FACTORS AFFECTING WOUND HEALING SYSTEMIC FACTORS LOCAL FACTORS





























- Slides: 45

FACTORS AFFECTING WOUND HEALING • SYSTEMIC FACTORS • LOCAL FACTORS

FOCTORS AFFECTING WOUND HEALING Systemic factors 1. Age 2. Drugs 3. Vitamins 4. Trace Elements 5. Nutrition 6. Illness / Immunity

FOCTORS AFFECTING WOUND HEALING Local Factors 1. 2. 3. 4. 5. 6. 7. Infection Foreign Bodies Mechanical Stress/ Pressure Wound Hydration Temperature Ionizing Radiation Oxygen Tension

SYSTEMIC FACTORS 1 - AGE • intrinsic physiologic changes ? wound healing. • increased incidence of diseases? incidence of wound healing problems. 4

SYSTEMIC FACTORS 2. DRUGS Antimetabolite drugs : ? inhibiting early Cell proliferation & wound DNA & Protein synthesis. STEROIDS: ? Inhibit the inflammatory phase of wound healing. 5

SYSTEMIC FACTORS 2. DRUGS cont… Anti-neoplastic agents ? • Decreased leukocyte and fibroblast proliferation. • Decreased wound contraction and protein synthesis. • Decreased collagen secretion and increased activity of collagenases. NSAIDs ? • Decrease collagen synthesis by 45% even at normal levels.

SYSTEMIC FACTORS 3. NUTRITION • Precise calorie requirements for optimal healing? • Protein depletion - prolongs inflammatory phase, impairs fibroplasia. • • Methionine required forming disulfide bonds in collagen synthesis. Arginine deficiency results in decreased wound-breaking strength and wound collagen accumulation. Carbohydrates - energy source for leukocytes. Fats ? no significant effects, but Fats are essential elements of all cell membranes. • • • 7

SYSTEMICFACTORS 4 -Vitamins VITAMIN C • Ascorbic acid enhances Neutrophil function , increases Angiogenesis • Vitamin C deficiency failure in collagen synthesis & cross- linking.

SYSTEMIC FACTORS VITAMIN - A • Vitamin - A is required for Epithelial & Bone tissue development , cellular differentiation & immune system function. • • 9

SYSTEMIC FACTORS VITAMIN -E • Systemic vitamin -E inhibits the inflammatory response & collagen synthesis , thereby possibly impeding the healing process.

SYSTEMIC FACTORS Zinc • Collagen synthesis , DNA synthesis , cell division & protein synthesis • Deficiency decreased fibroblast proliferation, decreased collagen synthesis , impaired overall wound strength & delayed epithelialization. Copper • required for Collagen crosslinking. 11

SYSTEMIC FACTORS 6. Associated Illnesses / Immunity • Cancer , infection , peripheral vascular diseases, smoking – all negatively affect wound healing. • Immuno- dysfunction leads to decreased chemotaxis , phagocytosis , intracellular killing & collagen synthesis

Diabetes mellitus • Susceptable to infection attenuated Inflammatory response impaired chemotaxis inefficient bacterial killing • Impaired lymphocyte & leukocyte function • Increased collagen degradation & decreased deposition

LOCAL FACTORS 1 - INFECTION Probably the most common cause of delayed healing. • • Staphylococcus species, Streptococcus Enterococci Escherichia coli. 14

LOCAL FACTORS 1. INFECTION…… • Bacteria (phospholipase) prolong the inflammatory phase & interfere c epithelialization , contraction & collagen deposition.

LOCAL FACTORS 2 - Foreign Bodies Clot , necrotic debris , dirt , suture , glass etc • Prolong inflammatory phase. • Lead to infection. • Increased duration of Re-epithelialization.

LOCAL FACTORS 3. Mechanical Stress / Pressure • Undue pressure may lead to ischaemia of the wound , chronic wounds , should be off-loaded.

LOCAL FACTORS 4. Wound Hydration • Moist wound increases rate of Re-epithelialization.

LOCAL FACTORS 5. Temperature • Environment temperature greater than 30 o. C increases tensile strength.

LOCAL FACTORS 6. IONIZING RADIATION • Causes endothelial cell injury fibrosis and delayed tissue repair. • Inhibit Angiogenesis. • keratinocytes & fibroblasts are most sensitive to radiation. 20

LOCAL FACTORS 7. OXYGEN TENSION • Low oxygen tension effect on all aspects of wound healing. • Collagen synthesis requires oxygen as a cofactor 21

Summary of factors affecting different steps

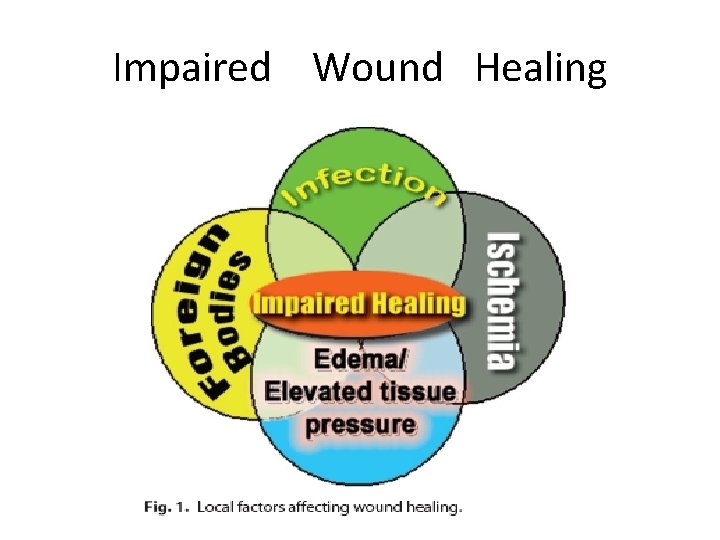
Impaired Wound Healing

Complications Of Wound Healing Categories 1. Deficient scar formation (wound dehiscence ulceration), 2. Excessive scar formation (keloid, hypertrophic scar) 3. Contractures , and 4. Exuberant granulations.

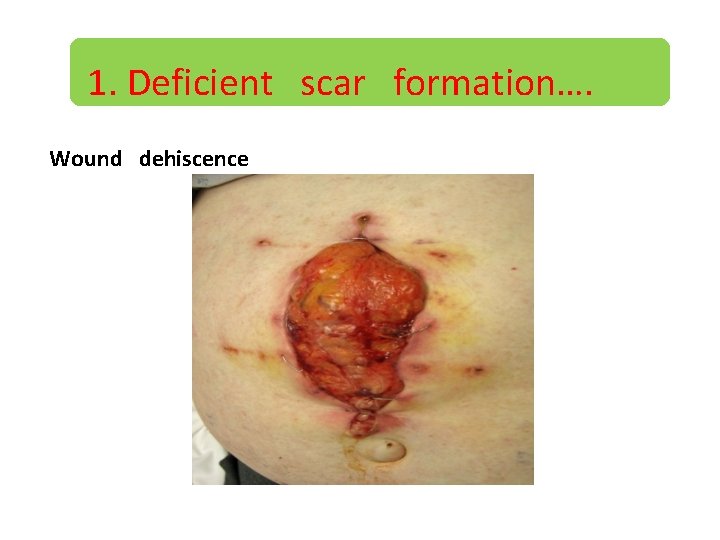
1. Deficient scar formation • Two types 1. Wound dehiscence 2. Ulceration 1. Wound dehiscence : Surgical complication in which a wound breaks open along surgical suture. • Risk factors: age, diabetes, obesity, poor knotting , trauma to the wound after surgery.

1. Deficient scar formation…. Wound dehiscence

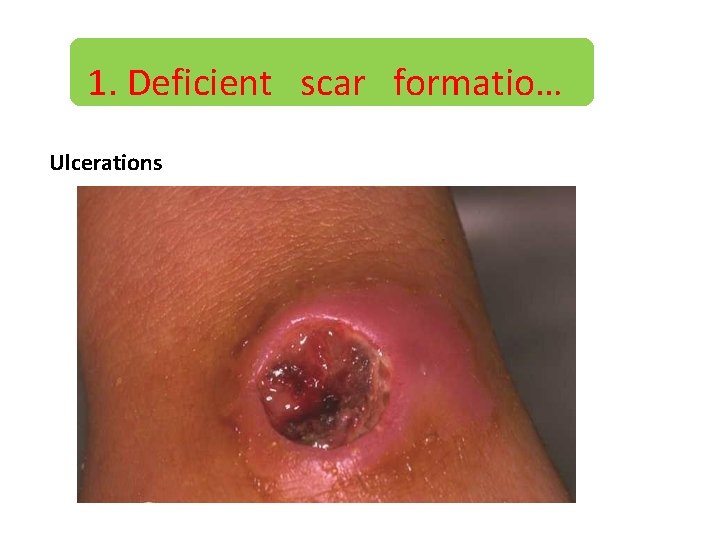
1. Deficient scar formation…. 2. Ulceration An ulcer is a breach in the epithelium of the skin or mucous membrane

1. Deficient scar formatio… Ulcerations

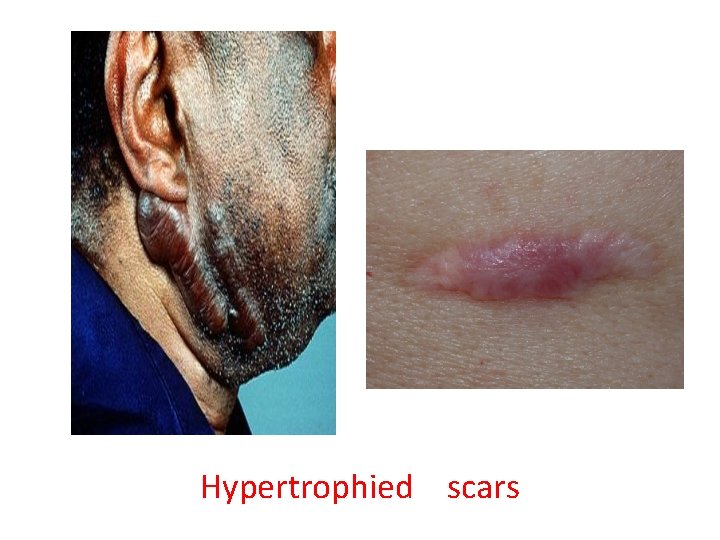
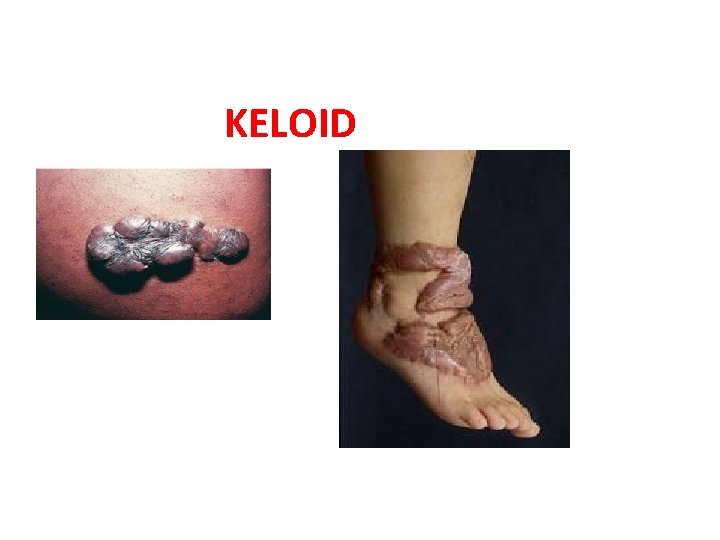
2. Excessive Formation Of The Repair Components • collagen over - expression called SCARING • Two types • HYPERTROPHIC SCARS • Keloid 1. HYPERTROPHIC SCARS : overproduction of collagen , which causes the scar to be raised above the surrounding skin . ( red , raised , itchy & tender) 2. Keloid : Excessive stiff collagen bundled growth over-extending the tissue. (surgery , accident, acne)

Hypertrophied scars

KELOID

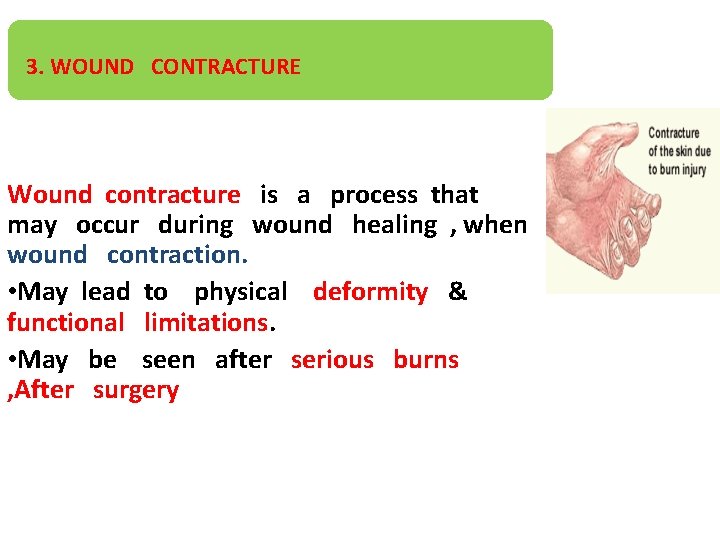
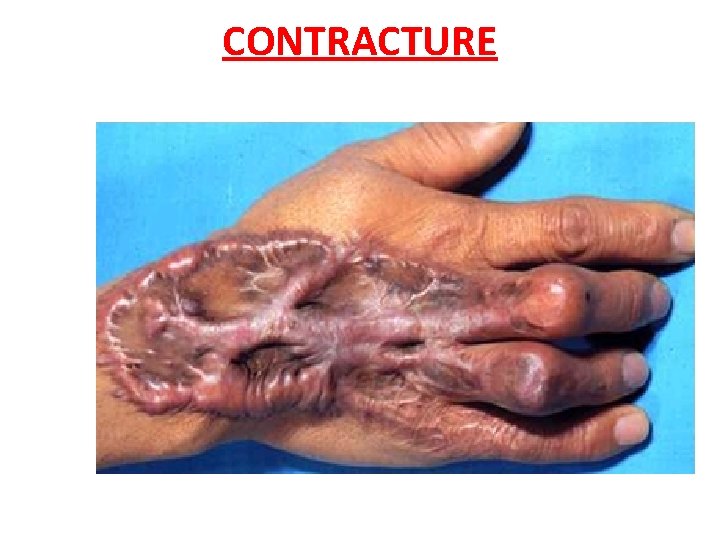
3. WOUND CONTRACTURE Wound contracture is a process that may occur during wound healing , when wound contraction. • May lead to physical deformity & functional limitations. • May be seen after serious burns , After surgery

CONTRACTURE

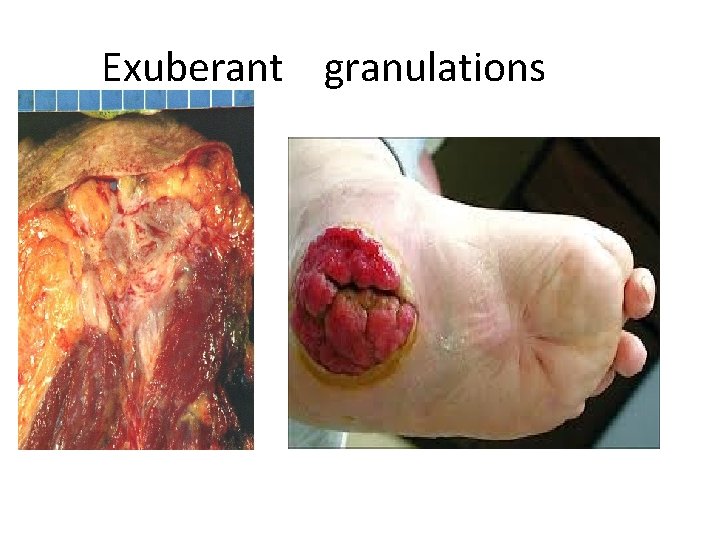
4. EXUBERANT GRANULATIONS • Exuberant granulations is excessive proliferation of granulation tissue in healing wounds.

Exuberant granulations

HEALING OF FRACTURE

TYPES OF FRACTURES • • • Traumatic / Pathological Complete / Incomplete Simple [Closed ] / Communted [Splinte Ring of Bone ] / Compound [Communicating to skin surface ]

HEALING OF BONES • Primary Union • Secondary Union

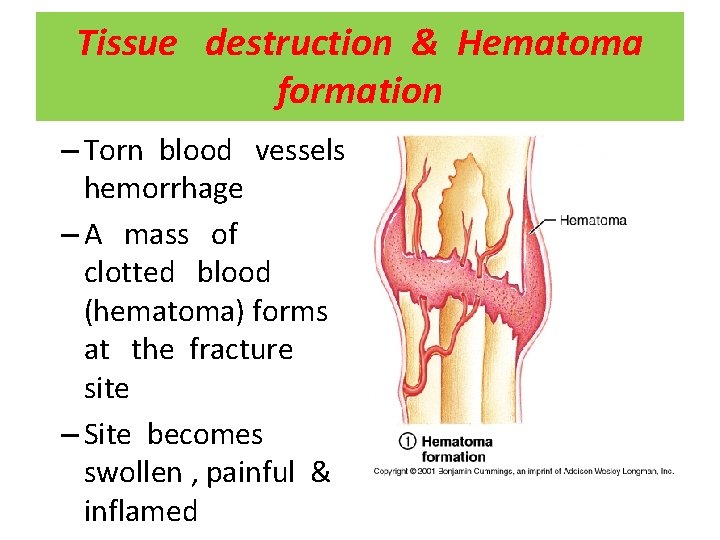
Tissue destruction & Hematoma formation – Torn blood vessels hemorrhage – A mass of clotted blood (hematoma) forms at the fracture site – Site becomes swollen , painful & inflamed

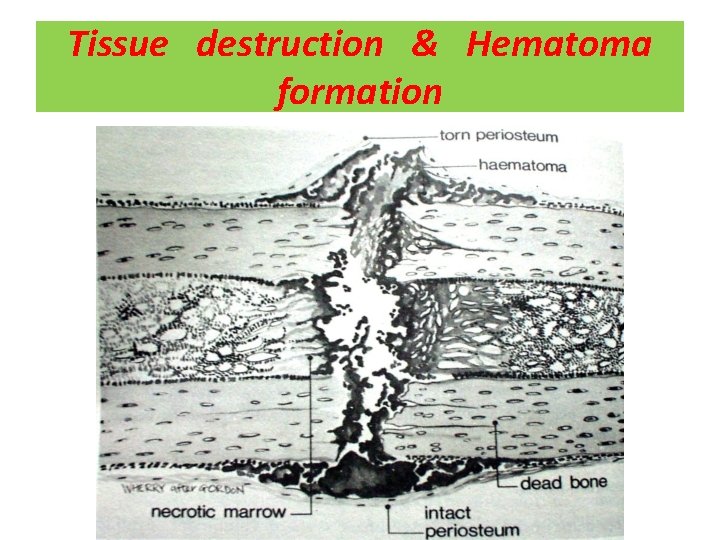
Tissue destruction & Hematoma formation

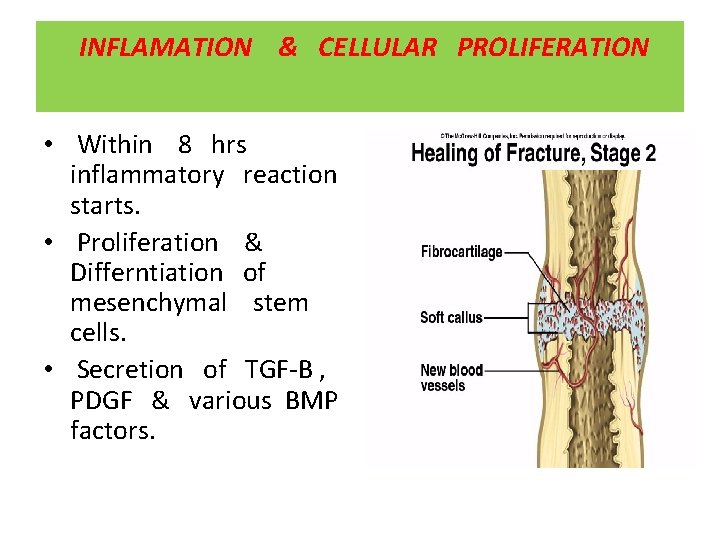
INFLAMATION & CELLULAR PROLIFERATION • Within 8 hrs inflammatory reaction starts. • Proliferation & Differntiation of mesenchymal stem cells. • Secretion of TGF-B , PDGF & various BMP factors.

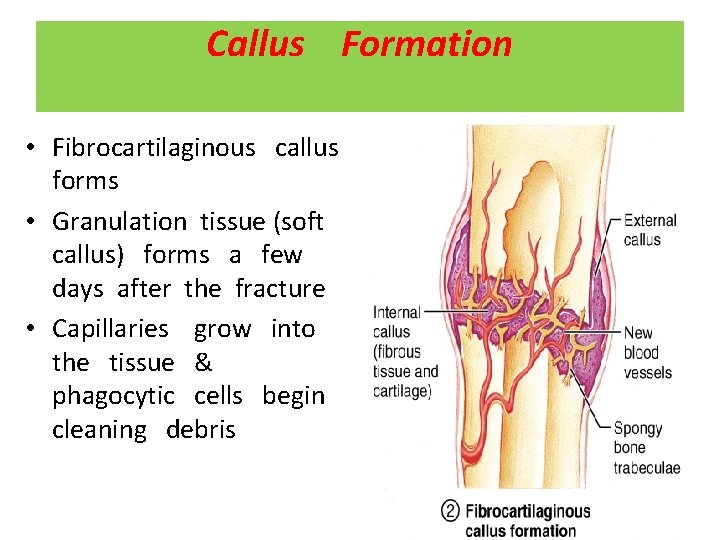
Callus Formation • Fibrocartilaginous callus forms • Granulation tissue (soft callus) forms a few days after the fracture • Capillaries grow into the tissue & phagocytic cells begin cleaning debris

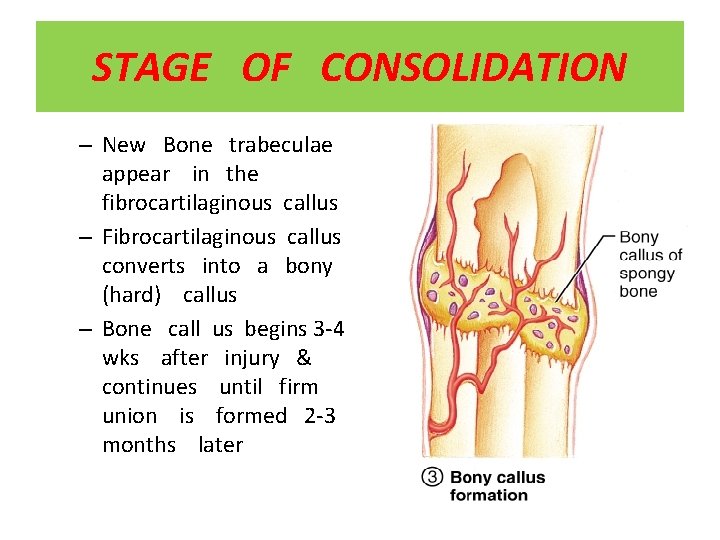
STAGE OF CONSOLIDATION – New Bone trabeculae appear in the fibrocartilaginous callus – Fibrocartilaginous callus converts into a bony (hard) callus – Bone call us begins 3 -4 wks after injury & continues until firm union is formed 2 -3 months later

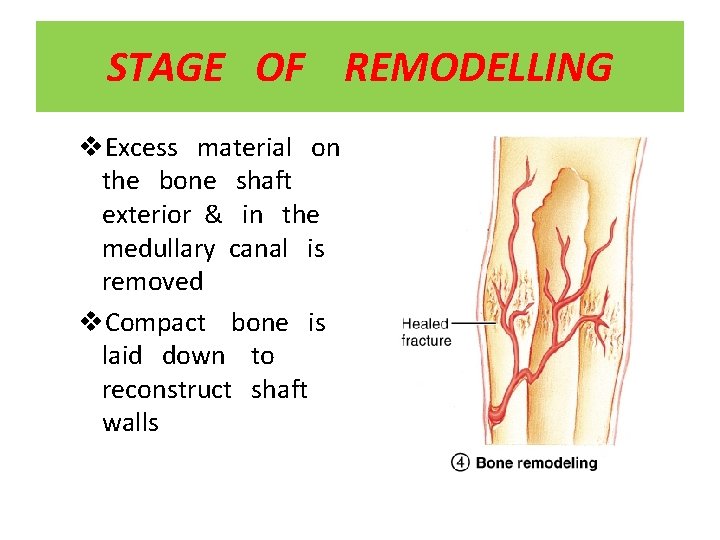
STAGE OF REMODELLING v. Excess material on the bone shaft exterior & in the medullary canal is removed v. Compact bone is laid down to reconstruct shaft walls

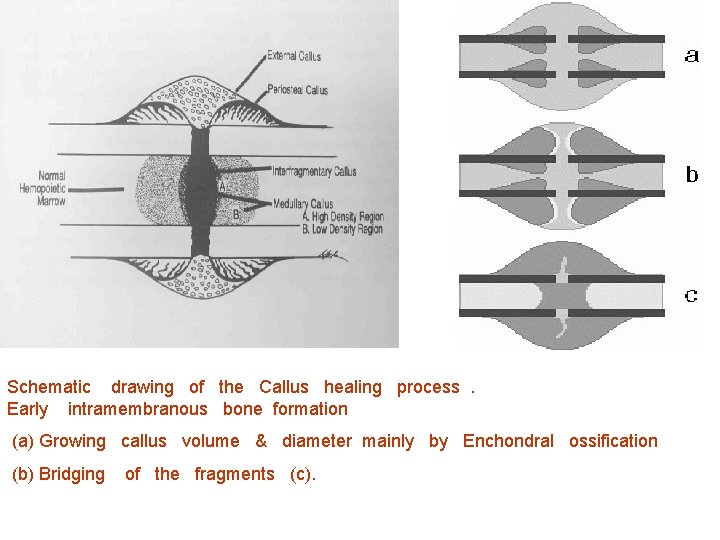
Schematic drawing of the Callus healing process. Early intramembranous bone formation (a) Growing callus volume & diameter mainly by Enchondral ossification (b) Bridging of the fragments (c).