Exploring Health Literacy Issues in Tennessee TENNESSEE CHARITABLE

Exploring Health Literacy Issues in Tennessee TENNESSEE CHARITABLE CARE NETWORK TENNESSEE’S MEMBERSHIP ASSOCIATION OF CHARITABLE HEALTHCARE CLINICS JULY 2015

Background �Tennessee Charitable Care Network (TCCN) Formed in 2014 Membership organization for 22 of the 46 known clinics that deliver health care to people without access to insurance coverage in communities throughout the state Vital resource and advocate for the vulnerable populations and communities served by its members Majority of TCCN members receive funding through the state’s Health Care Safety Net Fund

Health Literacy Workshop �Sponsored by the Tennessee Department of Health (TDH) to bring together TCCN members for interactive dialogue �Provided opportunities for charitable clinic leaders to share their experiences in how health literacy issues impact patient care and outcomes generate preliminary recommendations about best practices to address specific barriers to care.

Providing Care from East to West

Sharing Stories, Finding Common Ground BARRIERS AND COMMONALITIES

Barriers to Health Literacy �Cultural barriers �Finances/financial literacy �Language barriers �Limited/little formal �Social/environmental education �No medical home �Behavioral health �Lack of understanding �Patient/provider relationship �Lack of knowledge �Personal issues �Health insurance

Commonalities Among Clinic Patients �Barriers seen in most clinic patients on a daily basis �Clinic patients experience significant stressors �Many patients experience multiple barriers �Clinics often become the “support system” for people without means �Many clinics must informally take on the role of “social worker” �Medicine alone cannot solve these issues – “we provide hope” �A lot of issues can be defined by a knowledge deficit �Cultural issues are not just related to foreign born patients
Charitable Clinics Provide Hope

IMPACT HEALTH LITERACY’S IMPACT ON HEALTH OUTCOMES

Obesity Measures: BMI & Skin fold th TN ranked 47 in obesity and 49 th in physical inactivity TN had 5 th highest rate of childhood obesity in 2010 5 of 10 top 10 causes of death in TN (2013) related to obesity Characteristics of Population Characteristics of Health System • 50% of clinic patients diagnosed with obesity and • Focuses on symptoms not causes of chronic 39% are physically inactive. conditions. • Physical inactivity increased by 17% among • Limited funds invested in prevention resources. adults in TN. • Limited awareness of the complex determinants of • Low-income communities have fewer grocery obesity. stores. • Cultural and language barriers may not be adequately • Obesity associated with lower education levels addressed in providing instructions for weight loss. and poverty. • Patients with insurance may receive preferential • Patients unable to read or comprehend treatment. nutritional labels. • Limited awareness of community resources available • Low-income families rely on “fast food” options. • Focus on wellness is limited when patients present • Cultural tradition of eating higher fat foods. with multiple conditions requiring immediate attention. Interactions • Materials about nutrition/weight loss are not always available in culturally sensitive formats and language. • Providers need strategies to address health literacy barriers (motivational interviewing and goal setting). • Increase provider knowledge about community resources accessible to the patient population. • “Wellness programs” provide information on nutrition & physical activities in a supportive environment.

Obesity OBESITY – Problem Statements: � The number of people with low levels of physical activity (less than 30 minutes 5 x/week) is a contributing factor in the growing epidemic of obesity in the U. S. and in Tennessee. Obese individuals face significant health consequences in comparison to the active population. � Inadequate nutritional education, limited understanding of healthy eating guidelines, and lack of access to quality foods are direct contributors to obesity. Evidence shows that obesity is linked to many serious health problems including heart disease, stroke, diabetes and some types of cancer. These conditions are among the leading causes of death in the U. S. and are more prevalent with obese individuals when compared to populations consuming proper nutrition. � Financial limitations of low-income individuals and families negatively impact access to quality nutrition and access to community resources for weight loss when compared to higher income populations. The incidence of obesity has grown at an alarming rate throughout the southern U. S. and in Tennessee.
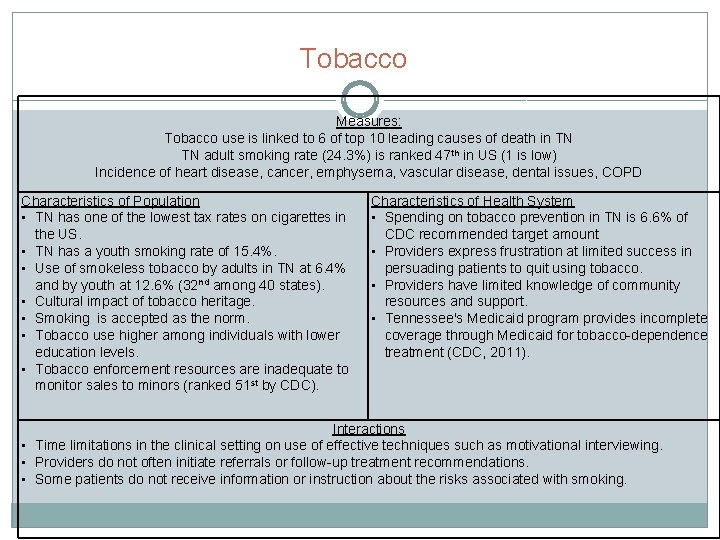
Tobacco Measures: Tobacco use is linked to 6 of top 10 leading causes of death in TN TN adult smoking rate (24. 3%) is ranked 47 th in US (1 is low) Incidence of heart disease, cancer, emphysema, vascular disease, dental issues, COPD Characteristics of Population • TN has one of the lowest tax rates on cigarettes in the US. • TN has a youth smoking rate of 15. 4%. • Use of smokeless tobacco by adults in TN at 6. 4% and by youth at 12. 6% (32 nd among 40 states). • Cultural impact of tobacco heritage. • Smoking is accepted as the norm. • Tobacco use higher among individuals with lower education levels. • Tobacco enforcement resources are inadequate to monitor sales to minors (ranked 51 st by CDC). Characteristics of Health System • Spending on tobacco prevention in TN is 6. 6% of CDC recommended target amount • Providers express frustration at limited success in persuading patients to quit using tobacco. • Providers have limited knowledge of community resources and support. • Tennessee's Medicaid program provides incomplete coverage through Medicaid for tobacco-dependence treatment (CDC, 2011). Interactions • Time limitations in the clinical setting on use of effective techniques such as motivational interviewing. • Providers do not often initiate referrals or follow-up treatment recommendations. • Some patients do not receive information or instruction about the risks associated with smoking.

Tobacco TOBACCO – Problem Statements: � There is a high prevalence of smoking in the State of TN and even higher incidence of smoking among the populations served by free and charitable clinics. Since TN is ranked by CDC Best Practices as the 45 th worse state in terms of spending on anti-tobacco media campaigns, we are not reaching enough adults or youth with effective prevention and cessation messages to increase knowledge or impact behaviors. � There is an increase in health risks associated with adult smokers with income under $25 k annually and with high school or less education levels. These same populations face multiple barriers in accessing smoking cessation programs and medications. � Cigarette smoking by youth and young adults has immediate adverse health impacts and increases the incidence of chronic health disease throughout the life span. Tennessee is not focusing adequate resources on enforcement or prevention/cessation promotion to lower the number of youth and young adults who begin or continue smoking.

Adult Oral Health Measures: ER visits, Dental referrals & frequency of dental visits Caries rate & Number of people missing teeth Incidence of preventive treatment for children (sealants) Characteristics of Population Characteristics of Health System • 20% of adults in TN have lost 6 or more teeth • Tennessee is among 6 states that do not cover • Only 66% of adults in TN visited a dentist in dental care for Medicaid enrollees 21 and older. 2010 • The number of dentists available in “safety net” • Cultural norm to get dentures at young age. settings is inadequate to need. • Non-elderly low-income adults mention lack of • The U. S. Dept. of HHS categorizes 94 percent funds/ insurance as barrier to care. of Tennessee counties (89 of 95) as having • Fear /anxiety. dental health professional shortage areas. • TN ranked 37 th for smoking and 41 st for • County health departments provide only smokeless tobacco use in 2011 (CDC). emergency dental care to adults • Poor nutrition increases risk for dental caries. Interactions • ER staff lack knowledge about how to treat dental patients and lack resources. • Dentists have insufficient knowledge about low income populations and their cultural issues. • Patients and PCPs have limited knowledge about the importance of regular dental care to adult health. • There is a lack of patient education about connection between healthy foods and dental health. • Stopgap measures in primary care utilized in the absence of affordable dental care. • Patient education should include an emphasis on the benefits of continuing care.

Adult Oral Health ORAL HEALTH – Problem Statements: � In Tennessee, the availability of ongoing, regular, preventive affordable dental care for adults is limited to universities, FQHCs, and faith-based clinics (and many of these see more children than adults). This reflects the ADA’s report that fewer than 2% of the nation’s dentists work in safety net settings (August 2011). � In Tennessee, 33. 7 % over 65 have had all teeth extracted. According to Oral Health America’s State of Decay report, Tennessee is ranked 49 th in the nation for adequacy of dental care. The barriers to adult dental care, including lack of funds/insurance, fear, lack of knowledge about benefits of preventive care, and avoidance due to cultural norms and language barriers, have not been adequately addressed in order to improve access to care leading to better dental outcomes. � ER visits for preventable oral disease are on the rise with very limited efficacies. Contributing factors include lack of access to dentists, lack of knowledge/education, and financial issues/lack of insurance. All adult visits, especially 20 – 40 years, are increasing every year; the number is under-documented due to patients who present with multiple issues. Oral disease is more common (by 5 x) than the number of patients presenting to ER with burns. There is an estimate of more than 53, 000 dental ER visits per year in TN (Pew Center).

Sharing Tools and Techniques TOOLS CURRENTLY IN USE BEST PRACTICES CASE SCENARIOS

Sharing Tools and Techniques �Current Health Literacy Assessment Tools and Techniques: Pre-treatment 1: 1 interviews with inquiry about fluency Chronic disease assessment survey Motivational interviewing Thorough check-out/review with nurse after seeing provider Requirement for patient to see provider for all prescription med renewals Monthly visits/assessment Oral Health literacy and home practice – pre and post survey Opiate abuse evaluation Confirmation patient understands instructions through feedback/listening

“Best Practice” Strategies to Address Health Literacy Barriers �Samples include: Use of metaphors/stories with cultural relevance Drawing – “word pictures” Professional development for staff on cultural norms and serving the underserved Nurses write purpose of prescription on patient’s med bottle i. Translate (i. Phone, i. Pad) and other apps Use of props Wellness programs and group visits Sliding fee scales and PAPs for Rx Patient goals Health coaches
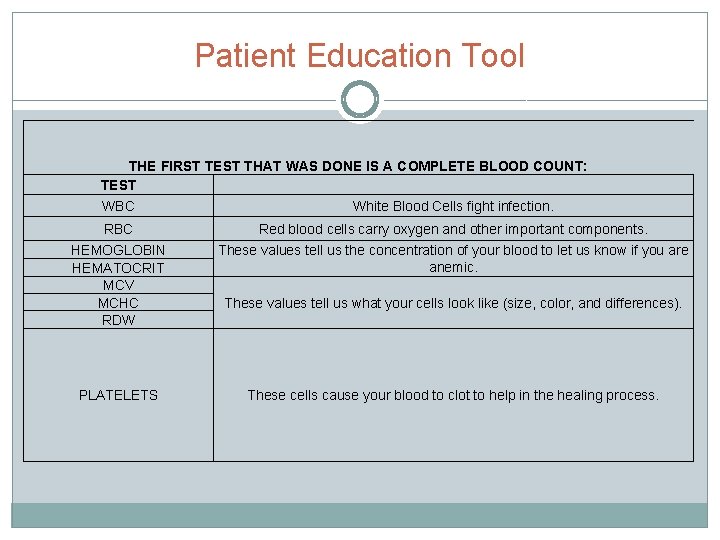

Patient Education Tool THE FIRST TEST THAT WAS DONE IS A COMPLETE BLOOD COUNT: TEST WBC White Blood Cells fight infection. RBC Red blood cells carry oxygen and other important components. HEMOGLOBIN HEMATOCRIT MCV MCHC RDW These values tell us the concentration of your blood to let us know if you are anemic. PLATELETS These cells cause your blood to clot to help in the healing process. These values tell us what your cells look like (size, color, and differences).

Case Scenarios: Use of Metaphors �A physician who had practiced in Alaska described the use of pictures and metaphors in communicating with native people who have distinctive cultures. �She described having observed a colleague who effectively used a culturally relevant metaphor and picture in communicating the need to take medication for a chronic condition. �She adapted the concept of metaphor with a male patient from a rural community in another state by using the concept of a “warning light” on a car to help him understand the importance of monitoring his blood pressure.

Case Scenarios: Nutrition �The administrator of a clinic serving a population with high incidence of obesity described the use of brightly colored portion control rings (available through Portion. Mate. TM) to help patients learn to measure healthy food portions. �Another urban clinic offers an on-site garden where patients and their families participating in a wellness program are involved in growing, harvesting and preparing vegetables from the community garden.

Case Scenarios: Engaging Patients �A physician from an organization that provides services to a patient population approximately 80% refugee or immigrant described the importance of having a “hospitality coordinator” to engage each personally upon arrival at the clinic. �The person in this role is friendly and proactive in assuring that the patient and his/her family feels welcome and engaged in care. �The same organization has a Patient Resource Room where tools, such as a computer with pre-bookmarked sites, are available to meet individual cultural and language needs.

Changing Lives

Finding Ways to Close the Gap INDIVIDUAL CLINIC / HEALTHCARE SYSTEM COMMUNITY-WIDE

Finding Ways to Close the Gap INDIVIDUAL Address Personal Issues & Promote Self-Worth �Denial motivational interviewing; help patient acknowledge their denial; counseling; support groups; interactive tools �Fear information via media and mass campaigns; less fear-based messages; develop trust with patients; “perfect love casts out fear” �Ownership Re-train medical community to be “coaches” rather than talking to/at patient �Compliance Find root causes; timely reminders of appointments; check out with a nurse; guided/assisted compliance via advocates; cultural competency

Finding Ways to Close the Gap CLINIC/HEALTHCARE SYSTEM � Assessment tools – what are barriers? How to know what to ask? � Cultural competency � Provider/staff training – build health education into school curriculum and strategies to address obesity � Messaging to communities/outside influence – culturally relevant � Increase funding to clinics to implement strategies hire, train, purchase computers, computers for patients, etc. � Negotiated rate for Language Line services � Telehealth to increase access � TV/Online diabetes health education � Share best practices for improving no show rate � Social service directory – online and up to date including dental, behavioral health, specialty resources (build on 211) � Leverage partnerships – health departments, health councils, etc.

Finding Ways to Close the Gap COMMUNITY-WIDE � Incentives for healthy outcomes � Reach/outreach to parents through school-age kids - kids will have better habits as adults � More sustainable/development activities – Support for farmers markets; SNAP cards at farmers markets; Community gardens � Community Health “Ambassadors” to convene activities/education � Funding for health literacy activities � Faith/community outreach via Health Ambassadors � Incentives/reasons for people to change habits Need to make it “cool” – the thing everyone is doing Well-known spokesperson Statewide challenge between towns/communities � Patient peers - Patients enlist each other Why do patients participate? Share that with others

Tennessee Thank You! Charitable Care Network (TCCN) https: //www. tccnetwork. org/home. html Christi Granstaff, Executive Director christigranstaff@bellsouth. net 615. 274. 9665 TCCN members are a statewide community of healthcare providers who have a shared sense of mission and face many of the same challenges. Given the complexity and scope of the problem, TCCN is grateful to partner with the Tennessee Department of Health to address the issues related to health literacy of vulnerable populations in Tennessee.
- Slides: 28