Fellows School Acute Heart Failure Brent C Lampert

Fellows School: Acute Heart Failure Brent C. Lampert, DO Aug 4, 2014 1

Outline § Definitions § Incidence § Diagnosis § Treatment § Diuretics, vasodilators, inotropes, UF, advanced therapies § Transition to discharge § RHC interpretation

Terminology § § § § § AHF Acute decompensated HF (ADHF) Acute on chronic systolic / diastolic HF Acute biventricular HF Acute HF syndrome Acute decompensation of chronic HF HFp. EF HFr. EF AHA 2013 HF Guidelines GDMT
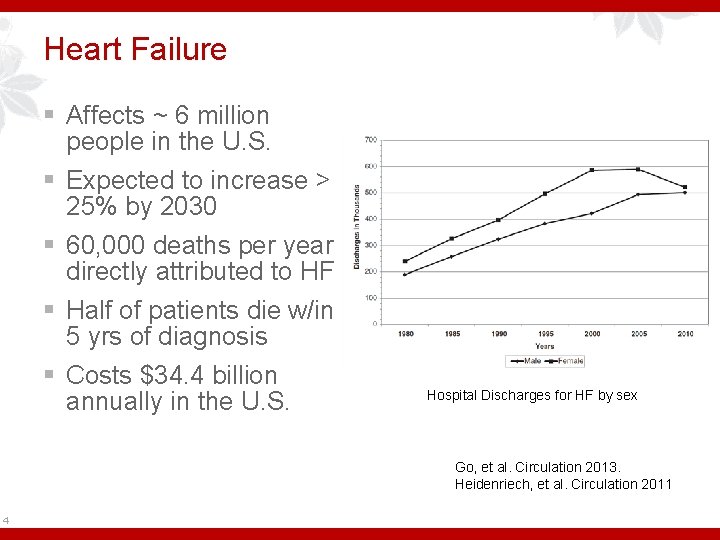
Heart Failure § Affects ~ 6 million people in the U. S. § Expected to increase > 25% by 2030 § 60, 000 deaths per year directly attributed to HF § Half of patients die w/in 5 yrs of diagnosis § Costs $34. 4 billion annually in the U. S. Hospital Discharges for HF by sex Go, et al. Circulation 2013. Heidenriech, et al. Circulation 2011 4

Introduction: AHF § Definition: new, gradual, or rapidly worsening heart failure signs & symptoms requiring urgent therapy § 1 million annual admissions in US: HF as primary diagnosis § 3 million annual admissions in US: HF as primary or secondary dx Gheorhiade M, et al. JACC 2009

Heart Failure Rehospitalizations § 30 day rehospitalization rate 27% in Medicare patients § 40% due to HF (at OSU within 7 days) § Higher early follow-up rate (in 7 days of discharge) associated with reduced 30 day event rates
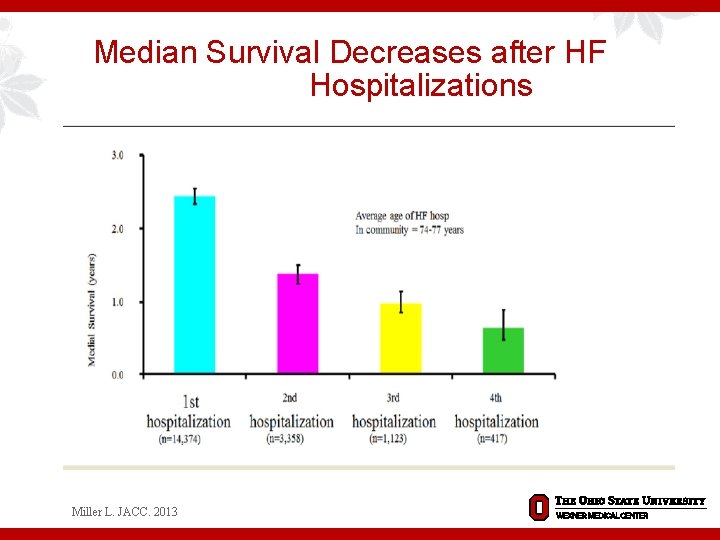
Median Survival Decreases after HF Hospitalizations Miller L. JACC. 2013

Etiologies of HF § Ischemia (#1) § Hypertension (#2) § Valvular § Inflammatory § Myocarditis, infectious, autoimmune. § Medications § Chemotherapy, chloroquin § Toxins § Ethanol, cocaine § Deposition § Amyloid, hemochromatosis § Rheumatologic § Endocrine disorders § Neuromuscular disease § Miscellaneous § Peripartum, tachycardiarelated, familial, sleep apnea, sarcoid. § Idiopathic (#3)

Common Factors Precipitating the HF Hospitalization § Noncompliance § Myocardial ischemia / infarction § Hypertension § Atrial fibrillation / arrhythmia § Addition of negative inotropic drugs (verapamil/diltiazem, β-blockers) § Pulmonary embolus § NSAID’s § Excessive ETOH / drugs § Endocrine abnormalities § Concurrent infections (Pneumonia, viral illness)

ADHF Diagnosis - Presentation § No single finding conclusive for diagnosing § Most common symptoms: progressive dyspnea, fatigue, cough, orthopnea, PND, edema, and/or weight gain § PE: § § § Tachypnea Tachycardia Crackles or wheezing (“cardiac asthma”) Extra cardiac sounds (S 3 and/or S 4) Elevated jugular venous pressure (use central lines for CVP) § Edema § Nausea / poor appetite 10
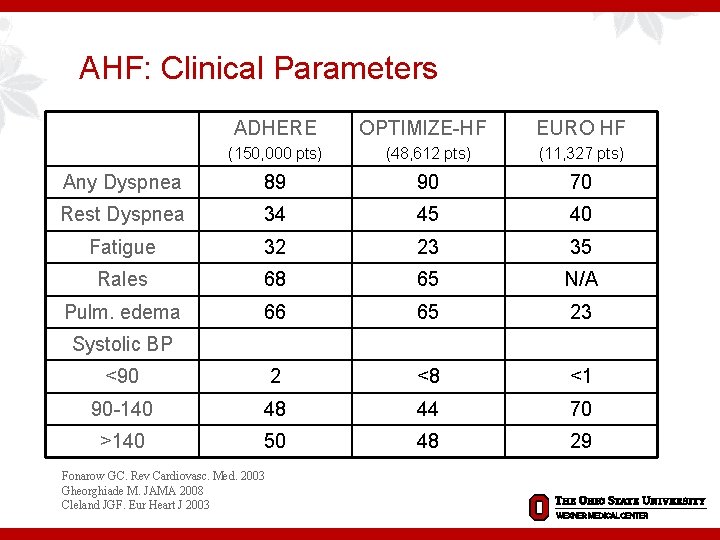
AHF: Clinical Parameters ADHERE OPTIMIZE-HF EURO HF (150, 000 pts) (48, 612 pts) (11, 327 pts) Any Dyspnea 89 90 70 Rest Dyspnea 34 45 40 Fatigue 32 23 35 Rales 68 65 N/A Pulm. edema 66 65 23 <90 2 <8 <1 90 -140 48 44 70 >140 50 48 29 Systolic BP Fonarow GC. Rev Cardiovasc. Med. 2003 Gheorghiade M. JAMA 2008 Cleland JGF. Eur Heart J 2003

ADHF Diagnosis - Presentation 12

ADHF Diagnosis - Testing § EKG to identify underlying causes (LVH, MI, afib) § CXR may reveal pulmonary vascular congestion, but normal chest xraydoes not exclude ADHF § CBC to identify anemia or infection § Chemistries to evaluate for renal dysfunction § Cardiac biomarkers if ischemia is suspected § BNP useful when the diagnosis is uncertain § > 400 pg/m. L predictive of heart failure as cause of dyspnea § < 100 pg/m. L have a very high negative predictive value for heart failure as a cause of dyspnea § Echocardiography in all patients with new onset heart failure § LHC in patients with suspected ACS 13
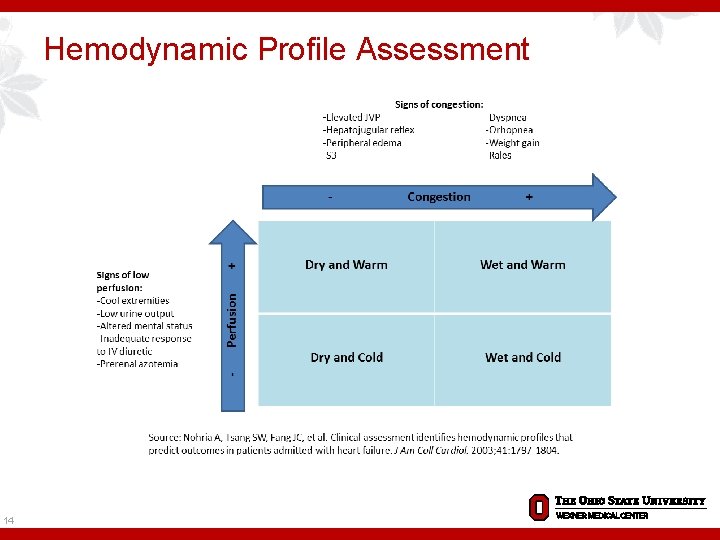
Hemodynamic Profile Assessment 14

ADHF – Initial treatment § Focus on hemodynamic & volume abnormalities and correct precipitating factors (ischemia/arrhythmias) § Diuretics, diuretics! § Start w/equal or greater dose of loop diuretic (IV) than outpatient regimen (furosemide - NOT BUMEX) § Short half-life; requires multiple doses or continuous infusion § IV continuous infusion & bolus dosing have similar efficacy § Be cognizant of detrimental effects on renal blood flow, GFR, electrolytes, neurohormones § Volume status, evidence of congestion, daily I/O, daily wts, potassium and creatinine frequently assessed § Low sodium diet (2 g daily or less) and fluid restriction (at least <2 L daily) should be considered 15
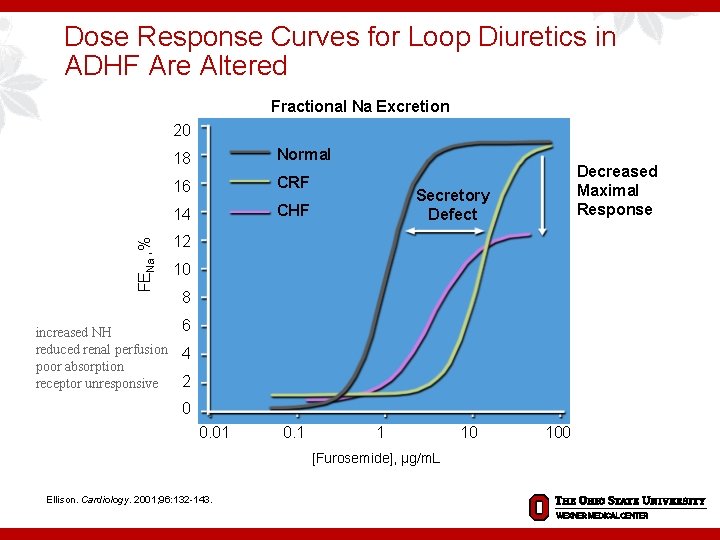
Dose Response Curves for Loop Diuretics in ADHF Are Altered Fractional Na Excretion FENa , % 20 18 Normal 16 CRF 14 CHF Secretory Defect 12 10 8 6 increased NH reduced renal perfusion 4 poor absorption 2 receptor unresponsive 0 0. 01 0. 1 100 [Furosemide], µg/m. L Ellison. Cardiology. 2001; 96: 132 -143. Decreased Maximal Response
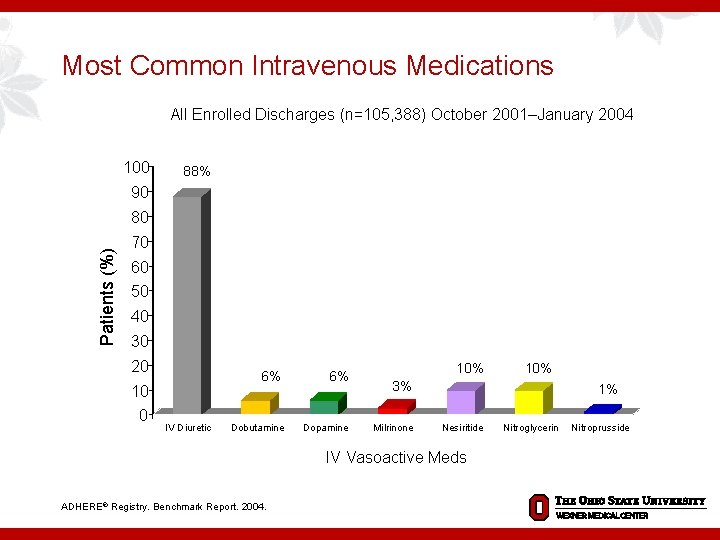
Most Common Intravenous Medications All Enrolled Discharges (n=105, 388) October 2001–January 2004 100 88% 90 Patients (%) 80 70 60 50 40 30 20 6% 10 0 IV Diuretic Dobutamine 6% Dopamine 10% 3% Milrinone 1% Nesiritide IV Vasoactive Meds ADHERE® Registry. Benchmark Report. 2004. 10% Nitroglycerin Nitroprusside

Acute HF – Options When Initial Diuretics Fail § Is there persistent “congestion” ? § Careful exam (JVP), labs, BNP § May need invasive hemodynamics § Continuous infusion of furosemide § 5 -40 mg/hr § § § Add thiazide (distal tubule diuretic) Ultrafiltration Additional Vasoactive therapy Inotropes Advanced therapies

Thiazide diuretics – “Booster” • HCTZ • Metolazone • Long ½ life • Does not need to be administered 30 min prior • Significant electrolyte disturbances • Chlorothiazide (Diuril) • IV • $$$
Ultrafiltration for Acute Heart Failure § Useful in patients w/ ADHF + renal insufficiency or diuretic resistance § Advantages: adjustable fluid removal rates, no effect on electrolytes, decreased neurohormonal activity § CARESS-HF § 188 pts w/ ADHF, worsened renal function § Stepped pharmacologic care (loop diuretics, metolazone, selective inotropes or vasodilators) vs. UF § No difference in weight loss § UF with increased Cr and more adverse events

Vasodilators § Rapid resolution of congestive symptoms, angina, HTN § Most patients will have high SVR (MAP/CO) § Improve SV, C. O. , right and left sided filling pressures without increase HR § Nitroglycerin, Nesiritide, Nitroprusside 21

Vasodilators - Nitroglycerin § Reduces LV filling pressures primarily through venodilation § Variable effect on SVR (depends on degree of elevation) § Improves myocardial blood flow (coronaries, LVEDP, HR) § Start at 5 -10 mcg/min and can titrate rapidly to effect (as high as 400 mcg/min) § Attention to intravascular volume (resistance in those with high RAP) and hypotension in those with low IVV, RV dysfunction, diastolic HF § Short half life § Tachyphylaxis can occur within hours § Avoid with PDE inhibitors 22

Vasodilators - Nitroprusside § Potent vasodilator with balanced venous & arterial effects § Short half-life (effects are gone w/in 10 minutes) § Rapidly reduces filling pressures, MVO 2, valve regurgitation § Rapidly increases SV § Significant increase in HR (or drop in BP) should stop infusion § Typically use with invasive hemodynamics § Potential for cyanide toxicity (rare) – limit to 48 hours § Dose starts at 0. 5 mcg/kg/min and titrate to hemodynamic effect Q 3 -5 minutes. 23

Vasodilators - Nesiritide § Recombinant human BNP § Venous and arterial dilation. Reduces BP, filling pressures and mild increase in CO; no increase in HR § Limited evidence for “natriuretic” effect in clinical studies. Does not replace diuretics. § Start at 0. 005 – 0. 01 mcg/kg/min; +/- bolus. Limited dose titration necessary. Long half-life. § As with all vasoactive therapies, must monitor BP, symptoms, renal function closely (multiple times per day) 24

Conclusions: Mild benefit in dyspnea No effect on outcomes No adverse effect on renal function Increased hypotension O’Connor et al. NEJM 2011

ADHF Treatment - Inotropes § Milrinone and dobutamine § For “cold” patients with evidence of hypoperfusion § Short-term therapy to maintain systemic perfusion and preserve end-organ performance until definitive therapy (revascularization, MCS, Transplant) or palliative therapy § Require continuous rhythm and frequent BP monitoring § Symptomatic hypotension or tachyarrhythmias should prompt consideration of dose reduction or discontinuing 26

ADHF Treatment - Milrinone § PDE inhibitor that increases myocardial inotropy by inhibiting degradation of cyclic AMP § Reduces systemic and pulmonary vascular resistance (via inhibition of peripheral phosphodiesterase) § Improves left ventricular diastolic compliance (lusitropy) § Increases cardiac index and decreases left ventricular afterload and filling pressures § Can be given with B-blockers § Typical dose: 0. 25 – 0. 75 mcg/kg/min 27

ADHF Treatment - Dobutamine § Acts primarily on beta-1 adrenergic receptors, with minimal effects on beta-2 and alpha-1 receptors § Increases stroke volume and cardiac output § Modest decreases in systemic vascular resistance and pulmonary capillary wedge pressure § Consider decrease / withdrawal B-blockers § ? Increased ventricular ectopy § Typical dose: 2 -20 mcg/kg/min 28

ADHF Treatment - Inotropes § Continue until euvolemia is achieved, or definitive therapy delivered § Wean gradually to avoid effects of sudden withdrawal including precipitous decreases in cardiac output § Failure to wean should prompt consideration of additional advanced therapies 29

ADHF Treatment – Advanced therapies § IABP is the most commonly used, easily placed, and least expensive support device § ECMO can provide cardiopulmonary support § Temporary support for patients failing all otherapies § Bypasses the pulmonary circulation and oxygenated blood returns to the patient via an arterial or venous route § Venovenous ECMO: primarily supports patients with severe respiratory failure § Venoarterial ECMO utilizes an extracorporeal pump to help with hemodynamic support § Short term VADS can be placed percutaneously or surgically 30
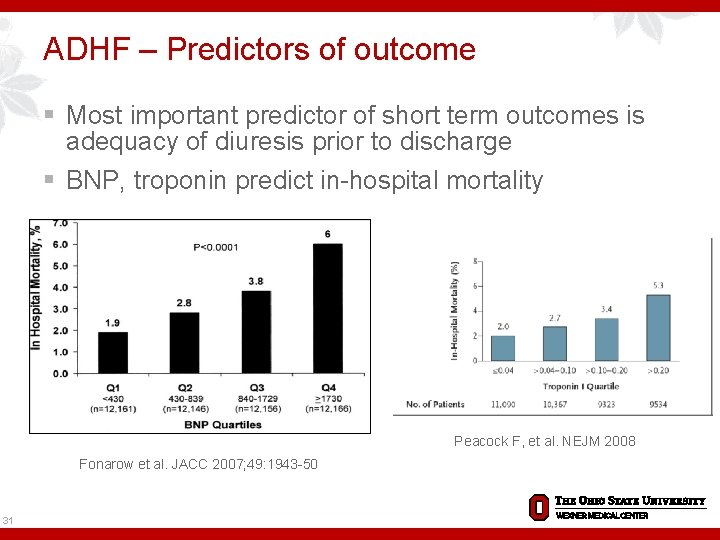
ADHF – Predictors of outcome § Most important predictor of short term outcomes is adequacy of diuresis prior to discharge § BNP, troponin predict in-hospital mortality Peacock F, et al. NEJM 2008 Fonarow et al. JACC 2007; 49: 1943 -50 31

ADHF – Discharge criteria Recommended for all Patients Should be considered Exacerbating factors addressed Near optimal volume status observed Transition from intravenous to oral diuretic successfully completed Patient and family education completed, including clear discharge instructions Left ventricular ejection fraction (LVEF) documented Smoking cessation counseling initiated Near optimal pharmacologic therapy achieved, including ACE inhibitor and beta blocker (for patients with reduced LVEF), or intolerance documented Follow-up clinic visit scheduled, usually for 7 to 10 days Oral medication regimen stable for 24 hours No intravenous vasodilator or inotropic agent for 24 hours Ambulation before discharge to assess functional capacity after therapy Plans for postdischarge management (scale present in home, visiting nurse or telephone follow up generally no longer than 3 days after discharge) Referral for disease management, if available Source: Lindenfeld, J, Albert NM, Boehmer JP, Collins SP, Ezekowitz JA, Givertz MM, Klapholz M, Moser DK, Rogers JG, Starling RC, Stevenson WG, Tang WHW, Teerlink JR, Walsh MN. HFSA 2010 Comprehensive Heart Failure Practice 32 Guideline. J Card Fail 2010; 16: e 1 -e 194.

ADHF - RHC § Value of RHC remains controversial § Randomized ESCAPE trial showed no benefit (or increased risk) of using RHC in mortality or days alive out of the hospital § Did not enroll all consecutive patients b/c many physicians would not enroll and risk a 50% chance of not having PA catheter § Routine RHC in HF not recommended; useful in subset of patients § 2013 ACC/AHA heart failure guideline: perform in patients “with respiratory distress or impaired systemic perfusion when clinical assessment is inadequate” 33
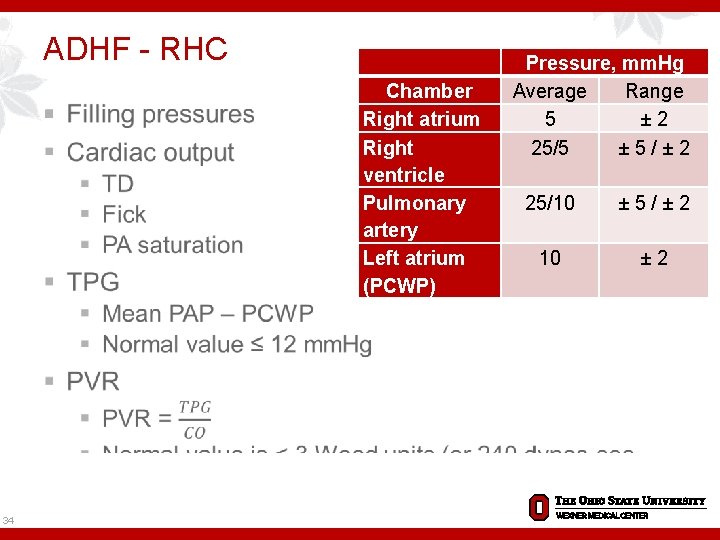
ADHF - RHC § 34 Chamber Right atrium Right ventricle Pulmonary artery Left atrium (PCWP) Pressure, mm. Hg Average Range 5 ± 2 25/5 ± 5 / ± 2 25/10 ± 5 / ± 2 10 ± 2
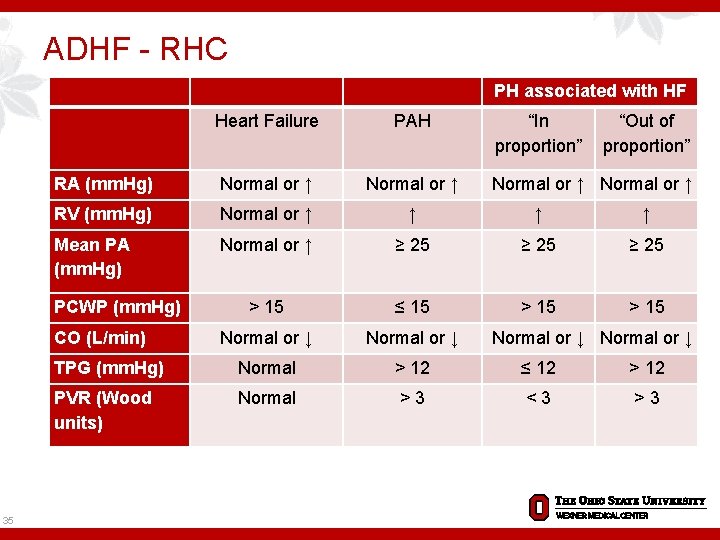
ADHF - RHC Heart Failure PAH RA (mm. Hg) Normal or ↑ RV (mm. Hg) Normal or ↑ ↑ Mean PA (mm. Hg) Normal or ↑ ≥ 25 > 15 ≤ 15 > 15 Normal or ↓ TPG (mm. Hg) Normal > 12 ≤ 12 > 12 PVR (Wood units) Normal > 3 < 3 > 3 PCWP (mm. Hg) CO (L/min) 35 PH associated with HF “In proportion” “Out of proportion” Normal or ↑ Normal or ↓

ADHF - RHC § RA 10, PA 50/24 (33), PCWP 26 § CO/CI 4. 7/2. 4, PA saturation 65% § Diagnosis? § Treatment? 36

ADHF - RHC § RA 20, PA 50/24 (33), PCWP 26 § CO/CI 4. 7/2. 4, PA saturation 65% § Diagnosis? § Treatment? 37

ADHF - RHC § RA 20, PA 50/24 (33), PCWP 26 § CO/CI 3. 1/1. 5, PA saturation 43% § Diagnosis? § Treatment? 38

ADHF - RHC § RA 18, PA 84/25 (45), PCWP 10 § CO 5. 0/2. 6, PA saturation 68% § Diagnosis § Treatment 39

ADHF - RHC § RA 18, PA 84/25 (45), PCWP 36 § CO 5. 0/2. 6, PA saturation 68% § Diagnosis § Treatment 40

Questions 41
- Slides: 41