FEVER AND RASH Prof H Herry Garna dr


















































- Slides: 65

FEVER AND RASH Prof. H. Herry Garna, dr. , Sp. A(K), Ph. D Infection – Tropical Disease Subdivision Department of Child Health, Faculty of Medicine Padjadjaran University, Hasan Sadikin General Hospital Bandung

Introduction n n Fever is often the first symptom noted by parents, common problem in clinic Wide range of severity: self limiting disease life-threatening Wrong first suspicion fatal outcome It is more likely to be caused by infection, but any inflammatory, neoplastic, immunologic or traumatic event can generate fever

Introduction n Knowledge of differential diagnosis is very important n Diagnosis - Accurate anamnesis - Physical examination - Supporting examination

Differential Diagnosis n n n Past history of infectious disease and immunization Type of prodromal period Feature of the rash Presence of pathognomonic or other diagnostic signs Laboratory diagnostic tests

Differential Diagnosis n Feature of the rash * Category: - Macular or maculo-papular: Morbilli, rubella, roseola infantum, scarlatina - Papulo-vesicular: Varicella, herpes zoster, variola * Character: discrete or confluent * Distribution, duration * The appearance associated with fever?

Etiologic Agents Infectious Diseases n Virus Classic viral exanthema: Measles, Rubella, Varicella Zoster Virus (VZV) Parvovirus, Roseola (HHV 6 and HHV 7) Others: HSV, EBV, HBV, Enterovirus, Dengue n Bacteria Scarlet fever, meningococcemia, typhoid fever Staphylococcal infection (sepsis, toxic shock syndrome)

Etiologic Agents n n Mycoplasma Rickettsia Noninfectious Diseases n Allergic: food, drugs, toxin, serum sickness n The etiology remains elusive: Kawasaki disease

Anamnesis n Demographic data n Appearance of rash n History of exposure n History of health before n History of disease in the family n Other complaint

Anamnesis Demographic Data n n n Age: neonate, infant, older children Sex Ethnic/race : Kawasaki disease ? Season: winter or dry season or not specific Certain geographic: endemic

Anamnesis Appearance of rash Location and distribution n Expansion and evolution n Correlation between rash and fever in the period of high fever (morbilli) in the period of decreasing fever (roseola infantum) n Pain or itching (drug eruption: itching) n

Anamnesis History of Exposure n n n Contac t with similar disease (house, others) Travel Pet, insects Medicine or other medical measures Immunization

Anamnesis History of health before n n n History of disease before Growth and development History of recurrent disease History of disease in the family Autoimmun ?

Anamnesis Other complaint n Local complaint (specific organ) n Systemic complaint (multiorgan/multisystem diseases)

Physical Examination n General condition/severity of disease n Characteristic of rash n With enanthema n Other physical disorders

Physical Examination General condition/severity of disease n Meningococcemia, Staphylococcal toxic syndrome Characteristic of rash Macule, papule, maculo-papule n Vesicle, pustule, bulla n Petechiae or purpura n Erythroderma: diffuse or local

Nonblanching lesions n n n Petechiae, purpura, and echymosis Difference size Petechiae diameter <2 mm Purpura 2 mm– 1 cm Echymosis diameter >1 cm

Physical Examination With enanthema n Mouth: Hand-foot-mouth disease? Buccal mucosa, palatum, pharyng, and tonsil n Genital mucosa Others n Arthritis, eye disorders, cardiac disorders n Hepatomegaly, splenomegaly, lymphadenopathy

Diffential Diagnosis of Fever and Rash Viruses Bacteria Other Maculo/papular Measles, rubella, HHV -6, Dengue EBV, HIV, enterovirus GABHS (scarlet fever) Salmonella, Lyme, Mycoplasma pneumoniae Rickettsia Vesicular, bullous VZV, HSV, Echovirus Coxsackievirus A, B (HFMD) Impetigo (GAS) Petechiae Hemorrhagic fever, Sepsis (N. men, CMV, EBV, VZV S. pneu, Hib) enterovirus Rat bite fever Rickettsia Diffuse erythroderma Dengue C. albicans GABHS (scarlet fever) TSS

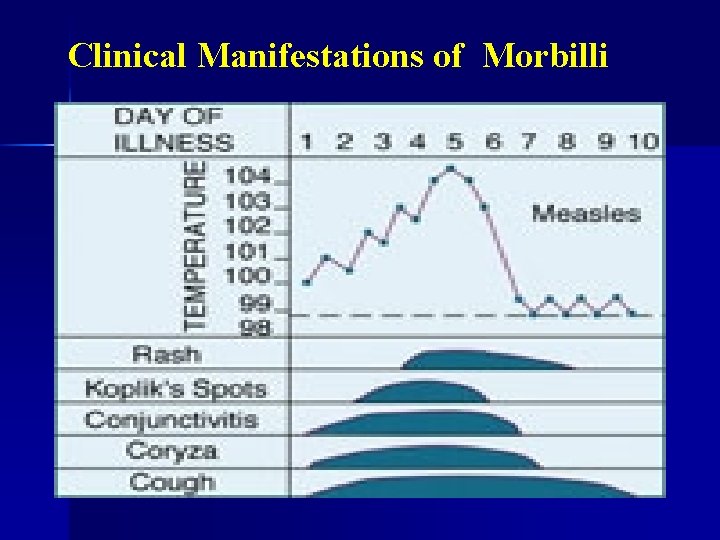
Morbilli (Measles, Rubeola) Clinical Appearance n Incubation period: 10– 12 days n Three stadia: prodromal—eruption— convalescents n Prodromal: 3– 5 days 3 C (Coryza, Conjunctivitis, Cough), fever, Koplick’s spots n Eruption: high fever (40– 40, 5°C) Typical rash: - Maculo-papular erythromatous - Confluence-general - Start from backside of ear (head) body and upper arm lower extremities during 3 days whole of body

Morbilli n n • • Endemic in developing countries Effective immunization program cases decreasing prone to older age group Lesion particularly at skin, mucous membrane, conjunctiva Serous exudate, mononuclear cell predominant

Diagnosis Anamnesis * Symptoms * History: contact, immunization n Clinical signs * Typical n Laboratory examination * Leukopenia * Relative lymphocytosis n

Clinical Manifestations of Morbilli

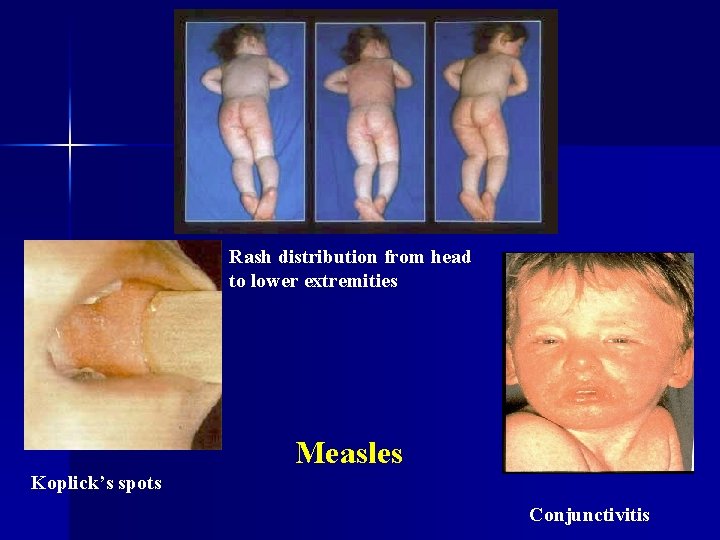
Rash distribution from head to lower extremities Measles Koplick’s spots Conjunctivitis

Morbilli Complications n n n Acute otitis media (10– 15%) Pneumonia interstitialis (50– 75% with radiologic abnormalities) Myocarditis and pericarditis Encephalitis (1/1, 000 cases) 7– 10 days after rash appearance (1/3 dead, 1/3 physical defect, 1/3 recover ) Subacute sclerosing panencephalitis (SSPE) (0, 2– 2 /100, 000 morbilli, mean incubation 7 years) CFR almost 100% after 6– 9 months

Complications n n n Persistent diarrhea Exaserbation of tuberculosis (TBC) Keratoconjunctivitis blindness Secondary bacterial infection of skin Noma

Rubella (German Measles) n n Prodromal sign: +/Rash: short period 3 days Typical sign: lymphadenopathy postauricular, suboccipital, posterior colli Problems in pregnant women congenital rubella syndrome

Clinical Manifestations Incubation period: 15— 21 days n Mild prodromal sign: - mild fever - adolescent: more severe n Rash: maculopapular face centrifugal to neck trunk, extremities 24 hours all of body resolve in 3 rd day n

Congenital Rubella Syndrome Depend on gestational age Abortus Stillbirth Congenital anomaly n Gravida 1– 4 weeks: 61% 5– 8 weeks: 26% 9– 12 weeks: 8% n

Congenital Rubella Syndrome n n Opthalmologic: Cataract - Micropthalmia Glaucoma - Chorioretinitis Cardiac: Septal defect - PDA Neurologic: Meningoencephalitis Microcephaly Mental retardation Auditoric: Sensorineural deafness

Exanthema Subitum (Roseola Infantum) n n Acute infection caused by human herpes virus 6 (some HHV 7) Mostly in infant Sporadic (sometimes epidemic) Typical feature: - Severity of clinical sign unproportionally with degree of fever - Simultaniously resolve of rash and clinical sign

Clinical Manifestation n n n Incubation period: 7– 17 days (mean 10 days) Most common in 6– 18 months old Fever - abruptly high: 39, 4– 41, 2°C - duration: 1– 5 days (mostly 3– 4 days) - convulsion can occur Mild clinical sign: mild pharyngitis and coryza Rash: not specific: macule/maculopapular, rose color chest extremities and neck face Appear while temperature has return to normal Disappear on 1– 2 days with normal skin

Prognosis n n Particularly good prognosis Bad prognosis: Hyperpyrexia with persistent convulsion

Scarlet Fever - Scarlatina Clinical manifestation n Incubation period: 1– 7 days (mean: 3 days) n Acute symptoms: high fever—headache— vomiting—chills n Signs: severe pharyngitis hyperemia— edema— exudate—dysphagia n Sometimes abdominal pain n Enlargement of lymph node

Scarlet Fever - Scarlatina Typical rash n Erythroderma diffuse (red sandpaper) n Reddish macule/papule blanching on pressure n Firstly on axilla, groin, and neck 24 hours all of body n Petechiae can occur Rash at chin and forehead (confluence): circumoral palor n n Usually: palms and soles of feet

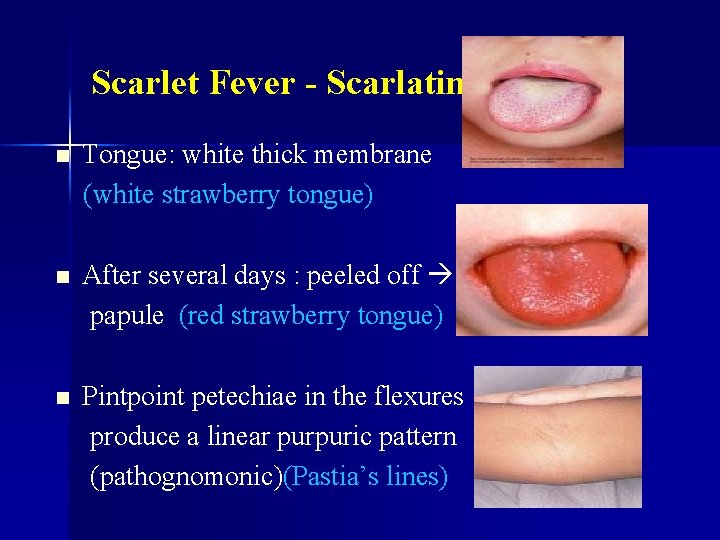
Scarlet Fever - Scarlatina n Tongue: white thick membrane (white strawberry tongue) n After several days : peeled off papule (red strawberry tongue) n Pintpoint petechiae in the flexures produce a linear purpuric pattern (pathognomonic)(Pastia’s lines)

Scarlet Fever (Scarlatina) A beta-hemolytic Streptococcus group pyrogenic toxin (erythrogenic toxin) Desquamation occur from end of 1 st week to 6 th week of disease Diagnosis: History and physical examination Pharyngeal swab: bacterial culture Serologic: ASTO/ASLO/ASO Complete blood count: leukocytosis CRP increased or +: not specific n

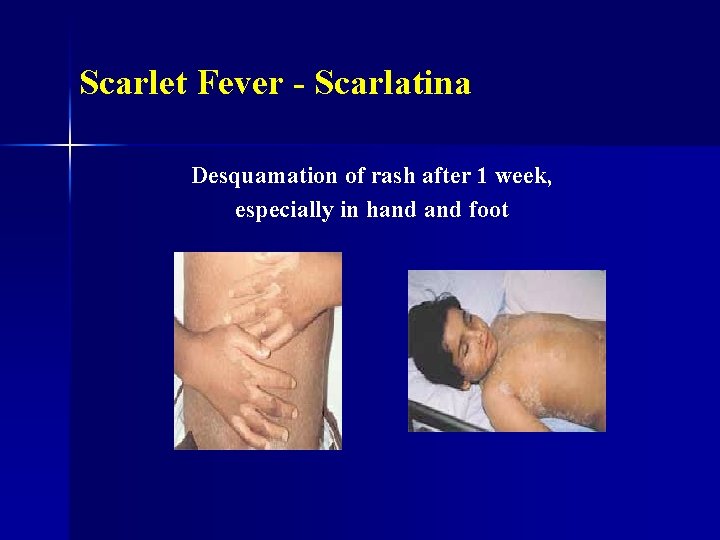
Scarlet Fever - Scarlatina Desquamation of rash after 1 week, especially in hand foot

Complications Local spread/per continuitatum: - Sinusitis – otitis media – mastoiditis - Retro/parapharyngeal abcess - Brochopneumonia - Servical adenitis n Hematogenic spread n - Meningitis – osteomyelitis – arthritis (septic) n Non suppurative (late) complications - Acute rheumatic fever n - Acute glomerulonephritis

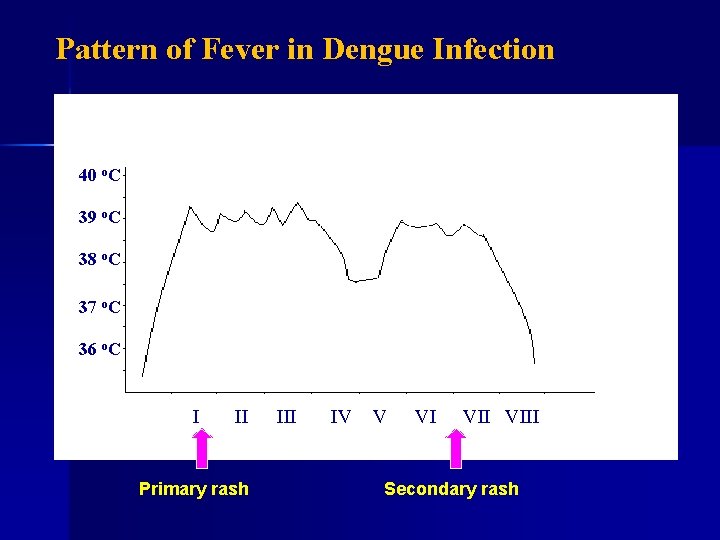
Dengue Fever (1) • Incubation period: 3– 14 days • Fever: suddenly high disappear: day-3 or 4 recover or dicrease: day-3 atau 4 , and appear again after 1– 3 days camel saddle Long of fever: 5– 7 days

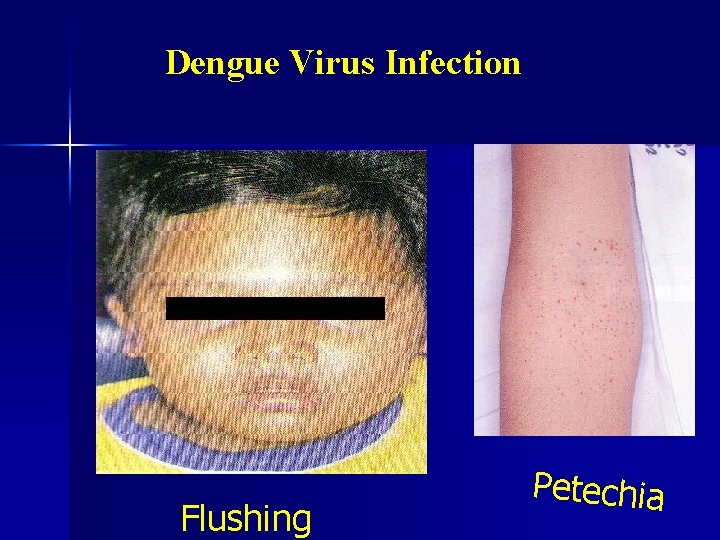
Dengue Fever (2) Other complaint • Headache, retro orbital pain • Joint pain, back pain (backborne fever) • Weakness, malaise • Flushing: face, neck • Photophobia, cough

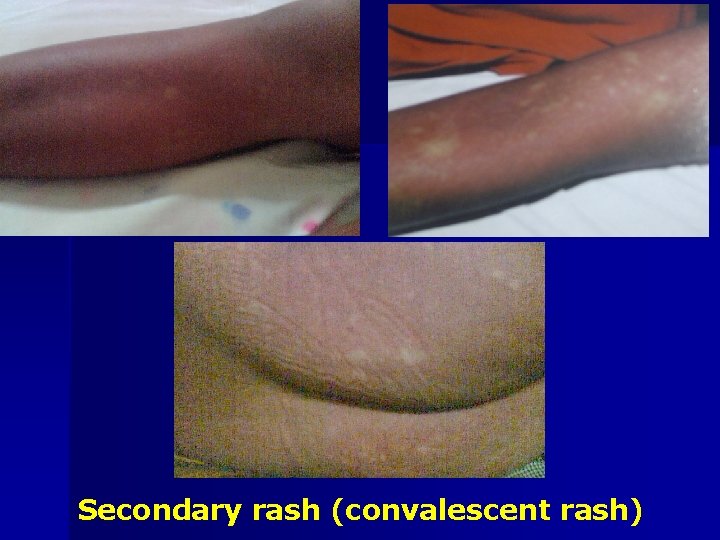
Dengue Fever (3) Skin rash Primary rash Rash: morbilliform (maculopapule): chest and joint fold Secondary rash After day-4, especially day-6 or day-7 Maculopapule/petechiae /purpura/mixed Confluence: usually hand foot Sometimes itching

Dengue Fever (4) • Hemorrhage ? • Although not usual hemorrhage - petechiae (skin) - epistaxis - gum bleeding, vomiting/with blood - menorrhage

Pattern of Fever in Dengue Infection 40 o. C 39 o. C 38 o. C 37 o. C 36 o. C I II Primary rash III IV V VI VIII Secondary rash

Dengue Virus Infection Flushing Petechia

Secondary rash (convalescent rash)

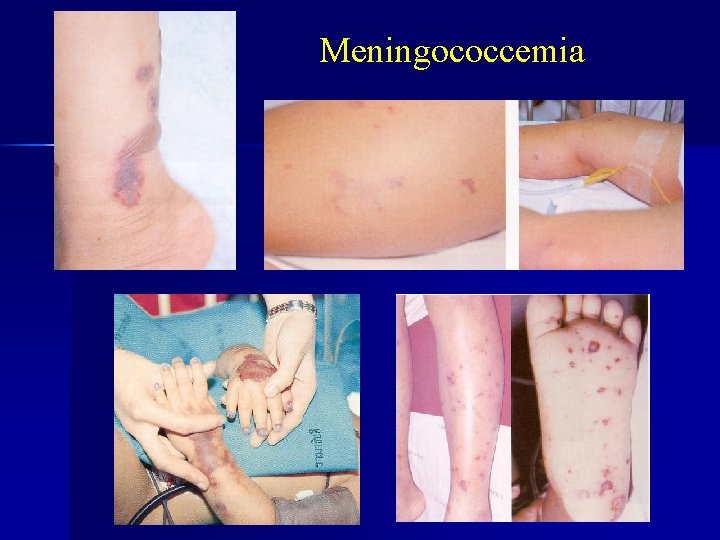
Meningococcemia n Etiology: Neisseria meningitidis (meningococcus) n Clinical manifestations – Acute fever, suddenly high – Hemorrhagic manifestations: petechia, purpura (fulminant) – Progressive severe meningitis, sepsis, septic shock

Meningococcemia

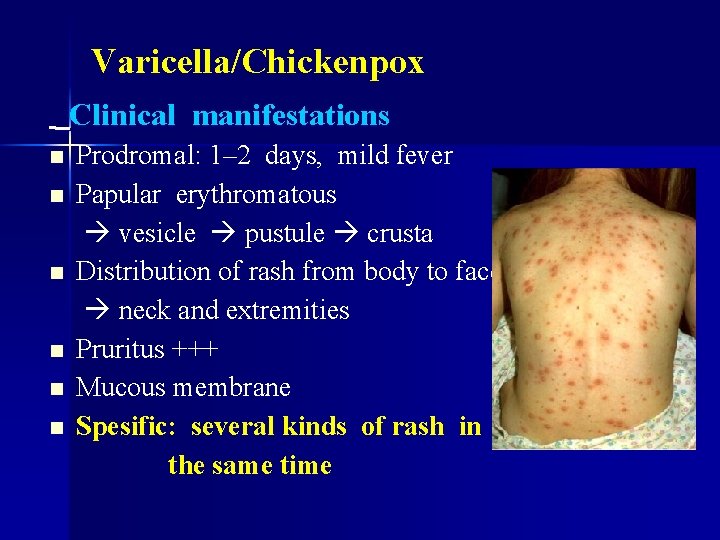
Varicella/Chickenpox Clinical manifestations n n n Prodromal: 1– 2 days, mild fever Papular erythromatous vesicle pustule crusta Distribution of rash from body to face neck and extremities Pruritus +++ Mucous membrane Spesific: several kinds of rash in the same time

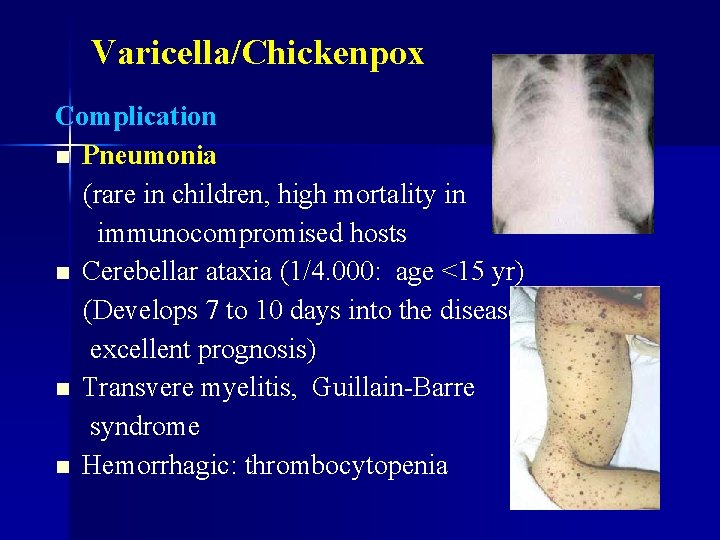
Varicella/Chickenpox Complication n Pneumonia (rare in children, high mortality in immunocompromised hosts n Cerebellar ataxia (1/4. 000: age <15 yr) (Develops 7 to 10 days into the disease, excellent prognosis) n Transvere myelitis, Guillain-Barre syndrome n Hemorrhagic: thrombocytopenia

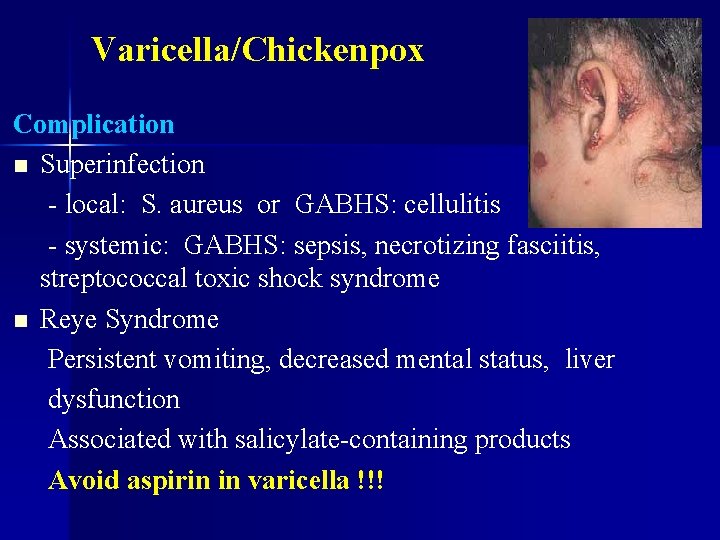
Varicella/Chickenpox Complication n Superinfection - local: S. aureus or GABHS: cellulitis - systemic: GABHS: sepsis, necrotizing fasciitis, streptococcal toxic shock syndrome n Reye Syndrome Persistent vomiting, decreased mental status, liver dysfunction Associated with salicylate-containing products Avoid aspirin in varicella !!!

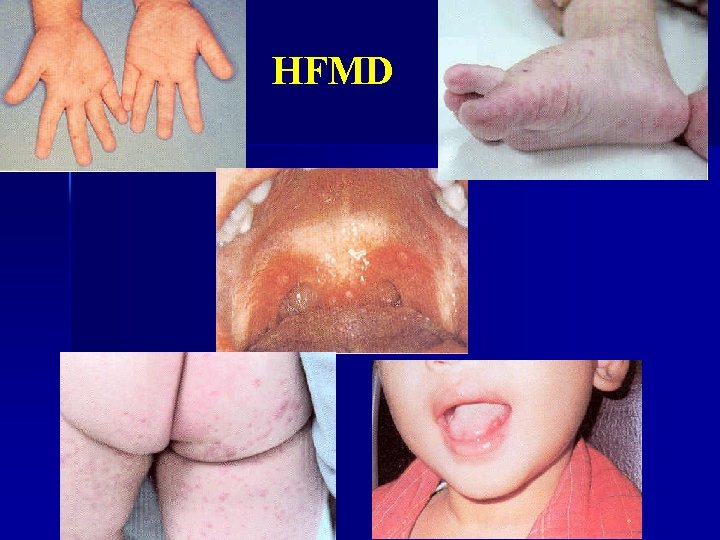
Hand-foot-mouth Disease Etiologi - Coxackie virus type 16 (A 16) >> - Enterovirus 71 encephalitis - Others: A 5, A 7, A 9, A 10, B 2, B 5 n n Fever, pharyngitis, salivation n Self-limiting, simptomatic therapy

HFMD

Kawasaki disease n n n n First described in 1967 Incidence: 67 cases /100, 000 in Japan 5. 6 cases/100, 000 in USA 85% in children < 5 years (peak 18– 24 mo) Rarely occurs in adolescent, adults or children < 6 mo M/F ratio 1. 4: 1 Occurs often in late winter and spring Etiology: Unknown Pathophysiology: « Superantigen theory » causing an intense vasculitis

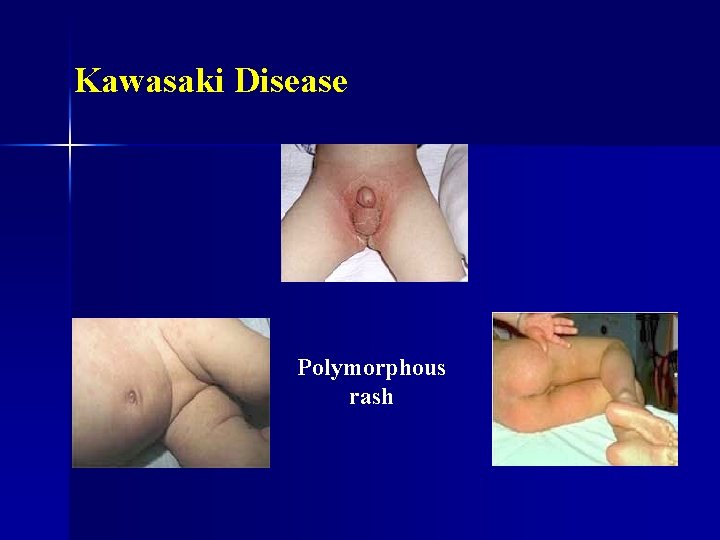
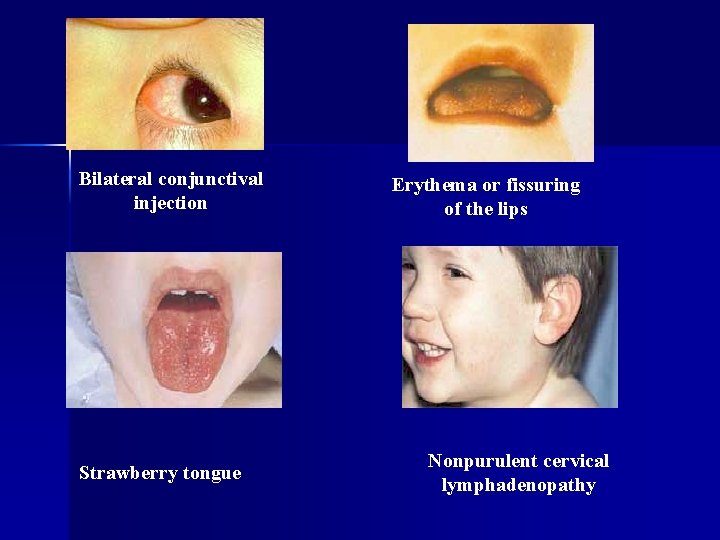
Kawasaki Disease n 1. 2. 3. Diagnosis: fever lasting more than 5 days, plus 4 of the following 5 criteria (other illnesses with similar clinical signs must be excluded): Polymorphous rash Bilateral conjunctival injection One or more of the following mucous membrane changes: - Diffuse injection of oral and pharyngeal mucosa - Erythema or fissuring of the lips - Strawberry tongue

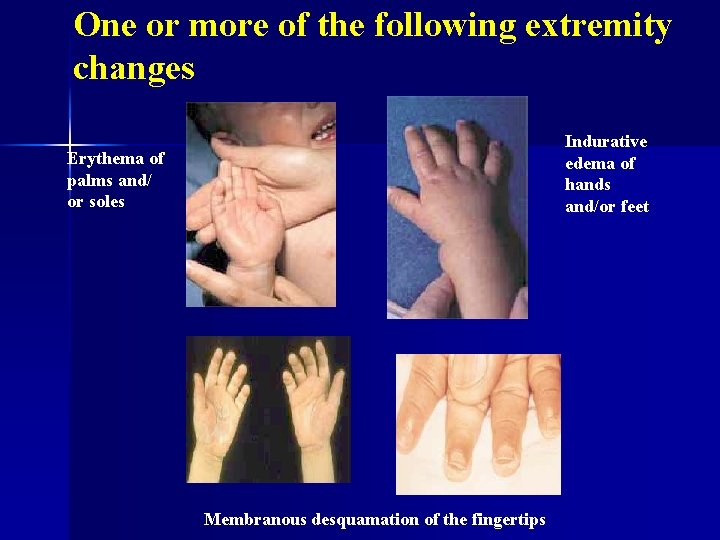
Kawasaki Disease 4. Acute, nonpurulent cervical lymphadenopathy (one lymph node must be >1. 5 cm) 5. One or more of the following extremity changes: - Erythema of palms and/or soles - Indurative edema of hands and/or feet - Membranous desquamation of the fingertips

Kawasaki Disease Polymorphous rash

One or more of the following extremity changes Indurative edema of hands and/or feet Erythema of palms and/ or soles Membranous desquamation of the fingertips

Bilateral conjunctival injection Strawberry tongue Erythema or fissuring of the lips Nonpurulent cervical lymphadenopathy

Conclusions

Children Who Present Fever and Rash Group 1 : children with symptoms of serious illness who require immediate intervention Group 2 : children with a clearly recognizable-and usually benign viral syndrome Group 3 : children who present early in the course of the disease, when the clinical picture and physical findings are nonspecific, and those with undifferentiated rashes with fever

Key Questions Acute or Chronic (Recurrent)? When did it start? Pattern of Spread? Sick or Well? Pruritic? Medications? Exposures?

Describe What You See Pattern/Distribution Diffuse or Localized? Mucous Membranes? Palms & Soles? Exposed vs. Unexposed Areas? n n n Individual Lesions Color Size Blanches? Characteristics Other Physical Findings


Common Primary Skin Lesions Macule : Circumscribed area of change in normal skin color, with no skin elevation or depression; may be any size Papule : Solid, raised lesion up to 0. 5 cm in greatest diameter Nodule : Similar to papule but located deeper in the dermis or subcutaneous tissue; differentiated from papule by palpability and depth, rather than size Plaque : Elevation of skin occupying a relatively large area in relation to height; often formed by confluence of papules

Common Primary Skin Lesions Vesicle : Circumscribed, elevated, fluid-containing lesion less than 0. 5 cm in greatest diameter; may be intraepidermal or subepidermal in origin Bulla : Same as vesicle, except lesion is more than 0. 5 cm in diameter Pustule : Circumscribed elevation of skin containing purulent fluid of variable character (i. e. , fluid may be white, yellow, greenish or hemorrhagic)