Faculty Staff Orientation Benefits Compensation Unclassified employees are

Faculty & Staff Orientation Benefits

Compensation �Unclassified employees are paid once a month, on the last working day of each month �Faculty are paid in ten (10) equal installments; those who are eligible can elect twelve (12) equal installments �http: //payroll. louisiana. edu/sites/payroll/files/Pay% 20 Option%20 Request. pdf �Direct deposit is mandatory *temporary employees are not eligible for the 12 month pay option

Sick Leave �Faculty and Staff earn one (1) day of sick leave for every month worked* �Staff (12 month employees) earn one (1) day of annual leave (vacation time) each month* �All paid leave is subject to Supervisor’s approval �Leave accumulates throughout State employment *earn rate increases after 3 years of service

Tuition Exemption �Full-time employees are able to attend six (6) hours of graduate or undergraduate classes per semester at a reduced rate. �Spouse and dependents of eligible employees are able to attend full-time at a reduced fee for undergraduate classes only. **This exemption extends to all UL System schools.

Retirement �No Social Security (FICA) contributions �Enrollment in Teachers’ Retirement System of Louisiana (TRSL) OR Optional Retirement Plan (ORP) required �Required contribution of 8%

Teachers’ Retirement System of Louisiana (TRSL) �Defined Benefit Plan �Pension based on final average compensation and number of years in system when eligible for retirement �www. trsl. org �Employees who separate from employment before retirement, are eligible for a refund of their contributions only.

Retirement Plans Teachers’ Retirement System of Louisiana (TRSL) Optional Retirement Plans (ORP) � Defined benefit plan �Defined contribution � Pension based on final average compensation and number of years in system when eligible for retirement � Employees who separate from state employment before retirement are eligible for a refund of their contributions only plan �Retirement account based on employee and employer contributions �Rights to defined benefit plan are irrevocably waved if enrolled in ORP �Employees are vested immediately
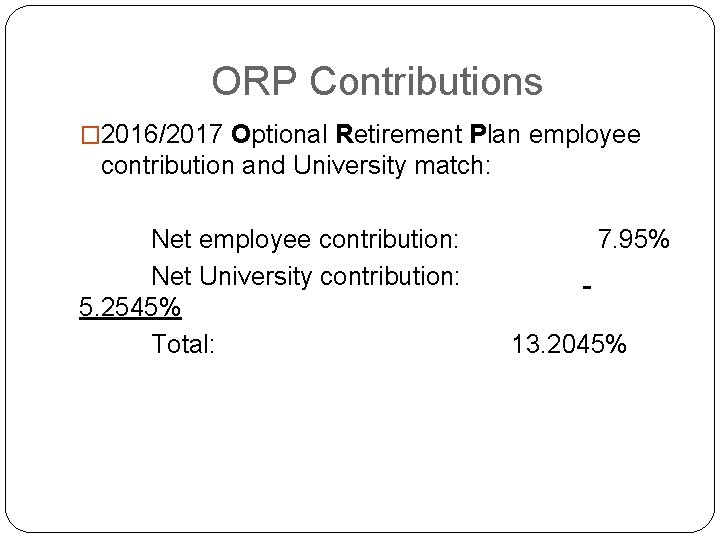
ORP Contributions � 2016/2017 Optional Retirement Plan employee contribution and University match: Net employee contribution: Net University contribution: 5. 2545% Total: 7. 95% 13. 2045%

Voya (formerly ING) �www. Voyaretirementplans. com/custom/laorp �Local Representative: Simone S. Bauer �ssbauer@voyafa. com �(337) 322 -5304

TIAA-Cref �http: //www 1. tiaa-cref. org/tcm/louisianaorp/ �Local Representative: Cameron Pettigrew �cpettigrew@tiaa-cref. org �(866) 842 -2951 ext. 257413

Valic �www. valic. com �Local Representative: Nicholas J. Grove �nicholas. grove@valic. com �(337) 344 -4712 �Local Representative: Daniel Poynot �Daniell. poynot@valic. com �(985)705 -2662

Timeline for Enrollment �Employees are automatically enrolled in TRSL �Those who enroll in ORP within 60 days of hire will receive employer contributions to ORP from date of hire �Employees can join ORP within 5 years of hire �If ORP is elected after 60 days, TRSL contributions will be moved to ORP; employer contributions will begin on next full paycheck �ORP election is irrevocable; membership in TRSL is no longer an option

Tax Deferred Annuity Plans � 403(b) and 457 plans available for additional retirement savings � 403(b) and 457 Plan Details � 403(b) and 457 Provider Contacts

Health Insurance

Health Insurance � State pays 75% of employee’s premium, and 50% of spouse and/or family members premium -Married couples who work for state agencies must split coverage to realize premium savings � Office of Group Benefits offers five (5) Plan options: Magnolia and Pelican plans are administered by Blue Cross/Blue Shield of LA, Vantage Medical Home HMO is administered by Vantage � Marriage license required for spouse coverage � Birth certificates required for coverage of dependent children age 26 and under � Social security numbers and dates of birth are required for all covered dependents � All plans offer Preventive Care (Wellness) benefits at no charge, subject to plan allowances � Referrals not required for Specialist visits

Important Facts Ø Enrollment is within 30 days of your hire date Ø Effective date of coverage Ø If you fail to enroll within the 30 days you cannot enroll until the annual enrollment period in October for an effective date of January

Your Responsibilities ØEnroll in a health plan ØApply for a life plan ØDetermine the amount of your Health Savings Account contribution if eligible ØEnroll in Flexible Spending Arrangement

Eligibility

ELIGIBILITY The following people can be enrolled as dependents: Ø Your legal spouse Ø Your children until they reach age 26 (coverage ends the last day of their birthday month) Ø No one can be simultaneously enrolled as both an employee and a dependent in the health or life insurance Ø No dependent can be covered by more than one employee or retiree Dependent verification is required

ELIGIBILITY Children are defined as: Ø Natural child of employee or legal spouse Ø Legally adopted child Ø Child by court-ordered legal guardianship

ELIGIBILITY Children are defined as: Ø Natural child of employee or legal spouse Ø Legally adopted child Ø Child by court-ordered legal guardianship

ELIGIBILITY Over-age Dependents: A covered child under age 26 who is, or becomes, incapable of sustaining employment is eligible to continue coverage as an overage dependent. Ø OGB must receive required medical records before dependent reaches age 26 Ø Definition of incapacity includes both mental and physical incapacity
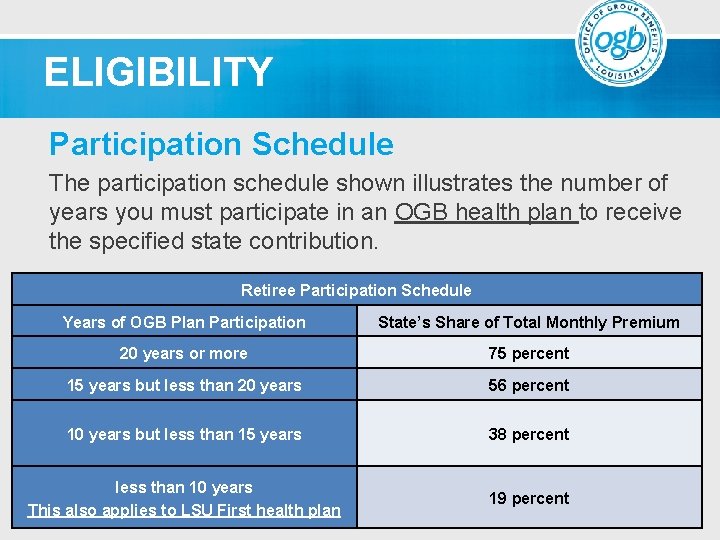
ELIGIBILITY Participation Schedule The participation schedule shown illustrates the number of years you must participate in an OGB health plan to receive the specified state contribution. Retiree Participation Schedule Years of OGB Plan Participation State’s Share of Total Monthly Premium 20 years or more 75 percent 15 years but less than 20 years 56 percent 10 years but less than 15 years 38 percent less than 10 years This also applies to LSU First health plan 19 percent

Plan Options

Pelican Plans OGB’s Pelican benefit options offer low premiums, in combination with employer contributions, to create the most affordable options for enrollees. Pelican plans offer coverage within the Blue Cross and Blue Shield nationwide network, as well as outof-network coverage.

Pelican HRA 1000 The Pelican HRA 1000 includes $1, 000 in annual employer contributions for employee-only plans and $2, 000 for family plans in a health reimbursement arrangement that can be used to offset deductibles and other out-of-pocket medical, nonpharmacy, costs throughout the year. The HRA funds are available as long as you remain enrolled in the Pelican HRA 1000 plan. Any unused funds will accrue to the in-network, out-of-pocket maximum (see following chart), allowing members to build up balances that cover eligible medical expenses.
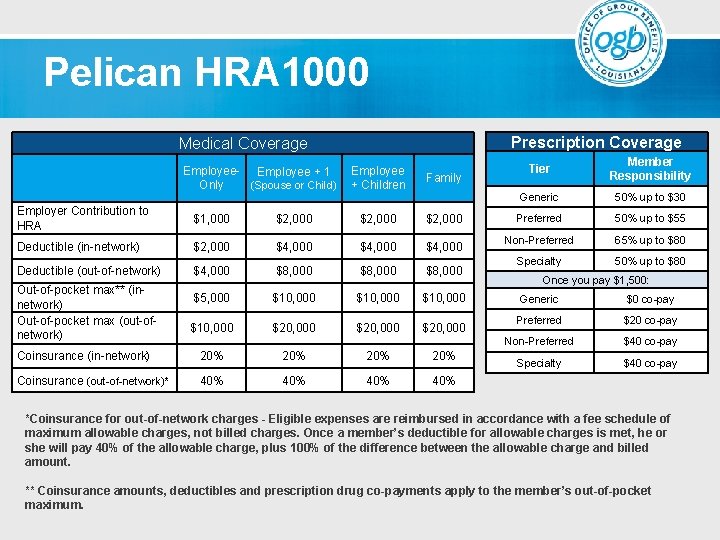
Pelican HRA 1000 Prescription Coverage Medical Coverage Employee- Employee + 1 (Spouse or Child) Only Employee + Children Family Employer Contribution to HRA $1, 000 $2, 000 Deductible (in-network) $2, 000 $4, 000 Deductible (out-of-network) $4, 000 $8, 000 $5, 000 $10, 000 $20, 000 Out-of-pocket max** (innetwork) Out-of-pocket max (out-ofnetwork) Coinsurance (in-network) 20% 20% Coinsurance (out-of-network)* 40% 40% Tier Member Responsibility Generic 50% up to $30 Preferred 50% up to $55 Non-Preferred 65% up to $80 Specialty 50% up to $80 Once you pay $1, 500: Generic $0 co-pay Preferred $20 co-pay Non-Preferred $40 co-pay Specialty $40 co-pay *Coinsurance for out-of-network charges - Eligible expenses are reimbursed in accordance with a fee schedule of maximum allowable charges, not billed charges. Once a member’s deductible for allowable charges is met, he or she will pay 40% of the allowable charge, plus 100% of the difference between the allowable charge and billed amount. ** Coinsurance amounts, deductibles and prescription drug co-payments apply to the member’s out-of-pocket maximum.

Pelican HSA 775 The Pelican HSA 775 offers our lowest premium in addition to a health savings account funded by both employers and employees. Employers contribute $200, then match any employee contributions up to $575. Employees can contribute additional funds on a pre-tax basis, up to $3, 400 for an individual and $6, 750 for a family, to cover out-of-pocket medical and pharmacy costs. Unused funds accrue every year with no limit. Unlike the HRA option, the money in an HSA is owned by the member even if he or she changes jobs or retires. This plan is available to Active Employees only.
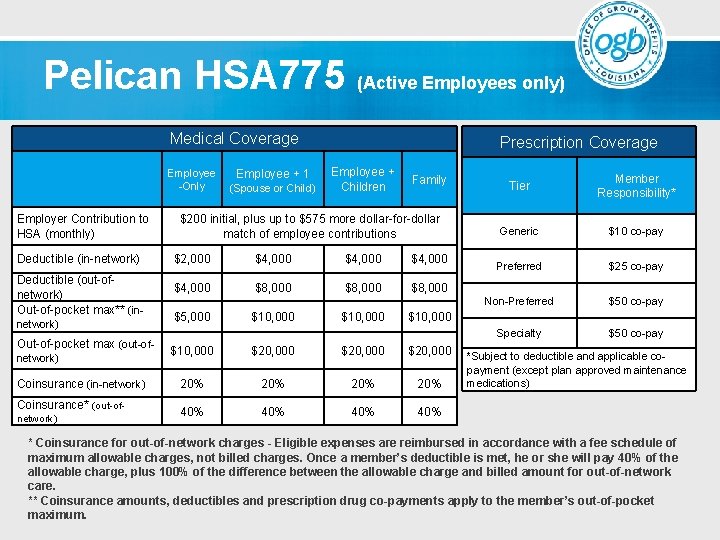
Pelican HSA 775 (Active Employees only) Medical Coverage Employee + 1 -Only (Spouse or Child) Employer Contribution to HSA (monthly) Deductible (in-network) Deductible (out-ofnetwork) Out-of-pocket max** (innetwork) Out-of-pocket max (out-ofnetwork) Coinsurance (in-network) Coinsurance* (out-ofnetwork) Prescription Coverage Employee + Children Family $200 initial, plus up to $575 more dollar-for-dollar match of employee contributions $2, 000 $4, 000 $8, 000 $5, 000 $10, 000 Tier Member Responsibility* Generic $10 co-pay Preferred $25 co-pay Non-Preferred $50 co-pay Specialty $50 co-pay $10, 000 $20, 000 20% 20% 40% 40% *Subject to deductible and applicable copayment (except plan approved maintenance medications) * Coinsurance for out-of-network charges - Eligible expenses are reimbursed in accordance with a fee schedule of maximum allowable charges, not billed charges. Once a member’s deductible is met, he or she will pay 40% of the allowable charge, plus 100% of the difference between the allowable charge and billed amount for out-of-network care. ** Coinsurance amounts, deductibles and prescription drug co-payments apply to the member’s out-of-pocket maximum.

Magnolia Local Plus (Nationwide In-Network Provider Plan) The Magnolia Local Plus option offers the benefit of nationwide in-network providers. The Local Plus plan provides the predictability of co-payments rather than using employer funding to offset out-of-pocket costs. This plan provides care in the Blue Cross and Blue Shield nationwide network. Out-of-network coverage is provided only in emergencies and may be subject to balance billing.
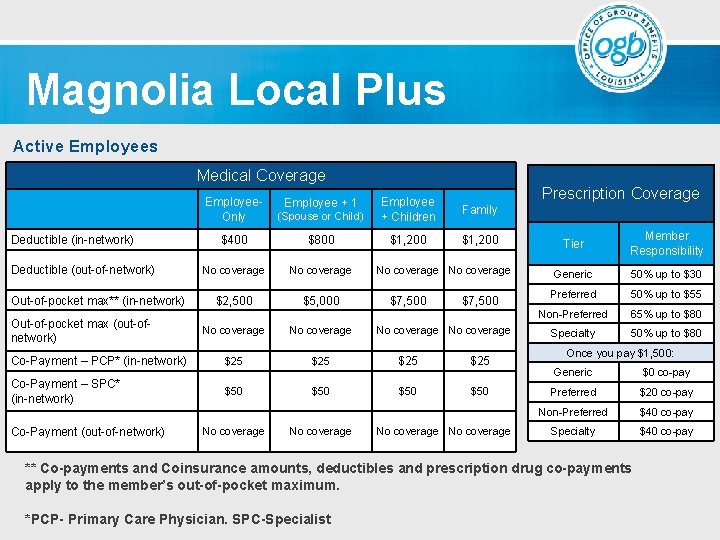
Magnolia Local Plus Active Employees Medical Coverage Deductible (in-network) Deductible (out-of-network) Out-of-pocket max** (in-network) Out-of-pocket max (out-ofnetwork) Employee. Only Prescription Coverage (Spouse or Child) Employee + Children Family $400 $800 $1, 200 No coverage $2, 500 $5, 000 Employee + 1 No coverage $7, 500 No coverage Co-Payment – PCP* (in-network) $25 $25 Co-Payment – SPC* (in-network) $50 $50 Co-Payment (out-of-network) No coverage No coverage Tier Member Responsibility Generic 50% up to $30 Preferred 50% up to $55 Non-Preferred 65% up to $80 Specialty 50% up to $80 Once you pay $1, 500: Generic $0 co-pay Preferred $20 co-pay Non-Preferred $40 co-pay Specialty $40 co-pay ** Co-payments and Coinsurance amounts, deductibles and prescription drug co-payments apply to the member’s out-of-pocket maximum. *PCP- Primary Care Physician. SPC-Specialist

Magnolia Open Access (Nationwide Providers) The Magnolia Open Access Plan offers coverage both inside and outside of Blue Cross’s nationwide network. It differs from the other Magnolia plans in that members enrolled in the Open Access plan will not pay co-payments at physician visits. Instead, once a member’s deductible for allowable charges is met, he or she will pay 10% of the allowable amount for in-network care and 30% of the allowable amount for out-of-network care. Out-of-network care may be balance billed. Though the premiums for the Open Access plan are higher than OGB’s other plans, its moderate deductibles combined with a nationwide network make it an attractive plan for members who live out of state or desire the flexibility to use an out-of-network provider.

Magnolia Open Access Active Employees Medical Coverage Employee. Only Deductible (in-network) Deductible (out-of-network) Out-of-pocket max** (innetwork) Out-of-pocket max (out-ofnetwork) Coinsurance (in-network) Coinsurance* (out-ofnetwork) Emergency Room Co-pay Prescription Coverage (Spouse or Child) Employee + Children Family $900 $1, 800 $2, 700 $2, 500 $5, 000 $7, 500 $3, 700 $7, 500 $11, 250 Employee + 1 10% 10% 30% 30% $150; Waived if admitted Tier Member Responsibility Generic 50% up to $30 Preferred 50% up to $55 Non-Preferred 65% up to $80 Specialty 50% up to $80 Once you pay $1, 500: Generic $0 co-pay Preferred $20 co-pay Non-Preferred $40 co-pay Specialty $40 co-pay *Coinsurance for out-of-network charges - Eligible expenses are reimbursed in accordance with a fee schedule of maximum allowable charges, not billed charges. Once a member’s deductible is met, he or she will pay 40% of the allowable charge, plus 100% of the difference between the allowable charge and billed amount for out-of-network care. **Coinsurance amounts, deductibles and prescription drug co-payments apply to the member’s out-of-pocket maximum.

Magnolia Local (Limited In-Network Provider Only Plan) The Magnolia Local plan is a limited provider innetwork only plan for members who live in specific coverage areas. Magnolia Local is a health plan for members who want local access, affordable premiums and a new approach to health care. Out-of-network coverage is provided only in emergencies and may be subject to balance billing.

Magnolia Local has two networks: Community Blue is a select, local network designed for members who live in the parishes of East Baton Rouge, West Baton Rouge, Ascension, Bossier & Caddo. You have access to the following hospitals in the Baton Rouge and Shreveport regions: Baton Rouge Shreveport • Baton Rouge General Hospital Blue Connect Blue. Connect is a select, local network designed for members who live in the parishes of Acadia, Evangeline, Iberia, Jefferson, Lafayette, Orleans, St. Landry, St. Martin, St. Mary, St. Tammany & Vermilion. You have access to the following hospitals in the Greater New Orleans, Lafayette and St. Tammany regions: Greater New Orleans St. Tammany • Ochsner Medical Center Northshore • Ochsner Health System • St. Tammany Parish Hospital Lafayette • Lafayette General Health System • Opelousas General • Abbeville General Hospital • Iberia Medical Center
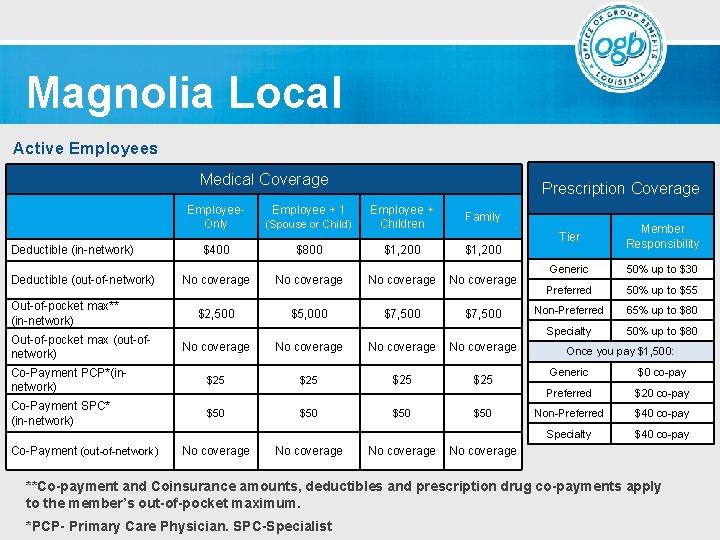
Magnolia Local Active Employees Medical Coverage Deductible (in-network) Deductible (out-of-network) Out-of-pocket max** (in-network) Out-of-pocket max (out-ofnetwork) Prescription Coverage Employee. Only (Spouse or Child) Employee + Children Family $400 $800 $1, 200 No coverage $2, 500 $5, 000 $7, 500 Employee + 1 No coverage Co-Payment PCP*(innetwork) $25 $25 Co-Payment SPC* (in-network) $50 $50 Co-Payment (out-of-network) No coverage $50 No coverage Tier Member Responsibility Generic 50% up to $30 Preferred 50% up to $55 Non-Preferred 65% up to $80 Specialty 50% up to $80 Once you pay $1, 500: Generic $0 co-pay Preferred $20 co-pay Non-Preferred $40 co-pay Specialty $40 co-pay No coverage **Co-payment and Coinsurance amounts, deductibles and prescription drug co-payments apply to the member’s out-of-pocket maximum. *PCP- Primary Care Physician. SPC-Specialist
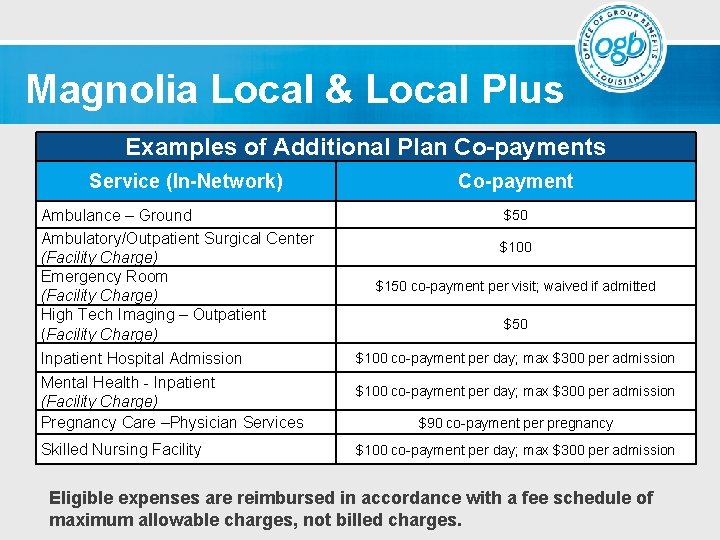
Magnolia Local & Local Plus Examples of Additional Plan Co-payments Service (In-Network) Ambulance – Ground Ambulatory/Outpatient Surgical Center (Facility Charge) Emergency Room (Facility Charge) High Tech Imaging – Outpatient (Facility Charge) Inpatient Hospital Admission Mental Health - Inpatient (Facility Charge) Pregnancy Care –Physician Services Skilled Nursing Facility Co-payment $50 $100 $150 co-payment per visit; waived if admitted $50 $100 co-payment per day; max $300 per admission $90 co-payment per pregnancy $100 co-payment per day; max $300 per admission Eligible expenses are reimbursed in accordance with a fee schedule of maximum allowable charges, not billed charges.
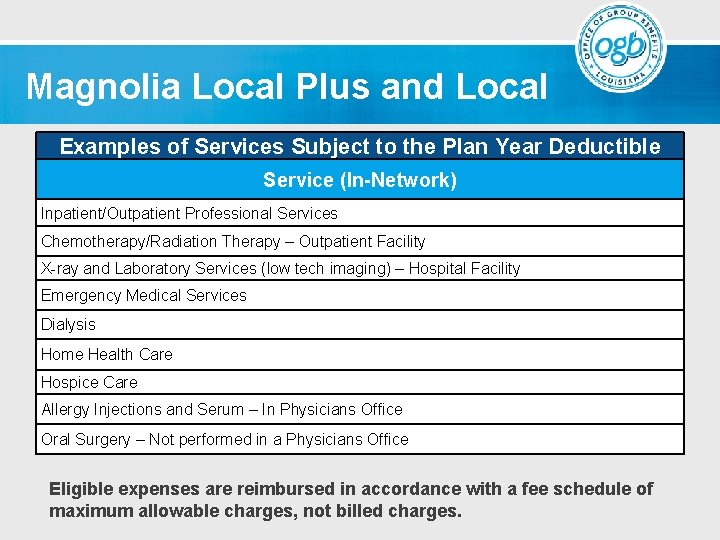
Magnolia Local Plus and Local Examples of Services Subject to the Plan Year Deductible Service (In-Network) Inpatient/Outpatient Professional Services Chemotherapy/Radiation Therapy – Outpatient Facility X-ray and Laboratory Services (low tech imaging) – Hospital Facility Emergency Medical Services Dialysis Home Health Care Hospice Care Allergy Injections and Serum – In Physicians Office Oral Surgery – Not performed in a Physicians Office Eligible expenses are reimbursed in accordance with a fee schedule of maximum allowable charges, not billed charges.

Vantage Medical Home HMO is a patient-centered approach to providing cost-effective and comprehensive primary health care for children, youth and adults. This plan creates partnerships between the individual patient and his or her personal physician. This plan includes a preferred provider network, Affinity Health Network (AHN), which has lower co-payments for certain covered services as indicated by “AHN. ” This plan also includes out-of-network coverage.
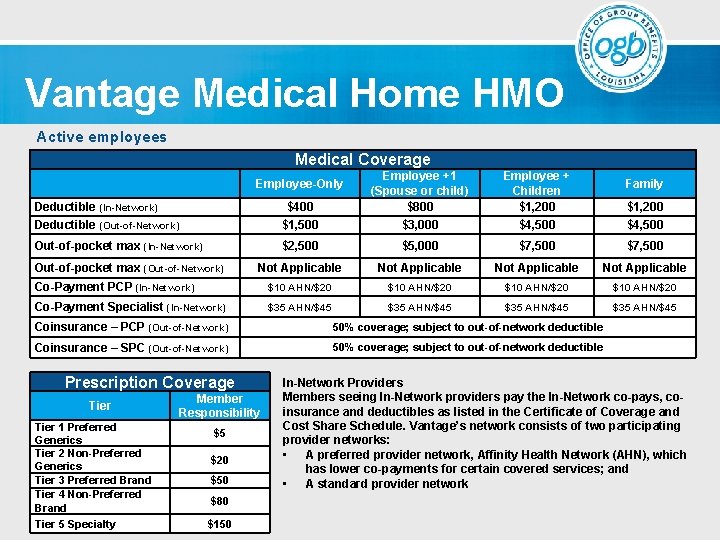
Vantage Medical Home HMO Active employees Medical Coverage Deductible (In-Network) Deductible (Out-of-Network) $400 $1, 500 Employee +1 (Spouse or child) $800 $3, 000 Out-of-pocket max (In-Network) $2, 500 $5, 000 $7, 500 Not Applicable Co-Payment PCP (In-Network) $10 AHN/$20 Co-Payment Specialist (In-Network) $35 AHN/$45 Employee-Only Out-of-pocket max (Out-of-Network) Employee + Children $1, 200 $4, 500 Family $1, 200 $4, 500 Coinsurance – PCP (Out-of-Network) 50% coverage; subject to out-of-network deductible Coinsurance – SPC (Out-of-Network) 50% coverage; subject to out-of-network deductible Prescription Coverage Tier 1 Preferred Generics Tier 2 Non-Preferred Generics Tier 3 Preferred Brand Tier 4 Non-Preferred Brand Tier 5 Specialty Member Responsibility $5 $20 $50 In-Network Providers Members seeing In-Network providers pay the In-Network co-pays, coinsurance and deductibles as listed in the Certificate of Coverage and Cost Share Schedule. Vantage’s network consists of two participating provider networks: • A preferred provider network, Affinity Health Network (AHN), which has lower co-payments for certain covered services; and • A standard provider network $80 $150

OGB encourages you to make sure you choose a doctor or hospital in your provider network when you need healthcare. By choosing network providers, you avoid the possibility of having your provider bill you for amounts in addition to applicable co-payments, coinsurance, deductibles and non-covered services. (Often referred to as balance billing. )

OGB encourages you to make sure you choose a doctor or hospital in your provider network when you need healthcare. By choosing network providers, you avoid the possibility of having your provider bill you for amounts in addition to applicable co-payments, coinsurance, deductibles and non-covered services. (Often referred to as balance billing. )

Other Benefit Offerings

Flexible Benefits What are Flexible Benefits? • Flexible Benefits are tax-saving benefits • They enable employees to save both state and federal income taxes on eligible payroll deductions for health care and dependent care
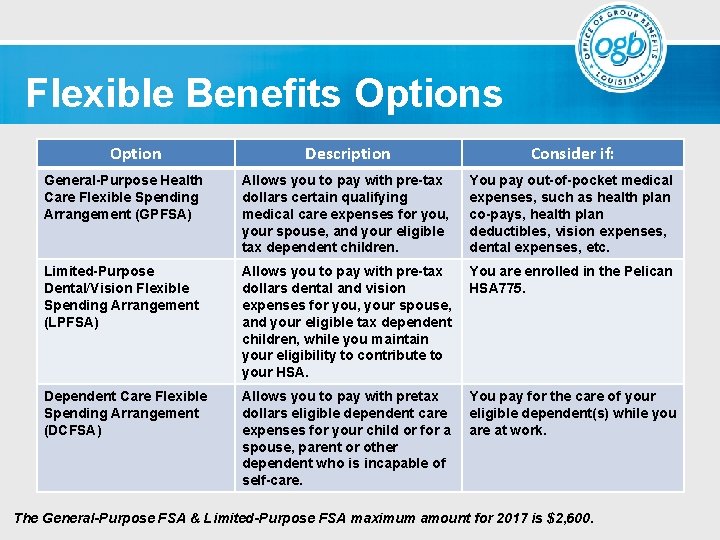

Flexible Benefits Options Option Description Consider if: General-Purpose Health Care Flexible Spending Arrangement (GPFSA) Allows you to pay with pre-tax dollars certain qualifying medical care expenses for you, your spouse, and your eligible tax dependent children. You pay out-of-pocket medical expenses, such as health plan co-pays, health plan deductibles, vision expenses, dental expenses, etc. Limited-Purpose Dental/Vision Flexible Spending Arrangement (LPFSA) Allows you to pay with pre-tax dollars dental and vision expenses for you, your spouse, and your eligible tax dependent children, while you maintain your eligibility to contribute to your HSA. You are enrolled in the Pelican HSA 775. Dependent Care Flexible Spending Arrangement (DCFSA) Allows you to pay with pretax dollars eligible dependent care expenses for your child or for a spouse, parent or other dependent who is incapable of self-care. You pay for the care of your eligible dependent(s) while you are at work. The General-Purpose FSA & Limited-Purpose FSA maximum amount for 2017 is $2, 600.

Dependent Care FSA • PLAN YEAR MAXIMUM AMOUNTS EMPLOYEE TAX STATUS SINGLE OR MARRIED FILING SEPARATELY SINGLE HEAD OF HOUSEHOLD MARRIED FILING JOINTLY MAXIMUM AMOUNT ALLOWED DEPENDENT $2, 500 Child under age 13; Older dependent incapable of self care $5, 000 Child under age 13; Older dependent incapable of self-care; Spouse incapable of self care

Discovery Benefits – Can be used to pay providers who VISA Benefits Debit Card accept VISA for eligible expenses for GPFSA, LPFSA and DCFSA – Full amount of General-Purpose FSA and Limited-Purpose FSA funds are available immediately – Dependent Care FSA funds are available upon deposit – Card is reloadable each year as long as the employee reenrolls Discovery Benefits – Card is replaced before expiration Contact Information: date o Phone: 1 -866 -451 -3399 o Email: customerservice@discoverybenefits. com o Website: www. Discovery. Benefits. com o Fax: 1 -866 -451 -3245
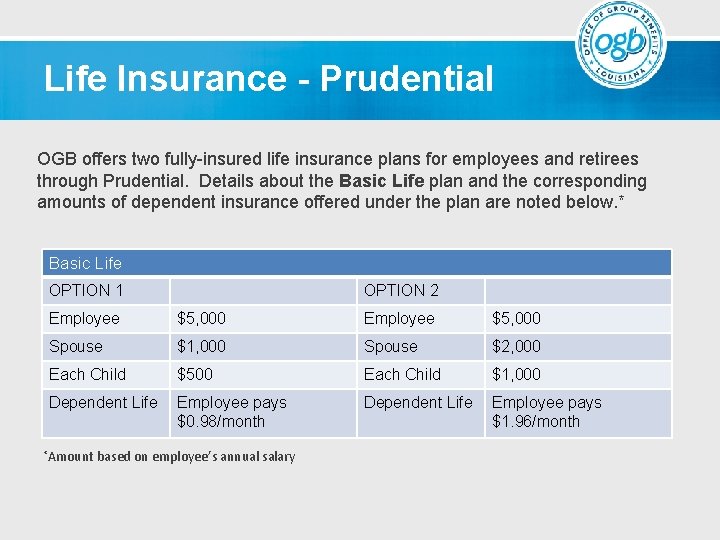
Life Insurance - Prudential OGB offers two fully-insured life insurance plans for employees and retirees through Prudential. Details about the Basic Life plan and the corresponding amounts of dependent insurance offered under the plan are noted below. * Basic Life OPTION 1 OPTION 2 Employee $5, 000 Spouse $1, 000 Spouse $2, 000 Each Child $500 Each Child $1, 000 Dependent Life Employee pays $0. 98/month Dependent Life Employee pays $1. 96/month *Amount based on employee’s annual salary
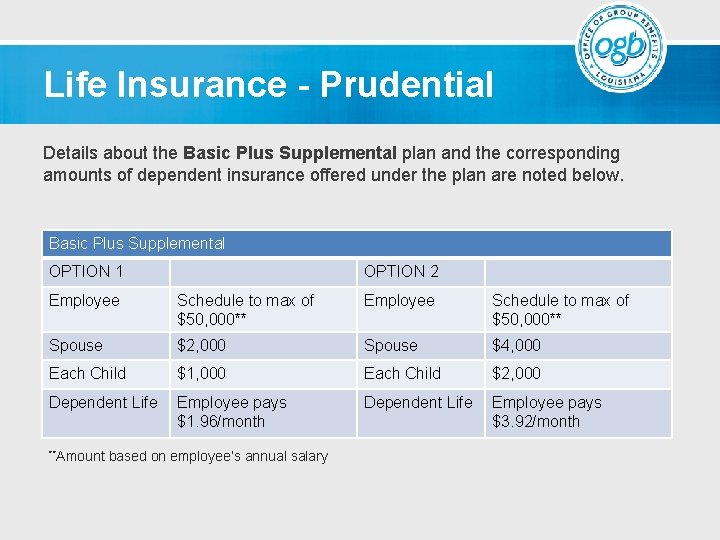
Life Insurance - Prudential Details about the Basic Plus Supplemental plan and the corresponding amounts of dependent insurance offered under the plan are noted below. Basic Plus Supplemental OPTION 1 OPTION 2 Employee Schedule to max of $50, 000** Spouse $2, 000 Spouse $4, 000 Each Child $1, 000 Each Child $2, 000 Dependent Life Employee pays $1. 96/month Dependent Life Employee pays $3. 92/month **Amount based on employee’s annual salary

Wellness 2017 Program Sept. 10, 2016 – Aug. 31, 2017

Live Better Louisiana What’s the Game Plan? Online Personal Health Assessment Preventive Onsite Health Checkup At least $120 savings on 2017 health insurance premium with Blue Cross.

Contact Information

Dental Insurance �Underwritten by Metlife �Monthly premium for Employee only = $37. 09 �Monthly premium for Employee plus Family = $100. 28 �Pays 100% for preventive services �Pays 50% for Orthodontia �Annual maximum benefits of $1, 500. 00 �Orthodontia maximum lifetime maximum $1, 000. 00 �Children's eligibility for dental coverage is from birth up to age 26 �www. metlife. com/mybenefits or www. metlife. com/dental

Dental Insurance (cont’d) �Deductible is $50 person �Percentages of payment are based on reasonable and customary amounts

Vision Insurance �Monthly premium for Employee only = $9. 13 �Monthly premium for Employee plus Family = $21. 42 �Co-payments for in-network services �Allowances for out-of-network services �Eye exam $10 copay �Frame allowance $130 �www. Metlife. com/vision

Long Term Disability Insurance �Underwritten by Met. Life �Provides up to 60% of annual salary till age 65 �Maximum benefit of $6, 000 per month �Premium is based on salary

Supplemental Cancer Insurance �Coverage through AFLAC �Provides cash payments based on diagnosis and treatment of cancer �Contact Representative Blake Adams at (337) 298 -7459 for premium and benefit information

Submission Deadlines �Completed insurance forms should be submitted by August 2, 2017 �Coverage begins September 1, 2017** �Human Resources Office, Martin Hall, Room 170 **Only attendees of the New Hire Orientation will be eligible for coverage to begin September 1 st – coverage for those who do not attend cannot begin before October 1 st.

Contact Information � Retirement questions � 403 (b)/Deferred Compensation questions � Retirement questions Shekethia Williams 482 -6248 Shekethia. Williams@Louisiana. edu Insurance/Cafeteria Plan questions Malika Oubre 482 -1014 malika@louisiana. edu � Office of Group Benefits 1 -800 -272 -8451 � Blue Cross/Blue Shield Customer Service 1 -800 -3924089 � Med. Impact (Prescriptions) 1 -800 -910 -1831 � Express Scripts (Prescriptions) 1 -866 -781 -7533
- Slides: 59