Febrile Neutropenia Chart Review and New Guideline Stephanie

Febrile Neutropenia Chart Review and New Guideline Stephanie Eason RN, CPHON Kids Rock Conference October 2014

Atlantic Canada Chart Review § APPHON reviewed charts of patients diagnosed with Febrile Neutropenia between Jan. 1, 2005 – Jan. 31, 2011 § NL; NS; NB; PEI § Janeway was only hospital in NL § Multiple sites in other provinces

Atlantic Canada Chart Review § Indicators examined were based on APPHON guideline for treatment of F/N: 1. time blood cultures were drawn 2. time antibiotics were started

How much time should pass between patient presentation and when blood cultures are drawn? 1. 2. 3. 10 minutes 30 minutes 1 hour

Time to Blood Cultures – Target: 30 Minutes § Atlantic Canada Department ER OPD Inpatient # cases 166 84 103 § Janeway Department ER MDC Inpatient # cases 39 17 20 mean (minutes) 93 86 71 mean (minutes) 73 67 27

WHY ? § § § Busy Sicker patients in ER Child does not appear unwell Unable to access CVAD Waiting for orders to be written

How much time should lapse between patient presentation and start of antibiotics? 1. 2. 3. 30 minutes 1 hour 2 hours
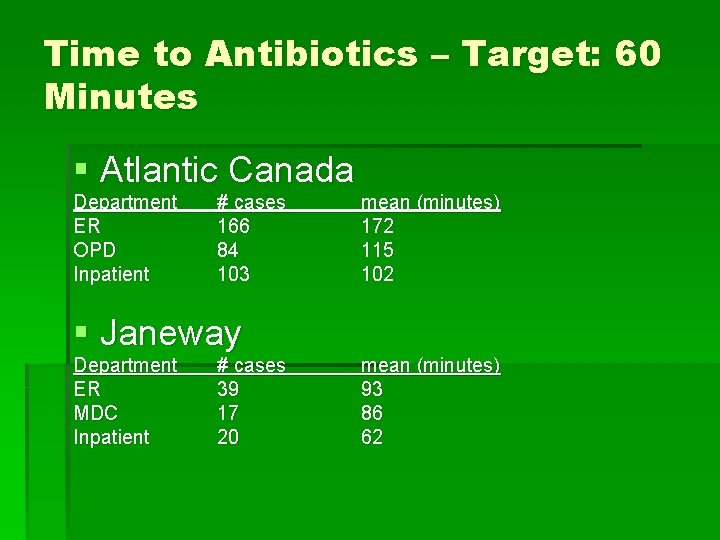
Time to Antibiotics – Target: 60 Minutes § Atlantic Canada Department ER OPD Inpatient # cases 166 84 103 § Janeway Department ER MDC Inpatient # cases 39 17 20 mean (minutes) 172 115 102 mean (minutes) 93 86 62

Why? § § § Waiting on lab results (CBC) Finding someone to access CVAD Busy Child does not look sick Not familiar with guideline for treatment Parent/patient interference

Conclusions § Significant time delays to drawing blood culture and to starting antibiotics across all departments and all sites. § Departments who saw more oncology patients were more likely to adhere to guideline.

Recommendations § More education is needed to disseminate APPHON Guideline for treatment of Febrile Neutropenia. § If CBC is not back in one hour—antibiotics need to be started. If it is later determined that the patient is not neutropenic, antibiotics can be discontinued. (increased rate of complications when abx delayed beyond 1 hour. Pediatric Blood and Cancer 60: 1299, 2013)


Definition of Fever* § Single elevation ≥ 38. 3 OC orally (37. 8 OC axillary) § Two elevations ≥ 38 OC orally (37. 5 OC axillary) taken at least 1 hour apart § Temperature taken by parents at home MUST be counted. * only for pediatric oncology patients

Definition: Neutropenia • ANC less than 0. 5 x 109/L OR 1 x 109/L and expected to fall ANC = (%segs + %bands) x total WBC count ------------------100 Mature neutrophils can be called neutrophils or segs. Immature neutrophils can be called stabs or bands.
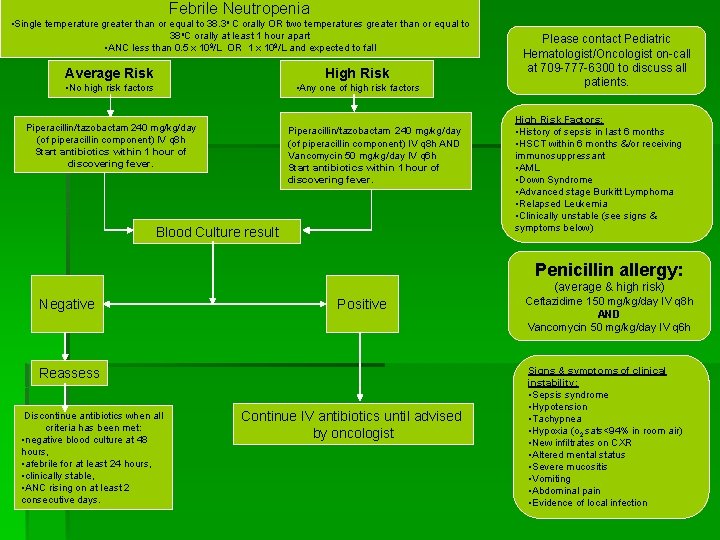
Febrile Neutropenia • Single temperature greater than or equal to 38. 3 o C orally OR two temperatures greater than or equal to 38 o. C orally at least 1 hour apart • ANC less than 0. 5 x 109/L OR 1 x 109/L and expected to fall Average Risk High Risk • No high risk factors • Any one of high risk factors Piperacillin/tazobactam 240 mg/kg/day (of piperacillin component) IV q 8 h Start antibiotics within 1 hour of discovering fever. Piperacillin/tazobactam 240 mg/kg/day (of piperacillin component) IV q 8 h AND Vancomycin 50 mg/kg/day IV q 6 h Start antibiotics within 1 hour of discovering fever. Blood Culture result Please contact Pediatric Hematologist/Oncologist on-call at 709 -777 -6300 to discuss all patients. High Risk Factors: • History of sepsis in last 6 months • HSCT within 6 months &/or receiving immunosuppressant • AML • Down Syndrome • Advanced stage Burkitt Lymphoma • Relapsed Leukemia • Clinically unstable (see signs & symptoms below) Penicillin allergy: (average & high risk) Negative Positive Reassess Discontinue antibiotics when all criteria has been met: • negative blood culture at 48 hours, • afebrile for at least 24 hours, • clinically stable, • ANC rising on at least 2 consecutive days. Continue IV antibiotics until advised by oncologist Ceftazidime 150 mg/kg/day IV q 8 h AND Vancomycin 50 mg/kg/day IV q 6 h Signs & symptoms of clinical instability: • Sepsis syndrome • Hypotension • Tachypnea • Hypoxia (o 2 sats<94% in room air) • New infiltrates on CXR • Altered mental status • Severe mucositis • Vomiting • Abdominal pain • Evidence of local infection

QUESTIONS ?


- Slides: 18