Exercise Therapy In Neuromuscular Disease 05102013 Maryam Tahmasbi

Exercise Therapy In Neuromuscular Disease 05/10/2013 Maryam Tahmasbi Sohi, MD Fellow in Neuromuscular Medicine Department of Neurology University of Kansas Medical Center

Objectives • Overview of different types of exercise • Physiologic responses to exercise • Review of available literature for specific neuromuscular disorders • Recommendations • Will not cover pulmonary rehabilitation

Different Types of Exercise

Flexibility Training • Involves stretching and range of motion • Reduces pain • Reduces spasticity • Increases joint blood flow and lubrication • Prevents contractures

Aerobic Exercise • • • Prolonged low-resistance Dynamic activity Large muscle groups Cardiopulmonary effects American College of Sport Medicine (ACSM) recommendation: – 30 minutes at 55%-90% of maximum heart rate or – 40 -85% of maximum oxygen uptake (VO 2 max) – 4 days a week

Aerobic Exercise-Benefits • • Improves functional exercise capacity Decreased psychological stress Improves quality of life Prevents secondary disease (DM, HTN, CAD) • Improves sleep • Helps maintain bone density if performed in a weight bearing manner • Produces greater independence with ADLs in elderly population

Maximal Aerobic Capacity (VO 2 Max) • Maximum capacity of an individual's body to transport and use oxygen during incremental exercise • Reflects the physical fitness of the individual • L/min or m. L/kg/min • Graded exercise test while measuring ventilation, O 2 and CO 2 • O 2 consumption remains unchanged despite an increase in workload
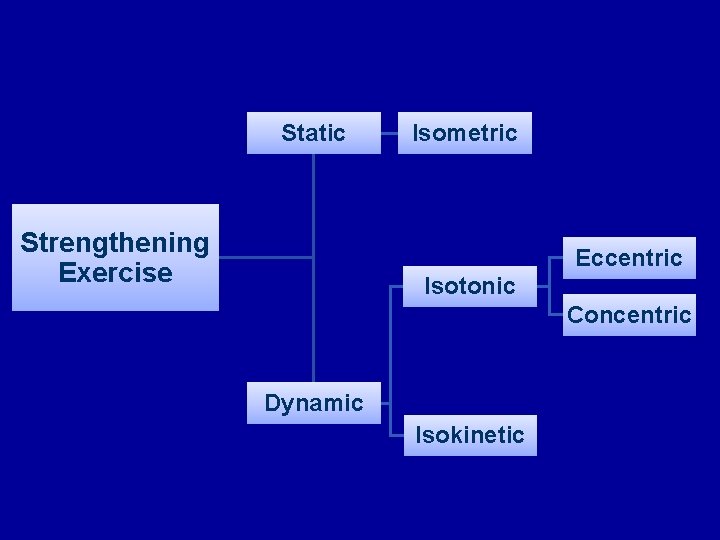
Static Strengthening Exercise Isometric Eccentric Isotonic Concentric Dynamic Isokinetic
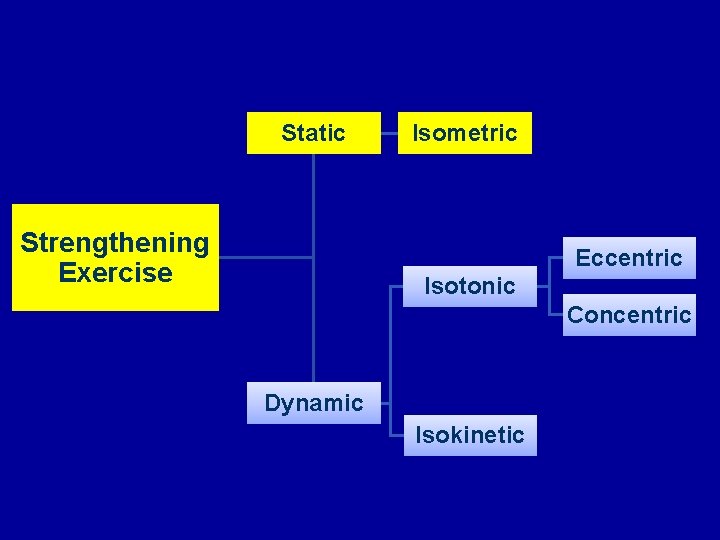
Static Strengthening Exercise Isometric Eccentric Isotonic Concentric Dynamic Isokinetic

Isometric Exercise • No change in muscle length • No visible joint movement • Primary use is for rehabilitation of joints with limited ROM due to injury or post op • Only increases strength within a limited range of motion (ROM)
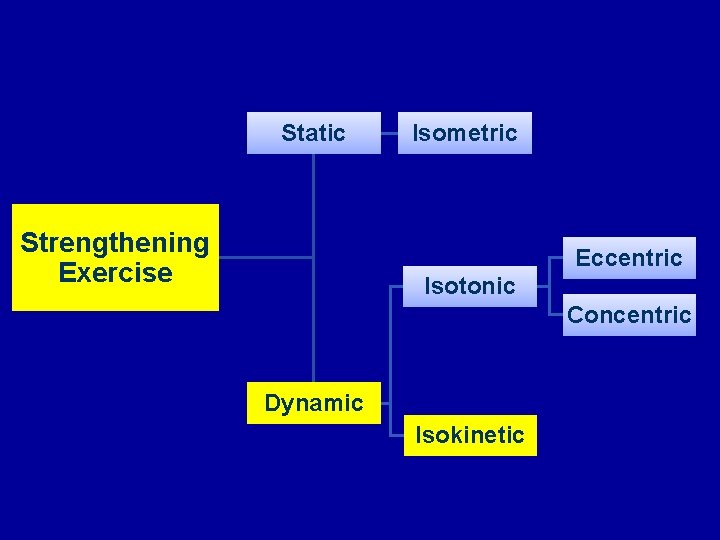
Static Strengthening Exercise Isometric Eccentric Isotonic Concentric Dynamic Isokinetic

Isokinetic Exercise • Constant speed • Variable resistance throughout the range of motion • Lower chance of injury • Athletic training for strengthening throughout the required ROM Nautilus- Upright Exercise Bike
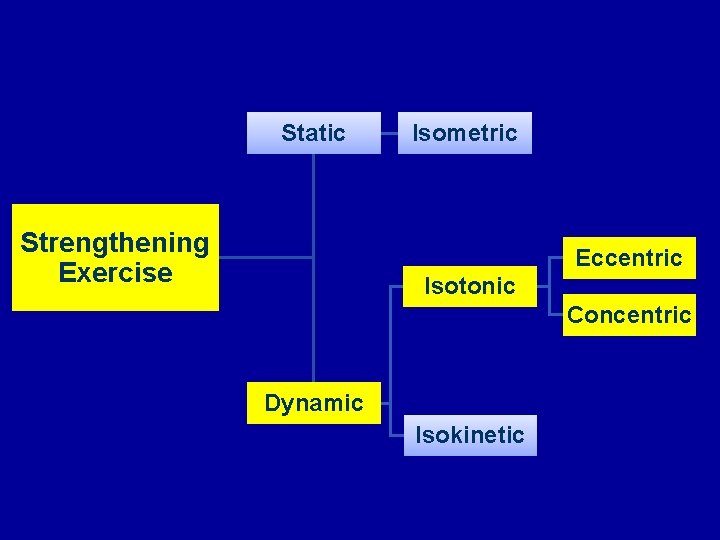
Static Strengthening Exercise Isometric Eccentric Isotonic Concentric Dynamic Isokinetic
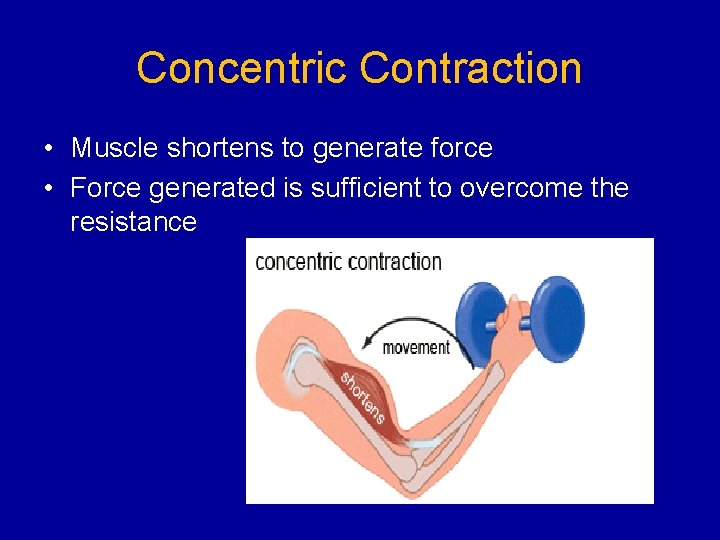
Concentric Contraction • Muscle shortens to generate force • Force generated is sufficient to overcome the resistance

Eccentric Contraction • Muscle fibers lengthen • Force generated is insufficient to overcome the external load on the muscle • Mean of decelerating a body part or object, or lowering a load gently rather than letting it drop • Negative training
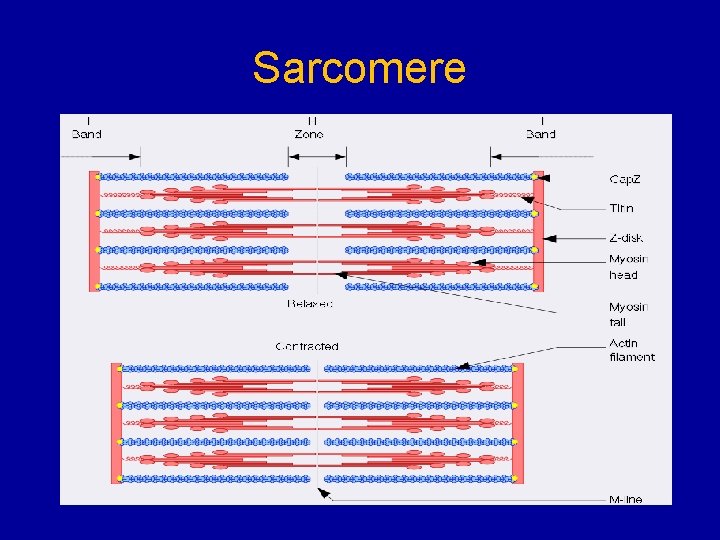
Sarcomere

Delayed-Onset Muscle Soreness (DOMS) • Muscular discomfort and pain • 24± 48 h after strenuous exercise • Proximal and distal muscle tendon junctions spreading throughout the entire muscle • Directly associated with the eccentric exercise (Asmussen 1952, 1956) • Objective findings: – Strength loss – Reduced range of motion – Elevated serum creatine kinase (CK)

DOMS • Z disk is the most vulnerable structure • Type II fiber- biased damage (Lieber & Fride n 1988) • Loss of desmin, inflammatory changes and necrosis in animals • Older men are not as susceptible (Lavender and Nosaka; 2006)

Physiologic Response to Exercise • Neural adaptation: – Accounts for early strength gain with training programs (2 weeks) – Increase in muscle strength without noticeable hypertrophy • Muscular Adaptation: – 6 -8 weeks to develop – Increase in muscle cross-sectional area (muscle hypertrophy) in response to resistive exercise – Fast twitch (type II) fibers more than type I

Cross-transference • Strength gain in the opposite, untrained limb following unilateral resistance training • Due to neural adaptation • Improves the strength of a unmovable injured limb or during post surgical period • Implication in research: – Cannot use the opposite limb as control – 7. 8 -10% improvement in strength of the untrained limb (Meta-analysis study)
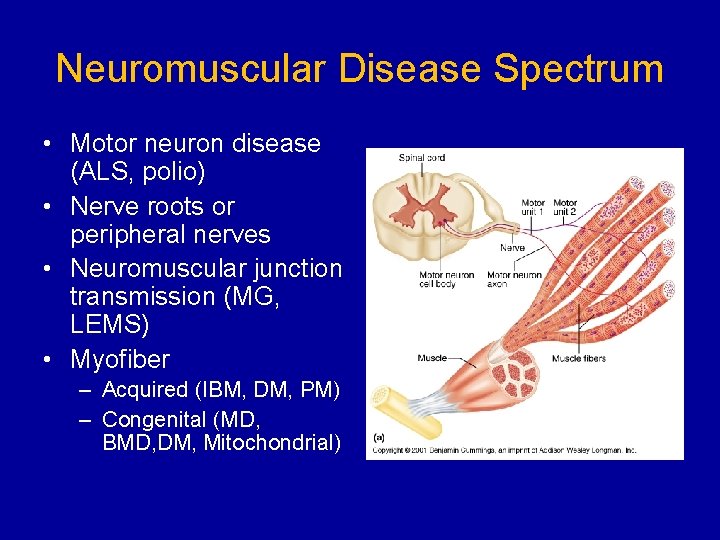
Neuromuscular Disease Spectrum • Motor neuron disease (ALS, polio) • Nerve roots or peripheral nerves • Neuromuscular junction transmission (MG, LEMS) • Myofiber – Acquired (IBM, DM, PM) – Congenital (MD, BMD, DM, Mitochondrial)

Questions to answer Safe? Beneficial?

Studies in NMDs • Limited number of studies • Methodological limitations – Lack of good controlled studies due to the rarity of NMDs – Grouped subjects with different NMDs with different disease type, severity, and rate of progression – Little uniformity regarding the type of exercise interventions (aerobic, strengthening, or combinations of exercise regimens), duration of exercise, intensity of exercise therapy, and initial state of physical activity and fitness – Lack of clearly identified primary and secondary outcome measures • Strength, endurance, fatigue, cardiopulmonary function, functional ability, activities of daily living, anxiety, depression, wellbeing, and pain

Muscular Dystrophies • Heterogeneous group of hereditary muscle diseases • Progressive muscle weakness • Muscle fiber damage, inflammation, necrosis, and regeneration • Defects in sarcolemmal and extracellular matrix proteins, essential in maintaining the cytoskeletal framework of the muscle fiber during muscle contraction
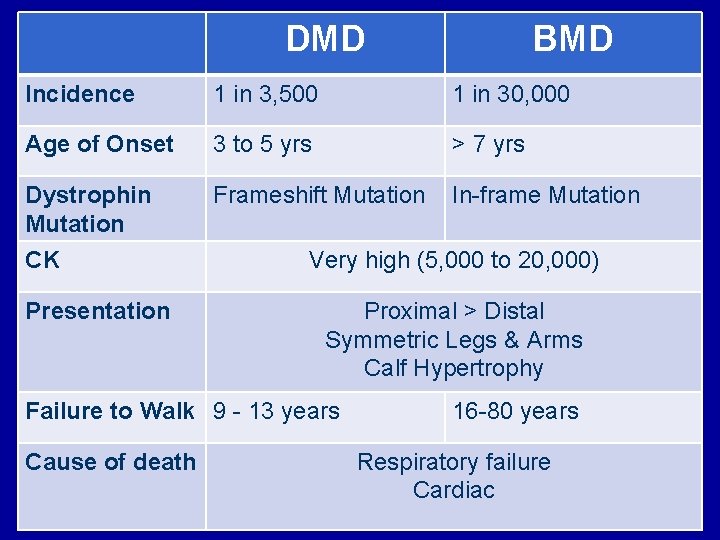
DMD BMD Incidence 1 in 3, 500 1 in 30, 000 Age of Onset 3 to 5 yrs > 7 yrs Dystrophin Mutation Frameshift Mutation In-frame Mutation CK Presentation Very high (5, 000 to 20, 000) Proximal > Distal Symmetric Legs & Arms Calf Hypertrophy Failure to Walk 9 - 13 years Cause of death 16 -80 years Respiratory failure Cardiac

Strengthening Exercise • Studies in dystrophin-deficient mdx mice have shown that dystrophic muscle is more susceptible to contraction-induced muscle damage compared to healthy mice • Available randomized control trials are small in size, with inconsistent methodologies and conflicting results • General consensus is that high resistance strengthening exercises are contraindicated in patients with dystrophinopathy
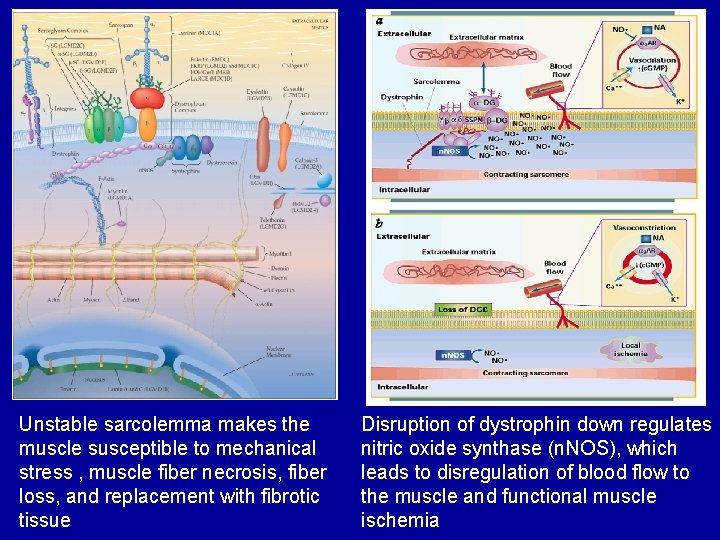
Unstable sarcolemma makes the muscle susceptible to mechanical stress , muscle fiber necrosis, fiber loss, and replacement with fibrotic tissue Disruption of dystrophin down regulates nitric oxide synthase (n. NOS), which leads to disregulation of blood flow to the muscle and functional muscle ischemia

Tadalafil-Muscle Ischemia-BMD “Tadalafil Alleviates Muscle Ischemia in Patients With Becker Muscular Dystrophy” • Randomized placebo-controlled crossover trial • Tadalafil (phosphodiesterase 5 A inhibitor) • Functional muscle ischemia is alleviated and normal blood flow regulation is fully restored in the muscles of men with BMD • There were no adverse events or side effects Martin et al 2012

Endurance Training and BMD Method: • Eleven patients with BMD and seven healthy subjects • All patients were ambulant • Onset of symptoms at age 8 ± 2 years • Asymptomatic cardiomyopathy (LVEF): 35– 45% in 3 patients • Forced vital capacity (FVC) was on average decreased by 14± 2% (within normal limits) Primary Outcomes: VO 2 max, Plasma Ck, and self report questionnaire Intervention: Cycled 50, 30 min sessions at 65% of their VO 2 max over 12 weeks, and six patients continued cycling for 1 year Sveen et al 2008

Endurance Training and BMD Results: – Improved VO 2 max by 47± 11% in patients (P 0. 005) – Weekly CK levels did not increase with training – No change in the number of central nuclei, necrotic and regenerating fibers – Strength in muscles involved in cycle exercise (knee extension, and dorsi- and plantar-flexion) increased significantly by 13 -40%. – Cardiac pump function, measured by echocardiography, did not change with training – All improvements and safety markers were maintained after 1 year of training Conclusion: – Moderate endurance training is safe to increase exercise performance and daily function in patients with BMD Sveen et al 2008

High Intensity Endurance Training “Creatine kinase response to high-intensity aerobic exercise in adult-onset muscular dystrophy” Method: • Fourteen patients with muscular dystrophy (BMD: 5, FSHD: 5 , LGMD 2 -I and LGMD 2 -A: 4 ) • Eight healthy subjects • 5 cycling tests at 65, 75, 85 and 95 % of VO 2 max • Heart rate and oxygen consumption were measured during tests • Plasma CK was measured before, immediately after, and 24 hours after exercise Anderson et al 2013

High Intensity Endurance Training Results: • Plasma CK increased after all exercise tests in all patients • In persons affected by LGMD 2 A, LGMD 2 I, and FSHD, plasma CK declined to the pre-exercise level 24 hours after exercise • Plasma CK remained elevated 24 hours after exercise in persons with BMD (only after the 95% of VO 2 max test) • The subjects never scored higher than 3. 5 on the leg pain VAS (immediately after exercise) Anderson et al 2013

High Intensity Endurance Training Conclusion: • High-intensity aerobic exercise is generally well-tolerated in persons with LGMD 2 and FSHD • Patients with BMD may be more prone to exercise induced damage • Closer supervision of training is warranted if high-intensity exercise is implemented Anderson et al 2013

Idiopathic Inflammatory Myopathies (IIM) • Heterogeneous group of rare disorders that present with acute, subacute, or chronic muscle weakness • Overlapping clinical manifestations • Divergent from the histopathological and pathogenetic standpoints • Generally respond well to immunosuppressive therapy • Inclusion body myositis (IBM), the most common IIM in the elderly, is clinically, histopathologically and pathogenetically distinct • IBM is refractory to all currently available therapies

Exercise and IIM • Studies in active and chronic disease phase have been reported • All demonstrated the safety and efficacy of exercise • Neuromuscular specialists usually wait for the first two to three months for strength and CK to start responding to pharmacotherapy before starting the strengthening exercise program • Early mobilization is important to prevent flexion contractures Dimachkie 2011

Exercise and IBM (Arnardottir et al, 2003): • A home exercise program, five days a week for 12 weeks, was found to be safe in seven patients. There was no strength deterioration, no change in serum CK, and no increased in muscle inflammation on biopsy (Johnson et al. , 2009): • Aerobic exercise program using a stationary cycle ergometer at 80% of the initial maximum heart rate (for two minutes less than the total time achieved during maximal aerobic test) combined with resistance isometric and isotonic exercises of the upper and lower limbs in a group of seven IBM cases. Besides demonstrating it to be safe, they found this exercise routine to improve aerobic capacity and muscle strength. Dimachkie 2011

Mitochondrial Myopathy • • Heterogeneous group of metabolic muscle disorders Mutation in either nuclear or mitochondrial DNA (mt. DNA) Brain and skeletal muscles are particularly susceptible Single-organ to multisystem disorders (muscle weakness or exercise intolerance, arrhythmia, dementia, movement disorders, stroke-like episodes, deafness, blindness, ophthalmoplegia, and seizures) • Heteroplasty: mt. DNA mutations coexist with wild-type mt. DNA (Mild phenotypes have higher proportions of wildtype mt. DNA) • Mature muscle cells have a high degree of mt. DNA mutations, whereas the level of mutations is low or undetectable in satellite cells

Exercise in MT-Myopathy • Resistance exercise serves as stimulus for satellite-cell induction within skeletal muscle, lowering the level of mutant mt. DNA and improving oxidative capacity (Murphy et al 2008) • The beneficial effects of endurance training have been reported in 8 published reports, with no adverse effects • Hypothesized to induce mitochondrial biogenesis and capacity for oxidative phosphorylation improve function

Amyotrophic Lateral Sclerosis (ALS) • Progressive degenerative disease of the upper and lower motor neuron • Majority of cases are sporadic (90%) • Hereditary defect in the superoxide dismutase (SOD) gene (20%) • Studies of exercise on SOD deficient mice suggest that endurance exercise training at moderate intensities slows disease progression, and increases lifespan • High-intensity exercise showed no improvement or hastened symptoms and death

Exercise and ALS • Twenty-five patients were randomized to receive a moderate daily exercise program (n=14) or control (n=11) • Outcome measures at baseline and after 3, 6, 9 and 12 months – – – Manual muscle strength testing Ashworth spasticity scale ALS functional rating scale (ALSFRS) Visual analog scale for pain Quality-of-life scale (SF-36) Drory et al 2001

Exercise and ALS • At 3 months, patients who performed regular exercise showed less deterioration on FRS and Ashworth scales, but not on other parameters • At 6 months, there was no significant difference between groups, although a trend towards less deterioration in the treated group on most scales was observed • At 9 and 12 months, there were too few patients in each group for statistical evaluation

Exercise and ALS Method: 27 patients with a diagnosis of ALS, FVCof ≥ 90% predicted, and ALS Functional Rating Scale (ALSFRS) score of 30 or greater were randomly assigned to a resistance exercise group (n=13) or to a usual care group (n=14) Results: - Eight resistance exercise subjects and 10 usual care subjects completed the trial - At 6 months, the resistance exercise group had significantly higher ALSFRS and SF-36 scores - No adverse events - Less decline in leg strength measured by MVIC Bello- Haas et al 2007

Post Polio Syndrome • Affects individuals who had a confirmed case of polio with a partial or fairly complete neurological and functional recovery after the acute episode • At least 15 years of neurological and functional stability • Presenting with gradual or abrupt onset of new muscle weakness, muscle atrophy, muscle pain, and fatigue • Persists for more than 1 year

Exercise in PPS • European Federation of Neurological Society (ENFS) task force determined that both aerobic training and progressive resistance exercise training can benefit individuals with PPS (2006) • Systematic analysis by Cup et al in 2008 determined that there is insufficient evidence to assess the effectiveness of muscle strengthening exercises, aerobic exercises, or a combination of these exercises in individuals with PPS Abresch et al 2009
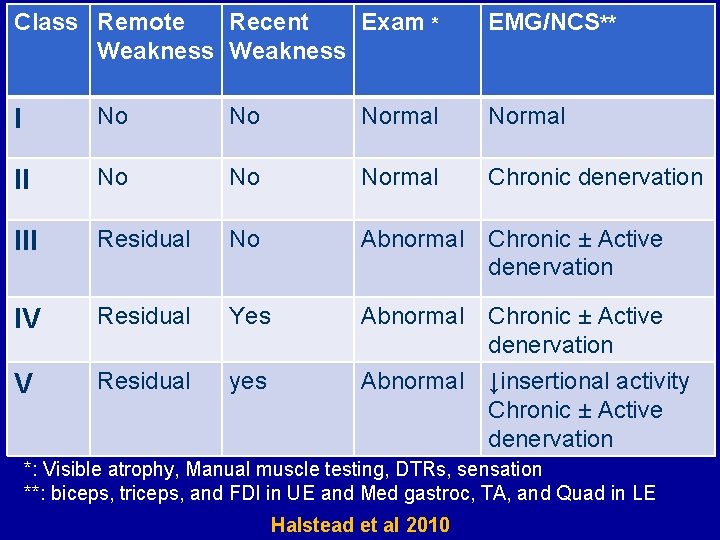
Class Remote Recent Exam * Weakness EMG/NCS** I No No Normal II No Normal Chronic denervation III Residual No Abnormal Chronic ± Active denervation IV Residual Yes V Residual yes Abnormal Chronic ± Active denervation Abnormal ↓insertional activity Chronic ± Active denervation *: Visible atrophy, Manual muscle testing, DTRs, sensation **: biceps, triceps, and FDI in UE and Med gastroc, TA, and Quad in LE Halstead et al 2010
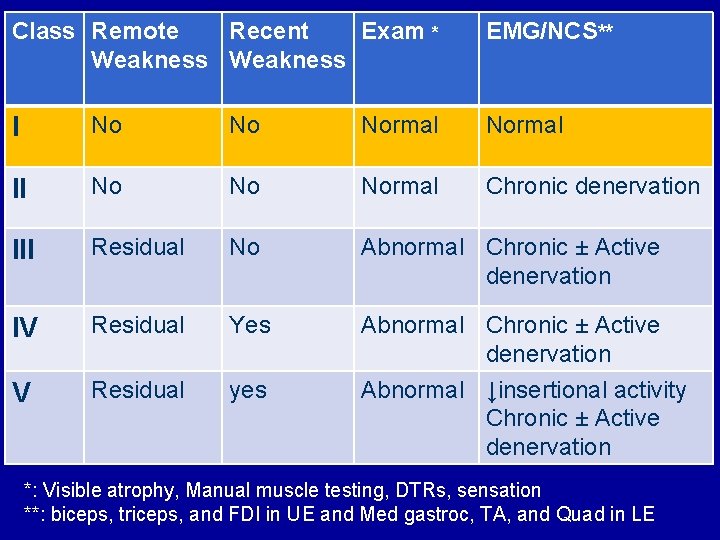
Class Remote Recent Exam * Weakness EMG/NCS** I No No Normal II No Normal Chronic denervation III Residual No Abnormal Chronic ± Active denervation IV Residual Yes V Residual yes Abnormal Chronic ± Active denervation Abnormal ↓insertional activity Chronic ± Active denervation *: Visible atrophy, Manual muscle testing, DTRs, sensation **: biceps, triceps, and FDI in UE and Med gastroc, TA, and Quad in LE

Proposed Exercise in PPS • Class 1: – Moderate intensity: 60 -80% maximal HR – Duration: 15 -30 min – Frequency: 3 -5/week Examples: • Swimming 25 -35 yards/min • Walking 5 -6 mph • Bicycle riding 12 -14 mph Halstead et al 2010
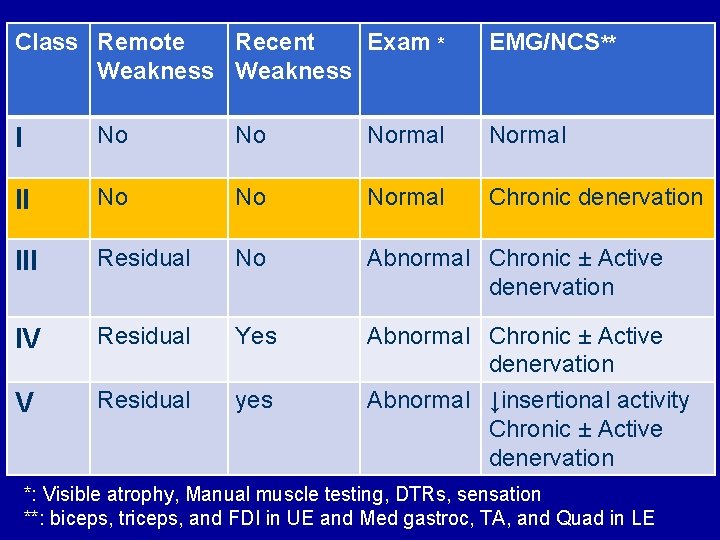
Class Remote Recent Exam * Weakness EMG/NCS** I No No Normal II No Normal Chronic denervation III Residual No Abnormal Chronic ± Active denervation IV Residual Yes V Residual yes Abnormal Chronic ± Active denervation Abnormal ↓insertional activity Chronic ± Active denervation *: Visible atrophy, Manual muscle testing, DTRs, sensation **: biceps, triceps, and FDI in UE and Med gastroc, TA, and Quad in LE

Proposed Exercise in PPS • Class II: – Moderate intensity: 60 -80% maximal HR – Duration: 15 -30 min – Frequency: 3 -4/week on alternate days – Pacing: perform 4 -5 min, rest 1 min *Decrease if pain, fatigue or new weakness Halstead et al 2010
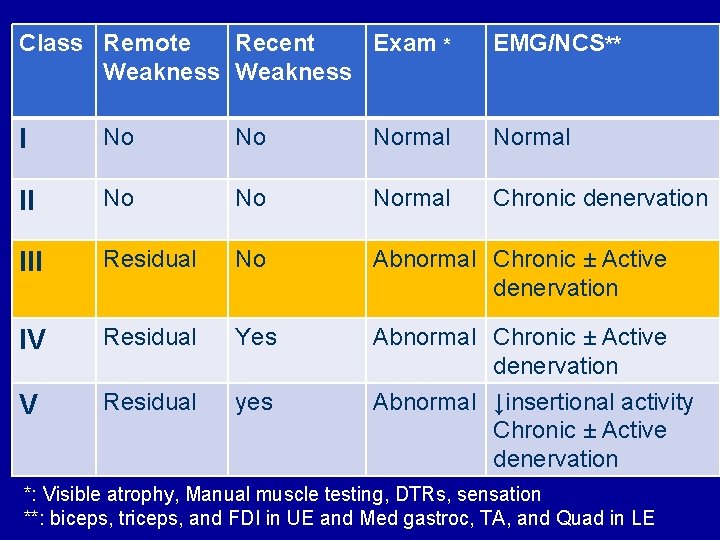
Class Remote Recent Exam * Weakness EMG/NCS** I No No Normal II No Normal Chronic denervation III Residual No Abnormal Chronic ± Active denervation IV Residual Yes V Residual yes Abnormal Chronic ± Active denervation Abnormal ↓insertional activity Chronic ± Active denervation *: Visible atrophy, Manual muscle testing, DTRs, sensation **: biceps, triceps, and FDI in UE and Med gastroc, TA, and Quad in LE

Proposed Exercise in PPS • Class III: – Low intensity: 40 -60% of max HR – Duration: 15 -20 min – Frequency: 3 -4/week – Pacing: Resting 1 min/2 -3 min of activity *modify if new weakness, pain or fatigue Halstead et al 2010
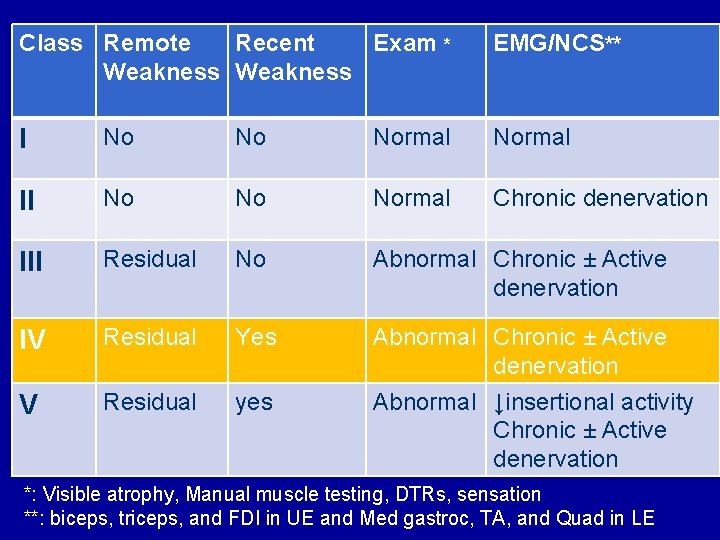
Class Remote Recent Exam * Weakness EMG/NCS** I No No Normal II No Normal Chronic denervation III Residual No Abnormal Chronic ± Active denervation IV Residual Yes V Residual yes Abnormal Chronic ± Active denervation Abnormal ↓insertional activity Chronic ± Active denervation *: Visible atrophy, Manual muscle testing, DTRs, sensation **: biceps, triceps, and FDI in UE and Med gastroc, TA, and Quad in LE

Proposed Exercise in PPS • Class IV: – Trial of rest to exclude overuse weakness – Daily active/passive stretching program – No cardiopulmonary aerobic exercise – If overuse is excluded, trial of monitored, non- fatiguing, progressive resistive exercise program – If overuse weakness, modify activity, use bracing, scooter, etc. Halstead et al 2010
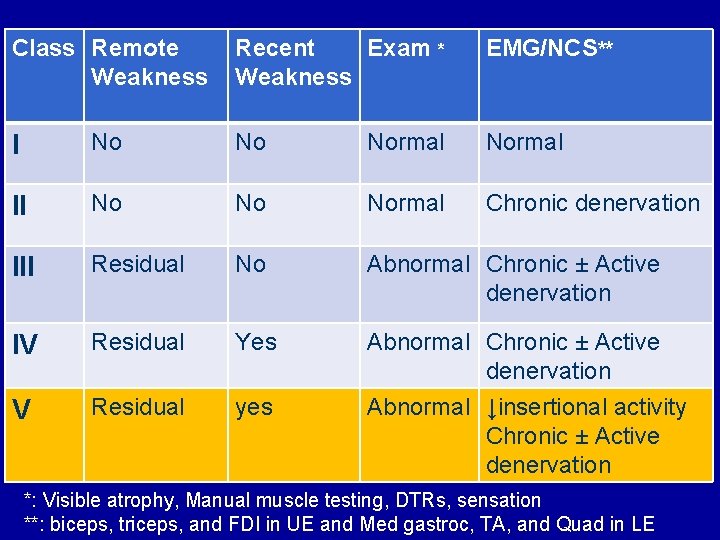
Class Remote Weakness Recent Exam * Weakness EMG/NCS** I No No Normal II No Normal Chronic denervation III Residual No Abnormal Chronic ± Active denervation IV Residual Yes V Residual yes Abnormal Chronic ± Active denervation Abnormal ↓insertional activity Chronic ± Active denervation *: Visible atrophy, Manual muscle testing, DTRs, sensation **: biceps, triceps, and FDI in UE and Med gastroc, TA, and Quad in LE

Proposed Exercise in PPS • Class V: – Performing activities of daily living – Bracing and/or wheelchair usually needed Halstead et al 2010

Diabetic Neuropathy • Pilot study • Seventeen subjects (8 males/9 females; age 58. 4± 5. 98; duration of diabetes 12. 4± 12. 2 years) • 10 - week supervised, moderately intense aerobic and resistance exercise program • Outcome measures: – Pain (visual analog scale) – Michigan Neuropathy Screening Instrument (MNSI) – Intraepidermal nerve fiber (IENF) density and branching RESULTS: • Significant reductions in pain, neuropathic symptoms, and increased intraepidermal nerve fiber branching from a proximal skin biopsy Pasnoor et al 2012

Conclusion 1. Individuals with NMDs should adopt an active lifestyle for its physical and psychological benefits 2. Stretching and range-of-motion exercises may be helpful in decreasing the discomfort due to the limited joint mobility 3. Moderate resistance exercise should be given to patients with antigravity strength or better to maintain strength Abresch et al 2012

Conclusion 4. Moderate aerobic exercise should be given to prevent deconditioning and loss of cardiopulmonary fitness 5. High-intensity exercises relative to an individual’s strength should be avoided 6. The intensity and frequency of exercise should be tailored to individual's level of physical fitness and need 7. The effects of exercise should be closely monitored Abresch et al 2012

What to Tell Patients? • • • Moderate: 40 -60% VO 2 Max or 60%of maximum HR Walking as fast as 100 steps per minute Breathing quickens, but not out of breath Develop a light sweat after about 10 minutes of activity • Can carry on a conversation, but you can't sing

What to Tell Patients? Vigorous exercise intensity • Breathing is deep and rapid • Develop a sweat after a few minutes of activity • Cannot say more than a few words without pausing for breath

References • Alexanderson H, Lundberg IE. The role of exercise in the rehabilitation of idiopathic inflammatory myopathies. Curr Opin Rheumatol 2005; 17: 164 -71. • Arnardottir, S. , Alexanderson, H. , Lundberg, I. E. , Borg, K. , 2003. Sporadic inclusion bodymyositis: pilot study on the effects of a home exercise program on muscle function, histopathology and inflammatory reaction. J. Rehabil. Med. 35 (1), 31– 35. • Cup EH, Pieterse AJ, Knuijt S, et al. Referral of patients with neuromuscular disease to occupational therapy, physical therapy and speech therapy: usual practice versus multidisciplinary advice. Disabil Rehabil 2007; 29: 717 -26. • Dimachkie MM. J Neuroimmunol. 2011 Feb; 231(1 -2): 32 -42. doi: 10. 1016/j. jneuroim. 2010. 013. Epub 2010 Nov 18. Review. • Drory VE, Goltsman E, Reznik JG, Mosek A, Korczyn AD. The value of muscle exercise in patients with amyotrophic lateral sclerosis. J Neurol Sci 2001; 191: 133 -7. • Fride n, J. & Lieber, R. L. 1998. Segmental muscle ®ber lesionsafter repetitive eccentric contractions. Cell Tissue Res 293, 165± 171

References • Haller RG, Wyrick P, Taivassalo T, Vissing J. Aerobic conditioning: an effective therapy in Mc. Ardle’s disease. Ann Neurol 2006; 59: 9228. • HALSTEADL, . S. 1991. Assessment and differential diagnosis for post-polio syndrome. Orthopedics 14(11): 1209 -12 17. • Hartling L, Mc. Alister FA, Rowe BH, Ezekowitz J, Friesen C, Klassen TP. Challenges in systematic reviews of therapeutic devices and procedures. Ann Intern Med 2005; 142: 1100 -11. • Johnson, L. G. , Collier, K. E. , Edwards, D. J. , Philippe, D. L. , Eastwood, P. R. , Walters, S. E. , Thickbroom, G. W. , Mastaglia, F. L. , 2009. Improvement in aerobic capacity after an exercise program in sporadic inclusion body myositis. J. Clin. Neuromuscul. Dis. 10 (4), 178– 184. • Martin EA, Barresi R, Byrne BJ, Tsimerinov EI, Scott BL, Walker AE, Gurudevan SV, Anene F, Elashoff RM, Thomas GD, Victor RG. Sci Transl Med. 2012 Nov 28; 4(162): 162 ra 155.

References • • Neuromuscular Disorders, treatment and management, Tulio E. Bertonrini, 115 -136. Olsen DB, Orngreen MC, Vissing J. Aerobic training improves exercise performance in facioscapulohumeral muscular dystrophy. Neurology 2005; 64: 1064 -6. Taivassalo T, Haller RG. Exercise and training in mitochondrial myopathies. Med Sci Sports Exerc 2005; 37: 2094 -101. Van der Kooi EL, Lindeman E, Riphagen I. Strength training and aerobic exercise training for muscle disease. Cochrane Database Syst Re 2005; (1): CD 003907 Van Tulder MW, Assendelft WJ, Koes BW, Bouter LM. Method guidelines for systematic reviews in the Cochrane Collaboration Back Review Group for Spinal Disorders. Spine 1997; 22: 2323 - 30. Taivassalo T, De Stefano N, Argov Z, et al. Effects of aerobic training in patients with mitochondrial myopathies. Neurology 1998; 50: 1055 -60. Taivassalo T, De Stefano N, Chen J, Karpati G, Arnold DL, Argov Z. Short-term aerobic training response in chronic myopathies. Muscle Nerve 1999; 22: 1239 -43. Mc. Donald CM, Abresch RT, Carter GT, et al. Profiles of neuromuscular diseases: Duchenne muscular dystrophy. Am J Phys Med Rehabil. 1995; 74: S 70–S 92.

Thank You
- Slides: 64