Fever Without Localizing Signs in 2013 Coburn Allen

Fever Without Localizing Signs in 2013 Coburn Allen, MD Pediatric Infectious Diseases Pediatric Emergency Medicine Dell Children’s Hospital

Objectives Ü Discuss the epidemiology of serious bacterial infections in febrile young children. Ü Review recent research that is relevant to this population. Ü Present evidence based recommendations (when available) for the evaluation and treatment of these processes.

Definitions Ü Fever = 38°C (100. 4°F), 39°C (102. 2°F) often used after 2 - 3 months Ü Hypothermia < 36°Celsius (96. 8°F) Ü Hyperpyrexia > 105. 5 or 106° F Ü SBI = Serious Bacterial Infections Ü Neonate = 0 -28 days Ü Young Infant = 0 -60 (or up to 90) days Ü FWLS = 0 -36 m old child with fever < 7 d and no recognized source after H/P, “non-toxic” Ü Fever of Unknown Origin (prolonged, all ages)

Toxic Criteria Ü “Toxic” appearance (A. K. A. septic) Ü Lethargy Ü Poor perfusion Ü Marked hypo/hyperventilation Ü Cyanosis Ü “Toxic” patients = full evaluation Ü 20% of “toxic” 0 -90 day old children have and SBI

SBI Epidemiology in FWLS Ü UTI (most common) Ü High risk populations (6 -8+%) Ü Girls 0 -24 m Ü Boys 0 -6 m, uncirc’d to 12 m Ü VUR, anatomic issues, recurrent UTIs Ü E. coli >> other GNRs, enterococcus Ü Occult bacteremia (OB)+/- meningitis Ü 0 -2 months: GBS, E. Coli, Listeria Ü 2 -36 months Ü Pneumococcus #1, decreased 85% if PCV

SBI Epidemiology Ü H. flu era (before 1990) Ü Pneumococcus #1 Ü H. flu type B Ü Meningococcus Ü Post H. flu era (1990 s) Ü Pneumococcus #1 Ü Salmonella Ü Meningococcus Ü Pneumococcal vaccine(s) era (2000 s)

Post-Hi. B SBI Epidemiology Ü Occult bacteremia Ü Lee and Harper, 1998; 3 -36 m, T > 102. 2 F Ü 1. 6% occult bacteremia Ü 92% pneumococcus, 5% Salmonella Ü Alpern et al, 1999; 2 -24 m, T > 102. 2 F Ü 1. 9% occult bacteremia Ü 83% pneumococcus, 5% Salmonella, 5% GABHS Ü 0. 03% meningitis/death Ü UTI Ü Boys (< 1 year) 2 -3%, 8% if uncircumcised Ü Girls (0 -2 years) 6 -8%, 20 -30% white infants

Pneumococcal Conjugate Vaccine (PCV), “Prevnar” Ü FDA, February 2000 Ü 7 serotypes (4, 6 b, 9 v, 14, 18 c, 19 f & 23 f) Ü Black, et al. , PIDJ 2000 Ü Double blind, Prevnar or meningococcus C Ü 37, 868, randomized 1: 1, 4 year follow-up Ü 40 cases invasive pneumococcus (fully vaccinated) Ü Ü Ü 39 of 40 in meningococcal group 97. 4% efficacy for vaccine serotypes, 89. 1% all serotypes 7% less OM, 20% less PETs, 20% less pneumonia Ü Alpern, et al. , 2001 Ü FWLS, occult bacteremia Ü 97% pneumoccus serotypes covered (83% expected) Ü Suggests the serotypes selected for vaccine focused on OB

Post-PCV Era FWLS Epidemiology Stoll et al. , Arch Pediatr Adolesc Med, 2004 Ü Retrospective, 12/2001 -3/2003, NY Pedi EC Ü 329 2 -36 m FWLS (T>39 C) Ü 3 (0. 9%) occult bacteremia (all pneumococcus) Ü One child twice, no Prevnar Ü Other child had serotype not in vaccine Ü 4 (1. 2%) contaminants Ü Only 28% at 7 m and 66% at 12 m “UTD” Ü CBC poor screening test

Post-PCV Era Occult Pneumococcal BCx + Ü Carstairs et al. , Ann Emerg Med, June 2007 Ü San Diego Ü 2000 -2002, Ü T > 100. 4, Ü BCx done Ü Compared any Prevnar to none

Post-PCV Era Occult Pneumococcal BCx + Ü Unvaccinated Ü 13 of 550 (2. 4%) pneumococcal + Ü All over 28 d Ü Half had pneumonia and bacteremia Ü Vaccinated (any) Ü NO pneumococcal cases Ü 15 contaminants (1. 8%) Ü 2 had E. coli + BCx with UTIs Carstairs et al. , Ann Emerg Med, June 2007

Other Post-Prevnar Data Ü MMWR, 2/08 Ü 77% reduction in “invasive Pneumococcal disease” Ü Herd immunity for unvaccinated Ü Arch Dis Child, 6/2008 Ü Compared occult bacteremia rates (Duke) Ü Post Prevnar era FWLS BCx + Ü 14 contaminants, 1 pathogen (no S. pneumo) Ü 95% reduction in OB rates pre/post Prevnar Ü 50% of FWLS pts. received abx Ü Eur J Emerg Med, 8/2009 Ü Spain, Retrospective, 3 -36 m with FWLS Ü OB 0. 23% if 2 Prevnar, 0. 82% if < 2 doses
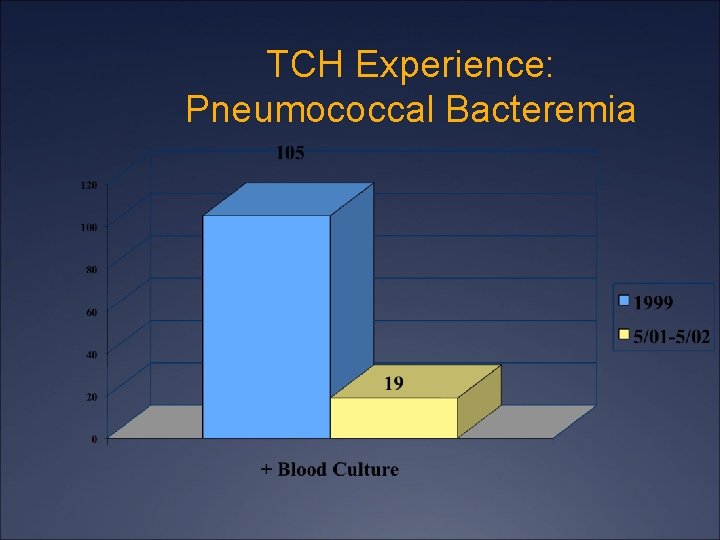
TCH Experience: Pneumococcal Bacteremia
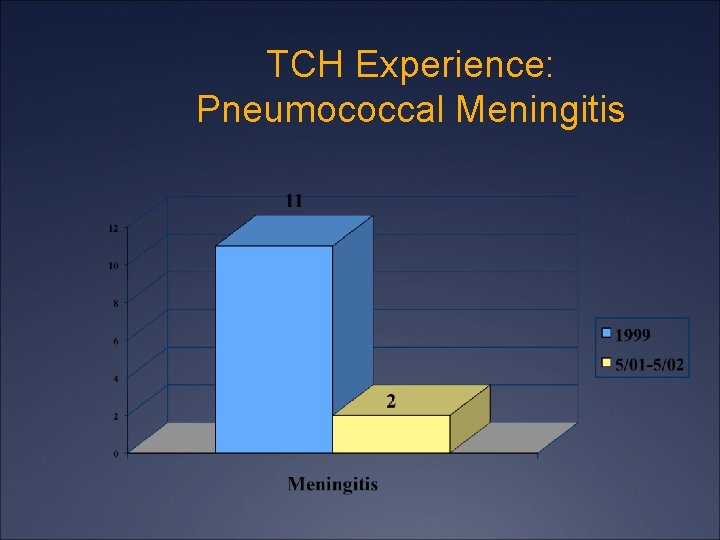
TCH Experience: Pneumococcal Meningitis
Typical SBI Pathogens in Young Infants Ü Prospective Cohort: 1 -90 d/o with fever (38°C) presenting to EC 1999 -2002 Ü N =1298 febrile infants Ü 105 (8%) SBI Ü UTI in 77 (73%) = 6% of cohort Ü 63 of 77 were E. coli Ü 6 of 77 had + BCx (all E. coli) Ü 1 of 77 had + CSF (Serratia marcesens) Ü Bacteremia in 28 (26%) = 2% of cohort Ü Meningitis in 9 (8%) = 0. 7% of cohort Ü 53% of pathogens resistant to ampicillin Byington CL, Pediatrics 2003
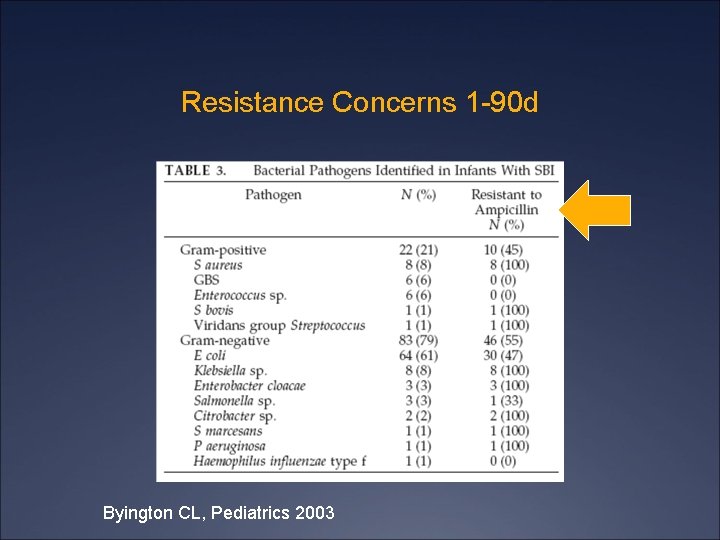

Resistance Concerns 1 -90 d Byington CL, Pediatrics 2003
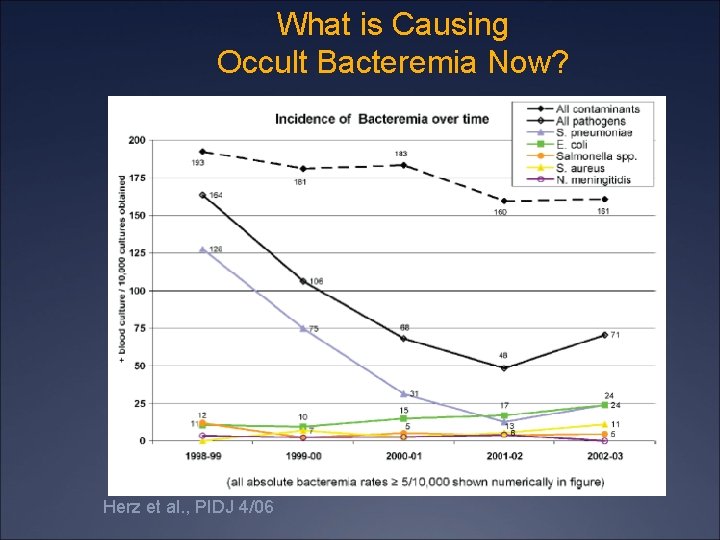
What is Causing Occult Bacteremia Now? Herz et al. , PIDJ 4/06

EBM Approach to FWLS Ü Understand/assign risk (high vs. low) Ü Look for a source Ü Tests, if needed Ü Treat, if needed Ü Good anticipatory guidance and follow-up

Low Risk SBI Criteria in Young infants with FWLS Clinical Criteria 1. 2. 3. Previously healthy, term infant Non-toxic No focal bacterial infection (except OM) Laboratory Criteria WBC 5 -15 K, <1. 5 K bands, or b/n ratio <0. 2 Gram stain un-spun urine negative (preferred), or neg LE and nitrite, or <5 WBC/hpf 3. If diarrhea, <5 WBC/hpf in stool 4. If CSF done, <8 WBC/mm 3 and NOS 1. 2.

“Low Risk Young Infants” Ü Review of literature: Baraff, 2000 Ü Total = 3, 161 , 1420 “low risk” Ü Total SBI rate 0. 9% in low risk Ü 0. 4% UTI Ü 0. 4% Occult Bacteremia Ü 0. 2% Bacterial Enteritis Ü NO Bacterial Meningitis in any of the low risk 0 -90 day olds from any of the studies

What is a viral source?

Viral Sources: Young Infants Ü RSV + Ü Vanderbilt, retrospective cohort (Titus and Wright) Ü 0 -8 weeks, fever (38 C), full eval in EC Ü 174 RSV+ Ü 2 with SBI (UTIs) Ü Corpus Christi, retro cohort (Purcell and Fergie) Ü 0 -90 d/o with RSV+ bronchiolitis Ü No bacteremia/meningitis Ü 1. 1% UTI Ü Influenza Ü Krief WI, et. al. , Pediatrics, July 2009 Ü 0 -60 d, fever (100. 4), rapid flu + vs – Ü Flu +, 2. 5% with SBI, (2. 4% UTI) Ü Flu -, 13. 3% with SBI, (10. 8% UTI, 2. 2% bacteremia, 0. 9% mening) Ü Recommend urine in Flu +
Viral Sources: Older Kids Greenes and Harper, PIDJ 1999 Ü 3 -36 m, T > 102. 2 F, blood culture done Ü Viral syndrome, 2 of 876 (0. 2%) bacteremia Ü Bronchiolitis, 1 of 411 (0. 2%) Ü Croup, 0 of 249 Ü Stomatitis, 0 of 123 Ü Varicella, 1 of 93 (1. 1%) Ü 1. 4% BCx = contaminants Kuppermann, Arch Ped Adol Med 1997 Ü 156 < 2 y/o w/ bronchiolitis; 0 Bcx +, 2% UTI

Is Diarrhea a Source? Ü Prospective, Texas Children’s Ü 3 -24 m/o, FWLS, w/ or w/o diarrhea Ü Cath Ucx if at risk for UTI Ü Boys 0 -6 m (circ), 0 -12 (uncirc) Ü Girls 3 m-24 m Ü Results (N = 231) Ü No diarrhea: 12. 4% had UTI Ü Diarrhea: 8. 5 % had UTI Cardone G, Allen CH, Caviness C, AAP 2009 NCE, Washington, D. C.

Newer OB Screening Tools Ü Absolute neutrophil count (Kuppermann, An Emerg Med 1998) Ü Occult bacteremia, 3 -36 m Ü > 10, 000 = 8. 1% vs. < 10, 000 = 0. 8% Ü Sensitivity 76%, specificity 78% Ü C-reactive protein (Pulliam, Peds 2001) Ü SBI, 1 -36 m Ü CRP > 7, sens 79%, spec 91% Ü Procalcitonin (Lopez, PIDJ 2003) Ü SBI vs. viral, 1 -36 m Ü PCT > 0. 6, sens 70%, spec 94%

SBI Markers Study Manzano, et. al. , Arch. Dis. Child, Jan 2011 Ü Prospective cohort, Quebec, 11/06 -11/07 (90%+ UTD) Ü 1 -36 m, FWLS (38 C), had CBC, BCx, UA/Cx, PCT, CRP Ü Compared labs vs. PE to detect SBI Ü Results Ü 328 (of 457) met inclusion criteria, 29% < 6 m Ü 16% (N= 54) with SBI Ü 89% UTIs (2 of 48 bacteremic, 2 of 48 had nl UA) Ü 7% (N = 4) “Pneumonia” Ü 2% (N = 1) Meningitis (meningococcal B) Ü 2% (N = 1) Occult bacteremia (S. pneumo 33)
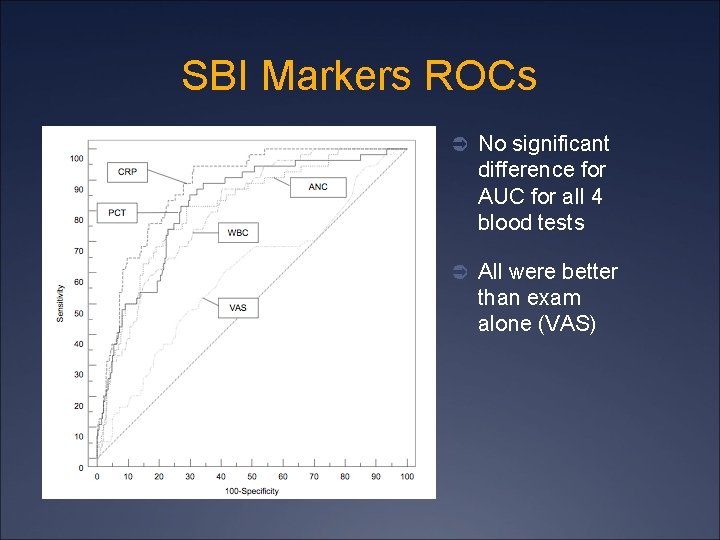
SBI Markers ROCs Ü No significant difference for AUC for all 4 blood tests Ü All were better than exam alone (VAS)
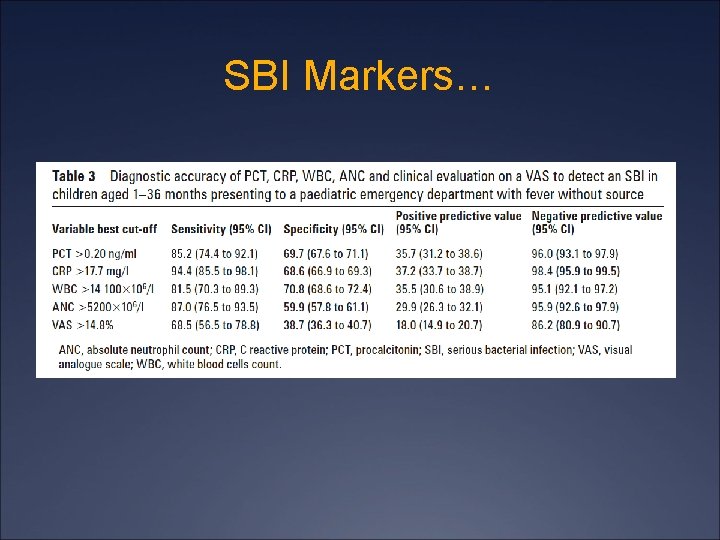

SBI Markers…

SBI Markers if UA normal (do they help? ) Only had 8 SBIs with normal UA Ü 2 UTIs (would have caught with Ucx) Ü 4 “Pneumonias” (could have been viral) Ü 1 Meningitis (no details provided) Ü 1 Occult bacteremia

Does having a PCT change clinical decisions? Ü Manzano (same) et. al. , Am. J. Emer. Med 2010 Ü Same study population Ü Half knew PCT value, half didn’t know Ü No difference in abx prescribing Ü No difference in decision to hospitalize Ü Value of the test “uncertain”
Occult Pneumonia Bachur et al. , An Emerg Med 1999 Ü WBC > 20, 000, T > 102. 2 Ü Normal PE = 26% occult pneumonia Ü Abnormal respiratory exam = 40% pneumonia Ü Bacteremia Ü No difference; pneumonia vs. no pneumonia Ü 6. 5% overall, all pneumococcus TCH post-PCV 7 experience Ü WBC > 25 k better predictor of + CXR Ü Lemke D, Allen CH, SPR 2010

UTI Screening Ü “Enhanced urinalysis” Ü (Hoberman, Peds 1993) Ü Unspun urine Ü Pyuria; > 10 WBC/hpf hemocytometer OR Ü Bactiuria (any) on Gram stain Ü Sensitivity 95. 8%, specificity 92. 6% Ü If neither, NPV 99. 8% Ü Spun urine Ü Gram stain 93% sensitive Ü Dip for LE or nitrite 88% sensitive Ü Sensitivities drop in young infants, 70 -80%

Management of FWLS 0 -28 d Ü Full evaluation Ü Ü Ü CBC, BCx Cath UA, UCx LP, +/- Rapid viral testing Consider LFTs in first 2 weeks Ü Admit Ü IV Abx Ü Amp/Gent (or observe off) if “low risk” Ü UA +, consider 3 rd gen. cephalosporin Ü Gram stain+, adjust therapy Ü IV Acyclovir if HSV suspected
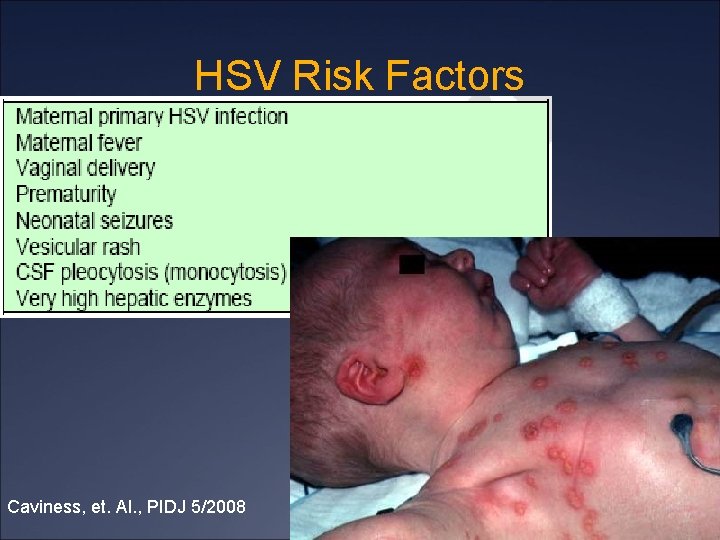
HSV Risk Factors Caviness, et. Al. , PIDJ 5/2008

Management FWLS 29 -60 d Ü Evaluation Ü CBC, BCx Ü Cath Ua, UCx Ü CSF if high risk, concern for meningitis Ü Categorize risk Ü High risk: Admit, LP if not done, IV abx Ü Abx based on screening Ü Ü Ü UA +, consider 3 rd gen cephalosporin Abnl WBC, consider ampicillin and cefotaxime LP abnl, based on stain, if Gram stain-, vanc/ctx Ü Low risk: Discharge, no abx without LP Ü Ceftriaxone 50 mg/kg if abx Ü F/u 1 day

Management FWLS 2 m-3 y Ü Evaluation Ü CBC (and hold BCx) Ü Less than 6 months (some say 4 m) Ü Unimmunized (Hi. B, PCV) Ü No viral source Ü Cath/CC UA, UCx Ü Boys 0 -6 m, 6 -12 if uncirc’d Ü Girls 0 -24 m Ü Low threshold if h/o recurrent UTIs, > 2 d fever Ü Rapid viral testing if changes care Ü Flu in high risk populations Ü Send BCx if ANC > 10 k, DON’T if not Ü CXR if WBC > 20 -25 k

Management FWLS 2 m-3 y Ü Disposition Ü Most discharged home, f/u 1 -2 days Ü Decisions to treat Ü ANC > 10 k; 50 mg/kg IM ceftriaxone Ü UA+; 3 rd gen PO cephalosporin Ü Pneumonia; PO beta lactam (i. e. amox) Ü Anticipatory guidance Ü Antipyretics Ü What to expect/worry about Ü Expect fever 3 -5+ days for most viral illnesses Ü Return if SOB, dehydration, irritable/lethargy/AMS

Management FWLS 2 m-3 y Positive Blood Cultures (Allen CH, Up. To. Date) Ü All should be reevaluated Ü Contaminant vs. Pathogen Ü Gram stain Ü Time to positivity Ü GPCs pairs/chains or confirmed Pneumococcus Ü Febrile: LP, if neg ceftriaxone home on PO amox Ü 30 -40 % still bacteremic Ü 4% meningitis Ü Afebrile/Well: reculture, no LP, PO amox Ü Other Pathogens: BCX, LP (except E. coli and Staph aureus after 3 m), admit IV abx

FWLS Epi: National Trends Simon AE, et. Al. , Peds Emerg Care, 6/2013 Ü 1. 6 million visits/yr, for FWLS in 2 -24 m in 2009 Ü 20% of ER visits in 2 -24 m are for FWLS Ü Decreased blood work done since 2004 Ü No significant change in UAs Simon AE, et. Al. , Peds, 12/11 Ü No tests in 56% of FWLS, 3 -36 m Ü 20% get CBC Ü 17% got UA (only 40% of girls with 39 C)

Happy Hunting!

TCH Algorithm: 0 -60 days
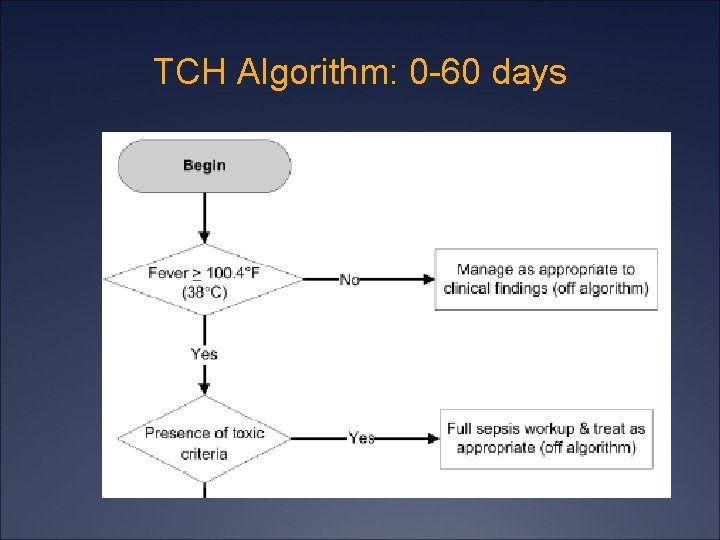
TCH Algorithm: 0 -60 days
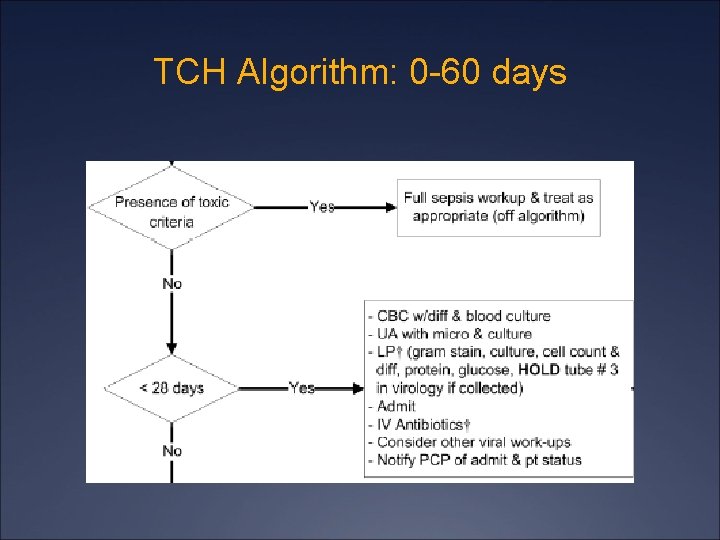
TCH Algorithm: 0 -60 days
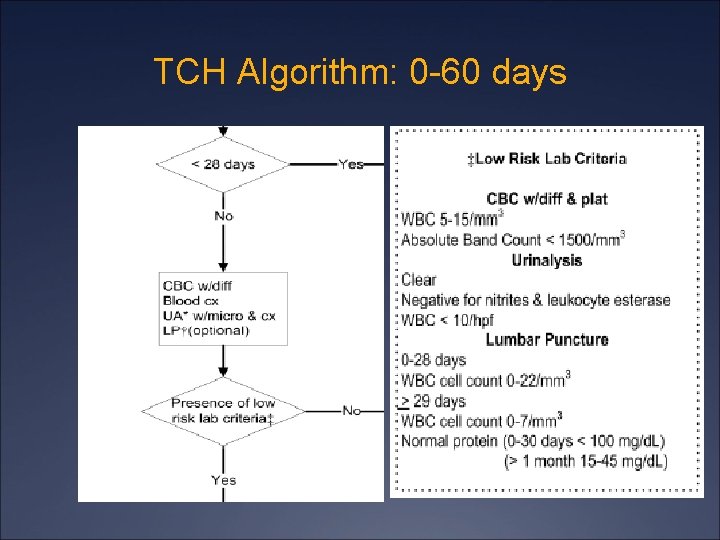
TCH Algorithm: 0 -60 days

TCH Algorithm: 0 -60 days

TCH Algorithm: 0 -60 days
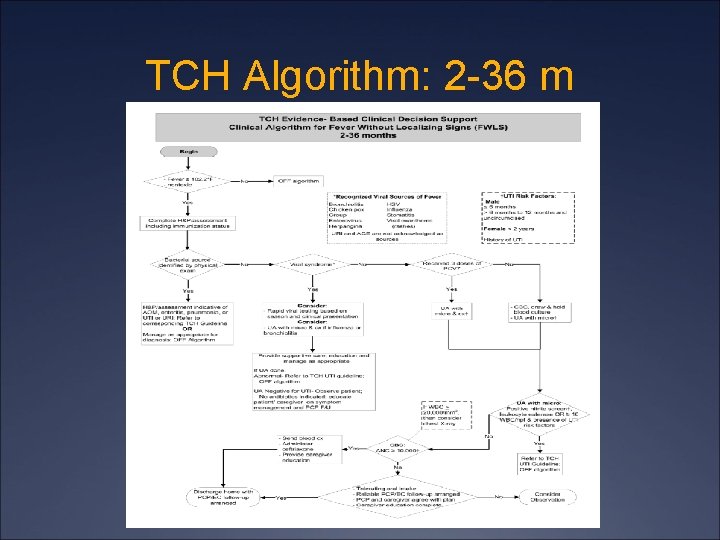
TCH Algorithm: 2 -36 m
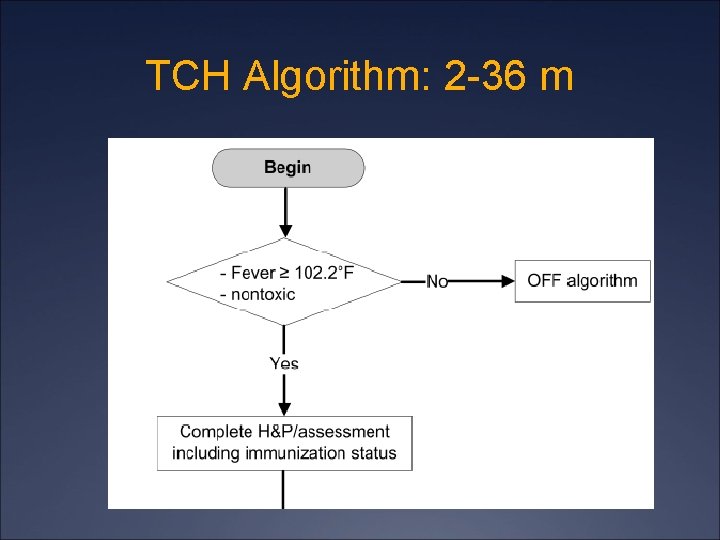
TCH Algorithm: 2 -36 m
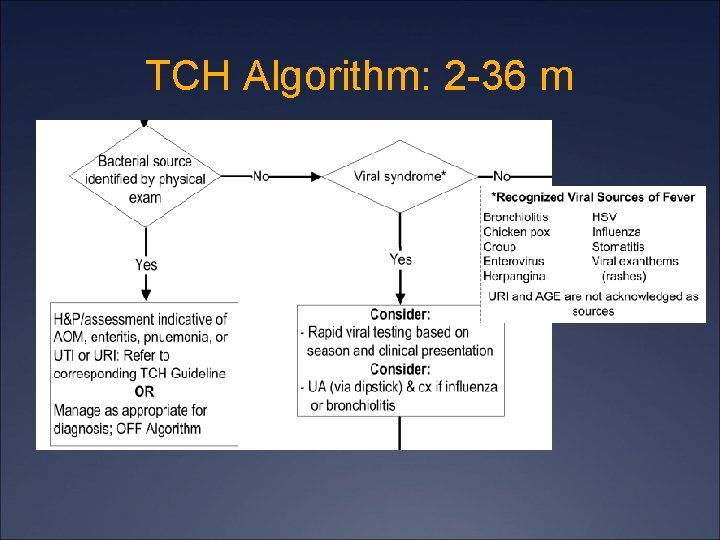
TCH Algorithm: 2 -36 m
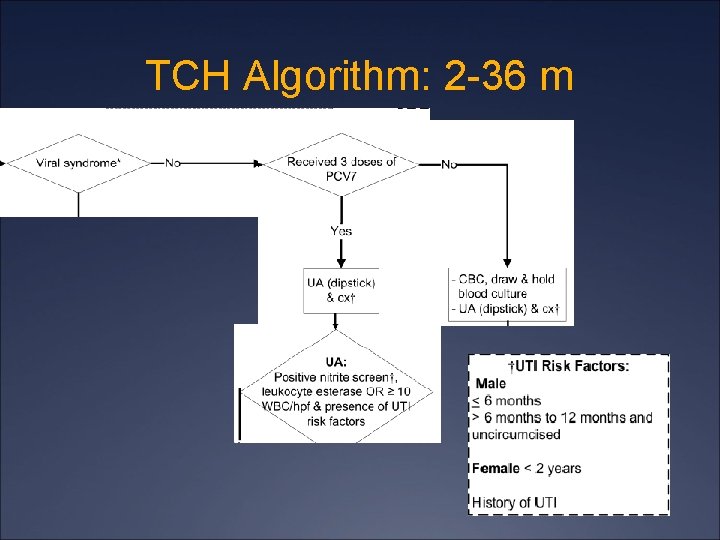
TCH Algorithm: 2 -36 m
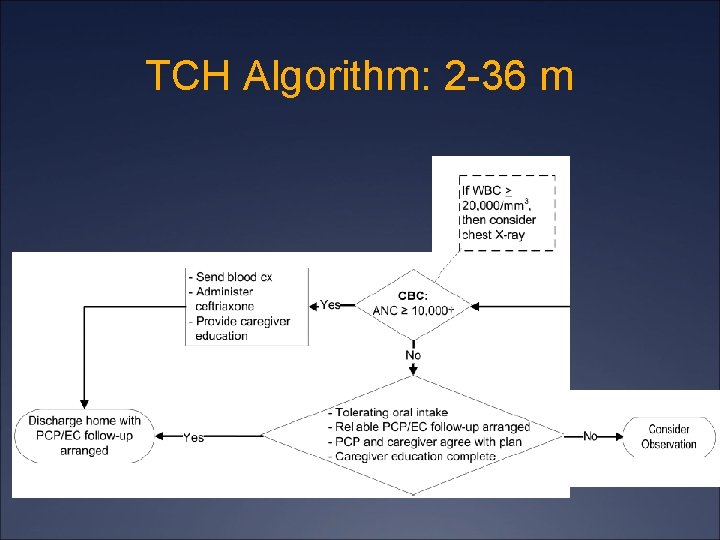
TCH Algorithm: 2 -36 m

Q/A
- Slides: 52