Fibromyalgia an evolving concept Robert M Bennett MD

Fibromyalgia an evolving concept Robert M. Bennett, MD, FACP, FRCP, MACR Professor of Medicine and Nursing Oregon Health & Science University

3 O years ago: West J Med 134: 405‑ 413, May 1981 “Fibrositis is a misnomer for a very common form of non-articular rheumatism. The name implies an inflammatory process in fibroconnective tissue which has never been
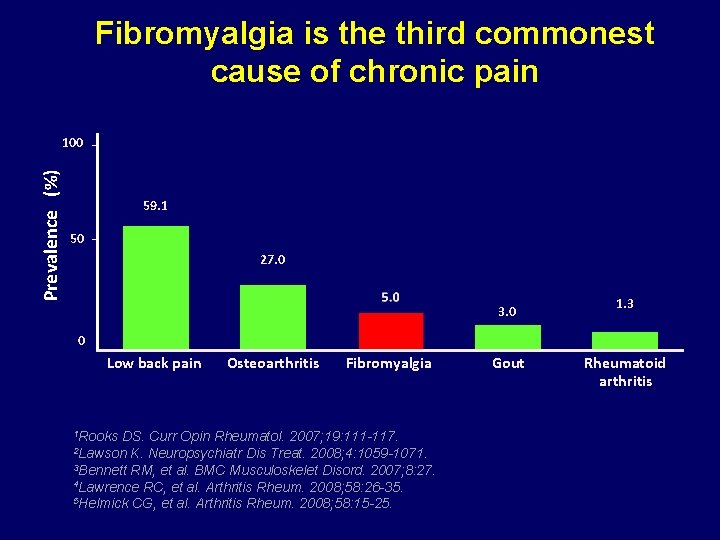
Fibromyalgia is the third commonest cause of chronic pain Prevalence (%) 100 59. 1 50 27. 0 3. 0 1. 3 0 Low back pain 1 Rooks Osteoarthritis Fibromyalgia DS. Curr Opin Rheumatol. 2007; 19: 111 -117. K. Neuropsychiatr Dis Treat. 2008; 4: 1059 -1071. 3 Bennett RM, et al. BMC Musculoskelet Disord. 2007; 8: 27. 4 Lawrence RC, et al. Arthritis Rheum. 2008; 58: 26 -35. 5 Helmick CG, et al. Arthritis Rheum. 2008; 58: 15 -25. 2 Lawson Gout Rheumatoid arthritis

30 years ago the cause of fibromyalgia was a puzzle Thought to be mainly a disease of muscles
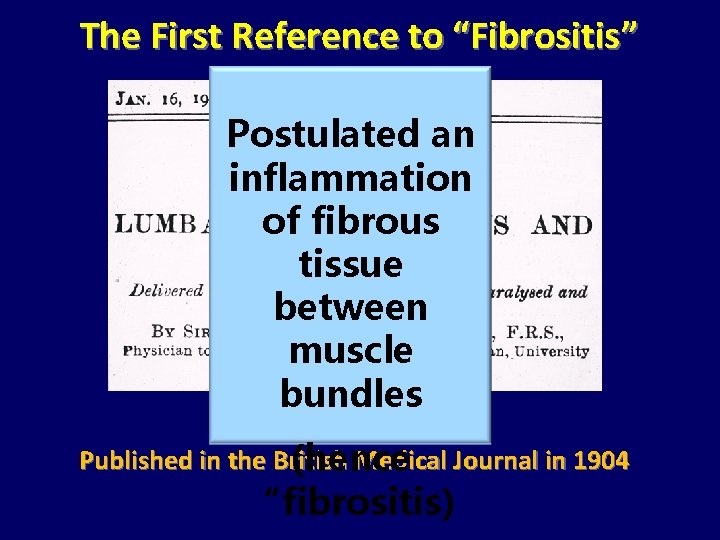
The First Reference to “Fibrositis” Postulated an inflammation of fibrous tissue between muscle bundles Published in the British Medical Journal in 1904 (hence “fibrositis)
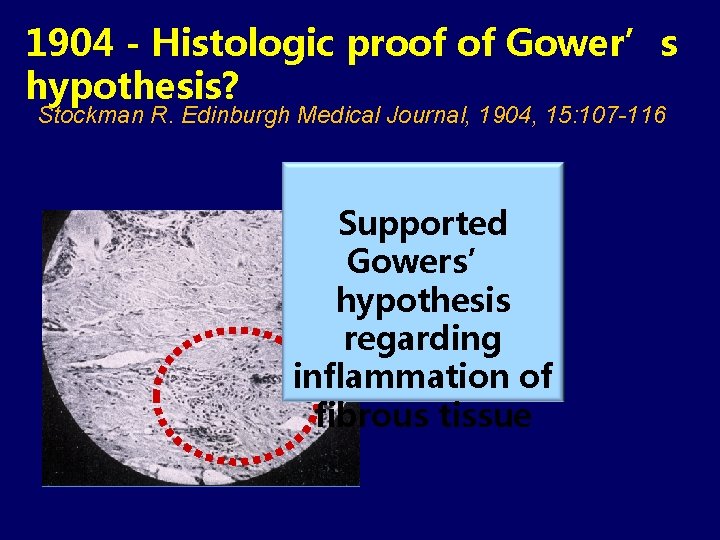
1904 - Histologic proof of Gower’s hypothesis? Stockman R. Edinburgh Medical Journal, 1904, 15: 107 -116 Supported Gowers’ hypothesis regarding inflammation of fibrous tissue

1915 - The first textbook on fibrositis All unexplained symptoms Llewellyn were attributed to “fibrositis” and Jones of Bath (i. e. a wastebasket diagnosis)
Understanding FM 1900 – 1930 s A disorder of Nerve painful muscles impulses Peripher al tissues
1904 - Histologic proof of Gower’s hypothesis? Stockman R. Edinburgh Medical Journal, 1904, 15: 107 -116 Stockman’s muscle histology could never be duplicated

“Psychogenic Rheumatism” FM was considered to be a result of psychoneurosi s Boland, Annals of the Rheumatic Diseases 1947; 6: 195 -203
“It’s all in your head” “Unexplained symptoms” are often still viewed as psychogenic in origin: Somatization Hypochondriasis Masked depression etc.

First “Scientific” Study in FM Moldofsky et al. Psychosomatic Med. 37: 341 -351, 1975
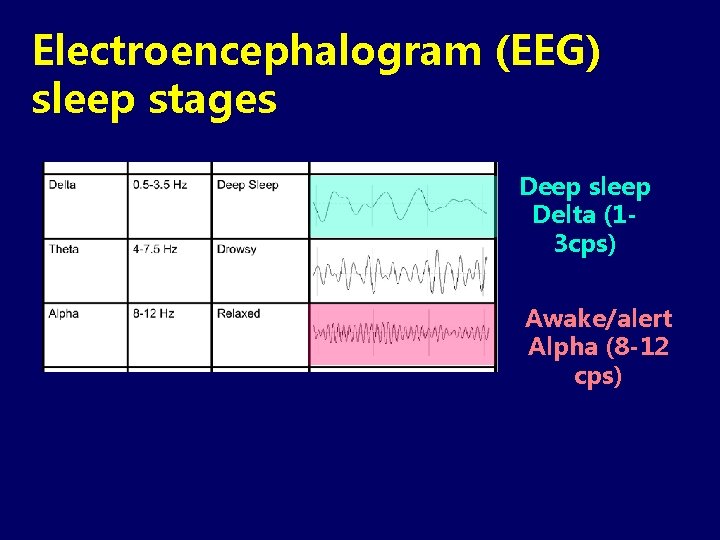
Electroencephalogram (EEG) sleep stages Deep sleep Delta (13 cps) Awake/alert Alpha (8 -12 cps)
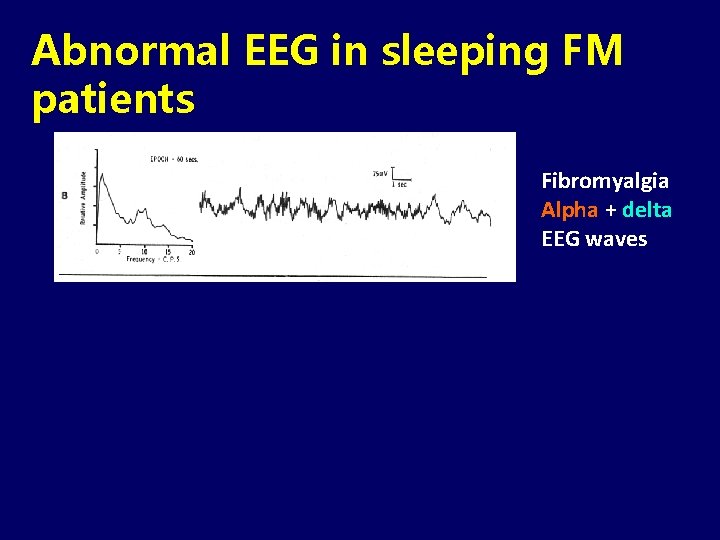
Abnormal EEG in sleeping FM patients Fibromyalgia Alpha + delta EEG waves Sleep disruption in healthy subjects caused pain and fatigue

1981 - First study comparing fibromyalgia patients to healthy individuals Yunus et al. Seminars Arthritis and Rheumatism 1981, 11: 151 -171

FM patients often have: Irritable bowel Irritable bladder Chronic fatigue Restless legs Dizziness “Fibro-fog” Cold intolerance Multiple sensitivities

1990 - The ACR Classification Criteria Arthritis Rheum. 1990; 33: 160 -172 In addition to American College of Rheumatology 1990 defining FM, of Fibromyalgia: Criteria for the Classification name was Report of thethe Multicenter Criteria Committee changed from “fibrositis” to F Wolfe, HA Smythe, MB Yunus, RM Bennett, C Bombardier, DL Goldenberg, P “fibromyalgia Tugwell, SM Campbell, M Abeles, and P Clark ”
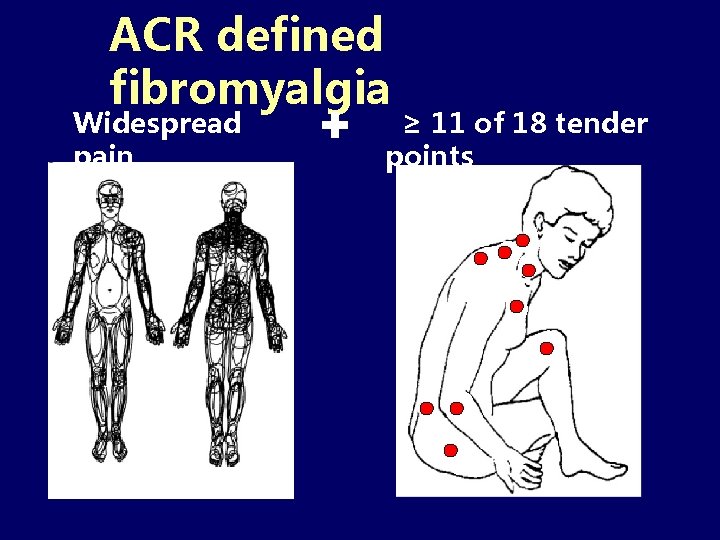
ACR defined fibromyalgia Widespread pain + ≥ 11 of 18 tender points
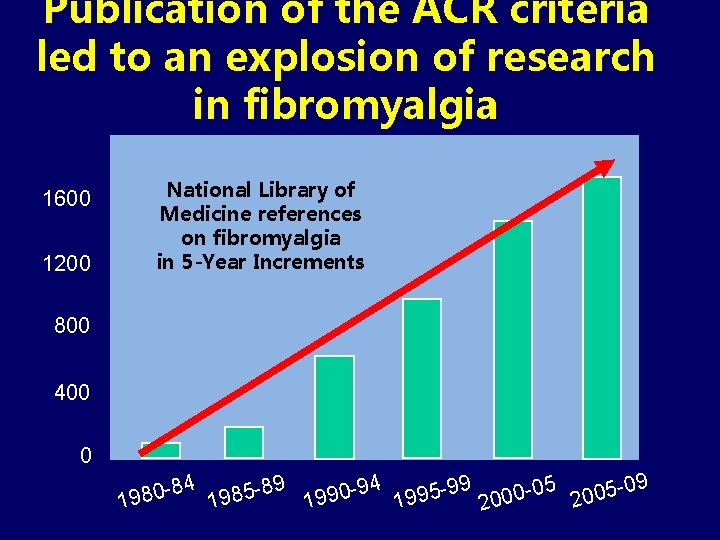
Publication of the ACR criteria led to an explosion of research in fibromyalgia 1600 1200 National Library of Medicine references on fibromyalgia in 5 -Year Increments 800 400 0 84 89 94 99 00 -05 005 -09 0 5 8 8 9 9 2 19 19 20
What has been found? Sensory impulses are amplified at level of spinal cord and brain in fibromyalgia patients “Central sensitization”
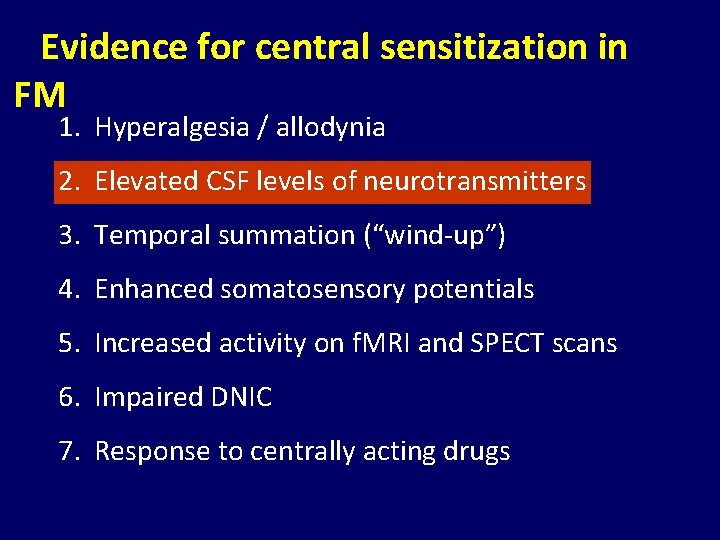
Evidence for central sensitization in FM 1. Hyperalgesia / allodynia 2. Elevated CSF levels of neurotransmitters 3. Temporal summation (“wind-up”) 4. Enhanced somatosensory potentials 5. Increased activity on f. MRI and SPECT scans 6. Impaired DNIC 7. Response to centrally acting drugs
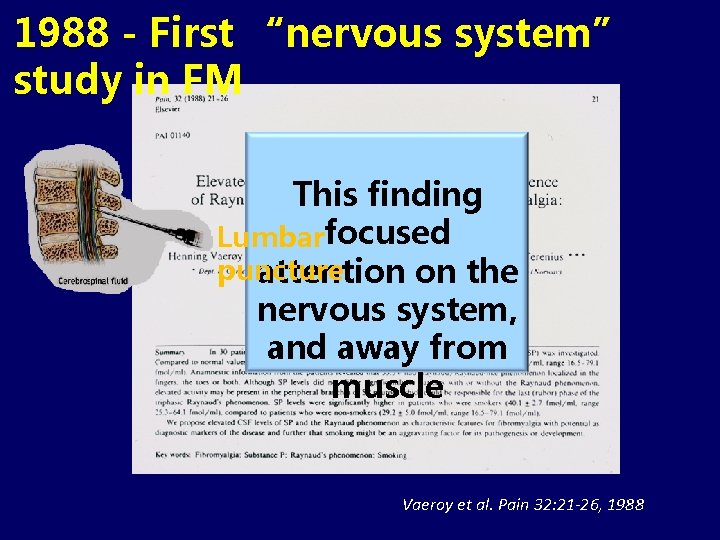
1988 - First “nervous system” study in FM Found that the This finding CSF of FM focused Lumbar puncture patientson had attention the elevatedsystem, levels nervous of substance P and away from muscle Vaeroy et al. Pain 32: 21 -26, 1988
Abnormal sensory processing in FM 1. Hyperalgesia / allodynia 2. Elevated CSF levels of neurotransmitters 3. Temporal summation 4. Enhanced somatosensory potentials 5. Increased activity on f. MRI scans 6. Impaired DNIC 7. Response to centrally acting drugs
Functional Brain Imaging SPECT MRS PET f MRI
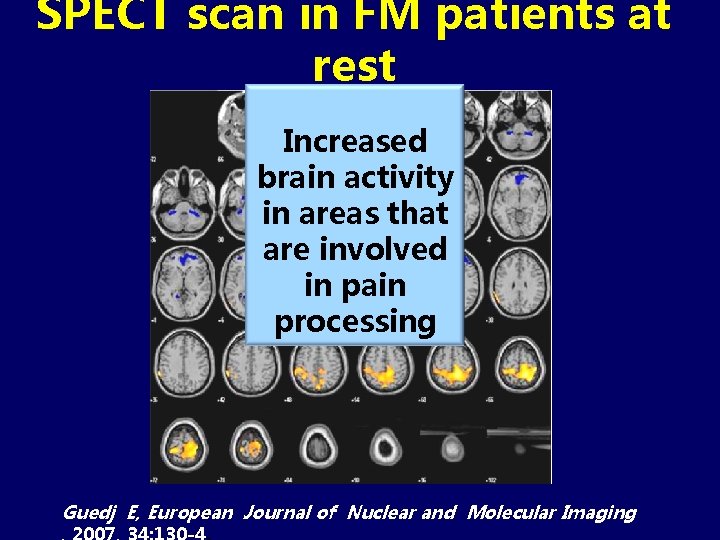
SPECT scan in FM patients at rest Increased brain activity in areas that are involved in pain processing Guedj E, European Journal of Nuclear and Molecular Imaging
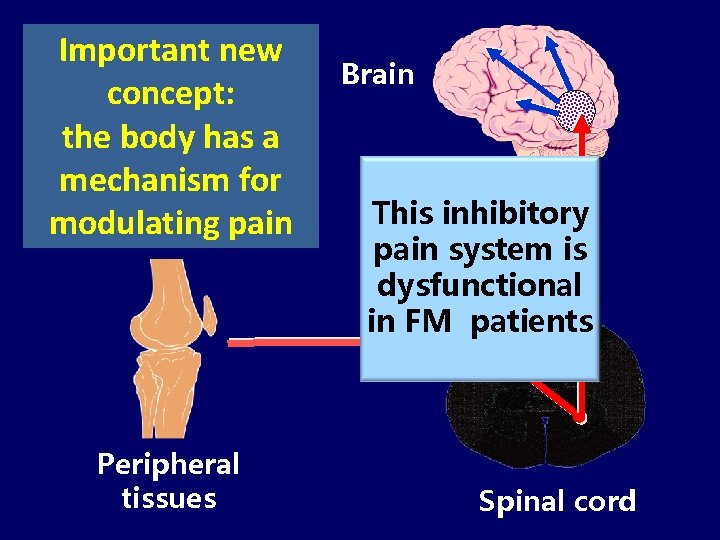
Important new concept: the body has a mechanism for modulating pain Brain Descendi This inhibitory ngsystem is pain inhibition dysfunctional in FM patients Peripheral tissues Spinal cord
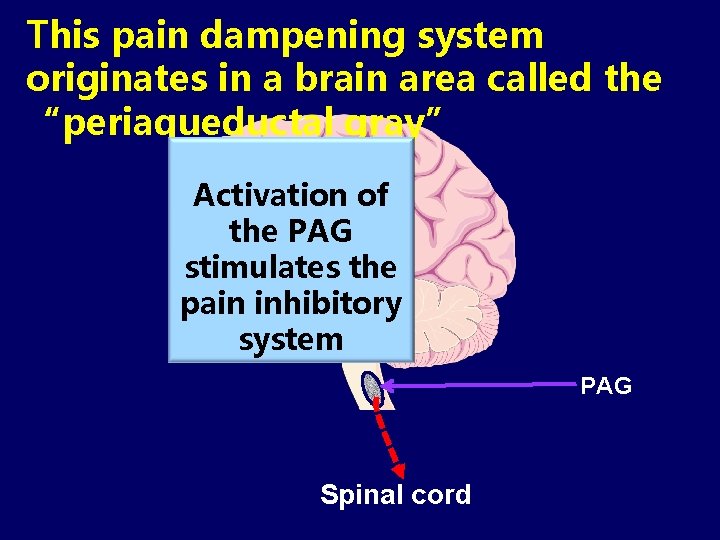
This pain dampening system originates in a brain area called the “periaqueductal gray” Activation of the PAG stimulates the pain inhibitory system PAG Spinal cord
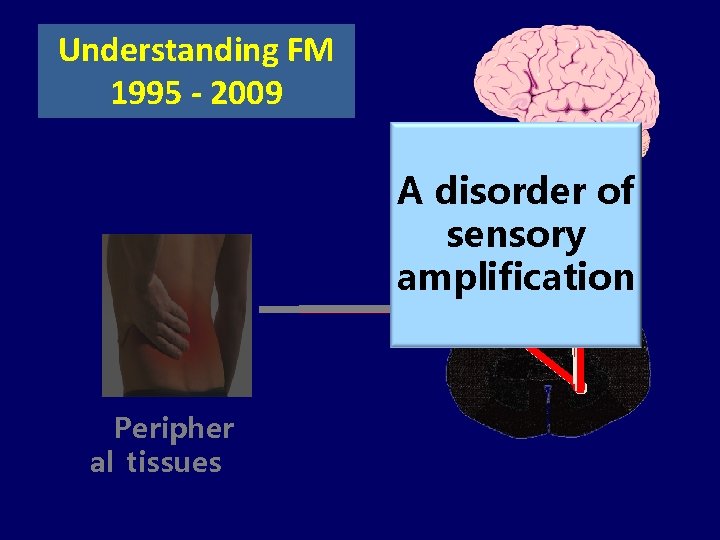
Understanding FM 1995 - 2009 A disorder of sensory amplification Peripher al tissues

2009 - What are “tender points” Found that FM tender points had the typical features of myofascial trigger points

What are myofascial trigger points? There are several hundred myofascial trigger point locations in the body

Understanding FM 2009 - present FM now thought to be a This latest disorder of both understanding of FM is peripheral pain crucial for planning generators effectiveand treatment strategies central sensitization Peripher al tissues

What causes fibromyalgia? Environmental insults Infections Trauma Prolonged stress PTSD Disordered sleep Alpha-delta sleep Sleep apnea Not just one gene but many Hereditary influences Genes (COMT, serotonin receptor) Epigenetics (changes in gene expression)

30 years ago the cause of fibromyalgia was a puzzle Thought to be mainly a disease of muscles

30 years later - some of the puzzle is now in place Pain s r o t a r gene Env nt ironm e G e n e s

Next speaker please

Fibromyalgia Information Foundation Spring Conference 2010 Welcome and orientation - Sharon Clark, Ph. D Fibromyalgia: An Evolving Concept - Robert M Bennett, MD Diagnosis and Mis-diagnosis - Atul Deodhar, MD Guided Stretch Break - Janice Holt Hoffman How Can I Help Myself? - Kim Dupree Jones, Ph. D How Can Medications Help Me? - Robert M Bennett, MD Roundtable: Questions and Answers - Drs Bennett, Deodhar and Jones, moderated by Dr Sharon Clark

Diagnosis and Misdiagnosis Atul Deodhar MD, FACR, MRCP Associate Professor of Medicine Medical Director, Rheumatology Clinics Oregon Health & Science University

Why do you need a specialist? • To make the correct diagnosis • To ‘rule out’ other causes of generalized pain • To ‘rule in’ common problems that go hand-inhand with fibromyalgia (sleep apnea, restless legs, irritable bowel, depression etc) • Fibromyalgia can co-exist with other rheumatic conditions and they shouldn’t be missed either • To develop a comprehensive treatment plan

How do I make the diagnosis of FM? • History & Physical Examination is usually enough to make the diagnosis of fibromyalgia • Blood tests & other investigations rule out other causes of generalized pain which may have different and effective treatments • It is not “since they could not find anything else on blood tests, they told me I have FM”

How do I make the diagnosis of FM? • FM patients usually have – Generalized Pain – Tenderness all over – Fatigue – Sleep disturbance – Depression/anxiety – Cognitive dysfunction – Irritable Bowel Syndrome • FM patients usually do not have – Weight loss – Joint swelling as seen in rheumatoid arthritis – Major organ (kidney, heart, lungs, brain) dysfunction – Abnormal lab tests

FM Symptoms Source: National Fibromyalgia Association Survey

Do I have ‘Lupus’? • Autoimmune disease affecting multiple organs in a specific fashion – generalized tenderness but nothing else on examination is not lupus! • Over-diagnosed with positive anti- Do I have ‘MS’? • Autoimmune disease that presents with specific neurological deficits – true weakness, sensation loss, visual loss etc. • Generalized tenderness but

“My MRI scan showed Arthritis” • MRI scans are extremely sensitive and show all sorts of ‘abnormalities’ which may or may not have any clinical relevance • Everyone in this room has ‘spurs’, bulging discs, degenerative discs, and “arthritis” in the spine but not everyone has chronic back pain • There is no direct correlation between what you find on the MRI scan and the ‘generalized pain and tenderness’ as seen in FM

Take Home Message • After the age of 30, completely normal MRI scan of the spine is as rare as hen’s teeth • There is poor correlation between ‘arthritis’ changes as seen on the MRI scan and patient’s symptoms

Other common causes of generalized pain • Chronic hepatitis C • Hypothyroidism, Hyperparathyroidism • Metastatic cancer, Multiple myeloma • Vitamin D Deficiency • Polymyalgia rheumatica • OA, RA, Sjögren’s syndrome, SLE
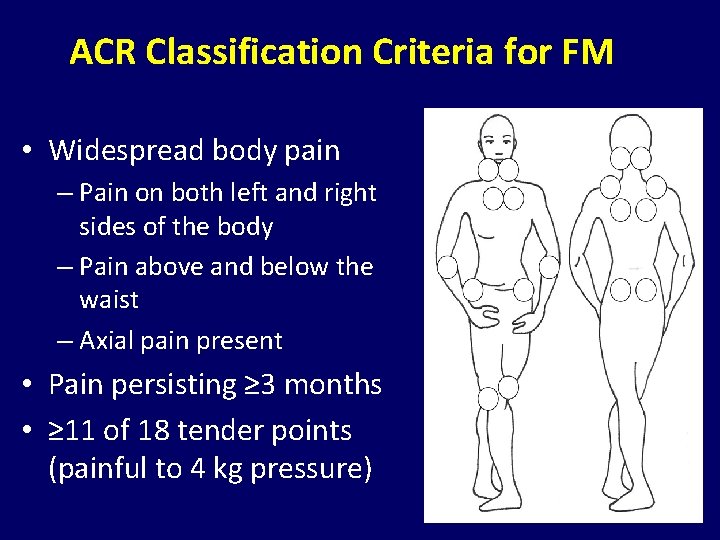
ACR Classification Criteria for FM • Widespread body pain – Pain on both left and right sides of the body – Pain above and below the waist – Axial pain present • Pain persisting ≥ 3 months • ≥ 11 of 18 tender points (painful to 4 kg pressure)

New ACR ‘Diagnostic Criteria’ for Fibromyalgia Symptom Severity Scale (0 -3) Widespread Pain Index • Cognitive symptoms • Shoulder girdle, L & R Waking Un-refreshed Upper arm L & R Fatigue Lower arm L & R 0 to 9 Hip buttock/trochanter L R Upper leg L & R Does Pt have somatic Lower leg L & R symptoms? Jaw L & R • No symptoms 0 to 3 Chest Few symptoms Abdomen 0 to 19 Moderate number Upper back Great deal of symptoms Lower back Neck Wolfe F. et al. Arthritis care & Research 2010; 62(5): 6

New ACR ‘Diagnostic Criteria’ for Fibromyalgia Patient can be Diagnosed as FM if they have: 1. Widespread pain index (WPI) 7 & symptom severity (SS) scale score 5 or WPI 3– 6 and SS scale score 9 2. Symptoms have been present at a similar level for at least 3 months 3. The patient does not have a disorder that would otherwise explain the pain Wolfe F. et al. Arthritis care & Research 2010; 62(5): 60

Take Home Message • Your doctor doesn’t have to ‘rule out’ other diseases to diagnose fibromyalgia • Fibromyalgia can co-exist with other diseases such as lupus, rheumatoid arthritis etc. • Be Aware: Once the diagnosis is made, there is a risk of blaming all symptoms on fibromyalgia

What else do I look for every time I see a patient with Fibromyalgia? • Sleep disturbance: – Sleep Apnea Syndrome – Restless Leg Syndrome • • Depression/Anxiety/Stress Functional status, de-conditioning Irritable Bowel Syndrome I also look for signs & symptoms that do not fit

Case Report • Helen H. is a frustrated 50 year old CEO of a small company who has been treated for fibromyalgia for the past 8 months. • “I just hate going to see the doctor. I’m there for fibromyalgia and instead of focusing on my pain complaints, he makes me answer questions and fill out questionnaires asking about my mood, sleep, bowel habits, and headaches. Why doesn’t he just ask about my fibromyalgia? ”

Was Helen’s doctor justified? • FM evaluation includes assessment of pain and other conditions that occur frequently with FM • Understanding the full symptom complex & its impact allows the doctor to develop an effective treatment plan • Improvement may initially occur with non-pain symptoms e. g. sleep, mood etc • Not utilizing non-pain conditions may result in missing the early treatment success & abandoning treatments that might eventually improve both pain & non-pain symptoms

Summary Ø In expert hands, FM diagnosis is straight forward, and is based on history & examination Ø Blood tests are not required to make the diagnosis, but they help rule out additional conditions with specific therapies Ø Several other conditions can go hand-in-hand with FM, e. g. sleep, mood, bowel disturbances Ø Be aware: New symptoms may or may not be related to FM: Don’t hesitate to ask


20 minute break and stretching with Janice Hoffmam

Fibromyalgia Information Foundation Spring Conference 2010 Welcome and orientation - Sharon Clark, Ph. D Fibromyalgia: An Evolving Concept - Robert M Bennett, MD Diagnosis and Misdiagnosis - Atul Deodhar, MD Guided Stretch Break - Janice Holt Hoffman How Can I Help Myself? - Kim Dupree Jones, Ph. D How Can Medications Help Me? - Robert M Bennett, MD Roundtable: Questions and Answers - Drs Bennett, Deodhar and Jones, moderated by Dr Sharon Clark

What Can I do for Myself? Kim Dupree Jones Ph. D, FNP-BC Associate Professor School of Nursing Oregon Health & Science University

1. Please select the most appropriate option • Medications and surgery are the only effective treatments that help fibromyalgia? 1. True 2. False

2. Please select the most appropriate option • The combination of medications, cognitive behavioral strategies, education, exercise, diet and physical therapy may be used to fully treat fibromyalgia. 1. True 2. False

Take Home Message To maximize benefit, treatments should match specific problems or symptoms. One size does not fit all

One Size Fits All Myth Ignoring individual differences Treating everyone the same Inconsistent results Providers may have little understanding of which treatments are worth your time

Non-pharmacological treatments for FM Delta wave sleep interruption. Meditation Muscle vibration Diet Neck support ECT Omega-3 fatty acid Education Operant conditioning EEG-driven stimulation Peripheral Electroacupuncture neurostimulation Electromagnetic shielding fabric Pool exercise + education Feldenkrais Psychomotor therapy Flexibility exercise Qigong + mindful Guided imagery meditation Homeopathic vellum Relaxation Hot packs Stress management Hydrogalvanic therapy Stretching exercise Hyperbaric oxygen Sulphur mud baths Hypnotherapy Tender point injections Laser therapy TENS Light therapy Transcranial direct Magnetized mattress current stimulation Manipulation + ultrasound Valerian bath Marital counseling Warm water exercise Massage Written emotional expression CBT, cognitive behavioral therapy; ECT, electroconvulsive therapy; EEG, electroencephalogram; TENS, transcutaneous 024 essential oil Acupuncture Aquatic exercise (deep water running) Aerobic exercise Aloe vera Amitriptyline + Stanger bath Anthocyanidins Autogenic training Balneotherapy Biofeedback Bioresonance therapy CBT Chlorella Connective tissue manipulation + ultrasound Cryotherapy (whole body) Dance/movement therapy 56 published studies electrical nerve stimulation.

Exercise Top 10 Principles: 1. Treat peripheral pain generators to minimize central sensitization 2. Minimize eccentric muscle work 3. Choose low-intensity non-repetitive exercise 4. Recognize the importance of restorative sleep 5. Address obesity and deconditioning 6. Create fibromyalgia-friendly exercise environment 7. Be aware of balance/dizziness problems 8. Conserve energy in daily life 9. Reverse pain postures (stretch anterior chest/strengthen back) 10. Start low and go slow Jones KD & Lipton G. Exercise interventions in fibromyalgia: Clinical applications from the evidence. Rheumatic Disease Clinics of North America. 2009; 35 (2), 373 -391. www. myagia. com

What are Cognitive Behavioral Strategies? Ø Understanding Treatment Options/Self. Advocacy Ø Time-based Pacing Ø Fatigue Control Ø Realistic Expectation/Boundary Setting Ø Pleasant Activity Scheduling Ø Decreasing Catastrophic Thinking & Distraction Hassett, AL & Gevirtz (2009) Nonpharmacologic treatment for fibromyalgia: patient education, cognitive-behavioral therapy, relaxation techniques and complementary and alternative medicine. Rheumatic Disease Clinics of North America. 35 (2), 393 -407.

Self-Management: Sleep Example Lifestyle Environment -Regular bed time/wake time - Steady room temperature - Get in bed when sleepy -Keep room dark -Silicone ear plugs -Use bed for sleep -No TV or computer -Ride the wave of pain -No guilt inducing exercise equipment -Caffeine in am only -No bills/mail (remember meds) -Private room (no pets/spouses…) Thermal Tips - Lower core temp signals sleep - Exercise, warm bath before bed -Socks, moisture wicking PJs Jones, K. D. , Kindler, L. L. & Lipton, G. (in press). Self-management strategies in fibromyalgia. Journal of Clinical Outcomes Management.

Diet Holton, K. F. , Kindler, L. L. & Jones, K. D. , & (2009). Potential dietary links for central sensitization in fibromyalgia: past reports, future directions. Rheumatic Disease Clinics of North America. 35 (2), 409 -420.

Eat More Fresh Food- Less Processed Foods • Some food additives contribute to FM: MSG, aspartame and l-cystine: – most canned soups & stocks – most flavored potato chip products (tortilla chips v Doritos) – many other snack or processed foods including protein shakes – many frozen dinners including diet foods and diet drinks – almost all US-originated fast foods, salad dressings, marinades – boxed including a seasoning packet in fibromyalgia: past Kindler, L. L. , Jones, K. D. , &meals Holton, K. (2009). Potential dietary links for central sensitization reports, future directions. Rheumatic Disease Clinics of North America. 35 (2), 409 -420. – Hydrolyzed protein, “natural flavors/spices” on food

Education & Self-Help EDUCATION / EXERCISE REST “Understanding Fitness How “The End of Stress as We Know Exercise Fuels Health and Fights It” Disease” by Bruce Mc. Ewen by Kim Jones “Full-Body Flexibility For Optimal Mobility and Strength” by Jay Blahnik “Does Stress Damage the Brain? ” by Douglas Bremner “The Relaxation and Stress Reduction Workbook” “Fall Proof! A Comprehensive by Martha Davis Balance & Mobility Training Program” “Managing Chronic Pain: A CBT by Debra J Rose Approach” by John Otis “The 10 Best Questions for Living with Fibromyalgia” by Dede Bonner “ 30 Scripts for Relaxation Imagery & Inner Healing” by Julie T Lusk

Your experiences shared

Find Your New Baseline Individual differences requires individualized treatment: • Adequate therapy of symptoms – Pain – Sleep. Fibromyalgia disturbancesis something – Depression/anxiety that you have, not who you are • Education – Accessible explanation of pathophysiology • Identifying and addressing your unique perpetuating factors • Setting realistic objectives- Try one Van Houdenhove, Luyten. Psychosomatics. 2008; 49(6): 470 -477.

Next speaker please

How can medications help me? Robert M. Bennett, MD, FACP, FRCP, MACR Professor of Medicine and Nursing at OHSU

HEALTH JOURNAL / By LEILA ABBOUD Staff Reporter of THE WALL STREET JOURNAL August 3, 2004 Off-Label Treatments, New Drugs Target Mysterious, Debilitating Fibromyalgia Drug companies are racing to develop drugs for a highly debilitating disease that has confounded doctors and plagued patients for years. The disorder, called fibromyalgia, causes people to feel chronic pain all over their bodies and suffer from a constellation of symptoms, including sleep disturbances, fatigue and headaches. An estimated four to six million Americans have fibromyalgia. Women are seven times as likely as men to develop it. Despite the large number of people afflicted, because of the mysterious nature of the disease, there is currently no drug approved specifically to treat it.

Now there are 3 drugs that are FDA approved for the treatment of fibromyalgia

FDA Approved Medications for Fibromyalgia Pregabalin (Lyrica) • Anticonvulsant Duloxetine (Cymbalta) • Antidepressant • Balanced SNRI Milnacipran (Savella) • Antidepressant • Balanced SNRI FDA-approved for fibromyalgia pain at 300 -450 mg/day in divided doses BID: –Start at low dose and increase as needed –Adjunctive therapy of partial epilepsy, neuropathic pain FDA-approved for treatment of fibromyalgia pain at 60 mg/day: –Start with lower dose and increase as recommended –Other indications: major depressive disorder, generalized anxiety disorder, diabetic peripheral neuropathic pain FDA-approved for fibromyalgia management at 100 -200 mg/day in divided doses BID: –Starting dose: 12. 5 mg; recommended increase to 100 mg/day Crofford LJ. Curr Opin Rheumatol. 2008; 20: 246 -250. Arnold LM, et al. Arthritis Rheum. 2004; 50: 2974 -2984. Arnold LM, et al. Pain. 2005; 119: 5 -15.

What does FDA approval mean? Ø The drug has been thoroughly tested and is better than a placebo Ø The adverse events are not generally very severe Ø However, with wider use important adverse events may lead to its being withdrawn from the market Ø As a generalization, the currently approved drugs for FM give about 30% relief of pain to about 30% of patients Ø Approved medications are seldom tested against each other
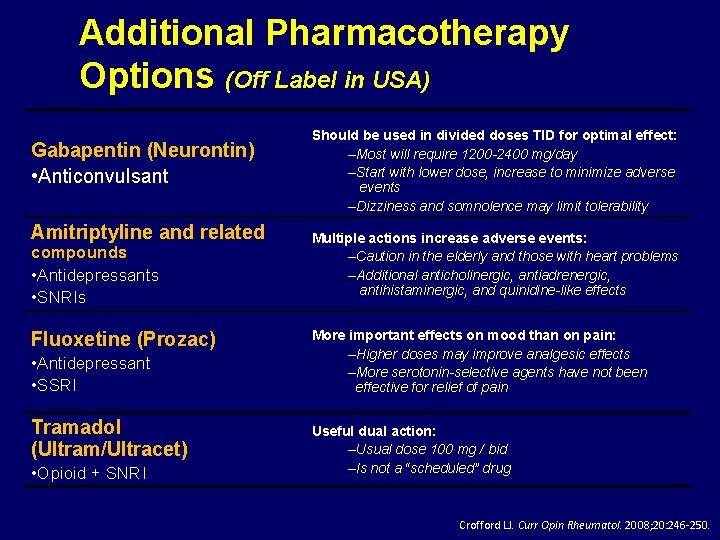
Additional Pharmacotherapy Options (Off Label in USA) Gabapentin (Neurontin) • Anticonvulsant Amitriptyline and related compounds • Antidepressants • SNRIs Fluoxetine (Prozac) • Antidepressant • SSRI Tramadol (Ultram/Ultracet) • Opioid + SNRI Should be used in divided doses TID for optimal effect: –Most will require 1200 -2400 mg/day –Start with lower dose, increase to minimize adverse events –Dizziness and somnolence may limit tolerability Multiple actions increase adverse events: –Caution in the elderly and those with heart problems –Additional anticholinergic, antiadrenergic, antihistaminergic, and quinidine-like effects More important effects on mood than on pain: –Higher doses may improve analgesic effects –More serotonin-selective agents have not been effective for relief of pain Useful dual action: –Usual dose 100 mg / bid –Is not a “scheduled” drug Crofford LJ. Curr Opin Rheumatol. 2008; 20: 246 -250.

What treatments do FM patients really use?
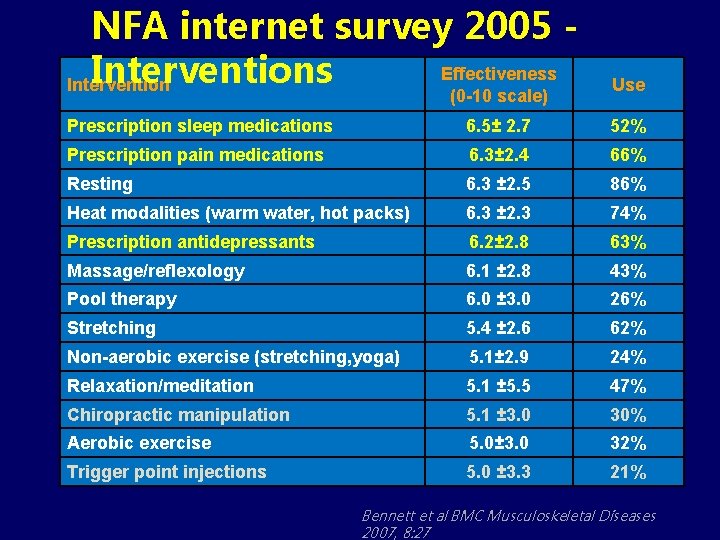
NFA internet survey 2005 Effectiveness Intervention Use Prescription sleep medications 6. 5± 2. 7 52% Prescription pain medications 6. 3± 2. 4 66% Resting 6. 3 ± 2. 5 86% Heat modalities (warm water, hot packs) 6. 3 ± 2. 3 74% Prescription antidepressants 6. 2± 2. 8 63% Massage/reflexology 6. 1 ± 2. 8 43% Pool therapy 6. 0 ± 3. 0 26% Stretching 5. 4 ± 2. 6 62% Non-aerobic exercise (stretching, yoga) 5. 1± 2. 9 24% Relaxation/meditation 5. 1 ± 5. 5 47% Chiropractic manipulation 5. 1 ± 3. 0 30% Aerobic exercise 5. 0± 3. 0 32% Trigger point injections 5. 0 ± 3. 3 21% (0 -10 scale) Bennett et al BMC Musculoskeletal Diseases 2007, 8: 27
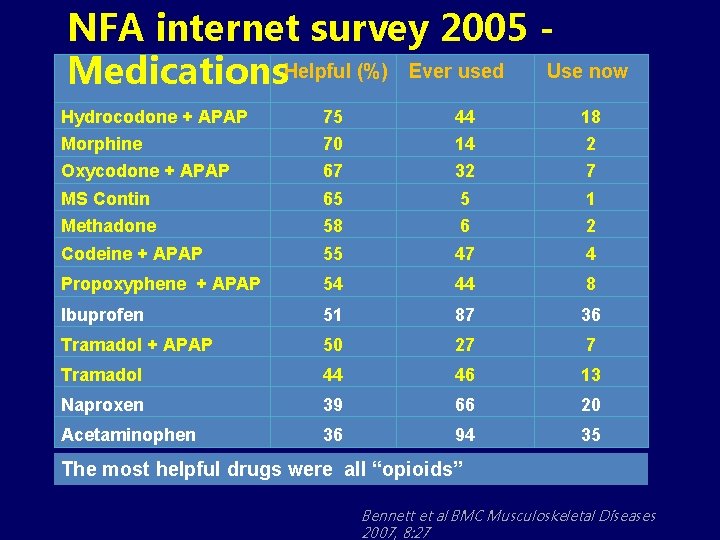
NFA internet survey 2005 Medications. Helpful (%) Ever used Use now Hydrocodone + APAP 75 44 18 Morphine 70 14 2 Oxycodone + APAP 67 32 7 MS Contin 65 5 1 Methadone 58 6 2 Codeine + APAP 55 47 4 Propoxyphene + APAP 54 44 8 Ibuprofen 51 87 36 Tramadol + APAP 50 27 7 Tramadol 44 46 13 Naproxen 39 66 20 Acetaminophen 36 94 35 The most helpful drugs were all “opioids” Bennett et al BMC Musculoskeletal Diseases 2007, 8: 27

Rational use of medications is dependent on understanding mechanisms of their action
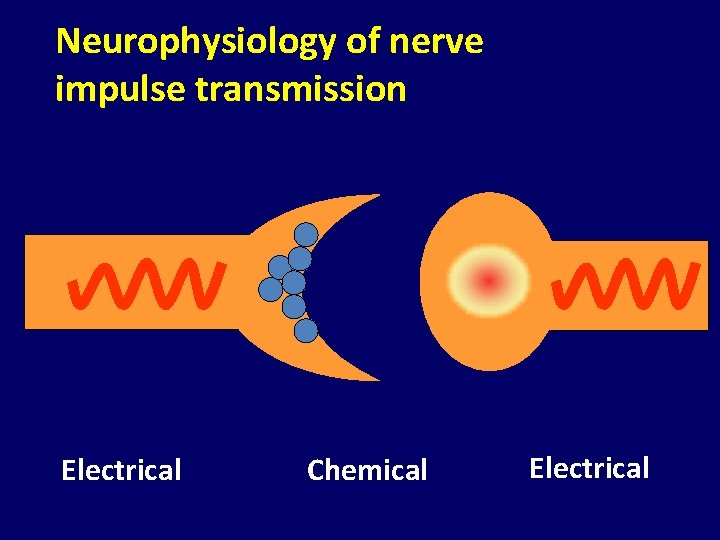
Neurophysiology of nerve impulse transmission Electrical Chemical Electrical

Modulation of Glutamate Release Inhibition of glutamate release Mechanism of action of anti-seizure medications Reduced output to brain
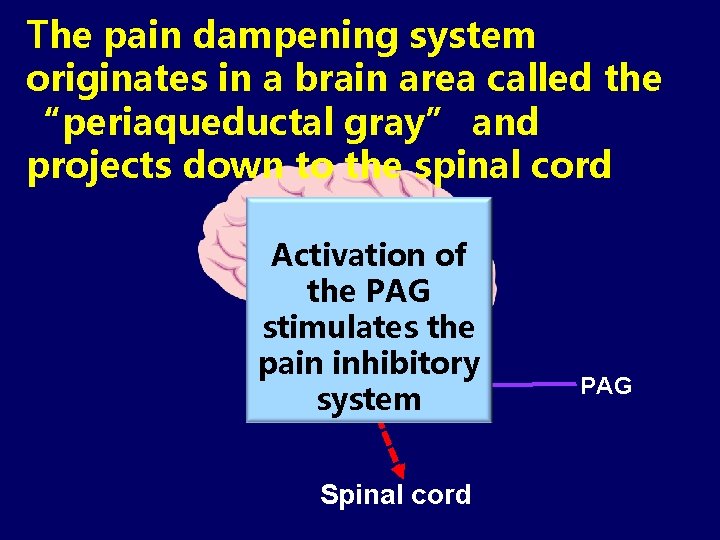
The pain dampening system originates in a brain area called the “periaqueductal gray” and projects down to the spinal cord Activation of the PAG stimulates the pain inhibitory system Spinal cord PAG
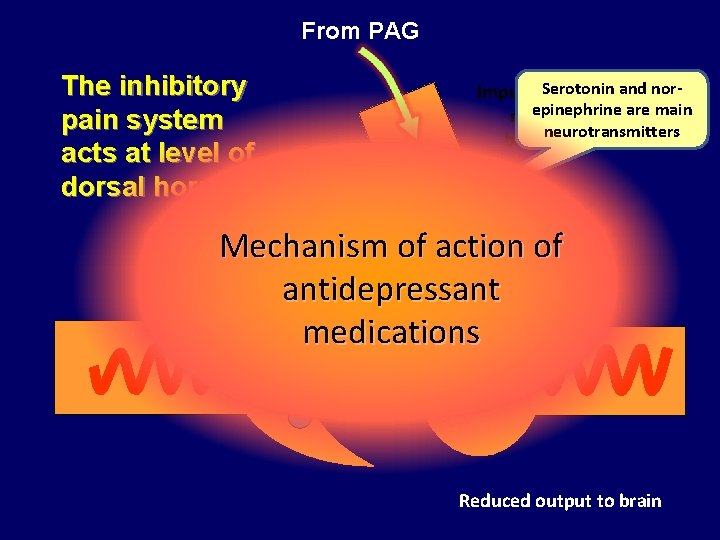
From PAG The inhibitory pain system acts at level of dorsal horn Impulses. Serotonin arise in and norepinephrine are main nuclei of neurotransmitters brainstem Mechanism of action of antidepressant medications Reduced output to brain

Sleep Disturbance Moldofsky et al. Psychosomatic Med. 37: 341 -351, 1975

Disturbed Sleep Chicken or Egg? Chronic Pain Disturbed sleep
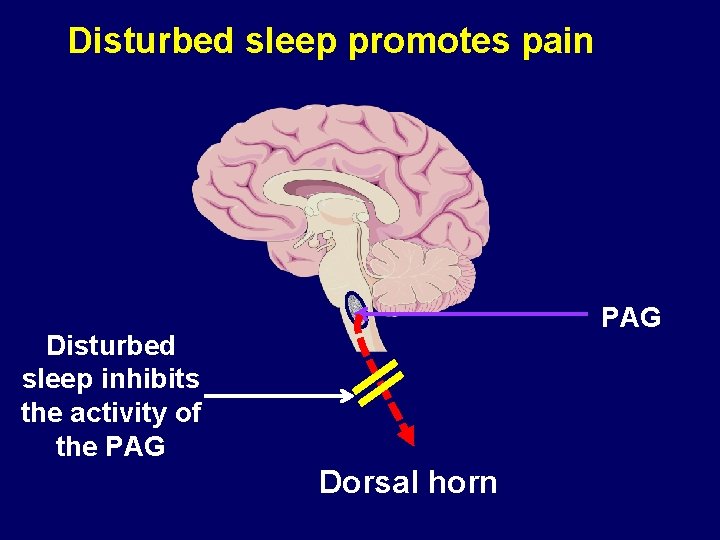
Disturbed sleep promotes pain PAG Disturbed sleep inhibits the activity of the PAG Dorsal horn

Treating disturbed sleep Ø Practice good sleep hygiene Ø Be evaluated for sleep disorders Ø Medications: § Amitryptyline (Elavil) § Cyclobenzaprine (Flexeril) § Zolpidem (Ambien) § Sodium oxybate (Xyrem)

Sodium oxybate (Xyrem) Currently under review by the FDA Improvements in sleep and fatigue Also improvemed pain, stiffness and FIQ

A basic reality Contemporary medications are of some help, but seldom reduce pain by more than 30%
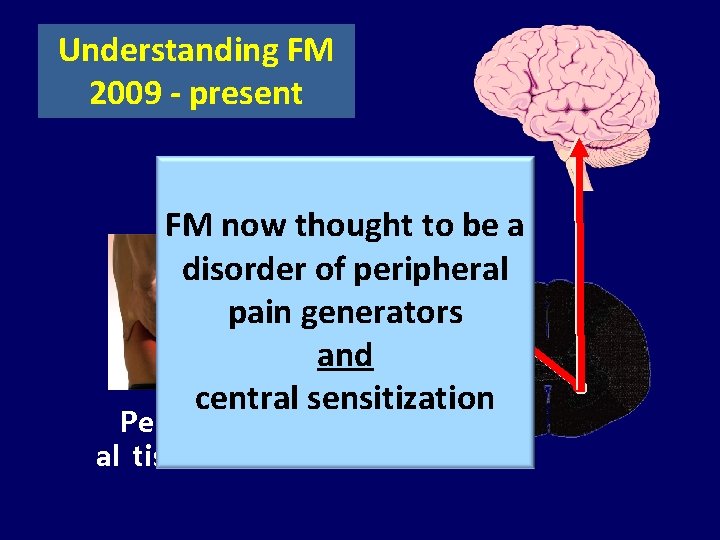
Understanding FM 2009 - present FM now thought to be a disorder of peripheral pain generators and central sensitization Peripher al tissues

Pain Generators • Osteoarthritis • Chronic headaches • Visceral pain • Myofascial pain The effective treatment • Inflammation • TMP of peripheral painsyndromes generators • is. Spinal an stenosis • Neuropathies essential component of • Injuries • Repetitive strain any fibromyalgia • Disc disorders Endometriosis treatment • plan

% of Patients Drug side effects (Duloxetine) † 45 40 35 30 25 20 15 10 5 0 † Placebo (N=120) Duloxetine 60 mg qd (N=118) Duloxetine 60 mg bid (N=116) ** † * Na e us a * * † * ** * s y e n ia is e th is s ea r c t s t x o u i e i i e h t t o g re en ro t rr e at l sn i n o d a J M p p o i u i y i n r p n h o t g y D A r a r s v A n m i r e h n D e p p el ed So y o N Co e s H F as ea N r c De Arnold LM et al. (2005), Pain 119(1 -3): 5 -15 *

Everything has side effects It must be all the herbal tea you are drinking

Too much serotonin N Engl J Med 2005; 352: 1112 -20. The serotonin syndrome is an adverse drug reaction that results from therapeutic drug use or inadvertent interactions between drugs

Serotonin syndrome Cause: excessive stimulation of serotonin receptors Presentation: Agitation or restlessness Nausea, vomiting and diarrhea Confusion , hallucinations Poor coordination Racing pulse Rapid changes in blood pressure Sweating Hyper-reactive reflexes Fever Seizures Coma

Serotonin syndrome – implicated drugs In some patients combinations of the following drugs can lead to a serotonin syndrome: SSRIs: citalopram (Celexa), fluoxetine (Prozac) SNRIs: duloxetine (Cymbalta), venlafaxine (Effexor) NDRIs: buproprion (Wellbutrin) MAOIs: isocarboxazid (Marplan) and phenelzine (Nardil) Analgesics: tramadol (Ultram), fentanyl (Sublimaze) Anti-migraine: sumatriptan (Imitrex) and zolmitriptan (Zomig) Anti-nausea: metoclopramide (Reglan) and ondansetron (Zofran) Bipolar: lithium (Lithobid) Cough: (Robitussin This risk dextromethorphan depends on genetic make-up (CYPDM) 450 genes) Herbal supplements: St. John's wort and ginseng

Individualize drug dosing based on metabolic profiling of CYP variants 2005 - The FDA-approved Ampli. Chip for analysis of CYP 2 D 6 and CYP 2 C 19, variants of CYP 450 1. Extensive metabolizers. Can be administered drug in "standard“ dosages 2. Intermediate metabolizers. Multiple drug therapy can turn in people into poor metabolizers. 3. Poor metabolizers. May develop drug accumulation and adverse reactions 4. Ultrarapid metabolizers. May experience either no effect or less-thanexpected effectiveness from their drug therapy

What about the placebo effect?
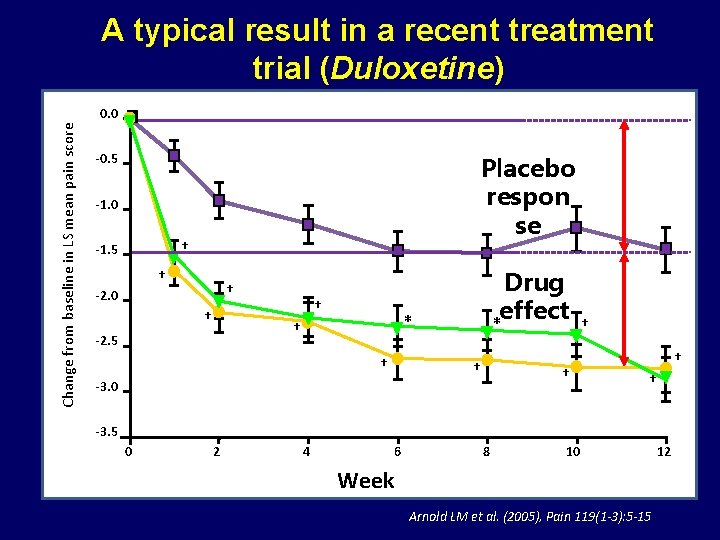
A typical result in a recent treatment trial (Duloxetine) Change from baseline in LS mean pain score 0. 0 -0. 5 Placebo respon se -1. 0 † -1. 5 Drug effect * † † -2. 0 † † * † -2. 5 † † † -3. 0 † -3. 5 0 2 4 6 8 10 Week Arnold LM et al. (2005), Pain 119(1 -3): 5 -15 12

The “placebo” effect is often maligned Take 2 placebos and callhealth me in Apparently your the morning insurance

The latest research has demonstrated the placebo effect’s physiology Compared the effects of an opioid and a placebo on activation of brain regions in an experimental model of

Placebo activation of PAG area The A placebo “placebo” caneffect be theis due equivalent to activation of taking of the descending oxycodone pain or a similar system via opioid the drug PAG Pain + opioid Pain + placebo Pain alone

My final piece of advice Practice activating your PAG

2 minute stretch break

Fibromyalgia Information Foundation Spring Conference 2010 Welcome and orientation - Sharon Clark, Ph. D Fibromyalgia: An Evolving Concept - Robert M Bennett, MD Diagnosis and Misdiagnosis - Atul Deodhar, MD Guided Stretch Break - Janice Holt Hoffman How Can I Help Myself? - Kim Dupree Jones, Ph. D How Can Medications Help Me? - Robert M Bennett, MD Roundtable: Questions and Answers - Drs Bennett, Deodhar and Jones, moderated by Dr Sharon Clark

Dr. Jones Is FM a form of depression?

Dr. Deodhar What else could it be?

Dr. Bennett Is FM inherited?

Dr. Jones Can FM be cured?

Dr. Deodhar What vitamins should I take?

Dr. Bennett Does the XMRV virus cause FM?

Dr. Jones Should I take pain killers?

Dr. Deodhar Should I move to Arizona?

Dr. Bennett Should I try muscle injections?

Dr. Jones Should I change jobs?

Dr. Deodhar Should I see a psychologist?

Dr. Bennett How should I prepare for surgery?

Dr. Jones Why do I hurt more when I exercise?

Dr. Deodhar What will happen to me?

Dr. Bennett What about drugs that are not FDA approved for fibromyalgia?

Thank you for attending this FIF conference These presentations are available on our website at: www. myalgia. com
- Slides: 123