EvidenceBased Low Vision Interventions for the Occupational Therapist

Evidence-Based Low Vision Interventions for the Occupational Therapist KIMBERLY HOLT, OTR, OTD

“The only thing worse than being blind is having sight but no vision. ” (Keller, 1996)

Purpose This continuing education program will educate occupational therapists (OTs) about evidence-based interventions that address low-vision, including low vision equipment, environmental modifications, reading ability, community accessibility, safety, and performance of activities of daily living (ADLs) and instrumental activities of daily living (IADLs) to allow clients to increase their participation in their desired occupations.

Course Outline Purpose Background and Stats of Low Vision Person-Environment-Occupation model Rehabilitative frame of reference Education of Therapists Occupational Performance Client Readiness Client Participation Occupational Therapy Interventions Specific Interventions for ADLs, IADLs, and Leisure Lab Activities Definitions Types of Diagnoses Lab exercise: Simulation glasses Outcome measures/Assessments Rehabilitation Team Medicare Vision 2025 Occupational Therapy Framework-III: Domain and Process
Prevalence of Low Vision The geriatric population, ages 65+, is expected to double by the year 2050. This translates to 1 in every 5 Americans. (Ortman, Velkoff, & Hogan, 2014) Age-related low-vision disorders are estimated to reach 68 million by the year 2030. (National Eye Institute [NEI], n. d. b) The American Occupational Therapy Association (AOTA) has recently identified low vision as an area of growing concern due to this increase of age-related vision loss and its impact on daily functioning (n. d. a).

What do you need to know? What is visual acuity? What is a visual field? What is low-vision? What does it mean for a person to be legally blind?

What is visual acuity? Visual acuity is a person’s vision usually measured at a distance of 20 feet. “If you have 20/20 vision, you can see clearly at 20 feet what should normally be seen at that distance. If you have 20/100 vision, it means that you must be as close as 20 feet to see what a person with normal vision can see at 100 feet. ” (American Optometric Association, AOA, 2015 c, p. 1)

What is a visual field? A visual field is the range or area of vision a person can see with his/her eyes fixed on one point. A normal visual field is approximately 60° medially towards the nose and 100° laterally towards the ear from medial central vision. The average person with normal vision has a 160° angle of vision in each eye. (AOA, 2015 a)

What is low-vision? Low-vision is a visual acuity of 20/60 or worse in the better eye that is not correctable by eyeglasses, contact lenses, or surgical interventions. (AOA, 2015 b)

What is blindness? Legal blindness is a visual acuity of 20/200 in the best eye or a visual field of 20° or less. (AOA, 2015 b)

What causes low-vision? 4 main low vision diagnoses which account for 75% of age-related vision deficits. (NEI, n. d. b) Macular Degeneration Glaucoma Cataracts Diabetic Retinopathy The complications of these diagnoses affect multiple areas of daily living. (Perlmutter, Bhorade, Gordon, Hollingsworth, & Baum, 2010)

Age-Related Macular Degeneration Age-related macular degeneration (AMD) blurs the central portion of vision. Damage to the macula causes AMD and results in blurry or dark portions of central vision. Medical treatments can slow the effects of the disease, but not reverse it. AMD affects daily activities such as reading, writing, driving, the ability to see faces of people or cooking dials, and any fine detail activity. (NEI, 2015 a)

Age-related Macular Degeneration Butterfly, April 19, 2014. Courtesy of Kimberly Holt. AMD butterfly, October 20, 2015. Courtesy of Kimberly Holt.

Age-Related Macular Degeneration “What affects the heart affects the eyes” Leading cause of low vision Modifiable Risk Factors Lifestyle Habits Weight Exercise Diet High BP High Cholesterol Smoking

Glaucoma causes loss to peripheral vision. Increased pressure in the eye causes damage to the optic nerve resulting in glaucoma. Medical treatment can stop or reduce progression of the disease. Glaucoma reduces a client’s ability to see items to the side and tunnel vision is a common name for this disorder. Glaucoma impacts balance, navigation, and body awareness. (NEI, n. d. a)

Glaucoma Butterfly, April 19, 2014. Courtesy of Kimberly Holt. Glaucoma butterfly, October 20, 2015. Courtesy of Kimberly Holt.

Glaucoma Leading cause of blindness Regular eye exams can help to diagnose and provide early treatment to preserve treatment. Eye drops Decrease intraocular pressure Risk Factors Hypertension Diabetes Heart disease Hypothyroidism

Cataracts are a clouding of the lens of the eye. Proteins clumping together decreases the amount of light that can pass through the lens of the eye. Medical treatment involves surgery to replace the damaged lens with an artificial lens. Cataracts blur all vision in the affected eye causing an interference with daily activities. Glare and double vision may also be involved with this disorder. It impacts reading, writing, and ADL/IADL tasks. (NEI, 2009)

Cataracts Butterfly, April 19, 2014. Courtesy of Kimberly Holt. Cataract butterfly, October 20, 2015. Courtesy of Kimberly Holt.

Diabetic Retinopathy Diabetic retinopathy presents as blind spots or floaters throughout the visual field. Damage to the blood vessels that feed the retina causes this disorder and it results from high blood sugar levels from diabetes. Medial treatment includes controlling the diabetes through interventions such as medicine, diet and exercise; these treatments can stop the progression of the disease and subsequent eye disorder. Diabetic retinopathy causes difficulty with everyday activities and the specific visual impairment varies from person to person. It impacts all daily activities depending on the portion of the visual field lost. (NEI, 2015 b)
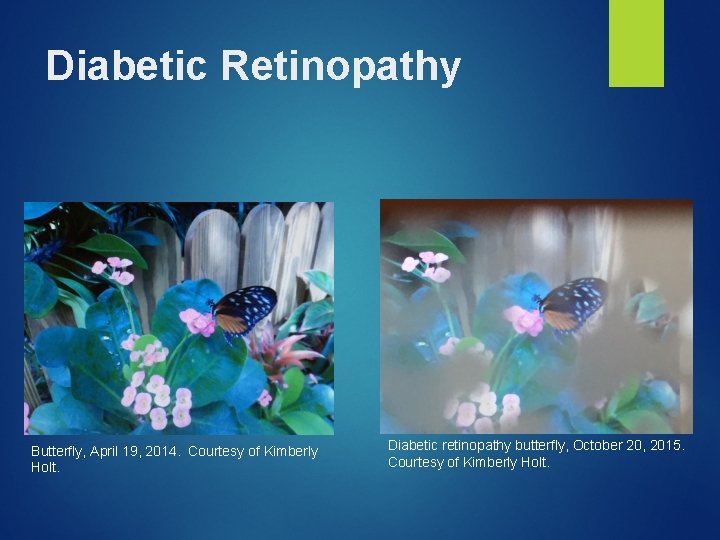
Diabetic Retinopathy Butterfly, April 19, 2014. Courtesy of Kimberly Holt. Diabetic retinopathy butterfly, October 20, 2015. Courtesy of Kimberly Holt.

Diabetic Retinopathy Leading cause of blindness in adults YOUNGER than 65 Modifiable risk factors Undiagnosed diabetes Poorly controlled glucose Poorly controlled BP Lack of exercise Poor diet Obesity

LAB EXERCISE #1 These vision simulation glasses allow us to understand what the visual impairments would look like.

Any Questions?

Low-Vision Rehabilitation Team Optometrists OD Diagnose, treat and manage vision disorder Evaluate and prescribe optic devices Provide low vision services Ophthalmologists MD Limited understanding of vision rehab Diagnose and prognosis disease process PRIMARY referral source for low vision services

Low Vision Team cont. Certified low-vision therapists (CLVT) Rehab professional Exam required OM, RT, Nurse, OT Help clients use remaining vision to perform ADL and use magnifiers Certified vision rehabilitation therapists (CRVT) Rehabilitation teacher Address ADL Experts in Braille College prep Occupational therapists 1991 OT able to treat Low vision clients – almost 20 years in low vision 70% of medically based services (Sokul-Mc. Kay & Michels, 2005)

Rehabilitation Team cont. Occupational therapists play an important role on the low-vision rehabilitation team. Occupational therapists can: Educate medical professionals Assist clients and their families adapt or compensate for vision loss. Teach clients compensatory and adaptive techniques. (Marinoff, 2012)

Medicare recognizes the need for low-vision services and covers low-vision as a primary and secondary diagnosis for treatment by an occupational therapist. (AOTA, n. d. b) Clinical experience has shown clients typically state they do not always see their vision deficits as a treatable condition; rather, they see it is as a product of the aging process.

Vision 2025 Occupational therapy maximizes health, wellbeing, and quality of life for all people, populations, and communities through effective solutions that facilitate participation in everyday living. (AOTA, 2017)

Occupational Therapy Framework -III: Domain and Process Occupational therapists can address deficits in clients’ performance skills, cultural, and personal interactions, and client factors as they relate specifically to low-vision disorders. (AOTA, 2014)

OT Framework III- cont. Many factors influence occupational performance Client Factors Values, beliefs, spirituality Body functions Sensory, motor, and mental Body structures Eyes

OT Framework III- cont. Performance Patterns Habits, routines, roles used in daily occupations Environment Physical Social Contexts Cultural, personal, temporal, and virtual

OT Framework III- cont. Vision deficits may affect a client’s: Performance Skills– affecting motor skills such as reaching, grasping and manipulating objects. Processing Skills – causing difficulties such as navigating within his or her environment or organizing items needed for a task. Cultural and Personal interactions - which could lead to withdrawal from desired activities and could cause clients to experience difficulty reading facial expressions or interpreting body language, which further complicates their personal interactions and may make social situations uncomfortable and awkward. (AOTA, 2014)

Person-Environment. Occupation model Using the Person-Environment-Occupation model (PEO), an occupational therapist can assist the person to increase the occupational performance with his or her desired activities by addressing the client’s identified areas of concern. (Law et al. , 1996) Vision loss causes a problem between a person and the environment, even in familiar settings.

Rehabilitative Frame of Reference Occupational therapists are able to treat their clients through the rehabilitative frame of reference by providing adaptations to the environment that use compensatory techniques to address the diagnosis or client factors related to low-vision. (Trombly, 2008) Evidence-based interventions are essential for the client with low vision to regain confidence and independence in their home and community environments. (Mohler, Neufeld, & Perlmutter, 2015)

Education of Therapists Education to therapists on low-vision interventions is essential. In one study, only 52% of occupational therapists felt they received adequate preparation in their educational process to treat clients diagnosed with low vision. (Winner, Yuen, Vogtle, & Warren, 2014) Another study concluded only 25% of therapists felt confident in performing assessments and interventions for vision loss. (Campion, Awang, & Ward, 2010)

Performance Vision loss is often a progressive disease, and clients often experience decreased independence and increased safety risks within their daily environments. It is important for therapists to assess and treat low-vision in clients given that vision has such a large influence on occupational performance. (Blaylock, Barstow, Vogtle, & Bennett, 2015)

Performance cont. A qualitative study examined the client and therapist’s perspective on how chronic conditions affect occupational performance in clients with low-vision. Low-vision affected clients’ performance of cooking, shopping, and going to work, and these were more difficult when a chronic condition affected their physical abilities as well. Clients also discussed how they compensated for their vision loss and other conditions with use of adaptive equipment, modifications to the environment, or changes in their routine. Therapists viewed dementia was the most inhibitory comorbidity, since it affects the ability to adapt to activities. (Barstow, Warren, Thaker, Hallman, & Batts, 2015)

Client Readiness A positive attitude and social support system enable a person to live purposefully with his or her vision loss; thus, the client will engage more in daily occupations. Clients’ readiness for change will influence their ability to adapt or compensate for vision loss. (Mohler, Neufeld, & Perlmutter, 2015)

Readiness cont. This qualitative study focused on the impact of vision loss. The researchers discussed clients’ views on how their vision loss was a pivotal point in their life, and the clients discussed how the loss of sight impacted their daily occupations. Learning adaptive techniques prepared the clients for the possible future decline of their vision. Many clients stated they struggled to find new purposeful ways to spend their time. (Girdler, Packer, & Boldy, 2008)

Client Participation The researchers reported, people with a visual impairment participate in daily activities less than the reference population without low-vision deficits. Occupational therapists can assist clients to make changes in areas of life that are meaningful and purposeful by recognizing and understanding the self-reported limitations of their clients. (Alma et. al, 2011) A Level I, randomized controlled trial (CEBM, 2011), noted a decrease in participation in daily activities when a client demonstrated a visual impairment of worse than 20/40 as compared to the normal visual acuity of better than 20/40. This study suggested that vision interventions could have a positive affect on a client’s daily functioning and quality of life. (Perlmutter, Bhorade, Gordon, Hollingsworth, & Baum, 2010)

Participation cont. This study concluded that clients who received singlecomponent training, such as leisure skills training, eccentric viewing techniques, or mobility skills, increased ADL participation, and decreased social isolation. The researchers concluded clients are more successful when taught how to use low-vision devices, problemsolving strategies, and when they are given information about resources in their community. (Liu, Brost, Horton, Kenyon, & Mears, 2013)

Assessments Most occupational therapy assessments address occupation or occupational performance; however, most do not address the visual functioning of the client. (Warren, 1998) Several assessments are available to determine the needs of a client with low-vision.

Canadian Occupational Performance Measure (COPM) A standardized client-centered outcome measure It allows therapist to measure the changes in a client’s perception of his or her occupational performance. This assessment can allow a therapist and client to make purposeful goals for low-vision therapeutic interventions. (Law et al. , 2014)

Brain Injury Visual Assessment Battery for Adults (bi. VABA) The bi. VABA is an assessment that helps determine what strategies a client will need to be successful with his or her therapeutic interventions. It focuses on multiple assessments for visual impairments such as visual acuity, contrast sensitivity, visual field, oculomotor function, and visual attention. (Warren, 1998)

Mini-Mental State Examination (MMSE) The MMSE determines cognitive function of a client. It allows a therapist to see if they are able learn and understand low-vision therapeutic interventions. Modifications to this test exclude the visual questions and use an adapted scoring method. (Folstein, & Mc. Hugh, 1975)

Low Vision Exam The low vision examination is usually complete by an ophthalmologist or optometrist. OT’s may complete depending on setting- to determine what vision is useable not what vision is gone. (very important distinction) Occupational therapists working in low vision should emphasize what abilities a client has remaining.

Components of a Low Vision Exam High contrast acuity Low contrast acuity Visual field integrity Color vision

Acuity is the ability to see small details and color. There are two types of high contrast acuity Distance Reading

High contrast Acuity High contrast acuity is measured by using a Snellen chart and is based on what a “normal” person can see at 20 feet. This test is used for standard vision. It is important to note that the Snellen Chart only tests to 20/200 and a person with low vision will usually require additional tests to determine accurate visual acuity.
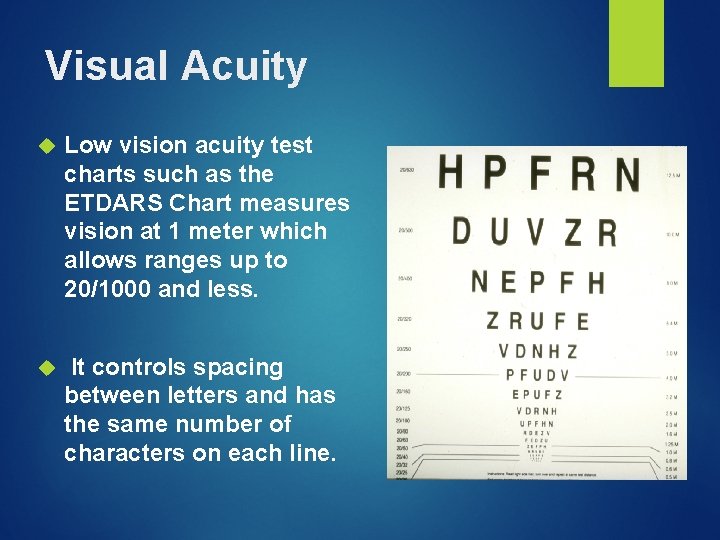
Visual Acuity Low vision acuity test charts such as the ETDARS Chart measures vision at 1 meter which allows ranges up to 20/1000 and less. It controls spacing between letters and has the same number of characters on each line.

MN Read Acuity Charts The MN Read Acuity Charts are continuoustext formatted visual acuity charts. They measure a client’s reading acuity and speed by having a client read sentences that progressively get smaller in print. This test allows the occupational therapist to determine the appropriate size of font needed for a client to read accurately. (Mansfield, Legge, Luebker, & Cunningham, 1994)

Example of the MN Read MNREAD, Precision Vision. Reprinted with permission.

Low Contrast Acuity Measures the ability to see an image as it blends with its background. Many environmental features are low contrast Impacts clients with macular deterioration

Low Contrast Acuity Impacts daily activities such as Water on a floor Clear glass with water Facial features Outdoor environments

Low Contrast Can you spot the water?

Good Contrast Sidewalk, July 14, 2017. Courtesy of Kimberly Holt. Sidewalk 2, July 14, 2017. Courtesy of Kimberly Holt.

Low Contrast Sensitivity Chart The Pelli. Robson Chart is an example of a low contrast evaluation.

Visual Field Exam Microperimetry examines only the central 20* of visual field Performed by low vision MD or OD. As OT’s we can request print out of results from Dr. ’s to help us understand what areas of the visual field are impaired.

Clinical Assessments for OT Occupational Therapists should screen for scotomas in the central visual field of clients. Provides information on clients ability for success with reading and occupational performance of tasks.

Central Visual Screen- Clock Test

Clock Test Have client look at center of clock and without moving his/her eyes, instruct the client to identify if any areas are distorted, blurry, or missing. Make sure client does NOT move/scan clock face. Note any areas identified by the client This indicated the area of the potential scotoma or blind spot.

Occupational Therapy Interventions Occupational therapy interventions to address lowvision include: Eccentric Viewing Reading/Writing Magnification Lighting Sensory substitutions Mobility Adaptive/Assistive Devices Home safety (Fok, Polgar, Shaw, & Jutai, 2011; Nguyen, Weismann, & Trauzettel. Klosinski, 2009; Vukicevic & Fitzmaurice, 2009)

Eccentric Viewing cont. The eccentric viewing technique involves focusing the central vision or blurred area on a different portion of the object or words to allow the client to use their peripheral vision to read. While this technique can be difficult to learn, continuing to practice the technique can allow this technique to become second nature. (Galbraith, n. d. )

Eccentric Viewing Eccentric viewing does not change or improve vision; rather, it is a technique that can benefit clients in their everyday life. Eccentric viewing is a visual technique that clients with macular degeneration or central vision loss can use to increase their reading skills needed for ADL/IADL tasks. (Galbraith, n. d. )

Eccentric Viewing cont. Instruct the client to look at the center of the target and without moving his/her eyes locate eth area of the clock that was blurry/distorted before. Instruct the client to look above the card to see if the clock becomes more complete and clear. You can cue the client by moving your and in the direction you want them to look. Repeat with moving the eyes above/below and left /right of the image to find the best location to complete the image. When the PRL is located explain to the client what this area is and how it will be used for task completion.

Preferred Retinal Locus (PRL) The PRL is the site of the best vision when the fovea is damaged. Once a client has located their PRL – eccentric viewing training techniques can be taught to the client

Eccentric Viewing cont. R

Eccentric Viewing Once a client is able to locate their PRL, they will need to work on purposeful eye movements. Locate and fixate on target (clock or letter) Gaze shirt between target Track a moving target View targets near and far Pre reading exercises Comprehension exercises

Eccentric Viewing cont. The results of one study indicated that utilizing eccentric viewing techniques is a useful strategy when performing ADL activities, and a significant improvement was noted after eccentric viewing training in near vision loss. (Vukicevic & Fitzmaurice, 2009) While some studies showed improvement in reading and ADL tasks, researchers in this study stated the full potential of eccentric viewing trainings needed more research. (Gaffney, Margrain, Bunce, & Binns, 2014)

Eccentric Viewing Cont. Eccentric Viewing techniques can impact the performance of daily activities in clients with agerelated macular degeneration. The study concluded that training in eccentric viewing techniques has a positive effect on daily living skills. (Hong, Park, Kwon, & Yoo, 2014)

Magnification Clients with low-vision have difficulty with reading tasks. Occupational therapists can teach clients compensatory techniques, and they can teach clients how to use adaptive devices to assist with this task. A higher magnification, such as 10 x power, would allow for a smaller viewing area as compared to a 3 x power magnifier. Many types of magnifiers are available. Stand magnifiers Hand-held magnifiers Telescopes or a monocular Neck wrap magnifiers Magnification lamps (American Foundation for the Blind, 2015 b)

Magnification Once a client can read without magnification utilizing their PRL a magnifier can be introduced. Educate the client on limitation of the device Restrictions of field of view Maximum size of magnification

Magnifier Use. Stand Magnifier Lay magnifier on the reading material Have the person wear glasses if they use them Slide the magnifier across the line of print To move to the next line of print Return the magnifier to the left side by pulling it back over the line of print just read Move to the next line of print

Magnifier Use. Hand Held Magnifier Begin by laying the magnifier on the page and then pull it away until the print comes into focus. Move the magnifier across the pate To move to the next line of print Return the magnifier to the left side by pulling it back over the line of print just read Move the magnifier down to the next line This magnifier requires greater control of a person’s PRL
![Magnifiers 4 x hand-held magnifier [Image]. Reprinted with permission from LS&S. 3 x stand Magnifiers 4 x hand-held magnifier [Image]. Reprinted with permission from LS&S. 3 x stand](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-76.jpg)
Magnifiers 4 x hand-held magnifier [Image]. Reprinted with permission from LS&S. 3 x stand magnifier [Image]. Reprinted with permission from LS&S. 10 x hand-held magnifier [Image]. Reprinted with permission from LS&S. 10 x stand magnifier [Image]. Reprinted with permission from LS&S.
![Magnifiers Cont. Monocular [Image]. Reprinted with permission from LS&S. Magnifying lamp [Image]. Reprinted with Magnifiers Cont. Monocular [Image]. Reprinted with permission from LS&S. Magnifying lamp [Image]. Reprinted with](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-77.jpg)
Magnifiers Cont. Monocular [Image]. Reprinted with permission from LS&S. Magnifying lamp [Image]. Reprinted with permission from LS&S. Neck-wrap magnifier [Image]. Reprinted with permission from LS&S.
![High Tech Electronic Magnification CCTV [Image]. Reprinted with permission from LS&S. Desktop CCTV High Tech Electronic Magnification CCTV [Image]. Reprinted with permission from LS&S. Desktop CCTV](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-78.jpg)
High Tech Electronic Magnification CCTV [Image]. Reprinted with permission from LS&S. Desktop CCTV

High Tech – Electronic Magnification Ruby HD from Freedom Scientific Stand units paired with computers

Lab Exercise #2 – Low Vision Trial

Writing A client may need assistance with writing tasks. They will need to be able to read what they have written. Teach the client the PBS technique Print Block Letters Space it out Have client write a shopping list /then write using PBS technique – which is easier to read? Writing guides can be useful but difficult to use.

PBS Technique PBS, July 17, 2014. Courtesy of Kimberly Holt.

Reading The loss of the ability to read is a major problem for clients when performing everyday activities. Sans serif typefaces such as Arial or Veranda are easier to read than serif typefaces such as Times New Roman. A font size of 16 to 18 points is optimal for reading with or without the use of a magnifier. (Russell-Minda et al. , 2007) Moderately strong evidence supports the use of electronic magnification. Strong evidence supports increased reading abilities in clients participating in an occupational therapy intervention program. (Smallfield, Clem, & Myers, 2013)

Reading Cont. In one study, reading ability increased from 16% to 94% with the use of low-vision aids such as a hand-held magnifier or closed-circuit television (CCTV). Reading speed increased with the use of a visual aid in clients with a visual acuity of less then 20/200. (Nguyen, Weismann, & Trauzettel-Kloswinski, 2009)

Lighting can impact multiple activities in a person’s daily routine. Types of light bulbs Incandescent – being phased out Fluorescent – best overall lighting, even illumination, some strobing, limited with variety Halogen – task and room lighting, minimal glare, even illumination / but Hot lighting – not to close to client LED – instant on , expensive, bulb life is years Natural lighting

Lighting cont. Lighting fixtures Table lamps Floor lamps Gooseneck lamps Under counter lighting Disk Lights Automatic night lights (American Foundation for the Blind, 2015 a)

Lighting cont. These researchers performed a qualitative study to determine if assistive lighting could reduce falls in clients with low vision. The researchers identified seven themes important in assistive lighting: appropriate, sufficient, even, adjustable, sustainable, simple, and adaptable. The study concluded that assistive lighting, whether portable or fixed, helps clients perform many daily activities such as navigating their environment, meal preparation, grooming tasks, and medication management. (Fisk & Raynham, 2014)

Lighting cont. Perlmutter et al. (2013) developed a Home Environment Lighting Assessment (HELA) to assess home lighting of older adults with low vision. While this assessment will be useful for near task lighting, it is not designed for overall lighting such as a bedroom or hallway, which is crucial for mobility and safety.
![Lighting Examples Disc light [Image]. Reprinted with permission from LS&S. Task lamp [Image]. Reprinted Lighting Examples Disc light [Image]. Reprinted with permission from LS&S. Task lamp [Image]. Reprinted](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-89.jpg)
Lighting Examples Disc light [Image]. Reprinted with permission from LS&S. Task lamp [Image]. Reprinted with permission from LS&S. Gooseneck lamp [Image]. Reprinted with permission from LS&S.

Sensory Substitutions Sensory substitution is an alternative to devices, and clients can utilize their sense of touch or hearing to compensate for vision loss. Since vision impacts most daily activities, teaching clients safe techniques and how to use adaptive devices are important interventions. (Williams, Ray, Griffith, & De l’Aune, 2011) Sensory Substitutions Liquid level indicator Bump dots Tactile Paint Beads of safety pins to identify clothing Talking devices

Sensory Substitutions cont. Sensory substitutions are a common strategy used for clients with impaired sight. The researchers in this study evaluated the use of sensory devices. A long cane and braille are the two sensory substitutions most frequently used throughout time. (Williams, Ray, Griffith, & De l’Aune, 2011)
![Tactile Dots and Paint Bump dot black [Image]. Reprinted with permission from LS&S. Bump Tactile Dots and Paint Bump dot black [Image]. Reprinted with permission from LS&S. Bump](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-92.jpg)
Tactile Dots and Paint Bump dot black [Image]. Reprinted with permission from LS&S. Bump dot clear [Image]. Reprinted with permission from LS&S. Bump dot orange [Image]. Reprinted with permission from LS&S. Tactile paint orange [Image]. Reprinted with permission from LS&S.

Environments Clients may have increased difficulty navigating environments due to: Lighting – glare, brightness, unevenness Background contrast – sidewalks and stairways may not be marked Background patterns – moving people on sidewalks in restaurants (can’s judge speed of movements), multiple patterns in a home, or in a building (brick wall/ tile floor) Obstacles/hazards – objects on floor

Mobility Maneuvering unfamiliar environments can be hazardous and confusing. Teaching clients to use a blind cane or assistive animal can allow them to explore the community independently. (Barstow, Warren, Thaker, Hallman, & Batts, 2015) Utilizing adaptive markings such as contract paint or tactile skid strips can increase safety and mobility at home.

Mobility cont. A grounded theory qualitative study assessed the effects of low-vision on clients with mobility issues. The authors concluded that clients want others to see them as normal, not as having a visual disability. Clients preferred to make mobility choices that were the least invasive of others and resembled the normal mobility of others. (Ball & Nicole, 2015)

Assistive Devices Clients can use multiple devices and adaptive techniques to help accommodate vision loss. Assistive devices can range from low tech to high tech, inexpensive to costly, and portable to fixed. A client may use a low-vison assistive device in any area of daily occupations. Meal preparation assistive devices Talking devices Magnifiers Technological interventions Computer programs

Assistive Devices cont. A qualitative study focused on why older adults choose a particular low vision assistive device (LVAD). The need for selecting low-vision interventions and devices is important for understanding the positive and negative aspects of LVAD from a client’s point of view. The study concluded that interaction with low-vision service providers improved the client’s ability to obtain and successfully utilize LVAD. Occupational therapy services provided the participant with the training needed to use a selected device and resources. The study encouraged low-vision support groups to allow participants to exchange information about their experiences with adapting to their low-vision diagnosis and their LVAD used to increase independence in their daily routines. (Copolillo & Teitelman, 2005)

Assistive Devices cont. One study examined the effects of assistive device usage in clients with low vision and depression. The results showed that the use of optical devices for daily activities resulted in a decline in depression over time, allowing clients to increase their occupational performance. (Horowitz, Brennan, Reinhardt, & Mac. Millan, 2006) Another qualitative study identified seven categories of low vision device use. The study concluded that while many participants have multiple devices available to them, musical devices, note-taking devices, ADL aids, lighting, and magnifiers were labeled the most important to assist with daily occupations. (Fok, Polgar, Shaw, & Jutai, 2011)

Home Safety Assessments Many clients are choosing to age in place, thus requiring the need to ensure their safety at home through a standardized home assessment that focuses on clients with low vision. This study focused on examining three home safety assessments in regard to the participants’ perspective of the impact low vision plays in home safety. The authors concluded that common home assessments do not address a patient’s needs for intervention due to vision loss, making it difficult for occupational therapists to provide necessary recommendations for a patient’s safety. Occupational therapist will need further evaluation of how vision loss affects a participant’s safety within the home environment along with the commonly used assessments. (Barstow, Bennett, & Vogtle, 2011)

Low Vision Interventions for Activities of Daily Living Feeding Grooming Dressing Bathing Mobility (AOTA, 2014)

ADLs cont. Low-vision affects a client’s ability to perform daily occupations, and teaching clients adaptive techniques for compensation can be of great assistance. One study found that decreasing visual acuity increased limitations with ADLs, IADLs, mobility tasks, or a combination of the three. (Laitinen et al. , 2007)

ADLs cont. This study determined that clients receiving interventions required less assistance than those that did not receive the low-vision interventions. This study indicated that educating clients on problem-solving strategies could help maintain the ability to participate in ADL and IADL tasks longer even with declining vision. (Eklund, Sjostrand, & Dahlin-Ivanoff, 2008)

ADLs cont. In this study, occupational therapists trained clients in reading, lighting, and magnification skills specific to each client’s vision loss. Following three sessions, participants increased the ability to read medication labels from 58% to 94%. It is important for clients to understand the correct dosage and frequency of the prescribed medication. (Markowitz, Kent, Schuchard, & Fletcher, 2008)

Feeding Learning, sight, and sound (LS&S, n. d. ), LS&S Product Catalog. Reprinted with permission. Clock technique, November 2, 2015. Courtesy of Kimberly Holt.
![Hygiene and Grooming Magnifying nail clippers [Image]. Reprinted with permission from LS&S. Magnifying mirror Hygiene and Grooming Magnifying nail clippers [Image]. Reprinted with permission from LS&S. Magnifying mirror](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-105.jpg)
Hygiene and Grooming Magnifying nail clippers [Image]. Reprinted with permission from LS&S. Magnifying mirror [Image]. Reprinted with permission from LS&S. Magnifying lamp [Image]. Reprinted with permission for LS&S.

Dressing or Clothing Management Pin Identify, October, 2015. Courtesy of . Kimberly Holt Disc light [Image]. Reprinted with permission from LS&S. Button hook [Image]. Reprinted with permission from LS&S.
![Bathing Grab bar [Image]. Reprinted with permission from LS&S. Bathing Grab bar [Image]. Reprinted with permission from LS&S.](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-107.jpg)
Bathing Grab bar [Image]. Reprinted with permission from LS&S.
![Mobility Monocular [Image]. Reprinted with permission from LS&S. Cane [Image]. Reprinted with permission from Mobility Monocular [Image]. Reprinted with permission from LS&S. Cane [Image]. Reprinted with permission from](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-108.jpg)
Mobility Monocular [Image]. Reprinted with permission from LS&S. Cane [Image]. Reprinted with permission from LS&S. Contrast tape [Image]. Reprinted with permission from LS&S.

Low-Vision Interventions for Instrumental Activities of Daily Living Communication Management Financial Management Medication Management Meal Preparation Shopping (AOTA, 2014)
![Communication Signature guide [Image]. Reprinted with permission from LS&S. Envelope guide [Image]. Reprinted with Communication Signature guide [Image]. Reprinted with permission from LS&S. Envelope guide [Image]. Reprinted with](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-110.jpg)
Communication Signature guide [Image]. Reprinted with permission from LS&S. Envelope guide [Image]. Reprinted with permission from LS&S. Bold-lined paper [Image]. Reprinted with permission from LS&S. Task lamp [Image]. Reprinted with permission from LS&S. Letter writing guide [Image]. Reprinted with permission from LS&S. Big button telephone [Image]. Reprinted with permission from LS&S.
![Time Management Talking watch [Image]. Reprinted with permission from LS&S. Talking alarm clock [Image]. Time Management Talking watch [Image]. Reprinted with permission from LS&S. Talking alarm clock [Image].](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-111.jpg)
Time Management Talking watch [Image]. Reprinted with permission from LS&S. Talking alarm clock [Image]. Reprinted with permission from LS&S. Black face clock [Image]. Reprinted with permission from LS&S.
![Financial Management Talking calculator [Image]. Reprinted with permission from LS&S. Check writing guide [Image]. Financial Management Talking calculator [Image]. Reprinted with permission from LS&S. Check writing guide [Image].](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-112.jpg)
Financial Management Talking calculator [Image]. Reprinted with permission from LS&S. Check writing guide [Image]. Reprinted with permission from LS&S. Magnifying lamp [Image]. Reprinted with permission from LS&S.
![Medication Management Talking glucometer [Image]. Reprinted with permission from LS&S. Eye drop guide [Image]. Medication Management Talking glucometer [Image]. Reprinted with permission from LS&S. Eye drop guide [Image].](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-113.jpg)
Medication Management Talking glucometer [Image]. Reprinted with permission from LS&S. Eye drop guide [Image]. Reprinted with permission from LS&S. Jumbo pill boxes [Image]. Reprinted with permission from LS&S. Syringe magnifier [Image]. Reprinted with permission from LS&S. Sure shot [Image]. Reprinted with permission from LS&S.
![Meal Preparation Jumbo timer [Image]. Reprinted with permission from LS&S. Contrast cutting board [Image]. Meal Preparation Jumbo timer [Image]. Reprinted with permission from LS&S. Contrast cutting board [Image].](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-114.jpg)
Meal Preparation Jumbo timer [Image]. Reprinted with permission from LS&S. Contrast cutting board [Image]. Reprinted with permission from LS&S. Liquid level indicator [Image]. Reprinted with permission from LS&S. Contrast measure cups [Image]. Reprinted with permission from LS&S.

Shopping Identify cards, October 20, 2015. Courtesy of Kimberly Holt Shopping cards, October 20, 2015. Courtesy of Kimberly Holt.

Low Vision Interventions for Leisure Tasks Vision loss and the subsequent decrease in social participation can lead to client isolation. A client may withdraw from social interactions because shaking hands, making eye contact, and social greetings cause anxiety or discomfort along with the inability to perform the tasks due to vision loss. There are many devices to assist a client to continue with the leisure task of choice. (Berger, Mc. Ateer, Schreier, & Kaldenberg, 2013)

Leisure cont. This study examined leisure participation with older adults with low-vision. Environmental adaptation and problem-solving approaches were two of the four themes the researchers developed. Participants learned strategies that older adults with low vision use, to assist with everyday activities; these studies showed an increase in participation in ADLs. (Berger, Mc. Ateer, Schreier, & Kaldenberg, 2013)
![Leisure Activities Jumbo remote [Image]. Reprinted with permission from LS&S. Tactile dominos [Image]. Reprinted Leisure Activities Jumbo remote [Image]. Reprinted with permission from LS&S. Tactile dominos [Image]. Reprinted](http://slidetodoc.com/presentation_image_h/f76178cd958710e9d6f739112eaba24e/image-118.jpg)
Leisure Activities Jumbo remote [Image]. Reprinted with permission from LS&S. Tactile dominos [Image]. Reprinted with permission from LS&S. Large print playing cards [Image]. Reprinted with permission from LS&S. Illuminated remote [Image]. Reprinted with permission from LS&S. Needle threader [Image]. Reprinted with permission from LS&S. Large print bingo cards [Image]. Reprinted with permission from LS&S.

APP S
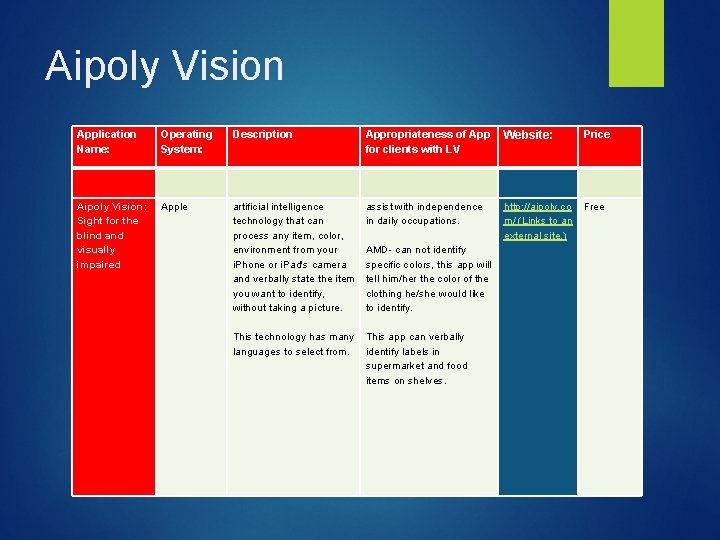
Aipoly Vision Application Name: Operating System: Description Appropriateness of App Website: for clients with LV Price Aipoly Vision: Sight for the blind and visually impaired Apple artificial intelligence technology that can process any item, color, environment from your i. Phone or i. Pad's camera and verbally state the item you want to identify, without taking a picture. This technology has many languages to select from. assist with independence in daily occupations. AMD- can not identify specific colors, this app will tell him/her the color of the clothing he/she would like to identify. This app can verbally identify labels in supermarket and food items on shelves. http: //aipoly. co Free m/ (Links to an external site. )
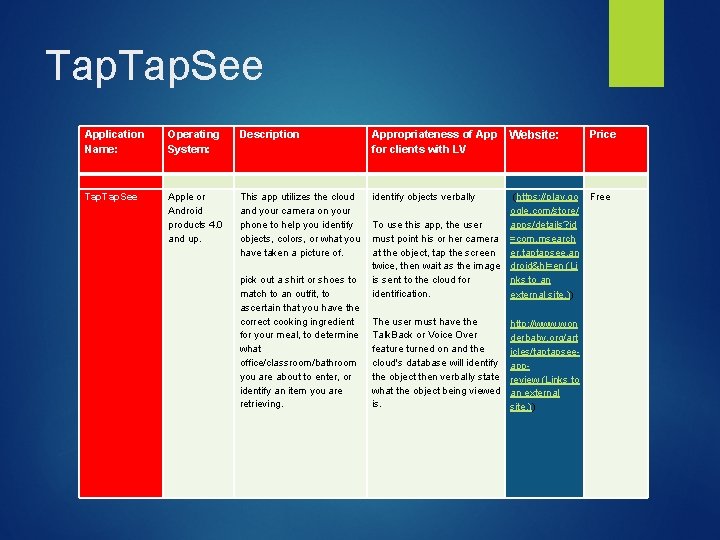
Tap. See Application Name: Operating System: Description Appropriateness of App Website: for clients with LV Price Tap. See Apple or Android products 4. 0 and up. This app utilizes the cloud and your camera on your phone to help you identify objects, colors, or what you have taken a picture of. pick out a shirt or shoes to match to an outfit, to ascertain that you have the correct cooking ingredient for your meal, to determine what office/classroom/bathroom you are about to enter, or identify an item you are retrieving. identify objects verbally To use this app, the user must point his or her camera at the object, tap the screen twice, then wait as the image is sent to the cloud for identification. The user must have the Talk. Back or Voice Over feature turned on and the cloud's database will identify the object then verbally state what the object being viewed is. (https: //play. go ogle. com/store/ apps/details? id =com. msearch er. taptapsee. an droid&hl=en (Li nks to an external site. )) Free http: //www. won derbaby. org/art icles/taptapseeappreview (Links to an external site. ))
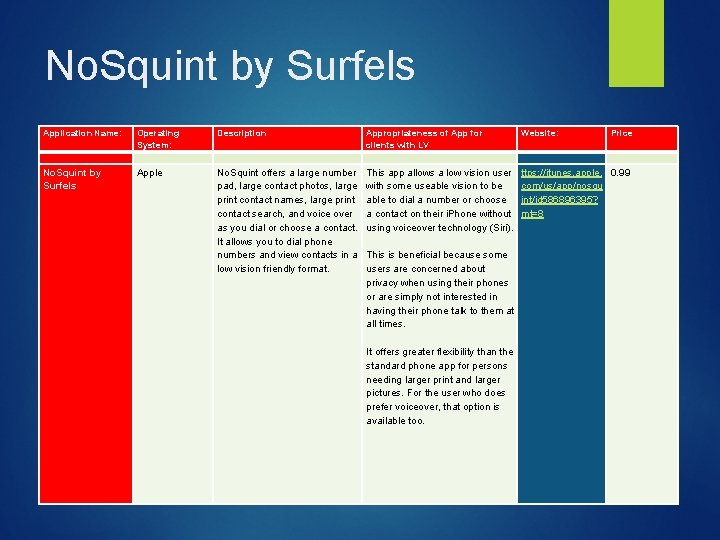
No. Squint by Surfels Application Name: No. Squint by Surfels Operating System: Description Apple No. Squint offers a large number pad, large contact photos, large print contact names, large print contact search, and voice over as you dial or choose a contact. It allows you to dial phone numbers and view contacts in a low vision friendly format. Appropriateness of App for clients with LV Website: Price This app allows a low vision user with some useable vision to be able to dial a number or choose a contact on their i. Phone without using voiceover technology (Siri). This is beneficial because some users are concerned about privacy when using their phones or are simply not interested in having their phone talk to them at all times. It offers greater flexibility than the standard phone app for persons needing larger print and larger pictures. For the user who does prefer voiceover, that option is available too. ttps: //itunes. apple. 0. 99 com/us/app/nosqu int/id 586896395? mt=8
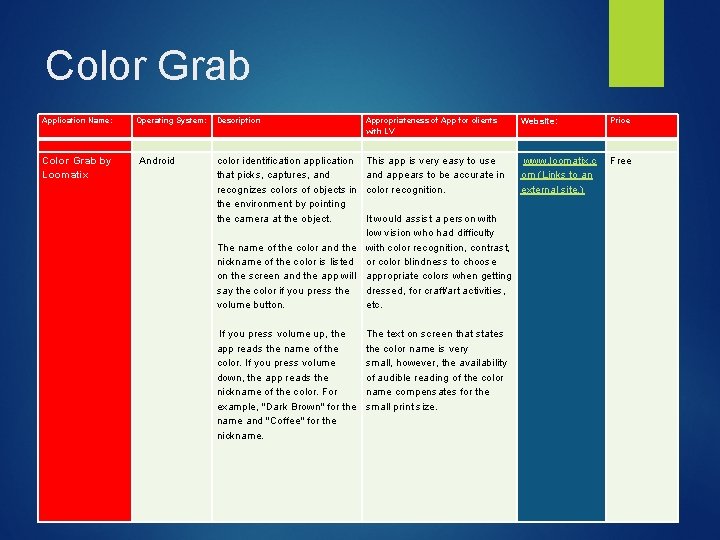
Color Grab Application Name: Operating System: Description Appropriateness of App for clients with LV Website: Price Color Grab by Loomatix Android color identification application that picks, captures, and recognizes colors of objects in the environment by pointing the camera at the object. The name of the color and the nickname of the color is listed on the screen and the app will say the color if you press the volume button. If you press volume up, the app reads the name of the color. If you press volume down, the app reads the nickname of the color. For example, "Dark Brown" for the name and "Coffee" for the nickname. This app is very easy to use www. loomatix. c and appears to be accurate in om (Links to an color recognition. external site. ) It would assist a person with low vision who had difficulty with color recognition, contrast, or color blindness to choose appropriate colors when getting dressed, for craft/art activities, etc. The text on screen that states the color name is very small, however, the availability of audible reading of the color name compensates for the small print size. Free
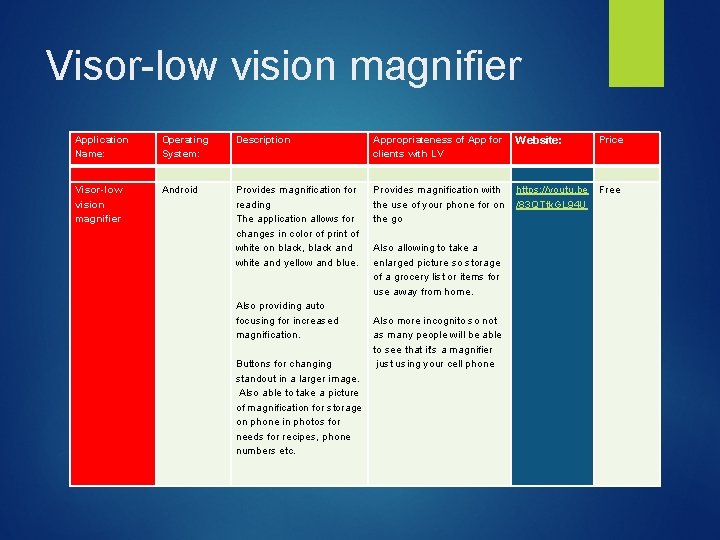
Visor-low vision magnifier Application Name: Operating System: Description Appropriateness of App for clients with LV Website: Price Visor-low vision magnifier Android Provides magnification for reading The application allows for changes in color of print of white on black, black and white and yellow and blue. Also providing auto focusing for increased magnification. Buttons for changing standout in a larger image. Also able to take a picture of magnification for storage on phone in photos for needs for recipes, phone numbers etc. Provides magnification with https: //youtu. be the use of your phone for on /83 QTtk. GL 94 U the go Also allowing to take a enlarged picture so storage of a grocery list or items for use away from home. Also more incognito so not as many people will be able to see that it's a magnifier just using your cell phone Free
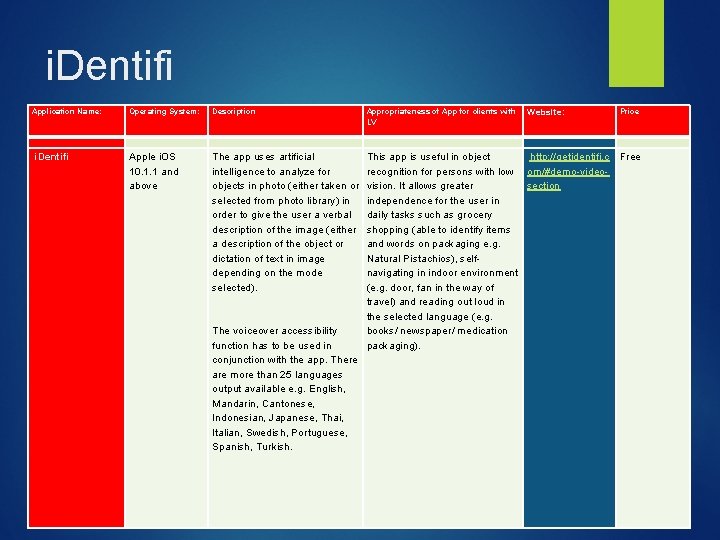

i. Dentifi Application Name: Operating System: Description Appropriateness of App for clients with LV Website: Price i. Dentifi Apple i. OS 10. 1. 1 and above The app uses artificial intelligence to analyze for objects in photo (either taken or selected from photo library) in order to give the user a verbal description of the image (either a description of the object or dictation of text in image depending on the mode selected). The voiceover accessibility function has to be used in conjunction with the app. There are more than 25 languages output available e. g. English, Mandarin, Cantonese, Indonesian, Japanese, Thai, Italian, Swedish, Portuguese, Spanish, Turkish. This app is useful in object http: //getidentifi. c Free recognition for persons with low om/#demo-videovision. It allows greater section independence for the user in daily tasks such as grocery shopping (able to identify items and words on packaging e. g. Natural Pistachios), selfnavigating in indoor environment (e. g. door, fan in the way of travel) and reading out loud in the selected language (e. g. books/ newspaper/ medication packaging).
Digit-Eyes Application Name: Operating System: Description Appropriateness of App for clients with LV Website: Price Digit-Eyes by Digital Miracles, LLC Apple IOS 6. 1 or later This app reads UPC and QR codes and provides text and audio response identifying the item, with specific details such as brand, flavor, size, cooking directions, or dosage information, with a database of over 37 million products. Users can also create their own labels by voice or text, including washable labels for clothing. read codes on hard-to-see items and tell the user the songs on a CD and the color of the nail polish or distinguish antibiotic ointment from hydrocortisone cream. purchase or print QR labels at home and personalize them by scanning a blank label and recording a message that is stored and retrieved when the label is scanned again, allowing the user to place labels wherever needed, such as: on dates in a calendar to remember appointments or a friend’s birthday, on leftover food with a description and preparation date, on a house key for easier identification, and on folders of important documents for legal and financial management. https: //itunes. appl e. com/us/app/digit eyes/id 376424490 ? mt=8 (Links to an external site. ) Full version 9. 99 Digit-Eyes Lite Free
i. Move Application Name: Operating System: Description Appropriateness of App for clients Website: with LV Price i. Move Apple i. OS 8. 0 or later Used for navigation. The app is fully accessible with Voice. Over and is easy to navigate and use; all buttons are clearly labeled. i. Move supports independent mobility of visually impaired people. Know the address where they are; Know points of interest around them (e. g. schools, stations, pubs, etc. ); Record speech notes associated to the person's location. A speech note will be played every time the person is close to the place where it has been recorded; Customize the messages. For example, the person can choose to be warned about the address where they are, the current orientation and speed, about speech notes, nearby points of interest, etc. Promote independence in navigating familiar environments. completing IADL's such as going into town to take care of banking needs, paying bills, or simply for socialization such as to go visit a family member or a friend. In addition, the i. Move app is available in many different languages, which make it much more useful to a greater number of people. http: //www. everywar Free etechnologies. com/ ( Links to an external site. )
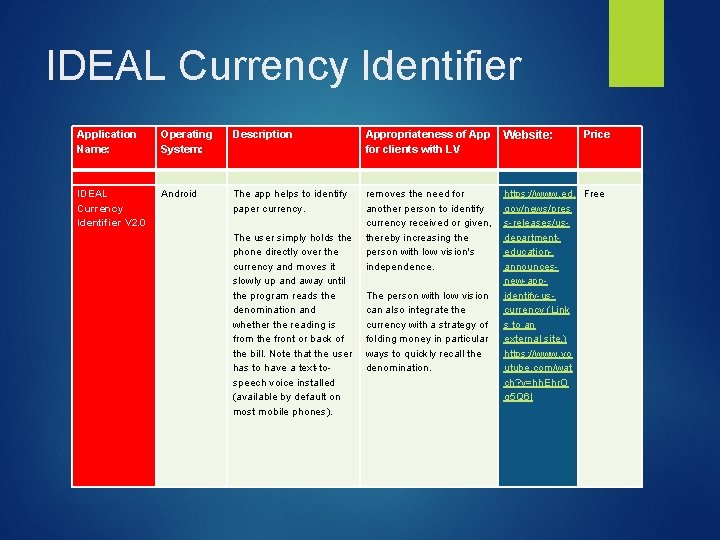

IDEAL Currency Identifier Application Name: Operating System: Description Appropriateness of App Website: for clients with LV IDEAL Currency Identifier V 2. 0 Android The app helps to identify paper currency. The user simply holds the phone directly over the currency and moves it slowly up and away until the program reads the denomination and whether the reading is from the front or back of the bill. Note that the user has to have a text-tospeech voice installed (available by default on most mobile phones). removes the need for another person to identify currency received or given, thereby increasing the person with low vision's independence. The person with low vision can also integrate the currency with a strategy of folding money in particular ways to quickly recall the denomination. Price https: //www. ed. Free gov/news/pres s-releases/usdepartmenteducationannouncesnew-appidentify-uscurrency (Link s to an external site. ) https: //www. yo utube. com/wat ch? v=hh. Ehr. O g 5 Q 6 I

Other Apps Look. Tel Money Reader Look. Tel Recognizer Take a picture and ask a person in real time for an answer Eye. Note Identifies objects stored into system by consumer Viz. Wiz Reads currency – paper and coins US paper currency identifier Color Id free Identifies colors using camera on phone in real time

Questions?

Lab Activity #3 Glucometer Use

Lab Trials #4 Write Check Pour Glass of Water Read Can good labels Measure in syringe Play cards Write grocery list cursive/PBS Medication Management

Kitchen Kitchen, October 20, 2015. Courtesy of Kimberly Holt.

Cooking, October 20, 2015. Courtesy of Kimberly Holt.

Water Glass

Bathroom, October 20, 2015. Courtesy of Kimberly Holt.

Medication Medicine, October 20, 2015. Courtesy of Kimberly Holt.
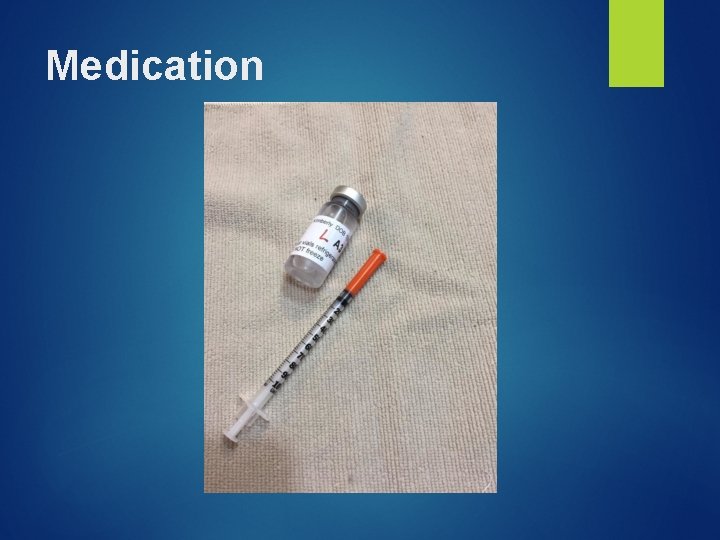
Medication

Clothing Management Clothing, October 20, 2015. Courtesy of Kimberly Holt.

Closet Organization

Communication Telephone, November 2, 2015. Courtesy of Kimberly Holt.

Reading Book, October 20, 2015. Courtesy of Kimberly Holt.

Mobility Stairs, October, 2015. Courtesy of Kimberly Holt.

Mobility Wall, July 14, 2017. Courtesy of Kimberly Holt. Hallway, July 14, 2017. Courtesy of Kimberly Holt.

Mobility Hallway, July 14, 2017. Courtesy of Kimberly Holt. Outdoor shadow, July 17, 2017. Courtesy of Kimberly Holt.

Office/Desk Space Messy Desk, September 24, 2017. Courtesy of Kimberly Holt.

Bedroom

Hospital/SNF Room

Closing… Low-vison affects clients in all areas of their life. “Since occupation is central in the process of adapting to age-related vision loss, then occupation therapy… has a moral obligation to contribute” to these disease processes (Girdler, Packer, & Boldy, 2008, p. 118). Together we can make a difference for these clients and help them regain independence.

Any Questions or Comments?

References Alma, M. , Van Der Mei, S. , Melis-Dankers, B. , Van Tilburg, T. , Groothoff, J. , & Suurmeijer, T. (2011). Participation of the elderly after vision loss. Disability and Rehabilitation, 33(1), 63 -72. doi: 10. 3109/09638288. 2010. 488711 American Foundation for the Blind. (2015 a). Lighting and glare. Retrieved from http: //www. visionaware. org/info/everyday-living/home-modification-/lighting-and-glare/123 American Foundation for the Blind. (2015 b). What are low vision optical devices? Retrieved from http: //www. visionaware. org/info/your-eye-condition/eye-health/low-vision-opticaldevices/1235 American Occupational Therapy Association. (2007). AOTA’s Centennial Vision and executive summary. The American Journal of Occupational Therapy, 61(6), 613 -614. American Occupational Therapy Association. (2014). Occupational therapy framework: Domain and process (3 rd ed. ). The American Journal of Occupational Therapy, 68, S 1 -S 51. American Occupational Therapy Association. (n. d. a). Emerging niche in productive aging. Retrieved from http: //www. aota. org/Practice/Productive-Aging/Emerging-Niche/Low-Vision. aspx American Occupational Therapy Association. (n. d. b). Living with low vision. Retrieved from http: //www. aota. org/about-occupational-therapy/; atients-clients/adults/lowvision. aspx American Optometric Association. (2015 a). Glaucoma. Retrieved from http: //www. aoa. org/patientsand-public/eye-and-vision-problems/glossary-of-eye-and-vision-conditions/glaucoma? sso=y

References American Optometric Association. (2015 b). Low vision. Retrieved from http: //www. aoa. org/patients-and -public/caring-for-your-vision/low-vision? sso=y American Optometric Association. (2015 c). Visual Acuity: What is 20/20 vision? Retrieved from http: //www. aoa. org/patients-and-public/eye-and-vision-problems/glossary-of-eye-and-visionconditions/visual-acuity? sso=y Ball, E. , & Nicolle, C. (2015). Changing what it means to be “normal”: A grounded theory study of the mobility choices of people who are blind or have low vision. Journal of Visual Impairment & Blindness, 109(4), 291 -301. Barstow, B. A. , Bennett, D. K. , & Vogtle, L. K. (2011). Perspectives on home safety: Do home safety assessments address the concerns of clients with vision loss? The American Journal of Occupational Therapy, 65(6), 635 -642. Barstow, B. , Warren, M. , Thaker, S. , Hallman, A. , & Batts, P. (2015). Client and therapist perspectives on the influence of low vision and chronic conditions on performance and occupational therapy intervention. The American Journal of Occupational Therapy, 69(3), 1 -8. Berger, S. , Mc. Ateer, J. , Schreier, K. , & Kaldenberg, J. (2013). Occupational therapy interventions to improve leisure and social participation for older adults with low vision: A systematic review. The American Journal of Occupational Therapy, 67(3), 303 -311. Blaylock, S. , Barstow, B. , Vogtle, L. , & Bennett, D. (2015). Understanding the occupational performance experiences of individuals with low vision. British Journal of Occupational Therapy, 78(7), 412 -421. doi: 10. 1177/030802215577641

References Campion, C. , Awang, D. , & Ward, G. (2010). Broadening the vision: The education and training needs of occupational therapists working with people with sight loss. British Journal of Occupational Therapy, 73(9), 413 -421. Center for Evidence-Based Medicine. (2011). OCEBM levels of evidence. Retrieved from www. /cebm. net/ocebm-levels-of-evidence/ Copolillo, A. , & Teitelman, J. (2005). Acquisition and integration of low vision assistive devices: Understanding the decision-making process of older adults with low vision. The American Journal of Occupational Therapy, 59(3), 305 -313. Eklund, K. , Sjostrand, J. , & Dahlin-Ivanoff, S. (2008). A randomized controlled trial of a health-promotion programme and its effect on ADL dependence and self-reported health problems for the elderly visually impaired. Scandinavian Journal of Occupational Therapy, 15, 68 -74. doi: 0. 1080/11038120701442963 Fisk, M. , & Raynham, P. (2014). Assistive lighting for people with sight loss. Disability & Rehabilitation: Assistive Technology, 9(2), 128 -135. Fok, D. , Polgar, J. , Shaw, L. , & Jutai, J. (2011). Low vision assistive technology device usage and importance in daily occupations. Work, 39, 37 -48. doi: 10. 3233/WOR-2011 -1149 Folstein, M. , Folstein, S. , & Mc. Hugh, P. (1975). “Mini-Mental State”: A practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research, 12, 189 -198. doi: 10. 1016/0022 -3956(75)90026 -6 Gaffney, A. , Margrain, T. , Bunce, C. , & Binns, A. (2014). How effective is eccentric viewing training? A systematic literature review. Ophthalmic & Physiological Optics, 34, 427 -437.

References Galbraith, J. (n. d. ). Living well with low vision: Self-training in eccentric viewing. Retrieved from http: //lowvision. preventblindness. org/library/low-vision-rehabilitation/self-training-in-eccentric-viewing Girdler, S. , Boldy, D. , Dhaliwal, S. , Crowley, M. , & Packer, T. (2010). Vision self-management for older adults: A randomised controlled trial. British Journal of Ophthalmology, 94(2), 223 -228. Girdler, S. , Packer, T. , & Boldy, D. (2008). The impact of age-related vision loss. Occupational Therapy Journal of Research, 28(3), 110 -120. Hong, S. , Park, H. , Kwon, J. , & Yoo, E. (2014). Effectiveness of eccentric viewing training for daily visual activities for individuals with age-related macular degeneration: A systematic review and meta-analysis. Neuro. Rehabilitation, 34(3), 587 -595. Horowitz, A. , Brennan, M. , Reinhardt, J. , & Mac. Millan, T. (2006). The impact of assistive device use on disability and depression among older adults with age-related vision impairments. Journal of Gerontology, 61 B, S 274 -S 280. Keller, H. (1996). In C. Ward (Ed. ). Helen Keller: The story of my life (Dover Print Editions ed. ). New York: Dover Publications Inc. Laitinen, A. , Sainio, P. , Koskinen, S. , Rudanko, S. , Laatikainen, L. , & Aromaa, A. (2007). The association between visual acuity and functional limitations: Findings from a nationally representative population survey. Ophthalmic Epidemiology, 14, 333 -342. doi: 10. 1080/01658100701473713 Law, M. , Baptiste, S. , Carswell, A. , Mc. Coll, M. , Polatajko, H. , & Pollock, N. (2014). COPM: Canadian Occupational Performance Measure (5 th ed. ). Ottawa, Ontario: CAOT Publications ACE.

References Law, M. , Cooper, B. , Strong, S. , Stewart, D. , Rigby, P. , & Letts, L. (1996). The person-environment-occupation model: A transactive approach to occupational performance. Canadian Journal of Occupational Therapy, 63(1), 9 -23. Liu, C. , Brost, M. , Horton, V. , Kenyon, S. , & Mears, K. (2013). Occupational therapy interventions to improve performance of daily activities at home for older adults with low vision: A systematic review. The American Journal of Occupational Therapy, 67(3), 279 -287. Mansfield, J. , Legge, G. , Ludbker, A. , & Cunningham, K. (1994). MNRead Acuity Charts: Continuous-text reading -acuity charts for normal and low vision. Long Island City, NY: Lighthouse Low Vision Products. Marinoff, R. (2012). Referral patterns in low vision: A survey of mid-south tri-state eye care providers. Journal of Behavioral Optometry, 23(1), 13 -23. Markowitz, S. , Kent, C. , Schuchard, R. , & Fletcher, D. (2008). Ability to read medication labels improved by participation in a low vision rehabilitation program. Journal of Visual Impairment & Blindness, 102(12), 774 -777. Mohler, A. , Neufeld, P. , & Perlmutter, M. (2015). Factors affecting readiness for low vision interventions in older adults. The American Journal of Occupational Therapy, 69(4), 1 -10. National Eye Institute. (2009). Facts about cataract. Retrieved from https: //nei. nih. gov/health/cataract_facts National Eye Institute. (2015 a). Facts about age-related macular degeneration. Retrieved from https: //nei. nih. gov/health/maculardegen/armd_facts

References National Eye Institute. (2015 b). Facts about diabetic eye disease. Retrieved from https: //nei. nih. gov/health/diabetic/retinopathy National Eye Institute. (n. d. a). Facts about glaucoma. Retrieved from https: //nei. nih. gov/health/glaucoma_facts National Eye Institute. (n. d. b). Information for healthy vision: Low vision. Retrieved from http: //nei. nih. gov/lowvision Nguyen, N. , Weismann, M. , & Trauzettel-Klosinski, S. (2009). Improvement of reading speed after providing of low vision aids in patients with age-related macular degeneration. Acta Ophthalmologica, 87, 849 -853. Ortman, J. , Velkoff, V. , & Hogan, H. (2014). An aging nation: The older population in the United States. Retrieved from https: //www. census. gov/prod/2014 pubs/p 25 -1140. pdf Perlmutter, M. , Bhorade, A. , Gordon, M. , Hollingsworth, H. , & Baum, M. C. (2010). Cognitive, visual, auditory, and emotional factors that affect participation in older adults. The American Journal of Occupational Therapy, 64(4), 570 -579. Perlmutter, M. , Bhorade, A. , Gordon, M. , Hollingsworth, H. , Engsberg, J. , & Baum, M. C. (2013). Home lighting assessment for clients with low vision. The American Journal of Occupational Therapy, 67(6), 674 -682. Russell-Minda, E. , Jutai, J. , Strong, G. , Campbell, K. , Gold, D. , Pretty, L. , & Wilmot, L. (2007). The legibility of typefaces for readers with low vision: A research review. Journal of Visual Impairment & Blindness, 101(7), 402 -415.

References Smallfield, S. , Clem, K. , & Myers, A. (2013). Occupational therapy interventions to improve the reading ability of older adults with low vision: A systematic review. The American Journal of Occupational Therapy, 67(3), 288 -295. Sokol-Mckay, D. , & Michels, D. (2005). Facing the challenges of macular degeneration: Therapeutic interventions for low vision. OT Practice, 10(9), 10 -15. Spence, C. (2014). The skin as a medium for sensory substitution. Multisensory Research, 27(5), 293 -312. Trombly, C. (2008). Conceptual foundations for practice. In M. Radomski, & C. Trombly (Eds. ), Occupational therapy for physical dysfunction (6 th ed. , pp. 1 -22). Philadelphia: Lippincott, Williams, & Wilkins. Vukicevic, M. , & Fitzmaurice, K. (2009). Eccentric viewing training in the home environment: Can it improve the performance of activities of daily living? Journal of Visual Impairment & Blindness, 103(5), 277 - 290. Warren, M. (1998). Brain Injury Visual Assessment Battery for Adults. Lenexa, KS: vis. ABILITIES Rehab Services. Williams, M. , Ray, C. , Griffith, J. , & De l’Aune, W. (2011). The use of a tactile-vision sensory substitution system as an augmentative tool for individuals with visual impairments. Journal of Visual Impairment & Blindness, 105(1), 4550. Winner, S. , Yuen, H. , Vogtle, L. , & Warren, M. (2014, January/February). Factors associated with comfort level of occupational therapy practitioners in providing low vision services. American Journal of Occupational Therapy, 68, 96 -101. doi: 10. 5014/ajot. 2014. 009142

Kimberly Holt, OTR, OTD 409 -790 -0219 Kimberly_holt@hotmail. com
- Slides: 158