EVOLUTION OF A SYSTEM WIDE CVO WAMSS MEETING














- Slides: 16

EVOLUTION OF A SYSTEM WIDE CVO WAMSS MEETING – WALLA, WA – APRIL 26, 2017

OBJECTIVES Understand the set-up and organization of a Health System CVO Understand how a CVO benefits your hospital/health system Understand how bringing Provider Enrollment into your Credentialing world is a beneficial Understand the importance of having a single source of truth database Understand how to set-up and implement quality monitoring, matrix and reporting in your credentialing and provider enrollment processes

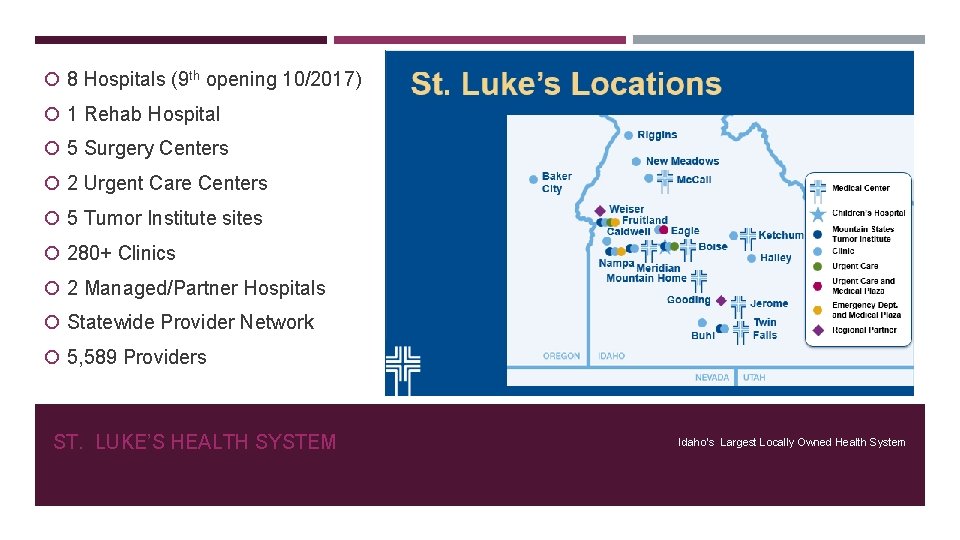
8 Hospitals (9 th opening 10/2017) 1 Rehab Hospital 5 Surgery Centers 2 Urgent Care Centers 5 Tumor Institute sites 280+ Clinics 2 Managed/Partner Hospitals Statewide Provider Network 5, 589 Providers ST. LUKE’S HEALTH SYSTEM Idaho’s Largest Locally Owned Health System

WHY CENTRALIZE & STANDARDIZE? Credentialing is expensive Credentialing is time consuming Lots of duplication Long & varying turnaround times Frustrated providers, physician services, administration

BENEFITS TO FACILITIES TO PROVIDERS Cost savings ONE application & forms Increased productivity Standardized requirements Elimination of duplication Shorter processing times Streamlined processes One source of truth – record Increased efficiency Increased accuracy Increased regulatory compliance documentation TO MSSPs More time to. . Update Bylaws & documents Develop policies Improve meeting preparation & follow-up Assist Medical Staff Dedicated coordinator Leadership Provider Enrollment & Increased efficiency Credentialing done simultaneously Increased regulatory compliance Audit Ready Files

CVO CREATION CVO was created in 2010 2, 472 providers 5 staff members 4 Hospitals Credentialing Only Expanded Services Provider Enrollment (2011) Database Management and Single Source of Truth (2012) Rapidly grew

CVO CURRENT DAY & ORGANIZATION 14 Employees Numerous Facilities 3 Services Lines: Credentialing (5, 589 providers) Database Management (14, 646) Provider Enrollment (1, 376 providers)

CREDENTIALING Initial Appointment Sending the application through verification Reappointment Specialty cycle alignment Sending the application through verification Expirable Management (10, 372 annually) Notices 60 days prior & Follow-up Ongoing Monthly Monitoring Privilege Maintenance Delegated Credentialing Audits Audit Help & Assistance

PROVIDER ENROLLMENT What is Provider Enrollment? The overall process of gathering credentials information, completing payer applications, obtaining signatures, submitting applications to payers, verifying enrollment effective dates and maintaining the enrollments. Initial Enrollment Why doing it well matters § Faster enrollments mean faster reimbursement § Less denials & write-offs mean more money Benefits of including it in your credentialing process § One stop shopping § Seemless process § Less ‘hands in the pot’ Recredentialing Out-of State Medicaid, Railroad Medicare, Workers Comp Enrollments Maintenance: Changes Claim Resolution Terms

DATABASE MANAGEMENT - SINGLE SOURCE OF TRUTH Maintains a complete provider database Prior to Single Source of Truth § Numerous provider databases § Data integrity was non-existent § Confusion & frustration Credentialed, referring, ordering Provides system-wide reports, directories, exports Exports to all downstream systems including EPIC Benefits of being the single source of truth § Increased data integrity § One place to provide updates § One place to request data/reports § Happier customers all around Credentialing database support Automated forms, letters, reports, emails, faxes, processes Standard workflows Provides Software Training Troubleshooting Builds reports, letters, forms, modules

SUCCESSES Improved Turnaround Times Faster Enrollment with Payors – MORE $$ Less claim denials and deactivations Audit Ready Files Increased compliance with regulatory standards Increased Provider & MSSP Satisfaction Decreased costs Zero expired documents Online Application & Privileges Paperless credentialing files Aligned reappointments Improved data integrity


OUR QUALITY PROGRAM Monthly Monitoring & Reporting Activity Numbers 100% File Review Turnaround Times Quality Reporting Tool Credentialing & Provider Enrollment Errors & Omissions Provider Satisfaction Initial & Recredentialing Client Satisfaction Billing Hold Dollars Controllable Write-offs: Enrollment Database Audits Written Standard Operating Policies Individual Coordinator Feedback Reports Quarterly & Yearly Quality Report Sent out & shared throughout system

SAMPLE OF QUALITY SCORECARDS

WHAT’S IN OUR FUTURE System Bylaws System Privileges System Peer Review/OPPE/FPPE Processes One System Credentials Committee

TAWNA MILES-KNIGHT, CPCS CVO DIRECTOR ST. LUKE’S HEALTH SYSTEM – BOISE, ID milest@slhs. org (208) 381 -8744