Fertilization Pregnancy Embryonic Development Fertilization Human sperm fertilizable

Fertilization, Pregnancy, Embryonic Development

Fertilization • Human sperm fertilizable 48 -72 h after ejac – Isthmic preparation • Human ova fertilizable 24 -48 h after ov’n • Ampulla • Sperm hyaluronidase penetrates corona radiata

• Ovum ZP 3 – Glycoprotein – Recognition • Sperm membr FA-1 – Prot receptor tyr kinase – Act’n autophosph’n cell prot phosph’n – Act’n voltage gated Ca channels AR • Release, act’n acrosin (trypsin-like) – Penetration ZP
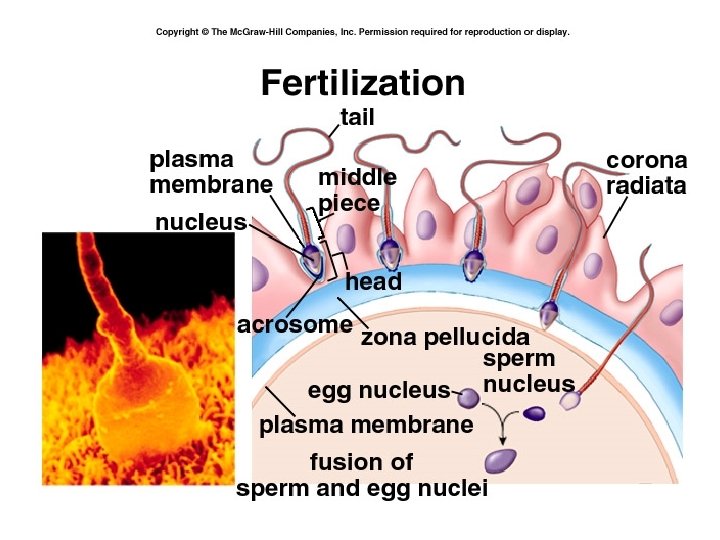

• Sperm head fuses w/ oocyte • 2 nd Meiotic div’n – Mature oocyte + polar body – Mech’s to prevent polyspermy • Fusion male, female pronuclei diploid zygote • Mitosis morula blastocyst • Blastocyst uterus • Implantation dev’t chorion, placenta
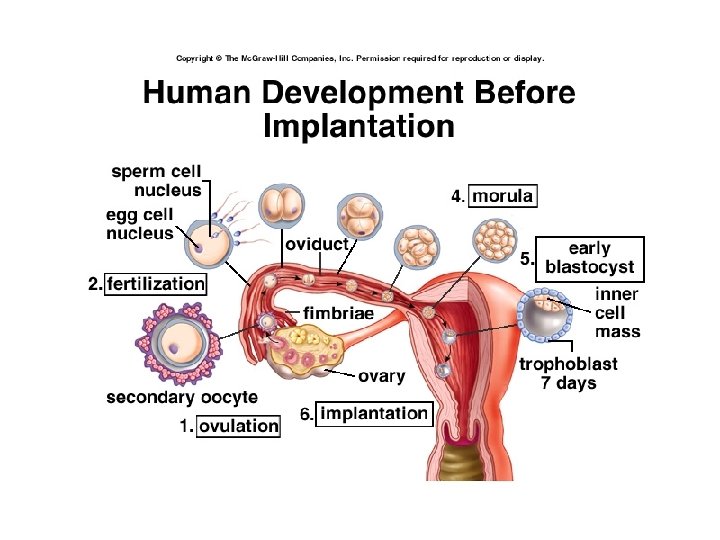

Implantation, Early Embryo Development • Implantation begins 5 -6 d after fert’n (d 21 cycle) – Completed 11 fert’n d – Coincides w/ peak prod’n progesterone by CL (midluteal) • Progesterone impt to preparation decidual, secretory endometrium – If no fert’n, CL would begin decline now

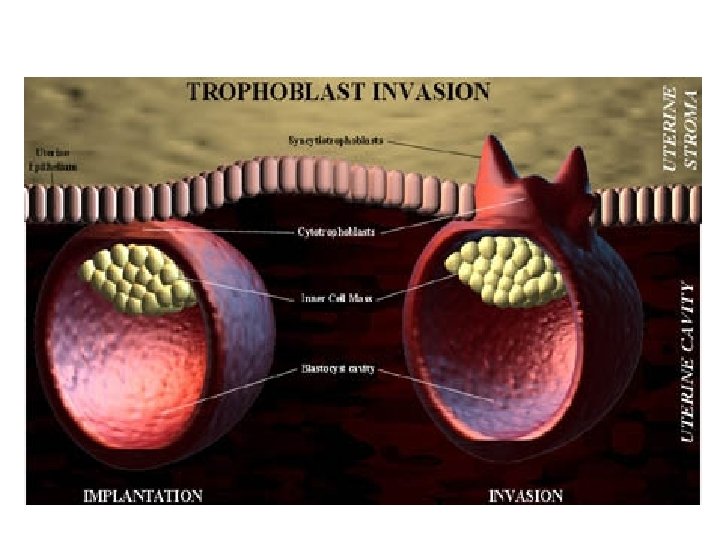
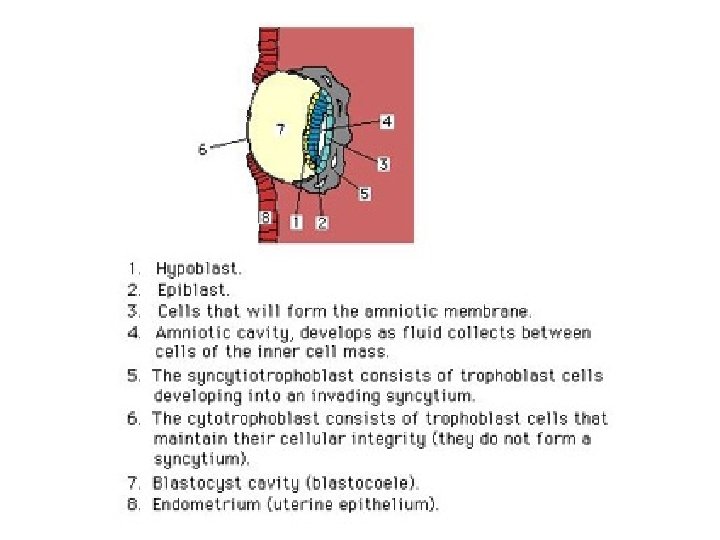
• Inner blastocyst cell mass embryo proper • Outer cells = trophoblasts – Contact, signal uterine epith • EGF receptor on embryo nec • Uterine cell cytokine (LIF) nec – Two cell pop’ns • Syncytiotrophoblasts • Cytotrophoblasts
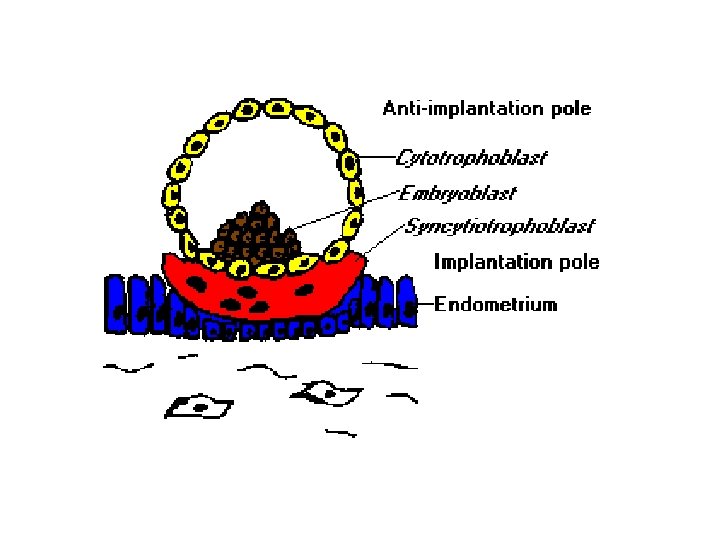

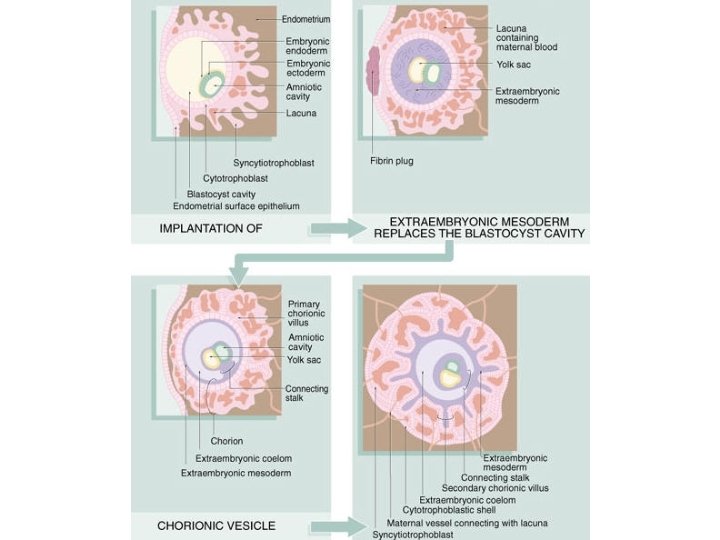
• Syncytiotrophoblast – postmitotic surface layer – From fusion of cytotrophoblast plasma membr’s – Form initial chorionic shell • Erodes endometrial capillaries, veins • Perfused by maternal blood • Cytotrophoblast – mitotic cells – Inner cells = Langhans or villous • Form chorionic villi – Peripheral cells • Form trophoblastic shell • Form trophoblastic cell columns
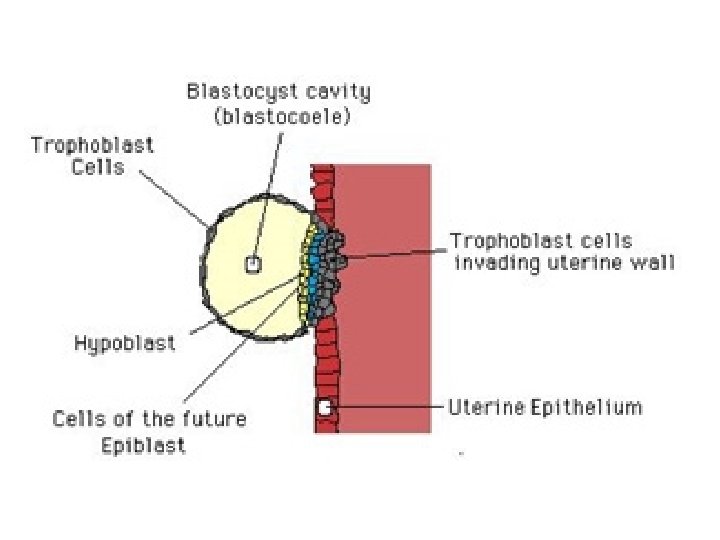

• Syncytiotrophoblast cells secrete h. CG maternal circ’n – Detectable w/in 24 h beginning implantation – Incr’s w/ incr’d trophoblast cell mass (peak end 1 st trimester) – Functions: • Stim’s luteal function • Induces morning sickness – Stim area postrema of brain n/v • Stim’s fetal androgen secr’n – Impt to masculinization of fetal genitalia

• h. CG stim’s luteal function – Incr’s hormone prod’n at CL – Progesterone uninterrupted • Mandatory until parturition – Functioning CL mandatory for maintenance first 7 wks • At 5 wks after fert’n, placental prod’n progesterone sufficient – Hormones @ sustained CL strong neg feedback at ant pit • Plasma FSH, LH suppressed • Gonadotrophs unresponsive to Gn. RH


• Chorionic villi dev by 2 nd week after fert’n – Blood vessels here • Spiral endometrial arteries – Anchors to endometrium, placenta – Development her umbilical cord • Definitive placenta at 11 -12 fert’n wk – Structures can withstand high maternal blood pressure – Incr’d placental perfusion correlates w/ peak plasma h. CG concent’s
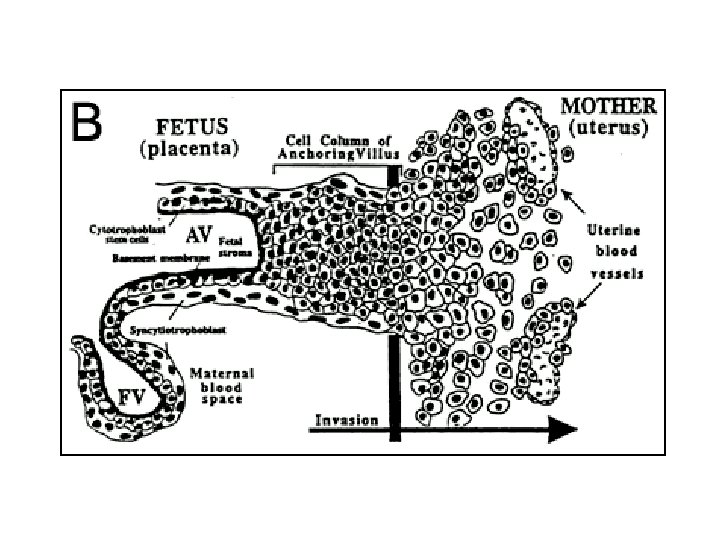
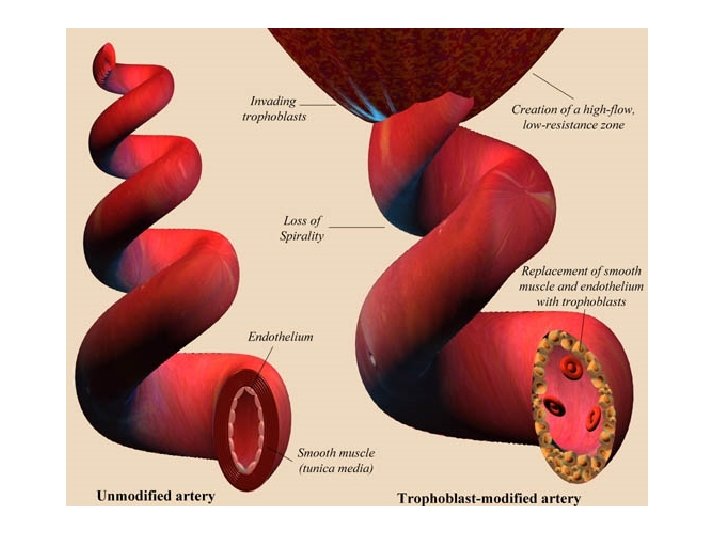

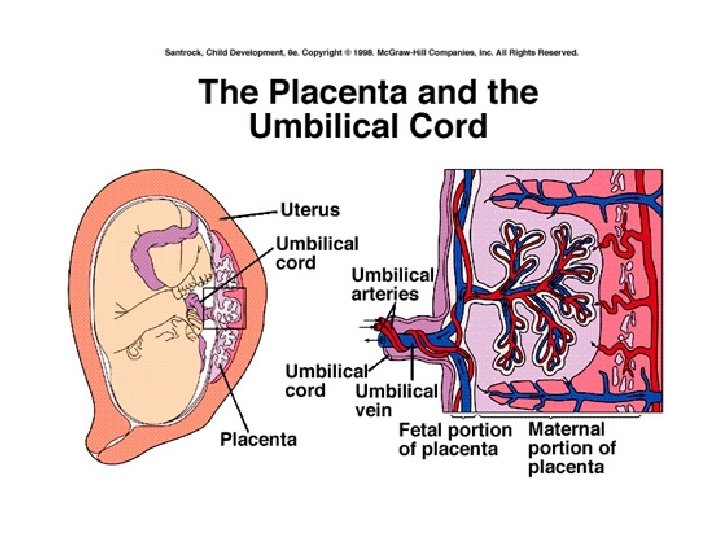
Placenta • Interface between maternal, fetal tissues – Maternal = decidua • Endometrial lining • Falls off at parturition • Supplied by spiral arteries – Fetal cells = trophoblasts • Exchange organ • Barrier
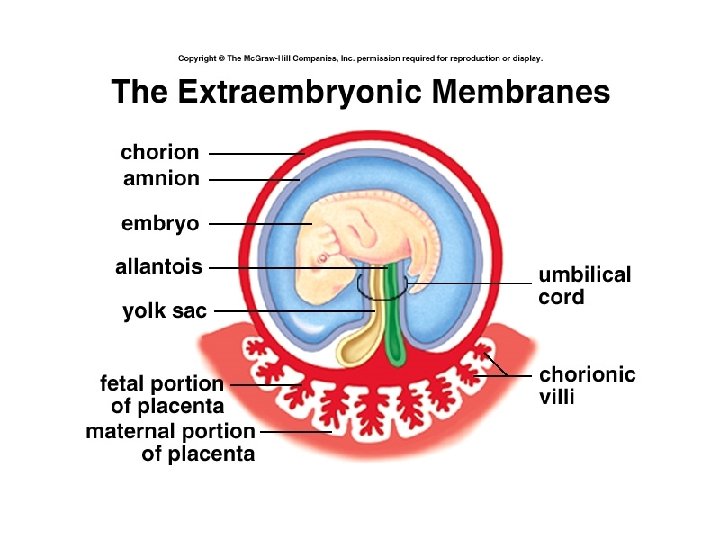
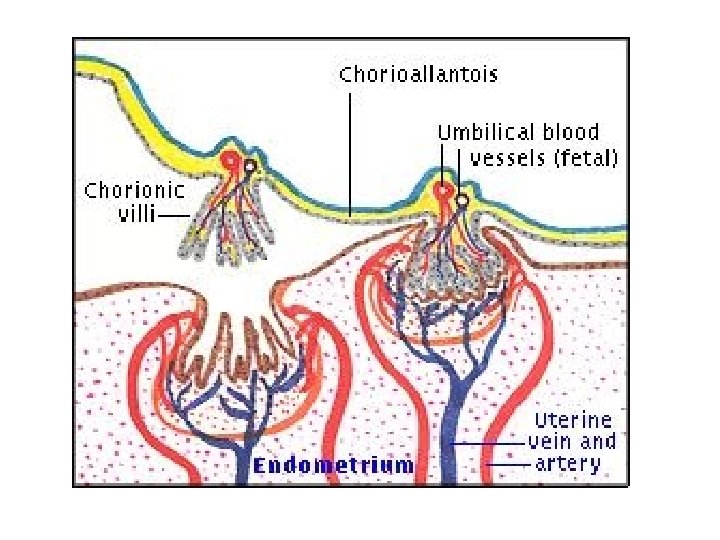
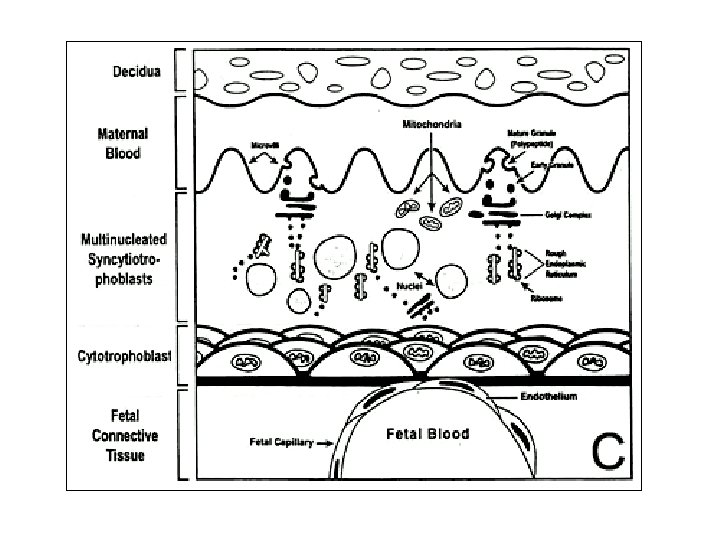

• “Incomplete twin of fetus” – GI, lung, kidney – Immunologic • Transfer immunoglobulins (exc Ig. G) • Prevent fetus rejection – Endocrine • Synth hormones, binding prot’s • Transport hormones • Degrade hormones

• Placenta secretes variant of GH – GH-V – Replaces maternal GH @ 15 -17 w gestation – May promote fetal growth – May be impt to pancreatic islet cells • Causes rising plasma IGF-1 – Neg feedback suppression pit GH

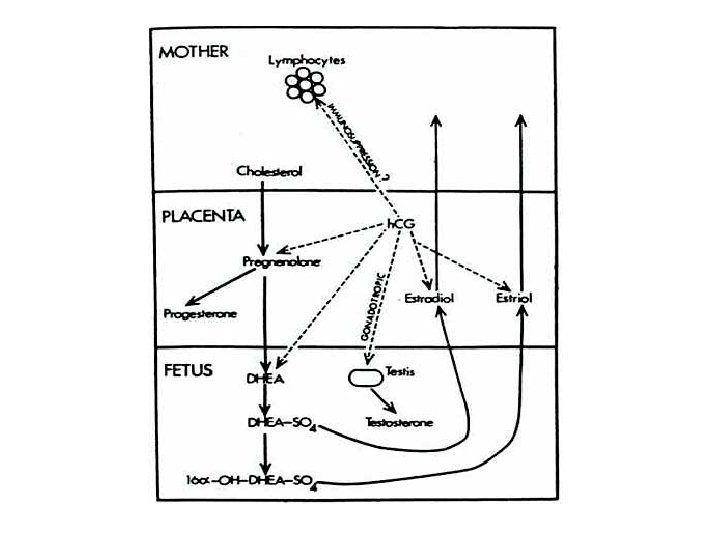
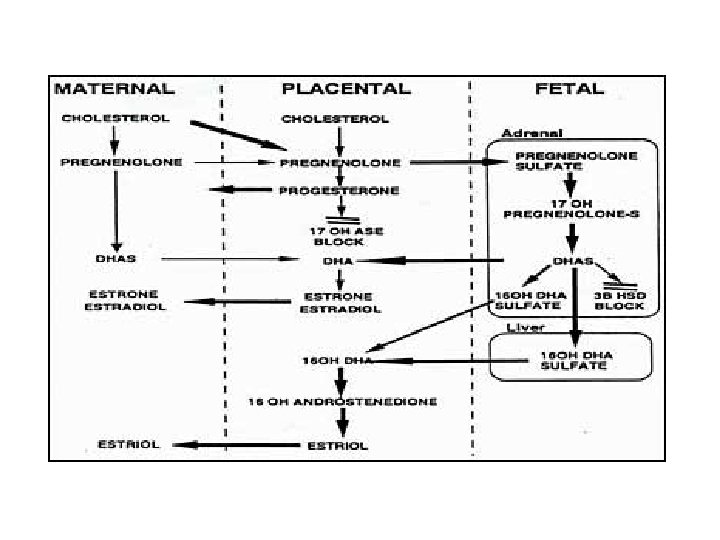
Fetoplacental Unit • Sim to theca lutein, granulosa lutein cooperation in progesterone/E 2 production • 3 Main hormonal groups – Estrogens – Progesterone – Corticosteroids
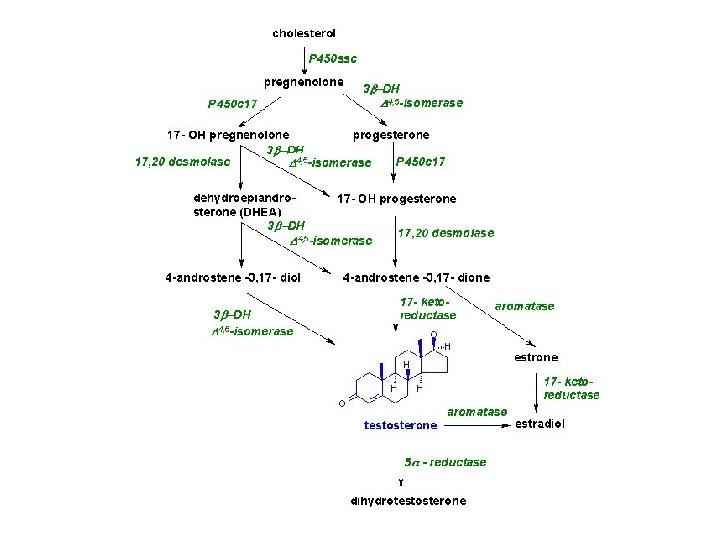

• Estrogens – From androgens by fetal adrenal cortex – Fetus doesn’t express 3 bhydroxysteroid dehydrogenase (isomerase) • So all pregnenolone dehydroepiandrosterone (DHEA) – Placenta doesn’t express p 450 C 17 • Can’t make 17 -OH progesterone • Can’t make androstenedione • Can’t make DHEA – Impt to protection female fetus from androgens – Placenta makes mostly estriol • Sensitizes uterine smooth muscle to oxytocin

• Progesterone – Syncytiotrophoblasts synth de novo • From cholesterol derived from maternal plasma – Placenta expresses much p 450 scc • Tubulovesicular mitochondria • Placenta can’t synthesize cholesterol • Pregnenolone progesterone – Placenta doesn’t express p 450 C 17 • So only progesterone – Enters both fetal, maternal circulations

• Corticosteroids – In fetus, progesterone is precursor to adrenocortical hormones – Glucocorticoids • Gen’ly growth inhibitors, so minimized • Placental enz’s break down maternal glucocort’s – Uses maternal ACTH at fetal adrenal cortex – Diff enzymes expressed @ diff dev’l stages – 25 th gestational week, rising corticosteroids • Impt to feedback mech’s • Impt to organ maturation

Embryonic Development/ Endocrinology • Innate bisexual potential decision to male or female • Sex determination – Chromosomal (Y=male) – Gonadal (testis=male) – Genal (external genitalia) – Sexual/gender identity (psychosocial) – Sexual orientation (attraction)

Chromosomal Sex • Established during fert’n • Fusion male/female pronuclei diploid chromosomal # • Oocyte – X sex chromosome • Sperm – X or Y sex chromosome – Female normal karyotype 46, XX – Male normal karyotype 46, XY

Gonadal Sex • Established during embryonic development – 5 th week – urogenital ridge dev’d • Adjacent adrenal gland – 6 th week – indifferent gonad from urogenital ridge • Requires expression WT-1 gene zinc-finger transcription factor – Nec for gonad, kidney expression (mice) • Requires expression Steroidogenic Factor-1 (SF-1)

• SF-1 – Impt to induction steroidogenic enz’s (mice) – Impt to dev’t adrenal glands, gonads, ventromedial nucleus hypothal (mice) – Impt to dev’t testis from indiff gonad • Stim’s testic differentiation Sertoli cell appearance • Stim’s Sertoli prod’n AMH = Anti. Mullerian Hormone = MIF • Stim’s expression steroidogenic enzymes by dev’ng Leydig cells

Testis Development • Mandatory expression Sex determining Region Y (SRY gene) SRY transcription factor (= Testis Determining Factor (TDF)) – Related to SOX genes that are impt to development cartilage, testis • SRY transcription factor probably suppresses Dosage Sensitive Sex reversal (DSS) gene – DSS suppresses SF 1 – So SRY disinhibition SF-1
• Now SF-1 testicular differentiation – Sertoli cells – Steroidogenic enz’s in Leydig cells – AMH • Mullerian ducts would dev into female tract • AMH inhibition dev’t Mullerian ducts

Sertoli Cells in Developing Testis • Secr’s AMH – 43 -50 d embryonic life – Paracrine – Involution Mullerian duct • Absence AMH Mullerian duct dev’t regardless of sex steroid env – Fallopian tubes, uterus, upper vagina – Normal condition in females
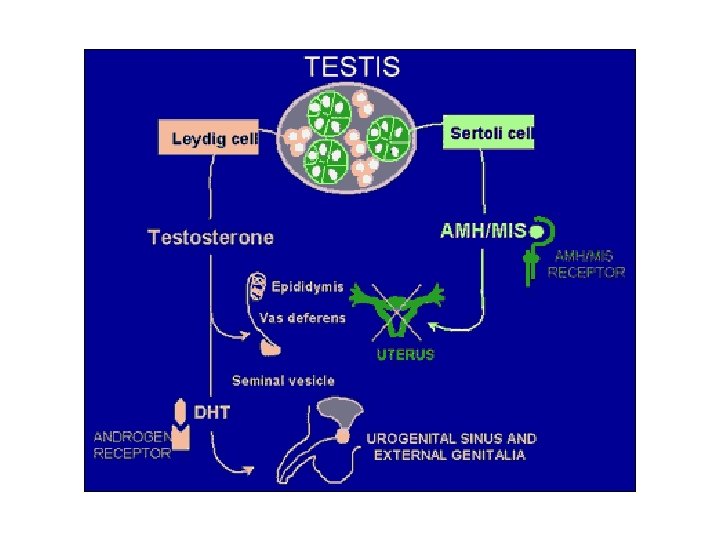

Leydig Cells in Developing Fetus • Secrete testosterone from embryonic d 60 (wk 8 -9) • Not yet controlled by hypothal-hypophyseal system • h. CG crucial – Rising during 1 st trimester – Declines after wk 12 – Stim’s synth testosterone in developing Leydig cells

• Testosterone – Stim’s dev’t Wolffian duct structures • Give rise to epididymis, vas deferens, seminal vesicles – Must be present before embryo wk 12 – Must be converted to DHT for masculinization external genitalia, prostate dev’t
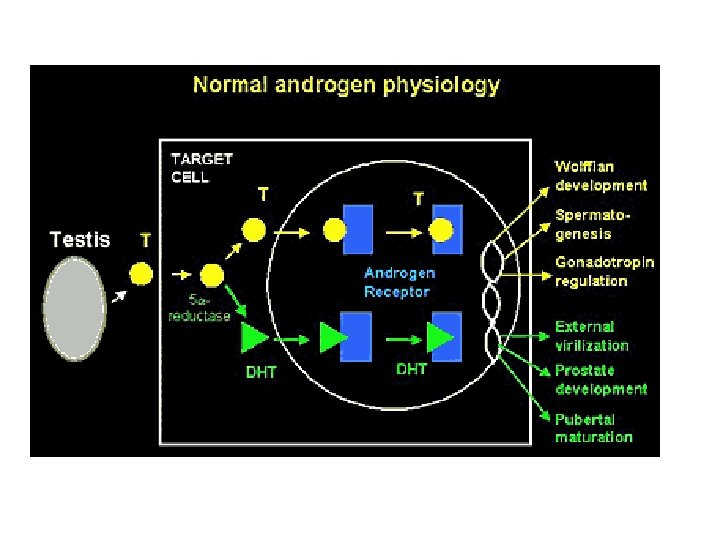

Fetal Gonad Sex Steroid Synthesis • 17 a hydroxylase activity dominant – Pregnenolone 17 a hydroxypregnenolone and 17 a hydroxyprogesterone – androgen synth • Testes testosterone • Ovary androstenedione, testosterone precursors for estrogen – Estradiol
- Slides: 46