Family Medicine John Brill MD MPH Alan Wolkenstein

Family Medicine John Brill, MD, MPH Alan Wolkenstein, MSW Hamilton Jeyaraj, MD, PG 3

Goals 1. 2. 3. v Discuss strategies for teaching behavioral sciences, community medicine and practice management Present our longitudinal curriculum using common family medicine visits to teach these areas Discuss strategies for small group learning using ‘PBL’ Share evaluation results and resident perspectives on the curriculum

Why Change? Problems & Opportunities v One month rotation for each area v Different faculty v No linkages/ connection v Rotations consistently rated among ‘least useful’ in resident survey v Concern regarding isolating these areas from ‘the science’ of family medicine v v RRC recommendations for longitudinal training in Behav Science Opportunity to create an experiential bridge between patients’ health concerns and residents’ limited experiences Changing from month-long to 4 week block rotation schedule Community Med faculty program director

Before/After Commun Med- 1 month v Psych- 1 month v Pract Mgmt- 1 month v Total 3/36 months; 8. 5% Curriculum; 33 other months, 4 electives v Fam Med– 6 weeks/year v Integrated Comm Med, Psych, Pract Mgmt v Total 18/156 weeks; 11. 5% curriculum; 34. 5 other 4 -week blocks, 4. 5 electives v

Family Medicine Curriculum Goal: Integrate training in behavioral sciences, community health and practice management within context of most common visits seen in ambulatory family medicine v Structure v 6 -week seminar each year of residency v 3 different seminars (A, B, C), each offered 2 x/year, each with 3 modules v Each module includes PBL, pharmacy, practice management and community components v
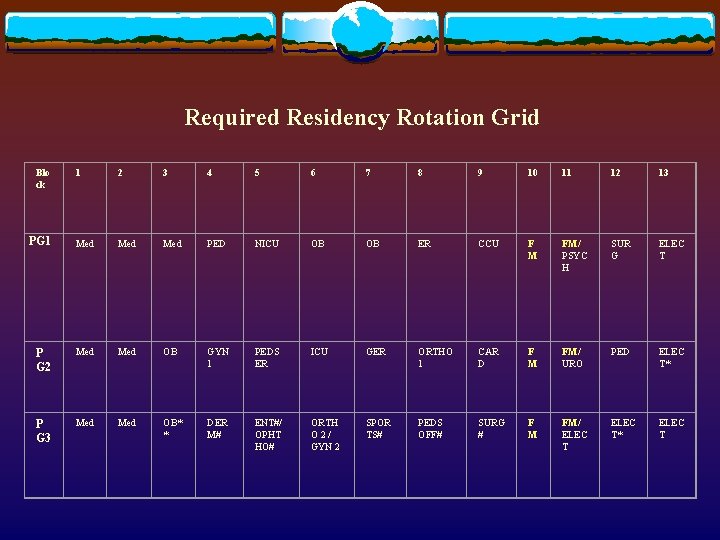

Required Residency Rotation Grid Blo ck 1 2 3 4 5 6 7 8 9 10 11 12 13 PG 1 Med Med PED NICU OB OB ER CCU F M FM/ PSYC H SUR G ELEC T P G 2 Med OB GYN 1 PEDS ER ICU GER ORTHO 1 CAR D F M FM/ URO PED ELEC T* P G 3 Med OB* * DER M# ENT#/ OPHT HO# ORTH O 2 / GYN 2 SPOR TS# PEDS OFF# SURG # F M FM/ ELEC T* ELEC T

Seminar Subject Overview Seminar Modules A Diabetes Prenatal Care Prevention in Adults B Cardiovascular Disease Substance Abuse Prevention in Seniors C Respiratory Disorders Injuries Prevention in Children
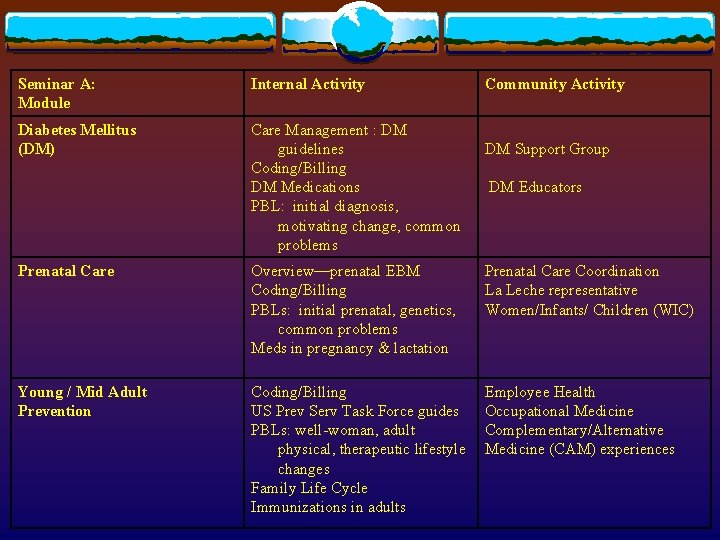

Seminar A: Module Internal Activity Community Activity Diabetes Mellitus (DM) Care Management : DM guidelines Coding/Billing DM Medications PBL: initial diagnosis, motivating change, common problems DM Support Group DM Educators Prenatal Care Overview—prenatal EBM Coding/Billing PBLs: initial prenatal, genetics, common problems Meds in pregnancy & lactation Prenatal Care Coordination La Leche representative Women/Infants/ Children (WIC) Young / Mid Adult Prevention Coding/Billing US Prev Serv Task Force guides PBLs: well-woman, adult physical, therapeutic lifestyle changes Family Life Cycle Immunizations in adults Employee Health Occupational Medicine Complementary/Alternative Medicine (CAM) experiences
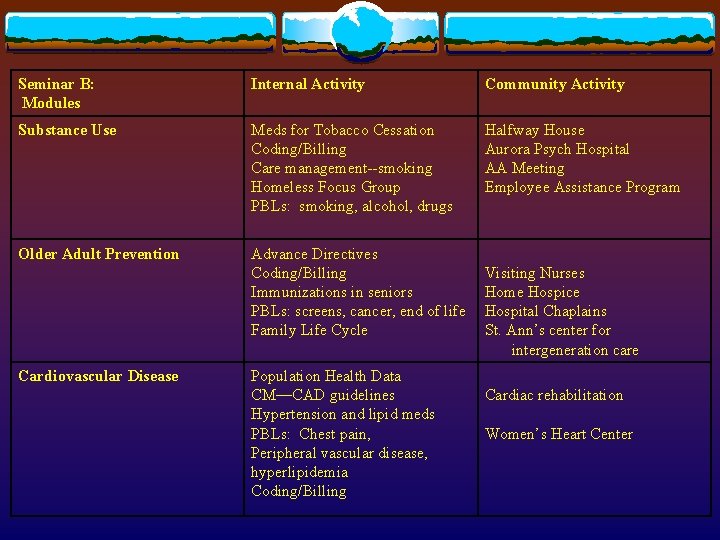
Seminar B: Modules Internal Activity Community Activity Substance Use Meds for Tobacco Cessation Coding/Billing Care management--smoking Homeless Focus Group PBLs: smoking, alcohol, drugs Halfway House Aurora Psych Hospital AA Meeting Employee Assistance Program Older Adult Prevention Advance Directives Coding/Billing Immunizations in seniors PBLs: screens, cancer, end of life Family Life Cycle Visiting Nurses Home Hospice Hospital Chaplains St. Ann’s center for intergeneration care Cardiovascular Disease Population Health Data CM—CAD guidelines Hypertension and lipid meds PBLs: Chest pain, Peripheral vascular disease, hyperlipidemia Coding/Billing Cardiac rehabilitation Women’s Heart Center

Seminar C: Modules Internal Activity Community Activity Respiratory Disease CM: Asthma guidelines & data Asthma Meds & Control Plan PBLs: Pediatric lung disease, URI, COPD Coding/Billing URI Medications Asthma School Tuberculosis (TB) clinic Pulmonary Rehabilitation Injuries Domestic Violence Home Visit PBLs: Back Pain, Strains & Sprains, overuse injuries Occupational Medicine Pain meds Coding/Billing Sexual Assault Center Women’s Shelter Child Prot Services Work-Hardening Program Occup Medicine Childhood Prevention Reach Out and Read Health Educ Center Coding/Billing Birth to 3 PBLs: Nutrition, Developmental Head Start Assessment, child Lead Program neglect/abuse School clinics Vaccines in children Day Care Family Life Cycle
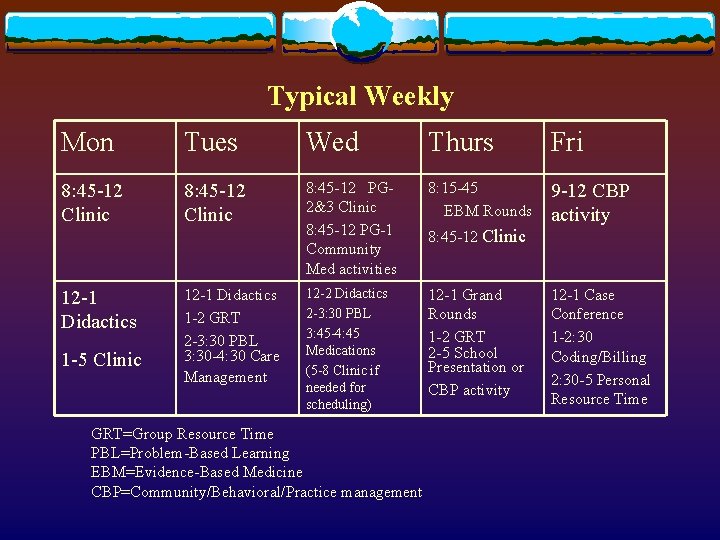

Typical Weekly Mon Tues Wed Thurs Fri 8: 45 -12 Clinic 8: 45 -12 PG- 2&3 Clinic 8: 45 -12 PG-1 Community Med activities 8: 15 -45 EBM Rounds 9 -12 CBP activity 12 -2 Didactics 2 -3: 30 PBL 3: 45 -4: 45 Medications (5 -8 Clinic if needed for scheduling) 12 -1 Grand Rounds 1 -2 GRT 2 -5 School Presentation or CBP activity 12 -1 Didactics 1 -5 Clinic 12 -1 Didactics 1 -2 GRT 2 -3: 30 PBL 3: 30 -4: 30 Care Management GRT=Group Resource Time PBL=Problem-Based Learning EBM=Evidence-Based Medicine CBP=Community/Behavioral/Practice management 8: 45 -12 Clinic 12 -1 Case Conference 1 -2: 30 Coding/Billing 2: 30 -5 Personal Resource Time

Program Resources v v v v Family physician faculty Behavioral scientist faculty PBL facilitators Pharm D Faculty Administrative assistant Care management instructor Billing and Coding instructor 0. 1 FTE 0. 2 FTE 20 times 2 hrs/ year 30 hrs/ year 0. 1 FTE 18 hrs/ year 30 hrs/ year


“PBL” v Problem-based learning (PBL) is a pedagogical strategy of "active learning" pioneered at Mc. Master University, Hamilton, Ontario, Canada. v The defining characteristics of PBL are: v Learning is driven by challenging, open-ended problems. v Learners work in small collaborative groups. v Teachers take on the role as "facilitators" of learning. Accordingly, learners are encouraged to take responsibility for their group and organize and direct the learning process with support from a tutor or instructor. v
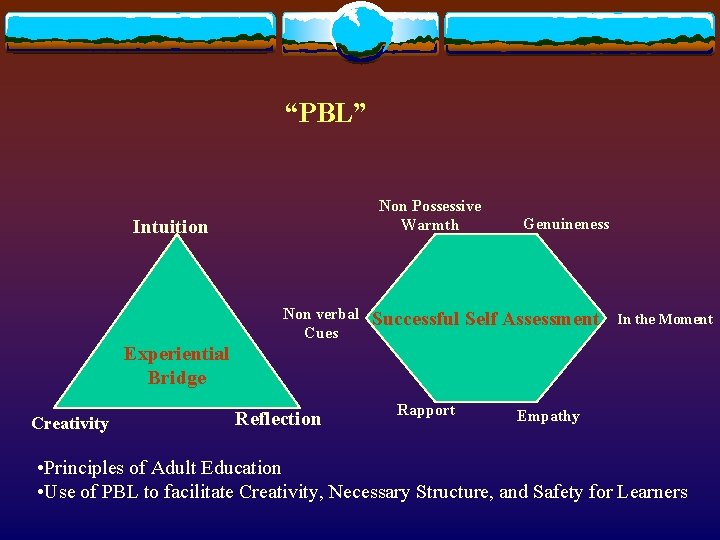
“PBL” Non Possessive Warmth Intuition Non verbal Cues Genuineness Successful Self Assessment In the Moment Experiential Bridge Creativity Reflection Rapport Empathy • Principles of Adult Education • Use of PBL to facilitate Creativity, Necessary Structure, and Safety for Learners

"To study medicine without books is to sail an uncharted sea, while to study medicine only from books is not to go to sea at all. " Sir William Osler More on Vast and Endless Sea
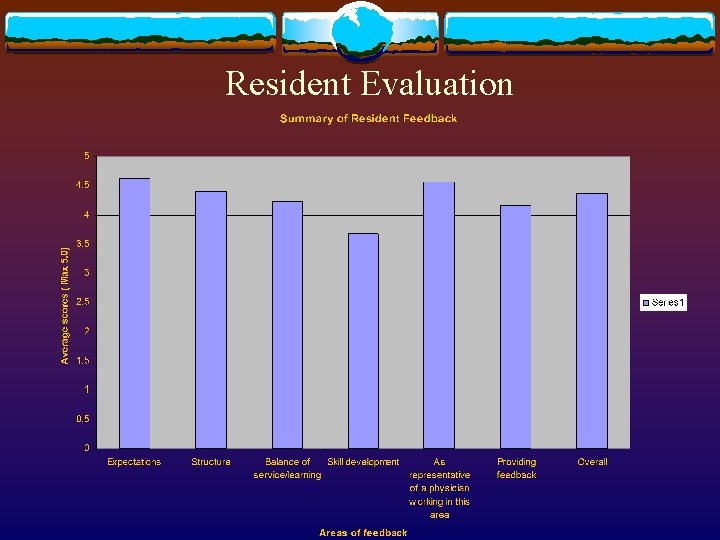
Resident Evaluation

Qualitative Comments: Best aspects of this rotation v Identification of various resources available in the community v Focus on common problems encountered in family practice clinic during PBL. v Evidence Based Medicine sessions v Coding and billing sessions.

v Time management in the clinic setting. v Improved interpersonal skills as a result of group discussions during PBL. v Multidisciplinary approach to teaching ( Faculty, pharmacist, social worker, coders). v Resource time

v Developing empathy for the patients ( role play scenarios) v Public outreach education ( Presentation at middle school) v Small group learning v Community outreach clinic

Areas to Improve v Improved scheduling. v Include more procedure oriented activity v More feedback would be helpful v Schedule more time in the lab to get acquainted with common lab tests.

Personal opinion v Becoming a “ Family Physician” v Increased confidence in diagnosing and management of commonly encountered problems. v Developing skills to work as a team and opportunity to develop leadership qualities. v Areas to improve.

“ Sometimes I sits and thinks, other times, I just sits” M. Evan Wolkenstein

References ü ü ü ü ü 1. Thompson R, Haber D, Fanuiel L, Krohn K, Chambers C. Community-oriented primary care in a family practice residency program. Family Medicine. 28(5): 326 -30, 1996 May. 2. Rubenstein HL, Franklin ED, Zarro VJ. Opportunities and challenges in educating community-responsive physicians. American Journal of Preventive Medicine. 13(2): 104 -8, 1997 Mar-Apr. 3. Cashman SB, Fulmer HS, Anderson RJ. Opportunities and challenges in educating community-responsive physicians. Comment on: Am J Prev Med. 1997 Mar-Apr; 13(2): 104 -8; American Journal of Preventive Medicine. 13(6): 407, 1997 Nov-Dec. Am J Prev Med. 13(6): 407, 1997 Nov-Dec. 4. Nuovo J, Balsbaugh T, Barton S, Davidson E, Fox-Garcia J, Gandolfo A, Levich B, Seibles J. Development of a diabetes care management curriculum in a family practice residency program. Disease Management. 7(4): 314 -24, 2004. 5. King RV, Murphy-Cullen CL, Krepcho M, Bell HS, Frey RD. Tying it all together? A competency-based linkage model for family medicine. Family Medicine. 35(9): 632 -6, 2003 Oct. 6. Parnanen H, Kumpusalo E, Takala J. Primary health care ICD--a tool for general practice research. International Journal of Health Planning & Management. 15(2): 133 -48, 2000 Apr-Jun. 7. Kirkwood CR, Clure HR, Brodsky R, Gould GH, Knaak R, Metcalf M, Romeo S. The diagnostic content of family practice: 50 most common diagnoses recorded in the WAMI community practices. Journal of Family Practice. 15(3): 485 -92, 1982 Sep. 8. Phillips WR, Haynes DG. The Domain of Family Practice: Scope, Role, and Function. Fam Med 2001; 33(4): 273 -7. 9. Cardarelli R, Sanders M. Ambulatory teaching and evidence-based medicine: applying classroom knowledge to clinical practice. Family Medicine. 37(2): 87 -9, 2005 Feb.

Contact us v John Brill, MD, MPH john. brill. md@aurora. org v Alan Wolkenstein, MSW alan. wolkenstein@aurora. org v Hamilton Jeyaraj, MD, PG 3 hamilton. jeyaraj@aurora. org Aurora St. Luke’s Family Medicine Residency 2801 W. KK Parkway #175 Milwaukee WI 53215 414. 649. 7909
- Slides: 25