EvidenceBased Practice and the Future of Nursing Suzanne

Evidence-Based Practice and the Future of Nursing Suzanne Prevost, RN, Ph. D Associate Dean for Practice University of Kentucky College of Nursing President-Elect – Sigma Theta Tau International

The Evolution of Evidence-Based Practice

What is - Evidence? Anything that provides material or information on which a conclusion or proof may be based; used to arrive at the truth, used to prove or disprove the point at issue. (Webster)

Evidence-Based Practice • Evidence-Based Practice – Conscientious, explicit and judicious use of current best evidence with clinical expertise, and patient values to make decisions about the care of patients. (Sackett, 2000) • Evidence-based nursing practice is the process of shared decision-making between practitioner, patient and significant others, based on research evidence, the patient’s experiences and preferences, clinical expertise, and other robust sources of information. (STTI , 2007)

• EBP is both a process and a product… requiring that the evidence which is produced – is also applied to practice. (D. Rutledge, 2002)

Evolution of EBP • 1991 – Evidence-based medicine -first described in the American College of Physicians Journal Club. • 1992 – the Evidence-based Medicine Working Group described it as a “paradigm shift” in JAMA – Clinical observations and experience, principles of pathophysiology, knowledge gained from authoritative figures, and common sense -- are no longer a sufficient guide for clinical practice, decision-making, or the development of practice guidelines

Evolution of EBP • Early 1990’s – US Prev. Services TF – began developing EB Guidelines for Screening and Prevention • 1992 – AHCPR (now AHRQ) – started publishing systematic reviews and consensus statements in the form of Clinical Practice Guidelines, starting with the guideline for Acute Pain, 19 guidelines were produced from ’ 92 -’ 96 • 1993 - the first annual Cochrane Colloquia was held at the New York Academy of Sciences • 1993 – Online Journal of Knowledge Synthesis for Nursing

Evolution of EBP 1997 – Jan 2011 – 198 Evidence Reports published by the EBP centers – May, 2005 – Episiotomy Use – “…no health benefits from episiotomy…routine use is harmful …”

Recent Evidence Reports 193. Alzheimer's Disease and Cognitive Decline 192. Lactose Intolerance and Health 190. Enhancing Use and Quality of Colorectal Cancer Screening 189. Exercise-induced Bronchoconstriction and Asthma 188. Impact of Consumer Health Informatics Applications 187. Treatment of Overactive Bladder in Women 185. Management of Ductal Carcinoma in Situ (DCIS) 184. Treatment of Common Hip Fractures 151. Nurse Staffing and Quality of Patient Care 140. Tobacco Use: Prevention, Cessation, and Control This is just one example of literature syntheses that are available to support EBP.

Nurse Staffing and Quality of Patient Care • Objectives: To assess how nurse to patient ratios and nurse work hours were associated with patient outcomes in acute care hospitals • Results: Higher RN staffing was associated with less mortality, failure to rescue, cardiac arrest, hospital acquired pneumonia, and other adverse events. Limited evidence suggests that the higher proportion of RNs with BSN degrees was associated with lower mortality and failure to rescue. More overtime hours were associated with an increase in hospital related mortality, nosocomial infections, shock, and bloodstream infections.

Evolution of EBP • 1998 – Evidence-Based Nursing journal debuted • 1999 – The UK Department of Health stipulated that, to enhance the quality of care, nursing, midwifery, and health visiting practice must be evidence-based • 2002 - JCAHO begins requiring monitoring of evidencebased core measures • 2004 – World. Views on Evidence-Based Nursing • 2004 – AACN began publishing “Practice Alerts”
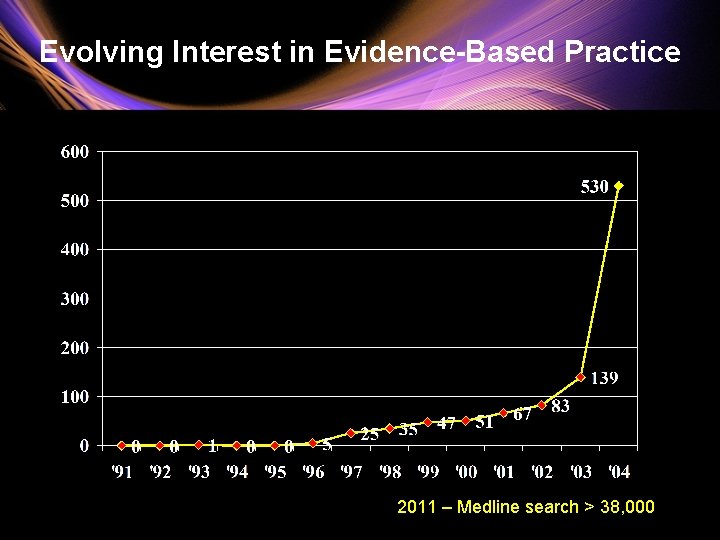
Evolving Interest in Evidence-Based Practice 2011 – Medline search > 38, 000

Within one decade, the concept of evidence-based practice has evolved and been embraced by nurses in nearly every clinical specialty, across a variety of roles and positions, and in locations around the globe. EBP – means many things to many people

Factors Contributing to Emphasis on Evidence-Based Nursing Practice • Scientific knowledge expansion – Knowledge expands exponentially q 2 yrs – 12 yrs. from now – 128 x as much knowledge • Knowledge availability -- The Internet • Highly educated nurses in clinical settings – APNs – focusing on evidence-based clinical problem-solving – Clinical Nurse Researchers – DNP Movement

Factors Contributing to Emphasis on Evidence-Based Nursing Practice • Aggressive pursuit of cost-effectiveness • Focus on quality of care, Risk & error reduction • Highly educated consumers • JCAHO/Accreditation expectations • Increased attention to institutional image – Magnet hospital movement

• Most nurses agree that EBP is important… but how do we make it happen?

What is the 1 st step toward EBP for the practicing nurse? • Asking good clinical questions • Nurses must be empowered to ask critical questions in the spirit of looking for opportunities to improve nursing care and patient outcomes • Risk-taking environment

Nursing vs. Medical Questions • Often more exploratory • Less frequently focused on intervention selection • Less evidence to support many nursing interventions • Most nursing interventions have less capacity for harm • Many nursing challenges often go beyond individual clinical interventions (e. g. nurse staffing, education, recruitment)

Clinical Nursing Questions • In postoperative patients, does prn or ATC analgesic administration yield better pain relief? • Among critically ill patients, is controlled or open visitation more effective in reducing patient anxiety?

Questions for APNs • In acute care hospitals, is the CNS more effective by focusing on a specific patient population or a specific unit? • What else?

What kind of questions might the Nurse Manager ask? • On medical-surgical units, do 12 hour or 8 hour shifts result in more medication errors?

Key Questions to Ask When Considering EBP • • Why have we always done “it” this way? Do we have evidence-based rationale? Or, is this practice merely based on tradition? Is there a better (more effective, faster, safer, less expensive, more comfortable) method? • What approach does the patient (or the target group) prefer? • What do experts in this specialty recommend?

Key Questions to Ask When Considering EBP • What methods are used by leading/benchmark, organizations? • Do the findings of recent research suggest an alternative method? • Are organizational barriers inhibiting the application of best practices in this situation? • Is there a review of the research on this topic? • Are there nationally recognized standards of care, practice guidelines, or protocols that apply?

Steps in the EBP Process • Developing a well-built question • Finding evidence-based resources to answer the question • Evaluating the strength and applicability of the evidence • Applying the evidence to practice • Evaluating the effects

• Once we agree upon the question that poses an opportunity for improvement, then we must find the evidence • Where should we look? • Are all forms of evidence equivalent in quality?

Strength of Evidence • • • Level I - meta-analysis of multiple studies Level II - experimental studies, RCTs Level III - quasiexperimental studies Level IV - nonexperiemental studies Level V - case reports, clinical examples AHCPR/AHRQ • At what level is most nursing evidence?

AACN Levels of Evidence • Level A (Armola, et al. , C C Nurse, 2009) • Meta-analysis or metasynthesis of multiple controlled studies, supporting a specific action • Level B • Controlled, randomized, or nonrandomized studies, supporting a specific action • Level C • Qualitative, descriptive or correlational studies or systematic reviews with consistent results • Level D • Peer-reviewed prof. organ. standards with studies to support them • Level E • Theory-based evidence from expert opinion or case studies • Level M • Manufacturer’s recommendations only

What constitutes the “Evidence” in Evidence-Based Practice? “Evidence-based practice has been defined as the use of the best clinical evidence from systematic research (referring to meta -analysis, integrated reviews, & RCTs – as the gold standard). …Others (often nurses) believe that experimental studies, observational studies, and correlational studies are also suitable evidence. ” C. Goode, Applied Nursing Research, 2000

University of Colorado Multidisciplinary Evidence-Based Practice Model • Emphasizes that all types of research can be evaluated for their contribution • Recognizes the use of 9 non-research sources of evidence: – Pathophysiology, Retrospective or Concurrent Chart Review, Quality Improvement or Risk Data, International and Local Standards, Infection Control Data, Clinical Expertise, Benchmarking Data, Cost. Effectiveness Analysis, and Patient Preferences

A major dilemma for the practicing nurse: Finding the time, access, and research expertise that are needed to search and analyze the evidence to find answers to their clinical questions. For those of you who are already pursuing EBP, which of these issues pose the greatest challenges for you?

Finding the Evidence • Don’t reinvent the wheel • If other experts have reviewed the evidence on your topic … start there

Preprocessed Evidence (A. Di. Censo, 2009)

Resources to Support Evidence-Based Practice • • Government agencies Cochrane Collaboration Professional Organizations Benchmark Institutions
AHRQ – Agency for Healthcare Research and Quality

Cochrane Collaboration • “an international, independent, not-for-profit organization of over 27, 000 contributors from more than 100 countries, dedicated to making up-to-date, accurate information about the effects of health care readily available worldwide. • Contributors produce systematic assessments of healthcare interventions, known as Cochrane Reviews, which are published online in The Cochrane Library. • Rely heavily on RCTs • Primarily focused on effectiveness of interventions, more medical and pharmaceutical than nursing
Cochrane Collaboration http: //www. cochrane. org

Substitution of Drs by Nurses in Primary Care Objectives: to evaluate the impact on patient outcomes, processes of care, and costs. Outcomes included: morbidity; mortality; satisfaction; compliance; and preference. Studies were included if nurses were compared to doctors providing a similar primary health care service. Doctors included: general practitioners, family physicians, pediatricians, internists or geriatricians. Nurses included: nurse practitioners, clinical nurse specialists, or advanced practice nurses. Results: 4253 articles were screened, 25 articles met our inclusion criteria. No appreciable differences were found between doctors and nurses in health outcomes, processes of care, or cost; but patient satisfaction was higher with nurse-led care.

Professional Nursing Organizations Supporting Evidence-Based Practice • • • AACN AWHONN AORN ONS Sigma Theta Tau

Am. Assoc. of Critical Care Nurses Succinct dynamic directives…supported by evidence to ensure excellence in practice and a safe and humane work environment. • • • Venous Thromboembolism Prevention Oral Care in the Critically Ill Noninvasive BP Monitoring Verification of Feeding Tube Placement Ventilator Associated Pneumonia Dysrthymia Monitoring • Published since 2005 • Available free on AACN website • Include ppt presentations and audit tools

Oncology Nursing Society • EBP Resource Center • http: //onsopcontent. ons. org/toolkits/evidence/ • Also provides topical toolkits, on specific topics, plus: • How To Find The Evidence • How To Critique Evidence • How To Develop An Evidence Based Presentation • Evidence Based Practice Education Guidelines • Evidence on Clinical Topics • How to Change Practice • Levels of Evidence Table

Sigma Theta Tau EBP Initiatives • Strategic Plan • Online Resources – NKI http: //www. nursingknowledge. org > 200 resources for EBP – some free, some for purchase • New Award for EBP (formerly Clin Scholarship) • Conferences – – International EBP and Research Congress July, 2010 – Orlando July, 2011 – Cancun July, 2012 – Australia

Journals Supporting EBP – – Evidence-Based Nursing Online Journal of Clinical Innovations World. Views on Evidence-Based Nursing The Online Journal of Knowledge Synthesis for Nursing – (archived, no longer being published) – Reflections on Nursing Leadership (Vol 28, 2)

Local vs. Global Evidence • Institutional/Local > National/International – CPI Data/Research Results – Standards & Protocols/Practice Guidelines – Expert Advice – Patient/Family Preferences

Values and Preferences EBN - integration of the best evidence available, nursing expertise, and the values and preferences of the individuals, families and communities … Yasmin Amarsi, RNL, 2002: “The crux is to ensure that EBN attends to what is important to nursing and that caring is not sacrificed on the altar of scientific evidence. ”

Amy’s Blog • I consulted a well-regarded oncologist in New York. After the tests she regretfully informed me that my disease was not curable. She recommended an evidence-based course of medications aimed at slowing the progression. Before I committed, I wanted a second opinion. I secured an appointment with the pre-eminent researcher/ clinician in inflammatory breast cancer. … • The building was beautiful, the staff attentive. …I had no doubt that the care would be top-notch. • Everything changed when I sat down with the physician. He never asked about my goals for care. He recommended an aggressive approach of chemotherapy, radiation, mastectomy, and more aggressive chemotherapy. My doctor in New York had said this was the standard, evidence-based protocol for patients in Stage III B…But since I am in Stage IV (with mets) she said I wouldn’t get the benefit of this aggressive, curative approach.

• “All of my patients use this protocol, ” he said. • I was shocked. “Does this mean I could get better? ” I asked. • “No, this is not a cure. ” he answered. “But if you respond to the treatment, you might live longer, although there are no guarantees. ” • My goals are to maximize my quality of life so I can live, work, and enjoy my family … Would I undergo a year or more of grueling, debilitating treatment only to live with spinal fractures if the cancer progressed? … Would I get the possibility of quantity and no quality? • I pressed him. “Why do the mastectomy? If the cancer has already spread to my spine. You can’t remove it. ” • His brow furrowed. “Well, you don’t want to look at the cancer, do you? ” He made it sound like cosmetic surgery. • Right now, I feel fine. I can work. I am pain free. Did I want to trade that for a slim chance of a little extra time (no guarantees, of course)?

• “But what about the side effects of radiation? ” I asked. “I’ve heard they are terrible. ” • He frowned and seemed annoyed by my questions. “My patients don’t complain to me about it, ” he replied. • Inwardly, I shook my head. Of course his patients never complained to him. Most of them were probably unaware that less aggressive treatments were viable options. To me, there were real drawbacks. Undergo aggressive therapy that might buy me a longer life…at what cost? I might never recover my health for the limited period of time I have. • This doctor, top in his field, was reflecting the bias of our medical system towards focusing (evidence-based) survival. He was focused only on quantity and forgot about quality.

• The patient’s goals and desires, hopes and fears, were not part of the equation. He was practicing one-size-fits-all (cookbook? ) medicine that was not going to be right for me, even though scientific studies showed it was statistically more likely to lengthen life. • Based on a perverse set of metrics, this oncologist was offering technically the “best” care America had to offer. • Yet this good care was not best for me. It wouldn’t give me health. Instead, it might take away what health I had. It doesn’t matter if care is cutting-edge, technologically advanced, (and evidence-based); if it doesn’t take the patient’s goals into account, it may not be worth doing.

• I returned to my original New York oncologist. • I was determined not only to choose treatment that would maximize the healthy time I had remaining, but also to use that time to call on our health care institutions and professionals to make a real commitment to listening to their patients.

Moving Toward our Destiny Evidence-based practice is every nurses’ responsibility What can you do to make this goal a reality?

Educator’s Role – EB Education for EB Practice – Base educational content on evidence – Seek the most current forms of evidence, e. g. journals & online sources vs. texts – Encourage students to question and challenge – Teach research content in a manner that is interesting and useful

Manager/Administrator’s Role – Encourage inquisitive minds – Promote risk-taking and flexibility in the clinical environment – Incorporate EBP activities into performance evals – Provide time & resources – unit internet access – Provide support personnel – Empower staff to make EB practice changes – Acknowledge and reward EB improvements

Researcher’s Role – Remain clinically in touch – Conduct clinically useful studies – Support clinicians in accessing and synthesizing the evidence – Collaborate with clinicians and patients – Disseminate findings that are understandable and accessible – Emphasize clinical implications

Nurse Clinician’s Role – “Worry and Wonder” – Be the Inquiring Mind – Question clinical traditions – Stay abreast of the literature - guidelines – Find your niche – and become the expert – Collaborate with APNs & researchers – Be an advocate for evidence-based changes – LISTEN to your PATIENTS – to guard patient & family preferences

Join us: STTI Research & EBP Congress July 11 -14, 2011

THE 2010 IOM REPORT ON THE FUTURE OF NURSING 59
Center to Champion Nursing in America http: //championnursing. org • Center to Champion Nursing in America is an initiative of AARP, the AARP Foundation and the Robert Wood Johnson Foundation. The Center, a consumer-driven, national force for change, works to increase the nation’s capacity to educate and retain nurses who are prepared and empowered to positively impact health care access, quality, and costs.

Nursing has an unprecedented opportunity to have one voice on behalf of patient care… • 18 member committee – Donna E. Shalala (Chair), President, University of Miami – Linda Burns Bolton (Vice Chair), Vice President and Chief Nursing Officer, Cedars-Sinai Health • Evidence based • IOM part of National Academy of Sciences – Private, nonprofit, society of distinguished scholars engaged in scientific research, dedicated to the furtherance of science and technology and to their use for the general welfare 61

Interprofessional Team-Based Competencies • IPEC Expert Panel Presentation • HRSA, Macy Foundation, Robert Wood Johnson Foundation, and ABIM Foundation • • Amy Blue, Ph. D Jane Kirschling, DNS, RN, FAAN Madeline Schmitt, Ph. D, RN, FAAN-Chair Thomas Viggiano, MD, MEd 62
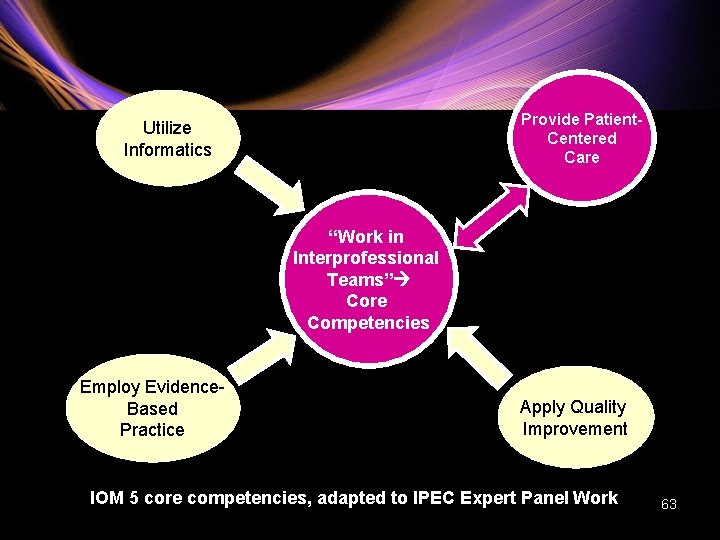
Provide Patient. Centered Care Utilize Informatics “Work in Interprofessional Teams” Core Competencies Employ Evidence. Based Practice Apply Quality Improvement IOM 5 core competencies, adapted to IPEC Expert Panel Work 63

Institute of Medicine October 2010 Report: The Future of Nursing Leading Change, Advancing Health 1. Remove scope-of-practice barriers 2. Expand opportunities for nurses to lead and diffuse collaborative improvement efforts 3. Implement nurse residency programs 4. Increase the proportion of nurses with a baccalaureate degree to 80% in 2020 5. Double the number of nurses with a doctorate by 2020 6. Ensure that nurses engage in lifelong learning 7. Prepare and enable nurses to lead change to advance health 8. Build an infrastructure for the collection and analysis of interprofessional health care workforce data

IOM Key Message RECOMMENDATION NO. 1 Nurses • Remove should scope-ofpractice to practice the full barriers extent of their education & training 65

The many faces of advanced practice registered nurses in 2011 High quality, safe, affordable health care provided by teams of health care professionals

Health care reform • Survey published in JAMA 2008, only 2% fourthyear medical students plan to work in general internal medicine (primary care) after graduation, despite need for 40% increase in number of primary care physicians in the U. S. by 2020 • Association of American Medical Colleges predicts shortage of 35, 000 -44, 000 primary care physicians by 2025 • Expanded opportunities for APRNs 67

Hospital care… • Evolution of opportunities for advanced practice registered nurses – Change in residency hours – 24 x 7 coverage – Evolving recognition of specialty needs 68
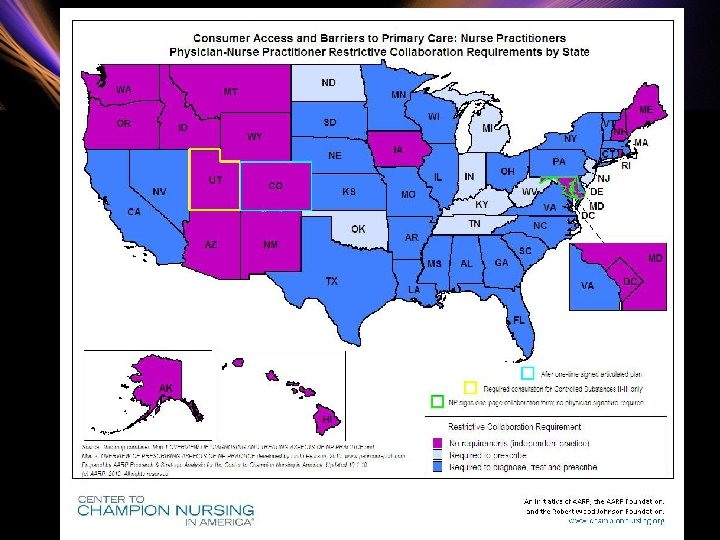
69

National barriers • National nursing organizations are working to § Improve APRN reimbursement, Medicare reimburses NPs and CNSs at 85% of physician rate § Amend rules that prohibit APRNs from ordering such things as home health and hospice services or diabetic shoes

Recent national advances Medicare now – Allows NPs to serve as the attending for a hospice patient – Allows Governors of states to opt out of supervision rule for CRNAs – 16 states have opted out – Reimburses CNMs at 100%

“Messaging” ü Barriers to practice reduce access to care ü Main issue is access to care and this should define our focus

IOM Key Message Nurses should achieve higher levels of education & training through an improved education system that promotes seamless academic progression RECOMMENDATION NO. 3 • Implement nurse residency programs New graduates and nurses in transition 73

The Problem – Transition to Practice: Promoting Public Safety • 35 to 60% new nurses leave position in first year of practice, estimated replacement cost $46, 000 to $64, 000 per nurse • 10% typical hospital’s nursing staff comprised of new graduates • New nurses experience increased stress 3 -6 months after hire, increased stress levels are risk factors for patient safety and practice errors

• NCSBN – transition programs reduce 1 st year turnover from 35 -60% to 6 -13%, results in positive return on investment from 67 to 885%

University Healthsystem Consortium (UHC) and American Assoc. of Colleges of Nursing A one year education and support program to assist new BSN graduates employed as staff nurses on clinical units to transition to professional nursing practice Now 54 sites nationwide in 25 states › Over 12, 000 BSNs have been enrolled nationwide National research component to determine the best practice for integrating new BSN nurses into the workforce
What is the Residency Research Showing? Retention nationally 94. 4% for new grad first year vs. about 73% without residency Surveys completed initially, 6 months, and 12 months; scores improve in new graduate’s ability to › organize and prioritize › communicate and be leaders at bedside › decreased stress over the year (less so at Kentucky)

IOM Key Message Nurses should achieve higher levels of education & training through an improved education system that promotes seamless academic progression RECOMMENDATION NO. 4 • Increase the proportion of nurses with a baccalaureate degree to 80% by 2020 78

Rationale (Institute of Medicine, 2011, p. 169 -170) “Several studies support significant association between educational level of RN and outcomes for patients in acute care settings, including mortality” 79
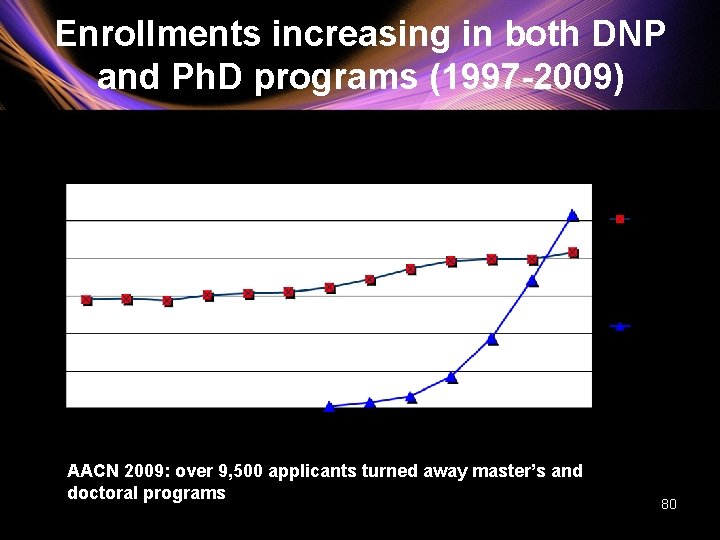
Enrollments increasing in both DNP and Ph. D programs (1997 -2009) AACN 2009: over 9, 500 applicants turned away master’s and doctoral programs 80

IOM Key Message Nurses should achieve higher levels of education & training through an improved education system that promotes seamless academic progression RECOMMENDATION NO. 6 • Ensure that nurses engage in lifelong learning 81

Faculty partner with health care organizations • Develop and prioritize competencies so curricula updated regularly across all programs – go beyond task-based proficiencies to higherlevel competencies • demonstrate mastery over care management knowledge domains • provide foundation decision-making skills under variety clinical situations across care settings 82

Academic administrators • Require all faculty – participate continuing professional development – Perform cutting-edge competence in practice, teaching, and research 83

Health care organizations and schools of nursing • Foster culture of lifelong learning • Provide resources for interprofessional continuing competency programs • If offer continuing competency programs, regularly evaluate for flexibility, accessibility, and impact on clinical outcomes 84

Institute of Medicine October 2010 Report: The Future of Nursing Leading Change, Advancing Health 2. Expand opportunities for nurses to lead and diffuse collaborative improvement efforts 7. Prepare and enable nurses to lead change to advance health 8. Build an infrastructure for the collection and analysis of interprofessional health care workforce data 85

…IN CONCLUSION ü We must commit to take action on recommendations from IOM report ü Affirm that this is about access to patient-centered care and health care reform ü Essential that nurses mobilize ü Not just to support nursing, but more importantly – to support the public 86
- Slides: 86