Fetal Death BY GHAIDAA ALARAJ DEFINITION Fetal death

Fetal Death BY GHAIDAA AL-ARAJ

DEFINITION • Fetal death : • refers to babies with no signs of life after 24 w of gestation or weighing > 500 gm. • IUFD , Stillbirth, ? ? • Neonatal Death : within 28 days • of life mostly due to complications during birth, prematurity malformations; infections acquired either at home or in hospital
INCIDENCE • 4 /1000 births • IMPACTS 1 -medicolegal risk • 2 -health care system. 3 -emotion

CAUSES the RCOG guideline no. 55 states that parents should be told that no specific cause is found in 50% cases Maternal , fetal , placental.

MATERNAL CAUSES 1 - Obesity (>30 kg/m 2): proven, modifiable, highest ranking • • 2 - Maternal age (>35 yrs) and paternal age • 3 - Smoking/alcohol/drug abuse • 4 - Infections (malaria, hepatitis, influenza, syphilis, sepsis) • 5 - Medical diseases DM, HTN, THYROID DISEASES • 6 -Pre-existing diseases (, anaemia, ) • 7 -Autoimmune disorders (APS, SLE) • 9 -Thrombophilias • • 10 -Cholestasis of pregnancy • • 11 - Rh incompatibility , abruption, pprom, multifetal gestation , labour related • (preterm, uterine rupture)

FETAL CAUSES • 1 -MULTIPLE GESTATION • 2 -IUGR • 3 -CONGENITAL ANOMALIES • 4 -INFECTIONS • 5 - HYDROPS (IMMUNE & NON-IMMUNE) • 6 -G 6 PD DEFICIENCY • 7 -BIRTH DEFECTS •

PLACENTAL CAUSES • 1 -ABRUPTION • 2 -CORD ACCIDENTS • 3 - PLACENTAL INSUFFICIENCY • 4 -PLACENTA PREVIA • 5 - TTTS • 6 - CHORIOAMNIONITIS • 7 -PROM • 8 - FETO-MATERNAL HEMORRHAGE • 9 - ECV ? ? ? •

HOW TO APPROACH FETAL DEATH ? History : absence of fetal movements, • loss of signs & symptoms of pregnancy , other? • Physical exam : decreased fundal height • , no fetal movements , difficult palpation of fetal parts • , fetal heart sound not audible. . x-ray abdomen in the past Robert’s sign : appearance of gas shadow (in 12 hours) Spalding sign: collapse skull bones (usually appears 7 days after ) Ball sign : hyperflexion of the spine • Helix sign : gas in umbilical arteries • Crowding of the ribs shadow • •
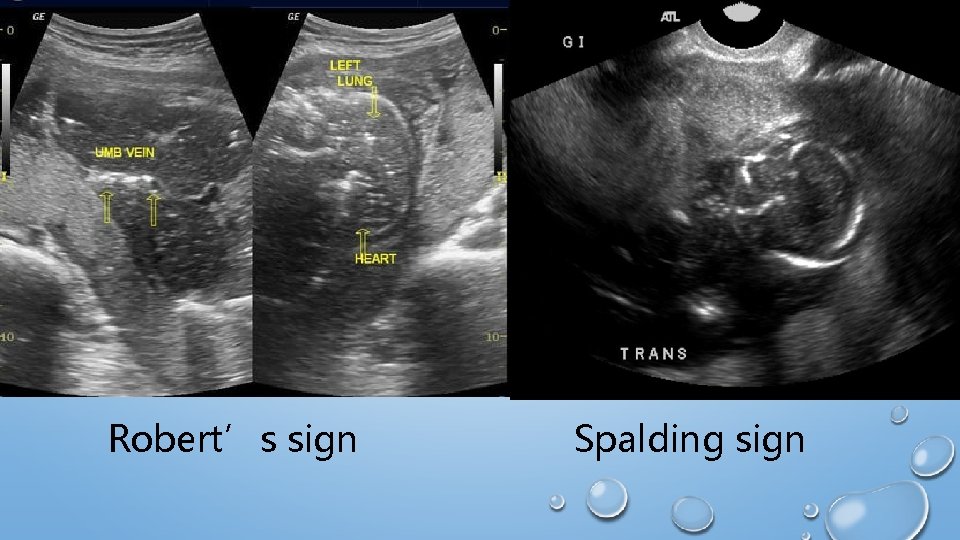
Robert’s sign Spalding sign

DIAGNOSIS REAL-TIME ULTRASONOGRAPHY • is essential for the accurate diagnosis of IUFD. 1 - Abcence of fetal heart beat , 2 -Abcence of fetal movemevt , , • 3 -Gross distortion of fetal anatomy , • 4 -Soft tissue edema , • 5 -Echogenic amniotic fluid fetal demise fragments • # a second opinion should be obtained whenever practically possible # mothers should be prepared for the possibility of passive fetal movement. if the mother reports passive fetal movement after the scan to diagnose iufd, a repeat scan should be offered. •

Investigations of the cause • clinical assessment and laboratory tests should be recommended to assess maternal • wellbeing (including coagulopathy) and to determine the cause of death, the chance of recurrence and possible means of avoiding further pregnancy complications. Tests recommended for women • CBC, blood grouping • FIBRINOGEN • COAGULATION PROFILE • • KLEIHAUER • CRP • Maternal serology • Maternal bacteriology • maternal HBA 1 C • maternal THYROID FUNCTION

WHAT IS THE BEST PRACTICE FOR DISCUSSING THE DIAGNOSIS AND SUBSEQUENT CARE? • if the woman is unaccompanied, • an immediate offer should be made to call her partner, relatives or friends. • discussions should aim to support maternal/parental choice. • parents should be offered written information to supplement discussions • empathetic techniques must be used.

COMPLICATIONS : ? ? •

LABOUR AND BIRTH • recommendations about labour and birth should take into account the • mother’s preferences as well as her medical condition and previous • intrapartum history. • women should be strongly advised to take immediate steps towards delivery if there is sepsis, preeclampsia, placental abruption or membrane rupture, but a more flexible approach can be discussed if these factors are not present. vaginal birth is the recommended mode of delivery for most women more than 85% of women with an IUFD labour spontaneously within three • weeks of diagnosis • vaginal birth can be achieved within 24 hours of induction of labour for IUFD in about 90% of women • caesarean birth might occasionally be clinically indicated by virtue of maternal condition. . . •

Induction of labour • misoprostol can be safely used for induction of labour in women with a single previous CS • and an IUFD but with lower doses • women with more than two CS deliveries or atypical scars should be advised that the safety • of induction of labour is unknown • mechanical methods of induction might increase the risk of ascending infection in the presence of IUFD women labouring with a scarred uterus women undergoing VBAC should be closely • monitored for features of scar rupture. • oxytocin augmentation can be used for VBAC, but the decision should be made by a • consultant obstetrician.

LACTATION • women should be advised that dopamine agonists successfully suppress lactation in a • very high proportion of women and are well tolerated by a very large majority; cabergoline is superior to bromocriptine. • dopamine agonists should not be given to women with hypertension or pre-eclampsia.

postmortem examination parents should be offered full postmortem examination to help explain the cause of an • IUFD. • parents should be advised that postmortem examination provides more information than other (less invasive) tests. • attempts to persuade parents to choose postmortem must be avoided; individual, cultural and religious beliefs must be respected. • written consent must be obtained for any invasive procedure on the baby including tissues taken for genetic analysis. • parents should be offered a description of what happens during the procedure. postmortem examination should include external examination with birth weight, histology • of relevant tissues and skeletal x-rays. • pathological examination of the cord, membranes and placenta should be recommended • whether or not postmortem examination of the baby is requested. the examination should be undertaken by a specialist perinatal pathologist. • parents who decline full postmortem might be offered a limited examination (sparing certain organs)

DISCUSS CONTACT BABY : 1 -Some parents order minimal contact • 2 -Other wish take baby home • 3 -Others creat memory box •

legal issues obstetricians and midwives should be • aware of the law related to stillbirth. • the following practice guidance is derived from statute and code of practice. • stillbirth must be medically certified by a fully registered doctor or midwife. • the doctor or midwife must have been present at the birth or examined the baby after birth. • police should be contacted if there is suspicion of deliberate action to cause stillbirth. • the baby can be registered as indeterminate sex awaiting further tests.

psychological and social aspects of care perinatal death is • associated with increased rates of admission owing to postnatal depression • counselling should be offered to all women and their partners • debriefing services must not care for women with symptoms of psychiatric disease in isolation. • parents should be advised about support groups. follow up • the wishes of the woman and her partner should be • considered when arranging follow-up • women should be offered general prepregnancy advice • women should be advised to avoid weight gain • family planning , control medical condition. 28. thank you •

THANK YOU
- Slides: 21