EvidenceBased Treatments for Major Depressive Disorders Learning Objectives

Evidence-Based Treatments for Major Depressive Disorders

Learning Objectives • After this presentation, participants will be able to: • Identify one evidenced based intervention for depressive disorders. • Articulate the goals of one evidenced based intervention. • Describe the key processes, steps, and/or skills involved in implementing the highlighted evidenced based intervention with students. 2

Brief Overview of Key Features Depressive Disorders 3

Key Features of Depressive Disorders • Definition: A period of two weeks or longer during which there is either depressed mood or loss of interest or pleasure, and at least four other symptoms that reflect a change in functioning, such as problems with sleep, eating, energy, concentration, and self-image. • Ages 12 to 17 only: In 2015, an estimated 3 million adolescents had at least one major depressive episode in the past year. 4

General treatment considerations for depression 5

Treatment considerations • Psychosocial /non-pharmacological interventions include psychoeducation, cognitive behavioral therapies, and group supports • Address current psychosocial stressors and identify support resources • The SIF is a good JC tool to identify stressors and risk • Employ a variety of physical activities ranging from yoga to crossfit • Collaboration with recreation department is typically used as an adjunctive treatment support • An estimated time of 10 -24 weeks is needed per defined episode • Utilization of Job Corps own Youth 2 Youth program 6

Evidence-based treatment: Psychotherapy 7

Psychotherapy • Cognitive behavioral therapy (CBT): • evaluates, challenges, and modifies dysfunctional thoughts that maintain depression • largest weight of evidence for its efficacies • can be used as a monotherapy focusing on cognitive distortions • Interpersonal psychotherapy (IPT): • structured and brief intervention addressing social issues that maintain depression 8

Psychotherapy • Problem solving therapy (PST): • teaches to define problems, develop multiple solutions, and provide support • brief and supportive • Behavioral activation: • involves increasing pleasant activities or positive interactions between a person and his/her own environment 9

Evidence-Based Brief Intervention for Depressive Disorders • Job Corps is EAP model—brief therapy focused on employability • How do we help students most effectively within EAP model? • Brief Cognitive Behavioral Therapy (CBT): Empirically based, effective, time limited therapy (4 -8 sessions)—Targets key functional impacts of depression • Collaboration with center staff (counselors, RAs, education, trade, etc. ) • Referral off-center for ongoing/more extensive therapy • Referral to CP or off-center psychiatrist for medication, if indicated 10

Brief Cognitive Behavioral Therapy (CBT) • Psychoeducation about anxiety and CBT approach + setting specific therapy goals • Somatic/relaxation skills training: how to self-monitor depression, use muscle relaxation, diaphragmatic breathing, imagery, etc. • Cognitive: learn to identify and challenge negative thoughts, identify positive self-talk, realistic expectations • Exposure: imagined and in vivo gradual exposure to feared situations—impact of avoidance on maintaining anxiety and negatively impacting employability • Problem Solving: learning skills to recognize changeable problems and identify and implement solutions • Social skills/assertiveness/nonverbal skills training (often part of CBT for depressive disorders) • Relapse Prevention: review skills learned, anticipate problems/symptom recurrence, skills to use/when to reach out for help 11

Problem Solving Skills: Effective problem solving for situations that can change: SOLVED method 12

Pharmacological Treatments (antidepressants) • Most, if not all, major depressive disorders will require some form of medication support in order to achieve success in treatment • It is important to assist your client in obtaining an adequate medication evaluation and for you to maintain support especially through the initial portion of medication treatment • As a non-medical provider, it is strongly encouraged that you establish a relationship with the student’s medication provider so that you may coordinate treatment for optimal results • Pharmacological treatments will be covered in other webinars 13

Case Study: Major Depression 18 -year-old female comes to the clinic complaining of inability to sleep, appetite disturbance, low energy, and troubles in the classroom. She has reported depressive episodes in the past and is worried that she might be suffering from depression again. The treatment regimen best-suited for these complaints would be: a. CBT b. CBT as a monotherapy focusing on cognitive distortions c. PST d. Psychoanalysis 14

Disruptive Mood Dysregulation • Because of the newness of this diagnostic category, there are very few evidence-based treatment studies • Multiple studies exist on children ranging in age from 8 -16 with the cautionary note to avoid diagnosing children with bipolar disorder • Brief cognitive therapies would definitely be appropriate 15

Case Study: Disruptive Mood Dysregulation Disorder 19 -year-old female is referred from academics because of unruliness in the classroom, disrespectful language toward staff, social difficulties with peers, no one wants to room with her, unstable dating relationships and generalized lack of responsibility for her own actions. The best treatment regimen for this patient would be: a. CBT b. PST c. IPT d. Psychoanalysis 16

Bipolar I and Bipolar II • Bipolar I: The individual has experienced one or more episodes of mania. Most will have depression as well but not all. Episode must last at least 7 days or result in hospitalization • Bipolar II: A subset of Bipolar I during which individuals experience depressive episodes shifting back and forth with hypomanic episodes but never a full manic episode (more likely to be observed in the JC population than Bipolar I) 17

Differentiating between bipolar disorders • Bipolar I: Criteria must be met for at least one manic episode and depressive episode • Bipolar II: One or more major depressive episodes and at least one episode of hypomania, with possible periods of level mood between episodes • Cyclothymic disorder: Chronic, fluctuating mood disturbance involving numerous periods of hypomanic symptoms and periods of depressive symptoms • Substance/medication-induced bipolar and related disorders: Symptoms of bipolar associated with substance intoxication or withdrawal • Bipolar and related disorder due to another medical condition: Symptoms of bipolar associated with another medical condition • Other specified bipolar and related disorder: Symptoms of bipolar do not meet full criteria for any other disorder • Unspecified bipolar and related disorders: Same as above; used when clinician chooses not to specify reason criteria is not met 18

Teens and Young Adults with Bipolar disorder • Less than 5% of children and young adults experience bipolar disorder but its symptoms include an ongoing combination of highs and lows that occur more rapidly than in their adult counterparts. • Manic symptoms include severe changes in mood like silliness, irritability, unrealistic highs in self-esteem, talks too fast, too much and uninterruptible, distractible, and can engage in high risk behaviors such as jumping off a roof believing no harm can come. • Depressive symptoms include persistent sadness, loss of enjoyment, low energy, poor concentration, and changes in sleeping and eating habits. 19

Celebrities Suffering From Bi-Polar Disorder • Vincent Van Gogh (painter) • Dale Chihuly (glass artist) • Jimmy Piersall (major-league baseball player) • Patty Duke (actress, author) • Jonathan Winter (comedian) • Kay Redfield, M. D. (physician, author) 20
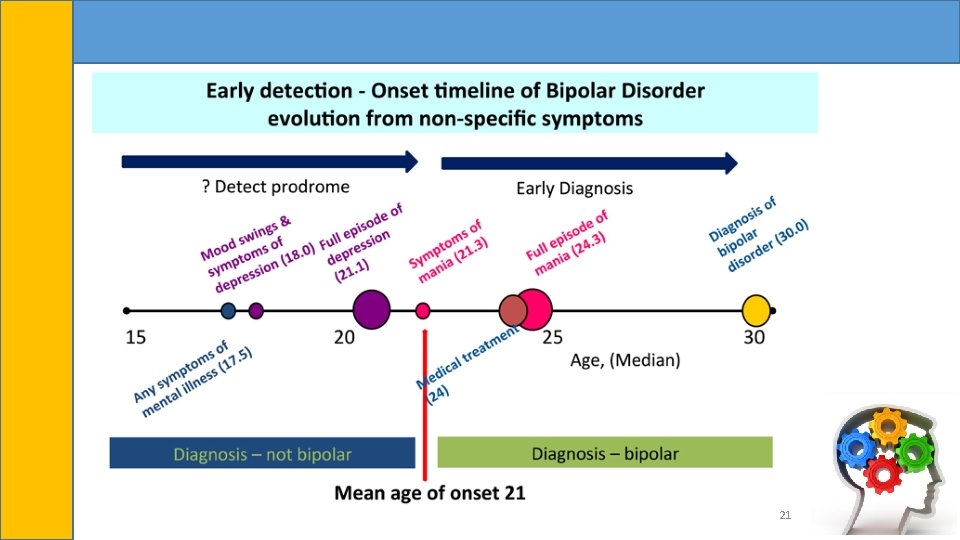
21

Treatment of Bipolar Disorder • Medications such as mood stabilizers, antipsychotics and antidepressants. • Psychotherapies such as cognitive behavioral therapy and familyfocused treatment. • Electroconvulsive therapy (ECT) • Self-management strategies and education. 22

Evidence-Based Treatment for Bipolar Disorder • Cognitive-based treatments are only effective when paired with a medication regimen • Behavioral therapies as outlined under major depressive disorders are basically the same 23

Evidence-Based Treatment for Bipolar Disorder: Myth or magic? • We use all of the same tools but we achieve more or less the same results over time “Since it is believed impossible to thrive in depression, mania, hallucination, and delusion, we are not taught how to thrive. We are instead taught only how to avoid the symptoms and live in fear that they might some day return. ” -Tom Wootton 24

Case study: Bipolar 21 -year-old male with established diagnosis of Bipolar II. He is currently relatively well managed with medication but needs guidance in everyday problem-solving and improvement of social skills. Evidence-based treatments might include: a. PST b. IPT c. CBT d. Psychoanalysis 25

Cyclothymic Disorder • Definition: Individuals experiencing mood cycling over a two year period, but have not met the diagnostic criteria for Bipolar I, Bipolar II, or Depressive disorder (please be careful to avoid ascribing “adult” symptoms to adolescents) • Symptoms include a two year period of hypomanic and depressive experiences, no history of diagnoses of manic, hypomanic, or depressive episodes, and are differentiated from medical and substance abuse conditions. They may impair social functioning. • Onset: Its prevalence is less than 1% of the population but does typically occur in adolescence and young adults. 26

Evidence-Based Treatments for Cyclothymic Disorder • These treatments are the same as noted for major depressive disorder • Cyclothymic disorder is frequently overlooked in young people because of they may have behavioral issues for other reasons (Van Meter and Youngstrom 2012) 27

Overview • We have just reviewed the role of evidence-based treatments relating to major depressive disorders and bipolar disorders and all of their relatives • Probably the single most important lesson for providers is to take a careful history and document it with any and all family history that is available to you • Secondly, and also terribly important is to forge an alliance with the medication prescribers whoever they may be. (For some this will be a psychiatrist, for many, this will be a family practitioner. ) • A combination of therapies will serve your client best 28

References • American Psychiatric Association (2014) Diagnostic and Statistical Manual of Mental Disorders (5 th edition). Washington, DC. • Cochrane Review (best evidence-based, standardized review available of more than 20 recent studies) Internet Mental Health. • Centers for Disease Control and Prevention (an overview of depression). • National Alliance on Mental Illness (NAMI) 29

References • Baldessarini, R. J. , and Vazques, G. Tondo, L. Treatment of Cyclothymic Disorder: Commentary. Psychotherapy Psychosomatic. 80: 131 -135. DOI: 10. 1159/000322234. • Bressert, S. 2016. Teens and Bipolar Disorder. Psych Central. Retrieved on October 14, 2016, from http: //psychcentral. com/lib/teens-and-bipolar-disorder/ • Van Meter, A. R, and Youngstrom, E. A. 2012. Cyclothymic disorder in youth: why is it overlooked, what do we know and where is the field headed? Neuropsychiatry 2(6): 509 -519. 30

References • www. nimh. nih. gov/health/statistics/prevalence/major_depressive_a dolesents, 2015_logo 148167. pdf • http: //psychcentral. com/lib/teens-and-bipolar-disorder/ • www. mdlinx. com/neurology/print-preview. cfm/690128 • https: //www. mentalhelp. net/articles/psychotherapy-evidence-based -treatments-for-major-depression/ 31

Self-Help Resources • Y 2 Y Job Corps www. Job. Corps. Y 2 Y. com • Support group locator: http: //www. dbsalliance. org/site/Page. Server? pagename=peer_supp ort_group_locator • https: //www. mentalhelp. net/articles/depression-major-depressionunipolar-varieties/ 32

33
- Slides: 33