Evidencebased chiropractic and documentation 1 2006 Good clinical

Evidence-based chiropractic and documentation 1 © 2006

Good clinical documentation • A record of a patient’s subjective complaints, objective findings, assessment, and plan for case management • Should represent the thought processes involved in patient care • Provides evidence of the patient’s progress Evidence-based Chiropractic 2 © 2006

Good clinical documentation (cont. ) • Practitioners are able to monitor patient progress accurately using good clinical documentation – Facilitates making the best possible clinical decisions • May alleviate problems associated with third party record reviews and medicolegal issues Evidence-based Chiropractic 3 © 2006

The value of valid & reliable outcome measures (OMs) • Beneficial to – Patients, because they are more likely to receive appropriate care – Practitioners, who use the information to formulate diagnoses and plan care – Third-party payers and patients, who will be more likely to receive legitimate services in return for monetary expenditures Evidence-based Chiropractic 4 © 2006

Utility of OMs • The utility of a test refers to its usefulness in meeting the needs of the patient, referrer, and payer • An OM should be sensitive to change – It should change in direct association with actual changes that occur in the patient characteristic being measured – Responsiveness Evidence-based Chiropractic 5 © 2006

Clinical practice guidelines • Systematically developed statements to assist practitioner and patient decisions about appropriate health care for specific clinical circumstances – Developed by experts in a field using an organized process – Evidence is assembled on the management of the kinds of conditions handled by practitioners Evidence-based Chiropractic 6 © 2006

Clinical practice guidelines development • Best evidence is located to give clinicians tools to provide optimal patient care • Steps in guidelines development 1. 2. 3. 4. 5. The subject area of the guideline is identified Guideline development groups are assembled Evidence is obtained and assessed Evidence is shaped into a clinical guideline The guideline is reviewed externally Evidence-based Chiropractic 7 © 2006

Consensus opinions • Expert opinions are sought when there is little or no scientific evidence available • One must consider that they are merely the opinions of a panel of experts • The Delphi method – A method often used in guidelines development to establish a group position – Involves serial input from a group of panel members via questionnaires Evidence-based Chiropractic 8 © 2006
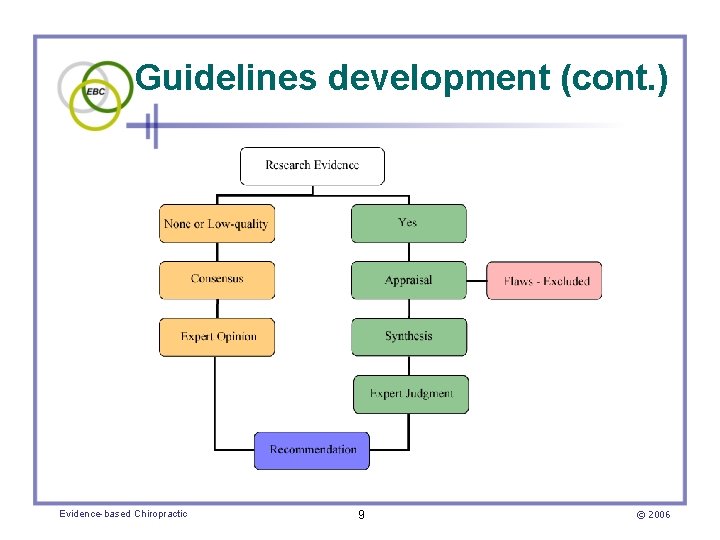
Guidelines development (cont. ) Evidence-based Chiropractic 9 © 2006

Guidelines differ in quality • Quality depends on the rigor of the methods used in their development – e. g. , the Guidelines for Chiropractic Quality Assurance and Practice Parameters (Mercy guidelines) • Evidence-based guidelines – Follow a rigorous development process – Are based on the highest quality scientific evidence Evidence-based Chiropractic 10 © 2006

Guidelines may have disadvantages • Evidence on a condition or treatment may be unavailable or of low-quality – In which case guidelines may only serve to inform clinicians about the lack of evidence • Guidelines only address one condition at a time – However, in practice patients often present with several complaints Evidence-based Chiropractic 11 © 2006

Guidelines - disadvantages (cont. ) • Recommended treatment options may not always be appropriate – Each patient is unique – There may be contraindications to treatment – Patient preferences must be considered • Consequently, guidelines should never be utilized as a treatment “cookbook” Evidence-based Chiropractic 12 © 2006

Guidelines - disadvantages (cont. ) • Guidelines should be updated periodically to incorporate new information – Although the time-frame for updates is variable – Depends on how rapidly change occurs in a topic or field • The Mercy guidelines mentioned that they should be updated, but never were Evidence-based Chiropractic 13 © 2006

Assessing the validity of guidelines • Were good development methods used? – Methods should be thoroughly described – Rigorous systematic methods of evidence selection and appraisal should be used • Will the recommendations facilitate the care of your patients? – Should be applicable to the chiropractic setting and to chiropractic patients Evidence-based Chiropractic 14 © 2006

Assessing the validity of guidelines (cont. ) • Are the patient populations from the source articles similar to your patients? – For instance, disease prevalence or risk factors may be different • Keep in mind that guidelines are not prescriptive statements – They are designed to provide assistance and direction to patient care Evidence-based Chiropractic 15 © 2006

Best practices • The organizational use of evidence to improve practice • Definition – Activities, disciplines and methods that are available to identify, implement and monitor the available evidence in health care • Sometimes confused with clinical guidelines, but they are actually different Evidence-based Chiropractic 16 © 2006

OMs commonly used in chiropractic • The choice of OMs depends on – Objectives for the patient or requirements of the party or stakeholder who will receive the information • OMs useful to clinicians and patients involve measures such as pain and function • Payers are interested in cost-efficient patient management and patient satisfaction • Employers may be interested in seeing their injured employees return to work ASAP Evidence-based Chiropractic 17 © 2006

Health-related quality of life (HRQL) measures • Questionnaires that are designed to assess the physical, psychological, emotional, and social well-being of patients • Reported from the patient’s perspective – Criticized as being subjective and unreliable – However, HRQL measures are typically more reliable than “objective” OMs Evidence-based Chiropractic 18 © 2006

HRQL measures (cont. ) • Findings are meaningful to patients • HRQL measures are helpful in the assessment of patients’ functional limitations • They are appropriate and useful in monitoring the effects of treatment Evidence-based Chiropractic 19 © 2006

Two general categories of HRQL measures • Generic instruments – Designed to evaluate patients’ overall health status – e. g. , the SF-36 health survey and the Sickness Impact Profile • Specific instruments – Designed to assess specific conditions, patient groups, or areas of function – e. g. , the Neck Disability Index Evidence-based Chiropractic 20 © 2006

General categories of HRQL measures (cont. ) • Condition-specific instruments have advantages over generic – They evaluate elements of function that are relevant to the specific condition under consideration – As a result, they are generally more responsive to changes in patients’ primary conditions Evidence-based Chiropractic 21 © 2006

Measures of pain • Measures of pain and function are the most commonly used OMs in chiropractic • It is not possible to measure pain directly – It must be estimated from replies to oral or written queries – The process can be influenced by the patient’s culture, conditioning, education, etc. – Then the pain replies must be interpreted by the clinician Evidence-based Chiropractic 22 © 2006

Measures of pain (cont. ) • Quite a few tools are available that can convert the subjective experience of pain into valid and reliable measures • Once chosen, the same instrument should be used for follow-up evaluations Evidence-based Chiropractic 23 © 2006

Numeric Rating Scale (NRS) • a. k. a. , numeric pain scale or 11 -point pain scale • Very common in research and practice • Patients estimate the severity of their pain on a 0 to 10 scale – 0 = no pain – 10 = worst possible pain Evidence-based Chiropractic 24 © 2006

NRS (cont. ) • Patients are asked to circle the number that matches their level of pain • May be used verbally • e. g. , “On a 0 to 10 scale, where 0 means no pain and 10 is the worst possible pain, what is your level of pain? ” Evidence-based Chiropractic 25 © 2006

NRS (cont. ) • Interpretation of the intensity of NRS pain scores – 1 -4 = mild pain – 5 -6 = moderate pain – 7+ = severe pain • 101 -point NRS (NRS-101) – Occasionally encountered in the literature – Provides little more than the 11 -point scale Evidence-based Chiropractic 26 © 2006
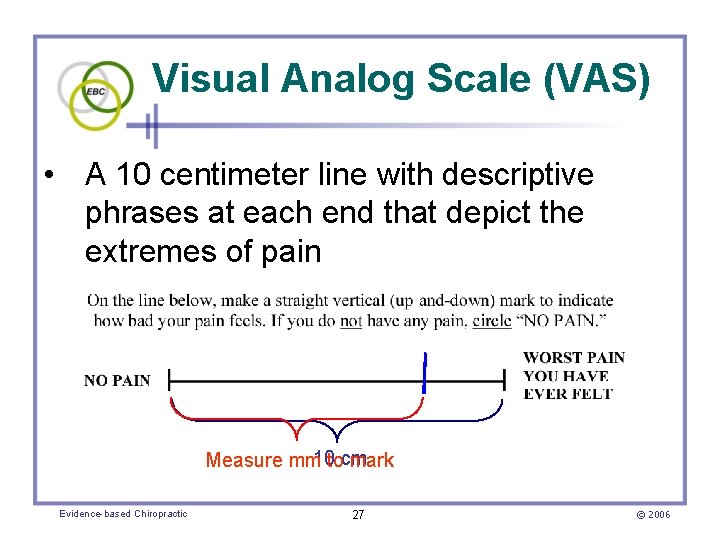
Visual Analog Scale (VAS) • A 10 centimeter line with descriptive phrases at each end that depict the extremes of pain 10 cm Measure mm to mark Evidence-based Chiropractic 27 © 2006

Other uses of NRS & VAS • Measure the impact pain has on daily living – e. g. , sleep interference and lifting capacity COMPLETELY INTERFERES DOES NOT INTERFERE • Can also be adapted to assess anxiety or depression levels in patients Evidence-based Chiropractic 28 © 2006

Characteristic Pain Intensity (CPI) • A scale that averages the patient’s pain levels right now, typical or on average, and when it is at its worst • Patients presenting for evaluation at a particularly good or bad time are able to convey their true pain level better • Uses 3 VAS pain intensity ratings that represent different points in time Evidence-based Chiropractic 29 © 2006

CPI (cont. ) Evidence-based Chiropractic 30 © 2006

CPI (cont. ) • In research, the CPI correlated better with measures of pain-related disability, pain medication use, and standard pain measures than individual ratings • CPI scores were more normally distributed Evidence-based Chiropractic 31 © 2006

Verbal Rating Scales (VRS) • A scale that depicts pain intensity using a series of adjectives that reflect the extremes of pain (e. g. , from no pain to intense pain) • Patients are asked to choose the adjective that best describes their pain level by selecting from a list of possibilities Evidence-based Chiropractic 32 © 2006
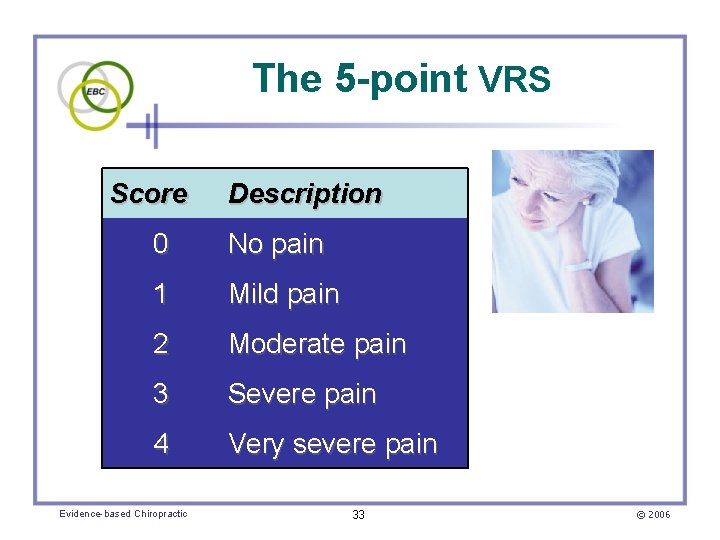
The 5 -point VRS Score Description 0 No pain 1 Mild pain 2 Moderate pain 3 Severe pain 4 Very severe pain Evidence-based Chiropractic 33 © 2006

VRS (Cont. ) • The VRS is preferred by patients because of its simplicity • It is not as sensitive or reliable as other pain scales • VRS data can easily be misinterpreted because word descriptions may not have the same meaning for different persons Evidence-based Chiropractic 34 © 2006

Tenderness Rating Scales • Used to quantify the degree of discomfort associated with palpation, typically of myofascial tissues • The patient’s interpretation of tenderness is correlated with the examiner’s observation of their reaction to a pain stimulus which can help objectify information gained from palpation Evidence-based Chiropractic 35 © 2006

Tenderness rating of soft tissue Grade 0 1 2 3 4 Evidence-based Chiropractic Definition No tenderness Mild tenderness without grimace or flinch Moderate tenderness with grimace or flinch Severe tenderness with marked flinch or withdrawal Unbearable tenderness, patient withdraws with light touch 36 © 2006

Pain drawings • Patients simply shade or mark the regions of a blank body image where they are experiencing pain • Can be used independently or incorporated into questionnaires • Their utility can be enhanced when used along with other OMs Evidence-based Chiropractic 37 © 2006
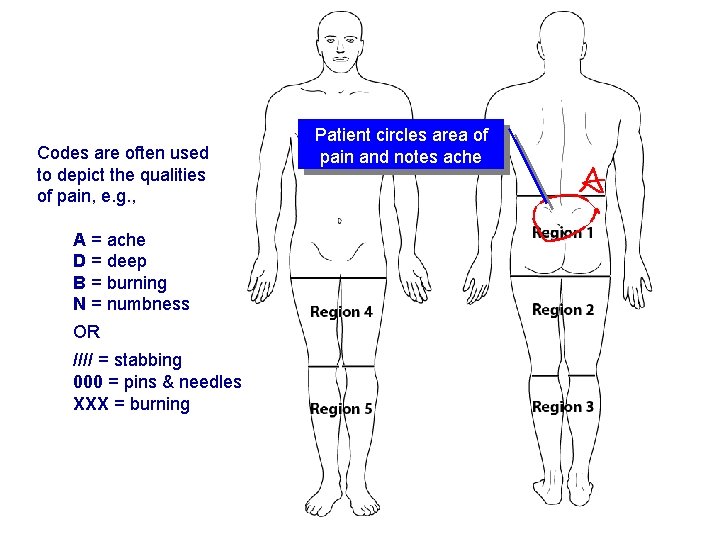
Pain drawings (cont. ) Codes are often used to depict the qualities of pain, e. g. , Patient circles area of pain and notes ache A = ache D = deep B = burning N = numbness OR //// = stabbing 000 = pins & needles XXX = burning Evidence-based Chiropractic 38 © 2006
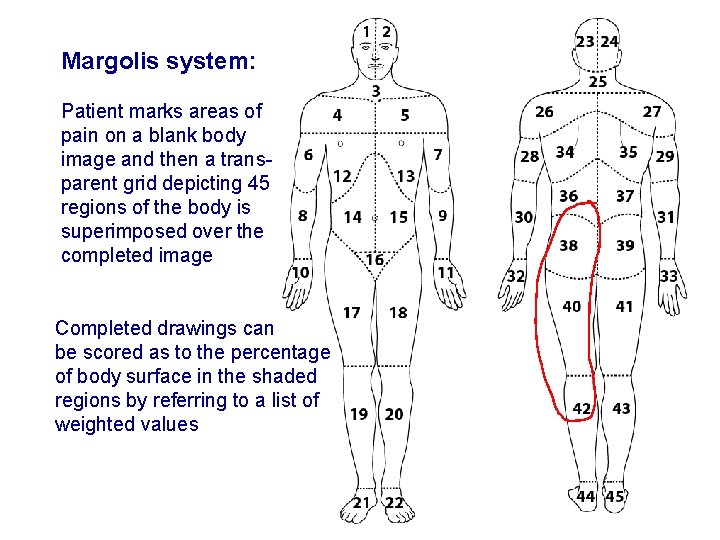
Margolis system: Patient marks areas of pain on a blank body image and then a transparent grid depicting 45 regions of the body is superimposed over the completed image Completed drawings can be scored as to the percentage of body surface in the shaded regions by referring to a list of weighted values Evidence-based Chiropractic 39 © 2006
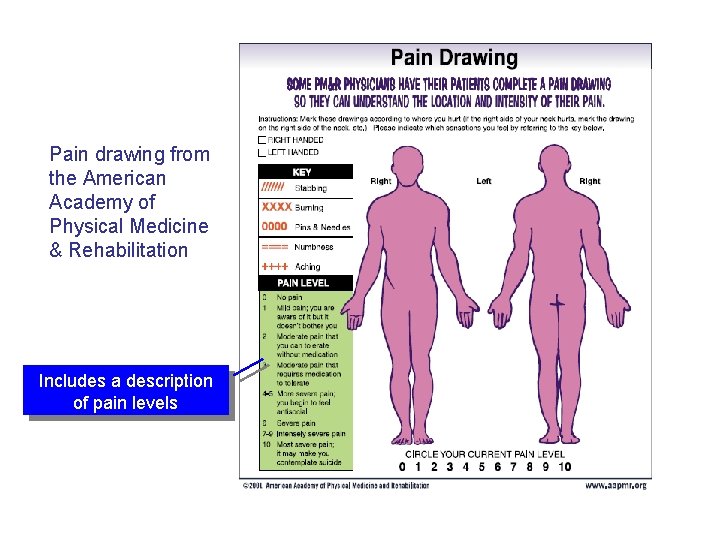
Pain drawing from the American Academy of Physical Medicine & Rehabilitation Includes a description of pain levels Evidence-based Chiropractic 40 © 2006

Pain drawings (cont. ) • Test-retest reliability has been established in several studies, even when administered in diverse settings • Sometimes used by clinicians to identify psychological disturbances in patients – However, this method has low sensitivity and positive predictive value Evidence-based Chiropractic 41 © 2006

Mc. Gill Pain Questionnaire (MPQ) • Developed by Melzak in 1975 • Provides a quantitative measure of pain • One of the most widely tested pain measures of all time – Often used as a gold standard, against which newly developed pain instruments are tested Evidence-based Chiropractic 42 © 2006

MPQ (cont. ) • Made up of 3 major classes of word descriptors, including words that describe – Sensory qualities – Affective, in terms of tension, fear, and autonomic responses to the pain – Evaluative words that describe the intensity of the pain Evidence-based Chiropractic 43 © 2006

MPQ (cont. ) • Consists of 4 major parts: 1. A pain drawing 2. 78 pain descriptors (e. g. , sharp, intense, pinching) that span 20 categories 3. Questions that assess how the pain changes over time and what relieves or increases it 4. A pain intensity section Evidence-based Chiropractic 44 © 2006
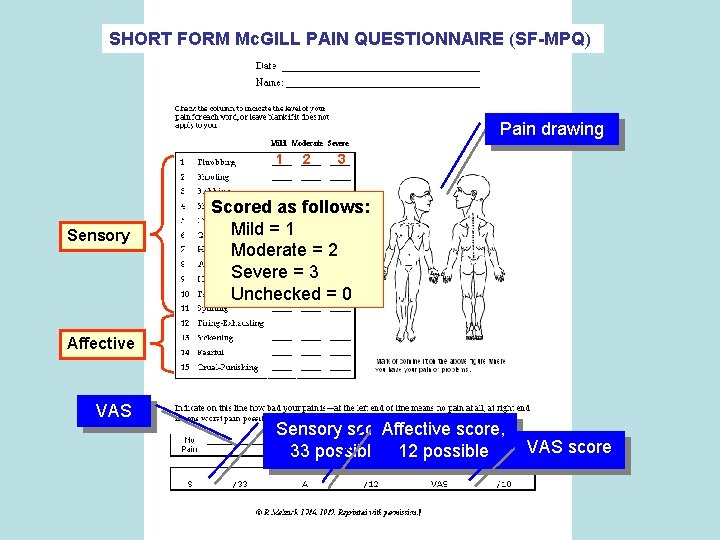
SHORT FORM Mc. GILL PAIN QUESTIONNAIRE (SF-MPQ) Pain drawing 1 Sensory 2 3 Scored as follows: Mild = 1 Moderate = 2 Severe = 3 Unchecked = 0 Affective VAS Evidence-based Chiropractic Sensory score, Affective score, VAS score 33 possible 12 possible 45 © 2006

Psychometric measures • Questionnaires that deal with patients’ emotional and psychological state • Chronic pain can bring about anxiety, depression, and hopelessness • It can aggravate existing depression • In some cases, depression cause chronic pain Evidence-based Chiropractic 46 © 2006

Psychometric measures (cont. ) • Psychometric questionnaires can be used by chiropractors to screen pain patients • Mild depression associated with pain can be monitored • When persistent or more than mild, some patients may need a psychological referral Evidence-based Chiropractic 47 © 2006

Beck Depression Inventory (BDI) • The most commonly used selfadministered scale for measuring depression world-wide • Can be integrated into a busy clinical practice without difficulty – Requires no special training to administer • 21 items dealing with statements about how patients perceive themselves Evidence-based Chiropractic 48 © 2006

BDI (cont. ) • For example – – 0 – “I don't feel disappointed in myself” 1 – “I am disappointed in myself” 2 – “I am disgusted with myself” 3 – “I hate myself” • Score 10 -18, patient is mildly depressed • 19 -21 may have borderline clinical depression Evidence-based Chiropractic 49 © 2006

BDI (cont. ) • The test’s validity and reliability has been established • It has high internal consistency and high content validity • Good discriminate validity – Is able to distinguish depressed from nondepressed subjects • It is sensitive to change Evidence-based Chiropractic 50 © 2006

Symptom Checklist-90 -Revised (SCL-90 -R) • A psychometric questionnaire that can be used to assess pain in musculoskeletal patients • Contains 90 items that can be completed in 12 -15 minutes • Each item is graded on a five-point (0 -4) scale of distress that ranges from “not at all” to “extremely” Evidence-based Chiropractic 51 © 2006

SCL-90 -R (cont. ) • Its reliability, validity, and utility has been well-established • Can be used by all types of health care professionals to screen patients for psychological involvement Evidence-based Chiropractic 52 © 2006

Measures of function • Questionnaires that evaluate activity limitations associated with a variety of conditions – e. g. , back pain, knee pain, asthma • General health assessment questionnaires and many physical tests are also considered measures of function Evidence-based Chiropractic 53 © 2006

Oswestry Disability Index (ODI) • a. k. a. , Oswestry low back pain disability questionnaire • One of the most commonly used OMs in the management of spinal disorders • Its validity and reliability has been well established • It is appropriate for both research and clinical practice Evidence-based Chiropractic 54 © 2006

ODI (cont. ) • At least four versions are available • The original authors recommend that the ODI 2. 0 version be used • The Revised ODI omitted the original section 8 that deals with sex, replacing it with a section about the changing degree of pain Section 8: Sex Life My sex life is normal and causes no extra pain. My sex life is normal but causes some extra pain. My sex life is nearly normal but is very painful. My sex life is severely restricted by pain. My sex life is nearly absent because of pain. Pain prevents any sex life at all Evidence-based Chiropractic 55 © 2006

ODI (cont. ) • Consists of 10 sections that each have 6 statements dealing with activities of daily living and pain – Is self-administered – Typically completed in less than 5 minutes – Scoring is straightforward and can be performed by a staff member • Statements describe the level of disability associated with various activities Evidence-based Chiropractic 56 © 2006

ODI (cont. ) • Scoring – A value is assigned for statements ranging from 0 to 5 – The first statement has a value of 0 and the last statement a 5 • If a patient chooses more than one box in a section, the highest score is to be taken • Statement values from each section are then combined to get a total score Evidence-based Chiropractic 57 © 2006

ODI (cont. ) Total scored ODI score (%) = 100 Total possible score • Where – Total scored is the total of all the statements selected by the patient – Total possible score is the number of sections completed by the patient times five Evidence-based Chiropractic 58 © 2006

ODI (cont. ) 18 ODI score (%) = 100 = 40% 45 Not 50 because the patient left out a section • If the patient completes all 10 sections, simply multiply their raw score by 2 to convert to a percentage Evidence-based Chiropractic 59 © 2006
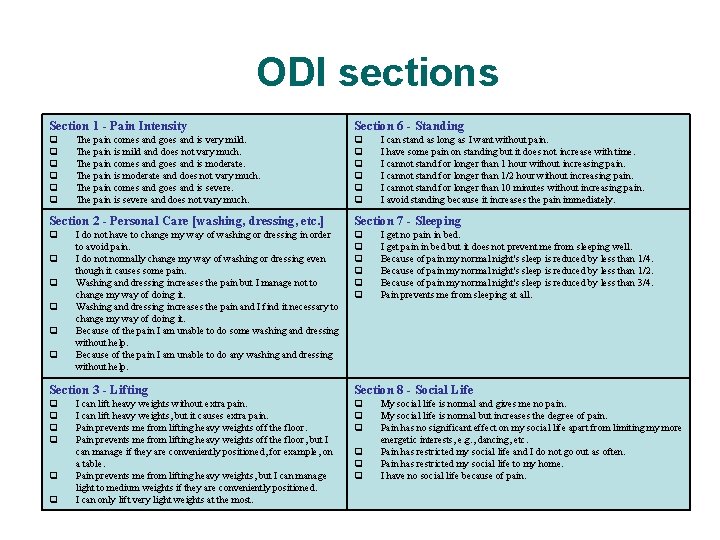
ODI sections Section 1 - Pain Intensity Section 6 - Standing The pain comes and goes and is very mild. The pain is mild and does not vary much. The pain comes and goes and is moderate. The pain is moderate and does not vary much. The pain comes and goes and is severe. The pain is severe and does not vary much. I can stand as long as I want without pain. I have some pain on standing but it does not increase with time. I cannot stand for longer than 1 hour without increasing pain. I cannot stand for longer than 1/2 hour without increasing pain. I cannot stand for longer than 10 minutes without increasing pain. I avoid standing because it increases the pain immediately. Section 2 - Personal Care [washing, dressing, etc. ] Section 7 - Sleeping I do not have to change my way of washing or dressing in order to avoid pain. I do not normally change my way of washing or dressing even though it causes some pain. Washing and dressing increases the pain but I manage not to change my way of doing it. Washing and dressing increases the pain and I find it necessary to change my way of doing it. Because of the pain I am unable to do some washing and dressing without help. Because of the pain I am unable to do any washing and dressing without help. I get no pain in bed. I get pain in bed but it does not prevent me from sleeping well. Because of pain my normal night's sleep is reduced by less than 1/4. Because of pain my normal night's sleep is reduced by less than 1/2. Because of pain my normal night's sleep is reduced by less than 3/4. Pain prevents me from sleeping at all. Section 3 - Lifting Section 8 - Social Life I can lift heavy weights without extra pain. I can lift heavy weights, but it causes extra pain. Pain prevents me from lifting heavy weights off the floor, but I can manage if they are conveniently positioned, for example, on a table. Pain prevents me from lifting heavy weights, but I can manage light to medium weights if they are conveniently positioned. I can only lift very light weights at the most. Evidence-based Chiropractic 60 My social life is normal and gives me no pain. My social life is normal but increases the degree of pain. Pain has no significant effect on my social life apart from limiting my more energetic interests, e. g. , dancing, etc. Pain has restricted my social life and I do not go out as often. Pain has restricted my social life to my home. I have no social life because of pain. © 2006
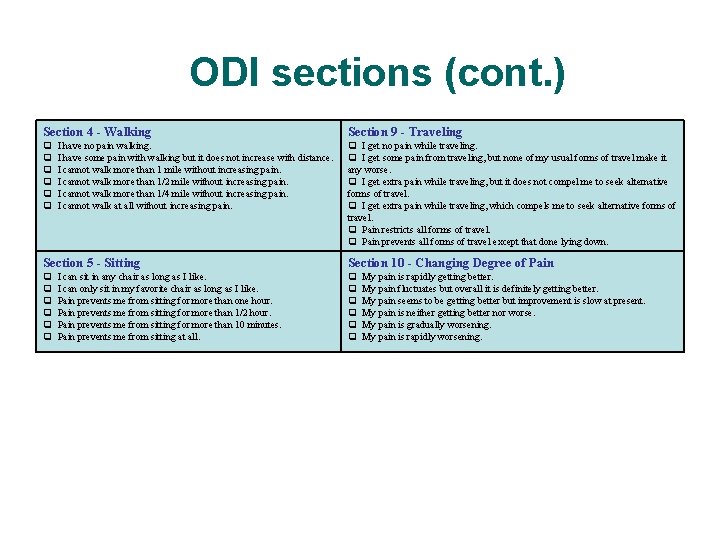
ODI sections (cont. ) Section 4 - Walking Section 9 - Traveling I get no pain while traveling. I get some pain from traveling, but none of my usual forms of travel make it any worse. I get extra pain while traveling, but it does not compel me to seek alternative forms of travel. I get extra pain while traveling, which compels me to seek alternative forms of travel. Pain restricts all forms of travel. Pain prevents all forms of travel except that done lying down. I have no pain walking. I have some pain with walking but it does not increase with distance. I cannot walk more than 1 mile without increasing pain. I cannot walk more than 1/2 mile without increasing pain. I cannot walk more than 1/4 mile without increasing pain. I cannot walk at all without increasing pain. Section 5 - Sitting Section 10 - Changing Degree of Pain I can sit in any chair as long as I like. I can only sit in my favorite chair as long as I like. Pain prevents me from sitting for more than one hour. Pain prevents me from sitting for more than 1/2 hour. Pain prevents me from sitting for more than 10 minutes. Pain prevents me from sitting at all. Evidence-based Chiropractic My pain is rapidly getting better. My pain fluctuates but overall it is definitely getting better. My pain seems to be getting better but improvement is slow at present. My pain is neither getting better nor worse. My pain is gradually worsening. My pain is rapidly worsening. 61 © 2006
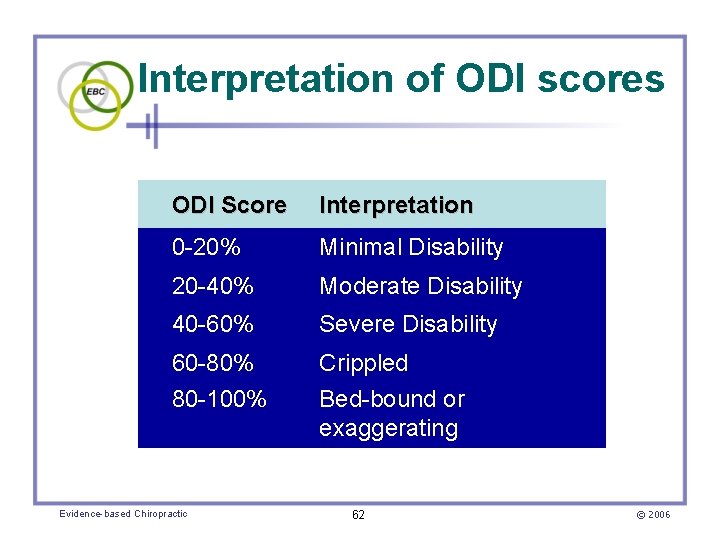

Interpretation of ODI scores ODI Score Interpretation 0 -20% Minimal Disability 20 -40% Moderate Disability 40 -60% Severe Disability 60 -80% 80 -100% Crippled Bed-bound or exaggerating Evidence-based Chiropractic 62 © 2006

ODI clinically important difference • In order to distinguish patients who have improved from those who have not, the minimum clinically important difference that is needed is 6 ODI points – Other researchers have calculated it to be as high as 15 points • To be clinically important, a patient would have to improve by at least 6 ODI points Evidence-based Chiropractic 63 © 2006

Roland-Morris Questionnaire (RMQ) • Has been shown to be a valid and reliable instrument for the assessment of low back disability • Sensitive to change over time for low back pain patients • Its popularity is comparable with ODI Evidence-based Chiropractic 64 © 2006

RMQ (cont. ) • Consists of 24 questions that deal with low back pain and function • Can be completed by patients in about 5 minutes • Can be scored by the doctor or a staff member in about one minute 0 = no pain and normal function 24 = maximum pain and diminished function Evidence-based Chiropractic 65 © 2006

RMQ (cont. ) • When compared with the ODI, the Roland. Morris was found to be simpler, faster and more acceptable to patients • RMQ is a more sensitive measure of activity intolerances in acute and subacute patients • ODI is more sensitive for identifying activity intolerances in chronic patients Evidence-based Chiropractic 66 © 2006

RMQ questions 1. I stay at home most of the time because of my back. 2. I change position frequently to try to get my back comfortable. 3. I walk more slowly than usual because of my back. 4. Because of my back, I am not doing any jobs that I usually do around the house. 5. Because of my back, I use a handrail to get upstairs. 6. Because of my back, I lie down to rest more often. 7. Because of my back, I have to hold on to something to get out of an easy chair. 8. Because of my back, I try to get other people to do things for me. 9. I get dressed more slowly than usual because of my back. 10. I only stand up for short periods of time because of my back. 11. Because of my back, I try not to bend or kneel down. 12. I find it difficult to get out of a chair because of my back. 13. My back is painful almost all of the time. 14. I find it difficult to turn over in bed because of my back. 15. My appetite is not very good because of my back. 16. I have trouble putting on my sock (or stockings) because of the pain in my back. 17. I can only walk short distances because of my back pain. 18. I sleep less well because of my back. 19. Because of my back pain, I get dressed with the help of someone else. 20. I sit down for most of the day because of my back. 21. I avoid heavy jobs around the house because of my back. 22. Because of back pain, I am more irritable and bad tempered with people than usual. 23. Because of my back, I go upstairs more slowly than usual. 24. I stay in bed most of the time because of my back. RMQ score = 4 Evidence-based Chiropractic 67 © 2006

RMQ (cont. ) • Roland Morris did not provide an interpretation of the varying degrees of disability as in ODI – However, scores of 13 or more denote significant disability and an unfavorable outcome (Von Korff and Saunders) • Clinical improvements over time can be graded based on the analysis of serial questionnaires Evidence-based Chiropractic 68 © 2006

RMQ (cont. ) • Percentage of improvement can be calculated as follows: Baseline RMQ score - Follow-up RMQ score Baseline RMQ score 100 • For example: – If a patient’s baseline score was 12 and post score 2 12 -2 12 Evidence-based Chiropractic 100 = 83% improvement 69 © 2006

RMQ clinically important difference • The minimum clinically important difference for RMQ evaluations was 4 to 5 points in one study and 8. 6 to 9. 5 in another • A patient would have to improve by at least 4 RMQ points in order to consider their condition as being improved Evidence-based Chiropractic 70 © 2006

Neck Disability Index (NDI) • A modification of the Oswestry Low Back Pain Disability Index – Developed in 1989 by Howard Vernon, DC • In 1991, Vernon and Mior published a study in JMPT on its reliability and validity • Ten other studies have confirmed the original report’s findings Evidence-based Chiropractic 71 © 2006
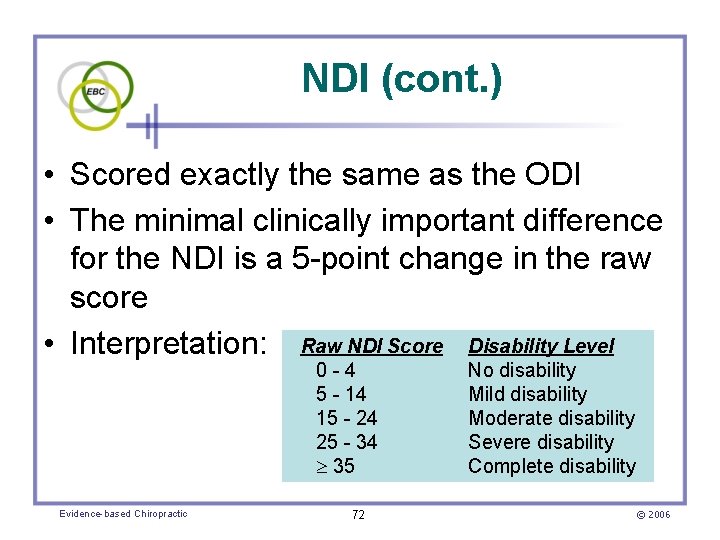
NDI (cont. ) • Scored exactly the same as the ODI • The minimal clinically important difference for the NDI is a 5 -point change in the raw score • Interpretation: Raw NDI Score Disability Level 0 - 4 5 - 14 15 - 24 25 - 34 35 Evidence-based Chiropractic 72 No disability Mild disability Moderate disability Severe disability Complete disability © 2006

Example NDI section • Section 1 - Pain Intensity I have no pain at the moment. The pain is very mild at the moment. The pain is moderate at the moment. The pain is fairly severe at the moment. The pain is very severe at the moment. The pain is the worst imaginable at the moment. Evidence-based Chiropractic 73 © 2006

Example NDI section • Section 5 - Headaches I have no headaches at all. I have slight headaches which come infrequently. I have moderate headaches which come frequently. I have severe headaches which come frequently. I have headaches almost all the time. Evidence-based Chiropractic 74 © 2006

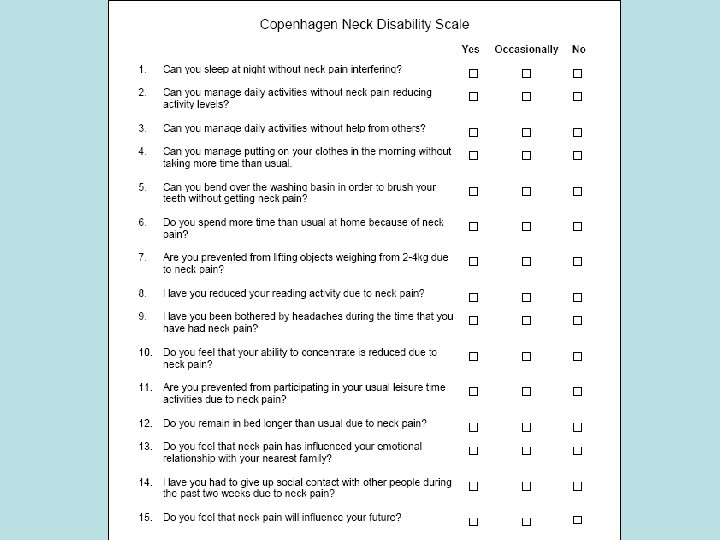
Other neck specific questionnaires • Copenhagen Neck Functional Disability Scale • Northwick Park Neck Pain Questionnaire • Neck Pain and Disability Scale • Patient-Specific Functional Scale • However, the NDI is encountered much more frequently and has been revalidated in diverse study populations Evidence-based Chiropractic 75 © 2006
Evidence-based Chiropractic 76 © 2006

Whiplash Disability Questionnaire (WDQ) • Uses the basic components of the NDI, plus questions on emotional health, social activity, and fatigue • Uses an 11 -point (0– 10) numerical scale for the patients’ responses – The minimum clinically important difference is 15 points • Has excellent internal consistency and test-retest reliability Evidence-based Chiropractic 77 © 2006

WDQ Evidence-based Chiropractic 78 © 2006

Headache Disability Inventory (HDI) • A 25 question survey designed for patients with cervicogenic headaches – 12 emotional questions – 13 functional questions • Useful in assessing the impact of headache on daily living • Construct validity, internal reliability, and test-retest reliability is good Evidence-based Chiropractic 79 © 2006

HDI (cont. ) • The maximum HDI score is 100 points • HDI scores ranging from 2 to 32 are considered mild, from 33 to 59 are moderate, and 60 or greater are severe • At least a 29 -point change must occur from test to retest before the changes can be attributed to a patient’s treatment Evidence-based Chiropractic 80 © 2006
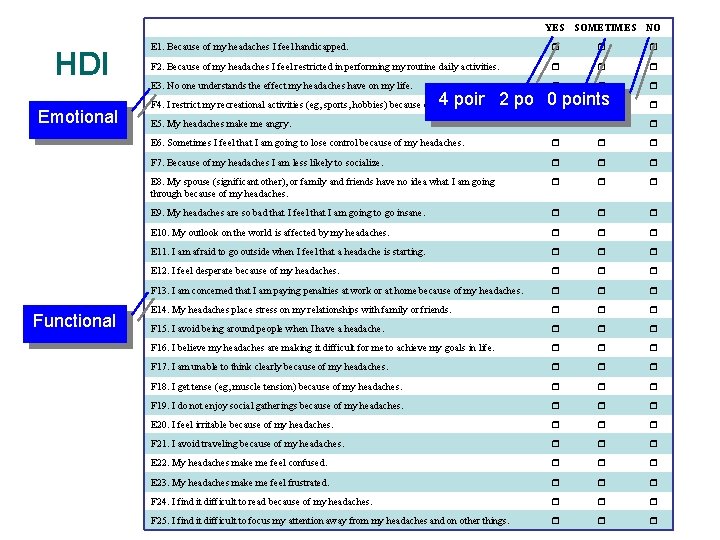
YES HDI Emotional Functional SOMETIMES NO E 1. Because of my headaches I feel handicapped. F 2. Because of my headaches I feel restricted in performing my routine daily activities. E 3. No one understands the effect my headaches have on my life. 4 points 2 points 0 points F 4. I restrict my recreational activities (eg, sports, hobbies) because of my headaches. E 5. My headaches make me angry. E 6. Sometimes I feel that I am going to lose control because of my headaches. F 7. Because of my headaches I am less likely to socialize. E 8. My spouse (significant other), or family and friends have no idea what I am going through because of my headaches. E 9. My headaches are so bad that I feel that I am going to go insane. E 10. My outlook on the world is affected by my headaches. E 11. I am afraid to go outside when I feel that a headache is starting. E 12. I feel desperate because of my headaches. F 13. I am concerned that I am paying penalties at work or at home because of my headaches. E 14. My headaches place stress on my relationships with family or friends. F 15. I avoid being around people when I have a headache. F 16. I believe my headaches are making it difficult for me to achieve my goals in life. F 17. I am unable to think clearly because of my headaches. F 18. I get tense (eg, muscle tension) because of my headaches. F 19. I do not enjoy social gatherings because of my headaches. E 20. I feel irritable because of my headaches. F 21. I avoid traveling because of my headaches. E 22. My headaches make me feel confused. E 23. My headaches make me feel frustrated. © 2006 F 24. I find it difficult to read because of my headaches. Evidence-based Chiropractic 81 my headaches and on other things. F 25. I find it difficult to focus my attention away from

Migraine Disability Assessment (MIDAS) questionnaire • Consists of only 7 items – 5 items contribute to the overall score • MIDAS is based on the Headache Impact Questionnaire (HIQ) – MIDAS scoring is easier and scores are more intuitively meaningful than HIQ scores • Test-retest reliability and internal consistency are good Evidence-based Chiropractic 82 © 2006

MIDAS questionnaire (cont. ) • Scores are derived from 3 domains of activity 1. Lost time from work for pay 2. Housework or chores 3. Leisure activities • The final MIDAS score is total number of headache-related missed days from these domains Evidence-based Chiropractic 83 © 2006

A and B do not contribute to the overall MIDAS score Evidence-based Chiropractic 84 © 2006

MIDAS questionnaire (cont. ) Grading system for the MIDAS questionnaire Score 0 - 5 6 – 10 11 - 20 > 20 Evidence-based Chiropractic Definition Minimal or infrequent disability Mild or infrequent disability Moderate disability Severe disability 85 Grade I III IV © 2006

36 -item short-form questionnaire (SF-36) • a. k. a. , RAND 36 -item health survey • A general health questionnaire that consists of 36 items • Assesses patients’ health status from their point of view • Used extensively in research and clinical practice – Has good internal consistency and reliability Evidence-based Chiropractic 86 © 2006

SF-36 (cont. ) • Self administered – Takes about 5 -10 minutes for patients to complete – Patients must be at least 14 years of age – Can also be administered via face-to-face interview or by telephone • Scoring reports on 8 health scales, 2 summary measures, and self-perceived changes in health status Evidence-based Chiropractic 87 © 2006

SF-36 assesses 8 health concepts related to physical, emotional, or psychological distress 1. Limitations in physical activities because of health problems 2. Limitations in usual role activities because of physical health problems 3. Bodily pain 4. General health perceptions 5. Vitality 6. Limitations in social activities because of physical or emotional problems 7. Limitations in usual role activities because of emotional problems 8. Mental health Evidence-based Chiropractic 88 © 2006

SF-36 vs. RAND 36 • Both were developed as part of the Medical Outcomes Study (MOS) • They contain the same questions, but the scoring procedures are different • RAND 36 is free at: – http: //www. rand. org/health/surveys_tools/mos_core_36 item. html • SF-36 is available for a fee at – http: //www. sf-36. org Evidence-based Chiropractic 89 © 2006

SF-36 sample questions 1. In general, would you say your health is: (Circle One Number) Excellent 1 Very good 2 Good 3 Fair 4 Poor 5 2. Compared to one year ago, how would your rate your health in general now? (Circle One Number) Much better now than one year ago Somewhat better now than one year ago About the same Somewhat worse now than one year ago Much worse now than one year ago Evidence-based Chiropractic 90 1 2 3 4 5 © 2006
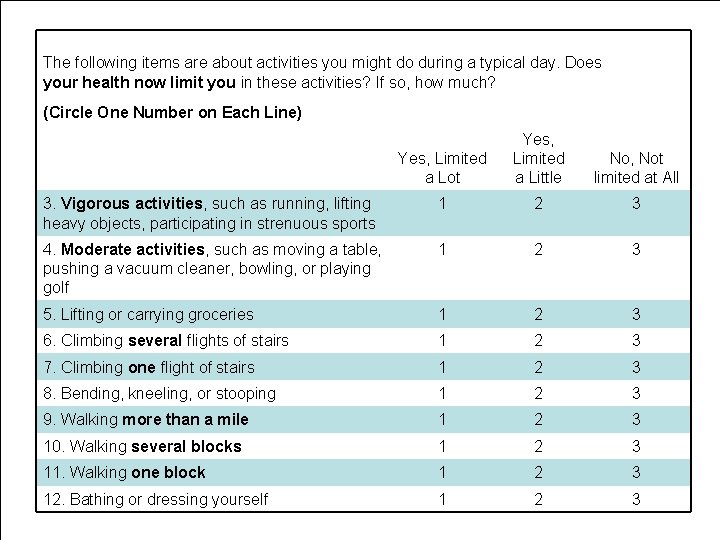
The following items are about activities you might do during a typical day. Does your health now limit you in these activities? If so, how much? (Circle One Number on Each Line) Yes, Limited a Lot Yes, Limited a Little No, Not limited at All 3. Vigorous activities, such as running, lifting heavy objects, participating in strenuous sports 1 2 3 4. Moderate activities, such as moving a table, pushing a vacuum cleaner, bowling, or playing golf 1 2 3 5. Lifting or carrying groceries 1 2 3 6. Climbing several flights of stairs 1 2 3 7. Climbing one flight of stairs 1 2 3 8. Bending, kneeling, or stooping 1 2 3 9. Walking more than a mile 1 2 3 10. Walking several blocks 1 2 3 11. Walking one block 1 2 3 12. Bathing or dressing yourself Evidence-based Chiropractic 91 © 2006

20. During the past 4 weeks, to what extent has your physical health or emotional problems interfered with your normal social activities with family, friends, neighbors, or groups? (Circle One Number) Not at all 1 Slightly 2 Moderately 3 Quite a bit 4 Extremely 5 21. How much bodily pain have you had during the past 4 weeks? (Circle One Number) None 1 Very mild 2 Mild 3 Moderate 4 Severe 5 Very severe 6 Evidence-based Chiropractic 92 © 2006

SF-12 • Even shorter than the SF-36, yet it is still valid • Includes only 12 of the SF-36 items – 1 or 2 items from each of the 8 health concepts are included • Available from – http: //www. sf-36. org Evidence-based Chiropractic 93 © 2006

Dartmouth COOP chart system • Dartmouth Primary Care Cooperative Information Project chart system • A patient friendly measure of functional health status that is simple to administer and score • Designed for use with adults and adolescents Evidence-based Chiropractic 94 © 2006

Dartmouth COOP (cont. ) • Queries the patient about their function in the preceding 2 weeks • Measures 9 dimensions of health – Physical, Emotional, Daily Activities, Social Support, Pain, and Overall Health • Consists of a series of 9 charts – Each has a title, a functional status question, and 5 responses to choose from Evidence-based Chiropractic 95 © 2006

Dartmouth COOP (cont. ) • Can be self-administered by the patient or administered by the clinician or staff member. • Scoring is reported to be easy – A high score (4 or 5) on any of the charts is considered abnormal • Available from Debbie Johnson at the Dartmouth COOP Project, – Deborah. Johnson@Dartmouth. edu Evidence-based Chiropractic 96 © 2006
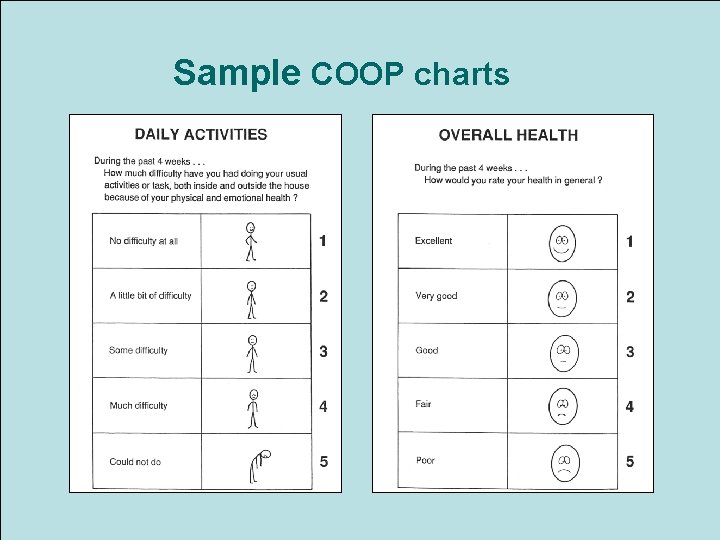
Sample COOP charts Evidence-based Chiropractic 97 © 2006

Sickness Impact Profile (SIP) • A general health questionnaire that is commonly used in research – Rarely used in clinical practice because of its lengthiness (It consists of 136 items) • Consists of 14 subscales that deal with illness and the related activity levels of ill patients • Is valid and reliable as an OM for use with low back pain patients Evidence-based Chiropractic 98 © 2006

SIP (cont. ) • Statements only apply to patients on the day of the evaluation • Incorporates physical and psychosocial domains of health • Considered a “gold standard” as an OM of self-reported pain – Because of its widespread use in research and its well-established reliability and validity Evidence-based Chiropractic 99 © 2006

Physiologic OMs • Assessments that are performed by the examiner • Includes the evaluation of range of motion, muscle strength, postural analysis, x-ray analysis, etc. • Often considered to be more reliable than qualitative measures, but the opposite is often true Evidence-based Chiropractic 100 © 2006

Range of motion (ROM) • Commonly used in clinical practice – Its validity and reliability is variable – Depends on the region being examined and the evaluation method used • Lumbar ROM assessment by dual inclinometry has shown to be valid and reliable – Especially pertaining to forward flexion Evidence-based Chiropractic 101 © 2006

ROM (cont. ) • Other studies have concurred, but measurements were always performed apart from other exam procedures • In a study where ROM was measured during usual clinical practice, most scores were not reliable • Lumbar ROM reliability also depends on the extent of examiner training Evidence-based Chiropractic 102 © 2006

ROM (cont. ) • The time of day measurements are taken also influences results • Thus, lumbar ROM evaluated in a clinical environment may not be reliable, even if experimental evidence suggests otherwise • Measurement of cervical spine ROM is reliable using dual inclinometry – However, visual observation is not Evidence-based Chiropractic 103 © 2006

Algometry • The use of an algometer (a. k. a. , pain threshold meter) – A hand-held rubber-tipped force gauge that registers kilograms per square cm or pounds per square inch when pressure is applied – Used to quantify the amount of surface pressure that is associated with subjective pain tolerance or tenderness Evidence-based Chiropractic 104 © 2006

Algometry (cont. ) • The rubber tip is placed over an area to be examined and increasing pressure is applied • Patients are asked to report pain or tenderness levels – Pressure threshold is the minimum amount of pressure needed to cause pain – Pressure tolerance is the maximum amount of pressure the patient can tolerate Evidence-based Chiropractic 105 © 2006

Algometry (cont. ) • Pain associated with algometry testing can be used in conjunction with a tenderness rating scale • Algometry has been tested in a variety of settings and on different types of tissues – Its reliability and validity has generally been good Evidence-based Chiropractic 106 © 2006

Recommended OMs to assess patients with back pain 1. VAS 2. Roland-Morris or Oswestry questionnaire 3. SF-12 or SF-36 4. Days off work or activity intolerances to reflect disability 5. Overall satisfaction with care Evidence-based Chiropractic 107 © 2006

Use the validated form a test in clinical practice • Do not modify anything • Use the version that was presented in the original research • OMs that have been altered can not be considered valid – Even something as minor as changing the order of questions Evidence-based Chiropractic 108 © 2006
- Slides: 108