Examination of hemostasis Stanislav Matouek Hemostatic disorders thrombosis

Examination of hemostasis Stanislav Matoušek
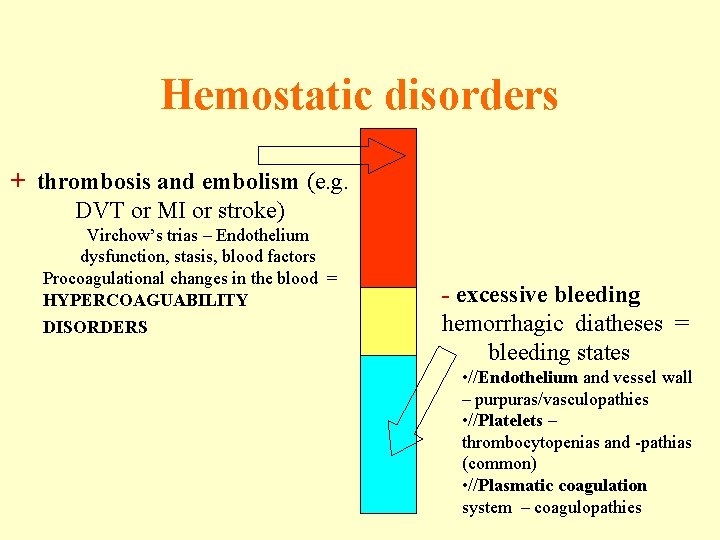
Hemostatic disorders + thrombosis and embolism (e. g. DVT or MI or stroke) Virchow’s trias – Endothelium dysfunction, stasis, blood factors Procoagulational changes in the blood = HYPERCOAGUABILITY DISORDERS - excessive bleeding hemorrhagic diatheses = bleeding states • //Endothelium and vessel wall – purpuras/vasculopathies • //Platelets – thrombocytopenias and -pathias (common) • //Plasmatic coagulation system – coagulopathies
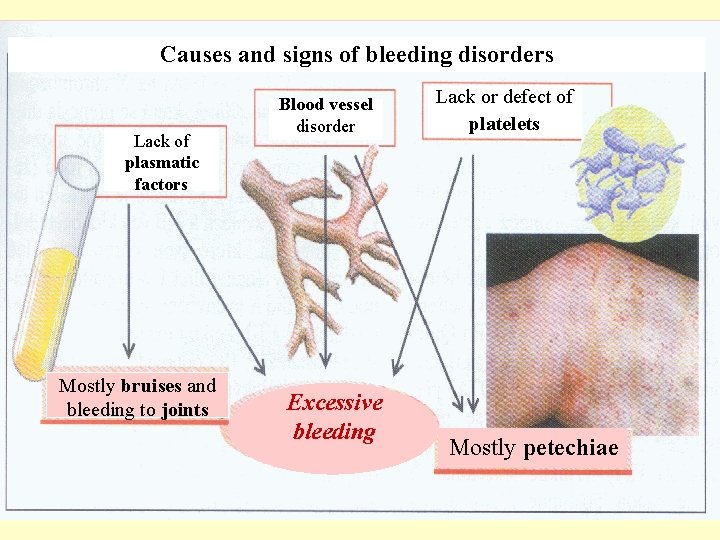
Causes and signs of bleeding disorders Lack of plasmatic factors Mostly bruises and bleeding to joints Blood vessel disorder Excessive bleeding Lack or defect of platelets Mostly petechiae

Disorders of primary hemostasis Platelets and vessels
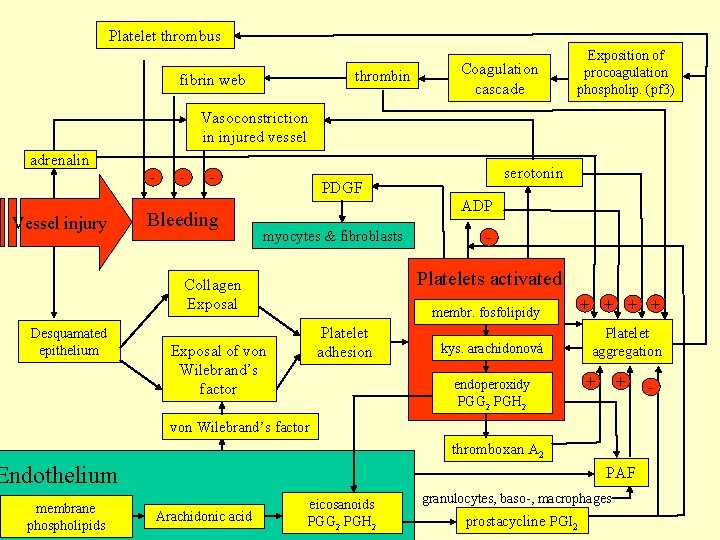
Platelet thrombus thrombin fibrin web Coagulation cascade Exposition of procoagulation phospholip. (pf 3) Vasoconstriction in injured vessel adrenalin Vessel injury - - - Bleeding PDGF ADP myocytes & fibroblasts - Platelets activated Collagen Exposal Desquamated epithelium serotonin Platelet adhesion Exposal of von Wilebrand’s factor membr. fosfolipidy + + kys. arachidonová Platelet aggregation endoperoxidy PGG 2 PGH 2 + + von Wilebrand’s factor thromboxan A 2 Endothelium membrane phospholipids PAF Arachidonic acid eicosanoids PGG 2 PGH 2 granulocytes, baso-, macrophages prostacycline PGI 2 -

Thrombocytopenia • 1) Production decreased↓ • 2) Consumption increased ↑ – A) with increased activity of thrombin – B) imuno-thrombocytopenia – C) other • 3) Combination of both mechanisms

Platelet count • 200 – 400 x 103/µL (109/L) = 200 000 – 400 000 /µL The risk of spontaneous bleeding is low if the number of platelets is > 30 000 /µL and blood vessels and coagulation system are intact

I) Thrombocytopenia from insufficient production • Aplastic disorder – Congenital – Acquired • Bone marrow damaged by medicaments (chemotherapy), chemicals (benzene), radiation, infection (HIV), autoantibodies • Infiltration of bone marrow (carcinomas, lymphomas, leukemia) • Myelodysplastic syndrome, Myelofibrosis • Defect in megakaryocyte maturation – vit. B 12 and folate deficiency Bone marrow aspiration (less megakaryocytes in aplastic)

2) Thrombocytopenia from increased consumption • A) Increased activity of thrombin – Disseminated intravascular coagulation – DIC – activation in infections/malignities (extracellular proteases)-chronic DIC • B) Imunothrombocytopenia (e. g. autoantibodies) – Idiopathic thrombocytopenic purpura- autoantibodies produced with unknown cause • Acute vs. chronic – Secondary ( SLE, lymphomas, HIV) – After medicaments • …. • Heparin induced – C) Other – Hypersplenism, artificial valve – TTP = Thrombotic thrombocytopenic purpura Activity of thrombin, clotting tests PT and a. PTT

Thrombotic thromboplastic purpura • ? Cause is probably damage to endothelium - release of von Willebrand factor - decreased degradation of v. Wf by its protease (antibodies against the protease, congenital? )
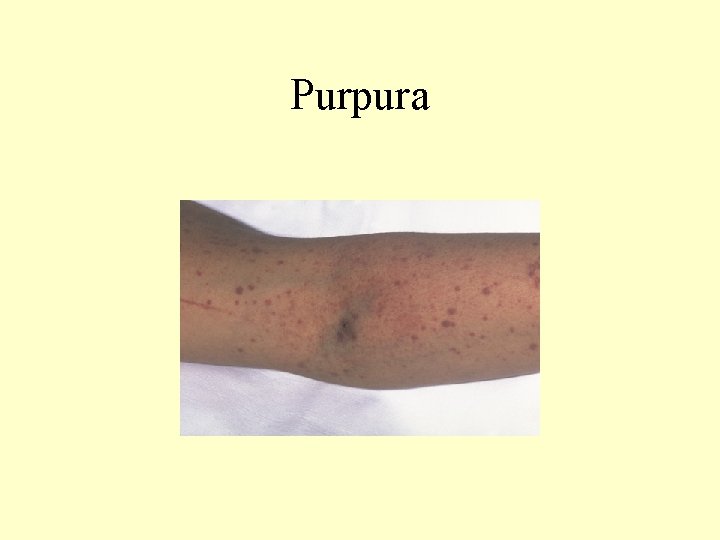
Purpura

3) Combination of low production and increased consumption – Liver cirrhosis

platelet dysfunction = thrombocytopathy • Congenital • Acquired – – – aggregation inhibitors therapy (aspirin, ticlopidin) platelets covered by Ig. A or Ig. M (multiple myeloma) Dextran (infusion, often given in bleeding) Uremia (Kidney failure) Essential Thrombocytosis (one of myeloproliferative diseases analogy of polycythemia vera) Normal number of platelets, bleeding time ↑ Clinically: Generally, it is difficult to stop bleeding (e. g. during surgery),

Bleeding time (Duke) • Standardized puncture of the earlobe, or standardized incision to the forearm with cuff inflated to 40 Torr. • We measure the time until the bleeding stops • 2 -5 min (2 -9 min in forearm) • Increased in platelet dysfunction and in von. Willebrand disease (but not in Hemophilia)

von. Willebrand disease • Missing or defective von. Willebrand factor • The factor is important in platelet adhesion (primary hemostasis) and serves also as a carrier for factor VIII (decrease of concentration of factor VIII leads to defect in coagulation) • Combined bleeding of petechial and hemophilic type • Congenital or acquired • Prevalence 1%, but generally mild symptoms (heterozygotes) • Prolonged bleending time (Duke) and a. PTT
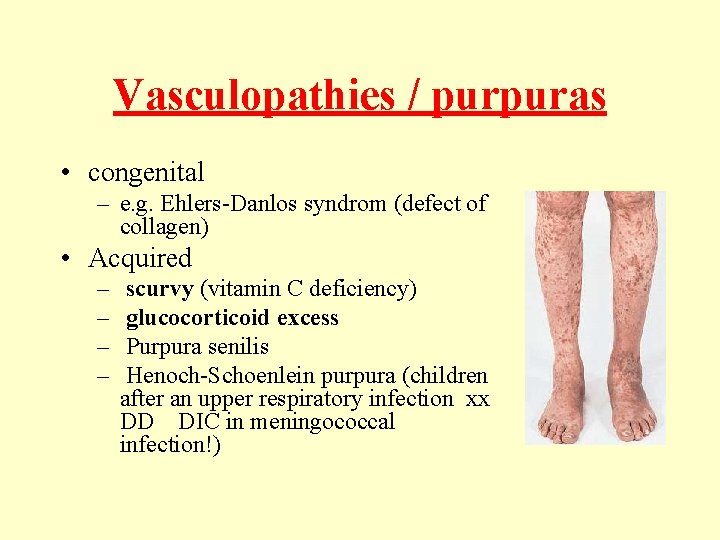
Vasculopathies / purpuras • congenital – e. g. Ehlers-Danlos syndrom (defect of collagen) • Acquired – – scurvy (vitamin C deficiency) glucocorticoid excess Purpura senilis Henoch-Schoenlein purpura (children after an upper respiratory infection xx DD DIC in meningococcal infection!)

Tourniquet test (Rumpel-Leede capillary-fragility test) – A blood pressure cuff is inflated to a point little bit above diastolic blood pressure during 5 min (10 min). – Positive, if more that 5 petechiae per square inch are found. – Vasculopathies, dengue fever diagnosis (more than 20 petechiae).

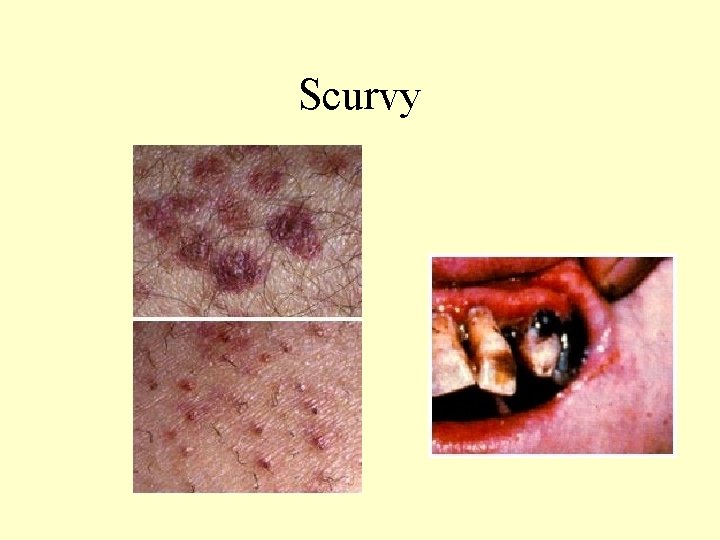
Scurvy

Secondary hemostasis disorders Plasma coagulation system
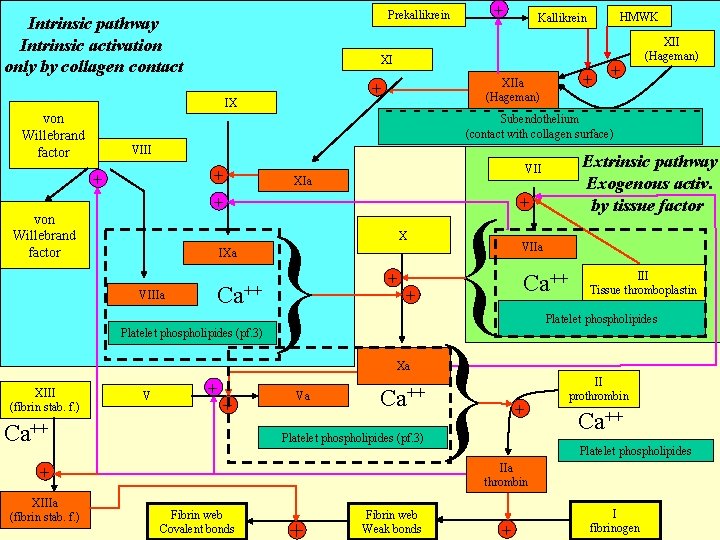
Prekallikrein Intrinsic pathway Intrinsic activation only by collagen contact HMWK Kallikrein XI + IX von Willebrand factor + + XIIa (Hageman) + XII (Hageman) - - - - -Subendothelium -------(contact with collagen surface) VIII + + + von Willebrand factor XIa { } } X IXa VIIIa Ca++ Platelet phospholipides (pf. 3) Extrinsic pathway Exogenous activ. by tissue factor VII + + + VIIa Ca++ III Tissue thromboplastin Platelet phospholipides Xa XIII (fibrin stab. f. ) V + + Ca++ + Platelet phospholipides (pf. 3) II prothrombin Ca++ Platelet phospholipides IIa thrombin + XIIIa (fibrin stab. f. ) Va Fibrin web Covalent bonds + Fibrin web Weak bonds + I fibrinogen
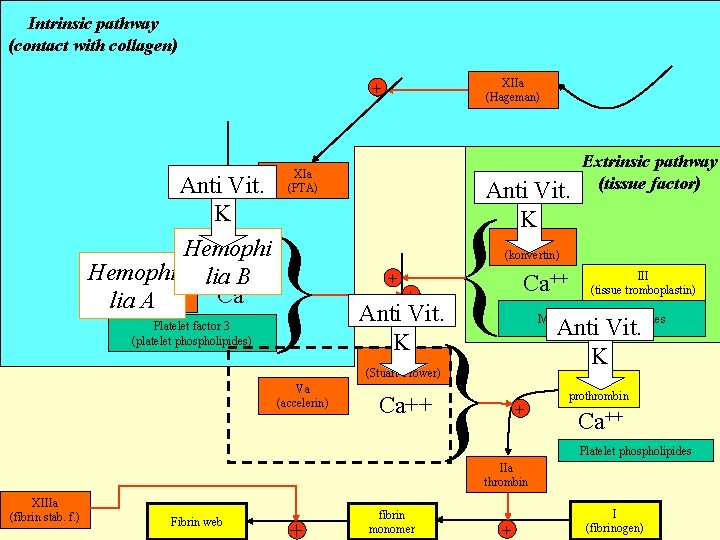
Intrinsic pathway (contact with collagen) XIIa (Hageman) + Anti+ Vit. K IXa Hemophi (Christmas) Hemophi lia B VIIIa ++ Ca (AF) lia A Platelet factor 3 (platelet phospholipides) XIa (PTA) Anti Vit. K { } } Extrinsic pathway (tissue factor) VIIa (konvertin) + + Ca++ Anti Vit. K Membrane phospholipides Anti Vit. K Xa (Stuart-Prower) Va (accelerin) Ca++ III (tissue tromboplastin) + II prothrombin Ca++ Platelet phospholipides IIa (thrombin) thrombin XIIIa (fibrin stab. f. ) Fibrin web + fibrin monomer + I (fibrinogen)

Queen Victoria of Britain Carrier of Hemophilia Tsar Nicolai II of Russia X-linked Greatgrandson Tsarevich Alexei Sufferer of Hemophilia

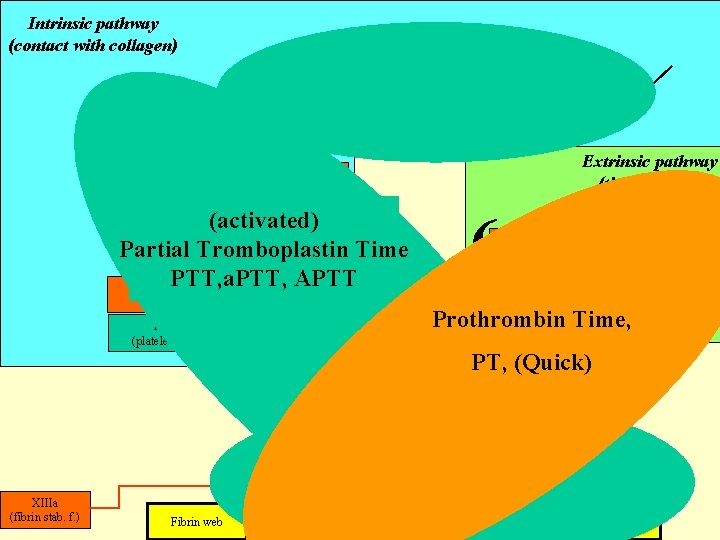
Intrinsic pathway (contact with collagen) XIIa (Hageman) + + Extrinsic pathway (tissue factor) XIa (PTA) { } } (activated) IXa Partial Tromboplastin Time (Christmas) APTT + VIIIa PTT, a. PTT, ++ + Ca (AF) Platelet factor 3 (platelet phospholipides) VIIa (konvertin) III Ca++ (tissue tromboplastin) Membrane phospholipides Prothrombin Time, Xa (Stuart-Prower) PT, (Quick) Va (accelerin) + IIa (thrombin) XIIIa (fibrin stab. f. ) Fibrin web + fibrin monomer + I (fibrinogen)
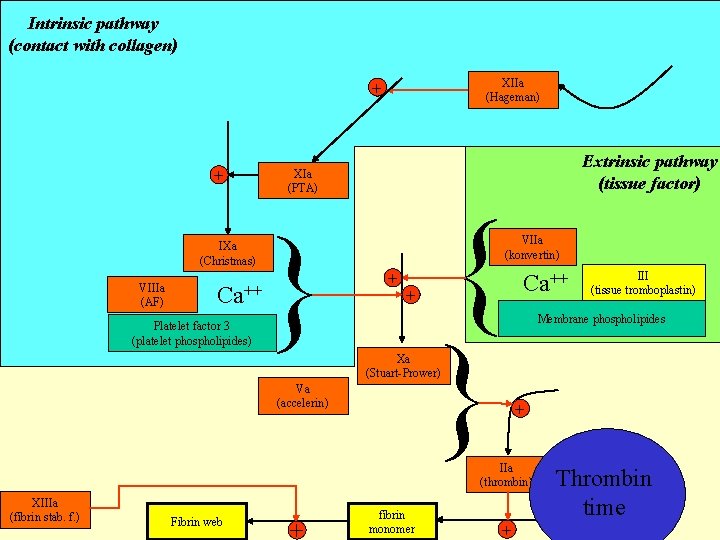
Intrinsic pathway (contact with collagen) XIIa (Hageman) + + IXa (Christmas) VIIIa (AF) Ca++ Platelet factor 3 (platelet phospholipides) Extrinsic pathway (tissue factor) XIa (PTA) { } } VIIa (konvertin) + + Ca++ III (tissue tromboplastin) Membrane phospholipides Xa (Stuart-Prower) Va (accelerin) + IIa (thrombin) XIIIa (fibrin stab. f. ) Fibrin web + fibrin monomer + Thrombin time I (fibrinogen)

a. PTT Citrate or oxalate plasma, We add phospholipids, Ca++, caolin or other negatively charged surface Time until clot formation (depends on the lab) ~ 25 - 39 s Monitoring of heparin therapy, intrinsic and common pathway, hemophilia

Prothrombin Time (Quick test) • Citrate or oxalate plasma, • We add phospholipids, Ca++, and tissue thromboplastin Time until clot formation (depends on the used thromboplastin) • ~ 12 -15 s • INR = PTtest/ PTnormal (norm 0. 8 – 1. 2) • Monitoring of anti vitamin K anticoagulant therapy (warfarin), extrinsic and common pathway
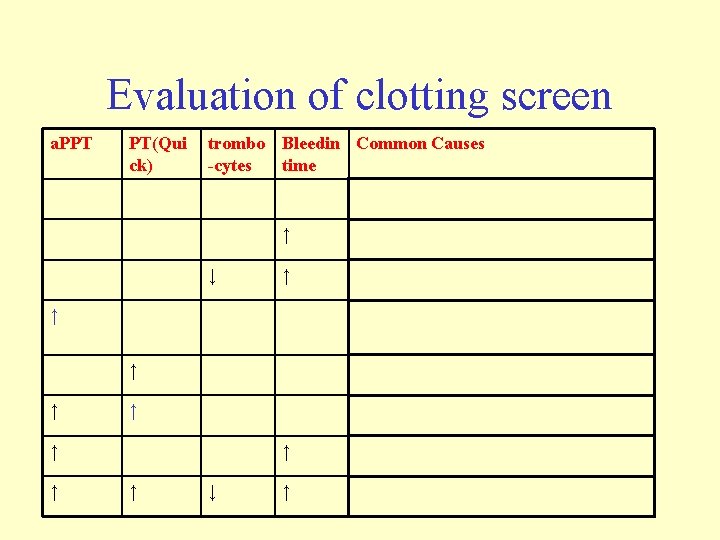
Evaluation of clotting screen a. PPT PT(Qui ck) trombo Bleedin Common Causes -cytes time Vessel disorder, f. XIII deficiency ↓ ↑ Thrombocytopathy ↑ thrombocytopenia ↑ ↑ Heparin, deficiency of VIII, IX, XII, HMWK, prekallikrein ↑ Factor VII deficiency ↑ Warfarin, vit. K deficiency, I, II, V, X ↑ ↑ ↑ ↓ ↑ von. Willebrand disease ↑ Liver disease, DIC, sepsis

Inhibition of coagulation
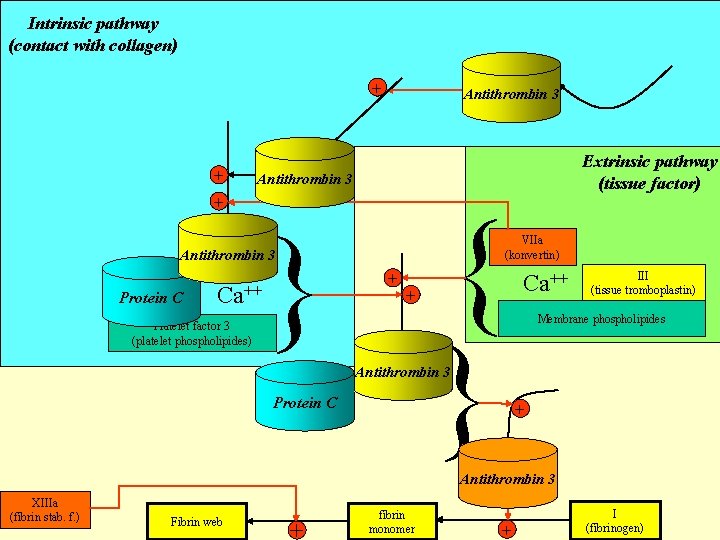
Intrinsic pathway (contact with collagen) XIIa + + + XIa Antithrombin (PTA) IXa Antithrombin (Hageman) 3 Extrinsic pathway (tissue factor) 3 { } } VIIa (konvertin) Antithrombin (Christmas) 3 VIIIa Protein (AF) C Ca++ Platelet factor 3 (platelet phospholipides) + + Ca++ III (tissue tromboplastin) Membrane phospholipides Xa Antithrombin (Stuart-Prower) 3 Va (accelerin)C Protein + IIa Antithrombin (thrombin) XIIIa (fibrin stab. f. ) Fibrin web + fibrin monomer + 3 I (fibrinogen)
Antithrombin 3 Antithrombin Antitrombin 33 Antithrombin 3 Protein C Antithrombin 3
Antithrombin 3 Protein C Antithrombin 3
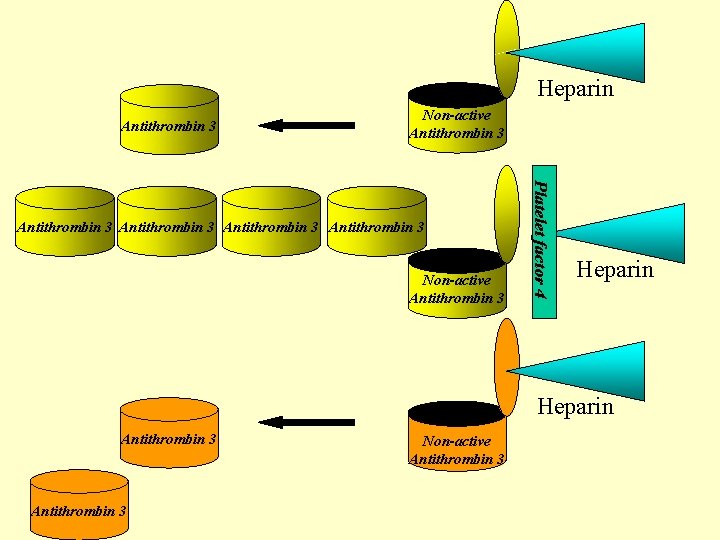
Heparin Non-active Antithrombin 3 3 Xa Antithrombin (Stuart-Prower) 3 XIa Antithrombin (PTA) 3 XIIa Antithrombin (Hageman) 3 Non-active Antithrombin 3 Platelet factor 4 IXa Antithrombin (Christmas) Heparin Antithrombin 3 IIa Antithrombin 3 (trombin) Non-active Antithrombin 3
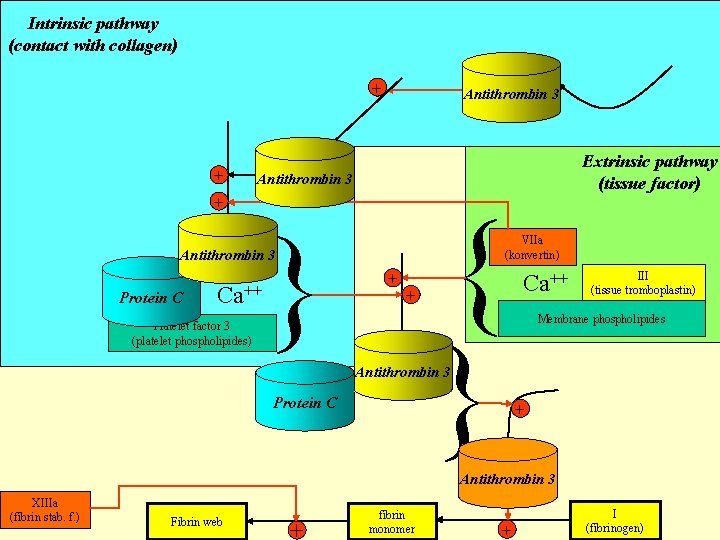
Intrinsic pathway (contact with collagen) XIIa + + + XIa Antithrombin (PTA) IXa Antithrombin (Hageman) 3 Extrinsic pathway (tissue factor) 3 { } } VIIa (konvertin) Antithrombin (Christmas) 3 VIIIa Protein (AF) C Ca++ Platelet factor 3 (platelet phospholipides) + + Ca++ III (tissue tromboplastin) Membrane phospholipides Xa Antithrombin (Stuart-Prower) 3 Va (accelerin)C Protein + IIa Antithrombin (thrombin) XIIIa (fibrin stab. f. ) Fibrin web + fibrin monomer + 3 I (fibrinogen)

Fibrinolysis =thrombolysis
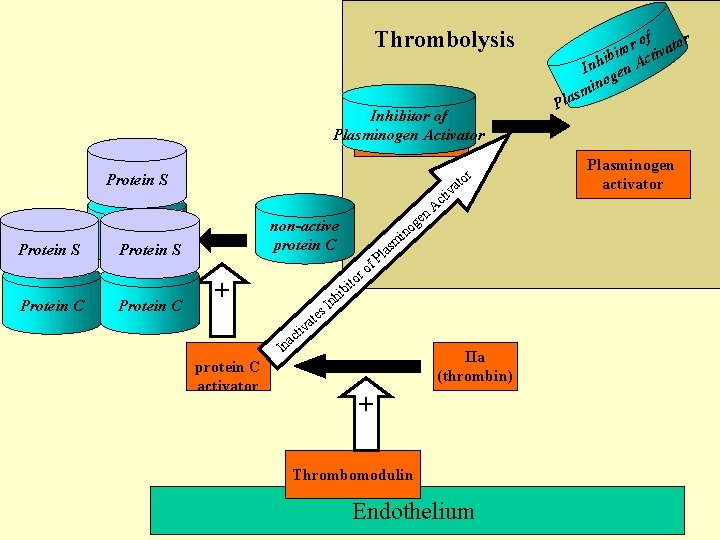
Thrombolysis Inhibitor of Aktivátor Plasminogen Activator plazminogenu Protein S VIIIa Protein C (AF) v non-active protein C Protein S Va Protein C (akcelerin) r ato f ro m las en g o in P ito + s ate b hi In tiv c a In protein C activator ti Ac IIa (thrombin) + Thrombomodulin Endothelium of tor r a o t ibi Activ h In gen ino m s a Pl Plasminogen activator

Hypercoaguability (thrombophilic) disorders
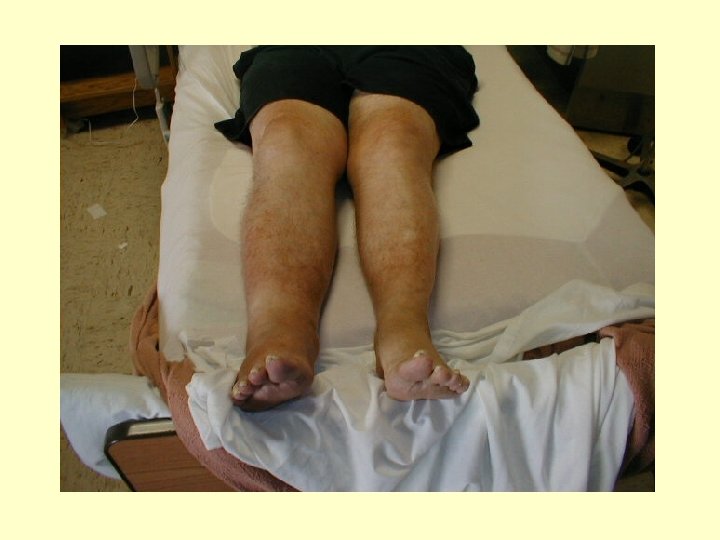

Most common hypercoagubility disorders • Mutation of factor V – Leiden mutation / insensitivity to protein C • Defect in Antithrombin III • Defect in Protein C • Defect in Protein S
- Slides: 40