Family Medicine Preventive Medicine The Power of Collaboration

Family Medicine & Preventive Medicine The Power of Collaboration Sallie Rixey MD, MEd Franklin Square Family Medicine Baltimore Dominic Geffken, MD, MPH Family and Community Medicine Dartmouth Medical School
Primary Care Specialty Care Preventiv e Medicine Public Health
Determinants of health Health care spending
Effective Efficacious Equitable Family Medicine 3 E ACGME-6 Competency Preventive Medicine

Given …that there is a need for leadership and an appropriately trained workforce to improve our health care system Given …that there are overlapping competencies in preventive medicine and family medicine to train those leaders and that workforce

Is there an opportunity for family medicine programs…and preventive medicine programs …to partner and take advantage of the synergy?

Goals FMPM Collaborative Bring together interested individuals and organizations to share… – new ideas – methods – strategies for overcoming barriers – resources Establish a process for continuing to work together


Today Panel Introduction Audience Introduction Who are you? What do you hope to learn? Background Preventive Medicine-Miriam Alexander MD, MPH Panel: brief history structure and curriculum strengths, areas for focus, outcomes Q&A Next Steps-Would we like to stay connected…and if so, what would we like to accomplish, and how might we do that? Luncheon-Kelechi Uduhiri, MD, MS, MPH Franklin Square Enhancing Prevention and Population Health Education Modules http: //www. aptrweb. org/pophealthmodules/ APTR project, with Mary Applegate MD, MPH Albany Anatomy of a FM General Preventive Medicine Practicum-Kelechi Uduhiri

• Department of Preventive Medicine, Loma Linda University Jamie Osborn PD • Department of Family Medicine, Oregon Health & Science University BJ Lynch R 2, and Heidi Guillett, graduate and now faculty representing CWRU/UHCMC • Department of Community and Family Medicine Dominic Geffken PD, Dartmouth Medical School • Johns Hopkins Bloomberg School of Public Health, Miriam Alexander GPM PD, president of the ACPM • Franklin Square Family Medicine, Margarete Everts, Franklin Square R 2 and Kelechi Uduhiri, Director HCHBC • Mary Applegate, Associate Dean for Public Health Practice University at Albany School of Public Health

…your turn… • Name and where you are from • What you would like to get from today

Incorporating Population Medicine Into Primary Care Residency Training Family Medicine July-August 2011 Vol. 43, No. 7 Dysinger, King, Foster, Geffken • Population Medicine Competencies • Program Descriptions – Training locations and sample activities for Population Medicine Training • Graduate Statistics • Barriers and Benefits • Financial Models • Program Similarities and Differences

What is Preventive Medicine? n “Preventive Medicine” as a medical specialty is a misnomer – “Population Medicine” more accurately encompasses the specialty CLINICAL • Individual/family • Diagnosis and treatment oriented (2º and 3º prev) • Collaborate with healthcare system • Personal service ethic • Lucrative - ? PREVENTIVE • Defined populations • Prevention/health promotion oriented • Collaborate with many actors • Public service ethic

Some Unique Features of Preventive Medicine • Use of prevention as a primary intervention • Grounded in a broad array of sciences • Basis in social justice philosophy • Link with government and public policy Merson, Black, Mills (2001)

Preventive Medicine Competencies • • • Epidemiology Biostatistics Environmental Health Occupational Health Services Administration Social and Behavior Health Sciences Informatics Genomics Communication Cultural Competence Global Health Policy and Law • Public Health Ethics • Clinical and Community Preventive Services • Management and Administration • Policy and law • Ethics • Leadership • Clinical and Community Preventive Services • Public Health Emergency Preparedness • Community-based Participatory Research

Training in Preventive Medicine l Medical School (4 years) l Preventive Medicine Residency Training components over a minimum of 3 years) (3 • 1 year of direct patient care-standard clinical training • 2 years of preventive medicine rotations- core then specialized years • Graduate school education in preventive medicine-MPH or equivalent l Preventive Medicine Board Exam

Graduate Education Component • Core didactics of PM—epi, biostats, environmental, social/behavioral/health services • Advanced GPM: advanced epi, more health services, clinical preventive medicine, ethics, management, budgetting, qi/qa • Residents area of interest policy, epidemiology, maternal/child health, obesity/food, vaccines, international health, • 1 + 2 + 3 = MPH

But What Do Preventive Medicine Doctors Actually Do? • Use epidemiology to find high-risk groups and design successful programs • Enhance quality and efficiency in healthcare systems • Help shape national and state health policies • Improve the delivery of preventive services among underserved and high-risk populations • Identify health and safety hazards in the workplace • Direct public health programs at all levels of government

Careers • • Local and state health departments Federal agencies (DHHS, DOD, others) Private industry (consultancy, pharma, HMOs) Non-government organizations Hospitals Universities/academia (research, teaching) Direct one on one patient care --

To Make Man Whole • Full spectrum of primary care experiences through the Loma Linda University Family Medicine Residency Program • Comprehensive exposure to population-based care and health-care systems through the Loma Linda University Preventive Medicine Residency Program. • Master’s in Public Health through the Loma Linda University School of Public Health • Experience unique exposures to our two areas of strength » Lifestyle Medicine » Global Health
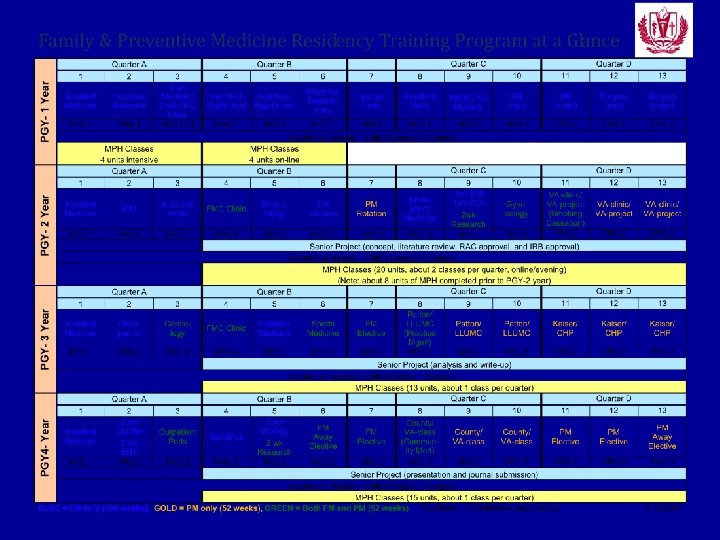

ABFM and ABPM board approval Combined 4 year Family Medicine Preventive Medicine Sallie Rixey MD, MEd Vice Chairman Department of Family Medicine Franklin Square Hospital Center Miriam Alexander MD, MPH Director General Preventive Medicine Johns Hopkins Bloomberg School of Public Health

The General Preventive Medicine Residency Program of the Johns Hopkins Bloomberg School of Public Health • One of the oldest preventive medicine residencies in the country • Over 400 physicians have completed the residency since its inception 1964 • Graduates have distinguished themselves in government, academia, industry, and international positions.

Mission To prepare physicians in theoretical, practical, and clinical knowledge and skills essential to leadership roles in the design, management, and evaluation of population-based approaches to health. Key goals: 1. to instill in residents the ability to synthesize clinical and populationbased approaches to disease prevention and health promotion 2. to view health issues on a broad continuum from local to international in perspective 3. to discover and apply knowledge toward the protection of the public's health 4. to provide residents with the management and epidemiologic skills needed to address the overall health needs of underserved populations 5. to provide residents with the clinical skills needed to treat specific diseases that disproportionately affect underserved populations.

FSFM • Med. Star Health – Not for profit regional system with 6 md and 3 dc hosp and diversified services from mri, vna, mpp, medicaid mco • 8 -8 -8 Family Medicine program in Baltimore County (2 o’clock on beltway) • Established in 1972 • FHC with 30, 000 visits per year • Rural training track in St Mary’s Co • HCH-BC • OB fellowship years when interest and funding available

• • • • • 2000 ACGME-6 – 6 FHC blocks (every semester, every year) March 2009 initial meeting with Dr. Alexander – Review of program requirements – Joint proposal drafted and vetted to both DIO’s July 2009 Joint proposal submitted to ABPM August 2009 rejected but interested August 2009 Michelle Cardona MD, MPH hired March 2010 Kelechi Uduhiri MD, MS, MPH hired June 2010 Faculty Development and pilot GPM practica July 2010 Joint proposal resubmitted to ABPM Feb 2011 ABPM approval June 2011 Joint proposal submitted to ABFM July 2011 ABFM approval July 2011 Marketing materials for Nationals July 2011 Posted on list serves September 2011 ADS number request and assigned October 2011 Request for increase in compliment October 20 2011 Increase in compliment granted October 2011 Interviewing timeline

FS/JHB • R 1 - Family Medicine Intern • R 2 – MPH coursework, 2 CC/wk, 1 call/block (13 blocks) • R 3 – Continue Family Medicine Residency with GPM Practicum • R 4 - Complete Family Medicine Residency GPM practicum with board eligibility in BOTH Family Medicine and Preventive Medicine

JHB GPM Practicum Rotations Management and Administration/Medical Management • Agency for Healthcare Research and Quality, Rockville, MD; *Tracy Wolff, MD, MPH • Anne Arundel County Department of Health, Annapolis, MD; Katherine Farrell, MD, MPH • Baltimore City Health Department, Baltimore, MD; Barbara Squires • Johns Hopkins Community Physicians, Baltimore, MD; Maura Mc. Guire, MD, MPH • National Institute for Allergy and Infectious Diseases, Bethesda, MD; Karl Western, MD • Public Citizen Health Research Group, Washington, DC; Sidney Wolfe, MD Biostatistics/Epidemiology • Anne Arundel County Department of Health, Annapolis, MD; Katherine Farrell, MD, MPH • Consultants in Epidemiology and Occupational Health, Washington, DC; Steven Lamm, MD, DTPH • Center for Biologics Evaluation and Research, Food and Drug Administration, Washington, DC; Robert Ball, MD, MPH • Indian Health Service; *James Cheek, MD, MPH • Special Program on Vaccines and Immunizations, Pan American Health Organization, Washington, DC (Jamaica/Guyana/Guatemala); Jon Andrus, MD • Public Citizen Health Research Group; Sidney Wolfe, MD Environmental/Occupational Medicine • Anne Arundel County Department of Health; Katherine Farrell, MD, MPH • Consultants in Epidemiology and Occupational Health, Washington, DC; Steven Lamm, MD, DTPH • Occupational Safety and Health Administration, Washington, DC; John Piacentino, MD, MPH • Maryland Department of the Environment, Baltimore, MD; *Philip Heard, MD, MPH • Maryland Department of Health and Mental Hygiene, Center for Maternal and Child Health, Baltimore, MD; Maureen Edwards, MD, MPH Clinical Preventive Medicine • Agency for Healthcare Research and Quality, Rockville, MD; *Tracy Wolff, MD, MPH • Johns Hopkins Community Physicians, Baltimore, MD; Maura Mc. Guire, MD, MPH

FS/JHB 13 equivalent blocks GPM • 8 blocks GPM practicum – blocked together either 2 -2 -2 -2 or 3 -3 -2 to allow for 8 -12 week rotations • 5 GPM practicum credits overlap with FM rotations – 2. 5 GPM credits from 4 FHC blocks – 1 occupational medicine credit from 2 blocks MS – 1. 5 GPM credits, 80 project hours for each of 3 of the following rotations (peds, OBG, Ger, ED) • 1 block of GPM = 160 hours (4 x 40 hours/wk) – Half block = 80 hours (4 x 20 hours / wk) • For FM residents (not combined program) – Longitudinal • 10 hrs / wk x 16 wks • 5 hrs / wk x 32 wks

Franklin Square Family Medicine Requirements • 6 total FHC blocks-1 block FHC every semester, every year – FHC curriculum – Allows for PCMH practicum in combined track • Minimum 1 block GPM practicum

Why should FM residents do GPM Practicum? Training doctors to build healthy communities

Family Physicians improve the health of communities when they are able to: • appreciate the importance of a population focus • learn to identify partners in the community • learn to identify gaps and barriers organizations experience in serving their clients • identify how different sectors (health and education) can reinforce each others limited resources • demonstrate proficiency in collaborating to improve the health of that population

FS/JHB Salary and Benefits • Stipend commensurate with FM resident • Complete benefits package from FS • R 2 year JH will remunerate equal to all of it’s R 2’s (MPH, stipend, meeting) and remainder from FS Vacation and Leave • FS policy for R 1, 3, 4 • JH policy for R 2 Co-Director oversight • DIO FS, JH RAC

Strengths � • Resources and commitment to excellence of the 2 institutions • Commitment to success by co-directors led to clear win/win discussions and transparency • Pilot residents • RRC and boards commitment to innovation (Perry Pugno and Terry Leigh) • The cloud and the times

� Areas of focus • Faculty development and culture change • FM-GPM practica, Occupational and Environmental Medicine • Interviewing schedules • Need to identify and recruit exceptional candidates because of work load • Lack of flexibility in the curriculum and coverage if down a resident • Ensure clear methods for double counting • 2 classes of residents clinically (reduced night float) • 2 institutions, 3 PD’s and agendas

outcomes • Preliminary data – 25% more US applicants – Step 1 and 2 scores noticeably higher – Applicants with MPH degrees – Resident interest in GPM practica

Combined Family Medicine Preventive Medicine Residency NH Dartmouth Family Medicine Residency and the Dartmouth Hitchcock Leadership Preventive Medicine Residency Dominic F. Geffken, MD, MPH October 22, 2011

Aim • PROGRAM AIM: To attract and develop physicians capable of leading the change and improvement of the systems where people and health care meet. In conjunction with existing clinical residency and fellowship programs, participants’ academic, applied leadership and practicum experiences in preventive medicine will focus on measuring outcomes and improving the technical, service and cost excellence of care for patients and populations.

Basics • NH Dartmouth Family Medicine Residency is a community based, unopposed Family Medicine Residency in Concord, NH. • Dartmouth Hitchcock Leadership Preventive Medicine Residency based at the Dartmouth Medical School. • MPH courses taken at The Dartmouth Institute. • Quality Improvement projects are conducted in the Family Health Center in Concord.
Where we are

Schedule-Years Year 1 Family Med Residency Year 2 Family Med Residency Year 3 Family Med Residency Year 4 Preventive Med Residency MPH courses / Prework for project Preventive Med Residency QI Project / Public Health work Year 5
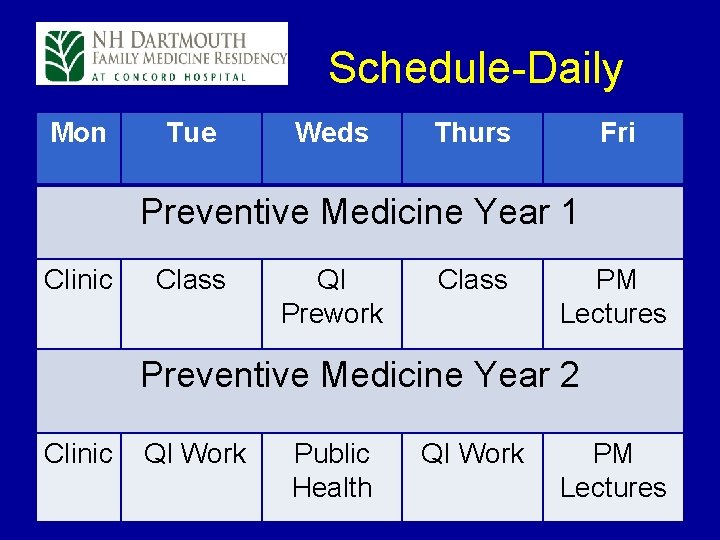
Schedule-Daily Mon Tue Weds Thurs Fri Preventive Medicine Year 1 Clinic Class QI Prework Class PM Lectures Preventive Medicine Year 2 Clinic QI Work Public Health QI Work PM Lectures

Unique Components • MPH Courses – 3 courses on implementation and measurement of QI projects. • Leadership training is a major component of the program • Each resident in the program has a coach that helps them form / implement QI Project. • PM builds on Team Membership skills taught in Family Medicine

What residents say • Role of the physician is evolving from treating patient to treating a population of patients consistently with the best evidence. Our job is to ensure ALL patients receive the right care at the right place, and at the right time. . . not just when we remember to • Understand your data and your clinic processes; there is variation among teams within the same department. Study representative tests from different processes and use the “clues” you find along the way to make change

What faculty say • The LPMR has attracted a higher caliber group of residents to the residency. • LPMR residents help transfer ideas of distributive leadership to rest of team. • LPMR residents bring new tools to measure QI projects to health center.

Where our graduates work • Faculty in family medicine residency • Leadership / QI in Health Care Organizations • Executive Leader in start up Health Care Organization. • Community Health Center QI Leader.

Acknowledgements • • • Dan Eubank, MD Paul Batalden , MD Wayne Dysinger, MD Carolyn Murray, MD, MPH Tina Foster, MD, MPH Gail Fayre, MD

Combined Residency in Family Medicine and Preventive Medicine Cleveland, Ohio

CWRU/UHCMC Mission: To foster resident individuality, growth and leadership in an academically rich and culturally diverse urban environment, emphasizing the development of excellent clinical skills in preventive care and expertise in applying and contributing to the scientific base for preventive medicine and public health practice.

CWRU/UHCMC • Both residencies in the Dept of Family Medicine – Separate FM and PM program directors – Both PDs are Family Medicine faculty • Training in both specialties over 4 years • Complete coursework at CWRU with option to obtain MPH • Complete a public health practicum during the fourth year

CWRU/UHCMC • R 1 - Family Medicine Intern • R 2 - Family Medicine Resident, start coursework • R 3 - Complete Family Medicine residency, continue coursework • R 4 - Complete coursework, Preventive Medicine practicum • Board eligibility in BOTH Family Medicine and Preventive Medicine

CWRU/UHCMC Partners • • Cuyahoga County Board of Health Cleveland Department of Public Health Shaker Heights Health Department Future directions: – Mc. Gregor Skilled Care Facility – Columbus Department of Health

History of PM Residency • Long history of FM residents pursuing MPH • First graduate 2011 with interests in medical informatics and computer modeling • Currently 1 PM resident with strong interest in Geriatrics • No FM/PM combined resident YET – No application thus far to ABFM/ABPM • Currently 2 PM-boarded CWRU faculty – Recent graduate also completed boards Oct. 2011 • Partnership with NEOMED – Multiple FM and PM dual boarded faculty

Combined Residency in Family Medicine, Public Health, and General Preventive Medicine Portland, Oregon

OHSU • Department of Family Medicine – FM program director, Combined track program director, both FM faculty • Department of Public Health and Preventive Medicine – PM program director • Training in both specialties over 4 years • Option to complete MPH through Oregon MPH program (OHSU, PSU, OSU) – Epi/Biostats or Health Management and Policy • Complete public health practicum during the fourth year

OHSU • R 1 - Family Medicine Intern • R 2 - Family Medicine Resident, start coursework • R 3 - Complete Family Medicine residency, continue coursework, electives • R 4 - Complete coursework, Preventive Medicine practicum • Board eligibility in BOTH Family Medicine and Preventive Medicine

History of FM/PM OHSU Residency • • 20 combined track graduates 2 combined track residents per year Separate match number through NRMP Board certification – FM: 20/20 – PM: 17/18, plus 2 board-eligible (2011 graduates) • MPH: 20/20 – Some residents entered with prior MPH

OHSU • Strong partnership with Portland State University - MPH coursework and faculty • Example Practicum Experiences: – Multnomah County Health Department – Oregon Health Department • Health Services Commission • Division of Epidemiology; Maternal/Child Health – Care. Oregon – Clackamas County Public Health Division – FQHCs

What do FM/PM trained physicians do? • Clinical Care – Clinical Preventive Medicine – Quality Improvement – Integration of PCMH – Leadership in care for underserved populations • FQHCs • RHCs

What do FM/PM trained physicians do? • Public Health/ Health Administration – Local public health officers – State public health officers – Epidemiologists – Medical directors for population-based entities • Medicaid managed care organizations • ACOs

What do FM/PM trained physicians do? • Health Policy/Research/Academic – Local level (clinic/organization, city, community) – State level • Reform (Oregon Health Services Commission) – National level • CDC (HIV/AIDS policy in Africa)

What do FM/PM trained physicians do? • International Opportunities – European CDC – WHO – NGO Health Advisor/Epidemiologist – Pediatric AIDS Corps

Why is this training useful for Family physicians? • Role of primary care providers in health system • Obtain invaluable perspective on caring for both individual patients and populations • Develop skills in systems-based practice and improvement • Develop broader perspective on what factors influence health

OHSU QI Systems-Based Practice Curriculum • FM/PM residents designed QI curriculum for all FM residents • Assistance of PSU MPH Advisor • Didactics focused during core months • Progressive curriculum – Personal Improvement Project • Month long practical experience in QI principles – Clinic-based Project • Year-long, team lead by FM faculty member and FM/PM R 4 – Community-based Project

How is Preventive Medicine different? • • Public health physicians Our patients are not just individuals, but also populations Prevention is central What instruments do we use? – Disease surveillance – Data analysis – Education – Advocacy – Policy – Program design – Research

Q&A Next Steps-Would we like to stay connected…and if so, what would we like to accomplish, and how might we do that? Luncheon-Kelechi Uduhiri, MD, MS, MPH Franklin Square Enhancing Prevention and Population Health Education Modules http: //www. aptrweb. org/pophealthmodules/ APTR project, with Mary Applegate MD, MPH Anatomy of a GPM Practicum for FM residents Health Care for the Homeless-Kelechi Uduhiri

• Brody School of Medicine Department of Public at East Carolina University • Duke University School of Medicine and School of Public Health • University at Albany, State University of New York with funding from the Centers for Disease Control. Featuring Educational Modules on: · Determinants of Health · Fundamentals of Epidemiology · Taking a Preventive History · Screening · Health Care Systems · Research to Practice · Outbreak Investigation and Disease Control This curriculum will feature Power Point presentations produced by subject-matter experts, supplemental materials to facilitate small group learning, and a bibliography of key resources.

Thank You Audience Panel FMEC
- Slides: 68