February 10 12 Sinclair Community College Ponitz Center

February 10 -12 Sinclair Community College Ponitz Center

Bipolar Disorder 1 & 2 Constance Ange, D. O. admin@doctorange. com (937) 498 -0068 AOA Board Certified Adult Psychiatry AOA Board Certified Child Psychiatry AMA Board Certified Adult Psychiatry AMA Board Certified Child Psychiatry American Board of Forensic Medicine
The most common first time presentation of Bipolar I and Bipolar II in the office is A. B. C. D. 9/9/2021 Mania Depression Mixed Impulsivity 25% 25% A. B. C. 25% D. 10 3

The first time BD is diagnosed the most common treatment is A. B. C. D. 9/9/2021 Antidepressants Antipsychotics Mood Stabilizers Benzodiazepines 25% 25% A. B. C. D. 10 4

I. DSM V II. Bipolar Prevalence III. Bipolar Trends IV. Bipolar Mixed States Outline V. Bipolar and Executive Function VI. Bipolar and Suicide VII. Bipolar and Sleep VIII. Bipolar and Substance Abuse IX. Bipolar and Seasonal Distribution 9/9/2021 X. Bipolar and Obesity XI. Bipolar and OCD XII. Bipolar and Cognitive Function XIII. Bipolar and Personality Traits XIV. Bipolar and Long Term Work Disability XV. Assessment Tools XVI. Bipolar and Pregnancy XVII. Bipolar and Compliance XVIII. Bipolar and ECT XIX. Bipolar and Treatment 5

DSM V Bipolar I 9/9/2021 For a diagnosis of Bipolar I an individual must meet the criteria for a manic episode Manic episode may have been preceded by and may be followed by hypomanic or major depressive episodes (Diagnostic and statistical manual of mental disorders: DSM-5, 2013) 6
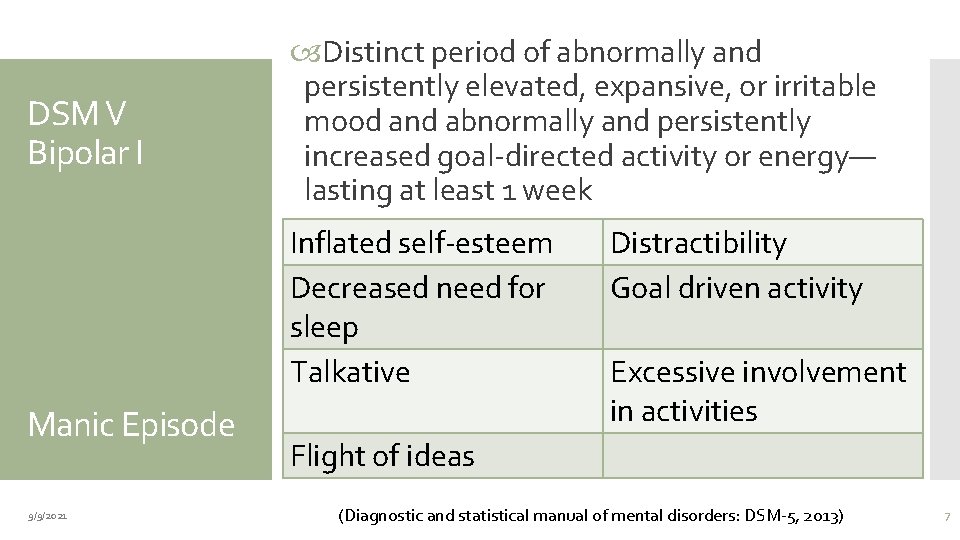
DSM V Bipolar I Distinct period of abnormally and persistently elevated, expansive, or irritable mood and abnormally and persistently increased goal-directed activity or energy— lasting at least 1 week Inflated self-esteem Decreased need for sleep Talkative Manic Episode 9/9/2021 Distractibility Goal driven activity Excessive involvement in activities Flight of ideas (Diagnostic and statistical manual of mental disorders: DSM-5, 2013) 7

DSM V Bipolar I Hypomanic Episode 9/9/2021 Similar BUT different from manic episode The episode is NOT severe enough to cause marked impairment in social or occupational functioning or to necessitate hospitalization. Common in Bipolar I, however not required for diagnosis (Diagnostic and statistical manual of mental disorders: DSM-5, 2013) 8
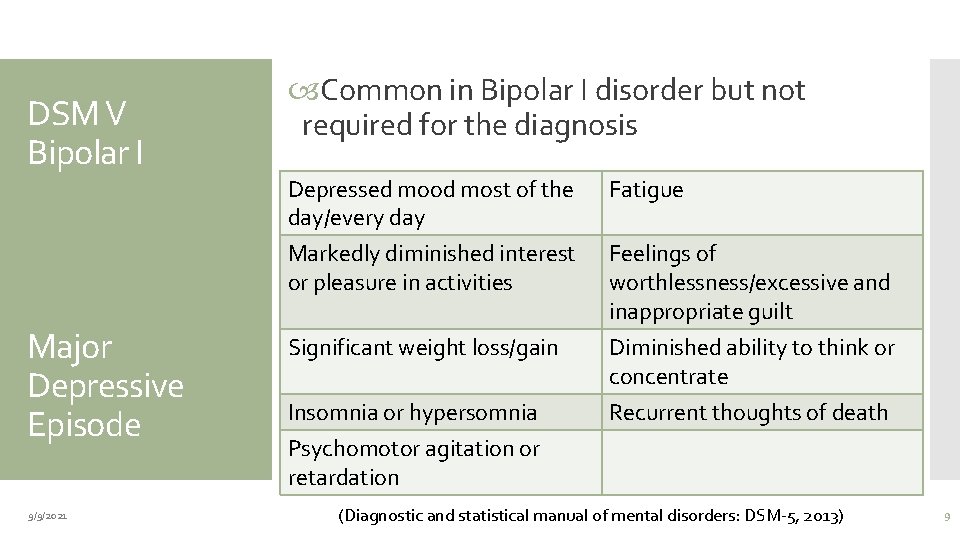
DSM V Bipolar I Major Depressive Episode 9/9/2021 Common in Bipolar I disorder but not required for the diagnosis Depressed mood most of the day/every day Fatigue Markedly diminished interest or pleasure in activities Feelings of worthlessness/excessive and inappropriate guilt Significant weight loss/gain Diminished ability to think or concentrate Recurrent thoughts of death Insomnia or hypersomnia Psychomotor agitation or retardation (Diagnostic and statistical manual of mental disorders: DSM-5, 2013) 9

DSM V Bipolar II 9/9/2021 For a diagnosis it is necessary to meet criteria for a current or past hypomanic episode AND the criteria for a current or past major depressive episode Never been a manic episode (Diagnostic and statistical manual of mental disorders: DSM-5, 2013) 10

Diagnosis has evolved so comparisons could be hard o. DSM III § Manic-depressive term replaced with BD Bipolar Prevalence o. DSM III-R § Diagnosis of Bipolar not otherwise specified o. DSM IV § Diagnosis of BD type 1 and BD type 2 o. DSM V § No studies as of 2013 Change in criteria was not great but significant increase in prevalence with DSM IV 9/9/2021 (Clemente et al. , 2015) 11

Boundaries remain unclear o Under-diagnosis—delayed ineffective treatment o Over-diagnosis—unnecessary exposure to medication Reflects movement away from diagnosis of Schizophrenia o “Lower” boundary Bipolar Trends § Subclinical mood conditions o “Lateral” boundary § Other mental health conditions (psychotic, anxiety, substance and personality disorders) o “Internal” boundary § Affective disorders § Mixed features that emerge in the context of depressive presentations (distractibility, agitation, irritability), which previously would have been regarded as superadded anxiety or agitated depression may now be subsumed by bipolarity 9/9/2021 (Sara & Malhi, 2015) 12
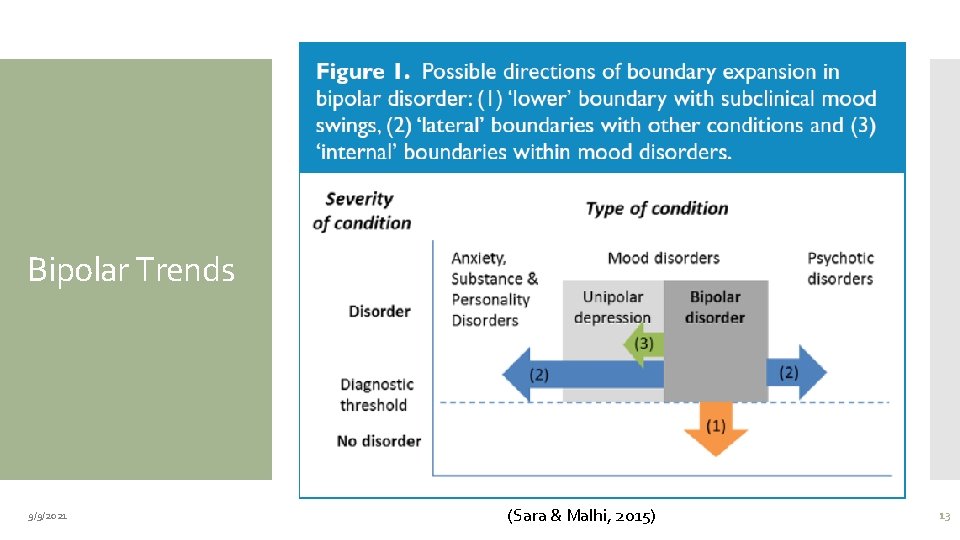
Bipolar Trends 9/9/2021 (Sara & Malhi, 2015) 13

Bipolar Trends 9/9/2021 Boundary Creep 1. Increased prevalence 2. Reduced average of individuals being treated 3. Reduced average of first diagnosis (Sara & Malhi, 2015) 14
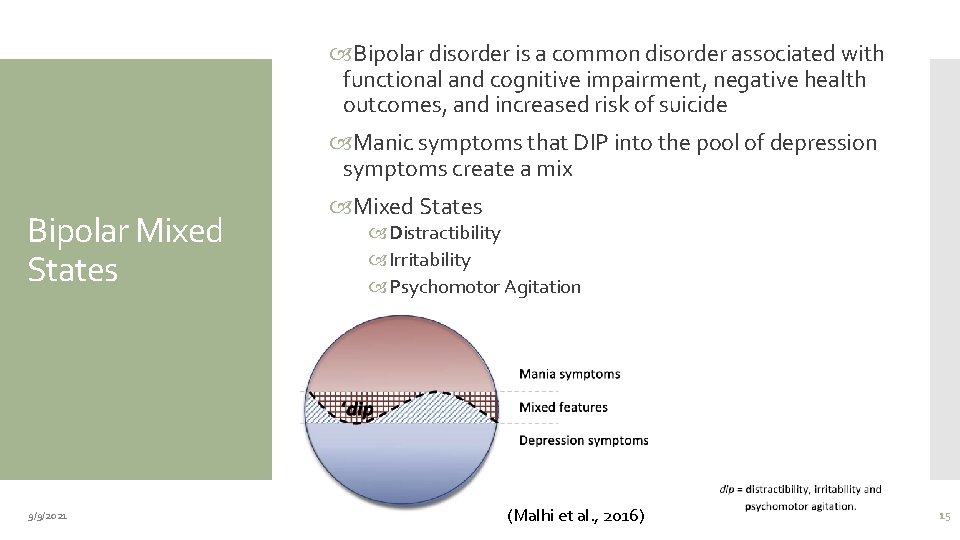
Bipolar disorder is a common disorder associated with functional and cognitive impairment, negative health outcomes, and increased risk of suicide Manic symptoms that DIP into the pool of depression symptoms create a mix Bipolar Mixed States 9/9/2021 Mixed States Distractibility Irritability Psychomotor Agitation (Malhi et al. , 2016) 15

Depressive onset is the most frequent type of onset—up to 66% Bipolar mixed states 9/9/2021 o. More frequently associated in females o. Higher number of recurrences o. Longer illness duration o. Rapid cycling course o. Higher suicidality rates o. Chronicity o. Anxiety comorbidity (Tundo et al. , 2015) 16

Manic onset (17%) Bipolar Mixed States 9/9/2021 o. Unmarried patients o. High number of hospitalizations o. Subsequent manic episodes o. Lifetime psychotic symptoms o. Comorbid alcohol misuse (Tundo et al. , 2015) 17

Mixed onset (15%) Bipolar Mixed States o. More frequent among females o. Subsequent mixed and depressive episodes with a higher-than expected frequency o. Low rates of remission o. High suicide attempts o. Comorbidity o. Negligible rate of rapid cycling course o. Poor response to treatment The number of episodes reported by patients is inaccurate (Martino et al. , 2016) 9/9/2021 (Tundo et al. , 2015) 18

Cognitive impairment is among the most common features of bipolar (and MDD) Bipolar and Executive Function 9/9/2021 o. During manic and depressive episodes o. Remain during euthymia and remission o. Causes functional impairment o. Impacts treatment response Executive Function o. Goal directed cognitive abilities o. Inhibitory control o. Cognitive flexibility o. Working memory (Cotrena et al. , 2016) 19

Executive impairments in BD Bipolar and Executive Function o. Abnormalities in frontolimbic circuits o. Reduced gene expression and neural density in the medial prefrontal cortex o. Volumetric reductions in the cingulate and frontoinsular cortices May be as severe as those identified in schizophrenia MDD is the 4 th largest cause of disability in the world BD o. Induce unemployment rates as high as 65% o. Render up to 75% of patients unable to return to premorbid levels of functioning 9/9/2021 (Cotrena et al. , 2016) 20

Bipolar disorder associated with sleep disturbances (Karthick et al. , 2015; Steinan et al. , 2016) Relationship between circadian rhythm-related genes and bipolar (Karthick et al. , 2015) Bipolar and Sleep 40% in remission have impaired sleep (Karthick et al. , 2015) Sleep disturbances may occur in 30 -60% of cases (Steinan et al. , 2016) Sleep disturbances during euthymic phase did not correlate well with core symptoms of depression o Sleep disturbances associated with but independent of affective symptoms (Karthick et al. , 2015) 9/9/2021 21

Bipolar and Sleep Suggested that medication nonadherence was the only independent predictor of poor sleep quality Sleep disturbances have also been noted to predate the onset of a new affective episode Nonpharmacological strategies Cognitive Behavioral Therapy o. Sleep Aids o. Daily regular sleep schedules 9/9/2021 (Karthick et al. , 2015) 22

Bipolar disorder has the highest comorbidity with SUD (substance use disorder) of all mental health disorders Life time prevalence Bipolar and Substance Abuse 9/9/2021 o 58% alcohol o 38% all other drug use Associated with impulsivity and self medication Most develop SUD prior to onset of BD Current substance abuse associated with threefold increase in the risk of violence (Alniak, Erkiran, & Mutlu, 2016) 23

Impulsivity does not predict violence SUD more effective predictor of violence Bipolar and Substance Abuse o. CSU much more predictive o. Youth, male gender, low education, positive symptoms, manic episode, previous history of physical assaults o. Most likely victim is family Violent group more likely to have criminal record and history of incarceration 9/9/2021 (Alniak, Erkiran, & Mutlu, 2016) 24

Bipolar and Seasonal Distribution 9/9/2021 Major mood episodes with main peak in spring–summer Smaller peak in Autumn for manic episodes Main peak in early winter and smaller peak in summer for depressive episodes The seasonal manic presentation of a subset cohort could be an epiphenomenon of a disrupted sleepwake cycle (Hochman et al. , 2016) 25

Bipolar and Obesity Patients with obesity seem to be prone to developing bipolar spectrum disorders and they present with specific personality traits High trait associations: o. Neuroticism Low trait associations: o. Conscientiousness o. Agreeableness 9/9/2021 (Dudek et al. , 2016) 26

Comorbidity of OCD and BD: Bipolar and OCD 9/9/2021 o. Earlier onset of BD o. More suicidal attempts o. First affective episode more likely to be major depression o. Seasonality and rapid cycling seemed to be higher o. Increased vulnerability to impulsivity (Ozdemiroglu et al. , 2016) 27

Bipolar and Cognitive Function 9/9/2021 Symptomatic BD associated with the following domains: o. Impairments in work and employment o. Social o. Psychological o. Physical o. Environmental (Baune & Malhi, 2016) 28

Work: Bipolar and Cognitive Function o. Disturbed work continuity (days off due to illness) o. Interpersonal problems with colleagues o. Stigma associated with disclosure of mental illness o. Compromise in social functioning Family: o. More likely to be separated, widowed, or divorced o 93% of care takers of patients with BD report at least moderate distress o Work, social, leisure time Dysfunctions persist long after symptomatic recovery 9/9/2021 (Baune & Malhi, 2016) 29

Cognitive Function: Bipolar and Cognitive Function 9/9/2021 o. Short and long term memory o. Executive functioning o. Verbal learning and memory o. Attention o. Processing speed (Baune & Malhi, 2016) 30

Differences in personality traits of MDD and BD when in the depressive state: o. Difficult to differentiate during depressive episode o. Five Factors of Personality § Agreeableness Bipolar and Personality Traits § Higher levels of A among cases of MDD compared to BD § Agreeableness is a dimension characterized by internal dispositions and attitudes related essentially to comprehension regarding others § Damage to one’s vision of self, grandiosity, inflated self-esteem § Conscientiousness § Extroversion § No difference § Neuroticism § No difference § Openness to Experience § No difference 9/9/2021 (Araujo et al. , 2016) 31

Bipolar and Long Term Work Disability 9/9/2021 Among 20 leading causes of disability worldwide 30 -60% of patients with BD even in syndromic remission are unable to attain their socio-vocational potential Work impairment similar to schizophrenia High rates of unemployment Failure to return o work following an episode High rate of work impairment (Arvilommi et al. , 2015) 32

After acute episode: Bipolar and Long Term Work Disability 9/9/2021 o 25% of patients granted a disability pension o. Predicted by higher age, male gender, depressive index episode, comorbidity with GAD or avoidant personality disorder, higher number of psychiatric hospital treatments o. Patients estimate of vocational abilities were surprisingly accurate (Arvilommi et al. , 2015) 33

Bipolar Assessment Tools Screening can be time consuming and costly while clinical benefits at the individual level may be significant—it is not known if the economic costs to the healthcare system support such an approach Screening tool should be brief and easy to complete by patients Mood disorder questionnaire (MDQ)– 13 questions o. Validated using DSM IV o 9/10 patients without BD successfully excluded o 7/10 patients with BD detected o 7/13 positive responses to the symptom-clustering provided good sensitivity 9/9/2021 (Baldassano, 2005) 34

Diagnosing Considerations: Bipolar Assessment Tools 9/9/2021 o. Current symptoms o. Historic symptoms o. Family history of mood disorders o. Response to previous treatment o. Complete medical history o. Complete physical exam o. Laboratory evaluation o. Substance abuse (Baldassano, 2005) 35

Bipolar Assessment Tools MDQ 9/9/2021 36
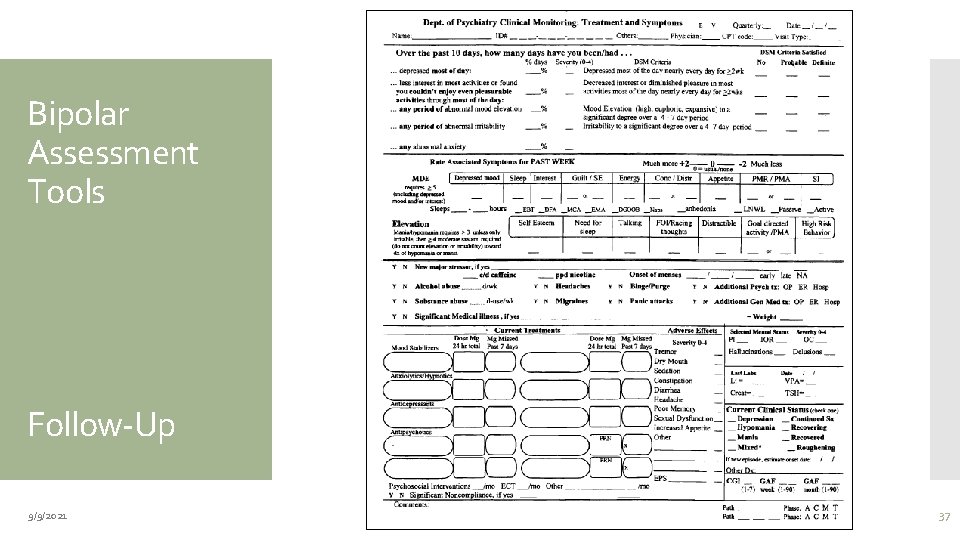
Bipolar Assessment Tools Follow-Up 9/9/2021 37

60 -70% of women with BD experienced mood episodes during pregnancy/postpartum period Risks if untreated: Bipolar and Pregnancy o Preterm labor o Decreased birth weight o Elevated levels of fetal stress hormones o Changes in neurobehavioral function of the infant Most likely diagnosed as depression therefore treated with antidepressant rather than mood stabilizers 5. 1% of prenatal, non-psychiatric population screened positive for high risk of BD Similar to 4. 4% lifetime prevalence of U. S. general population If screen for BD only in the previously depressed patients will miss 1/3 of BD cases 9/9/2021 (Merrill et al. , 2015) 38

Patients with more severe symptoms are associated with worse adherence Manic symptoms more likely to be non-adherent and can occur due to: Bipolar Disorder Compliance o Lack of insight o Distractibility o Lack of routine o Desire to prolong or maintain euphoria or sense of well-being Depression often outlasts and overshadows manic episodes over the life of an individual with BD o Cognitive impairment o Forgetting o Motivation More sever depressive symptoms were also associated with worse adherence High risk of relapse and poor prognosis 9/9/2021 (Sajatovic et al. , 2015) 39

Bipolar and ECT might carry an intrinsic mood-stabilizing effect with a positive implication for the freeinterval Significant reduction in morbidity Decreased number of hospitalizations— 90% Decreased number of episodes— 81% Increased usage of antidepressants Might influence cycle therefore contribute to relapses 9/9/2021 (Minnai et al. , 2016) 40

Bipolar Disorder Treatment Remember: BD is a chronic reoccurring illness associated with substantial morbidity and mortality Antidepressants o. Controversial Polytherapy is common o. Better adherence 9/9/2021 (Chang et al. , 2016) 41

Overtime— 10 year study o. Monotherapy—polypharmacy o. FGAs—SGAs Bipolar Disorder Treatment § SGAs associated with metabolic complications—weight gain, dyslipidemia, and diabetes o. Newly diagnosed BD patients received ADs in first year of treatment § Overtime significant decrease in AD use o. TCAs and SSRI decreased § SNRIs significantly increased o. Lithium and carbamazepine decreased § Valproate and lamotrigine increased o. BZDs have decreased 9/9/2021 (Chang et al. , 2016) 42

Bipolar Disorder Treatment 9/9/2021 Good responders were on an average of 3 drugs at any time during their treatment Lithium 49. 3% > carbamazepine 39. 9% Valproate 34. 8% > atypical 20. 7% Antidepressant 17. 8% > typical antipsychotic 11. 8% (Post et al. , 2016) 43

Lithium used as BD treatment for over 60 years Bipolar Disorder Treatment 9/9/2021 o. Prolonged duration of relapse o. Manic phase responded well (better than depression) o. Reduced suicide risk by 80% o. Adverse effects upon discontinuation: § Nausea § Diarrhea § Polyuria § Tremors (Shan, Makmor-Bakry, & Omar, 2016) 44

Factors associated with good lithium response: Bipolar Disorder Treatment 9/9/2021 o. Older age of disease onset o. Early onset of treatment o. Shorter lifetime inter-episode duration o. Longer first inter episode duration after lithium was started o. Higher morbidity burden (Shan, Makmor-Bakry, & Omar, 2016) 45
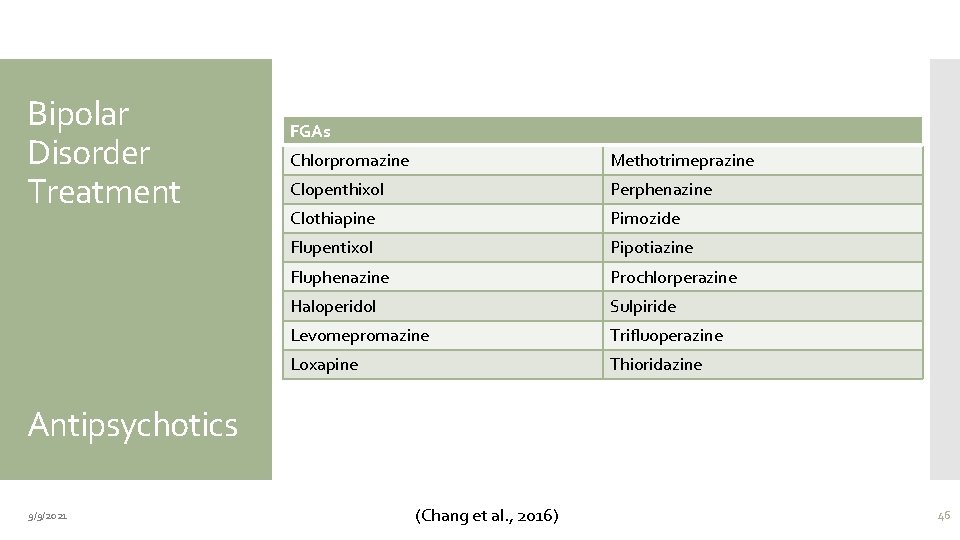
Bipolar Disorder Treatment FGAs Chlorpromazine Methotrimeprazine Clopenthixol Perphenazine Clothiapine Pimozide Flupentixol Pipotiazine Fluphenazine Prochlorperazine Haloperidol Sulpiride Levomepromazine Trifluoperazine Loxapine Thioridazine Antipsychotics 9/9/2021 (Chang et al. , 2016) 46
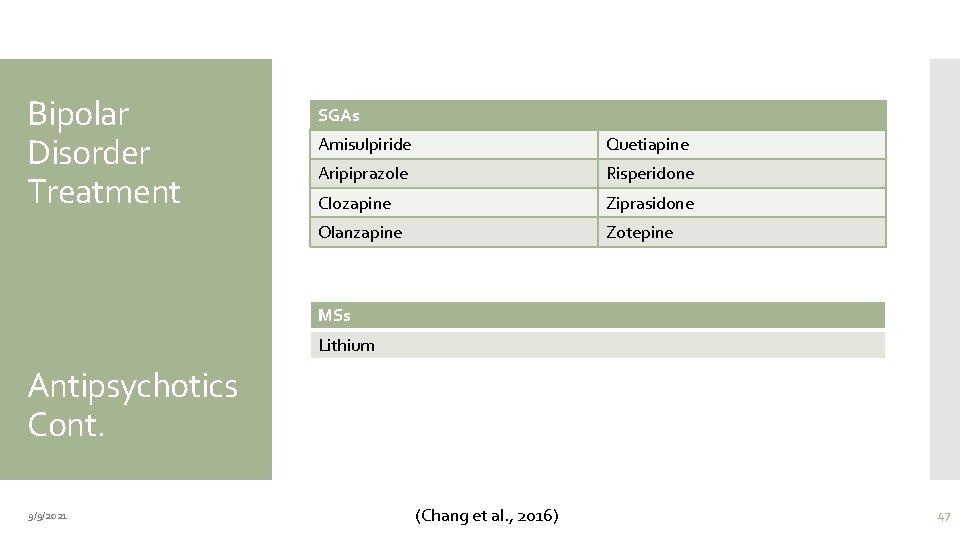
Bipolar Disorder Treatment SGAs Amisulpiride Quetiapine Aripiprazole Risperidone Clozapine Ziprasidone Olanzapine Zotepine MSs Lithium Antipsychotics Cont. 9/9/2021 (Chang et al. , 2016) 47
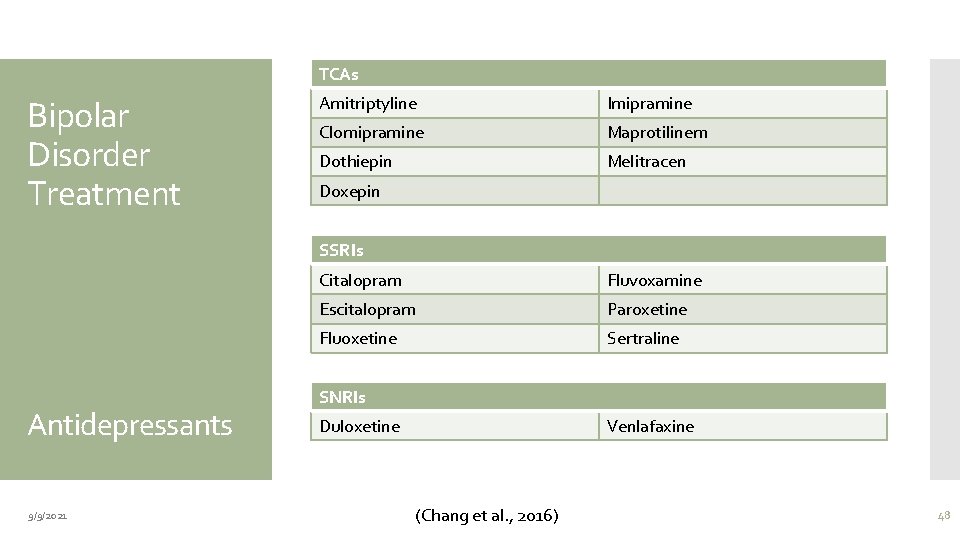
TCAs Bipolar Disorder Treatment Amitriptyline Imipramine Clomipramine Maprotilinem Dothiepin Melitracen Doxepin SSRIs Antidepressants 9/9/2021 Citalopram Fluvoxamine Escitalopram Paroxetine Fluoxetine Sertraline SNRIs Duloxetine Venlafaxine (Chang et al. , 2016) 48
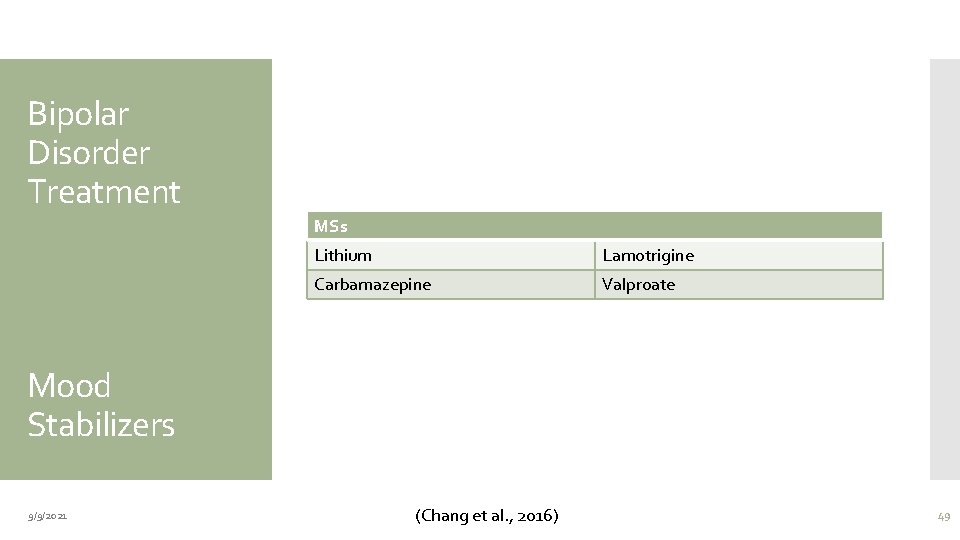
Bipolar Disorder Treatment MSs Lithium Lamotrigine Carbamazepine Valproate Mood Stabilizers 9/9/2021 (Chang et al. , 2016) 49
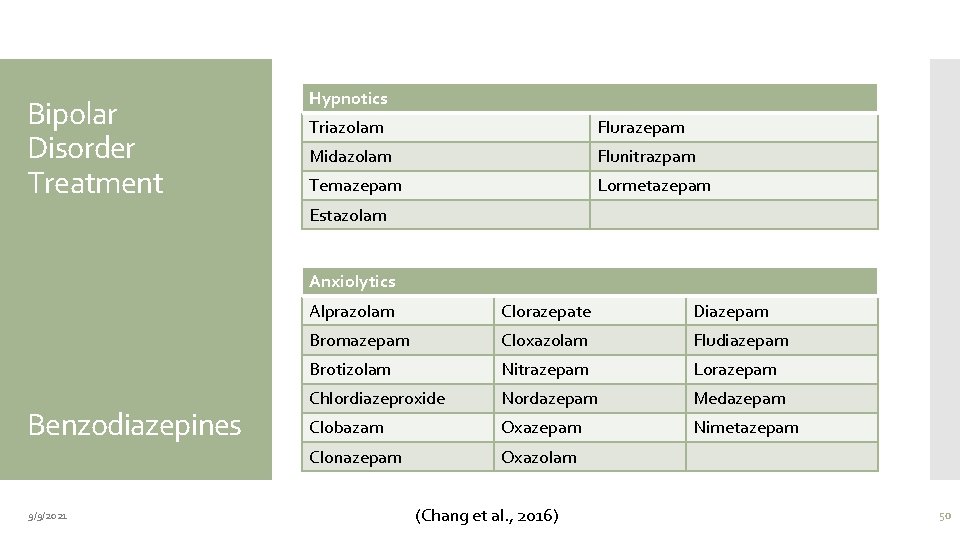
Bipolar Disorder Treatment Hypnotics Triazolam Flurazepam Midazolam Flunitrazpam Temazepam Lormetazepam Estazolam Anxiolytics Benzodiazepines 9/9/2021 Alprazolam Clorazepate Diazepam Bromazepam Cloxazolam Fludiazepam Brotizolam Nitrazepam Lorazepam Chlordiazeproxide Nordazepam Medazepam Clobazam Oxazepam Nimetazepam Clonazepam Oxazolam (Chang et al. , 2016) 50

Alniak, I. , Erkiran, M. , & Mutlu, E. (2016). Substance use is a risk factor for violent behavior I male patients with bipolar disorder. Journal of Affective Disorders, 193. Araujo, J. , Passos, M. , Molina, M. , Dilva, R. , Souza, L. (2016). Personality traits in the differentiation of major depressive disorder and bipolar disorder during a depressive episode. Psychiatry Research, 236. Arvilommi, P. , Suominen, K. , Mantere, O. , Valtonen, H. , Leppamaki, S. , Isometsa, E. (2015). Predictors of longterm work disability among patients with type I and II bipolar disorder: A prospective 18 month follow-up study. Bipolar Disorders, 17. Baldassano, C. F. (2005). Assessment tools for screening and monitoring bipolar disorder. Bipolar Disorders, 7. Baune, B. T. , Malhi, G. S. (2015). A review on the impact of cognitive dysfunction on social, occupational, and general functional outcomes in bipolar disorder. Bipolar Disorder, 17. References Chang, C. , Wu, C. , Huang, Y. , Chau, Y. , Tsai, H. (2016). Utilization of psychopharmacological treatment among patients with newly diagnosed bipolar disorder from 2001 to 2010. Journal of Clinical Psychopharmacology, 36. Clemente, A. S. , Diniz, B. S. , Nicolato, R. , Kapczinski, F. P. , Soares, J. C. , Firmo, J. O. , & Castro-Costa, E. (2015). Bipolar disorder prevalence: a systematic review and meta-analysis of the literature. Revista Brasileira de Psiquiatria, 37. doi: 10. 1590/1516 -4446 -2012 -1693 Cotrena, C. , Branco, L. D. , Shansis, F. M. , Fonseca, R. P. (2016). Executive function impairments in depression and bipolar disorder: association with functional impairment and quality of life. Journal of Affective Disorders, 190. Diagnostic and statistical manual of mental disorders: DSM-5. (2013). Washington, D. C. : American Psychiatric Association. Dudek, D. , Siwek, M. , Jaeschke, R. , Dembinska-kiec, A. , Arcoszewsla. A. , Hebal, F. , Matlok, M. , Major, P. , Malczewska-Malec, M. , Wnek, D. , Pilecki, M. , Rybakowski, J. (2015). Relationships between obesity, bipolar spectrum features, and personality traits: a case-control study. Eurpean Review for Medical and Pharmacological Sciences, 19. Hochman, E. , Valevski, A. , Onn, R. , Weizman, A. , Krivoy, A. (2016). Seasonal pattern of manic episode admissions among bipolar I disorder patients is associated with male gender and presence of psychotic features. Journal of Affective Disorder, 190. Karthick, S. , Kattimani, S. , Sarkar, S. , Bharadwaj, B. , Rajkumar, R. P. (2015). Quality of sleep in patients with bipolar I disorder. Journal of Psychiatic Practice, 21. 9/9/2021 51

Malhi, G. S. , Fritz, K. , Allwang, C. , Burston, N. , Cocks, C. , Devlin, J. , Harper, M. , Hoadley, B. , Kearney, B. , Klug, P. , Meagher, L. , Rowe, M. , Samir, H. , Way, R. , Wilson, C. , Lyndon, W. (2016). Are manic symptoms that ‘dip’ into depression the essence of mixed features? . Journal of Affective Disorder, 192. Martino, D. J. , Marengo, E. , Igoa, A. , Scapola, M. , Urtueta-Baamonde, M. , Strejilevich, S. A. (2016). Accuracy of the number of previous episodes reported by patients with bipolar disorder. Comprehensive Psychiatry, 65. Merrill, L. , Mittal, L. , Nicoloro, J. , Caiozzo, C. , Maciejewski, P. K. , Miller, L. (2015). Screening for bipolar disorder during pregnancy. Arch Womens Mental Health, 18. Minnai, G. P. , Salis, P. , Manchia, M. , Pinna, M. , Tondo, L. (2016). What happens to the course of bipolar disorder after electroconvulsive therapy? Journal of Affective Disorders, 195. Ozdemiroglu, F. , Sevincok, L. , Sen, G. , Mersin, S. , Kocabas, O. , Karakus, K. , Vahapoglu, F. (2015). Comorbid obsessive-compulsive disorder with bipolar disorder: A distinct form? . Psychiatry Research, 230. References Post, R. M. , Leverich, G. S. , Kupka, R. , Keck, P. E. , Mc. Elroy, S. L. , Altshuler, L. L. , Frye, M. A. , Rowe, M. , Grunze, HJ. , Suppes, T. , Nolen, W. A. (2016). Clinical correlates of sustained response to individual drugs used in naturalistic treatment of patients with bipolar disorder. Comprehensive Psychiatry, 66. Sajatovic, M. , Levin, J. , Sams, J. , Cassidy, K. A. , Akagi, K. , Aebi, M. E. , Ramirez, L. F. , Safren, S. A. , Tatsuoka, C. (2015). Symptom severity, self-reported adherence, and electronic pill monitoring in poorly adherent patients with bipolar disorder. Bipolar Disorder, 17. Sara, G. E. , & Malhi, G. S. (2015). Trends in diagnosis of bipolar disorder: Have the boundaries changed? Australian & New Zealand Journal of Psychiatry, 49. doi: 10. 1177/0004867415607987 Shan, G. W. , Makmor-Bakry, M. , Omar, M. S. (2016). Long term use of lithium and factors associated with treatment response among patients with bipolar disorder. Psychiatria Danubina, 28. Steinan, M. K. , Morken, G. , Lagerberg, T. V. , Melle, I. , Andreassen, O. A. , Vaaler, A. E. , Scott, J. (2016). Delayed sleep phase: An important circadian subtype of sleep disturbance in bipolar disorders. Journal of Affective Disorders, 191. Tundo, A. , Musetti, L. , Benedetti, A. , Berti, B. , Massimetti, G. , Dell’Osso, L. (2015). Onset polarity and illness course in bipolar I and II disorders: The predictive role of broadly defined mixed states. Comprehensive Psychiatry, 63. 9/9/2021 52

Thank You!
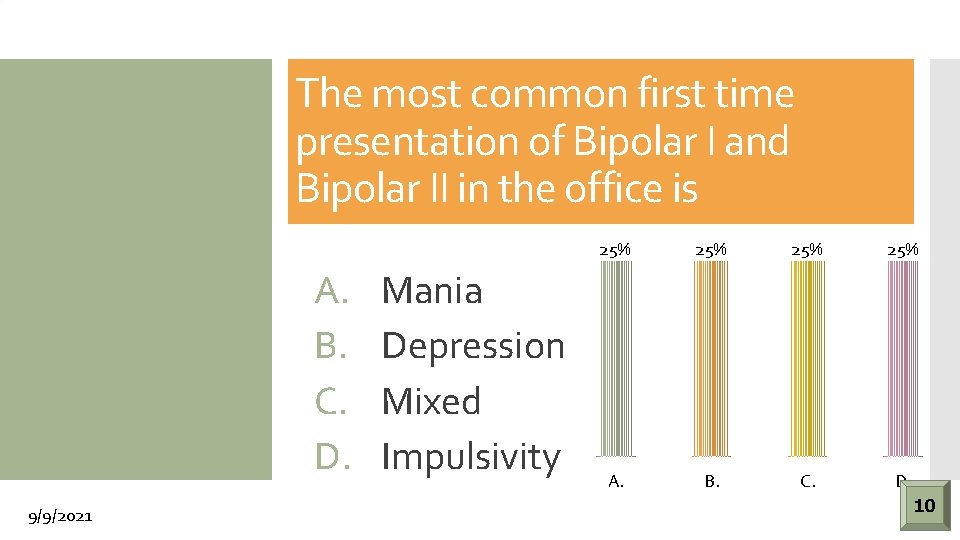
The most common first time presentation of Bipolar I and Bipolar II in the office is A. B. C. D. 9/9/2021 Mania Depression Mixed Impulsivity 25% 25% A. B. C. D. 1054

The first time BD is diagnosed the most common treatment is A. B. C. D. 9/9/2021 Antidepressants Antipsychotics Mood Stabilizers Benzodiazepines 25% 25% A. B. C. D. 1056
- Slides: 56