Femoral neck fractures different patients different problems AO

Femoral neck fractures; different patients, different problems AO Trauma Advanced Principles Course

Learning objectives • Specify the patient factors that influence indication decisions • Compare closed reduction versus open reduction with correct alignment and describe surgical approaches to achieve this • Explain reasons for choosing different implants available for femoral neck fractures • Evaluate and plan appropriate fixation techniques • Consider repair versus replacement in the elderly patient • List key outcome publications

Fracture classification Undisplaced Displaced • Easy to treat • Unstable • Easy to fix • Need for reduction • Low complication rate • • ORIF with better results Risk of avascular necrosis • Risk of implant failure (cut out) • Risk of nonunion
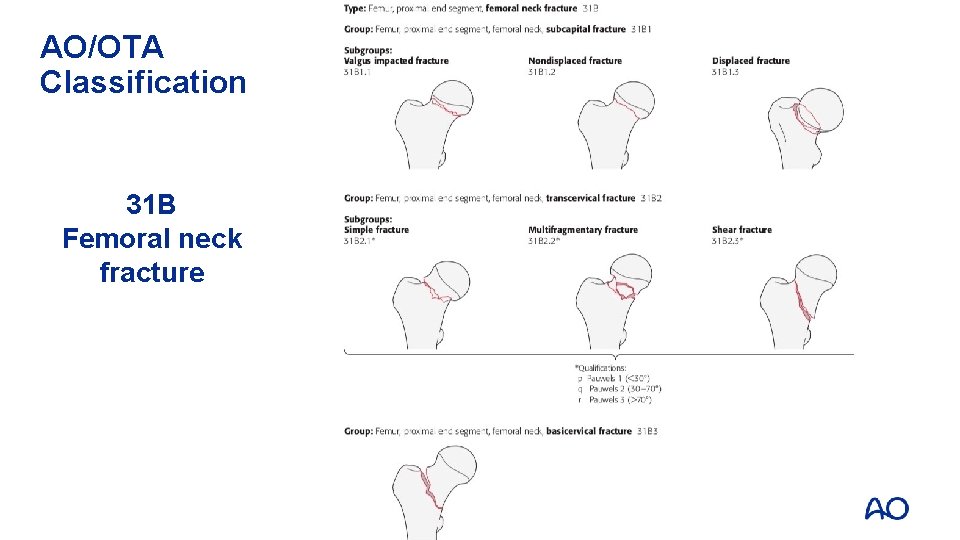
AO/OTA Classification 31 B Femoral neck fracture

Patients Young Old • High-energy trauma • Low-energy trauma • Polytrauma • Single trauma • Associated shaft fracture • Osteoporosis • High complication rate • Multimorbidity • Fixing, preserving joint • Mental disorder • As soon as possible • Hemostasis (med) • Every dislocated fracture • Heart disease

Methods ORIF Endoprothesis • Screws • Monopolar • Pins • Bipolar • Sliding hip screw • Total hip arthroplasty (THA) • Intramedullary device • Cemented • Uncemented

Advantages ORIF Endoprothesis • Preserves bone and joint • Fewer reoperations • Less invasive • More predictable function • Small approach • Less blood loss • Low infection rate • No cardiovascular harm • Fast preparation

Disadvantages ORIF Endoprothesis • Higher risk of reoperation • • Less predictable results Cardio-respiratory complications • Loss of joint and bone • Complex surgery • Complications more significant

Timing of operation Young patients Old patients • Minimize risk of avascular necrosis • Goal is early mobilization • Within 48 hours • Surgery as early as possible • Better within 24 hours • Joint decompression may be of value • Take care of dementia • Coagulation management • Prophylaxis of delirium • Structures and organization

ORIF/technique • As early as possible • Traction table optional • Anatomical reduction (most important) • Closed manipulation, internal rotation, pressing from anterior • Open reduction (Smith-Peterson or Watson-Jones approaches) • Provisional fixation with 2. 0 mm K-wires • Three screws or DHS • No solid evidence for choice of implant
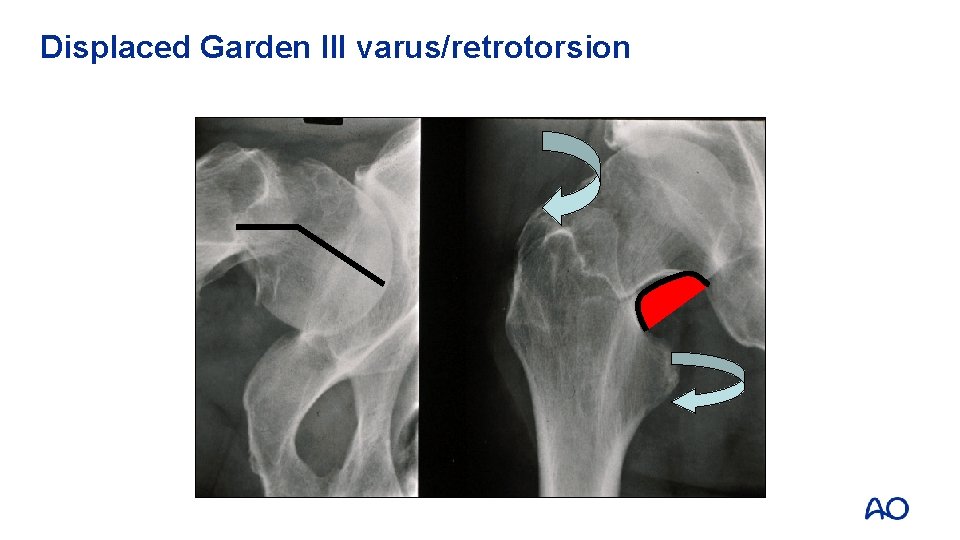
Displaced Garden III varus/retrotorsion
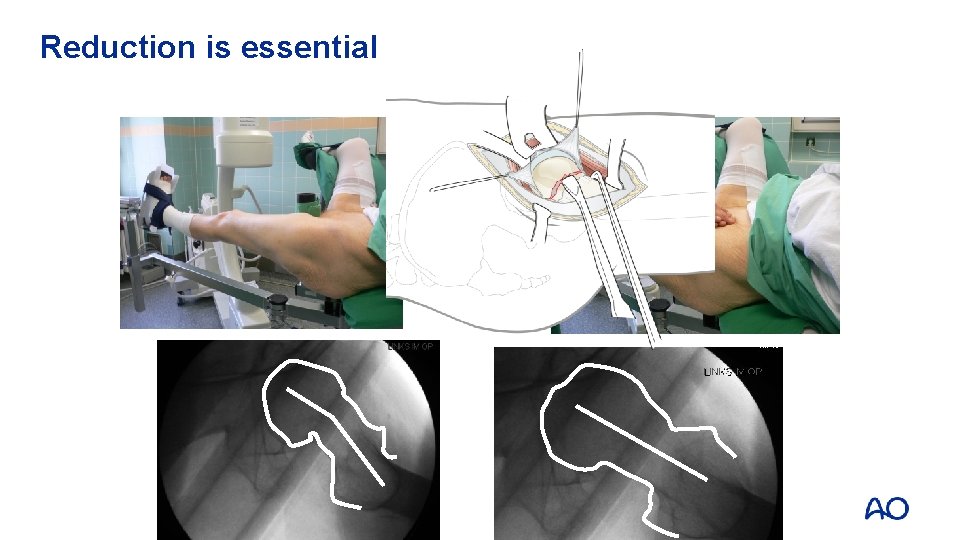
Reduction is essential
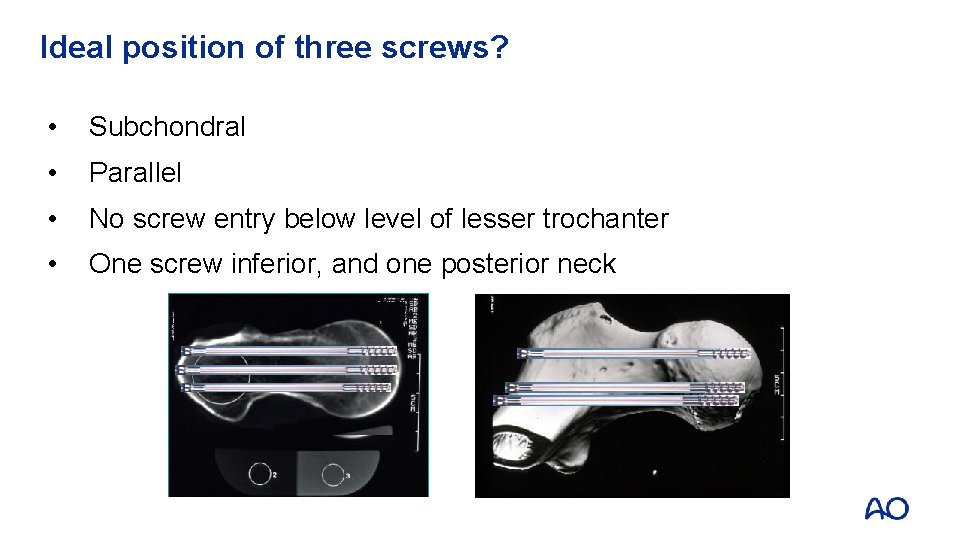
Ideal position of three screws? • Subchondral • Parallel • No screw entry below level of lesser trochanter • One screw inferior, and one posterior neck
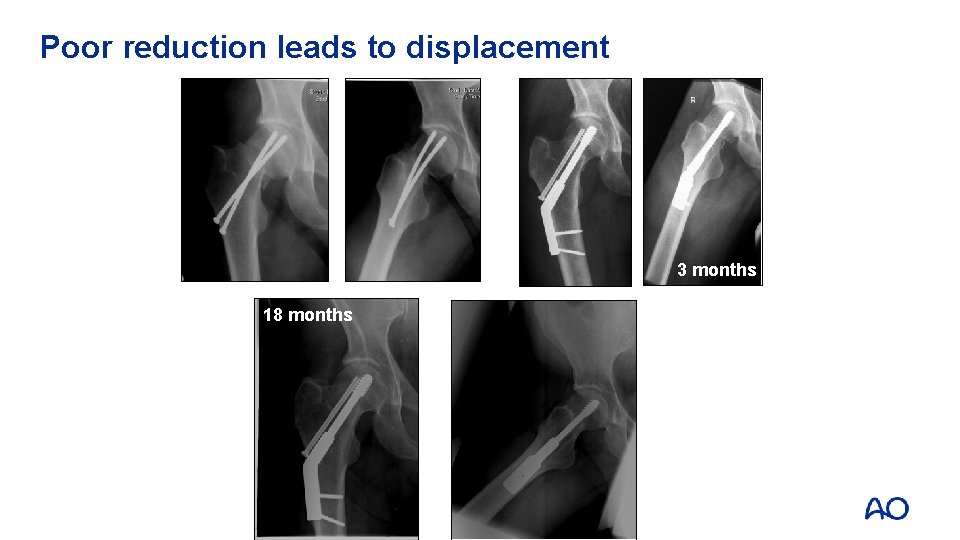
Poor reduction leads to displacement 3 months 18 months
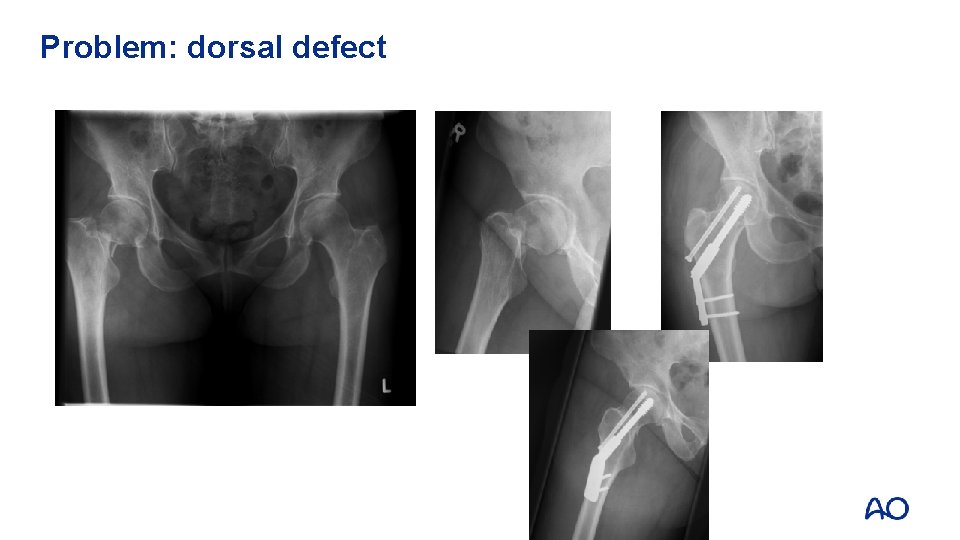
Problem: dorsal defect
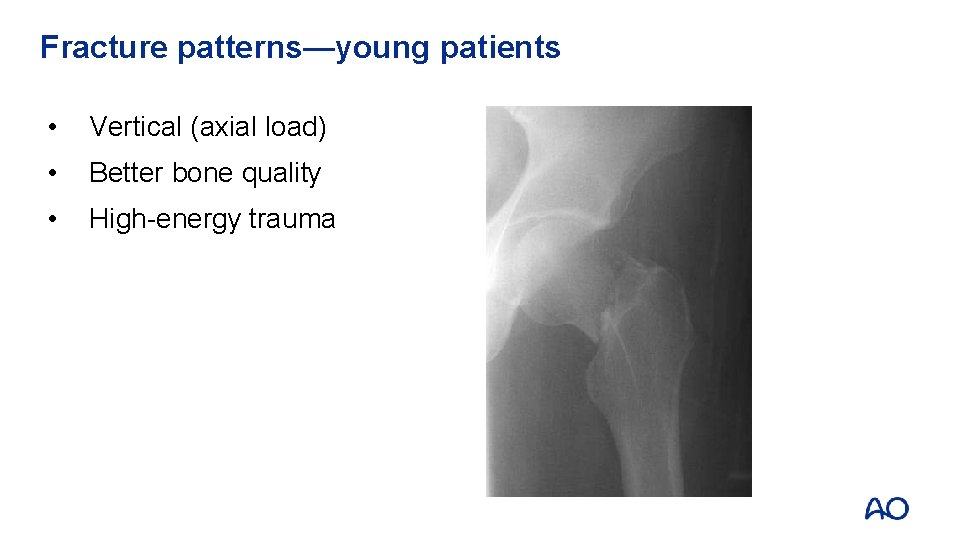
Fracture patterns—young patients • Vertical (axial load) • Better bone quality • High-energy trauma
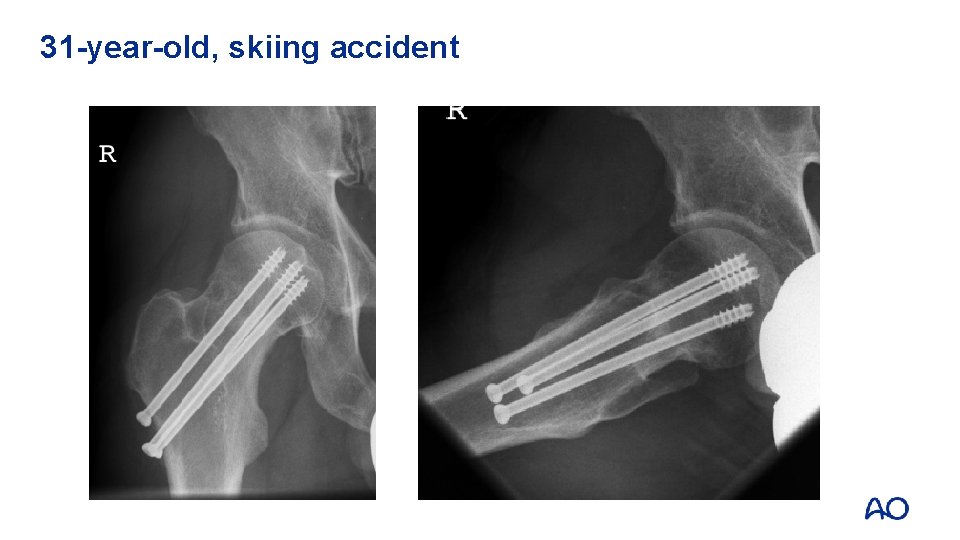
31 -year-old, skiing accident
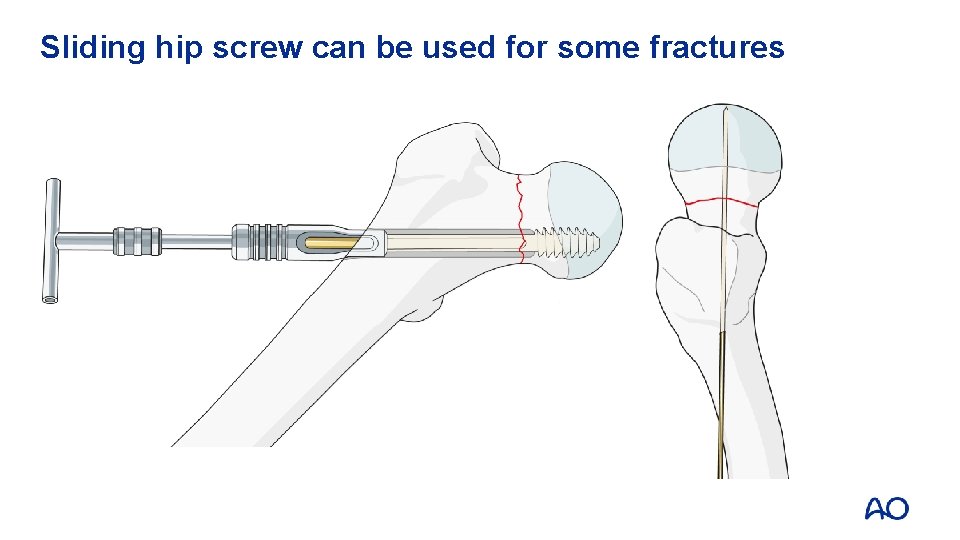
Sliding hip screw can be used for some fractures
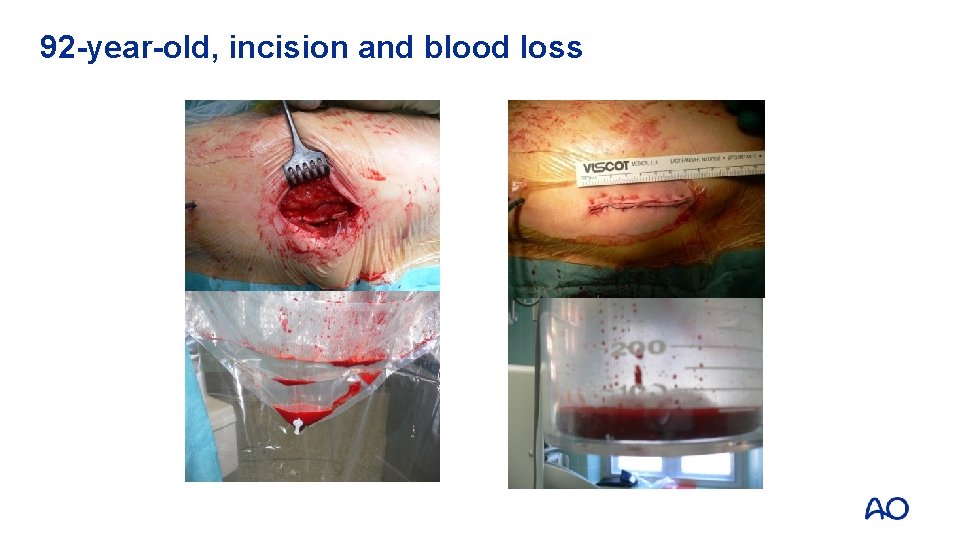
92 -year-old, incision and blood loss
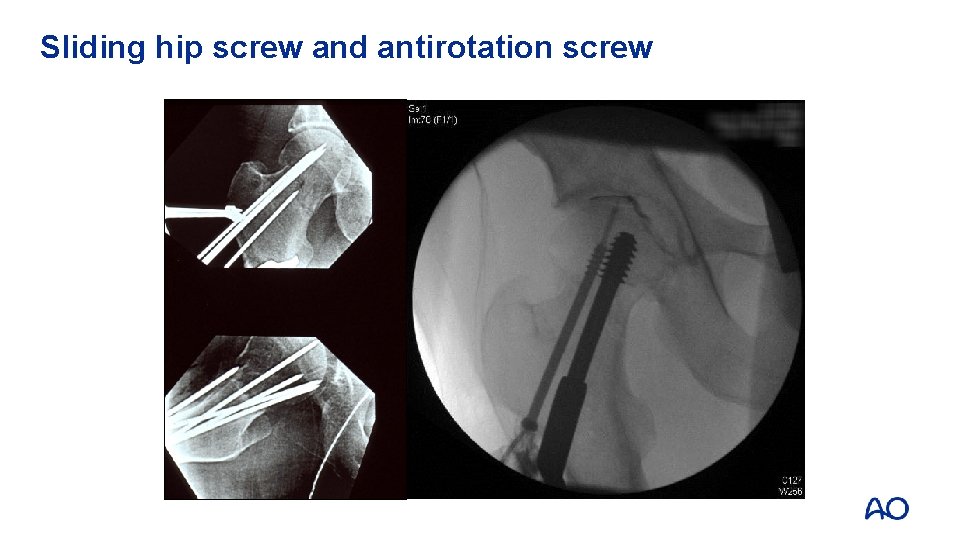
Sliding hip screw and antirotation screw

Does time of treatment matter? • Better results after < 6 hours (unclear) • More local complications after > 48 hours • More general complications after > 48 hours
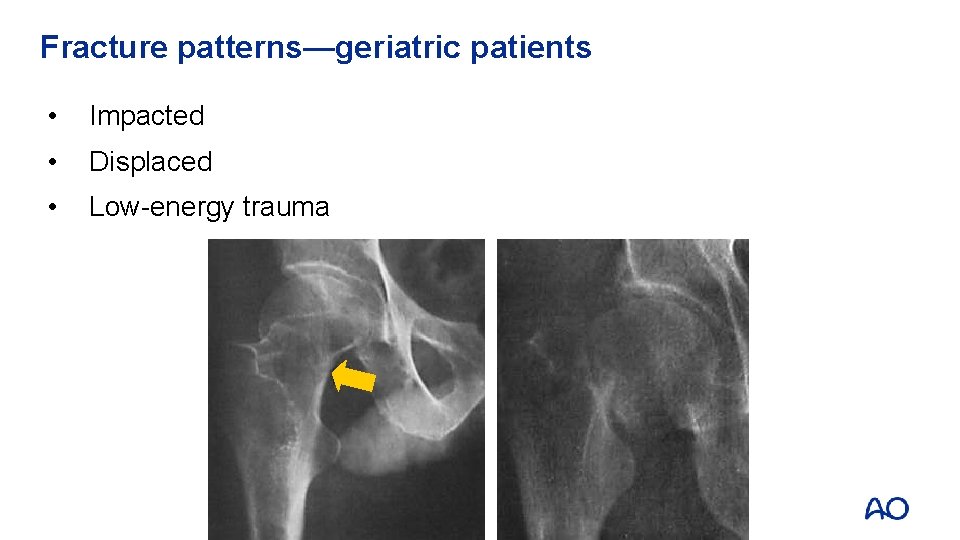
Fracture patterns—geriatric patients • Impacted • Displaced • Low-energy trauma

Decision making: fixation or arthroplasty • Fixation: • Valgus-impacted injuries • Younger, more active patients with reducible fractures • Arthroplasty: • Older patients, more comorbidities • Comminuted fractures • Poor bone quality

Decision making: arthroplasty-related issues • Younger and active patients: favor THA over hemiarthroplasty • Younger patients: likely uncemented • No evidence that bipolar is better than unipolar hemiarthroplasty • Older patients: hybrid THA (only shaft cemented)

Embolization risk during cemented arthroplasty • Be careful when opening the shaft • Jet-lavage or decompress the shaft • Cement stopper • Cement from distal to proximal
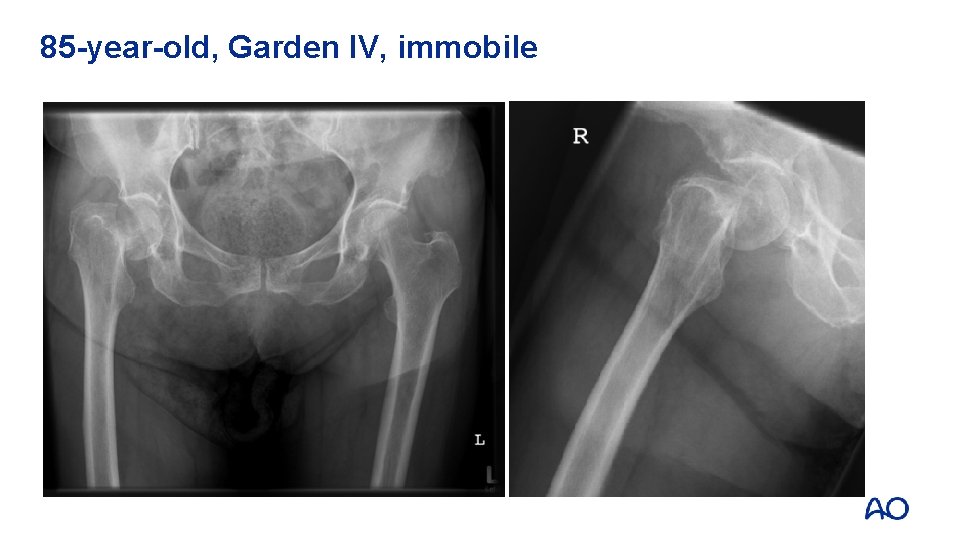
85 -year-old, Garden IV, immobile
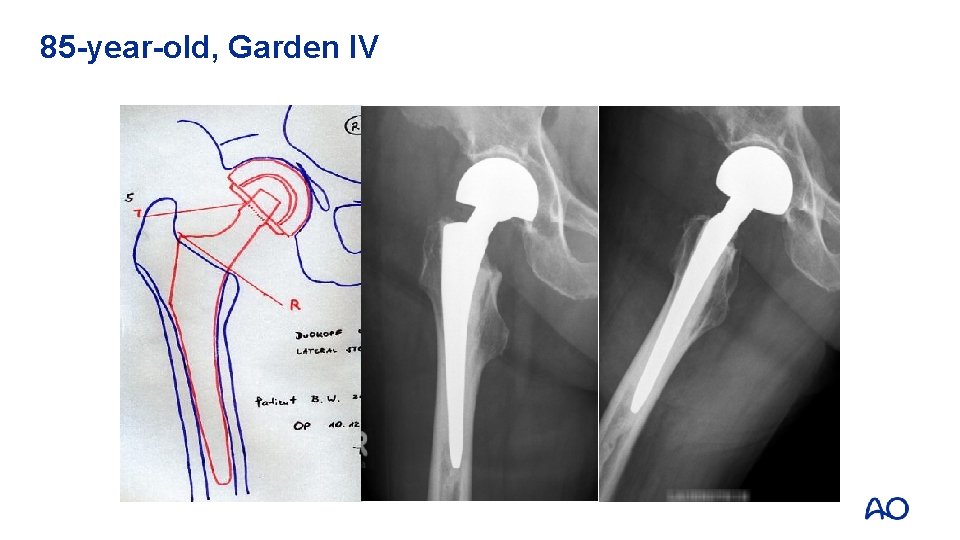
85 -year-old, Garden IV

Results: minimally or nondisplaced fractures ORIF Hemiarthroplasty • Smaller operative trauma • Less reoperations • Less blood loss • More infections • Shorter operation • Higher mortality • Less pain • Better function • More reoperations (1 year)

Results: displaced fractures ORIF Hemiarthroplasty • Three screws • Less reoperations • Less blood loss • More infections • Shorter operation • No higher mortality • More reoperations (93% vs 62%) • No difference in pain • Results comparable • Same number of dependencies

Decision making: geriatric hip fractures • Is it displaced? • How “young” and active is the patient? • Operating sooner is better, once patient is stable • Must manage any coagulation problems • Management of dementia/delirium • More reoperations after ORIF • Complications after endoprosthesis can be more serious • THA has fewer revisions than hemiarthroplasty

Take-home messages • Achieving anatomical reduction is essential in either closed or open techniques • Young patients require timely surgery, anatomical reduction (often open reduction), and stable fixation • Older patients need immediate, predictable mobilization • Geriatric patients are often best served by arthroplasty • THA may be best for most elderly patients, with most predictable outcome
- Slides: 31