Facilitybased HIV selftesting dramatically increases HIV testing in

Facility-based HIV self-testing dramatically increases HIV testing in Malawi: a cluster randomized trial Kathryn Dovel, Mike Nyirenda, Frackson Shaba, Ogechukwu Offorjebe, Kelvin Balakasi, Brooke Nichols, Khumbo Phiri, Khumbo Ngona, Alan Schooley, Risa Hoffman on behalf of EQUIP Innovations #AIDS 2018 | @AIDS_conference | www. aids 2018. org

Background HIV self-testing (HIVST) in sub-Saharan Africa is highly acceptable and increases testing when used in community-based models 1, 2 Remaining Questions: • Sustainability and Scalability • Quality assurance • Linkage to care What about Facility-Based HIVST? © UNAIDS STAR project, 2016 Study Objective: To assess facility-based HIVST among outpatients in Malawi using a cluster randomized trial 1 Choko AT, et al. PLo. S Med, 2015. 12(9): p. e 1001873. PP, et al. Curr Opin Infect Dis. 2018 Feb; 31(1): 14. 2 Indravudh
Study Design and Outcomes: • Non-blinded cluster randomized trial – Primary outcome: Proportion of outpatients tested for HIV – Secondary outcomes: HIV positivity rate, ART linkage, acceptability, and presence of adverse events Malawi: study districts Site Selection: • 15 high-burden facilities (outpatient departments) – 5 facilities per arm: block randomization by region and facility type Eligibility Criteria: • Adult (≥ 15 years) • Outpatient Data Collection: Sept 2017 -Feb 2018 • Exit surveys (subsample of outpatients) • Medical chart reviews 3 -months after enrollment

Study Arms Standard provider initiated testing and counseling (PITC) • Referrals for HIV tests (Determine) given during routine outpatient services • HIV testing usually completed in another building Optimized PITC • HIV testing (Determine) completed at the outpatient department before receiving routine outpatient services (morning testing) Facility-based HIVST • HIVST kits (Oraquick) in the waiting area before receiving routine outpatient services © WHO, 2016

Facility-Based HIVST Core Components • Universal opt-out testing in waiting area • Group HIVST demonstration/distribution • HIVST given to outpatients who: • tested ≥ 30 days ago; • never tested HIV-positive; • were comfortable with HIVST • Private rooms for interpretation • Post-counseling/linkage available • Locked boxes for confidential disposal of HIVST kits
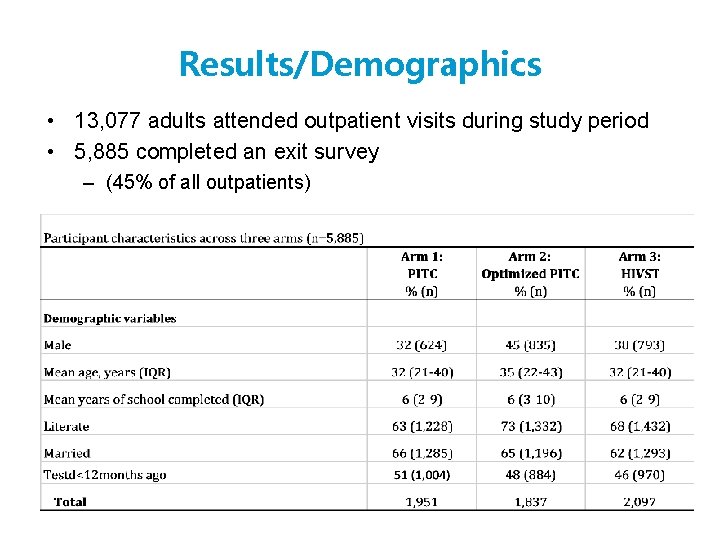
Results/Demographics • 13, 077 adults attended outpatient visits during study period • 5, 885 completed an exit survey – (45% of all outpatients)
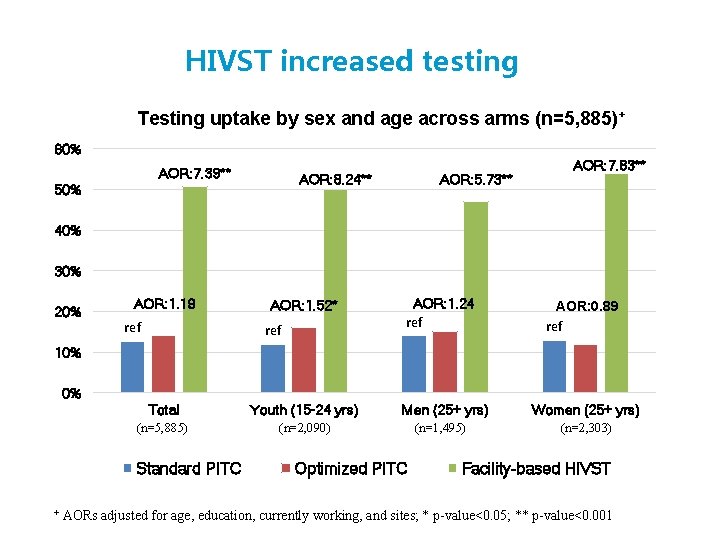
HIVST increased testing Testing uptake by sex and age across arms (n=5, 885)+ 60% AOR: 7. 39** AOR: 8. 24** 50% AOR: 5. 73** AOR: 7. 83** 40% 30% 20% AOR: 1. 19 ref AOR: 1. 52* ref AOR: 1. 24 ref AOR: 0. 89 ref 10% 0% Total Youth (15 -24 yrs) (n=5, 885) (n=2, 090) Standard PITC + Men (25+ yrs) Optimized PITC (n=1, 495) Women (25+ yrs) (n=2, 303) Facility-based HIVST AORs adjusted for age, education, currently working, and sites; * p-value<0. 05; ** p-value<0. 001
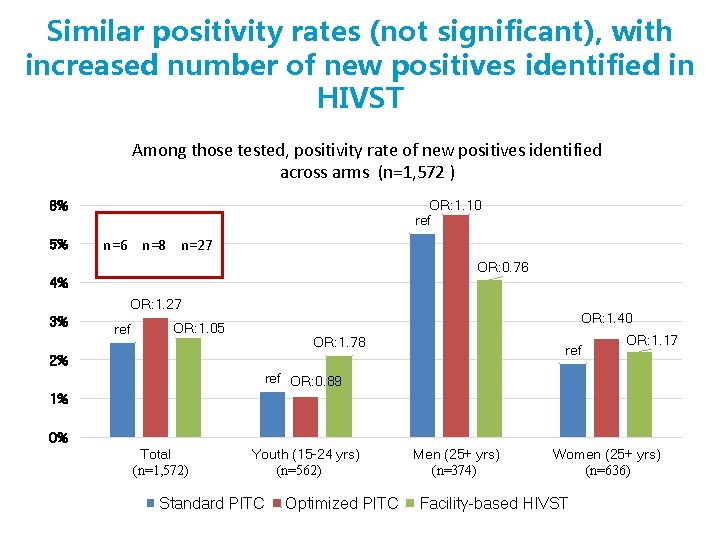
Similar positivity rates (not significant), with increased number of new positives identified in HIVST Among those tested, positivity rate of new positives identified across arms (n=1, 572 ) OR: 1. 10 ref 6% 5% n=6 n=8 n=27 OR: 0. 76 4% OR: 1. 27 3% ref OR: 1. 40 OR: 1. 05 OR: 1. 78 ref 2% OR: 1. 17 ref OR: 0. 89 1% 0% Total (n=1, 572) Youth (15 -24 yrs) (n=562) Standard PITC Optimized PITC Men (25+ yrs) (n=374) Women (25+ yrs) (n=636) Facility-based HIVST
HIVST had lower linkage rates, with increased number of ART initiates Too few positives to make concrete conclusions ART initiation within 3 months of testing HIV-positive: • Standard PITC: 5/6 (83%) • Optimized PITC: 8/8 (100%) • Facility-based HIVST: 19/27 (70%)
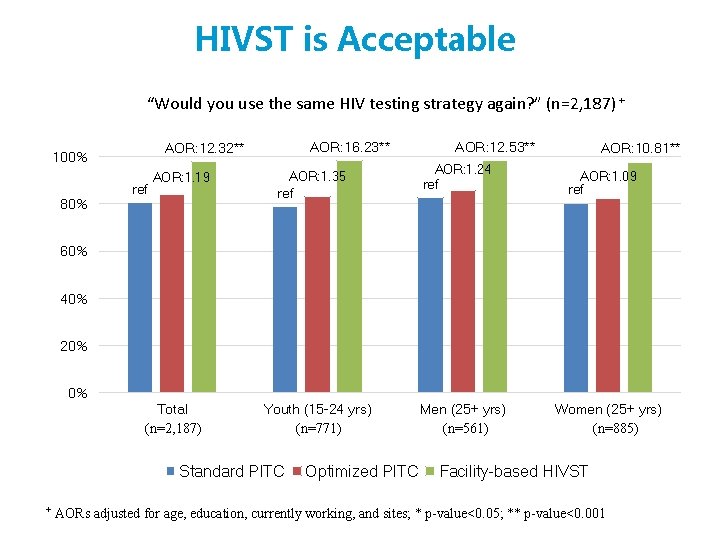
HIVST is Acceptable “Would you use the same HIV testing strategy again? ” (n=2, 187) + 80% AOR: 16. 23** AOR: 12. 32** 100% ref AOR: 1. 35 AOR: 1. 19 ref AOR: 12. 53** AOR: 1. 24 ref AOR: 10. 81** AOR: 1. 09 ref 60% 40% 20% 0% Total (n=2, 187) Youth (15 -24 yrs) (n=771) Standard PITC + Optimized PITC Men (25+ yrs) (n=561) Women (25+ yrs) (n=885) Facility-based HIVST AORs adjusted for age, education, currently working, and sites; * p-value<0. 05; ** p-value<0. 001
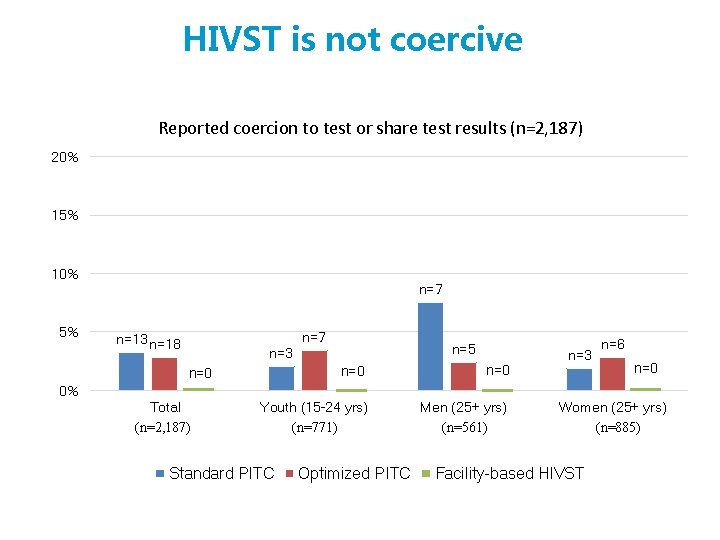
HIVST is not coercive Reported coercion to test or share test results (n=2, 187) 20% 15% 10% 5% n=7 n=13 n=18 n=5 n=3 n=0 Youth (15 -24 yrs) (n=771) Men (25+ yrs) (n=561) n=0 n=3 n=6 n=0 0% Total (n=2, 187) Standard PITC Optimized PITC Women (25+ yrs) (n=885) Facility-based HIVST

Conclusion Facility-based HIVST increased • Proportion of outpatients tested • Number of new positives identified, similar yield • Number of new ART initiates, lower linkage Facility-based HIVST is acceptable and not coercive Additional research on linkage is needed Additional information • Facility-based HIVST is cost-effectiveness: Brooke Nichols (THPEE 646) • Who opts-out of facility-based HIVST and why? : Frackson Shaba (WEPEE 682) • Acceptability of index partner HIVST: Ogechukwu Offorjebe (WEPEE 683)

Acknowledgments Funding • U. S. Agency for International Development (USAID) and the President’s Emergency Plan for AIDS Relief (PEPFAR) under Cooperative Agreement AID-OAA-A-15 -00070 • KD and RH receive support from the UCLA CFAR grant AI 028697 and the UCLA AIDS Institute. Acknowledgments • We are grateful to the health workers, mentors, research assistants, and clients who made the study possible • We are grateful to Sundeep Gupta, Eric Lungu, Misheck Mphanda, and Pericles Kalande for their contributions to the study #AIDS 2018 | @AIDS_conference | www. aids 2018. org
- Slides: 13