EvidenceBased Medicine and the Chinese Medicine Profession AN

Evidence-Based Medicine and the Chinese Medicine Profession AN EXPLORATION OF ATTITUDES AND BELIEFS IN RELATION TO EDUCATION AND CULTURAL CHANGE Belinda Anderson, Ph. D, LAc Academic Dean, Pacific College of Oriental Medicine (New York) Associate Professor, Albert Einstein College of Medicine Acupuncturist and Chinese Herbalist, New York University Fertility Center

Content � Brief history of how PCOM-NY got involved with research � Current externally funded research projects � NIH funded 5 -year Evidence Informed Practice research project � Pilot pre-grant data � Qualitative exploration of attitudes, beliefs and perspectives � Scientific worldview differences between MD and PCOM students � Conclusions and lessons learned

Brief History � My research background/history � � The NESA/Harvard NIH grant Partnering with Einstein � Interprofessional student exchange program � Faculty appointment � 3 externally funded research grants

Current Research Projects � � NIH National Center for Complementary and Integrated Health � K 07 Career development award � Evidence Informed Practice: Faculty and Curriculum Development � 2013 – 2018 Patient Centered Outcomes Research Institute (PCORI) � Acupuncture clinical trial � 2015 - 2018 Health Resources and Services Administration (HRSA) � Residency training program in wellness and prevention � 2015 – 2018 Council of Colleges for Acupuncture and Oriental Medicine � Investigating the scientific worldview differences between MD and PCOM students � 2016 - 2017

NIH EIP Project

Components � EIP skills/knowledge � Students � Developed a Foundations of EIP (FEIP) course – in all CM programs � Pre and post tested self-reported skills/knowledge and importance � Faculty � Online EIP modules – University of Minnesota � FEIP course in doctoral upgrade program � Incorporating EIP into 70% of didactic entry-level CM curriculum � Incorporating EIP into 100% of clinical entry-level CM curriculum � Attitudes/beliefs/perspectives � Pre-grant pilot data � Qualitative study

NIH EIP Project – Pilot Data � Surveys undertaken to provide data for the NIH proposal � Exploring faculty and student’s � Research skills and usage � Support for research � Attitudes, beliefs and perspectives about evidence-based medicine
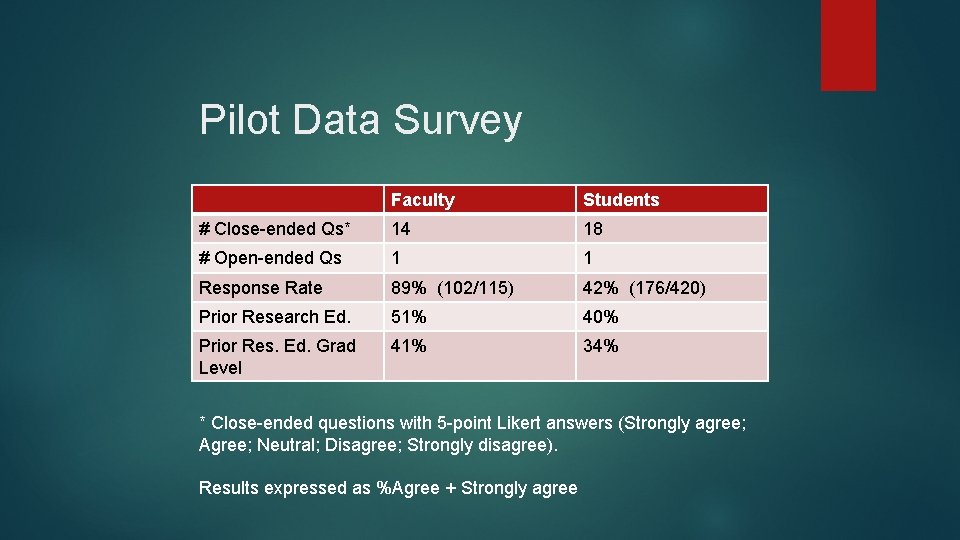
Pilot Data Survey Faculty Students # Close-ended Qs* 14 18 # Open-ended Qs 1 1 Response Rate 89% (102/115) 42% (176/420) Prior Research Ed. 51% 40% Prior Res. Ed. Grad Level 41% 34% * Close-ended questions with 5 -point Likert answers (Strongly agree; Agree; Neutral; Disagree; Strongly disagree). Results expressed as %Agree + Strongly agree
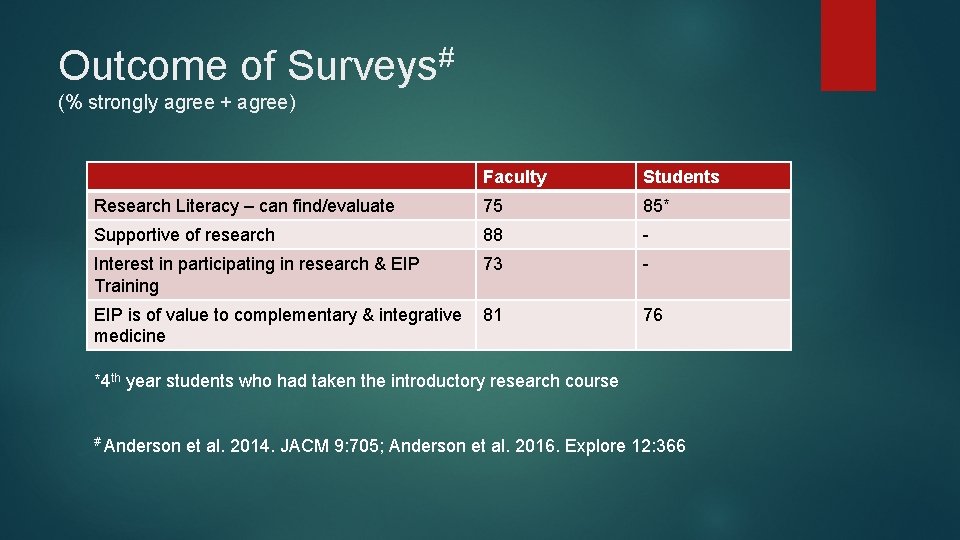

# Outcome of Surveys (% strongly agree + agree) Faculty Students Research Literacy – can find/evaluate 75 85* Supportive of research 88 - Interest in participating in research & EIP Training 73 - EIP is of value to complementary & integrative 81 medicine 76 *4 th year students who had taken the introductory research course # Anderson et al. 2014. JACM 9: 705; Anderson et al. 2016. Explore 12: 366
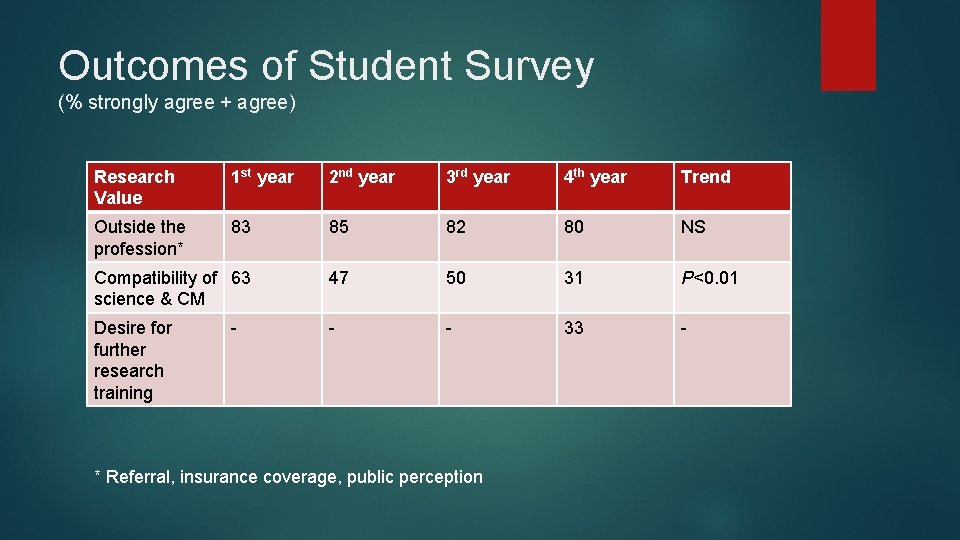
Outcomes of Student Survey (% strongly agree + agree) Research Value 1 st year 2 nd year 3 rd year 4 th year Trend Outside the profession* 83 85 82 80 NS Compatibility of 63 science & CM 47 50 31 P<0. 01 Desire for further research training - - 33 - - * Referral, insurance coverage, public perception
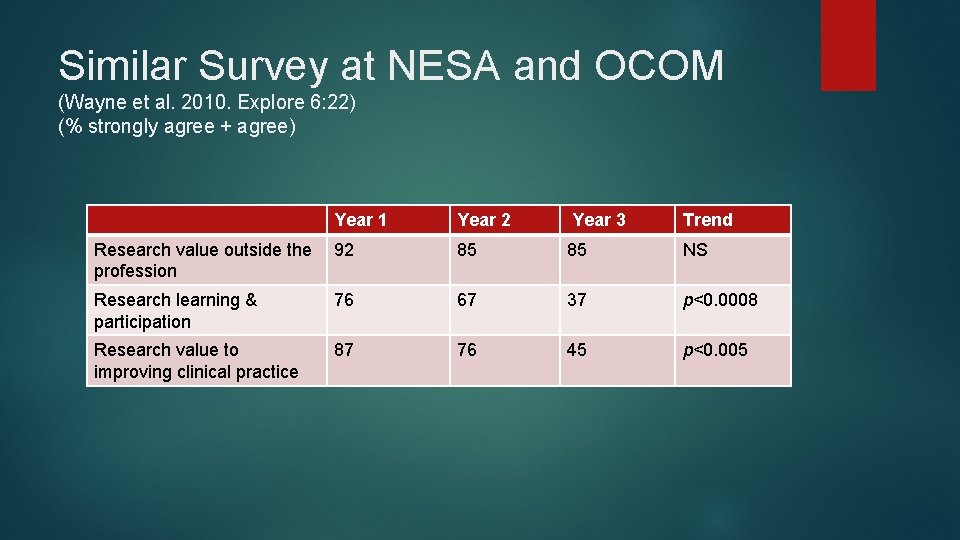
Similar Survey at NESA and OCOM (Wayne et al. 2010. Explore 6: 22) (% strongly agree + agree) Year 1 Year 2 Year 3 Trend Research value outside the 92 profession 85 85 NS Research learning & participation 76 67 37 p<0. 0008 Research value to improving clinical practice 87 76 45 p<0. 005

Challenges Going in � Resistance – themes from open-ended survey questions � Incompatible paradigms � Cooptation � Relevancy to CM practice � Cultural issues � These issues were not highlighted by the faculty needs analysis using the instrument developed at Northwestern Health Sciences University � Suspected unique challenges within CM profession

Qualitative study

Qualitative Study � First cohort taking Fundamentals of Evidence Informed Practice as part of the doctoral upgrade program (DACM) � Average years in practice 11. 5 � Analysis of online forums � Based on Kaptchuk and Miller (2005). What is the most ethical model for the relationship between mainstream and alternative medicine: opposition, integration or pluralism? Academic Medicine. 2005, 80: 286 -290 � They were asked to discuss the most ethical model for the relationship between mainstream and alternative medicine � 31 of 33 students participated � There were 33 initial posts (average 428 words/post), 127 response posts (average of four responses/initial post, with average length of response of 108 words).

Opposition/Integration/Pluralism (Kaptchuk & Miller 2005) � Opposition - rejection of alternative medicine by conventional medicine � Integration - amalgamating conventional and alternative therapies together in a holistic approach to the treatment of disease and promotion of wellness � Pluralism - conventional and alternative therapies used together, but where cooperation, research, and open communication and respect between practitioners preserves the integrity of each of the treatment systems
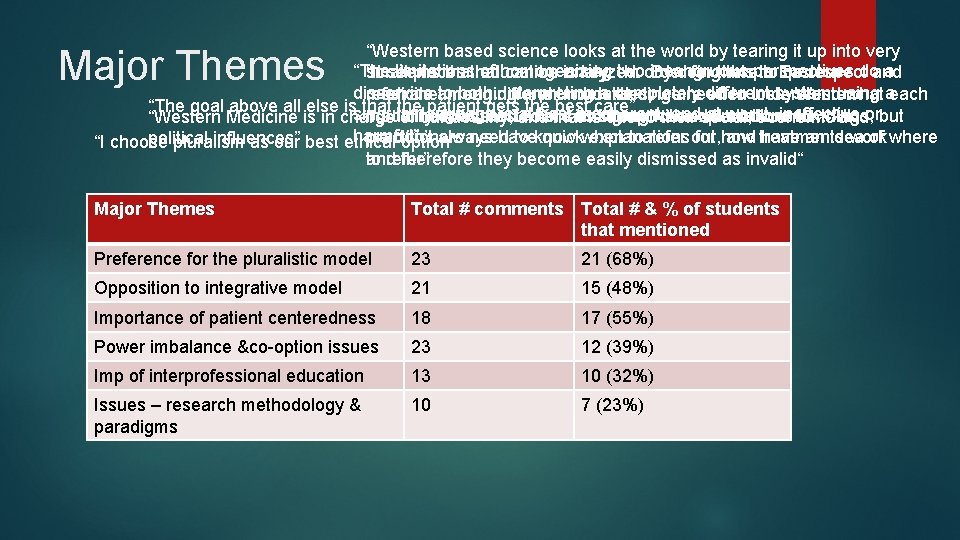
“Western based science looks at the world by tearing it up into very “The limitations of homogenizing two incongruous perspectives do a small pieces that can be analyzed. By doing this to Eastern “It seems that education is key. In order for there to be respect and disservice to both. Interpreting a completely different system using a medicine, meaning and understanding are often lost. Western referrals among different modalities, we need to understand what each “The goal above all else is that the patient gets the best care” singular language is at best incoherent, and at worst, ineffective or medicine is interested in coming up with explanations for things, but modality does, and where its strengths and limitations lie. All “Western Medicine is in charge of our destiny, and that is due to their social, economic and harmful”. we don’t always have quick explanations for how treatments work practitioners need to know when to refer out, and have an idea of where political influences” “I choose pluralism as our best ethical option” and therefore they become easily dismissed as invalid“ to refer” Major Themes Total # comments Total # & % of students that mentioned Preference for the pluralistic model 23 21 (68%) Opposition to integrative model 21 15 (48%) Importance of patient centeredness 18 17 (55%) Power imbalance &co-option issues 23 12 (39%) Imp of interprofessional education 13 10 (32%) Issues – research methodology & paradigms 10 7 (23%)
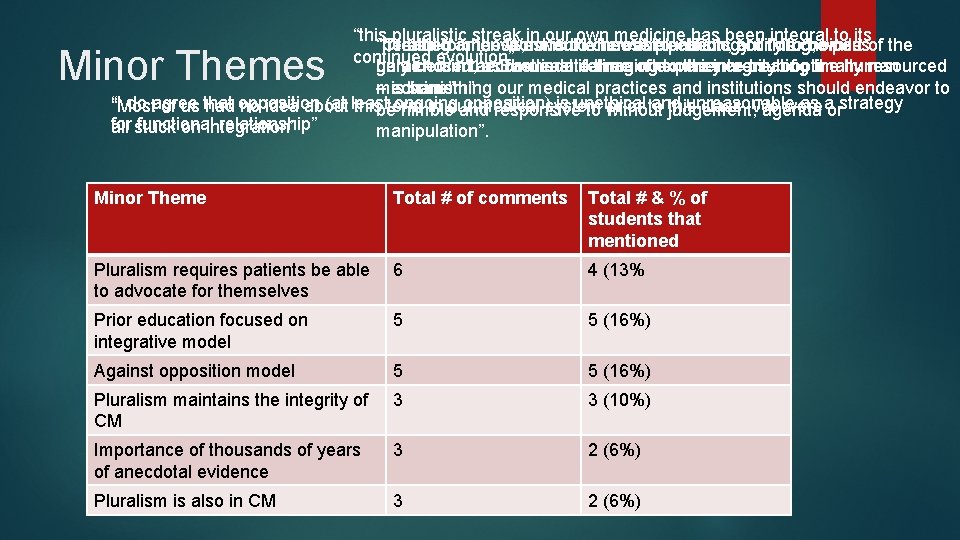
“this pluralistic streak in our own medicine has been integral to its “Creating an environment where the patients ability to be part of the “If I had to choose, I would choose pluralism, but this choice is “heralded in the West is the newest technology or drug, while continued evolution” game – and accommodate them when they are sub optimally resourced only chosen, as the least damaging to the integrity of our heralded in the East is a lifetime of experience treating the human – is something our medical practices and institutions should endeavor to medicine” mechanism” “I do agree that opposition (at least ongoing opposition) is unethical and unreasonable as a strategy “Most of us had no idea about this term in our medical system prior to this class. We were be nimble and responsive to without judgement, agenda or functional relationship” all stuck on integration” manipulation”. Minor Themes Minor Theme Total # of comments Total # & % of students that mentioned Pluralism requires patients be able to advocate for themselves 6 4 (13% Prior education focused on integrative model 5 5 (16%) Against opposition model 5 5 (16%) Pluralism maintains the integrity of CM 3 3 (10%) Importance of thousands of years of anecdotal evidence 3 2 (6%) Pluralism is also in CM 3 2 (6%)

Scientific Worldviews

Survey Instrument � Validated - Thinking about Science Survey Instrument – Cobern 2000 SLCSP 151. Kalamazoo, MI: Scientific Literacy and Cultural Studies Project � Designed to measure differences in scientific worldviews - socio-cultural resistance to, and support for, science � The instrument consists of 60 questions with 5 -point likert scale answers � Categories of Qs - epistemology; science and economy; science and the environment; public policy and science; science and public health; science, religion and morality; science, emotions and aesthetics; science, race and gender; and science for all

Research Questions � Do MD and CM students have different scientific worldviews? � Do students who chose, or not, to participate in the interprofessional exchange program have different scientific worldviews? � Does an inter-professional student education exchange program change their scientific worldviews?
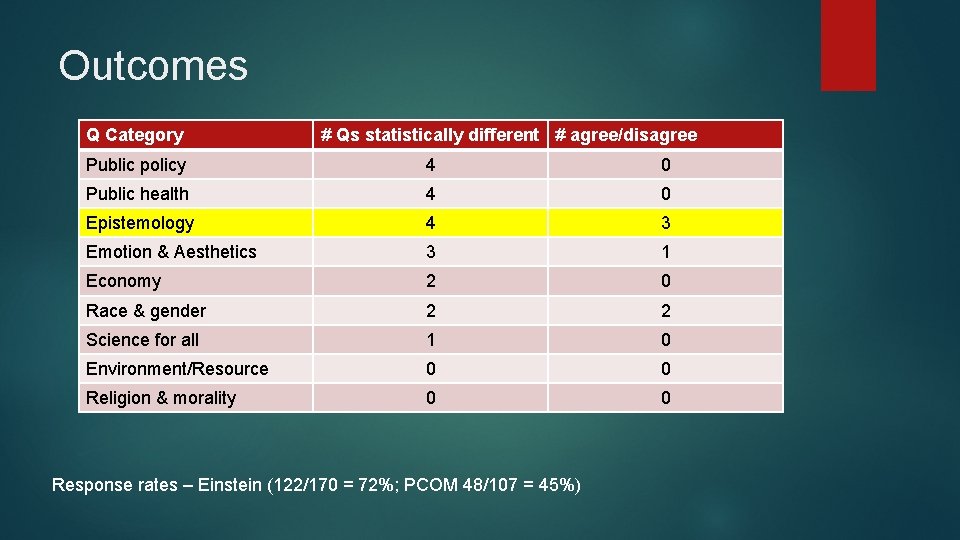
Outcomes Q Category # Qs statistically different # agree/disagree Public policy 4 0 Public health 4 0 Epistemology 4 3 Emotion & Aesthetics 3 1 Economy 2 0 Race & gender 2 2 Science for all 1 0 Environment/Resource 0 0 Religion & morality 0 0 Response rates – Einstein (122/170 = 72%; PCOM 48/107 = 45%)
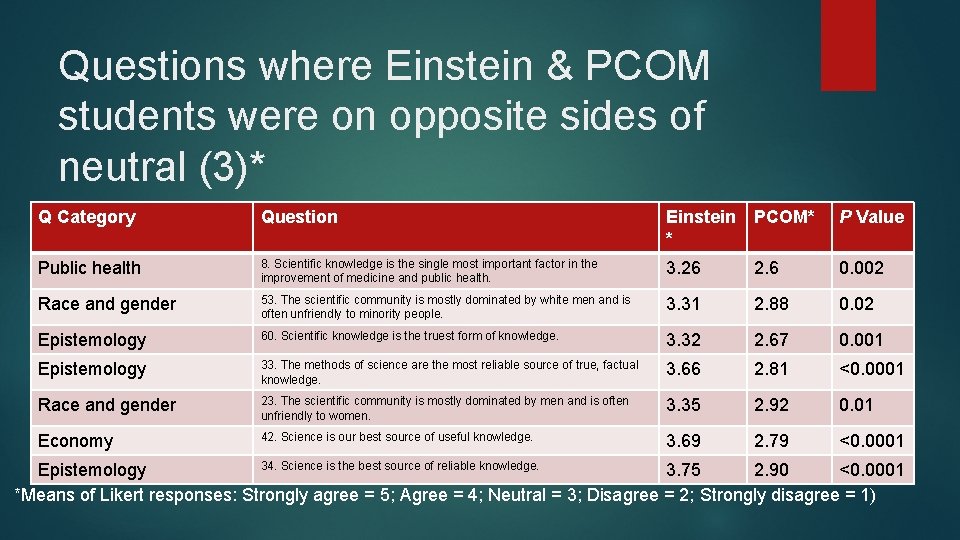
Questions where Einstein & PCOM students were on opposite sides of neutral (3)* Q Category Question Einstein * PCOM* P Value Public health 8. Scientific knowledge is the single most important factor in the improvement of medicine and public health. 3. 26 2. 6 0. 002 Race and gender 53. The scientific community is mostly dominated by white men and is often unfriendly to minority people. 3. 31 2. 88 0. 02 Epistemology 60. Scientific knowledge is the truest form of knowledge. 3. 32 2. 67 0. 001 Epistemology 33. The methods of science are the most reliable source of true, factual knowledge. 3. 66 2. 81 <0. 0001 Race and gender 23. The scientific community is mostly dominated by men and is often unfriendly to women. 3. 35 2. 92 0. 01 Economy 42. Science is our best source of useful knowledge. 3. 69 2. 79 <0. 0001 34. Science is the best source of reliable knowledge. Epistemology 3. 75 2. 90 <0. 0001 *Means of Likert responses: Strongly agree = 5; Agree = 4; Neutral = 3; Disagree = 2; Strongly disagree = 1)

Conclusions & Lessons Learned

Conclusions and lessons learned � CM students, faculty and practitioners: � Are not anti science � Understand support the role of research in legitimizing CM � But are concerned about: � Autonomy and continued authentic practice of CM � Cooptation � Inappropriate research methodology being used for CM � Keeping the patient at the center � The need for interprofessional education to engender respect and understanding

Acknowledgments � � Research mentors � Drs. Ben Kligler, Paul Marantz at Einstein � Dr. Roni Evans, University of Minesotta � Dr. Corbin Campbell, Teachers College Columbia University Research Colleagues � Drs. Diane Mc. Kee, Arya Nielsen, Claudia Citkovitz, � Funding bodies: NIH, PCORI, HRSA, CCAOM � Institutional support: PCOM, Einstein, Teachers College Columbia University

Thank you � Belinda (Beau) Anderson Pacific College of Oriental Medicine 110 William St, 19 th floor New York, NY 10038 212 982 3456 x 216 banderson@pacificcollege. edu
- Slides: 26