Female Reproductive System Development of ovarian oocytes By
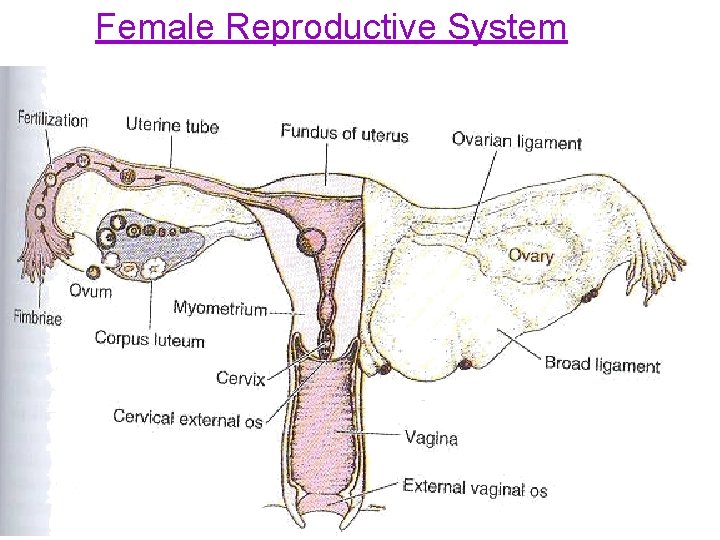
Female Reproductive System

Development of ovarian oocytes • By 3 rd week of intra-uterine life oogonia appear. • After multiple mitosis & by 3 rd month, oogonia st • • begin to enter the prophase of 1 st meiotic division, but stop at diplotene, forming 1 ry oocytes become surrounded by a single layer of flat follicular cells, forming primordial follicles. By the 7 th month, most oogonia are transformed into 1 ry oocytes. Most of primordial follicles undergo atresia. At puberty both ovaries contain about 400, 000 follicles.
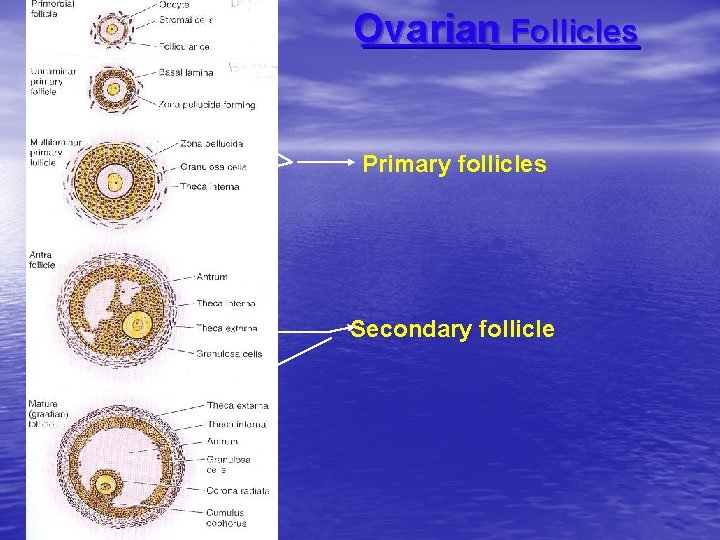
Ovarian Follicles Primary follicles Secondary follicle
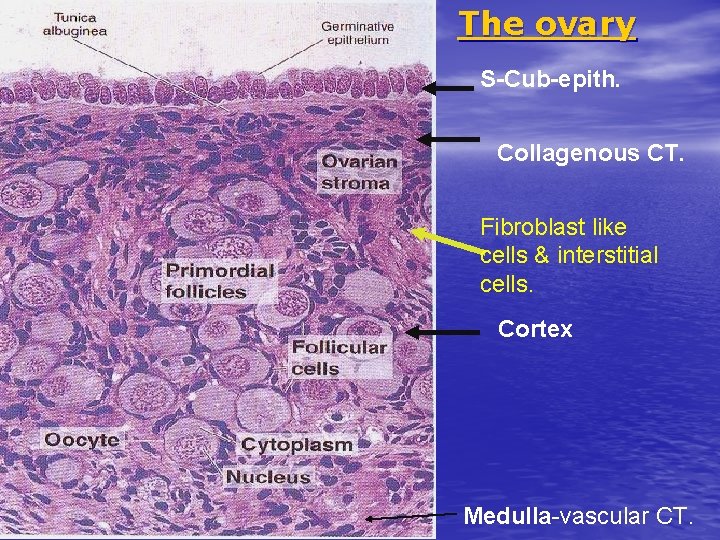
The ovary S-Cub-epith. Collagenous CT. Fibroblast like cells & interstitial cells. Cortex Medulla-vascular CT.
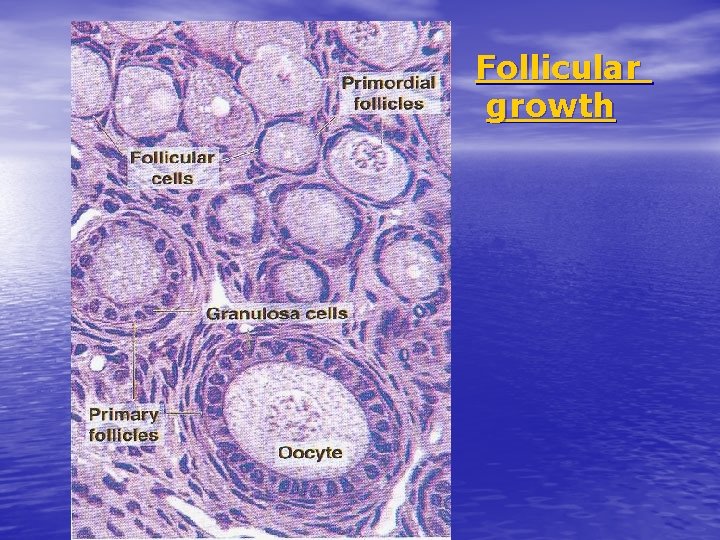
Follicular growth
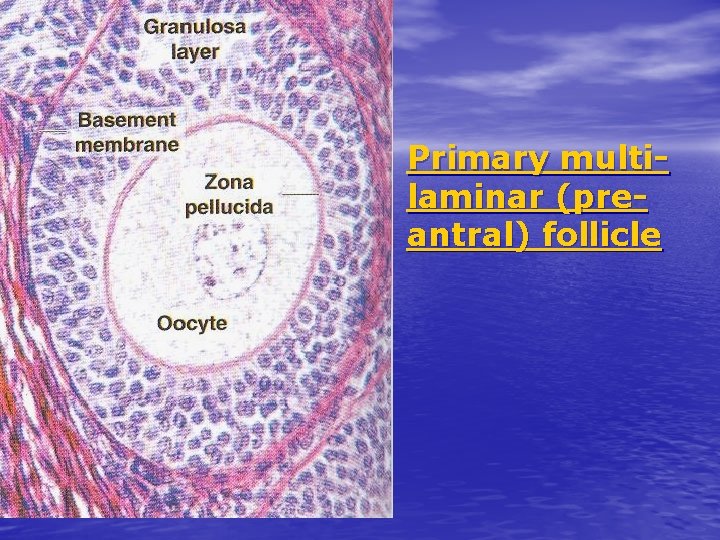
Primary multilaminar (preantral) follicle
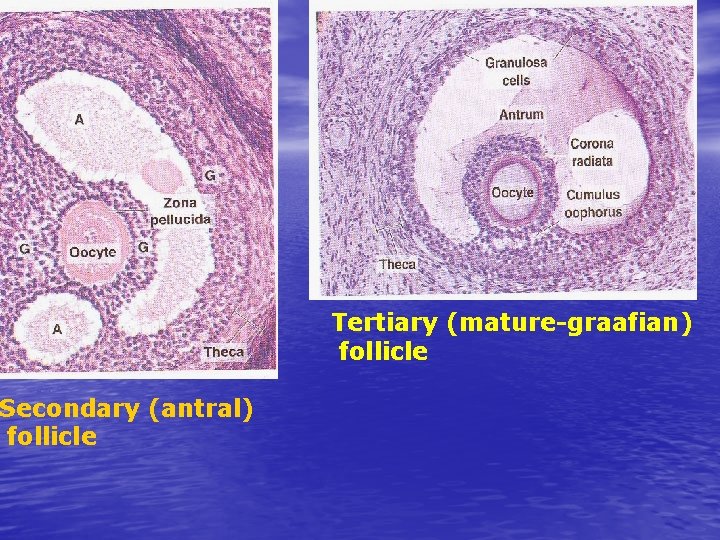
Secondary (antral) follicle Tertiary (mature-graafian) follicle

Growth of the follicles • At puberty, by the effect of FSH, a group (10 -20) of primordial follicle begins follicular growth which includes growth of the followings: • -Oocyte. • -Follicular(granulosa) cells. • -Stromal fibroblasts(theca cells).

Growth of oocyte • It increases in size(120µm). • Increase of nuclear size. • Increase number of mitochondria. • Increase r. ER. • Increase Golgi apparatus which becomes peripheral in position.

Growth of follicular cells 1 -Flat cells become cuboidal cells forming unilaminar primary follicle. 2 -By mitosis follicular cells will be formed of multiple layers of cuboidal cells forming multilaminar primary(preantral)follicle. 3 -Follicular(granulosa) cells and oocyte secrete glycoproteins that surround the oocyte Zona pellucida.

A- The oocyte is fixed in zona pellucida by microvilli. B-The layer of granulosa cells adherent to zona pellucida is fixed into to it by filopodia. 4 -Granulosa cells secrete liquid (liquor folliculi) between granulosa cells as multiple cavities forming secondary or antral follicle. 5 -The liquid containing cavities gather to form one cavity (single antrum) forming mature (graafian follicle). NB-follicular fluid is formed of plasma, glycosaminoglycans, steroid-binding protein and steroid hormones (estrogen-progesteroneandrogen)

Stroma fibroblasts • They differentiate to form theca cells which are: a-Theca interna (vascular)-cells are rich in s. ER & mitochondria with tubular cristaethey secrete androstendion that is changed by granulosa cell s into esterogen. b-Theca externa (fibroblasts). NB –the boundary between 2 layers of theca is not clear while between granulsa and theca cells there is clear basement membrane formed by granulosa cells.
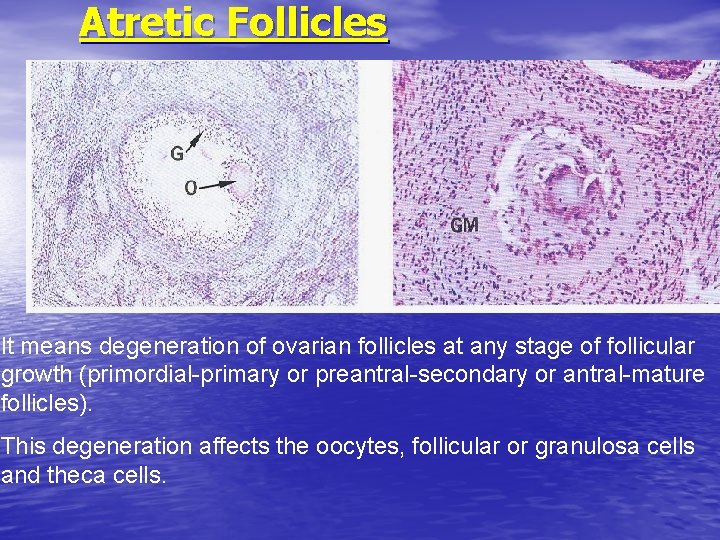
Atretic Follicles It means degeneration of ovarian follicles at any stage of follicular growth (primordial-primary or preantral-secondary or antral-mature follicles). This degeneration affects the oocytes, follicular or granulosa cells and theca cells.

Follicular atresia • Means degeneration of ovarian follicles at different stages of development. • Theca interna cells of atretic follicles change into Interstitial cells (in the stroma of cortical region) which secrete steroid hormone (androgen & estrogen) by the effect of LH.

Ovulation • Means rupture of mature follicle and liberation of 2 ry oocyte (with 1 st polar body), surrounded by zona pllucida and a group of granulosa cells (corona radiata). • Just before ovulation the 1 st meiotic division is completed ( giving 2 ry oocyts &1 st polar body). • Just after ovulation the 2 nd meiotic division begins and stops at metaphase stage. • 2 nd meiotic division is completed (giving an ovum) only if there is fertilization.

Corpus luteum • Is formed under the effect of pituitary LH. • It is the granulosa and theca interna cells of the ovulated follicle. • Granulosa cells increase in size ( not in number) giving granulosa lutein cells that secrete progesterone H. • Theca interna form theca lutein cells that secrete esterogen and progesterone. • There 2 types of corpus luteum: a-corpus luteum of menstruation lasts 14 day. b-Corpus luteum of pregnancy lasts 4 months (maintained by HCG)
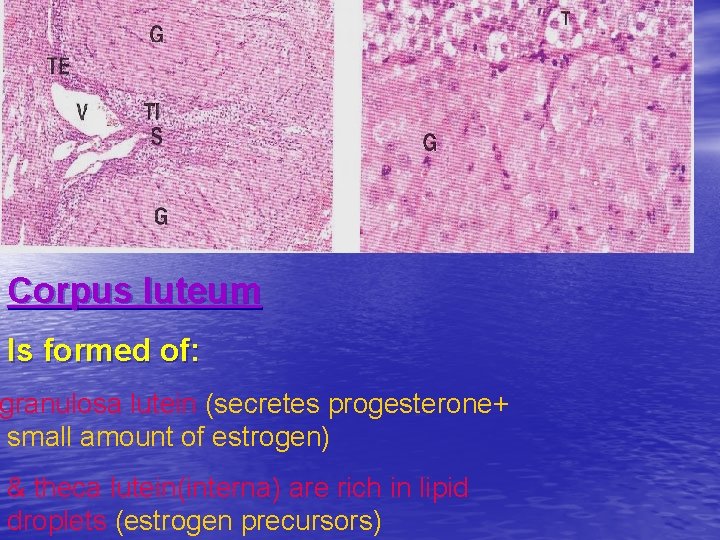
Corpus luteum Is formed of: granulosa lutein (secretes progesterone+ small amount of estrogen) & theca lutein(interna) are rich in lipid droplets (estrogen precursors)
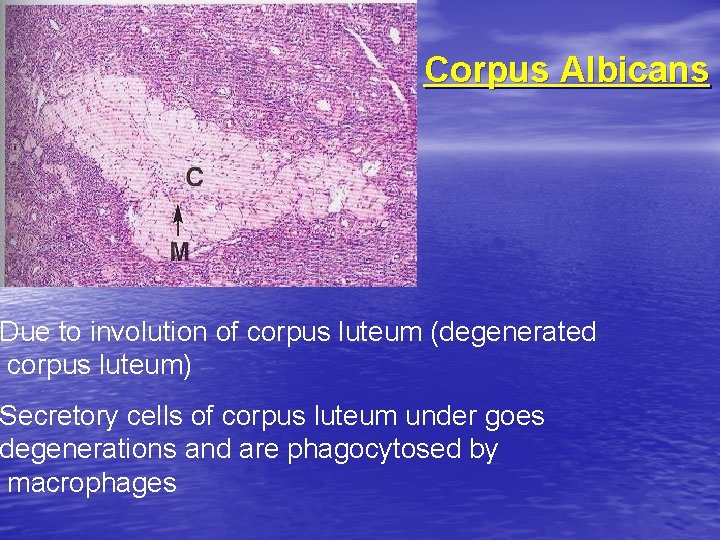
Corpus Albicans Due to involution of corpus luteum (degenerated corpus luteum) Secretory cells of corpus luteum under goes degenerations and are phagocytosed by macrophages
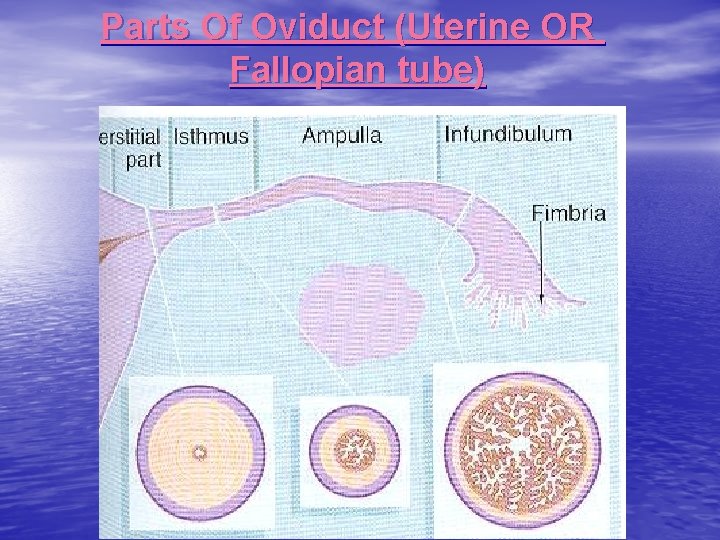
Parts Of Oviduct (Uterine OR Fallopian tube)
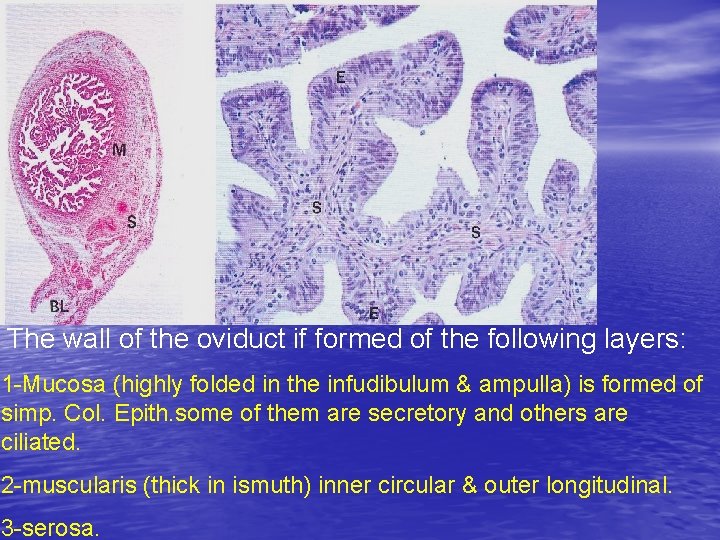
The wall of the oviduct if formed of the following layers: 1 -Mucosa (highly folded in the infudibulum & ampulla) is formed of simp. Col. Epith. some of them are secretory and others are ciliated. 2 -muscularis (thick in ismuth) inner circular & outer longitudinal. 3 -serosa.
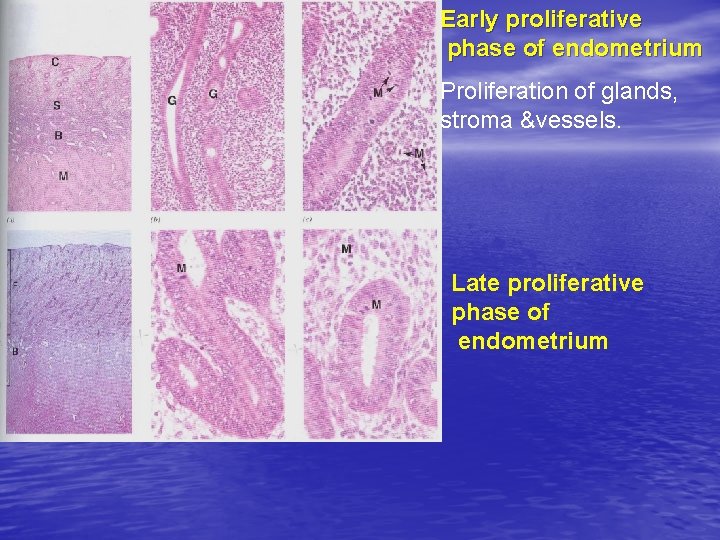
Early proliferative phase of endometrium Proliferation of glands, stroma &vessels. Late proliferative phase of endometrium
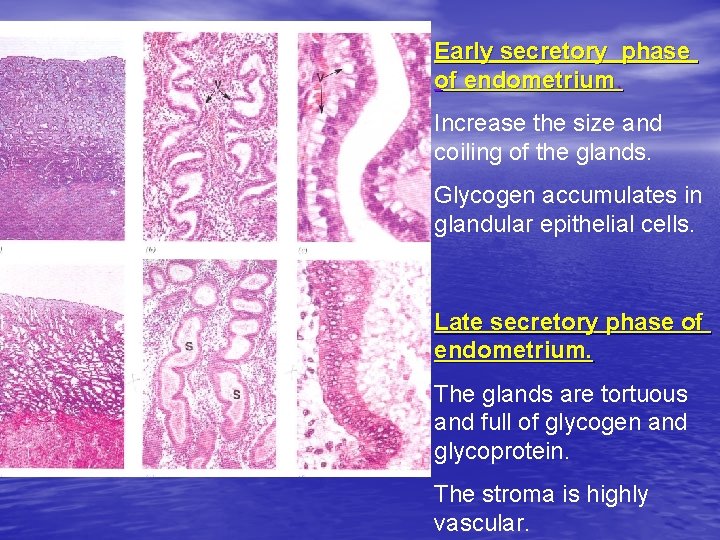
Early secretory phase of endometrium. Increase the size and coiling of the glands. Glycogen accumulates in glandular epithelial cells. Late secretory phase of endometrium. The glands are tortuous and full of glycogen and glycoprotein. The stroma is highly vascular.
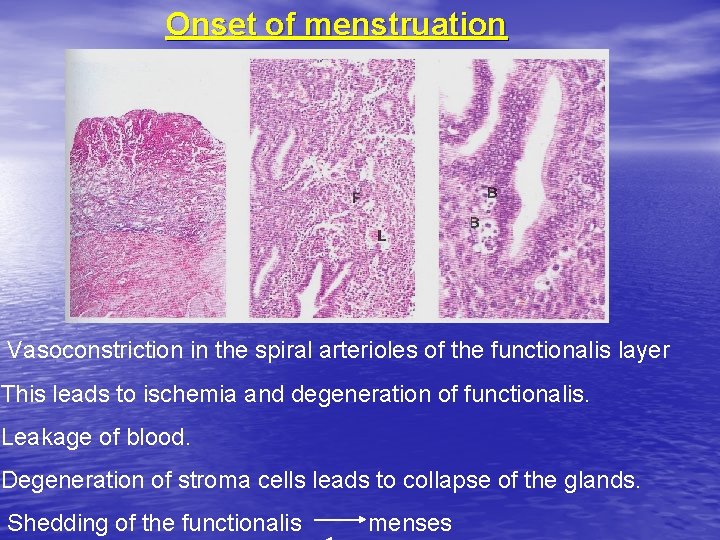
Onset of menstruation Vasoconstriction in the spiral arterioles of the functionalis layer This leads to ischemia and degeneration of functionalis. Leakage of blood. Degeneration of stroma cells leads to collapse of the glands. Shedding of the functionalis menses
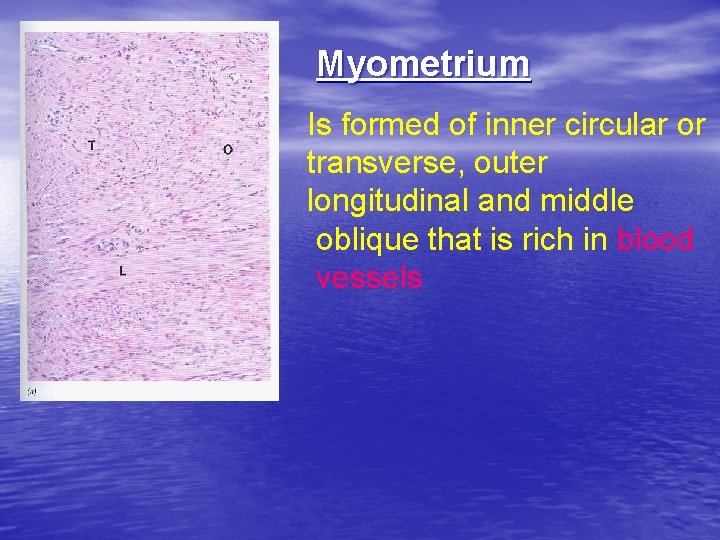
Myometrium Is formed of inner circular or transverse, outer longitudinal and middle oblique that is rich in blood vessels
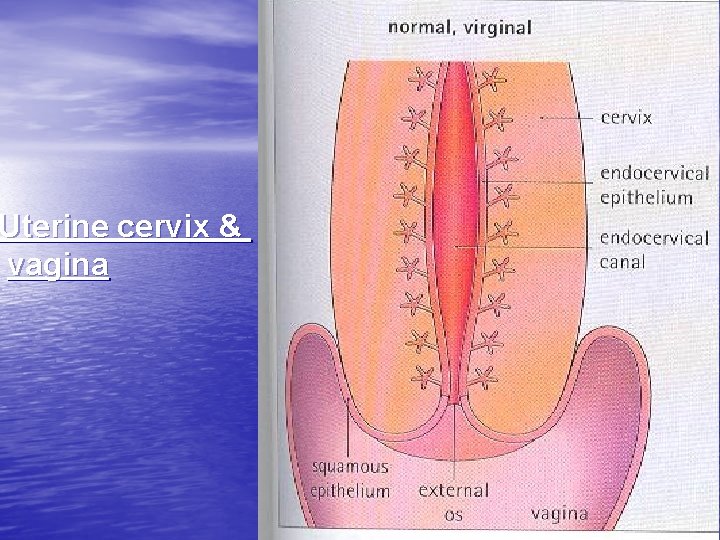
Uterine cervix & vagina
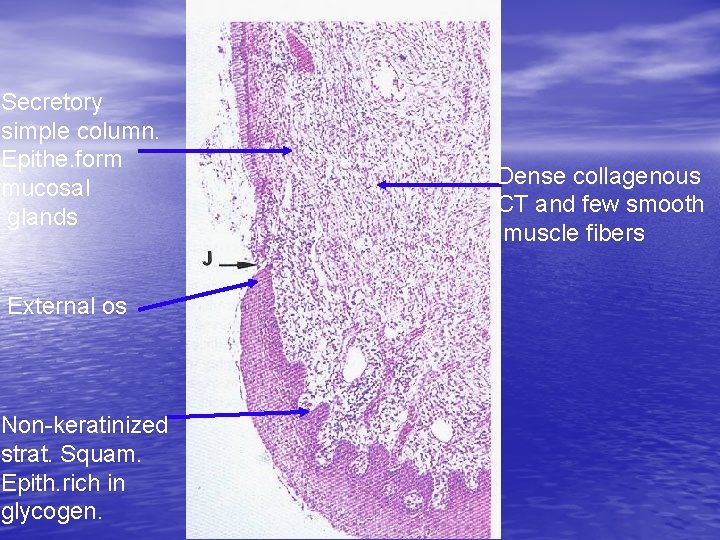
Secretory simple column. Epithe. form mucosal glands External os Non-keratinized strat. Squam. Epith. rich in glycogen. Dense collagenous CT and few smooth muscle fibers
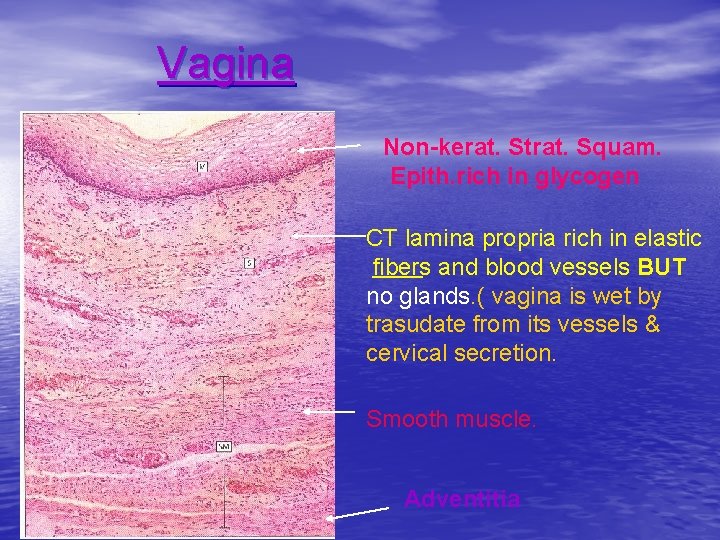
Vagina Non-kerat. Strat. Squam. Epith. rich in glycogen CT lamina propria rich in elastic fibers and blood vessels BUT no glands. ( vagina is wet by trasudate from its vessels & cervical secretion. Smooth muscle. Adventitia
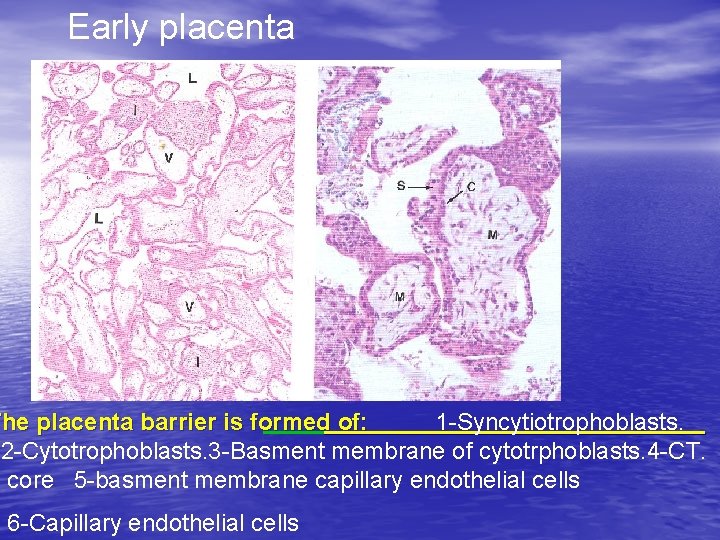
Early placenta The placenta barrier is formed of: 1 -Syncytiotrophoblasts. 2 -Cytotrophoblasts. 3 -Basment membrane of cytotrphoblasts. 4 -CT. core 5 -basment membrane capillary endothelial cells 6 -Capillary endothelial cells
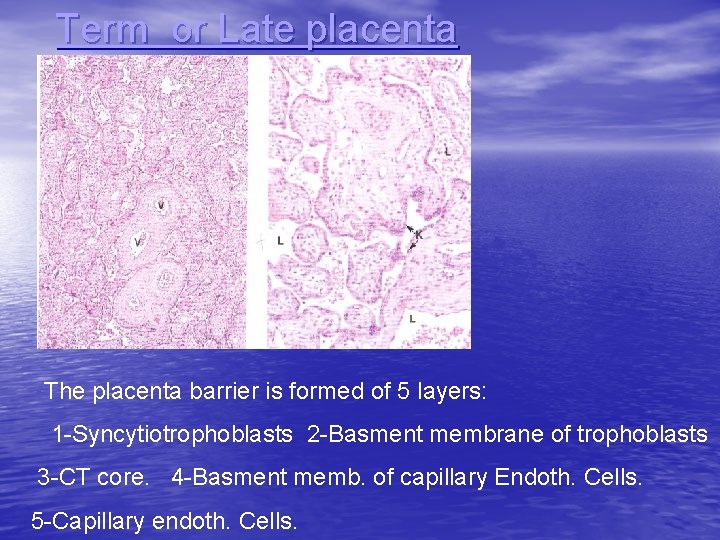
Term or Late placenta The placenta barrier is formed of 5 layers: 1 -Syncytiotrophoblasts 2 -Basment membrane of trophoblasts 3 -CT core. 4 -Basment memb. of capillary Endoth. Cells. 5 -Capillary endoth. Cells.
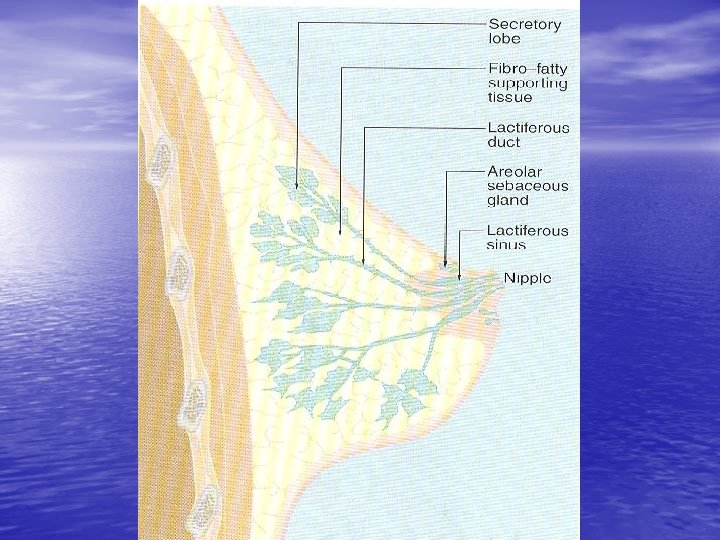
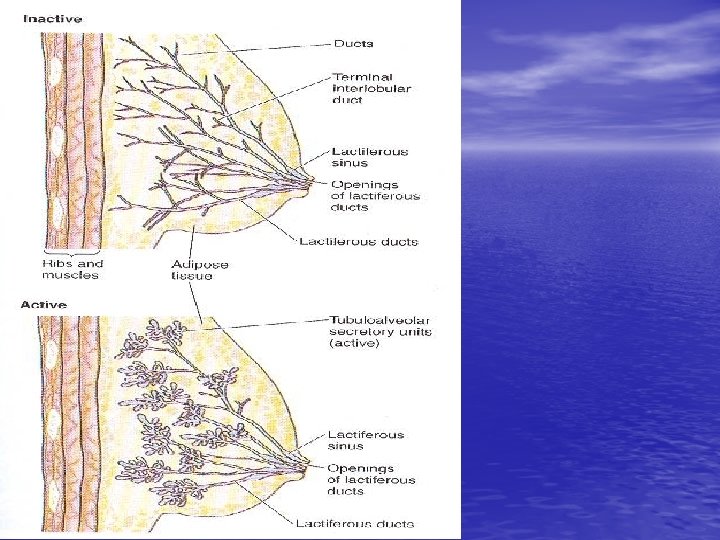
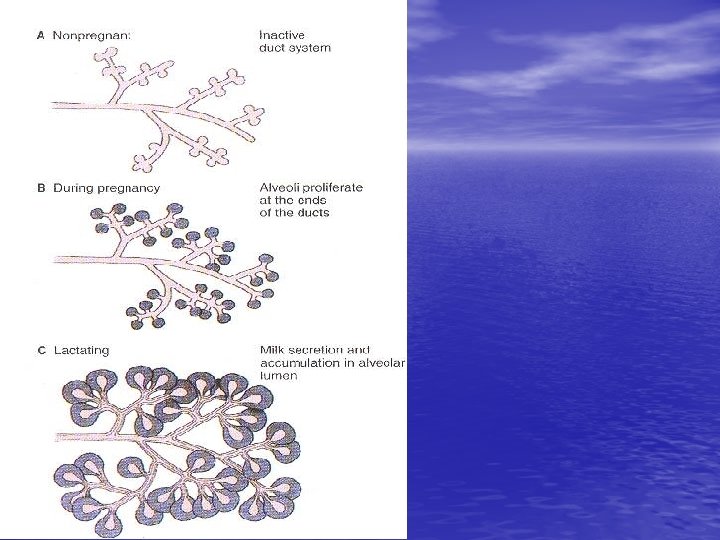
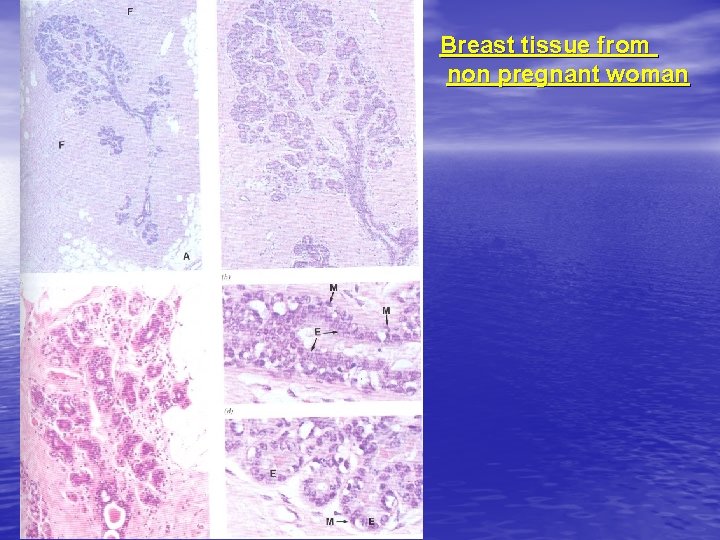
Breast tissue from non pregnant woman
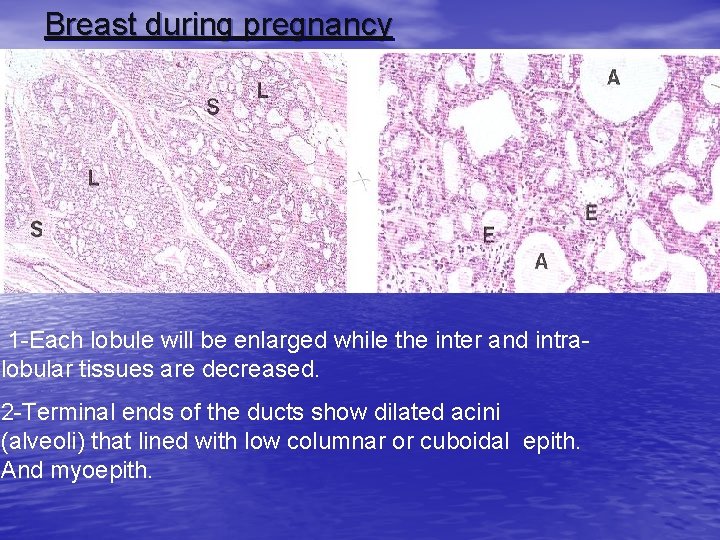
Breast during pregnancy 1 -Each lobule will be enlarged while the inter and intralobular tissues are decreased. 2 -Terminal ends of the ducts show dilated acini (alveoli) that lined with low columnar or cuboidal epith. And myoepith.
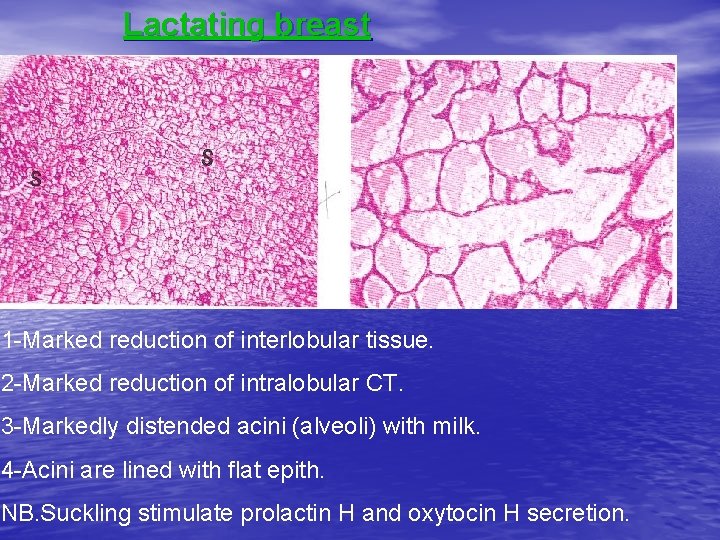
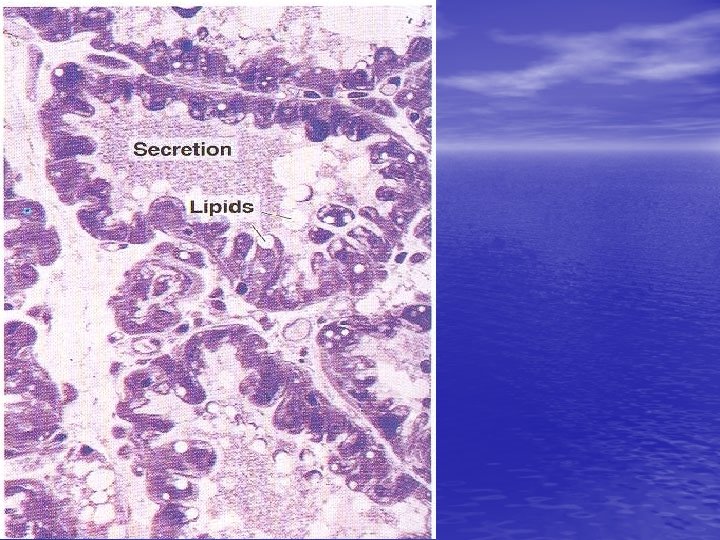
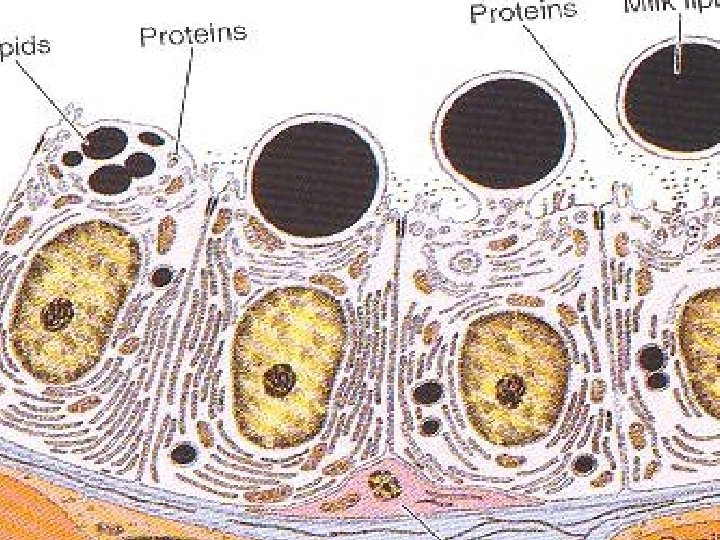
Lactating breast 1 -Marked reduction of interlobular tissue. 2 -Marked reduction of intralobular CT. 3 -Markedly distended acini (alveoli) with milk. 4 -Acini are lined with flat epith. NB. Suckling stimulate prolactin H and oxytocin H secretion.
- Slides: 39