Radio-with-Pete-Egoscue/298761

Ten Ways to Tame your Fibromyalgia Lindsay L. Kindler Clinical nurse specialist FIF

Self Care • Make “you” a priority • Schedule in time for yourself • Care for yourself as well as you others • Give yourself permission care for www. selfcareadvocacy. org

Creative Problem Solving • Modify daily activities • Make your environment work for you • Trade favors

Pace Your Activities • Alternate physically demanding activities with more restful activities • Break large jobs into smaller ones • Plan, be deliberate • Start where you are and keep progressing

Managing Your Sleep • Sleep schedule • Sleep environment • Pre-bedtime routine • Your own sleeping space www. dreamsoundtracks. com

Tame Your Stress • What helps you unwind? • Don’t “should” on yourself • Investigate your self talk www. thecomicshop. com • Practice saying “no”

Relaxation • • • Progressive muscle relaxation Guided imagery Meditation Passive disregard for thought Deep breathing www. thespiraltree. com

Pain Flares • Prevention of pain flares • Develop a flare plan • Share your flare plan with others www. research. unc. edu

Peripheral Pain Generators • Non-fibromyalgia sources of pain impact your fibromyalgia • Peripheral pain generators often respond to therapies that your FM does not respond to www. pioneerpandg. com

Manage Fibro Fog • Work on problems that can worsen fibro fog – – Sleep Pain Depression Stress • Use tools to maintain your sanity – One calendar for all activities – Elicit others to help Sketchedout. files. wordpress. com

How to Get Your Health Insurance Company to Do What You Need It To Do Rae Marie Gleason Executive Director National fibromyalgia Association

NFA & Patient Resources • Founded in 1997 by Lynne Matallana, a fibromyalgia patient Our Mission: To develop and execute programs dedicated to improving the quality of life for people with fibromyalgia.

NFA & Patient Resources • Resources: – Website: www. FMaware. org – FAME (Fibromyalgia Awareness Means Everything) Meetings – Fibromyalgia AWARE Magazine

NFA’s Access to Care Survey Early 2008 • NFA sent email requests for people with FM to share experiences with their health insurance providers • More than 1, 000 people responded most relating insurance complaints

National Association of Insurance Commissioners Top 5 reasons why consumers filed formal complaints against their insurance carriers in 2007: 1. Delay in claims handling 2. Denials of claims 3. Unsatisfactory settlement offers 4. Policy cancellation 5. Premium/insurance rates escalation

“More often than not, claims are deemed unjustified” In 2007 of 4, 915 complaints made in Texas, 78% were denied because actions of the insurance provider were found to be within the provisions of the health plan.

What Can Patients Do? • Realize there is a partnership between you and your insurance carrier • Take responsibility for your health care and communication between you and your carrier • Know your rights and what resources are available to help you navigate the insurance maze

Groundwork for a Successful Relationship 1. Understanding the Plan 2. Know your Broker 3. Request an Advocate (or case manager) Before You Need One 4. Find a Medical Mentor/Trusted Advisor 5. Seek out Financial Counseling

1. Understand the Plan • Choice of provider • Out-of-pocket costs • Paperwork you need to complete to ensure bills are paid • Your responsibility to understand policy limitations

1. Understand the Plan • Whether the plan makes exceptions that you can take advantage of • It is your responsibility to keep up on any changes in your policy – Ex: through the plans website, email/hardcopy communications received from your carrier)

2. Know your Broker • Most employer or group plans have a broker available to answer questions • Establish a relationship before your need him or her • When you need help, your name may stick out on a long list of messages to respond to • Can use to find out if your plan has a preapproved list of services for conditions like FM

3. Request an Advocate (or case manager) Before You Need One • Find out your plan’s criteria – some allow advocate coverage for chronic conditions • Advocates act as conduits between the plan and patient • Can help to facilitate payments for complex or unique cases

4. Find a Medical Mentor/Trusted Advisor • Could be a friend, relative or clinician • To help decipher insurance bills, accompany you to doctor visits, help make decisions about your care • When you live with a chronic pain condition, it is difficult to make good decisions • Can make the difference between good care and the best care possible

5. Seek out Financial Counseling • You have a legal right to financial counseling from any healthcare organization where you may receive care – Under Health Insurance Portability and Accountability Act (HIPPA) • Contact finance or patient accounting department of any hospital (or manager of your physician’s office)

5. Seek out Financial Counseling • They are not responsible by law to provide you care without payment • They are responsible by law to provide you with options for payment of your bill

After Your Provider Recommends Treatment 1. 2. 3. 4. 5. 6. Validate your care plan, especially for chronic conditions like fibromyalgia Run any physician treatment plan by your broker for approval prior to initiation Get it in writing! Communicate any special requirements to your advocate Make sure your provider has current insurance information Always request a copy of your records

1. Validate your care plan - especially for chronic conditions like fibromyalgia • Get at least one 2 nd opinion to help with questions about extent or type of treatment recommended • Discussion with your PCP about 2 nd opinion should be positive and help strengthen that important relationship

2. Run any physician treatment plan by your broker for approval prior to initiation

3. Get it in writing! • Get signed agreement to treatment regimen in writing from the plan representative • If that fails, then your medical mentor or broker can use the plan’s written policies to identify provisions to support payment for services

4. Communicate any special requirements to your advocate • Care you need that can only be provided by non-covered hospital or physician • Any special needs you have should qualify you for an advocate • Make certain advocate (or medical mentor) is assigned to your case

5. Make sure your provider has current insurance information • Forgetting to notify your HCP about any changes in your plan can result in denial of bills or major delays in payment • You are ultimately responsible for notification of changes • Inform your HCP office immediately regarding any changes • In addition to conversation by phone or in person – email or mail the information to help you maintain a written record of the information

6. Always request a copy of your records • If your insurance company is contemplating denial of coverage and is having a difficult time securing your records from your HCP, … having a copy of your information will show you received the services which will help your advocate dispute the denial more easily.

If Your Insurance Plan Isn’t Living Up To Its Obligation 1. 2. 3. 4. 5. 6. Turn to your broker - first line of defense Use your plan relationship - might be someone besides broker If you receive a request from your plan, respond to it ASAP Examine Explanation of Benefits Statement (EOBs) File an appeal and/or complaint - broker and/or advocate can assist you Involve non-profit resource organizations

1. Turn to your broker – first line of defense

2. Use your plan relationship – might be someone besides broker

3. If you receive a request from your plan respond to it ASAP • Might be used to stall process by plan • Regardless of legitimacy of request – plan representative will not proceed until you respond to request

4. Examine Explanation of Benefits Statement *** By law you must receive an EOB whenever bill is rejected. It will include: – – – – Provider name, date of service, service provided Provider’s charge for service Copayment, amount payable after deductibles Explanation of denial Telephone number and address where you may obtain clarification Information on how to file an appeal of a denial If any information is inaccurate, report it to the company & physician

5. File an appeal and/or complaint – broker and/or advocate can assist you • Your company has a process for filing complaints internally • You can follow the appeal process outlined in your EOB • Can simultaneously file complaint with your state’s department of health insurance – either general or specific that provides detail of your denial • Can consistently speak to or email to ensure followthrough

5. File an appeal and/or complaint – broker and/or advocate can assist you • Most states have hotlines manned by state employees who are there to help you • Identify one individual that you can consistently speak to or email to ensure follow-through

6. Involve non-profit resource organizations • Patient Advocacy Foundation – dedicated to “safeguarding patients through effective medication, assuring access to care, maintenance of employment and preservation of their financial stability relative to their diagnosis of life-threatening OR debilitating diseases

6. Involve non-profit resource organizations • Offers some free access to case managers and web-based helpline • Last resort – contact patient advocate firms who charge a fee to represent you, but are usually successful. Many work out settlements with insurance companies that minimizes or eliminates any additional costs to the patient

. . . TO SUM UP! • Be Proactive! If you don’t have the energy, rely on your team made up of your PCP, patient advocate and medical mentor to help you. Keep good records and build relationships in the plan with your broker and healthcare team. Use your pro-activity and organizational skills to hold others accountable.

Thank you

Thank you for supporting our research efforts www. myalgia. com
- Slides: 107