Evidence Based Medicine and Clinical Practice Guidelines Chapter

Evidence Based Medicine and Clinical Practice Guidelines 實證醫學、臨床診療指引 Chapter 14 Robert Hoyt MD William Hersh MD


One thing that is constant in life is change no one has entire knowledge


共同創立 Monitor Group, 2013年破產

Learning Objectives ∗ How health informatics help us make better clinical decisions


Learning Objectives After reviewing the presentation, viewers should be able to: ∗ State the definition and origin of evidence based medicine ∗ Define the benefits and limitations of evidence based medicine ∗ Describe the evidence pyramid and levels of evidence ∗ State the process of using evidence based medicine to answer a medical question ∗ Recall important online and smartphone evidence based medicine resources ∗ Describe the interrelationship between clinical practice guidelines, evidence based medicine, and electronic health records ∗ Define the processes required to create and implement a clinical practice guideline

Introduction ∗ Information technology has the potential to improve decision making through ∗ online medical resources, ∗ electronic clinical practice guidelines, ∗ electronic health records (EHRs) with ∗ decision support, ∗ online literature searches, ∗ digital statistical analysis and ∗ online continuing medical education

EBM Definition ∗ systematic approach to ∗ clinical problem solving ∗ integration of the ∗ best available research evidence with ∗ clinical expertise and ∗ patient values

Importance of EBM ∗ “Patients should receive care based on ∗ the best available scientific knowledge. ∗ Care should not vary illogically ∗ from clinician to clinician or ∗ from place to place” ∗ We are moving slowly ∗ from anecdotal evidence ∗ to randomized controlled trials (the National Academy of Medicine) 消化庫存及調節�量

Traditional Methods for Gaining Medical Knowledge ∗ Continuing Medical Education (CME): ∗ keeping medically or educationally up-to-date ∗ current methods do not work ∗ the pharmaceutical industry bombards ∗ clinicians and patients every day; ∗ often with misleading or biased information ∗ lack of time and ∗ “information overload” ∗ the volume of published material ∗ 1, 800 citations added daily to MEDLINE 共 32頁

The EBM Process to Answering a Clinical Question 1. 2. 3. 4. A clinical question is generated. Seek the best evidence using an EBM resource Critically appraise the evidence using tools Apply the evidence to the patient, l taking into account their values, l preferences and l circumstances

Example: For patients ∗ over age 65 ∗ with a suspected stroke or TIA, (暫時性腦缺血) ∗ which is the preferred initial imaging technique ∗ (MRI or CT or both)?

Terminology Used in Answering Clinical Questions ∗ Validity: ∗ Internal: ∗ Is the study believable? ∗ look for apparent biases or errors in ∗ selecting patients, ∗ measuring outcomes, ∗ conducting the study, or ∗ analyzing the results ∗ External: ∗ are the results generalizable to your population of interest? If you have a geriatric population results on teenagers might be irrelevant

Most Common Types of Clinical Questions ∗ Therapy Question: ∗ does the addition of Plavix to aspirin ∗ reduce the incidence of future strokes? ∗ Prognosis Question : ∗ will lowering the average blood pressure to less than 120/80 ∗ reduce the likelihood of a stroke?

Most Common Types of Clinical Questions ∗ Diagnosis Question : ∗ detecting a heart attack, ∗ which is more sensitive and specific ∗ ∗ CPK (細胞酵素) or troponin (心肌旋轉蛋 白)?

Most Common Types of Clinical Questions ∗ Harm Question : ∗ how many patients will have renal insufficiency (腎功能衰竭) ∗ due to an ∗ ace inhibitor (抗高血� � ) compared to a ∗ beta blocker? ∗ ∗ β阻斷藥 治療心律不齊

Most Common Types of Clinical Questions ∗ Cost question : ∗ which is more cost effective to reduce hospital readmissions for heart failure, ∗ inpatient case management or ∗ home health nursing care?
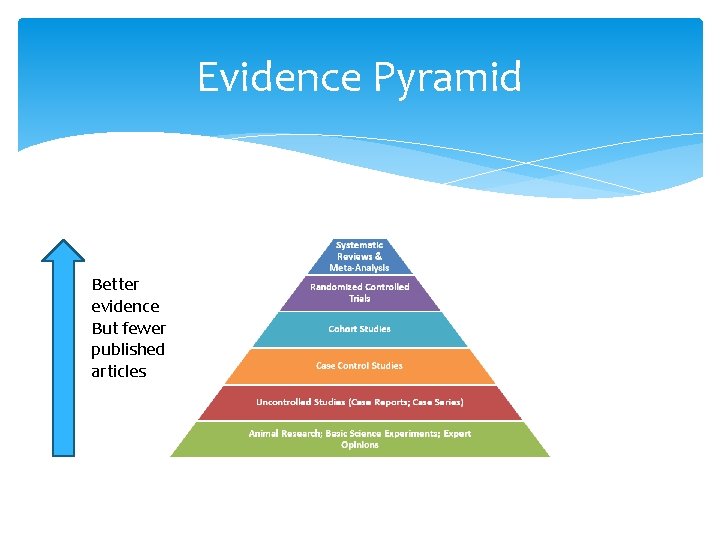
Evidence Pyramid Better evidence But fewer published articles

Evidence Pyramid Studies ∗ Case reports/case series : ∗ ∗ collections of reports on treatment of patients without control groups; much less scientific significance 大麻二酚

Evidence Pyramid Studies ∗ Case control studies : ∗ study patients ∗ with a specific condition ∗ compared with people who do not the condition; ∗ less reliable than randomized controlled trials ∗ 二手煙 ~~ 癌症 ∗ 回溯性研究 (retrospective study) ∗ 一組「罹癌」 ∗ 一組「未罹癌」 ∗ asked about their exposure to risk factors ∗ an odds ratio is calculated
∗ Quickly establishes associations (相關性) ∗ weaker in establishing causation (因果) ∗ best choice for rare conditions or diseases

Evidence Pyramid Studies ∗ Cohort (群體) studies : ∗ 有特定生活經歷的人群 ∗ Children who grew up in New Orleans during Hurricane Katrina ∗ evaluate and follow patients ∗ who have a specific exposure ∗ or receive a particular treatment over time and ∗ compare them with another group that is similar but has not been affected by the exposure being studied;
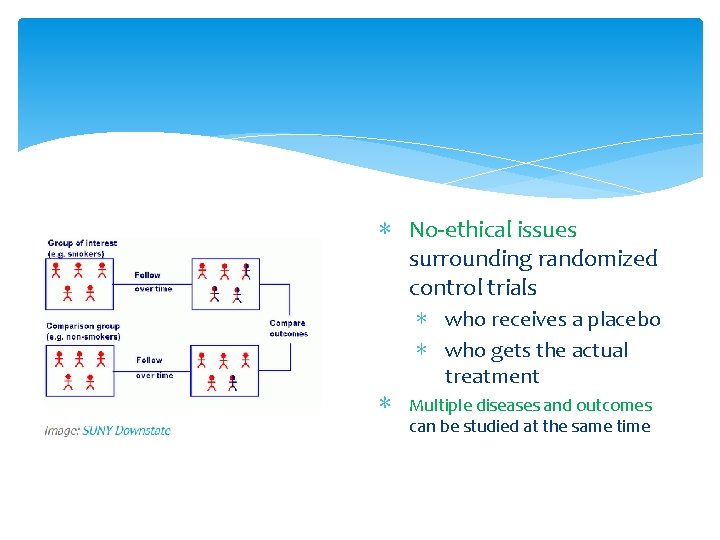
∗ No-ethical issues surrounding randomized control trials ∗ who receives a placebo ∗ who gets the actual treatment ∗ Multiple diseases and outcomes can be studied at the same time


∗ Randomized controlled trials (RCTs): ∗ subjects are randomly assigned to a treatment or ∗ a control group that received placebo or no treatment; ∗ only difference between the two groups is the intervention being studied. ∗ an active medication or a placebo ∗ “Double blinded” – ∗ both the investigators and ∗ the subjects ∗ do not know whether they received an active medication or a placebo ∗ RCTs are the gold standard design to test therapeutic interventions

Evidence Pyramid Studies ∗ Systematic reviews : ∗ protocol-driven comprehensive reproducible searches ∗ multiple RCTs ∗ the quality of individual RCTs is evaluated ∗ to answer a focused question ∗ several reviewers scan the medical literature with specific criteria

Evidence Pyramid Studies ∗ Meta-analyses : ∗ quantitative summary of systematic reviews using ∗ statistical techniques to combine the results of several studies, thereby leading to ∗ larger numbers (more statistical significance) and ∗ a wider range of patients

Levels of Evidence ∗ GRADE: ∗ Grading of Recommendations, Assessment, Development and Evaluation ∗ 證據評比系統 ∗ is a common framework to grade the quality of evidence, ∗ but many others exist

Levels of Evidence ∗ Level 1: High quality evidence derived from consistent RCTs ∗ Level 2: Moderate quality evidence inconsistent or less methodologically strong RCTs; or exceptionally strong observational evidence ∗ Level 3 : Low quality evidence, usually from observational studies ∗ Level 4: Very low quality evidence from flawed observational studies, indirect evidence or expert opinion

Chocolate consumption and the risk of cardiometabolic disorders 心血管代謝疾病 ∗ Highest level of chocolate consumption ∗ 37% ∗ Reduction in the risk of cardiovascular disease and stroke ∗ lowest level of chocolate consumption ∗ 29% ∗ Reduction in the risk of cardiovascular disease and stroke This magnitude of effect rivals the best available drugs and interventions used to prevent these diseases

Chocolate consumption and the risk of cardiometabolic disorders ∗ Observational studies ∗ likely exaggerated the magnitude of benefit ∗ Bias and confounding ∗ Chocolate users ∗ Healthier ? ∗ Wealthier ? ∗ More educated ?

Therapy trials Risk measurement Terminology ∗ Treated group ∗ 100 patients ∗ Received drug ∗ 5 suffer a heart attack over a period of 12 months ∗ Risk = 5/100 = 5% ∗ Experimental event rate ∗ (EER) ∗ Odds = (event occured) / (event will not occur) ∗ Odds = 5 / 95 = 0. 052

Therapy trials Risk measurement Terminology ∗ Control group (對照組) ∗ 100 patients ∗ Received placebo ∗ 7 suffer a heart attack over a period of 12 months ∗ Risk = 7/100 = 7% ∗ Control event Rate ∗ CER ∗ Odds = (event occured) / (event will not occur) ∗ Odds = 7 / 93 = 0. 075

Therapy trials Risk measurement Terminology ∗ Relative Risk Reduction ∗ RR ∗ = EER / CER ∗ RRR ∗ = (EER – CER) / CER ∗ = 5% / 7% =0. 71 ∗ = (7% - 5%) / 7% ∗ = 29%

Therapy trials Risk measurement Terminology ∗ Absolute Risk Reduction ∗ ARR ∗ = EER – CER ∗ = 7% - 5% = 2% ∗ (取�對� ) ∗ Number Needed to Treat ∗ NNT ∗ = 1 / ARR ∗ = 1 / 2% = 100 / 2 = 50

Limitations of the Medical Literature Low yield of excellent quality articles in general Many repeated studies show different results Results are very frequently inconclusive Many studies are poorly designed, have inadequate number of patients, and have some bias ∗ Many medical journals are now requiring registration of all clinical trials in public registries ∗ ∗

Limitations of EBM ∗ Different rating systems for evidence ∗ Different conclusions drawn by different people ∗ Reviews are very time intensive so ∗ reviews don’t exist for every medical condition ∗ RCTs are expensive, so ∗ often sponsored by drug companies, ∗ introducing bias

Limitations of EBM ∗ Some view EBM as “cook book medicine”

WHY NOT Evidence Based Health Informatics ∗ Early Hype ∗ Overly optimistic predictions of HIT on healthcare quality, safety, proficiency and cost reduction ∗ Based on expert opinions ∗ Government ∗ Early success stories came from organization with track record of home grown successful technology ∗ Technology pressure

WHY NOT Evidence Based Health Informatics ∗ Methodological challenges ∗ Most HIT studies ∗ Observational and retrospective ∗ Cause and effect are difficult to prove ∗ Randomized controlled trial is impossible ∗ e-prescribe vs. paper prescribe ∗ Lack of good qualitative and quantitative data

WHY NOT Evidence Based Health Informatics ∗ Failure to anticipate unintended consequences related to HIT adoption ∗ Technology unavailable ∗ Technology malfunctions ∗ Technology function but human error ∗ e-prescribe works but enter wrong dose ∗ Alert fatigue ∗ Alarm fatigue ∗ Upcoding with HER coding (lower coding)

EBM Resources JAMA Evidence Clinical Evidence Cochrane Library Cochrane Summaries Evidence Updates ACP Journal Club Practical Pointers for Primary Care ∗ Essential Evidence Plus ∗ ∗ ∗ ∗ Trip. Database OVID SUMSearch Bandolier Centre for EBM Best Bets Evidence Based Health Care

More EBM Resources ∗ ∗ Google (insert “evidence based”) NNT web site MDCalc has EBM calculator tools EBM for mobile technology: Med. Calc 3000 calculators are web based and exist for mobile platforms

Clinical Practice Guidelines

Clinical Practice Guidelines ∗ “systematically developed statements to assist practitioner and patient decisions about health care for specific clinical circumstances” ∗ Institute of Medicine 1990 ∗ CPGs are based on ∗ EBM and ∗ are generally embraced by most specialties around the world ∗ While they are embraced they are not always utilized by physicians for a variety of reasons

Clinical Practice Guidelines Steps 1. 2. 3. 4. 5. Panel of subject matter experts convene to evaluate an important medical problem (high cost, high risk, etc. ), usually with a disease management team, possibly IT, epidemiology, etc. Team reviews local issue and evidence and examines national evidence; balancing costs, benefits and risks Team evaluates the applicability of the guideline to the local scenario Leadership at the top and the medical and nursing staff are critical for acceptance in a healthcare system Implementation details are important as well; will it be paper or electronic based? Part of EHR?

IT assisted CPG potentially most beneficial ∗ Disease management ∗ 68% medicare budget ∗ 23% patient ∗ Five or more chronic conditions ∗ Quality management strategies ∗ Improve care ∗ Lower cost
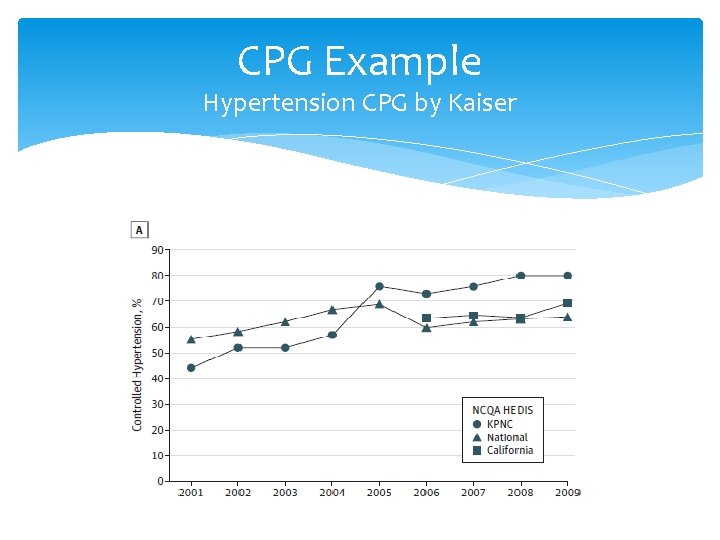
CPG Example Hypertension CPG by Kaiser

Electronic CPGs ∗ CPGs available for mobile technology ∗ Web based CPGs (risk calculators) ∗ ∗ ATP III FRAX Gail breast cancer risk assessment Stroke risk calculator ∗ EHR-based CPGs: ∗ Library of CPGs embedded in the EHR ∗ Order sets for new admissions

CPGs reality check ∗ Overall, patients received 54% of recommended care ∗ RAND study 2003 ∗ Major teaching hospital overuse statin therapy ∗ 69% overuse for primary prevention ∗ To prevent a disease ∗ 47% overuse for secondary prevention ∗ To prevent recurrence or progression 降膽固醇藥 他汀類藥物

Barriers to CPGs ∗ Practice setting: are the clinicians too busy or indifferent to new evidence? ∗ Contrary opinion: do the experts agree? ∗ Sparse data: is the evidence conclusive? ∗ Expect low initial acceptance ∗ CPGs can be too long, without a summary ∗ Lack of local champions ∗ CPGs may lack patient input with both the writing of the CPGs and the implementation ∗ Incentives to adopt may be missing for clinicians

CPG Resources ∗ ∗ ∗ National Guideline Clearinghouse National Institute for Health and Clinical Excellence Agency for Health Care Research and Quality Health Team Works Institute of Clinical Systems Improvement

Conclusions ∗ EBM is the pursuit of the best available evidence ∗ EBM is based on a hierarchy or pyramid of evidence ∗ There are multiple limitations of the medical literature and EBM ∗ The average clinician would benefit from understanding EBM and having tools available ∗ CPGs help standardize care based on EBM ∗ CPGs are becoming a routine part of EHRs
- Slides: 55