Examples of Diabetes Research Projects Diabetes Supercourse Alexandria

Examples of Diabetes Research Projects Diabetes Supercourse, Alexandria 11 Jan 2009

How Turkish and Arabic Speaking Communities (TASC) View Diabetes and Pre diabetes? A qualitative Study Nabil Sulaiman, Doris Young, John Furler, Elaine Hadj, Helen Corbett Medical Research Grants Restricted Purposes funds

Diabetes Australia Facts 2008 Type 2 Diabetes (T 2 DM) in CALD populations: 1. 2. 3. 4. Prevalence of diabetes Prevalence of risk factors Complications Hospitalisations due to nontreatable diabetes 5. Death rates due to diabetes

DM in M. E born Vs. Australian born • highest SRR for self-reported DM • ~ twice the rate (79. 8 vs 46. 2/1000) of DM • highest hospitalisations rate, and • 2 nd highest MRR from DM AIHW Cat. No. AUS 38. Canberra, 2003.

Diabetes & CVD in Hume n DALYs for diabetes in Hume is the highest in Victoria (6. 8 vs. 4. 1 per 1, 000 female) (6. 6 vs. 4. 5 per 100, 000 males) n DALYs for cardiovascular disease is the second highest in Victoria (31. 9 vs. 27. 6 per 1, 000 females) (35. 4 vs. 32. 2 per 1, 000 males)

Diabetes in Arabs & Turks n M. E. born highest age-standardised: – – – n Prevalence ratio in M (3. 60) and F (2. 43) Incidence ratios M(1. 73) F(2. 30) Hospitalisations ratios M(2. 07) F(1. 52) Death rates higher in Arabic speaking residents in NSW (25. 4 vs 13. 4 per 100, 000)

Diabetes in Arabs & Turks n >40% Arab American have dysglycemia: – 18% diagnosed or undiagnosed diabetes – 23% impaired fasting glucose or impaired glucose tolerance n 12. 3% in Turks living in Holland vs 3% in ethnic Dutch n 35% in Bahrain, 13% in Turkey

Risk Factors: Hume Household Survey (PHP 1999) n n 76% were physically inactive compared with 43% average for Victoria 62% had weight problems 39% had high cholesterol 49% smoked

What could be done? n 57% reduction of T 2 D by modifying physical activity and dietary change (Lindstrom et al, 2003 and Knowles et al, 2003) n Uptake of such lifestyle changes in lower SES & CALD groups has been poor n >50% of people born in M. E. countries did not undertake physical exercise compared with 34% of Australian-born

Meta-analysis of 11 trials in CALD 1. 2. 3. 4. 5. Improved Hb. A 1 c after intervention at 3 M Weight Mean Difference -0. 3% at 3 M and 0. 6% at 6 M Knowledge scores improved at 3 M Healthy life style improvement at 3 M No difference in secondary outcomes: lipid levels, qo. L, selfefficacy, BP

Aims § Explore insight, perception, attitudes and practices of TASC, in relation to physical activity (PA), diet and obesity § The feasibility of peer led model of engaging the community in diabetes prevention

Methods n Focus Groups In depth interviews with key informants (bilingual GPs, diabetes educators, practice nurses, dieticians, physios etc. n Develop culturally sensitive resources for TASC in Turkish and Arabic languages. n

Focus Groups - recruitment n Who? – Over the age of 45 years – Speaks Arabic or Turkish language – Family history of diabetes – Overweight – Don’t do exercise regularly n How? – BHS bilingual staff – Adult Day Activity Centre – Community Centre- Blair Street – Families and Friends

Participants n n n n n Three FG with Turkish speaking Two FG with Arabic speaking Mean age= 58. 8 (range 41 y – 73 y) F: M = 41 : 11 All living in and around Hume Interpreters from TIS Facilitators: Elaine Hadj and NS Transcribed by Sue Foley Analysis and cross analysis (NS& Helen)

Focus Group Themes What does the word ‘diabetes’ mean to you? n ? causes diabetes n ? factors associated with diabetes n ? factors increase risk of diabetes n ? diabetes and diet? n ? diabetes and overweight/ obesity n ? role of exercise in diabetes n

Focus Group Themes Is adult diabetes preventable? How can you prevent diabetes? n ? type of exercise is appropriate for your community/ yourself? How often do you/your community exercise n ? motivate you/ your community to do exercise n ? types of diet do you/your family/ community prefer? n ? diabetes and body weight n

Findings: what diabetes meant to you? n Acknowledgement of the severity: “it’s a bad disease which is second to cancer”, n Physical and psychological well being: “All of my ancestors, they have Diabetes, this why I said it is horrible disease, and some of them they had amputations of their limbs. Three of them their hands or their legs they were amputated, but one of them refused to do such a thing …. ”.

What diabetes meant to you? n Specific: – “It means stress” or “It means a lot of food that you can’t eat”. – “When the pancreas is not working so well it is not producing Insulin for the body to maintain the sugar levels and the amount of sugar in the blood goes quite high …”.

What do you associate with Diabetes? n n It affects the eyes swelling and ulceration of the legs (“The legs get swollen and sometimes blood will come out and it doesn’t heal”). n n n Cuts don’t heal Increased thirst and urination Poor dietary habits or eating the wrong food, limitations on food choices Stress (“Stress is one of the main things that causes illnesses”) Lack of exercise, Cholesterol, High blood pressure

Causes of diabetes § Lifestyle: Poor diet and eating habits § § “We eat so much, I don’t know, maybe because we eat so many times a day like 10 o’clock, 11 we eat. We eat …. and then we watch TV, we eat chips, so a sign of we eat all of the time. ” “I think its because we eat too much food, not the way we prepare, but we eat too much. ” § Stress and tension § § “Diet and stress. I am worried that it will come” “Anxiety is another reason behind many diseases, the anxiety, tension and stress” § “its destiny” § “its hereditary”

Causes: Anxiety, tension & stress § “That also stress causes Diabetes as well if someone is overly stressed for long lengthy periods. ” § “The Diabetes well the sugar level in my body if I was sad or happy it either picks up and goes quite high or drops down to very low levels with sadness or happiness. ” § “And I was adding to that stress that …illnesses including Diabetes is caused by stress. Stress is one of the main things that causes illnesses. ”

Causes: Food § § “fast food” as the culprit. “You get very sick when you have bad food. Fast food anyway. It’s terrible for your body and you getting sick. ” “I think I shouldn’t eat any Takeaway food. None whatsoever. I ate Mc. Donalds once and fell ill for a couple of days; so home cooking. What I mean is, they are too fatty. ” “Í think meat and rice in my opinion is not right, but again meat and bread also another issue. ”

Environmental factors § “climate change I don’t know that my sugar levels going to Turkey for instance is quite maintained when I am over there and when I come back here it creeps up again. ” § “I should say that it is not only going overseas but going to high places up in the hills or the forest or something, living there for a while I often maintain my sugar levels. ” § “I don’t know again but it is because of the clarity of the air maybe and the oxygen level is quite high. ”

Environmental factors - cont § “All the …. . the skin, the meat, they all contain additives and we eat every cold chicken for example; I believe that my condition had developed because of that. ” § “For example you go to Turkey and you get an egg, a village egg, it will be natural and the eggs here they don’t have any vitamins. ” § “(In Australia) it is the way they grow their food, everything has a chemical additive, if they want to grow bigger eggs, bigger fruit, there is chemicals ……. ”

Physical activity § Walking is good § It’s the cheapest exercise, it is healthy and it is outdoors § Exercise brings your blood sugars down § Helps with weight control § Improves blood circulation § Maintains sugar levels § Helps in weight reduction § Improved state of mind

Physical activity § “it is incidental walking yes that you don’t have the benefit of a car, you are only there for a short period but you have to walk a lot and at some places you have got no choice but to walk, you know 10 kilometres a day or 15. ” § “When I went to Syria I lost 8 Kilos I walked a lot and didn’t do any exercise bike, and I ate a lot. ……. Here you get into the car and you just drive in the car. ” § “the session I have had with a Diabetes Nurse and she told me that … My sugar levels were quite high up to 16 and 20 and when I have started walking which was recently I now walk every day and 1 ½ hours each day so my sugar levels have come down dramatically to about 7. ”

Barriers to regular exercise § Not feeling safe from dogs and other people (“Walking in the street is not safe. ”) § Housework to complete § Family commitments like babysitting, housework etc. § Women don’t make time for themselves § Laziness § Historically, exercise is not a part of Turkish life § Not culturally appropriate for older women to walk in the streets or go swimming (…. . 60, 70 year old woman going under and going swimming or walking, it is not looked upon as nice. ”) § Too old or too ill § Not enough time

Regular exercise & facilitators § § § When directed to do so by their doctor Group walks and group exercises Ethnic dancing Teacher or leader for walking and exercise groups Exercise equipment or machine at home Attending the gym and cycling Illness and illness prevention Weight control A desire to get out of the house, a means of socialising for relaxation (gardening) “As a community, unless you are ill and you have to exercise so you won’t die, then that is the motivation. ”

Diabetes prevention § “…. there are many factors for me, the diet, exercises and tensions, stress. ” § “Well, you can prevent by watching what you eat, doing exercise, walking, less stress, no stress, keep away from stress. ” § “You can’t prevent it from happening, but you can …… or the amount of Diabetes you get can be controlled. The severity of it. ”

Work and Diabetes § “As a person I only found that I had Diabetes when I left work after about six months of leaving work. ” § “I used to be working in the past and as I have given up work I have sustained Diabetes, I think it may have been because of inactivity that I have sustained Diabetes and not enough exercise anymore. ”

Other Causes § Obesity: “The amount of fat in your body that is as you get fatter you would have less chance of being active and inactivity causes … and your pancreas would slow down. ” § Old age § Ethnicity

Diabetes and diet. n Foods that were detrimental to their health and to the health of people with diabetes: – – – – Fast foods Fatty/oily food Sweets Breads Rice Pasta Many fruits Fatty meats

Diet and Diabetes § “Eating anything and everything” § “Sweets, bread. All sugary things are bad Certain fruits for instance … grapes, oranges. ” § “Eating has something to do with it of course, you can eat anything but you have to eat it in moderation. It is the amount of food that is quite important. ” § “I just gave up bananas and I found out that if you eat quite mature bananas that could have effects on your level of Diabetes but if you have not so mature like almost green bananas that is probably okay and having not 2 oranges but maybe ½ an orange or ½ an apple would be okay. ”

Diet and Diabetes § “we used to eat anything that was culturally appropriate we eat a lot of nuts and things so handfuls of it usually and she (diabetes educator) told us that you can eat these nuts still but only that fits in the palm of your hand. ” § “Because it is sour I tend to eat green apples and grape fruit tend to bring down the levels of sugar”. ……”Just like grape fruit and lemon I think it has the affect of dropping down the sugar level because of the sourness. The green apple has the same effect and the red apple lifts up the levels of Diabetes. ”

Foods that counter sweetness n “Because it is sour, I tend to (eat) green apples and grape fruit tend to bring down the levels of sugar. ” n ” I have read in the paper that eating Grape Fruit can cause death…. . ” I don’t know how but I read it in a health section of the paper, I used to like grape fruit but as Diabetics don’t take it anymore. I used to eat two grape fruits a day thinking it was a fruit of life, you know a fruit that would maintain your life, lengthen your life and I had a tree in the backyard when I learnt about the affects of it I chopped it down. ”

Diabetes and obesity Lots of weight, being overweight and it is heredity as well, you can’t help it sometimes. n “the main cause of Diabetes is being overweight and if someone is overweight they almost surely will have Diabetes”. n “What is happening is if you eat and keep the nutrition in your body without burning, it’s not like a petrol tank. If you went and filled up with petrol you can’t put more when it is full, but the body is able to take more and it stores more, it increases your risk. ” n

Health Education n n The doctor and the hospital In some instances nurses, dieticians and other educators Negative experiences with Doctors and Hospitals “I have been seeing the doctors and the Diabetes specialists for many years and they could not help me and I have just seen an educator here and she has helped me. ” Need for Interpreters“I went for an appointment (to have my eyes checked) and an interpreter wasn’t booked and with that I couldn’t understand what the doctor was saying and they have given me another appointment in a years time and now I don’t know what the hell is going on. ”

Community Empowerment Limited response n Volunteering for peer support is limited n Wiling to participate in peer-led diabetes prevention n Partnerships with: n – – – Local Council Community Health Centres Exercise centres

Health Education Resources n n n Written information to be shown to other family members or friends Information is best provided when translated to languages other than English Suggestions: – – – Doctors The hospital, Health Centres Ethno-specific newspapers, Brochures and flyers Community radio Meetings similar to the focus group to share information and provide support to one another

Conclusions Good understanding of the severity of diabetes n The need to alter life stye n More information n More education n Cultural and social barriers n Interventions: – Doctors – Groups n

Sulaiman ND, Furler JS, Hadj EJ, Corbett HM, Young D. Health Promot J Austr. 2007 Apr; 18(1): 63 -8

The Peer-led Diabetes Prevention Program for TASC in Melbourne

AIMS Develop an evidence based, culturally appropriate peer-led diabetes prevention resources and program for TASC Trial the program Evaluate the program using

Methodology- how? Design: Pre and post intervention trial (action research methods) Peer- leaders Diabetes prevention program Participants Evaluation

Methodology- how? 12 peer leaders recruited from TASC Program was developed (food, exercise, group dynamics. . etc) 2 - full days training of leaders Each leader engage 10 people

Training Program Principles of peer-led program Role of diet, physical activity and stress Group facilitation, engaging Motivational techniques and chronic disease self-management Leaders were paid for their training time, recruitment of participants and implementing the program.

Outcome Indicators Changes in knowledge and attitudes Changes in behaviours Changes in body weight and waist circumference

Data collection Questionnaire and interviews: knowledge, attitudes and behaviour "Three-day Food Diary" and physical activity) Weight, waist circumference were measured Pedometer to act as incentive for walking

RESULTS (N= 94) Gender: females (73%) Age: 47% (40 -45 y) and 25% (>55 y ) COB: l l l Turkey (45%) Iraq (39%) Lebanon (12%)

They get health information from: l l l l Doctors (92%) Television (70%) Friends (54%) Nurses (35%) Brochures (35%) Family (36%) Internet (29%) Ethnic media (29%).

What did you like? 77% appreciated the information 69% the skills learned 63% the support provided 95% learned healthy eating skills 70% maintaining healthy weight 75% how to loose weight 73% value regular exercise 48% information access and 42% attitudinal change

Effectiveness of the program using 10 -points scale 68% gave 9 or 10 points 18% gave 7 or 8 points 2% gave 5 points (undecided) 2% gave 3 or 4 points

Self-reported lifestyle changes Changes after program: 89% in food preparation 79% dietary intake 82% shopping 81% feeling of well being 79% physical activity 69% body weight

Weight and Waist Weight: significant reduction in weight [mean weight pre=78. 1 kg, post=77. 3; Z score=-3. 415 (P=0. 001) Waist circumference (Z=-2. 569, P=010)
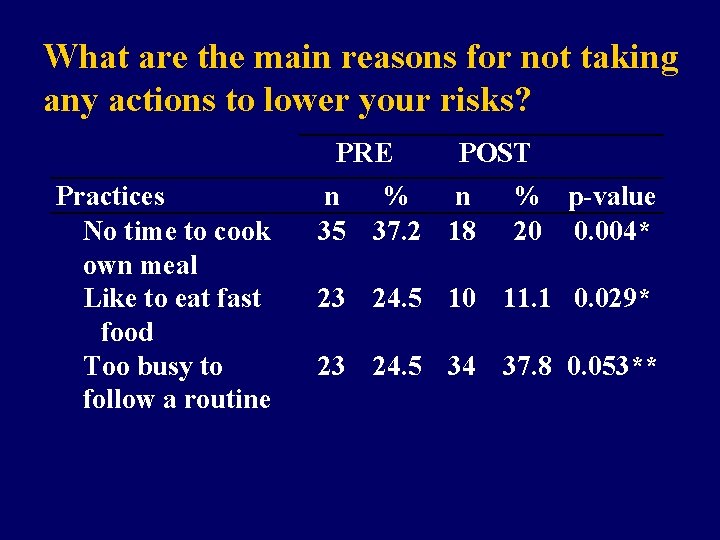
What are the main reasons for not taking any actions to lower your risks? PRE Practices No time to cook own meal Like to eat fast food Too busy to follow a routine POST n % n 35 37. 2 18 % p-value 20 0. 004* 23 24. 5 10 11. 1 0. 029* 23 24. 5 34 37. 8 0. 053**
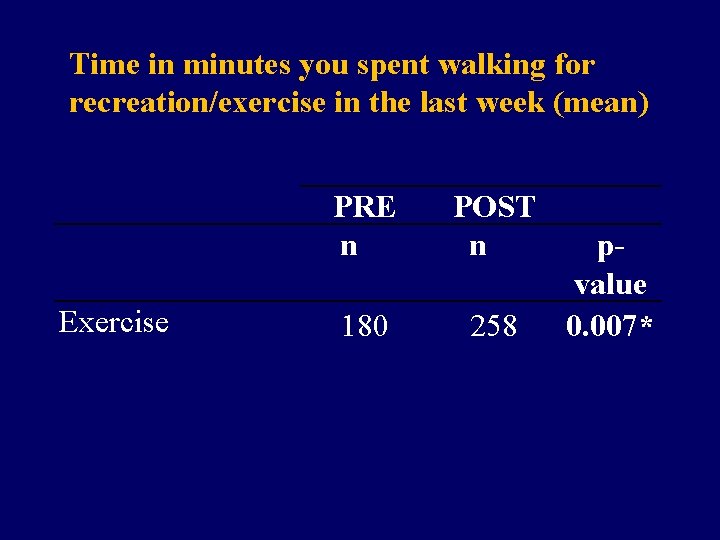
Time in minutes you spent walking for recreation/exercise in the last week (mean) Exercise PRE n POST n 180 258 pvalue 0. 007*
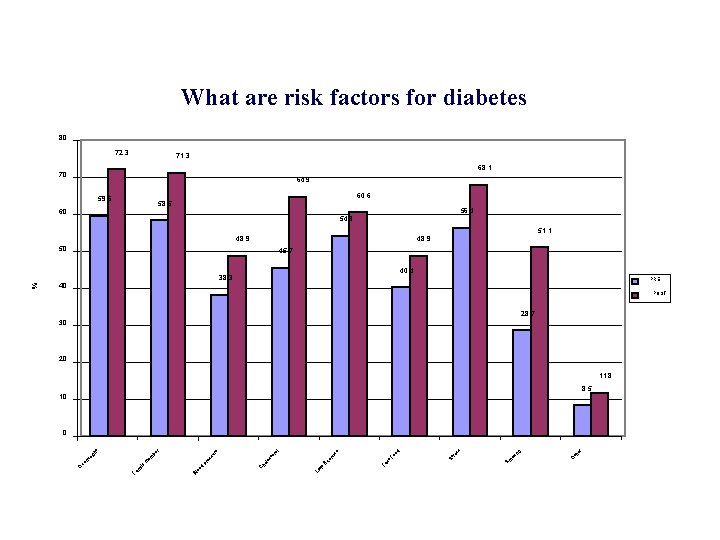
What are risk factors for diabetes 80 72. 3 71. 3 68. 1 70 64. 9 59. 6 60. 6 58. 5 60 56. 4 54. 3 51. 1 48. 9 50 45. 7 PRE POST 28. 7 30 20 11. 8 8. 5 10 O th er g in ok re ss Sm st Fa St d Fo o se Ex ttl e Li C ho le er ci st er ol re su pr es d Bl oo m ily m Fa ve rw ei em gh t be r 0 O % 40. 4 38. 3 40
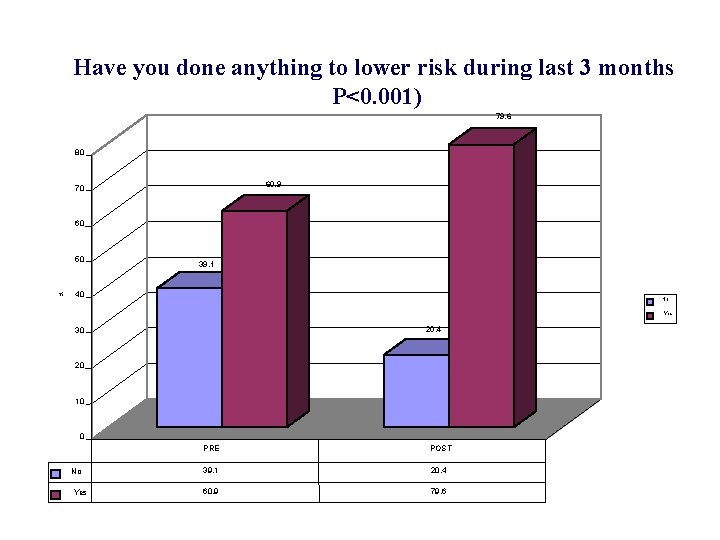
Have you done anything to lower risk during last 3 months P<0. 001) 79. 6 80 60. 9 70 60 50 % 39. 1 40 No Yes 20. 4 30 20 10 0 No Yes PRE POST 39. 1 20. 4 60. 9 79. 6
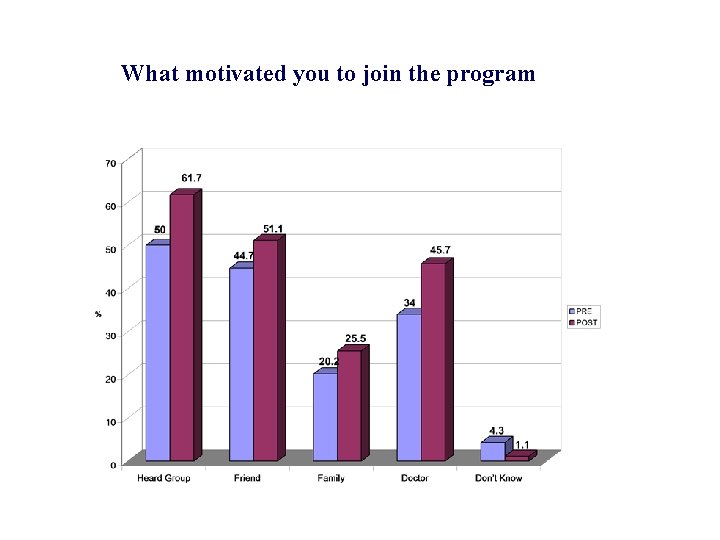
What motivated you to join the program

Conclusions 2. The program was effective in improving knowledge and enhancing exercise in Melbourne, Australia 3. Peer-led diabetes prevention program should be piloted/ replicated in Sharjah to explore feasibility

Conclusions Limited intervention • Administered by trained peers equipped with culturally appropriate education • Native language Significant improvement in: • knowledge and attitudes • limited changes in lifestyle behaviour • The changes were maintained three months after the intervention.

Thank you

Uptake of lifestyle However, uptake of such lifestyle changes has been poor Programs developed to enhance the uptake, such as: Ø Diabetes Nurse Educator Ø Coach program Ø Chronic Disease Self- management Ø Others
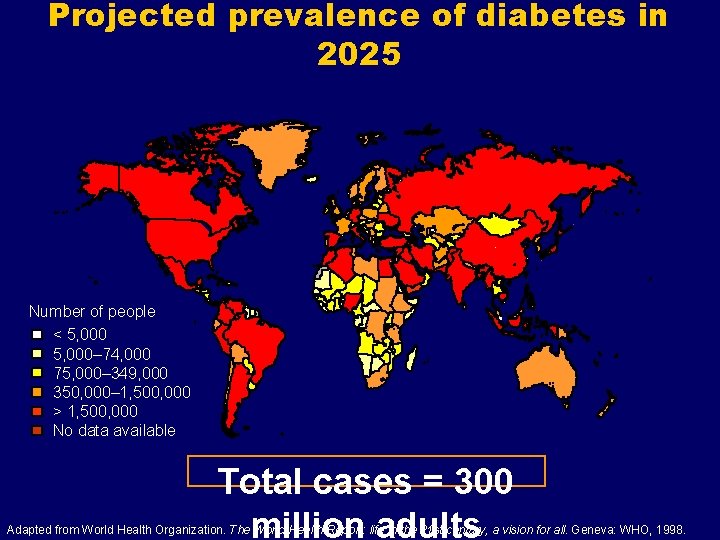
Projected prevalence of diabetes in 2025 Number of people < 5, 000– 74, 000 75, 000– 349, 000 350, 000– 1, 500, 000 > 1, 500, 000 No data available Total cases = 300 million adults Adapted from World Health Organization. The World Health Report: life in the 21 st century, a vision for all. Geneva: WHO, 1998.
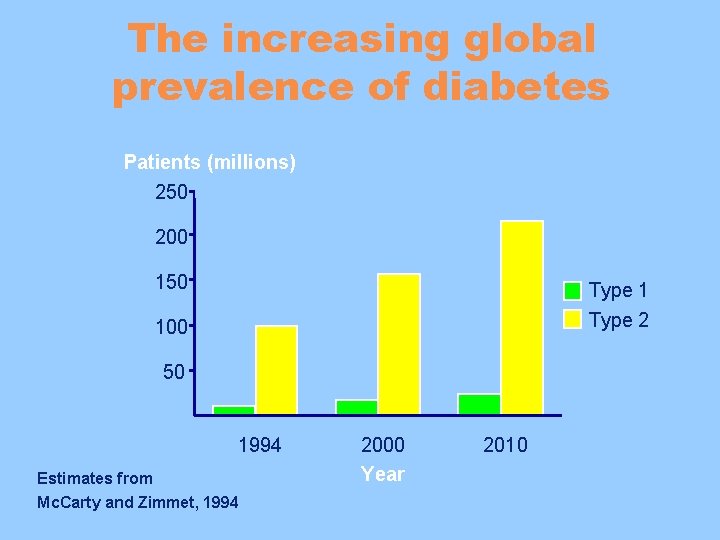
The increasing global prevalence of diabetes Patients (millions) 250 200 150 Type 1 Type 2 100 50 1994 Estimates from Mc. Carty and Zimmet, 1994 2000 Year 2010
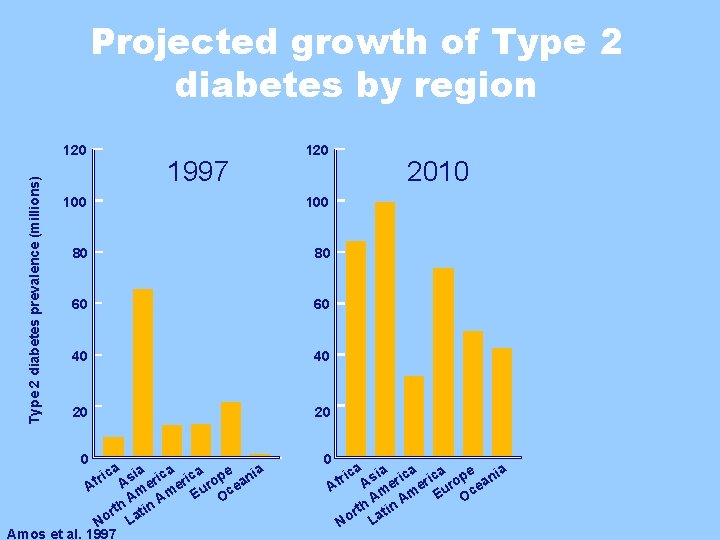
Projected growth of Type 2 diabetes by region Type 2 diabetes prevalence (millions) 120 1997 120 100 80 80 60 60 40 40 20 20 0 ica a a r Asi eric rope ani f e u ce A Am Am E O rth atin o L N Amos et al. 1997 2010 0 ca sia ica pe nia A er er uro ea c Am Am E O h n rt ti No La ri Af

Lifestyle modification Diet Exercise Weight loss Smoking cessation If a 1% reduction in Hb. A 1 c is achieved, you could expect a reduction in risk of: • • • 21% for any diabetesrelated endpoint 37% for microvascular complications 14% for myocardial infarction However, compliance is poor and most patients will require oral pharmacotherapy within a few years of diagnosis Stratton IM et al. BMJ 2000; 321: 405– 412.

Type 2 diabetes in different populations Lowest rates Highest rates (Rural India) Asian Indian (Fijian Indian) (Rural Kiribati) Micronesian (Urban Kiribati) (Rural Tunisia) Arab (Oman & UAE) (Central Mexico) Hispanic (US Mexican) (Rural China) Chinese (Mauritian Chinese) (Rural W. Samoa) (Urban W. Samoa) Polynesian (Rural Tanzania) African (US Afr. Amer. ) (Poland) European (Laurino, Italy) (Rural Fiji) Melanesian (Urban Fiji) 0 5 10 15 20 Prevalence of Type 2 diabetes (%) Amos et al. 1997 25

Diabetes Australia Facts 2008 T 2 DM in CALD populations: 1. 2. 3. 4. 5. Prevalence of diabetes Prevalence of risk factors Complications Hospitalisations due to non-treatable diabetes Death rates due to diabetes

Diabetes Australia Facts 2008 1. Prevalence of diabetes is increasing over time 2. Reduces quality of life 3. Preventable via lifestyle modifications 4. Some population groups are at higher risk including CALD

Meta-analysis of 11 trials in CALD 1. 2. 3. 4. 5. Improved Hb. A 1 c after culturally at 3 M Weight Mean Difference -0. 3% at 3 M and 0. 6% at 6 M Knowledge scores improved at 3 M Healthy life style improvement at No difference in secondary outcomes: lipid levels, qo. L, selfefficacy, BP, Hawthorne K, Robles Y, Cannings-John R, Edwards S. Culturally appropriate health education for type 2 diabetes in ethnic minority groups. Cochrane Database of Systematic Revies 2008 (3)
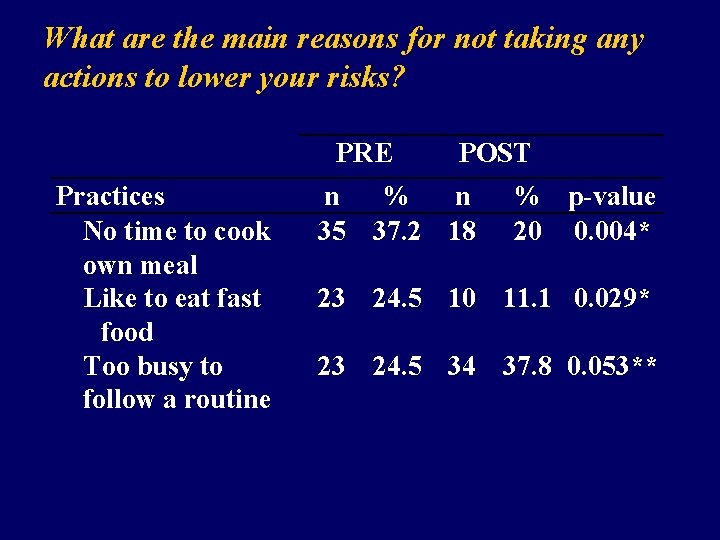
What are the main reasons for not taking any actions to lower your risks? PRE Practices No time to cook own meal Like to eat fast food Too busy to follow a routine POST n % n 35 37. 2 18 % p-value 20 0. 004* 23 24. 5 10 11. 1 0. 029* 23 24. 5 34 37. 8 0. 053**
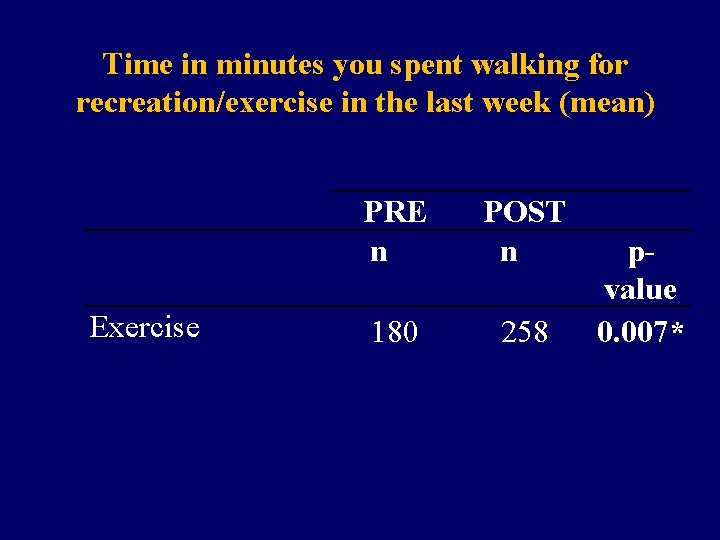
Time in minutes you spent walking for recreation/exercise in the last week (mean) Exercise PRE n POST n 180 258 pvalue 0. 007*

2. Qualitative Study Qualitative focus groups to investigate feasibility and cultural appropriateness, barriers and facilitators of known interventions in Sharjah

Aims The target setting is primary health care centers. People visiting all primary health care centers/ Hospitals in Sharjah will be targeted. Risk factors are: Diabetes Physical activity High cholesterol Unhealthy eating (poor diet) Smoking

Interventions

Interventions Case-finding/ screening for prediabetes and diabetes in PHC Consultation with doctors, nurses and patients to identify appropriate diabetes intervention Engaging people with diabetes/ pre-diabetes in CDSM programs and the COACH Family study to look at the genetic profile CME for doctors and nurses in EB diabetes management Training nurses to be diabetes nurse educators (DNE) to provide the interventions in PHC centres.


Models of Diabetes Care in PHC Dr Nabil Sulaiman The University of Sharjah The University Melbourne

This Presentation Trends in diabetes l Lifestyle interventions- evidence l Models of interventions in PHC: l Diabetes Nurse Educator (DNE) l COACH model l Chronic Disease Self management l

Diabetes in UAE High prevalence in the Gulf Countries. In the UAE the prevalence is: 24% of adults 40% with diabetes and IGT Diabetes is occurring in younger age

Environmental and behavioral changes New dietary habits (what and how we eat), Lack of physical activity, Overweight/ obesity, and Stresses of urbanization and working condition will lead to further rise of CVD and diabetes, and their risk factors.

Evidence RCT in Finland the USA have demonstrated that the incidence of diabetes can be reduced by about 57% by modifying: Physical activity and Diet (Tuomilehto et al 2001, Knowler et al 2002)

Lifestyle Changes However, uptake of such lifestyle changes has been poor Programs developed to enhance the uptake, such as: Ø Diabetes Nurse Educator Ø Coach program Ø Chronic Disease Self- management Ø Others

In Primary Health Care In Australia, people with T 2 D have 80% of their care in General Practice Diabetes requires the GP to practise biomedical, anticipatory and psychosocial care using evidencebased and patient-centred medicine and Patient to engage actively in managing their illness.

Diabetes Nurse Educator Trained nurse Engage, educate and empower patient to manage diabetes and impact of disease on patient and family Based on trust and partnership between PHC centre- Diabetes nurse educator and patient Patient determines agreed targets Continuity and access

Diabetes Coach Program Tested in Melbourne using RCTs for CVD Trained nurse or dietitian to do COACH Following diagnosis or after discharge from hospital Education and empowerment Patient determines agreed targets Follow up consultation or phone calls Showed benefit in several outcomes

Chronic disease self management Is an effective way in which patients are empowered to become more active and effective in managing their disease. Patient engages in “activities that protect and promote health, monitoring and managing of symptoms and signs of illness, managing the impacts of illness on functioning, emotions and interpersonal relationships and adhering to treatment regimes”


Chronic Disease Self Management (CDSM) Stanford University Kate Lorig Director of the Stanford Patient Education Research Center

Stanford CDSM Program Is a workshop where people with different chronic diseases attend Teaches the skills needed in the day-to-day management of treatment and to maintain and/or increase life’s activities. The Program has been adopted by NHS, the Diabetes Society of British Columbia in Canada, Kaiser Permanente, etc It has been translated into Chinese, Vietnamese, Norwegian, and Italian. The patient book is available in Japanese

Stanford Program Small-group workshops, Generally 6 weeks long, Meeting once a week for about 2 hours, Led by a pair of lay leaders with health problems of their own, The meetings are highly interactive, focusing on building skills, sharing experiences and support.

One Step Ahead Seminars for people with pre diabetes Evidence of reduction of 0. 5% Hb. A 1 C

Patient empowerment through CDSM Patient empowerment has a crucial role in the treatment of chronic disease: knowledge and skill development to understand manage one’s condition and the confidence to use that training for better self care and greater compliance Feeling of control and skill development to achieve a more interactive relationship with health care professionals, with the capacity to demand good quality care The patient becomes a better self advocate/agent, more able to get from the health system what they need in particular.
- Slides: 94