Femoral neck fractures Learning objectives Classify femoral neck

Femoral neck fractures

Learning objectives • Classify femoral neck fractures • Outline indications for internal fixation versus arthroplasty • Describe reduction and surgical techniques for internal fixation • Describe potential complications after treatment of femoral neck fractures

Incidence and causes • Elderly: • • • Majority (most commonly in the eighth decade) Low-energy trauma; simple falls Osteoporosis Women 1. 7 million hip fractures annually worldwide • Femoral neck = 53% of all proximal femoral fractures • Young: • Very rare • High-energy trauma • Men

Geriatric patients are problem patients • Disturbed physiological equilibrium • Reduced cognitive functions • Reduced mobility • Disturbed microcirculation • Substance abuse (eg, alcohol, antidepressants) • Pathological bone stock, especially osteoporosis High morbidity
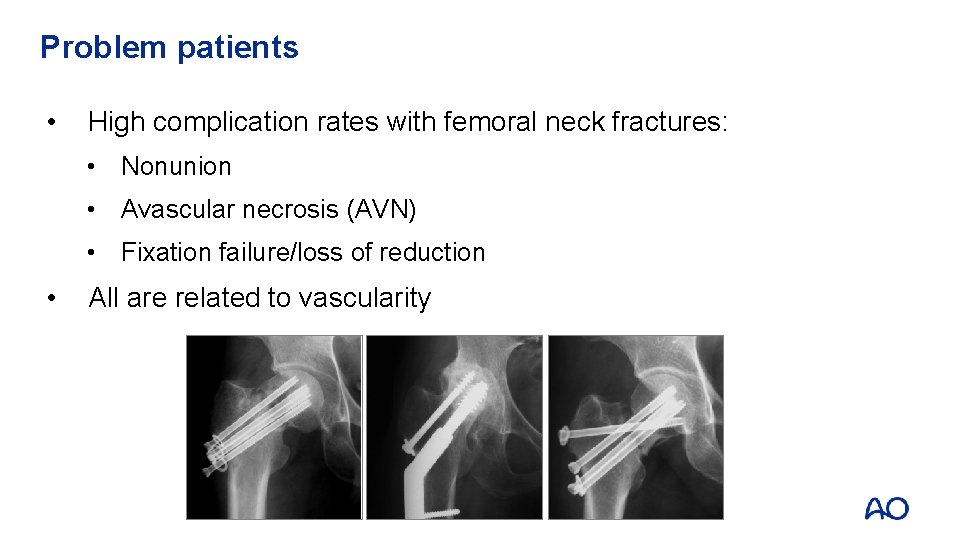
Problem patients • High complication rates with femoral neck fractures: • Nonunion • Avascular necrosis (AVN) • Fixation failure/loss of reduction • All are related to vascularity
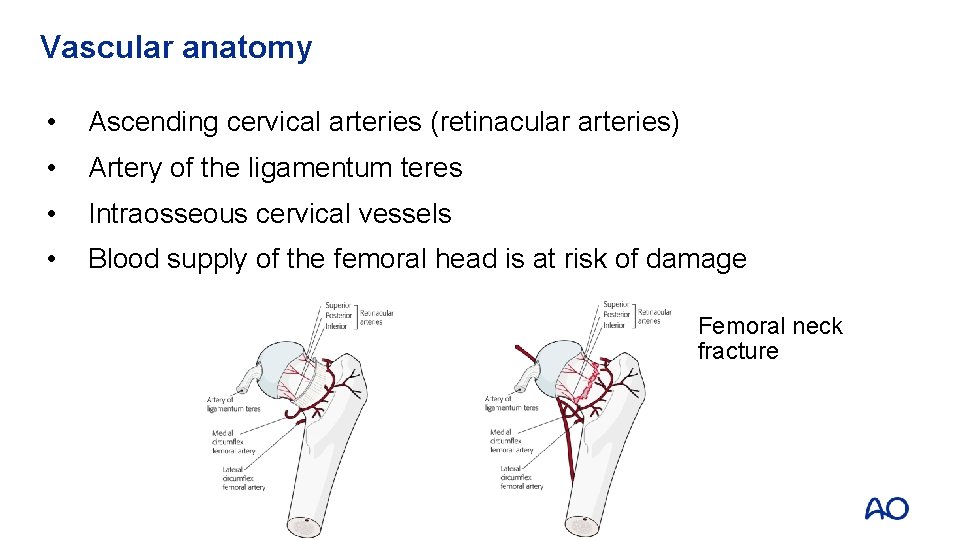
Vascular anatomy • Ascending cervical arteries (retinacular arteries) • Artery of the ligamentum teres • Intraosseous cervical vessels • Blood supply of the femoral head is at risk of damage Femoral neck fracture
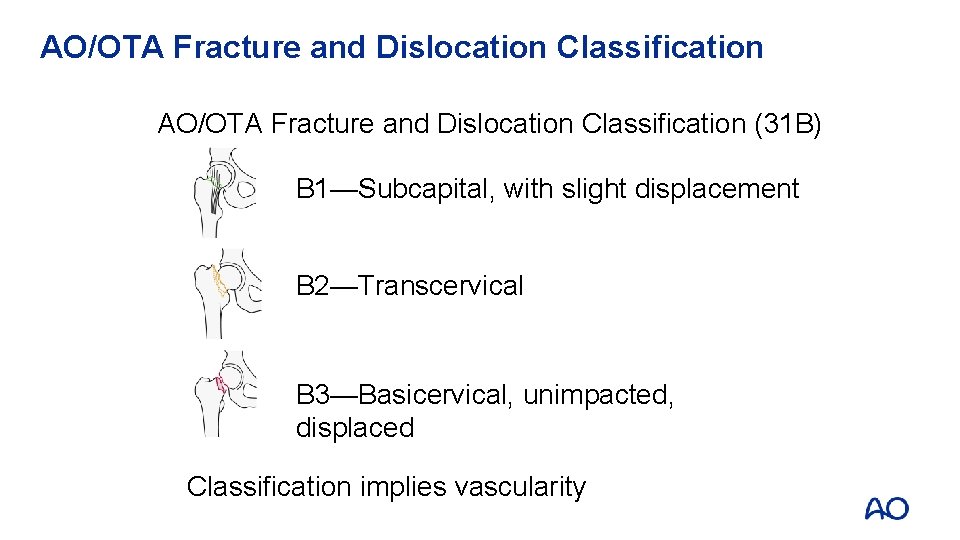
AO/OTA Fracture and Dislocation Classification (31 B) B 1—Subcapital, with slight displacement B 2—Transcervical B 3—Basicervical, unimpacted, displaced Classification implies vascularity
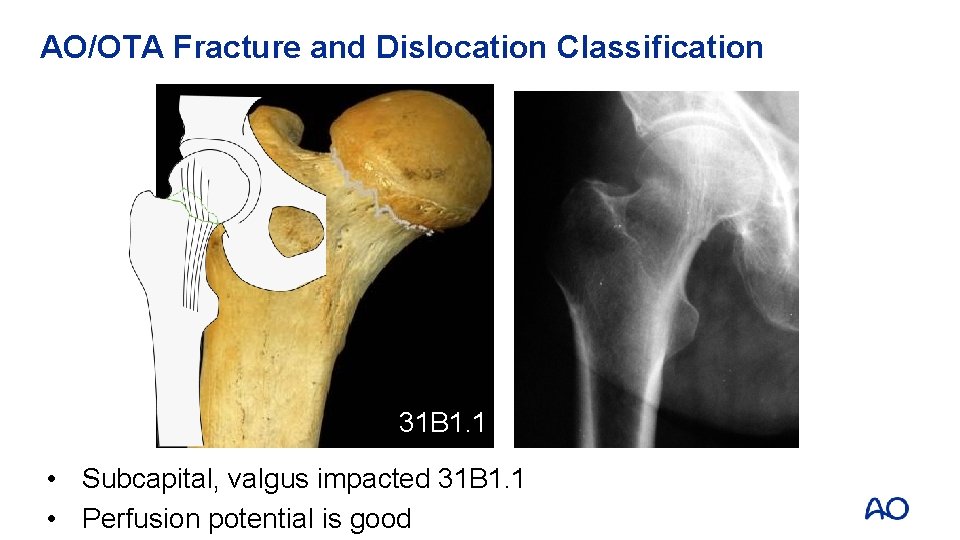
AO/OTA Fracture and Dislocation Classification 31 B 1. 1 • Subcapital, valgus impacted 31 B 1. 1 • Perfusion potential is good
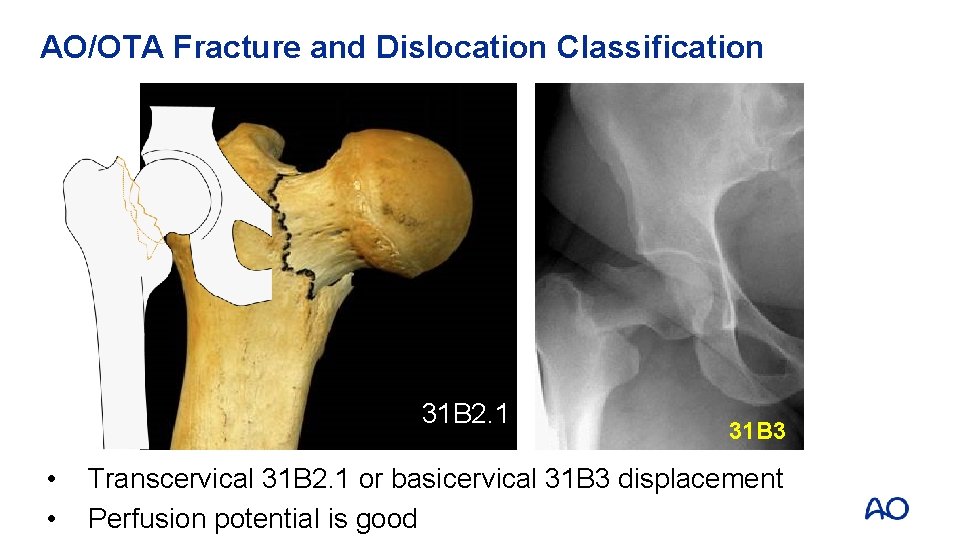
AO/OTA Fracture and Dislocation Classification 31 B 2. 1 • • 31 B 3 Transcervical 31 B 2. 1 or basicervical 31 B 3 displacement Perfusion potential is good
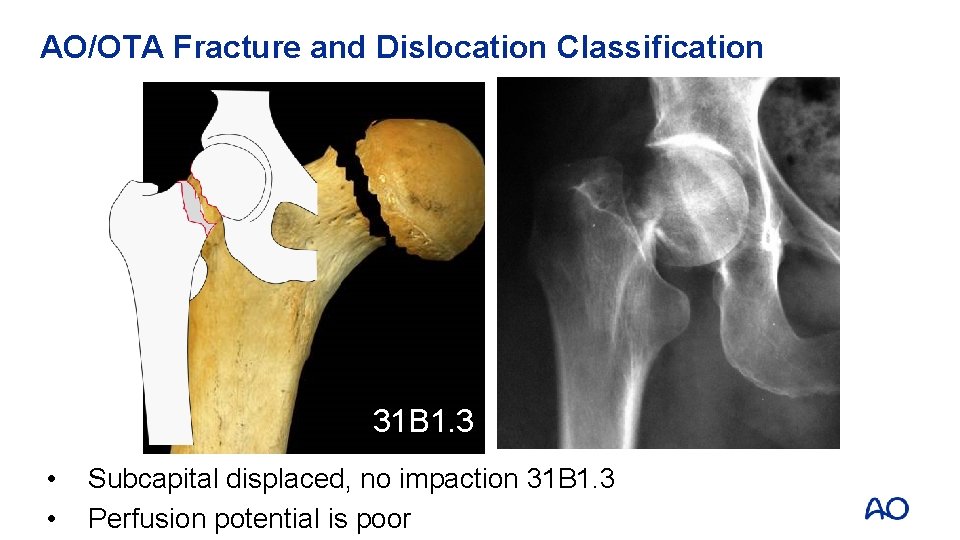
AO/OTA Fracture and Dislocation Classification 31 B 1. 3 • • Subcapital displaced, no impaction 31 B 1. 3 Perfusion potential is poor
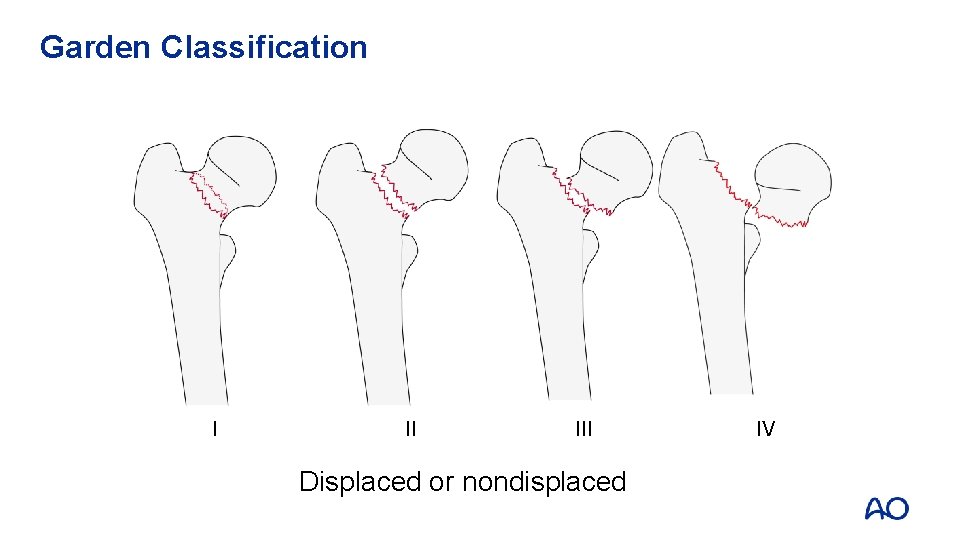
Garden Classification I II III Displaced or nondisplaced IV
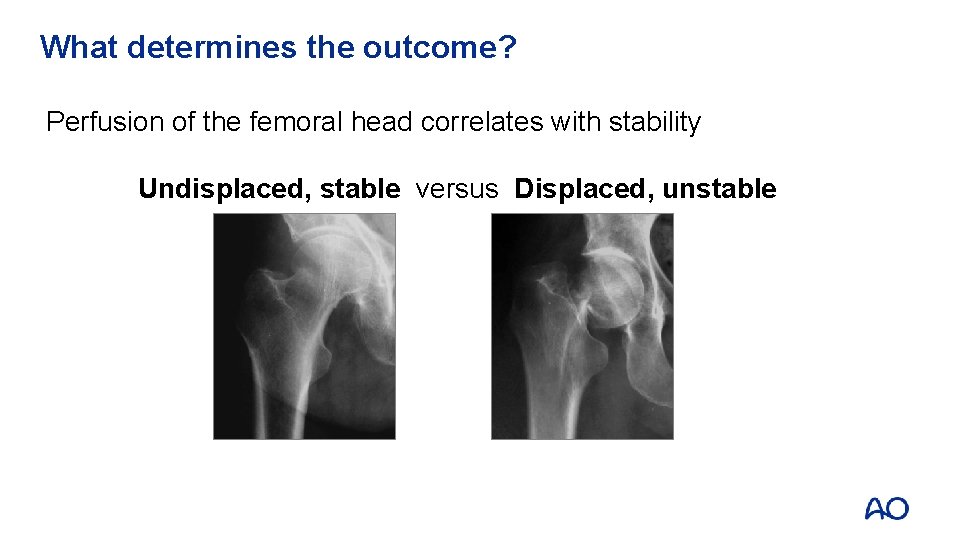
What determines the outcome? Perfusion of the femoral head correlates with stability Undisplaced, stable versus Displaced, unstable
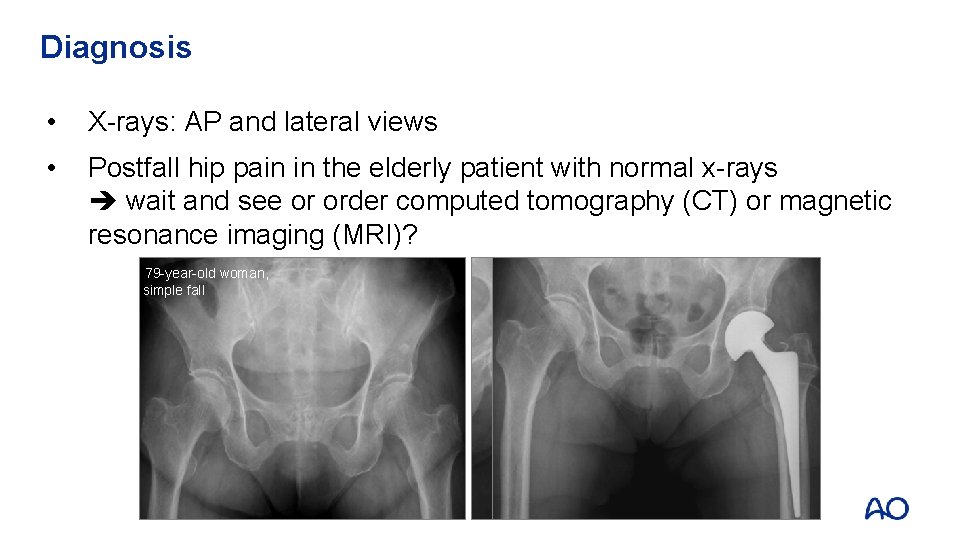
Diagnosis • X-rays: AP and lateral views • Postfall hip pain in the elderly patient with normal x-rays wait and see or order computed tomography (CT) or magnetic resonance imaging (MRI)? 79 -year-old woman, simple fall 15 days later
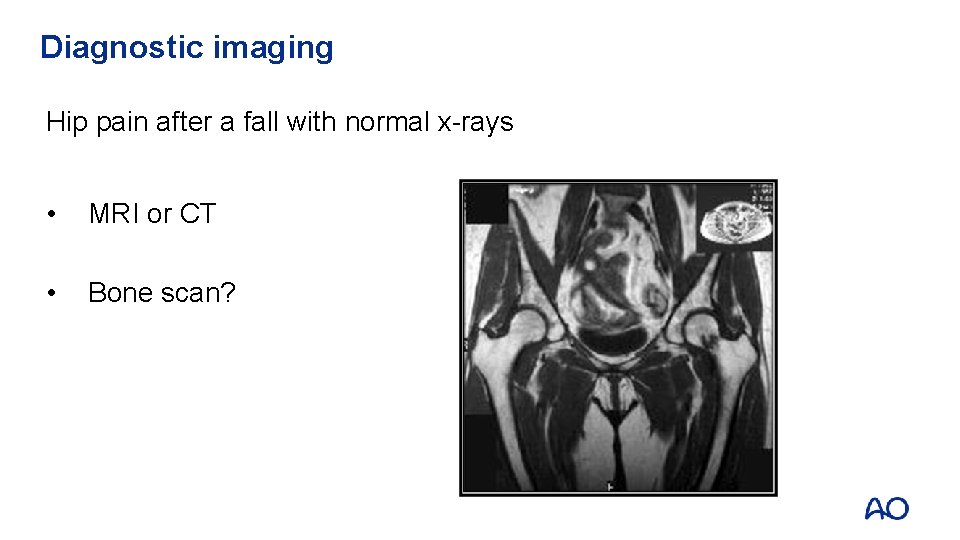
Diagnostic imaging Hip pain after a fall with normal x-rays • MRI or CT • Bone scan?
Timing of surgery Reduction and fixation as quickly as possible: • In young patients • In medically stable, elderly patients • Surgical urgency: • Trend toward better outcome with earlier surgery
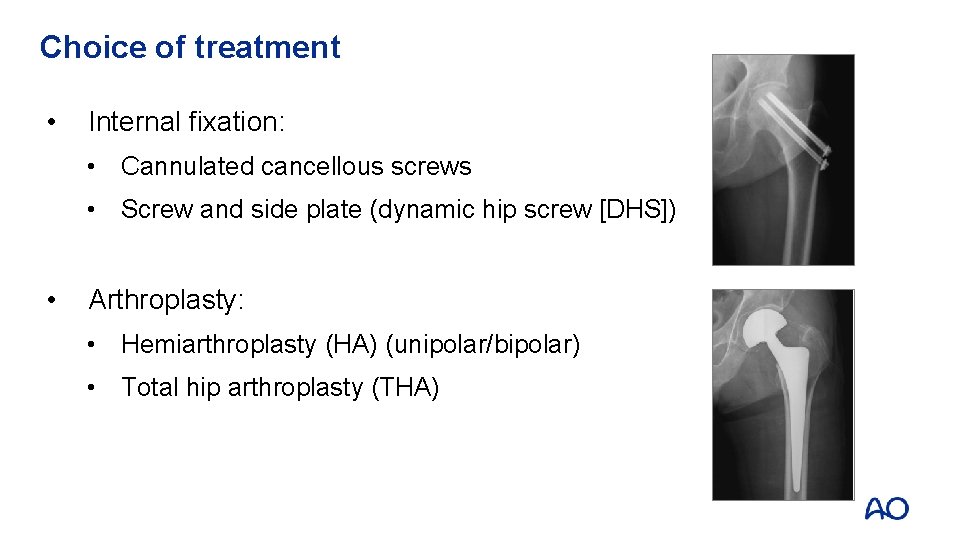
Choice of treatment • Internal fixation: • Cannulated cancellous screws • Screw and side plate (dynamic hip screw [DHS]) • Arthroplasty: • Hemiarthroplasty (HA) (unipolar/bipolar) • Total hip arthroplasty (THA)
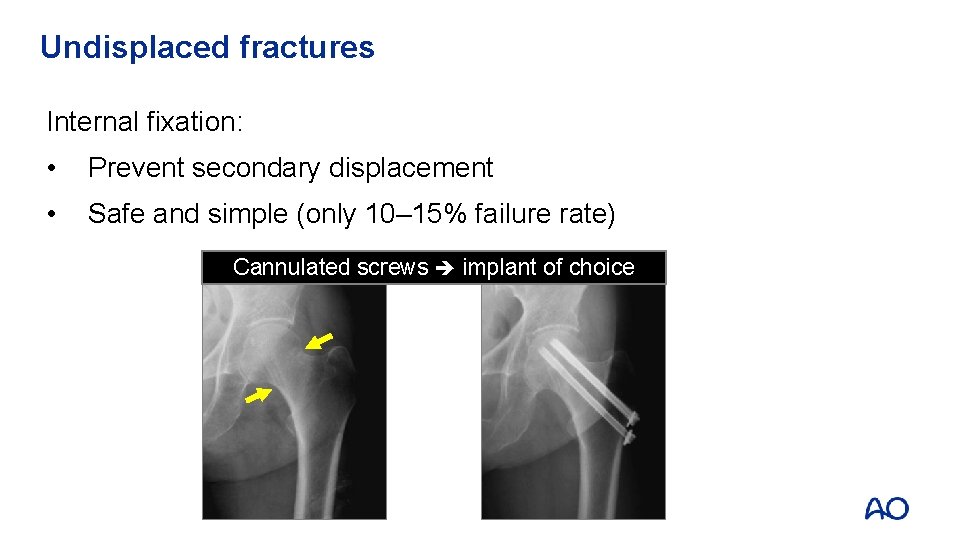
Undisplaced fractures Internal fixation: • Prevent secondary displacement • Safe and simple (only 10– 15% failure rate) Cannulated screws implant of choice
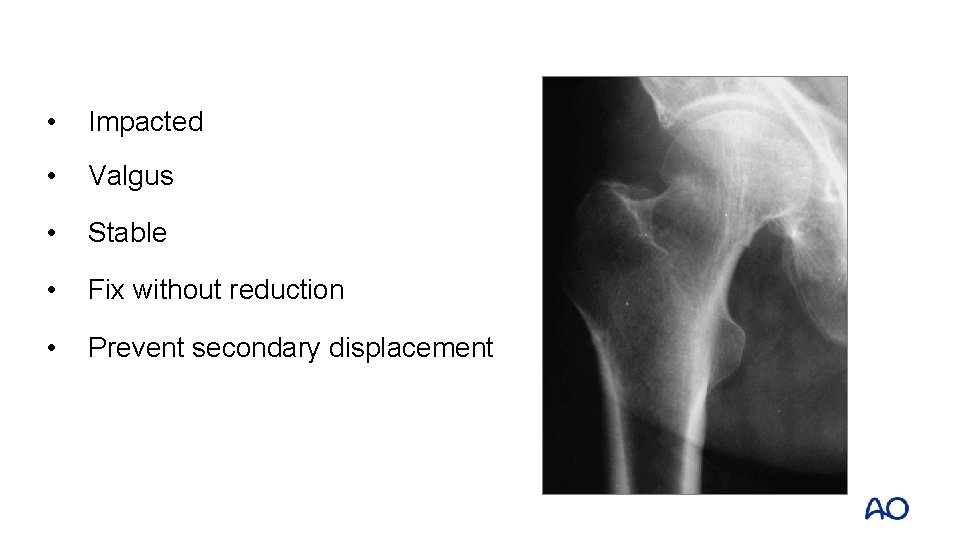
• Impacted • Valgus • Stable • Fix without reduction • Prevent secondary displacement
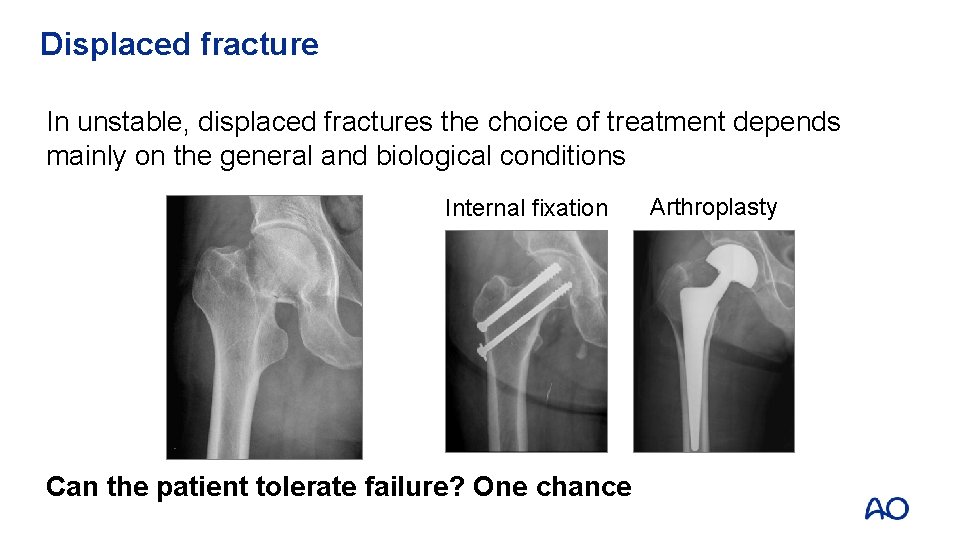
Displaced fracture In unstable, displaced fractures the choice of treatment depends mainly on the general and biological conditions Internal fixation Can the patient tolerate failure? One chance Arthroplasty
Internal fixation • Internal fixation is the treatment of choice for patients with high functional demands and good bone stock • Patients less than 65 years old and do not have a chronic illness Early reduction and internal fixation Decrease AVN of the femoral head
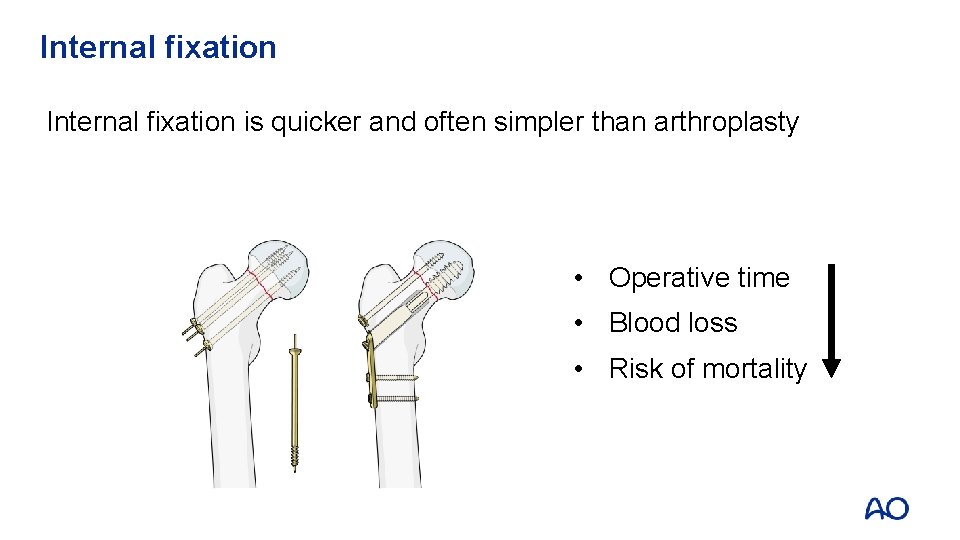
Internal fixation is quicker and often simpler than arthroplasty • Operative time • Blood loss • Risk of mortality
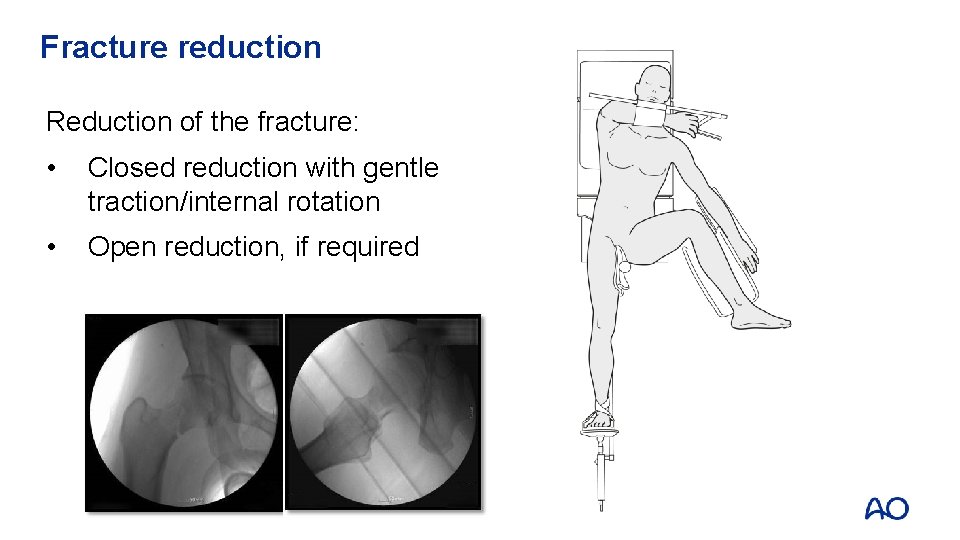
Fracture reduction Reduction of the fracture: • Closed reduction with gentle traction/internal rotation • Open reduction, if required
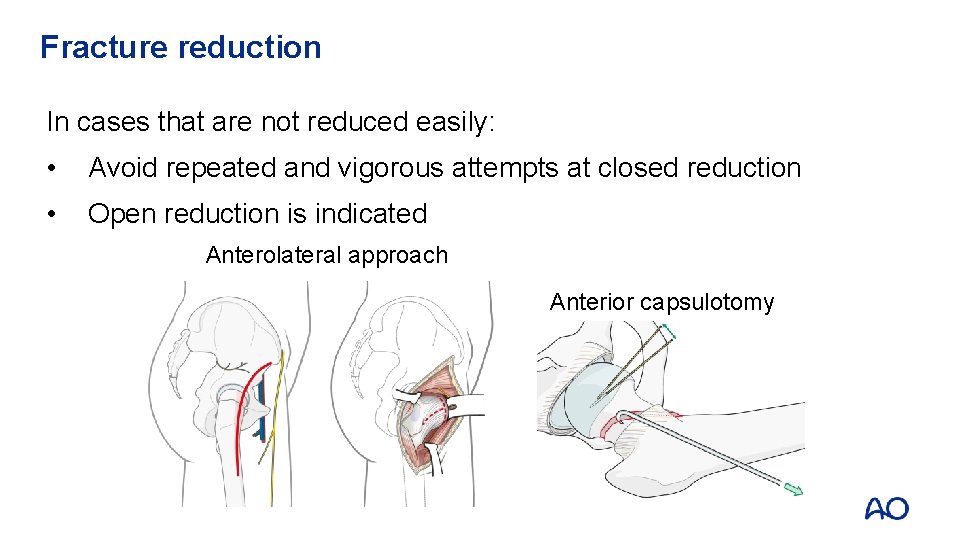
Fracture reduction In cases that are not reduced easily: • Avoid repeated and vigorous attempts at closed reduction • Open reduction is indicated Anterolateral approach Anterior capsulotomy
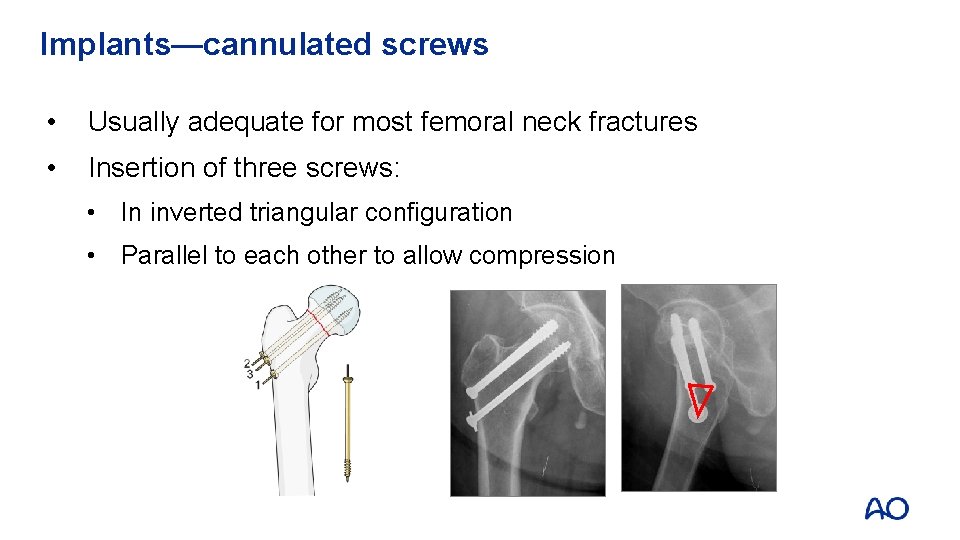
Implants—cannulated screws • Usually adequate for most femoral neck fractures • Insertion of three screws: • In inverted triangular configuration • Parallel to each other to allow compression
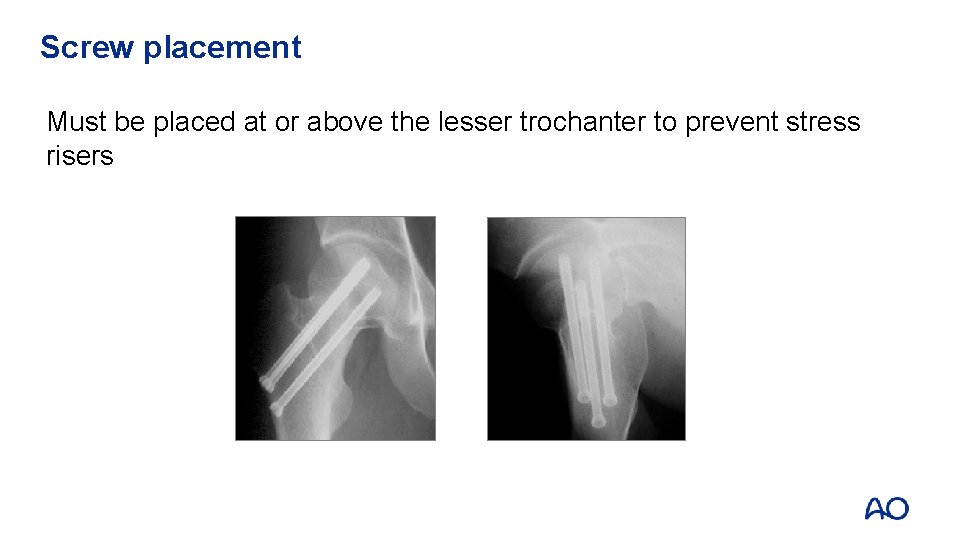
Screw placement Must be placed at or above the lesser trochanter to prevent stress risers
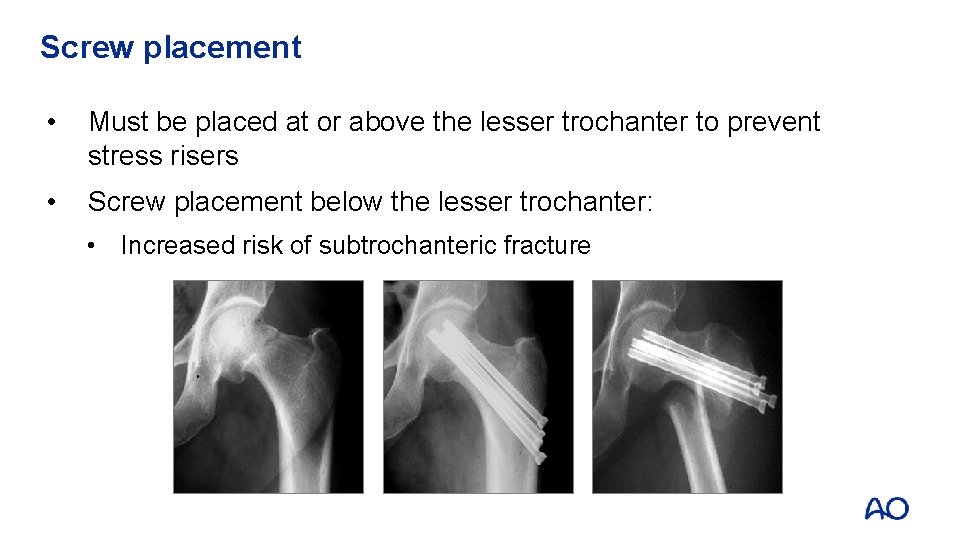
Screw placement • Must be placed at or above the lesser trochanter to prevent stress risers • Screw placement below the lesser trochanter: • Increased risk of subtrochanteric fracture
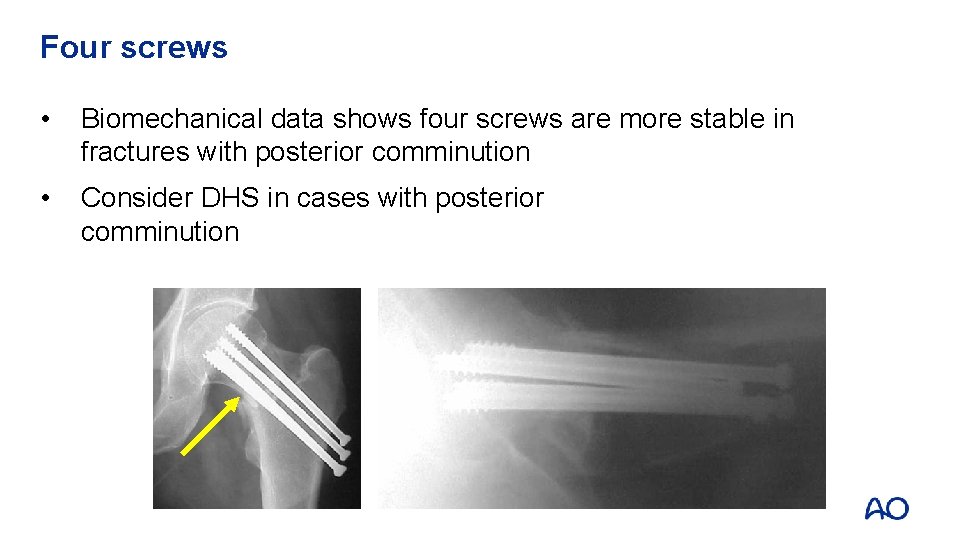
Four screws • Biomechanical data shows four screws are more stable in fractures with posterior comminution • Consider DHS in cases with posterior comminution
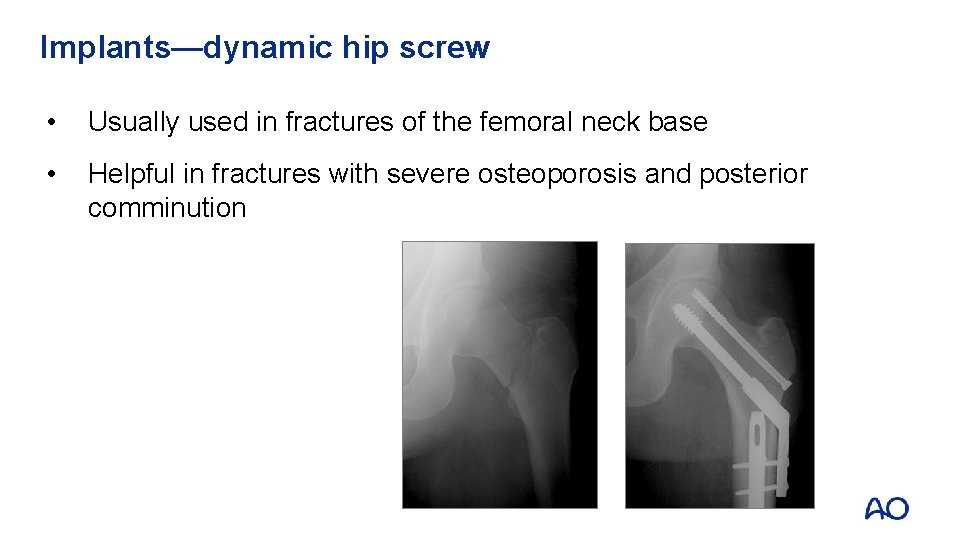
Implants—dynamic hip screw • Usually used in fractures of the femoral neck base • Helpful in fractures with severe osteoporosis and posterior comminution
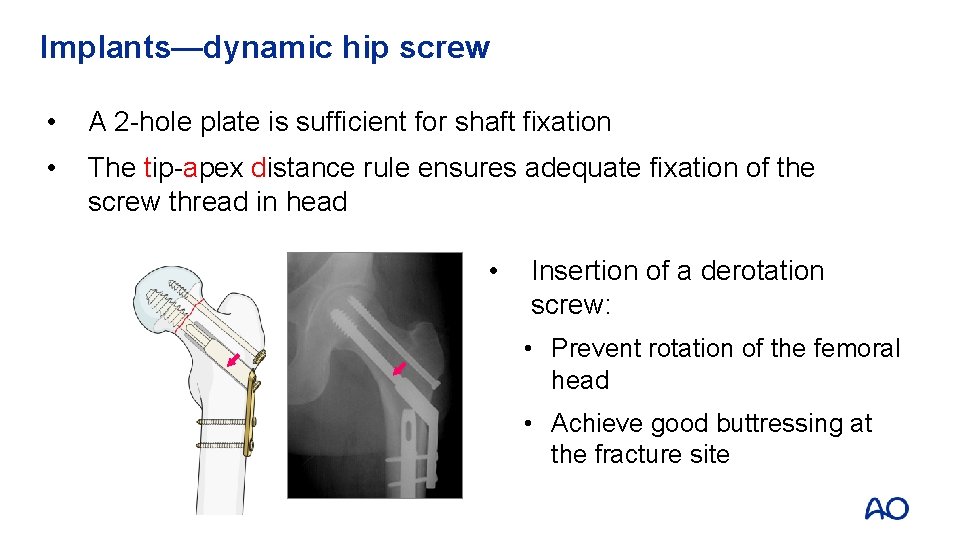
Implants—dynamic hip screw • A 2 -hole plate is sufficient for shaft fixation • The tip-apex distance rule ensures adequate fixation of the screw thread in head • Insertion of a derotation screw: • Prevent rotation of the femoral head • Achieve good buttressing at the fracture site
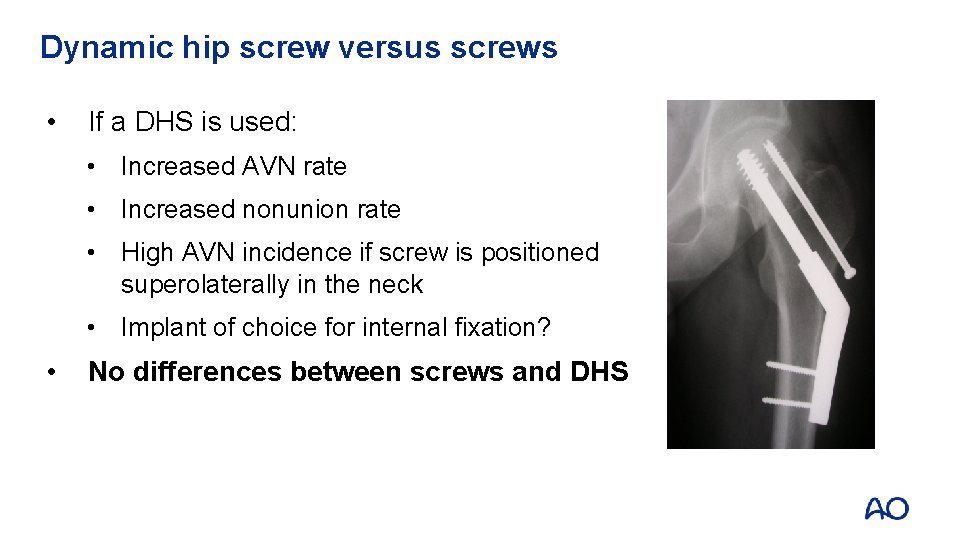
Dynamic hip screw versus screws • If a DHS is used: • Increased AVN rate • Increased nonunion rate • High AVN incidence if screw is positioned superolaterally in the neck • Implant of choice for internal fixation? • No differences between screws and DHS
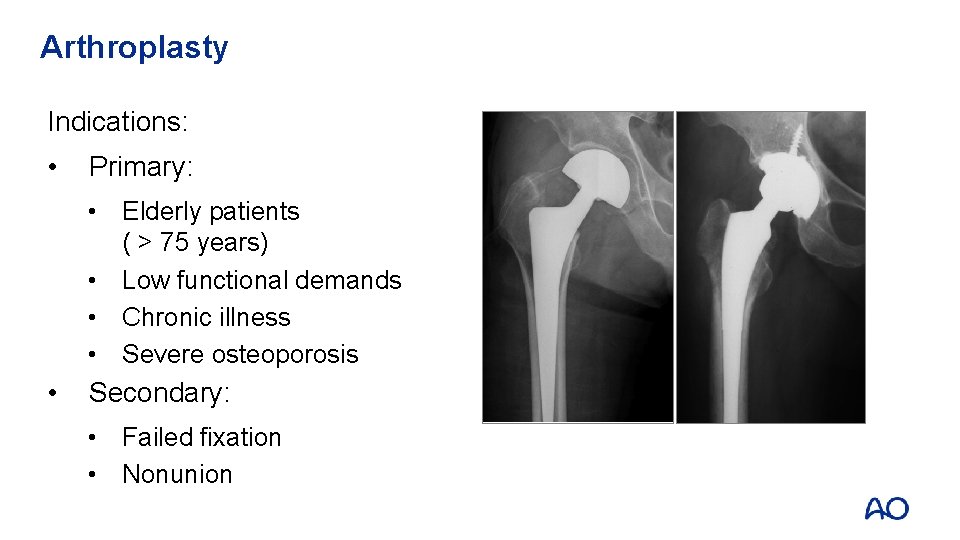
Arthroplasty Indications: • Primary: • Elderly patients ( > 75 years) • Low functional demands • Chronic illness • Severe osteoporosis • Secondary: • Failed fixation • Nonunion

Arthroplasty Advantages: • Allows immediate weight bearing • Eliminate AVN and nonunion • Significantly reduces the incidence of reoperation
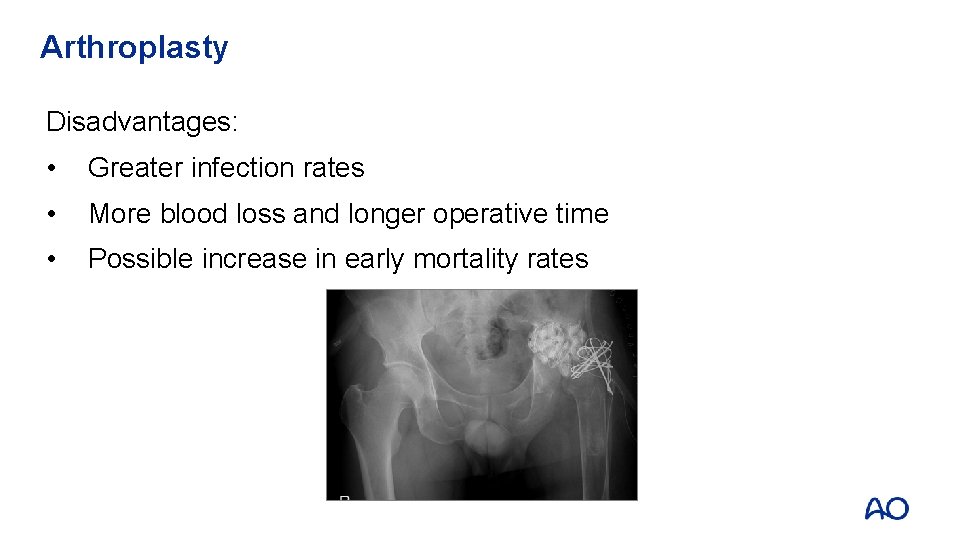
Arthroplasty Disadvantages: • Greater infection rates • More blood loss and longer operative time • Possible increase in early mortality rates

Hemiarthroplasty versus total hip arthroplasty • Less pain with THA • Greater mobility with THA • Lower revision rate with THA • More frequent dislocation in early stage with THA : • Patients with preexisting hip disease • Active, healthy patients without preexisting hip disease

Internal fixation versus arthroplasty—metaanalysis Internal fixation versus arthroplasty for displaced fractures of the femoral neck: • Early mortality: a trend toward increased mortality 4 months after arthroplasty • Revision surgery: significantly reduced risk of revision surgery with arthroplasty • Infection: significantly increased risk of infection with arthroplasty

Factors that influence decision making • Patient factors: • Osteoporosis • Medical comorbidities • Preinjury functional status • Fracture factors: • Displacement • Comminution • Some factors can not be controlled by surgeons
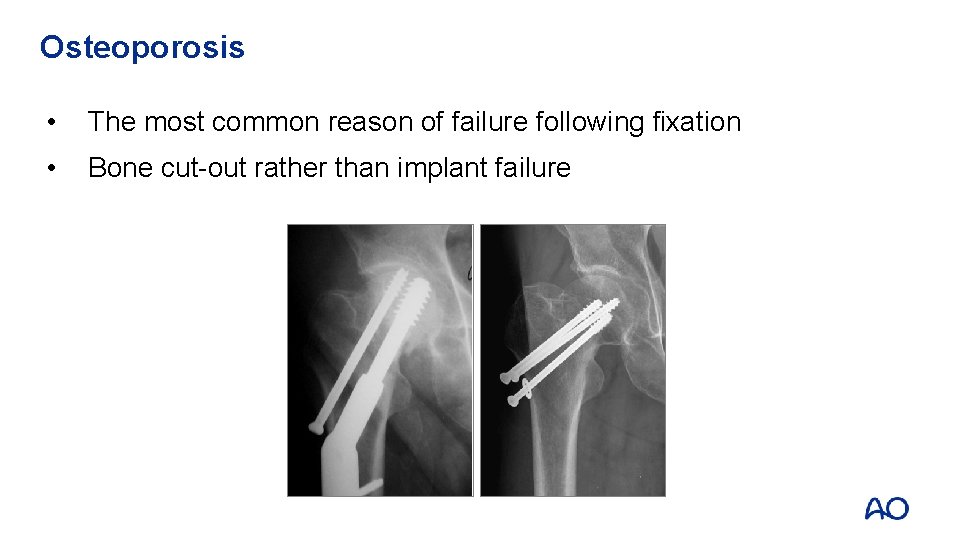
Osteoporosis • The most common reason of failure following fixation • Bone cut-out rather than implant failure

Medical comorbidity • Diabetes, heart disease, cerebral dysfunction, visual abnormality, prior skeletal injury, depression • Elderly patients with a displaced femoral neck fracture and multiple comorbidities • At higher risk for outcome failure

Preinjury functional status and age • Patients 65 years old or younger urgent anatomical reduction/internal fixation • Patients older than 75 years arthroplasty • Patients between 65 and 75 years (gray zone) • Decision must be based individually on patient factors • Physiological age is a better criterion than chronological age in deciding on HA
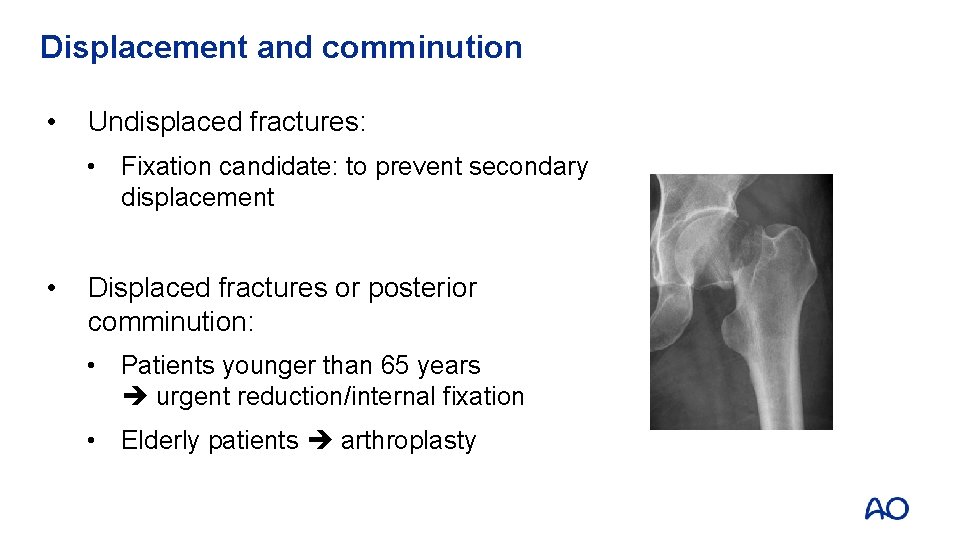
Displacement and comminution • Undisplaced fractures: • Fixation candidate: to prevent secondary displacement • Displaced fractures or posterior comminution: • Patients younger than 65 years urgent reduction/internal fixation • Elderly patients arthroplasty

Decision-making criteria Fixation versus hip replacement: • Age and fitness of the patient • Level of activity • Comorbid diseases (including hip osteoarthritis) • Displacement of the fracture • Quality of bone • Time since injury • Available implants • Surgeon’s experience

Take-home messages • Valgus impacted heads require fixation in situ • Displaced heads have higher rate of complications • Closed reduction achieved in most cases • Fixation options are three screws or DHS plus antirotation screw • Arthroplasty is indicated in the elderly when fracture is displaced 42
- Slides: 42