Exercise total body effects Immediate vs long term

Exercise: total body effects: Immediate vs. long term; Adaptive and Maladaptive Metro IB Sports, Exercise and Health Spring 2020 Stan Misler <stan. misler. il@gmail. com>
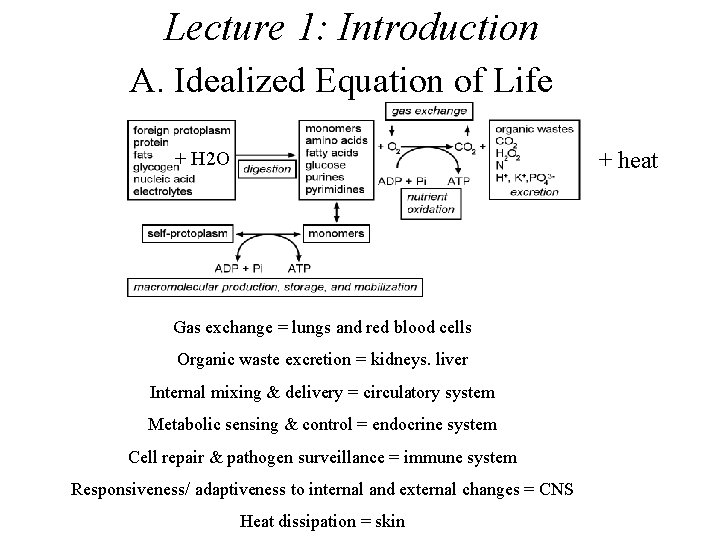
Lecture 1: Introduction A. Idealized Equation of Life + heat + H 2 O Gas exchange = lungs and red blood cells Organic waste excretion = kidneys. liver Internal mixing & delivery = circulatory system Metabolic sensing & control = endocrine system Cell repair & pathogen surveillance = immune system Responsiveness/ adaptiveness to internal and external changes = CNS Heat dissipation = skin
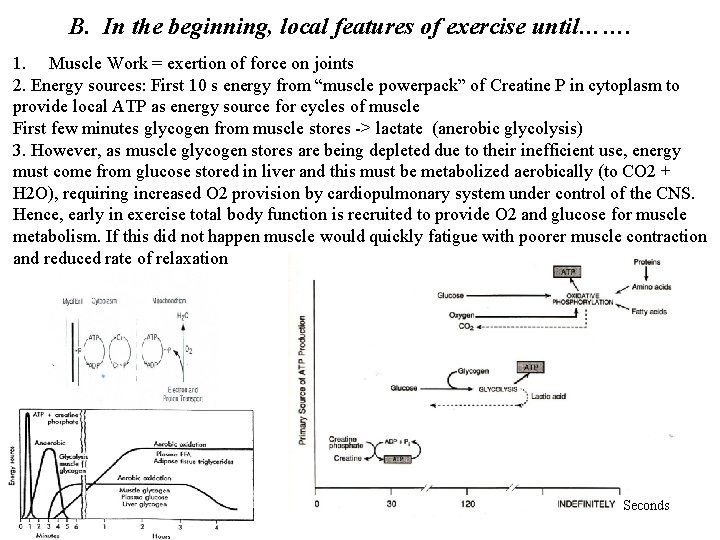
B. In the beginning, local features of exercise until……. 1. Muscle Work = exertion of force on joints 2. Energy sources: First 10 s energy from “muscle powerpack” of Creatine P in cytoplasm to provide local ATP as energy source for cycles of muscle First few minutes glycogen from muscle stores -> lactate (anerobic glycolysis) 3. However, as muscle glycogen stores are being depleted due to their inefficient use, energy must come from glucose stored in liver and this must be metabolized aerobically (to CO 2 + H 2 O), requiring increased O 2 provision by cardiopulmonary system under control of the CNS. Hence, early in exercise total body function is recruited to provide O 2 and glucose for muscle metabolism. If this did not happen muscle would quickly fatigue with poorer muscle contraction and reduced rate of relaxation Seconds

C. Systemic Control of Visceral Organ Function in Exercise a. Cerebral cortex and thalamus, which measure muscle contractile “need” and control “motor program” (recruitment of motor unit activity), also controls a “central visceromotor program” (CVMP), beginning in the hypothalamus of the brain and regulating visceral functions (circulatory, ventilator and endocrine) on a moment to moment basis CVMP controls heart’s pumping of blood supply, namely how often it contracts and how much blood it puts out with each contraction + decision of which peripheral vessels receive the blood supply. CVMP controls how often and how deeply we breathe to provide O 2 for aerobic metabolism of nutrients and take away and exhale CO 2 (receives into CVMP (through the endocrine system) controls how much glucose is released by liver for aerobic metabolism in muscle CVMP controls how much our skin sweats to allow for fluid evaporation and thus dissipation of excess heat of muscle contraction into the environment b. Tight CVMP coordination with motor program: responsiveness to multiple higher CNS inputs for preparation and performance of exercise: the thalamus as exercise rehearse + amygdala which recognizes scary scenes to be run away from. Recall “motor program” = pre-motor cortex excites a cortico-thalamic-basal ganglia-cerebellar axis to maximize efficiency and smoothness of motor activity & controls overall behavior (fear/flight)
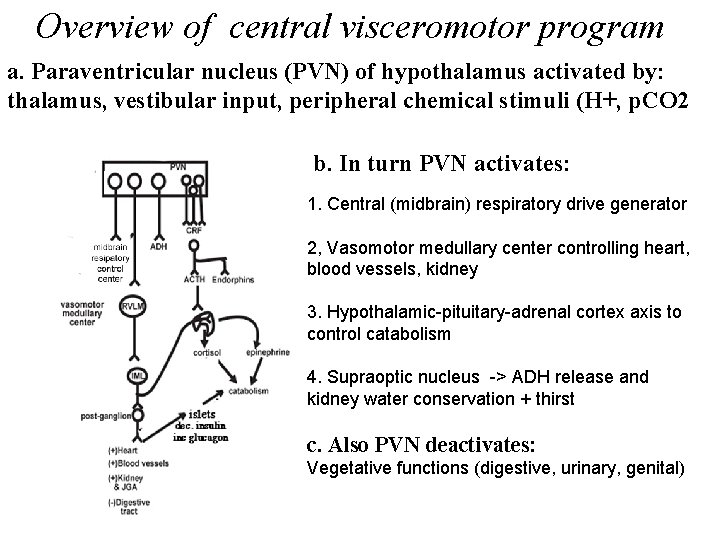
Overview of central visceromotor program a. Paraventricular nucleus (PVN) of hypothalamus activated by: thalamus, vestibular input, peripheral chemical stimuli (H+, p. CO 2 b. In turn PVN activates: 1. Central (midbrain) respiratory drive generator 2, Vasomotor medullary center controlling heart, blood vessels, kidney 3. Hypothalamic-pituitary-adrenal cortex axis to control catabolism 4. Supraoptic nucleus -> ADH release and kidney water conservation + thirst c. Also PVN deactivates: Vegetative functions (digestive, urinary, genital)
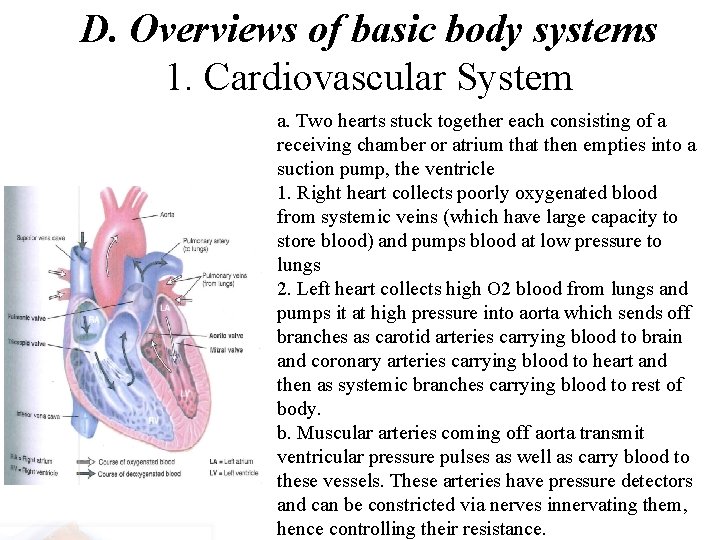
D. Overviews of basic body systems 1. Cardiovascular System a. Two hearts stuck together each consisting of a receiving chamber or atrium that then empties into a suction pump, the ventricle 1. Right heart collects poorly oxygenated blood from systemic veins (which have large capacity to store blood) and pumps blood at low pressure to lungs 2. Left heart collects high O 2 blood from lungs and pumps it at high pressure into aorta which sends off branches as carotid arteries carrying blood to brain and coronary arteries carrying blood to heart and then as systemic branches carrying blood to rest of body. b. Muscular arteries coming off aorta transmit ventricular pressure pulses as well as carry blood to these vessels. These arteries have pressure detectors and can be constricted via nerves innervating them, hence controlling their resistance.
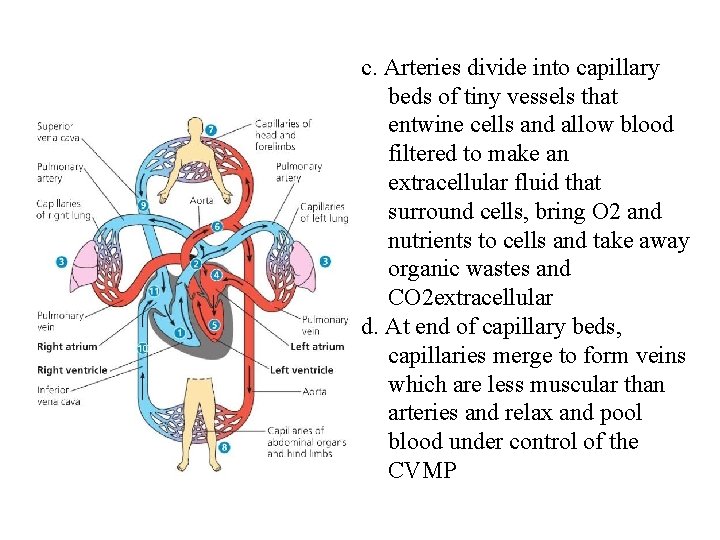
c. Arteries divide into capillary beds of tiny vessels that entwine cells and allow blood filtered to make an extracellular fluid that surround cells, bring O 2 and nutrients to cells and take away organic wastes and CO 2 extracellular d. At end of capillary beds, capillaries merge to form veins which are less muscular than arteries and relax and pool blood under control of the CVMP
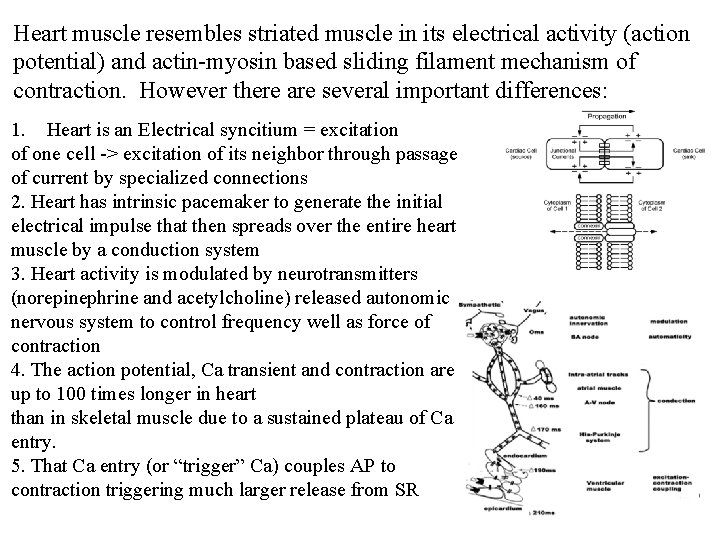
Heart muscle resembles striated muscle in its electrical activity (action potential) and actin-myosin based sliding filament mechanism of contraction. However there are several important differences: 1. Heart is an Electrical syncitium = excitation of one cell -> excitation of its neighbor through passage of current by specialized connections 2. Heart has intrinsic pacemaker to generate the initial electrical impulse that then spreads over the entire heart muscle by a conduction system 3. Heart activity is modulated by neurotransmitters (norepinephrine and acetylcholine) released autonomic nervous system to control frequency well as force of contraction 4. The action potential, Ca transient and contraction are up to 100 times longer in heart than in skeletal muscle due to a sustained plateau of Ca entry. 5. That Ca entry (or “trigger” Ca) couples AP to contraction triggering much larger release from SR
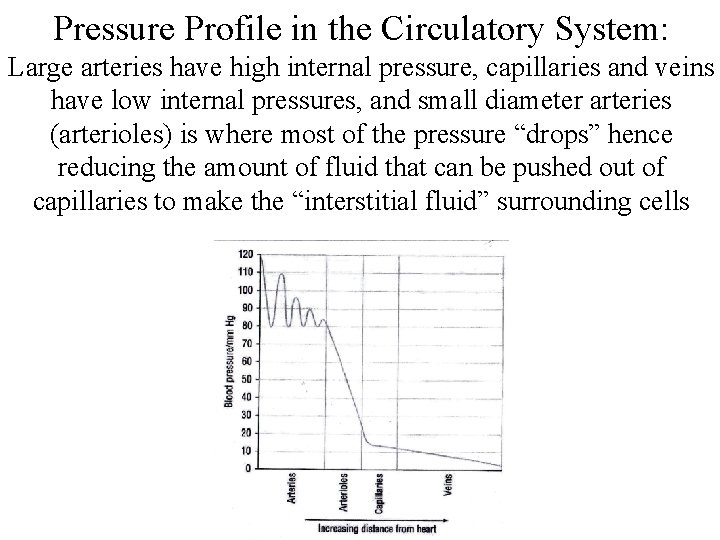
Pressure Profile in the Circulatory System: Large arteries have high internal pressure, capillaries and veins have low internal pressures, and small diameter arteries (arterioles) is where most of the pressure “drops” hence reducing the amount of fluid that can be pushed out of capillaries to make the “interstitial fluid” surrounding cells
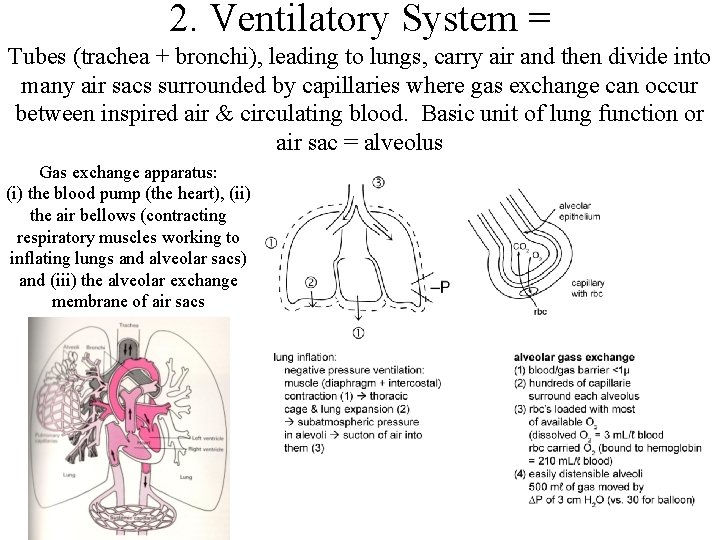
2. Ventilatory System = Tubes (trachea + bronchi), leading to lungs, carry air and then divide into many air sacs surrounded by capillaries where gas exchange can occur between inspired air & circulating blood. Basic unit of lung function or air sac = alveolus Gas exchange apparatus: (i) the blood pump (the heart), (ii) the air bellows (contracting respiratory muscles working to inflating lungs and alveolar sacs) and (iii) the alveolar exchange membrane of air sacs
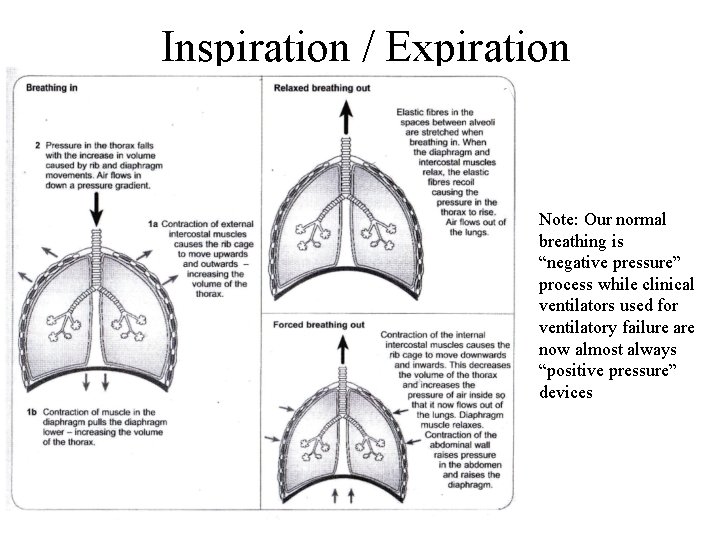
Inspiration / Expiration Note: Our normal breathing is “negative pressure” process while clinical ventilators used for ventilatory failure are now almost always “positive pressure” devices
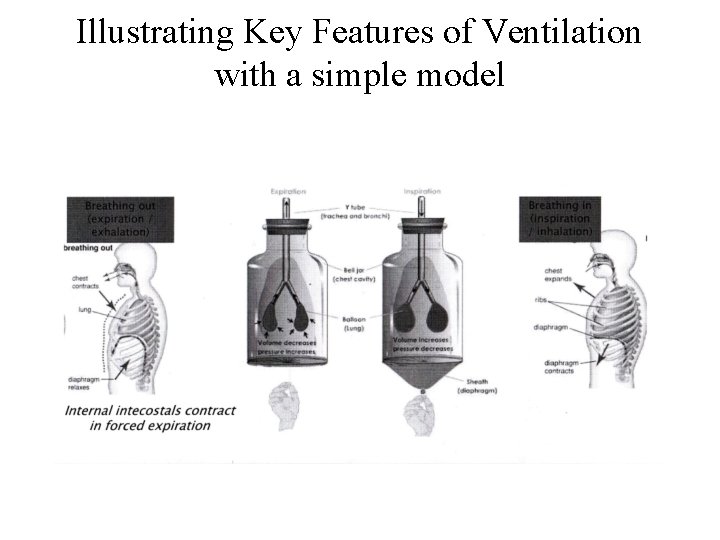
Illustrating Key Features of Ventilation with a simple model
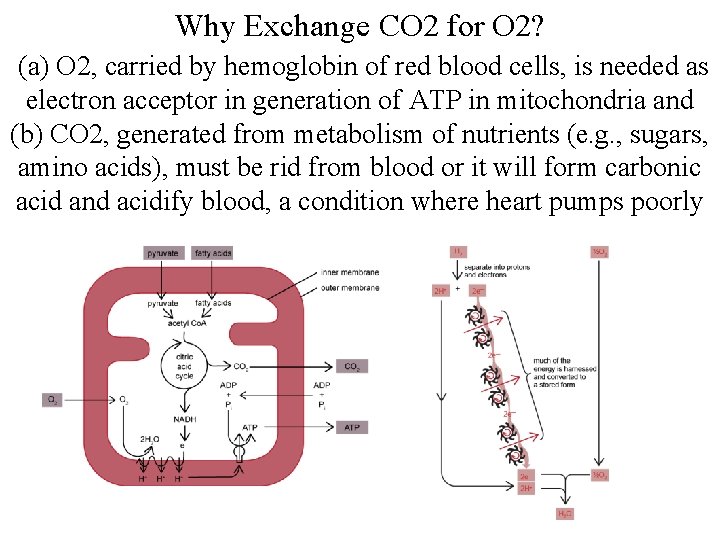
Why Exchange CO 2 for O 2? (a) O 2, carried by hemoglobin of red blood cells, is needed as electron acceptor in generation of ATP in mitochondria and (b) CO 2, generated from metabolism of nutrients (e. g. , sugars, amino acids), must be rid from blood or it will form carbonic acid and acidify blood, a condition where heart pumps poorly
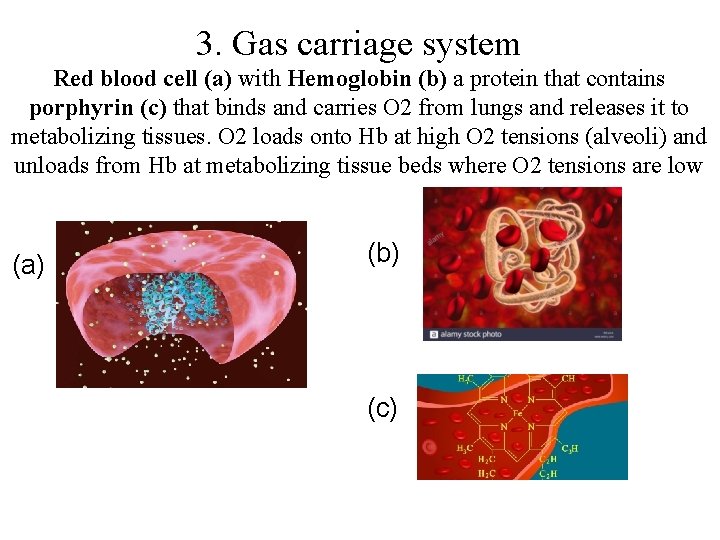
3. Gas carriage system Red blood cell (a) with Hemoglobin (b) a protein that contains porphyrin (c) that binds and carries O 2 from lungs and releases it to metabolizing tissues. O 2 loads onto Hb at high O 2 tensions (alveoli) and unloads from Hb at metabolizing tissue beds where O 2 tensions are low (a) (b) (c)
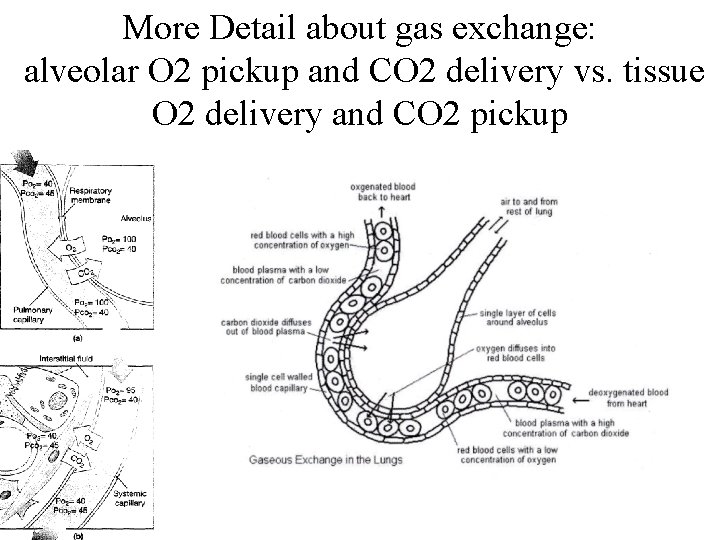
More Detail about gas exchange: alveolar O 2 pickup and CO 2 delivery vs. tissue O 2 delivery and CO 2 pickup

4. Excretory System: Kidney basic unit of function = nephron Kidney can get rid of nitrogen and other waste products while conserving salt and water when these are necessary to preserve blood volume as when lots of fluid is lost by sweat glands during body cooling by sweating
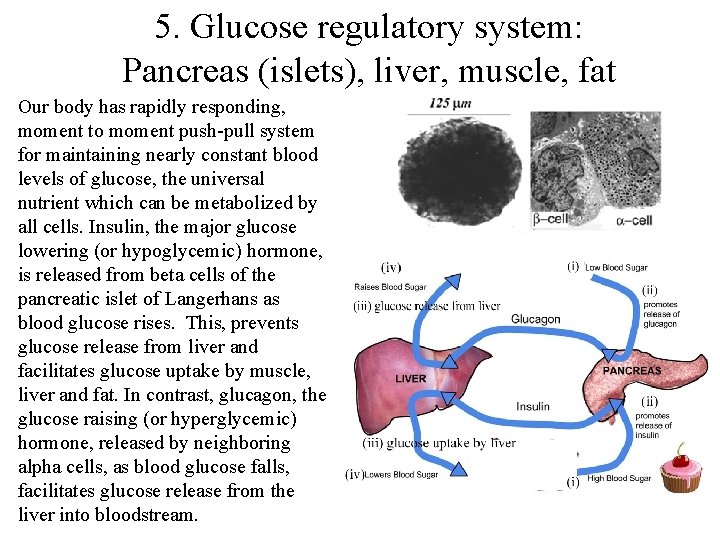
5. Glucose regulatory system: Pancreas (islets), liver, muscle, fat Our body has rapidly responding, moment to moment push-pull system for maintaining nearly constant blood levels of glucose, the universal nutrient which can be metabolized by all cells. Insulin, the major glucose lowering (or hypoglycemic) hormone, is released from beta cells of the pancreatic islet of Langerhans as blood glucose rises. This, prevents glucose release from liver and facilitates glucose uptake by muscle, liver and fat. In contrast, glucagon, the glucose raising (or hyperglycemic) hormone, released by neighboring alpha cells, as blood glucose falls, facilitates glucose release from the liver into bloodstream.

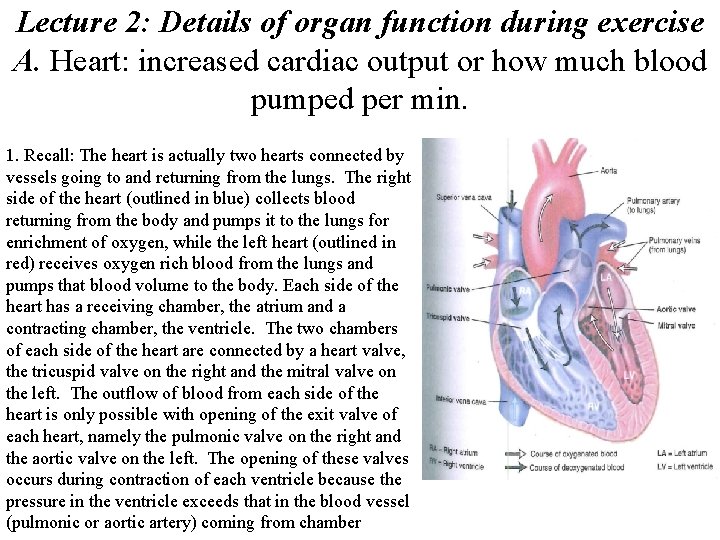
Lecture 2: Details of organ function during exercise A. Heart: increased cardiac output or how much blood pumped per min. 1. Recall: The heart is actually two hearts connected by vessels going to and returning from the lungs. The right side of the heart (outlined in blue) collects blood returning from the body and pumps it to the lungs for enrichment of oxygen, while the left heart (outlined in red) receives oxygen rich blood from the lungs and pumps that blood volume to the body. Each side of the heart has a receiving chamber, the atrium and a contracting chamber, the ventricle. The two chambers of each side of the heart are connected by a heart valve, the tricuspid valve on the right and the mitral valve on the left. The outflow of blood from each side of the heart is only possible with opening of the exit valve of each heart, namely the pulmonic valve on the right and the aortic valve on the left. The opening of these valves occurs during contraction of each ventricle because the pressure in the ventricle exceeds that in the blood vessel (pulmonic or aortic artery) coming from chamber
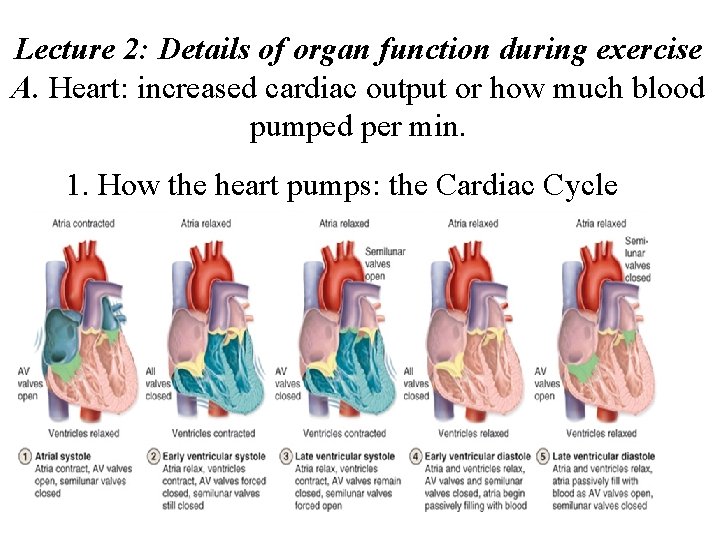
Lecture 2: Details of organ function during exercise A. Heart: increased cardiac output or how much blood pumped per min. 1. How the heart pumps: the Cardiac Cycle
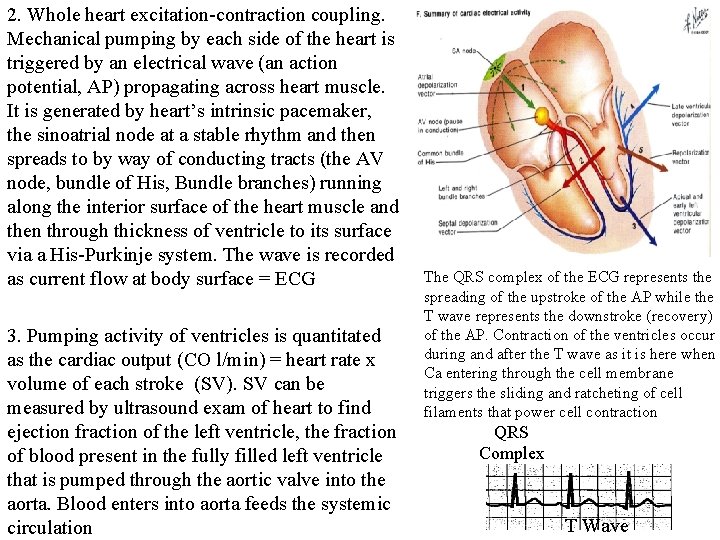
2. Whole heart excitation-contraction coupling. Mechanical pumping by each side of the heart is triggered by an electrical wave (an action potential, AP) propagating across heart muscle. It is generated by heart’s intrinsic pacemaker, the sinoatrial node at a stable rhythm and then spreads to by way of conducting tracts (the AV node, bundle of His, Bundle branches) running along the interior surface of the heart muscle and then through thickness of ventricle to its surface via a His-Purkinje system. The wave is recorded as current flow at body surface = ECG 3. Pumping activity of ventricles is quantitated as the cardiac output (CO l/min) = heart rate x volume of each stroke (SV). SV can be measured by ultrasound exam of heart to find ejection fraction of the left ventricle, the fraction of blood present in the fully filled left ventricle that is pumped through the aortic valve into the aorta. Blood enters into aorta feeds the systemic circulation The QRS complex of the ECG represents the spreading of the upstroke of the AP while the T wave represents the downstroke (recovery) of the AP. Contraction of the ventricles occur during and after the T wave as it is here when Ca entering through the cell membrane triggers the sliding and ratcheting of cell filaments that power cell contraction QRS Complex T Wave
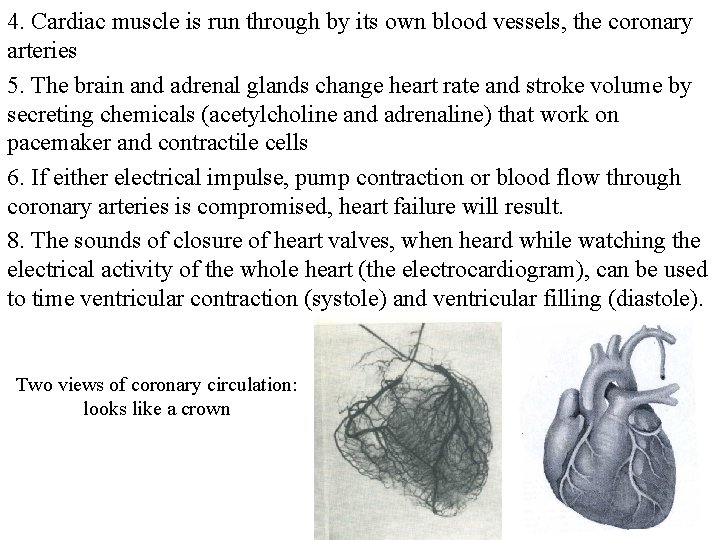
4. Cardiac muscle is run through by its own blood vessels, the coronary arteries 5. The brain and adrenal glands change heart rate and stroke volume by secreting chemicals (acetylcholine and adrenaline) that work on pacemaker and contractile cells 6. If either electrical impulse, pump contraction or blood flow through coronary arteries is compromised, heart failure will result. 8. The sounds of closure of heart valves, when heard while watching the electrical activity of the whole heart (the electrocardiogram), can be used to time ventricular contraction (systole) and ventricular filling (diastole). Two views of coronary circulation: looks like a crown

9. Dynamic exercise -> C. O. 5 -6 l/min 20 -25 l/min (<25% inc Part) (a) CVMP stimulates nerves to the heart to release adrenaline like compounds that increases SA node rate during exercise. This is known as a positive chronotropic effect of catecholamines on SA node (b) The same cardiac nerve also increases the force of contraction of the ventricle. This is known as positive inotropic effect on ventricles as well as the rate of relaxation of the ventricle so that it can fill with blood better in anticipation of the next contraction. This is known as positive lusotropic effect. Both of the latter effects can be mimicked by catecholamines released by adrenal glands also under same CVMP (c) Contraction of exercising muscle periodically empties it of blood thereby increasing venous return of blood thus providing it for increased cardiac output in part by stretching the sarcomeres of heart and putting them on more optimum part of length / tension (Starling) curve Note: If for some reason the heart has to be slowed, the vagus nerve can be recruited. It releases acetylcholine slowing the rate of depolarization and thus initiation of the action potential of the SA node = negative chronotropic effect
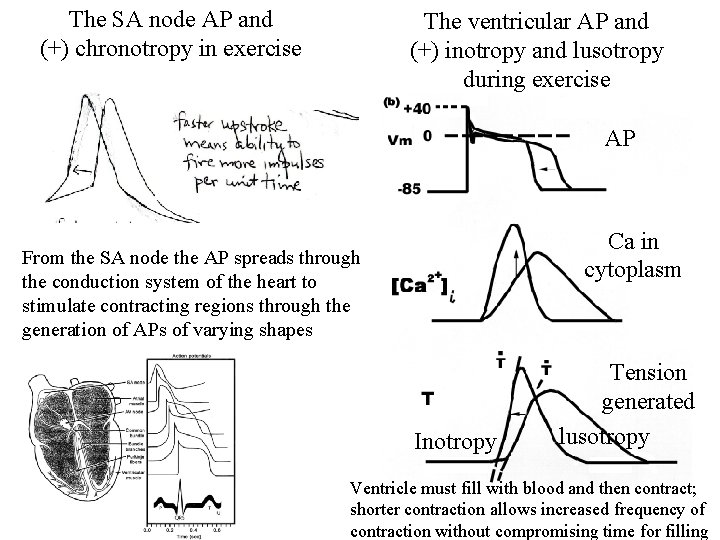
The SA node AP and (+) chronotropy in exercise The ventricular AP and (+) inotropy and lusotropy during exercise AP Ca in cytoplasm From the SA node the AP spreads through the conduction system of the heart to stimulate contracting regions through the generation of APs of varying shapes Inotropy Tension generated lusotropy Ventricle must fill with blood and then contract; shorter contraction allows increased frequency of contraction without compromising time for filling
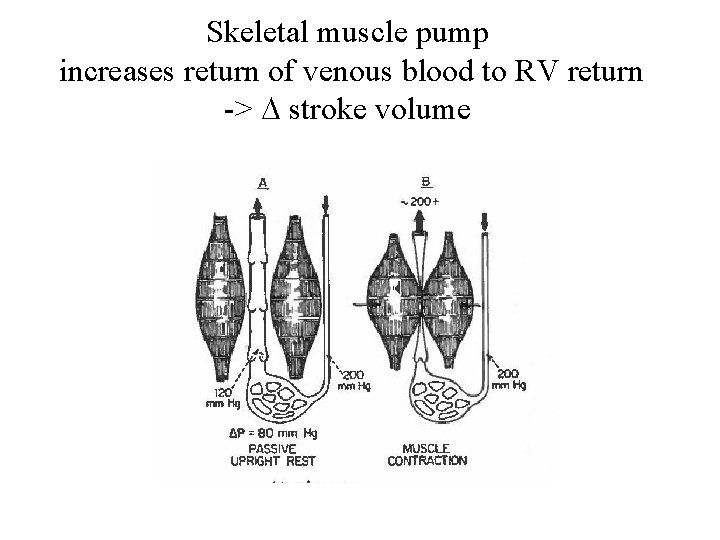
Skeletal muscle pump increases return of venous blood to RV return -> D stroke volume
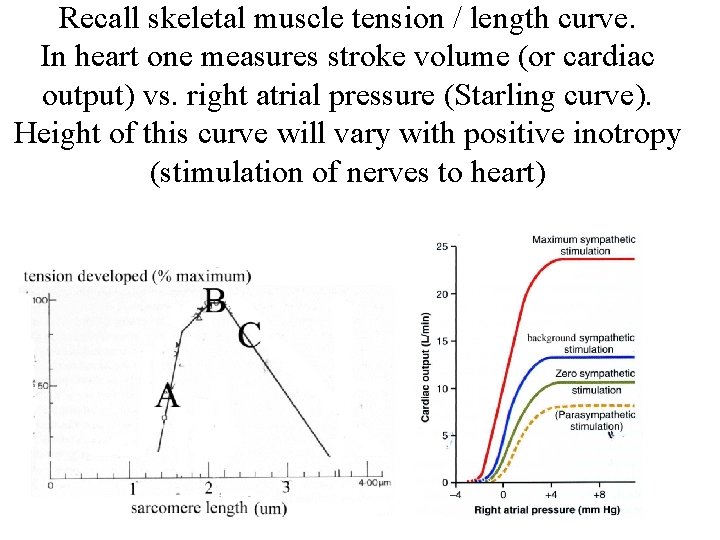
Recall skeletal muscle tension / length curve. In heart one measures stroke volume (or cardiac output) vs. right atrial pressure (Starling curve). Height of this curve will vary with positive inotropy (stimulation of nerves to heart)
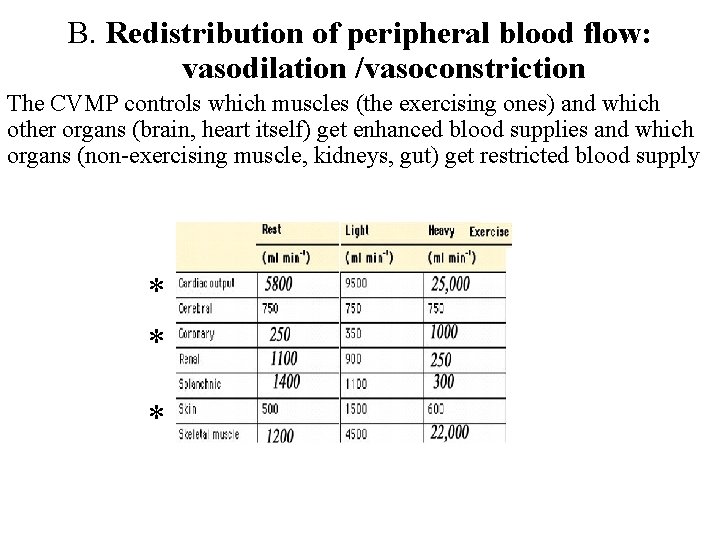

B. Redistribution of peripheral blood flow: vasodilation /vasoconstriction The CVMP controls which muscles (the exercising ones) and which other organs (brain, heart itself) get enhanced blood supplies and which organs (non-exercising muscle, kidneys, gut) get restricted blood supply * * *
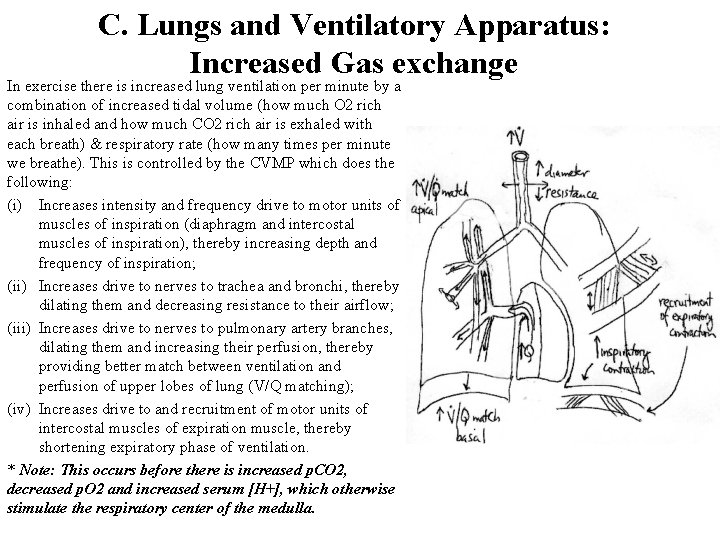
C. Lungs and Ventilatory Apparatus: Increased Gas exchange In exercise there is increased lung ventilation per minute by a combination of increased tidal volume (how much O 2 rich air is inhaled and how much CO 2 rich air is exhaled with each breath) & respiratory rate (how many times per minute we breathe). This is controlled by the CVMP which does the following: (i) Increases intensity and frequency drive to motor units of muscles of inspiration (diaphragm and intercostal muscles of inspiration), thereby increasing depth and frequency of inspiration; (ii) Increases drive to nerves to trachea and bronchi, thereby dilating them and decreasing resistance to their airflow; (iii) Increases drive to nerves to pulmonary artery branches, dilating them and increasing their perfusion, thereby providing better match between ventilation and perfusion of upper lobes of lung (V/Q matching); (iv) Increases drive to and recruitment of motor units of intercostal muscles of expiration muscle, thereby shortening expiratory phase of ventilation. * Note: This occurs before there is increased p. CO 2, decreased p. O 2 and increased serum [H+], which otherwise stimulate the respiratory center of the medulla.

D. Kidney function: stable to somewhat reduced With mild exercise, kidney filtration function remains stable even at somewhat lower blood flow to it (autoregulation). With intense exercise, kidney filtration decreases (temporary sacrifice of function to insure that there is no major loss of fluid, as maximum amount of body fluid needed to support increased cardiac output). Under both conditions kidney makes a very concentrated urine so nitrogen (urea) excretion remains intact even with low urine volumes

E. Skin and Sweat Gland function: Thermoregulation and Heat Loss. a. Perfusion of skin permits exposure of warm blood to body surface. Under this condition elaboration of sweat -> evaporation, heat transfer to the environment and return of cooled venous blood to central core, thereby cooling it b. However sweating of 1 -2 l/hr. decreased extracellular fluid volume (ECFV).

F. Glucose regulation: increased glucose utilization by exercising muscles a. CMVP stimulates release of glucagon that stimulates release of glucose from glycogen stores by liver. b. Increased levels of AMP in exercising muscle -> more insertion of glucose transporters into plasma membrane -> increased glucose uptake
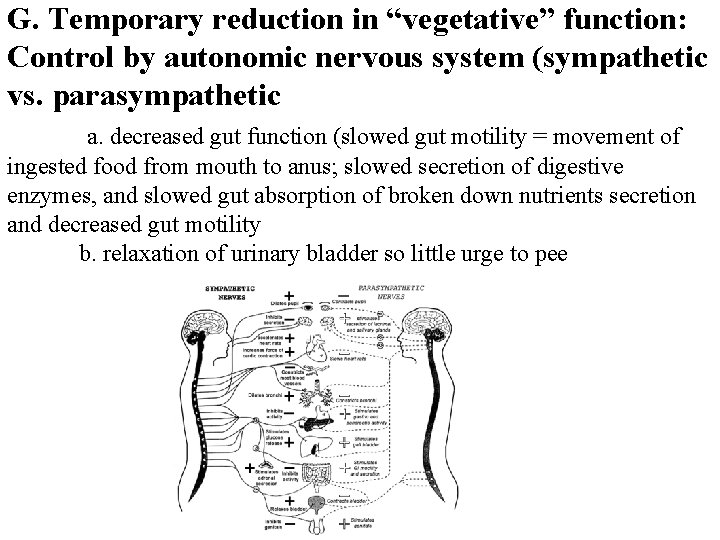
G. Temporary reduction in “vegetative” function: Control by autonomic nervous system (sympathetic vs. parasympathetic a. decreased gut function (slowed gut motility = movement of ingested food from mouth to anus; slowed secretion of digestive enzymes, and slowed gut absorption of broken down nutrients secretion and decreased gut motility b. relaxation of urinary bladder so little urge to pee

H. Hypothalamus -> higher level “stress response. ” (a) enhances cortical arousal = see and hear better (b) reduces pain = enhanced release of endorphins (c) depresses inflammation = enhanced release of ACTH (d) reduces anabolic function = decreases appetite and feeding


Lecture 3: Long Term Effects of Exercise: A. The Good (1) Optimizing function of skeletal and heart muscle (a) "remodeling hypertrophy” of muscle (1) more sarcomeres in parallel -> more tension at same length; (2) increased capillary mass adjacent to contracting muscle-> enhanced perfusion Net for heart: increases in end-diastolic volume and stroke volume, during rest and intense exercise results in the development of increased "vagal tone" (dec resting heart rate)

(b) biochemical function

(2) Training-induced changes in brain function (a) Motor learning -> increased “smoothness” of activity and decreased fall potential in elderly (1) change in the activation patterns of motor units (2) increase in the efficiency of CNS motor program (b) Exercise-induced euphoria or pain control = release of endorphins (cleavage product of ACTH) into cerebrospinal fluid bathing spinal cord and brain

(3) Exercise: Antidote to Obesity By stimulating the utilization of fat stores, exercise reduces or reverses lipotoxicity before it leads to multiorgan system diseases due to lipid accumulation in non-adipose tissue as a result of increased uptake of fat over glucose for metabolism

B. The bad of “overexercise” (1) Young female athlete’s triad in gynmasts, ballerinas and tennis players At 16 years of age BMI normal is only in 45%, and only 15% have normal bone thickness. Reduced caloric intake but twice recommended protein intake. Continuous physical stress -> disordered eating -> weight loss, amenorrhrea, osteoporosis players depressed body fat -> delayed onset or disordered hypothalmic-pituitary driven ovulatory rhythms + decreased estrogen for bone deposition

(2) Exercise-induced asthma A. Trachea and Bronchi are not just passive tubes with large air carrying lumena. 1. Goblet cells in epithelial layer make mucus to trap inhalant “junk” 2. Fluid transporting cells of epithelial layer secrete and reabsorb fluid to keep lumen moist 3. Smooth muscle layer can contract or relax to change diameter of lumen 4. Cartilage provides sturdiness to prevent tube collapse 5. Elastic layer allows lumen to be stretched larger as breath is taken in. B. Processes 1 -3 are impacted in asthma Goblet cells secrete mucus trapping particles Beating of ciliated cells moves mucus in direction of mouth from which it can be expectorated (spit out)
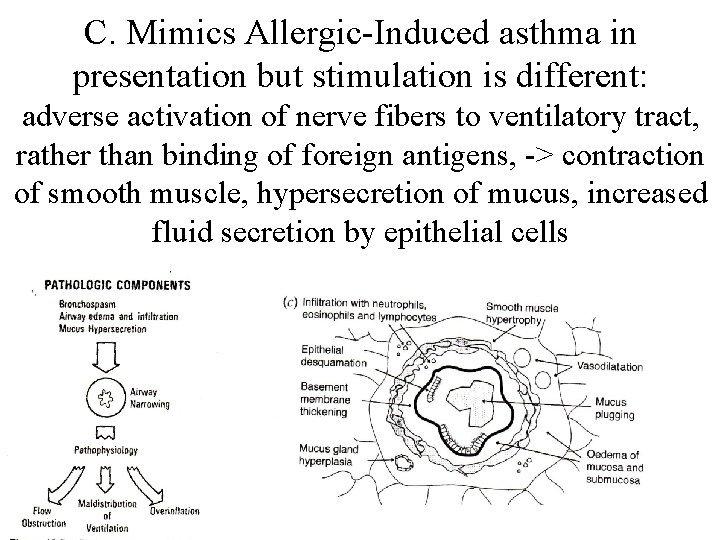
C. Mimics Allergic-Induced asthma in presentation but stimulation is different: adverse activation of nerve fibers to ventilatory tract, rather than binding of foreign antigens, -> contraction of smooth muscle, hypersecretion of mucus, increased fluid secretion by epithelial cells

(3) Overtraining and Burnout: Mild Stress Reaction fatigue muscle tenderness chronic muscle or joint pain disturbed sleep elevated resting heart rate elevated blood pressure emotional instability fatigue lack of enthusiasm regarding training and competition

C. Avoiding deleterious effects of exercise 1. Train slowly and continuously to avoid atrophy and reversion to low mitochondrial mass and low myoglobin content state 2. Don’t run in adverse locations without first training there. High altitudes-> hypoxia -> hyperventilation -> dec. exercise tolerance. Acclimatization progressive over 1 -2 months. Don’t run in smog! (CO binds to Hb and reduces O 2 carriage) 3. Be opportunistic! Pick a "springy" turf to store elastic energy in tendon; shadow a runner to dec energy spent to overcome airway resistance. 4. Pace yourself! Don’t deplete glycogen stores; early switchover from glucose to fat -> "hitting the wall” 5. Useful dietary manipulations: CHO loading; caffeine to inc early fat use and cardiac inotropy, creatine 6. Water replacement during exercise but not pre-loading 7. Pre-emptive bronchodilator Rx for cold or dust evoked asthma 8. Don’t be duped into doping (with erythropoietin or androgens) 9. Avoid overheating, exhaustion


Lecture 4: Predicting and Measuring Physiological Effects of Exercise = assessment of blood pressure, heart rate, cardiac stroke volume and output per minute , flow volume parameters of ventilation, maximum rate of O 2 consumption) Tools for measurement Sphygmomanometry Echocardiography Spirometry A-v p. O 2 difference (arterial vs. mixed venous blood)
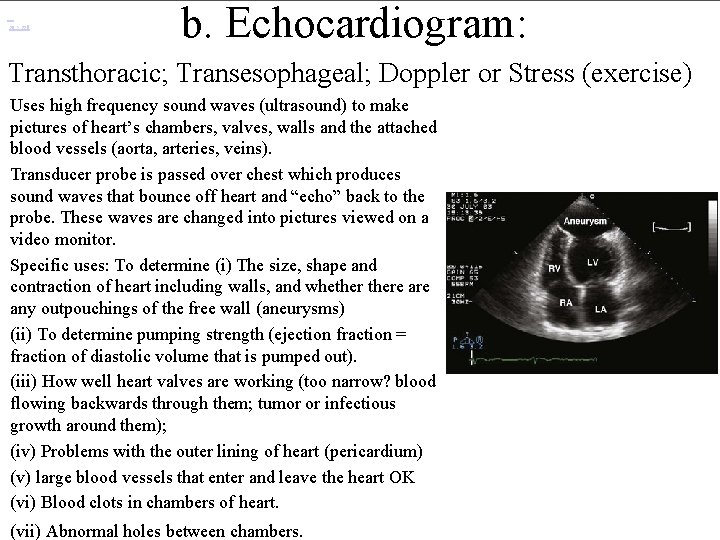
320 × 228 b. Echocardiogram: Transthoracic; Transesophageal; Doppler or Stress (exercise) Uses high frequency sound waves (ultrasound) to make pictures of heart’s chambers, valves, walls and the attached blood vessels (aorta, arteries, veins). Transducer probe is passed over chest which produces sound waves that bounce off heart and “echo” back to the probe. These waves are changed into pictures viewed on a video monitor. Specific uses: To determine (i) The size, shape and contraction of heart including walls, and whethere any outpouchings of the free wall (aneurysms) (ii) To determine pumping strength (ejection fraction = fraction of diastolic volume that is pumped out). (iii) How well heart valves are working (too narrow? blood flowing backwards through them; tumor or infectious growth around them); (iv) Problems with the outer lining of heart (pericardium) (v) large blood vessels that enter and leave the heart OK (vi) Blood clots in chambers of heart. (vii) Abnormal holes between chambers.
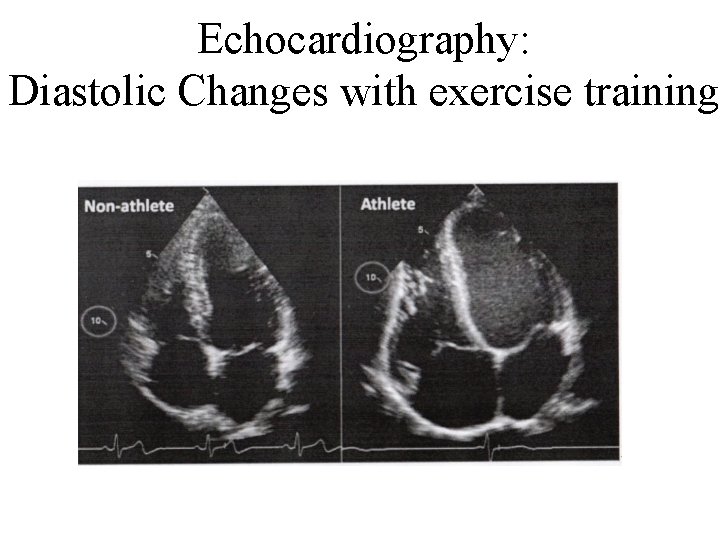
Echocardiography: Diastolic Changes with exercise training
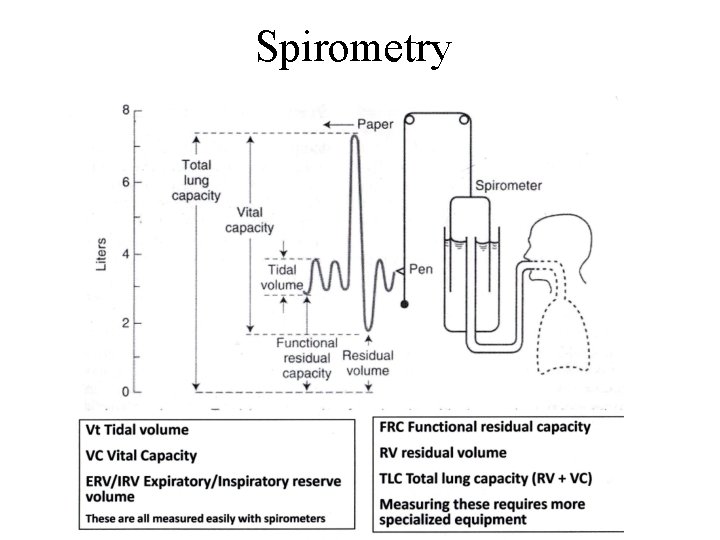
Spirometry
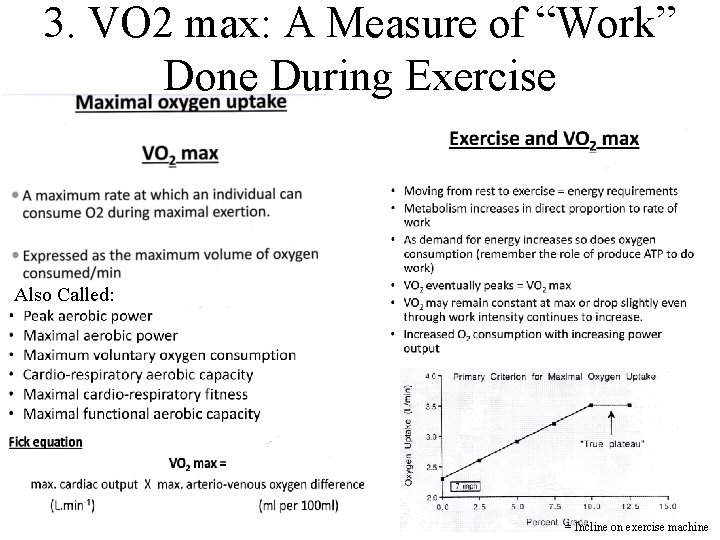
3. VO 2 max: A Measure of “Work” Done During Exercise Also Called: = Incline on exercise machine
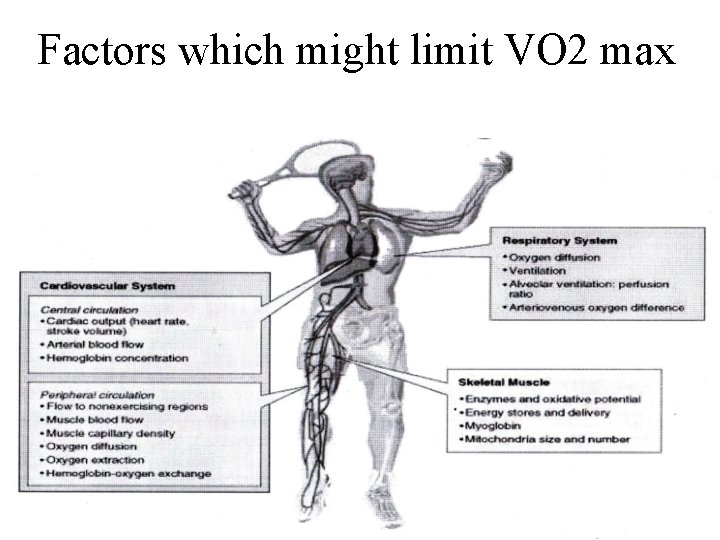
Factors which might limit VO 2 max
- Slides: 50