F Ahmadabadi Child Neurologist ARUMS 2014 INBORN ERRORS

F Ahmadabadi Child Neurologist ARUMS 2014 INBORN ERRORS OF METABOLISM

Every child with unexplained. . . Neurological deterioration Metabolic acidosis Hypoglycemia Inappropriate ketosis Hypotonia Cardiomyopathy Hepatocellular dysfunction Failure to thrive . . . should be suspected of having a metabolic disorder

When to suspect an IEM? Clinical: Vomiting Lethargy FTT Seizure Respiratory Coma Cardiomyopathy Odor Abnormal hair Dysmorphology Labs: Metabolic acidosis Hypoglycemia Hyperammonemia Reducing substances in urine Ketonuria Pancytopenia
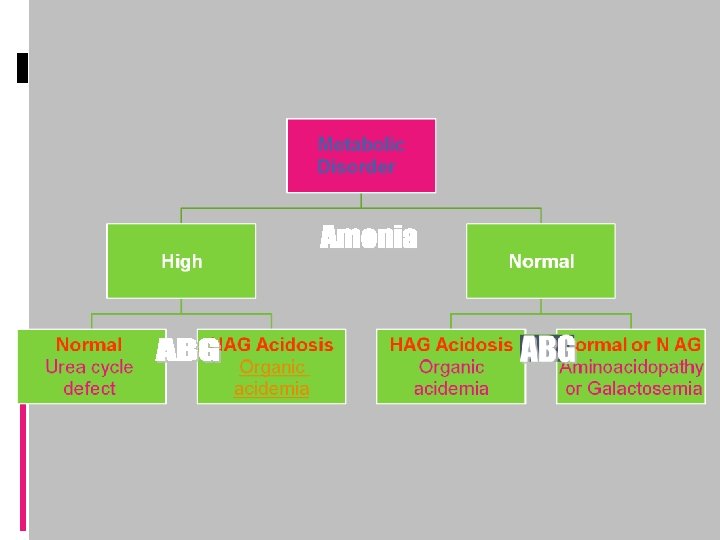
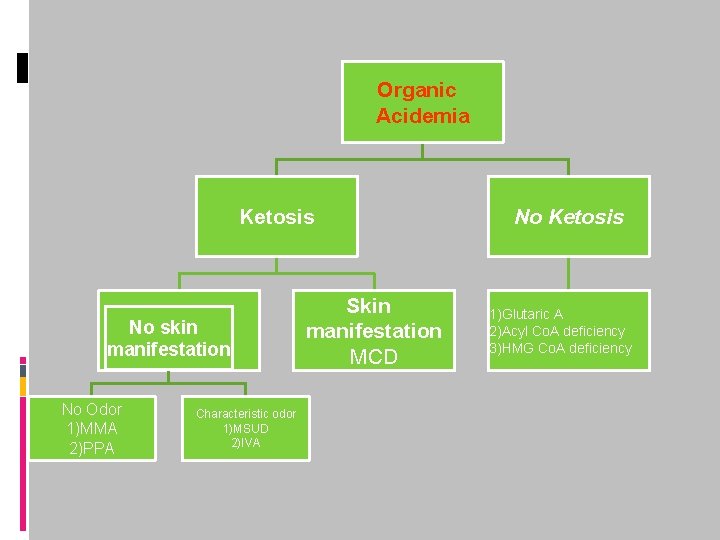
Organic Acidemia Ketosis No skin No manifestation No Odor 1)MMA 2)PPA Characteristic odor 1)MSUD 2)IVA Skin manifestation MCD No Ketosis 1)Glutaric A 2)Acyl Co. A deficiency 3)HMG Co. A deficiency
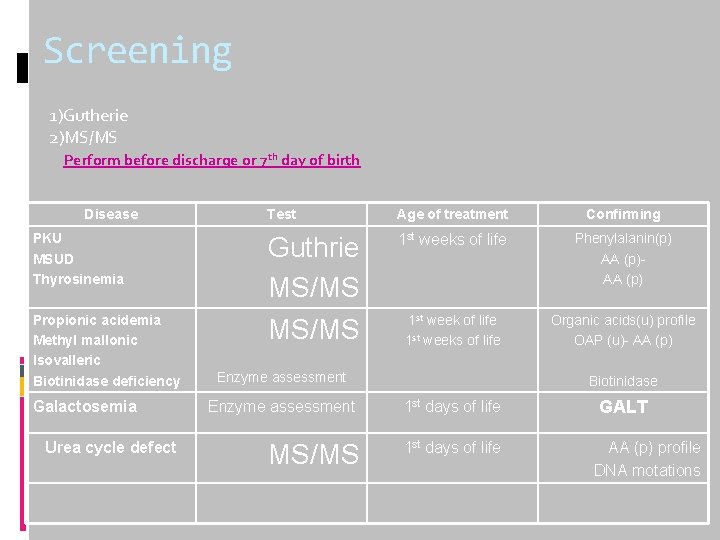
Screening 1)Gutherie 2)MS/MS Perform before discharge or 7 th day of birth Disease PKU MSUD Thyrosinemia Propionic acidemia Methyl mallonic Isovalleric Biotinidase deficiency Galactosemia Urea cycle defect Test Age of treatment Confirming Guthrie MS/MS 1 st weeks of life Phenylalanin(p) AA (p) 1 st week of life 1 st weeks of life Organic acids(u) profile OAP (u)- AA (p) Enzyme assessment Biotinidase Enzyme assessment 1 st days of life MS/MS 1 st days of life GALT AA (p) profile DNA motations

Treatment in hyprammonemia 1. D/C oral intake temporarily 2. Usually IVF’s with glucose to give 12 -15 mg/kg/min glu and at least 60 kcal/kg to prevent catabolism (may worsen PDH) 3. Bicarb/citrate 4. Carnitine/glycine 5. Na benzoate/arginine/citrulline 6. Dialysis--not exchange transfusion 7. Vitamins--often given in cocktails after labs drawn before dx is known Biotin, B 6, B 12, riboflavin, thiamine, folate

Metabolic Disorders Presenting as Severe Neonatal Disease 1. Disorders of Carbohydrate Metabolism • Galactosemia - presents with severe liver disease, gram negative sepsis, and/or cataracts Enz deficiency: Gal-1 -phos uridyl transferase, UDP-gal-4 -epimerase • Glycogen storage disease type 1 a & 1 b - presents as hypoglycemia Enz deficiency: Glucose-6 phosphatase Lactic Acidosis - presents as lactic acidosis +/- hypoglycemia Enz deficiency: Pyruvate carboxylase, Pyr dehydrogenase, etc. • Fructose intolerance - Needs fructose exposure, hypoglycemia and acidosis

Metabolic Disorders Presenting as Severe Neonatal Disease 2. Amino Acid Disorders • Maple syrup urine disease - presents with odor to urine and CNS problems • Nonketotic hyperglycinemia - presents with CNS problems • Enz deficiency: Branched chain ketoacid decarboxylase Enz deficiency: Glycine cleavage system Tyrosinemia - Severe liver disease, renal tubular dysfunction Enz deficiency: Fumaryl acetate Transient tyrosinemia of prematurity - progressive coma following respiratory distress

Metabolic Disorders Presenting as Severe Neonatal Disease 3. Urea Cycle Defects and Hyperammonemia 4. All present with lethargy, seizures, ketoacidosis, neutroenia, and hyperammonemia Ornithine carbamyl transferase (OTC) deficiency Carbamyl phosphate synthetase deficiency Citrullinemia Arginosuccinic Aciduria Argininemia Transient tyrosinemia of prematurity

Metabolic Disorders Presenting as Severe Neonatal Disease All present with lethargy, seizures, ketoacidosis, neutropenia, hyperammonemia, and/or hyperglycinemia 4. Organic Acid Defects • Methylmalonic acidemia • Proprionic acidemia • Isovaleric acidemia - odor of “sweaty feet” • Glutaric aciduria type II • Dicarboxylic aciduria 5. Miscellaneous • Peroxisomal disorders • Lysosomal storage disease • Pyridoxine dependent seizures

Amino acids metabolism diorders

Phenyl ketonuria AR Prevalence 1/10000 They are normal at birth.
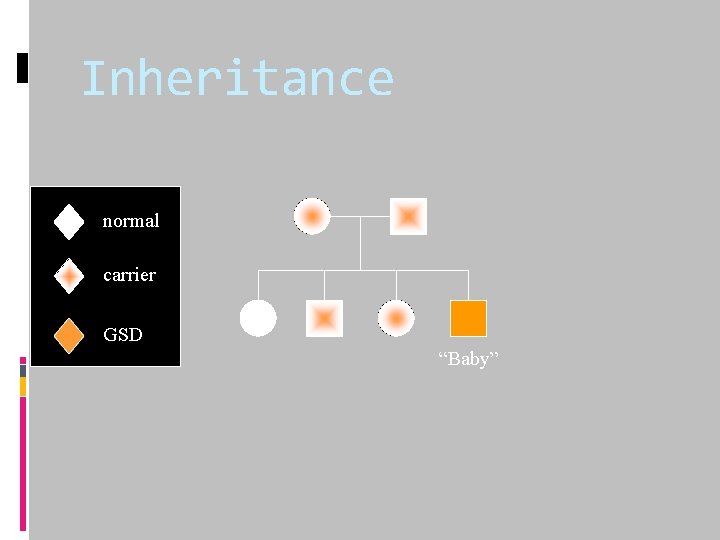
Inheritance normal carrier GSD “Baby”
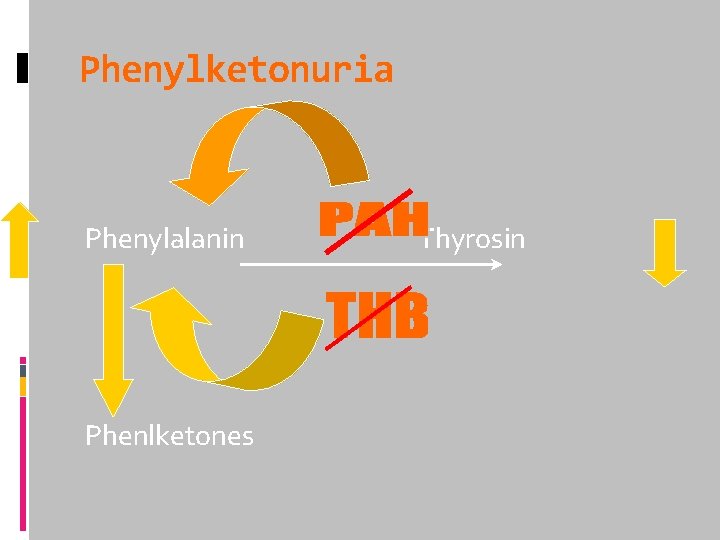
Phenylketonuria Phenylalanin Phenlketones Thyrosin

Clinical manifestation Normal at birth Severe MR(IQ<30) Blound appearance Odor Microcephalia Seborroic dermatitis Dominant maxilla

Diagnosis Ferric chloride test(urin phenyl ketones) Guthrie test Screening test MS/MS Phenylalanin>6 mg/dlit(360 mic M) Thyrosin (low) Diagnostic test

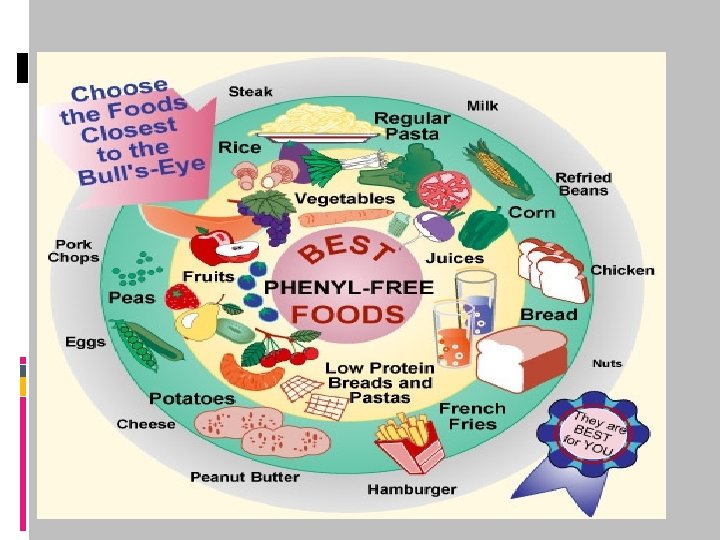
Treatment Low phenylalanin Regimen (Phenylalanin 2 -6 mg/dlit) Treatment must start in first 10 days of life. It must be continued till 10 -12 yrs old. In malignant PKU, Neurotransmitters are needed. (BH 4) + Maternal hyperphenylallanenimia MR-Microcephallia-CHD

Carbohydrate metabolism disorders

1)Galactosemia Lactose Glucose+Galactose -1_phosphate Glucose-1 -Phosphate

Clinical findings Feeding Hepatic failure (Bil –Coagulopathy -Glu) Tubulopathy (Acidosis-Glucosuria-A aciduria) Cataract E coli sepsis is more than others In older patients Learning disorders-Ovarian Failure Diagnosis: Screening Urin reducing substrare Diagnostic test RBCs Gal 1 -P U transferase
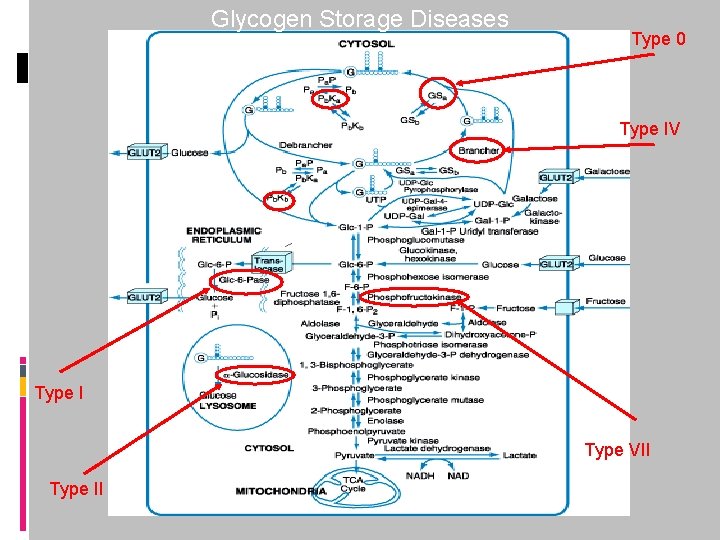
Glycogen Storage Diseases Type 0 Type IV Type I Type VII Type II
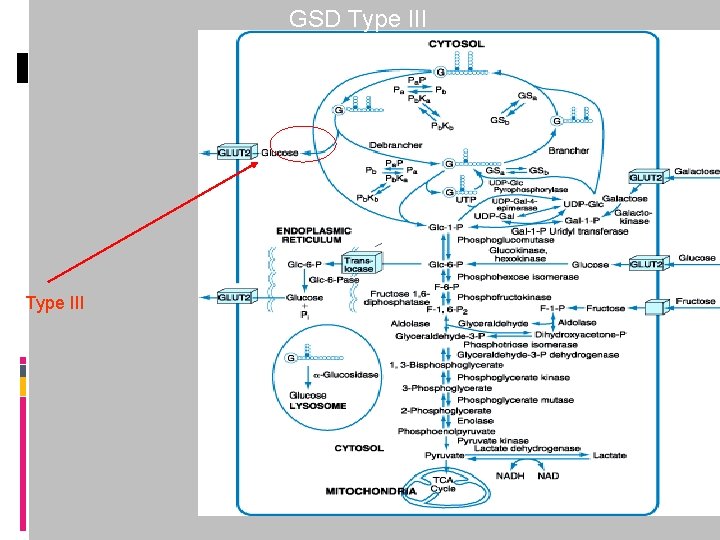
GSD Type III

2)Glycogen storage diseases 1) liver involement &Hypoglycemia (1 -6 -8) 2) Muscle involvement (5 -7) 3) Both of liver and Muscle (3) 4) Without any effect on Glucose & anearobic activities (2 -4)
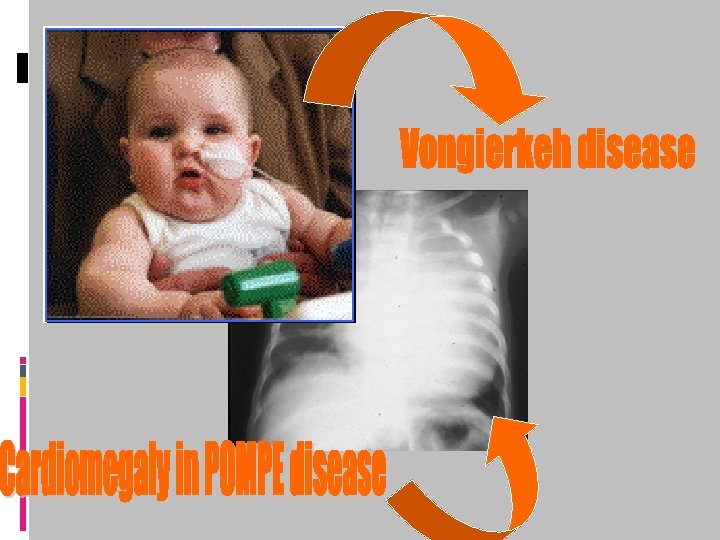
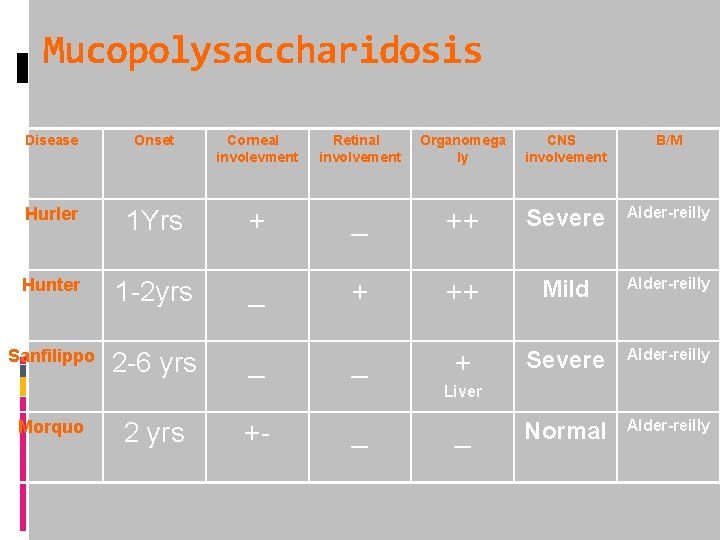
Mucopolysaccharidosis Disease Onset Corneal involevment Retinal involvement Organomega ly CNS involvement B/M Hurler 1 Yrs + _ ++ Severe Alder-reilly Hunter 1 -2 yrs _ + ++ Mild Alder-reilly Sanfilippo 2 -6 yrs _ _ + Severe Alder-reilly Normal Alder-reilly Liver Morquo 2 yrs +- _ _
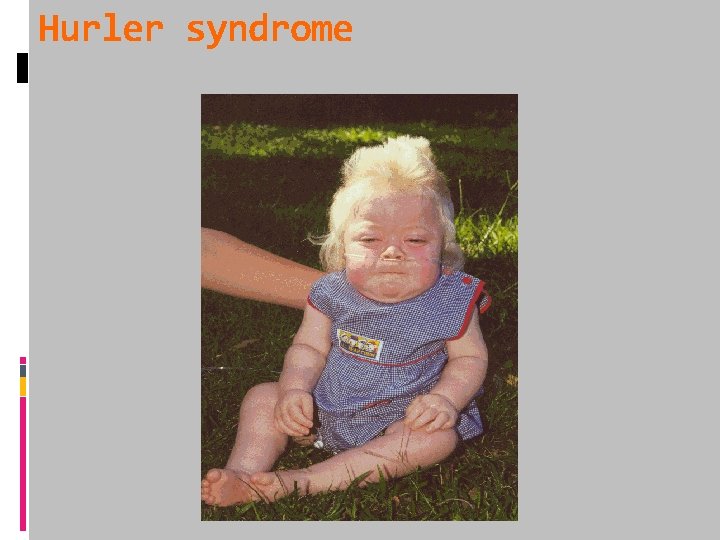
Hurler syndrome
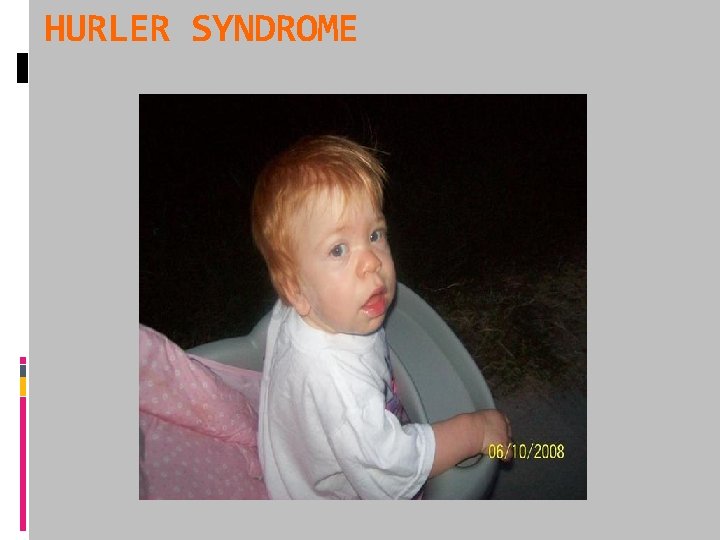
HURLER SYNDROME

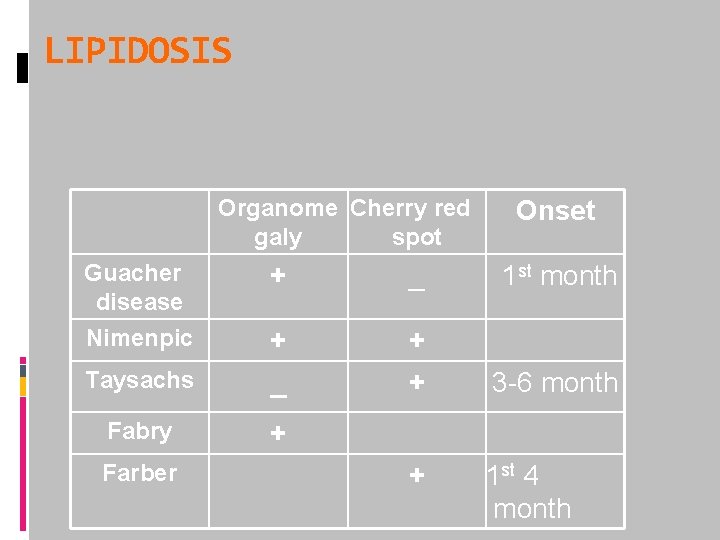
LIPIDOSIS Organome Cherry red galy spot Onset Guacher disease Nimenpic + _ + + Taysachs _ + 3 -6 month Fabry + + 1 st 4 month Farber 1 st month

Treatment in hyprammonemia 1. D/C oral intake temporarily 2. Usually IVF’s with glucose to give 12 -15 mg/kg/min glu and at least 60 kcal/kg to prevent catabolism (may worsen PDH) 3. Bicarb/citrate 4. Carnitine/glycine 5. Na benzoate/arginine/citrulline 6. Dialysis--not exchange transfusion 7. Vitamins--often given in cocktails after labs drawn before dx is known Biotin, B 6, B 12, riboflavin, thiamine, folate
- Slides: 32