Evidencebased Practice Choosing a Topic Triggers and Priorities

Evidence-based Practice: Choosing a Topic Triggers and Priorities Sally Kamai, RN, BSN, MBA-HCM Thanks to : Hawai‘i State Center for Nursing Marita G. Titler, Ph. D, RN, FAAN Rhetaugh Dumas Endowed Chair Department Chair Systems Populations and Leadership University of Michigan School of Nursing

Objectives Discuss considerations in selecting an EBP topic Demonstrate understanding of problemfocused and knowledge-focused triggers State factors involved in meeting organizational priority expectations
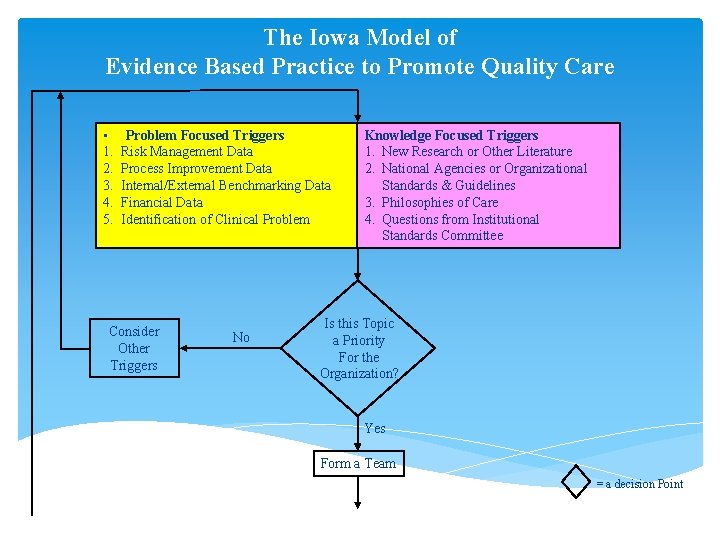
The Iowa Model of Evidence Based Practice to Promote Quality Care • 1. 2. 3. 4. 5. Problem Focused Triggers Risk Management Data Process Improvement Data Internal/External Benchmarking Data Financial Data Identification of Clinical Problem Consider Other Triggers No Knowledge Focused Triggers 1. New Research or Other Literature 2. National Agencies or Organizational Standards & Guidelines 3. Philosophies of Care 4. Questions from Institutional Standards Committee Is this Topic a Priority For the Organization? Yes Form a Team = a decision Point

How Do I Find a Topic? Ask: Is there a better method of clinical practice? Ask : Direct care givers Ask: What frustrates me every day at work? Ask: Why are we doing this way? What is the evidence?

Problem-focused Triggers Identify Clinical Problems Patient population Unit-specific? Discipline-specific? Procedures Identify operational problems Waste in system Flow issues Employee Engagement issues Efficiency Improvement needed ?

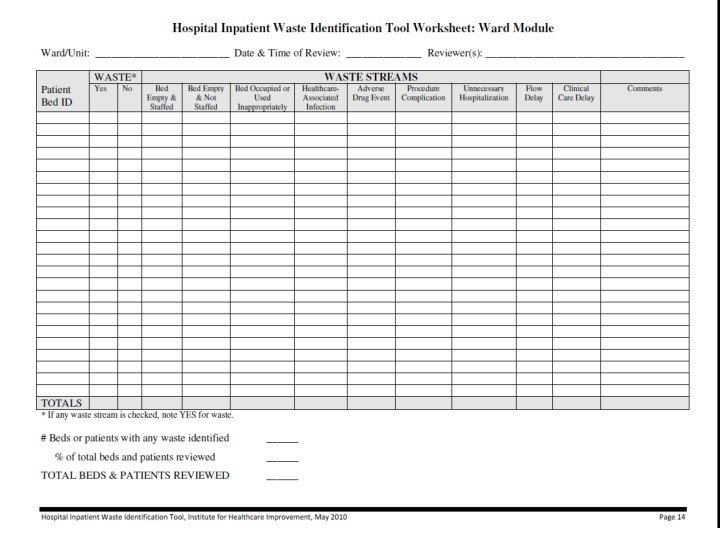
Where can I find the data? Risk Management Data Quality Improvement Data Internal/external benchmarking data Financial data Chart review Simple tally sheets Process maps Surveys

Knowledge –focused triggers New research or other literature National agencies, professional organizations, standards and guidelines Philosophies of care Questions from leadership, committees, surveying organizations (i. e. DOH or The Joint Commission)

Evidence-based Practice vs. “Doing It The Way We’ve Always Done It” Use of Trendelenburg position for hypotension Evidence: Head down position worsens shock, increases ICP, restricts ventilation, displaces only 1. 8% of total blood volume Keeping patient flat in bed is better!

Examples, continued Vital signs q 4 h at night on stable patients despite need for healing sleep Removing Urinary catheters only upon an MD order, when evidence has shown nurse-driven protocol is more efficient Continuing 12 hour shifts for nurses when research indicates adverse outcomes for nurses and patients Using Betadine prep for vaginal deliveries

Other Ways to Generate Topics Review quality and performance data Recurring clinical problems Adverse incident reports Review patient satisfaction data Surveys Creative thinking tools with staff

Creative Thinking Tools to Generate Topics Brainstorming at a staff meeting Graffiti board Running list of clinical issues Keep a list of great EBP topics for future Think tank of opportunities for improvement
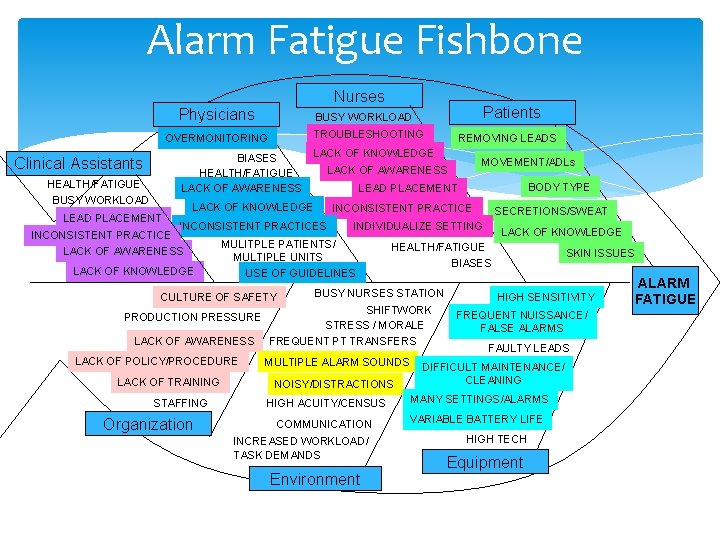
Alarm Fatigue Fishbone Nurses Physicians TROUBLESHOOTING OVERMONITORING BIASES HEALTH/FATIGUE LACK OF AWARENESS Clinical Assistants HEALTH/FATIGUE BUSY WORKLOAD LEAD PLACEMENT Patients BUSY WORKLOAD REMOVING LEADS LACK OF KNOWLEDGE MOVEMENT/ADLs LACK OF AWARENESS BODY TYPE LEAD PLACEMENT INCONSISTENT PRACTICE SECRETIONS/SWEAT INCONSISTENT PRACTICES INDIVIDUALIZE SETTING LACK OF KNOWLEDGE INCONSISTENT PRACTICE MULITPLE PATIENTS/ HEALTH/FATIGUE LACK OF AWARENESS SKIN ISSUES MULTIPLE UNITS BIASES LACK OF KNOWLEDGE USE OF GUIDELINES BUSY NURSES STATION CULTURE OF SAFETY SHIFTWORK PRODUCTION PRESSURE STRESS / MORALE LACK OF AWARENESS FREQUENT PT TRANSFERS LACK OF POLICY/PROCEDURE LACK OF TRAINING STAFFING Organization MULTIPLE ALARM SOUNDS NOISY/DISTRACTIONS HIGH SENSITIVITY FREQUENT NUISSANCE/ FALSE ALARMS FAULTY LEADS DIFFICULT MAINTENANCE/ CLEANING HIGH ACUITY/CENSUS MANY SETTINGS/ALARMS COMMUNICATION VARIABLE BATTERY LIFE INCREASED WORKLOAD/ TASK DEMANDS Environment 12 HIGH TECH Equipment ALARM FATIGUE
13
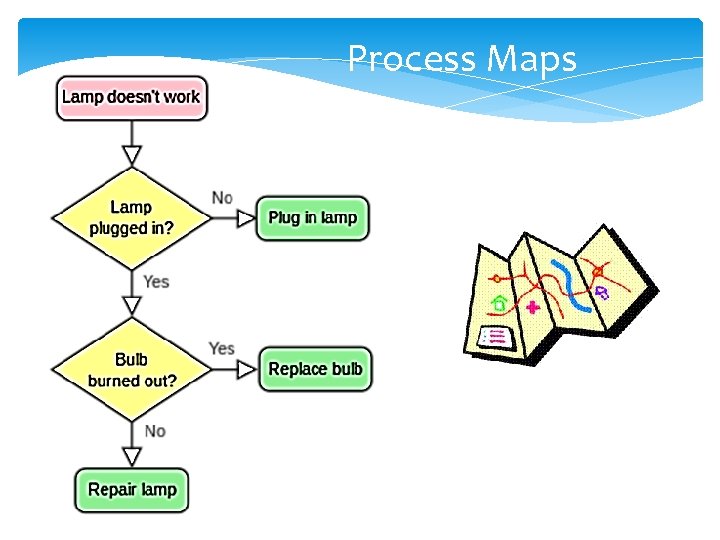
Process Maps 14
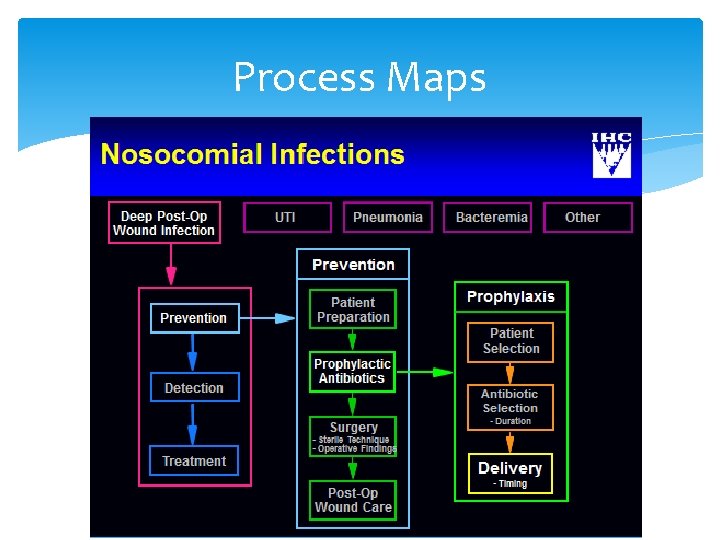
Process Maps 15
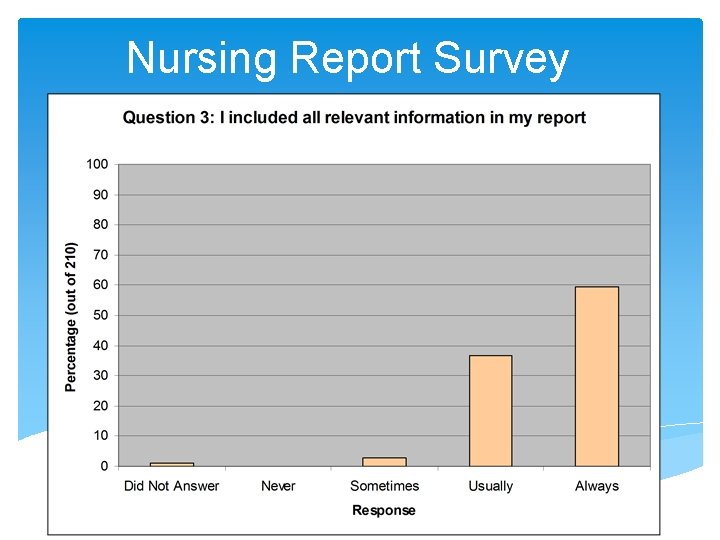
Nursing Report Survey 16
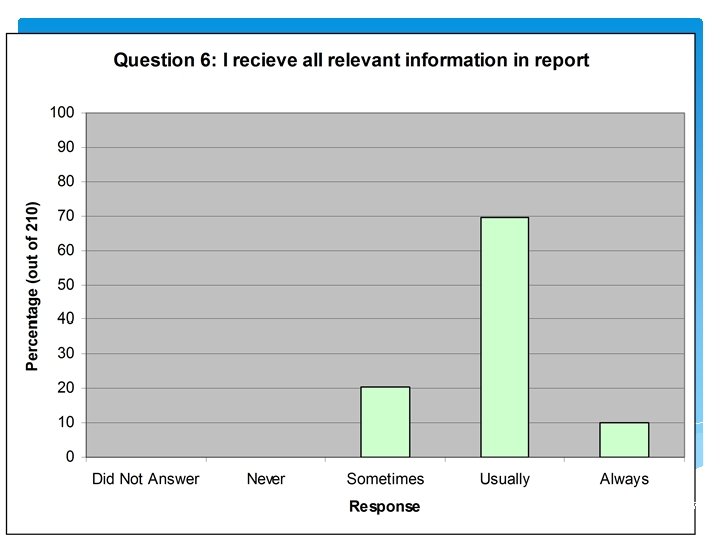
17
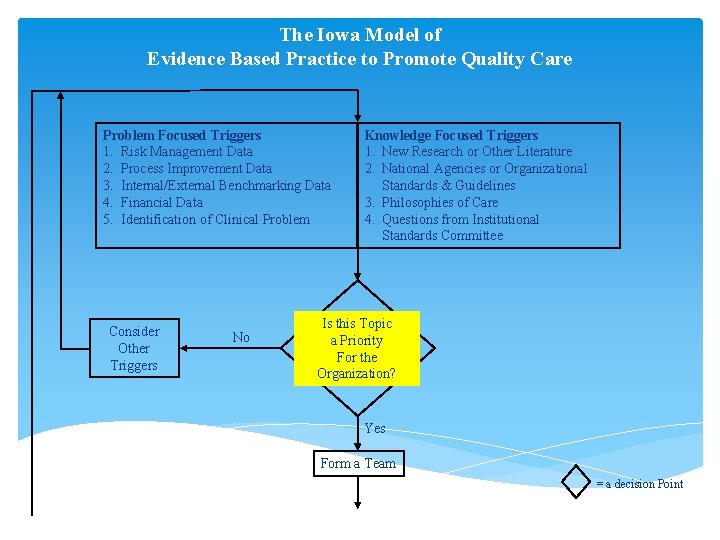
The Iowa Model of Evidence Based Practice to Promote Quality Care Problem Focused Triggers 1. Risk Management Data 2. Process Improvement Data 3. Internal/External Benchmarking Data 4. Financial Data 5. Identification of Clinical Problem Consider Other Triggers No Knowledge Focused Triggers 1. New Research or Other Literature 2. National Agencies or Organizational Standards & Guidelines 3. Philosophies of Care 4. Questions from Institutional Standards Committee Is this Topic a Priority For the Organization? Yes Form a Team = a decision Point

Is This Topic a Priority for the Organization?

Considerations for Organizational Priority for the organization – support mission, goals, current priorities? Priority for the department? Staff interest and commitment? Magnitude of the problem? Likelihood to contain costs and improve outcomes? “Landmines” and “sacred cows”? Applicability? Multidisciplinary?

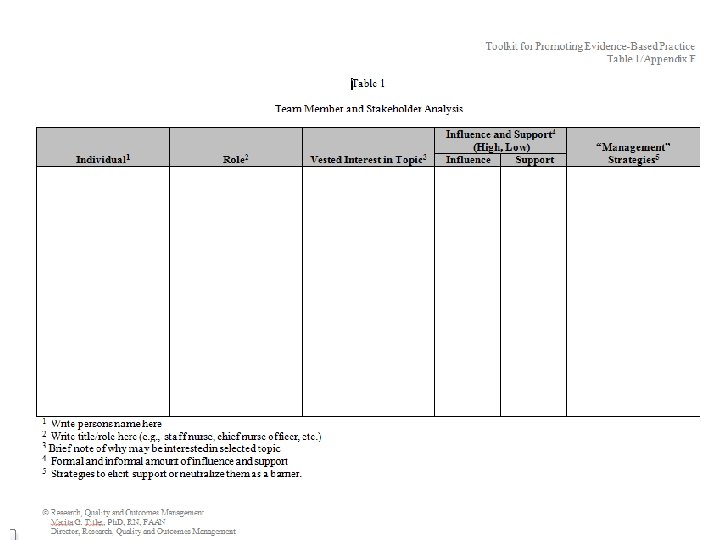
Tool to Use When Selecting a Topic

Forming a Team Sally Kamai, RN BSN, MBA-HCM Director, Clinical Improvement Hawai‘i Pacific Health Thanks To: Marita G. Titler, Ph. D, RN, FAAN Rhetaugh Dumas Endowed Chair Department Chair Systems Populations and Leadership University of Michigan School of Nursing Hawai‘i State Center for Nursing Evidence-based Practice Workshops Dr. Debra Mark

What is a Team? A group of people: with complementary skills committed to a common purpose and common performance goals/outcomes, Who hold themselves collectively responsible Leading Teams. Harvard Business School Press 2006 23

Benefits of a Team Broader knowledge base Greater creativity and perspective Shared risk Better problem -solving Shared workload More stimulating and motivating environment for work 24

Team membership Opinion Leader (s) APN – clinical expert Nurse Manager Users of the EBP Unit change champions Core group Physicians Colleagues from other disciplines depending on topic 25

Tips for selecting members Complementary mix of skills and problem solving abilities Decision-making skills Some with team experience Someone who is good at Excel!! Consider appointing a scribe or rotate scribes Choose for attitude, train for skills 26

Team formation Obtain leadership approval of team goals Keep team to 5 -7 members if possible, others can be “ad hoc” Have rules made by consensus, including attendance expectations Establish shared drive for info –sharing if possible Be clear about contributions and rewards A Team Charter can help 27

Team Stages Forming Storming Norming Performing

Team Leader or Project Director Designated leader or facilitator is key! Understands whole project and oversees process Keeps people on track, timelines, schedules Supports and guides members in achieving goals Fosters productive work relationships Liaison to leadership 29

Opinion leader Trusted to evaluate new information Respected and influential among peers Technically competent Dedicated member of group Believes in the idea, passionate about topic Example – A pediatric intensivist for NICU projects 30

Change Champions Informal leaders Expert clinicians Respected by team/co-workers Positive work relationships Committed to quality care AND your project! Persistent! Example – Experienced clinical ladder nurse 31
Mentor May help with most difficult steps Cheerleader for project to greater audience in organization Identify potential roadblocks and pitfalls in advance Provide expertise when needed Example : A supportive and influential manager or educator 32

Project Integration Team Who will help you with implementation on the “front lines” ? ? IT – Electronic medical record builds Nurse educators – orientation, on-going competency Unit managers Quality coordinators Physician colleagues Leaders in other disciplines 33

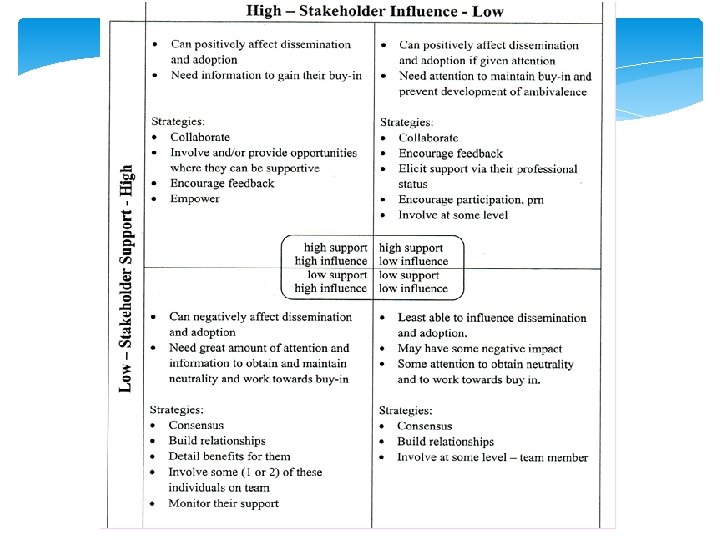
Stakeholder Analysis Matrix - Impact on dissemination and adoption Level of Support (high- to low) Level of Influence (High to low) Strategies for each combination Titler, M. G. (2002). Selection of a Topic for EBP: Appendix F/Figure 3. In Toolkit for Promoting Evidence-Based Practice. Iowa City, IA: RQ&OM, Department of Nursing Services and Patient Care, University of Iowa Hospitals and Clinics. 34
35

Stake Holder Analysis High influence/high support (e. g. nurse manager support of EBP topic) Low influence/high support (e. g. staff nurse enthusiastic of EBP topic) High influence/low support (e. g. new nurse manager not invested in EBP topic or EBP in general) Low influence/low support (e. g. staff nurse with minimal peer influence who is not enthusiastic of the EBP topic; “why do we need to change practice”) Titler, M. G. (2002). Selection of a Topic for EBP: Appendix F/Figure 3. In Toolkit for Promoting Evidence-Based Practice. Iowa City, IA: RQ&OM, Department of Nursing Services and Patient Care, University of Iowa Hospitals and Clinics. 36
37

Tips for Team success Keep leadership informed of progress Over-communicate to staff and managers Establish measurable outcomes Simple is usually better Establish a shared drive for literature-sharing 38

Tips for Team Success Have regular meeting times set up Start and stop on time Designate alternate team members Consider a team charter or written plan with timeline and deadlines Keep good records of processes 39

Your Turn !! Evaluate and discuss potential EBP topics Written Actions Plan : Topic Selection Tool

References and Thanks Dr. Marita Titler, Ph. D, RN, FAAN Rhetaugh Dumas Endowed Chair Department Chair Systems Populations and Leadership University of Michigan School of Nursing Hawai‘i State Center for Nursing Evidence Based Practice Workshop Dr. Debra Mark Leading Teams. Harvard Business School Press, 2006 41
- Slides: 41