Evaluation of the urologic patient Urinary tract is
























- Slides: 26

Evaluation of the urologic patient

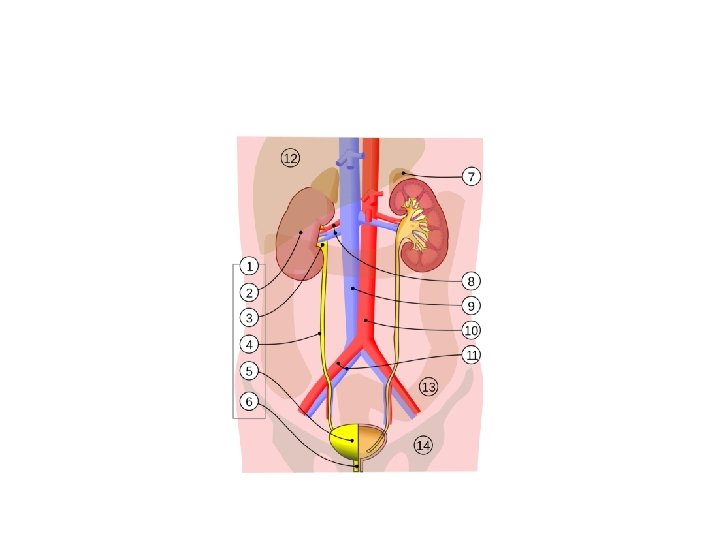
• Urinary tract is divided into upper and lower urinary tract • Upper urinary tract involve kidneys and ureters while lower urinary tract involve bladder and urethra and prostate in male • Kineys are paired, ovoid retroperitoneal structures , locate in posterior abdomen on each side of vertebral column

• The rt kidney is 1 -2 cm below the lt one and extend from 1 st to 3 rd lumbar vertebrae, the lt kidney from 12 th thoracic to 3 rd lumbar vertebrae • Each kidney is about 12 cm in length 6 cm in width and 3 cm in thickness, and weight 150 gm • Each kidney contain one million nephron


• Ureter : is bilateral muscular duct that carry urine from kidney to bladder • In adult it is about 30 cm in length • There is 3 narrowing in ureter PUJ, VUJ, when crossing iliac bifurcation • The ureter is divided into upper and middle and lower segment • Also divided into abdominal and pelvic ureter

• • • The basic approach of urologic patient include: History Physical examination Lab investigation Radiological assesment

history • Chief complaint and present illness • Pain: pain from GU tract is usually caused by inflammation or obstruction • Inflammation is sever when involve the parenchyma of the organ(pyelonephritis , prostatitis, epididymitis. • Inflammation of hollow viscus produce less sever pain (discomfort) such as cystitis or urethritis

• Tumor is painless unless cause obstruction or invasion of nerve • Renal pain: distension of capsule by obstruction or inflammation • Pain due to infection is steady while due to obstruction fluctuates in intensity • Pain involve the loin area and radiate to umbilicus or upper abdomen

• Also may associate with nausea and vomiting , because reflex stimulation of celiac ganglia or proximity of GI organ • Renal pain could be differentiated from intraperitoneal pathology: ptn with renal pain prefer to move around holding the loin area (rolling sign), and usually colicky in nature • Intraperitoneal pain radiate to shoulder and steady, ptn prefer to lie motionless

• Renal pain could be confused with radicular pain which is not colicky and altered by changing position • Shingle which caused by varicella zoster virus that cause chickenbox • Firstly it cause burning pain which followed by skin rash involve flank area • Usually unilateral

• Ureteral pain: usually secondary to obstruction, the pain caused by distension and peristalsis of smooth muscle to releive obstruction • The pain could radiate to inguinal or external genetalia • Stone at VUJ result in irritative voiding symptom

• Vesical pain: overdistension(AUR), inflammation, • Inflammatory condition of bladder usually cause intermittent suprapubic discomfort • Strangury: sharp stabbing suprapubic painat the end of voiding in ptn with cystitis • Constant suprapubic pain that not associated with lower abdominal swelling is rarely of urological origin • Slowly progressive bladder distention frequently cause no pain

• Prostatic pain • Poorly localized pain usually secondary to inflammation • Associate with irritative voiding symptom • Penile pain: in flaccid penis could be due to bladder or urethral inflammation, or paraphimosis • In erect penis : peyronie disease or priapism

• Scrotal pain: could be acute or chronic • Acute testicular pain usually secondary to torsion ot testicle or testicular appendex, epididymoorchitis • Chronic testicular pain usually result from non inflammatory condition such as hydrocele or varicocele • Because testicle arise in close proximity to the kidney, pain from the kidney may be referred to testicle

Hematurea Gross vs microscopic Timing of hematurea Association with pain Presence of clot Hematurea in adult is symptom of malignancy until proven otherwise • The mcc of GH over age of 50 is bladder cancer • Painful hematurea is the one that associate with loin pain , lower abdominal pain or dysurea • • •

Lower urinary tract symptom • Irritative symptom • Frequency: the most common urological symptom • Polyuric(DM, DI, excessive fluid intake) vs non polyuric frequency (decrease bladder capacity) • Normal adult voids 5 -6 times per day

• Nocturia: is one or more rise from sleep , and clinically significant if 2 or more • As with frequency it could be caused by increase urine output or decrease bladder capacity • Nocturnal polyuria is more than one third of urine output • Nocturea without frequency may occur in ptn with CHF and peripheral edema in whom urin output increase in night when they are supine • This aggravated by decreasing concentrating ability at night in geriatric ptn

• Dysuria: painful urination usually felt over urethral meatus and caused by inflammation • Urgency: strong desire to voide • Obstructive symptom • Poor stream , hesitancy, intermittency, post void drippling, straining, incomplete voiding • Straining: use of abdominal muscle to urinate which are used only at the end of voiding

• Intermittency: involuntary start stop of urinary stream • Postvoid dribbling: terminal release of drops of urine at the ending of voiding • Poor stream: decrease the force of urination • Hesitancy: delay in the initiation of urination • Obstructive and irritative symptom(LUTS): are not specific for prostate problem as could be result from another cause of BOO, or neurological disease or even bladder tumor

• Incontinence : involuntary loss of urine • Continuous incontinence: due to fistula that bypass the urethral sphincter most commonly vesicovaginal fistula, or ectopic ureter in female • Stress incontinence: leakage of urine with increase abdominal pressure • Urge incontinence: urine leak preceded by strong desire to void • Overflow incontinence: in ptn with chronic retention • Enuresis: incontinence that occur during sleep

• Hematospermia: is the presence of blood in semen, mostly result from non specific inflammation of prostate and seminal vesicle frequently after period of sexual abstinence • If persist for more than several weeks it should be investigated • Pneumaturia: presence of gas in urine, cause by recent catheterization, fistula with intestine, infection with gas forming organism

Urine analysis • Important test that should be done in all urologic patient • Complete urine test include chemical and microscopic analysis • Collection of urine sample • Male vs female vs infant • Sterile bag with adhesive collar good if negative

• Physical examination of urine • Colour: yellow in color due to urin chrome • Urine color change because of concentration , food, drugs, or pathology • Turbidity: urine is clear • Cloudy urine mostly phsphaturia example after milk ingestion or pyuria due to infection

Urine dipstick • PH the average ph is 6 -7. 5 • RTA acidic serum with alkaline urine • Uti alkaline urine indicate infection with urea splitting microorganism mostly proteus • USM secrete urease that convert ammonia to ammonium ion which cause alkaline urin and so promote formation of infection stone

• Hematurea • The chemical dtection of hematurea is based on peroxidase like activity of hb • Leukocyte esterase and nitrite test for bacteria and wbc • Gram negative bacteria convert nitrate to nitrite

• • Urin microscopy Low power magnification(100) High power magnification(400) Cells, cast, crystal, bacteria, parasite