Evaluating the Utility of the Ventriculogallbladder Shunt in

Evaluating the Utility of the Ventriculogallbladder Shunt in Pediatric Hydrocephalus: Long Term Outcomes and Complications Presented by Tristan Mackey 1 Co-authors: Kayla Schilling 1, Daniel Lee 1, Chris Troup 2, MD, Kristie Griffin 3, MD 1 University of South Carolina School of Medicine Greenville Health Children’s Hospital-Department of Pediatric Neurosurgery 3 Prisma Health Upstate-Department of General Surgery 2 Prisma

Introduction Hydrocephalus is a condition in which cerebrospinal fluid accumulates within the ventricular system of the brain in a manner that overwhelms its ability to handle the extra fluid 1, 2 This increase in CSF leads to pathological dilation of the ventricles which manifests itself in ways such as nausea, vomiting, headache, irritability, lethargy, bulging fontanelles, and decreased levels of consciousness 1, 2 It is estimated that approximately 6 in 10, 000 live births are complicated by hydrocephalus and if a neonate is diagnosed with hydrocephalus, there is a neonatal mortality rate before initial hospital discharge of 13%1, 3 This condition poses a significant financial and societal burden considering that every year pediatric hydrocephalus accounts for 38, 200 to 39, 900 hospital admissions, 391, 000 to 433, 000 hospital days, and $1. 4 to $2. 0 billion in total hospital charges in the United States 1, 4

Introduction We often think of hydrocephalus as being either communicating or noncommunicating, which is based on the etiology of the fluid accumulation Communicating hydrocephalus involves the production of too much CSF or a failure of the arachnoid granulations to successfully resorb CSF. This can be due to arachnoid calcifications, a choroid plexus papilloma, or various genetic/congenital causes 1, 2 Non-communicating hydrocephalus involves an obstruction within the brain’s ventricular system that impedes flow from one portion to the next. This can be due to an obstructive mass or tumor, fibrosis of blood products, congenital stenosis, or infection 1, 2 Depending upon the mechanism of hydrocephalus, various utilities can be utilized in the treatment of this condition. Different surgical interventions include an endoscopic third ventriculostomy, tumor excision, or placement of a shunt 1, 2

Introduction Shunt failure, which can occur through various mechanisms such as infection, hardware failure, or over-drainage of CSF, is common and often requires revision or complete replacement of a shunt 1 Studies have demonstrated that overall failure rates for new shunts is around 13% at 30 days and 29% at 1 year 1, 5, 6 A study of more than 40 children’s hospitals revealed the infection rate among uncomplicated initial CSF shunt placements to be approximately 11% within 24 months 1, 7 Most shunts are initially ventriculoperitoneal, meaning that the extra CSF drains into the peritoneal space If multiple shunt failures occur due to infection, abdominal adhesion formation, scar tissue, or various other reasons, then other options for shunt placement include the atria, pleura, or the gallbladder

Introduction Ventriculogallbladder shunts were first described by Smith et al. in a small case series in 19588 Since this time, their utility within pediatric hydrocephalus has been mostly for cases in which multiple shunt failures have occurred or when the peritoneum is not a viable option for placement Data and long-term outcomes for patients receiving a VGB shunt has been limited since their introduction with only 9 studies reporting outcomes and follow-up data in the literature The purpose of our study was to utilize data from our own institution and analyze that alongside data from all other studies that met our inclusion criteria in order to further the understanding of how effective VGB shunts are when treating pediatric hydrocephalus

Methods We completed a retrospective review using Epic of all patients who had received a shunt revision, for any reason, at our institution (Prisma Health-Upstate) from 2005 -2019 We identified 301 patients who received a shunt revision, with 9 of these being revised to a VGB shunt We then used their charts to identify why a VGB shunt was placed, shunt longevity, length of follow up, and any complications that occurred We then performed a literature review for all other studies that reported similar outcome measures and found 6 previous studies that met these criteria with a total of 67 patients who also had VGB shunts placed 9 -15 Our data were then analyzed in conjunction with these data in order to understand the effectiveness of VGB shunts across the time they have been utilized
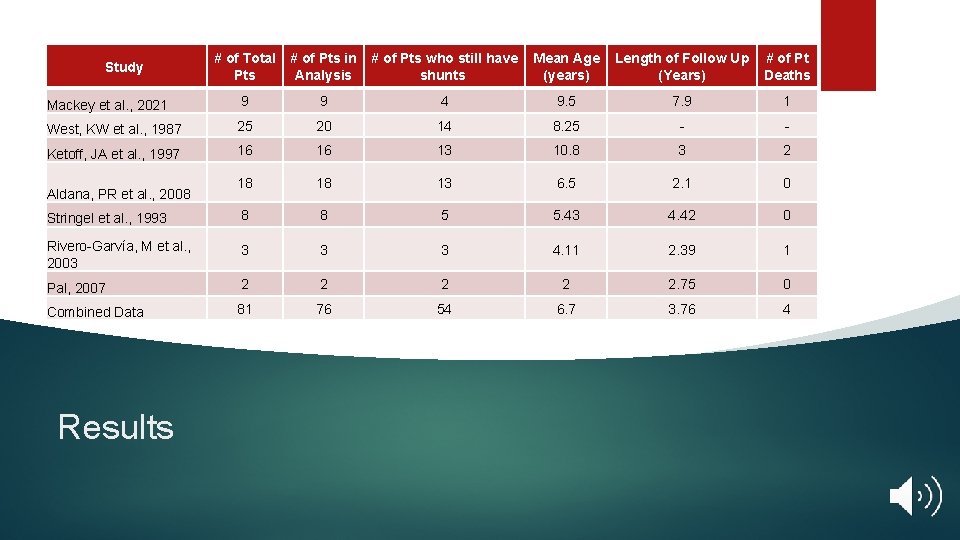
Study # of Total # of Pts in Pts Analysis # of Pts who still have shunts Mean Age (years) Length of Follow Up (Years) # of Pt Deaths Mackey et al. , 2021 9 9 4 9. 5 7. 9 1 West, KW et al. , 1987 25 20 14 8. 25 - - Ketoff, JA et al. , 1997 16 16 13 10. 8 3 2 18 18 13 6. 5 2. 1 0 Stringel et al. , 1993 8 8 5 5. 43 4. 42 0 Rivero-Garvía, M et al. , 2003 3 4. 11 2. 39 1 Pal, 2007 2 2 2. 75 0 Combined Data 81 76 54 6. 7 3. 76 4 Aldana, PR et al. , 2008 Results

Results Among the patients at our institution, 4 of the 9 (44. 4%) still had a VGB shunt at the time of the analysis. One of these died from complications unrelated to the shunt The VGB shunts in our study lasted an average of 4. 4 years (1, 608. 9 days), while the average length of follow up for our data set was 7. 9 years In the combined data set, 54 out of 76 patients (71%) had a VGB shunt in place after an average length of follow up of 3. 76 years. These data were for patients with an average of 6. 7 years Among all the studies, there were 4 deaths reported that were all unrelated to shunt complications 9 -15. These were all included in the data analysis Reasons for VGB shunt failure included: disconnection, distal shunt malfunction, proximal shunt malfunction, infection, gallbladder atony, and gallbladder “sludging” 9 -15 Reasons for initial VGB shunt placement included: VP shunt infections, obstruction by or difficulty placing due to abdominal adhesions, abdominal pseudocysts formation, non-absorptive peritoneum 9 -15

Conclusions Our data indicate that VGB shunts are a viable alternative to VP shunts, especially considering that we saw a 71% retention rate with average 3. 76 years of follow-up This data would indicate that VGB shunts are as good as VP shunts in their failure rates, since VP shunts have been demonstrated to have a 29% failure rate at 1 year in prior studies 1, 5, 6 From the VGB shunt failures in our data set, we do know that these shunts fail for similar reasons to VP shunts including infections and hardware malfunction 1, 2 Some unique problems that can occur with VGB shunts include gallbladder atony, sludging, or the future need for a cholecystectomy. Additionally, these shunts are more prone to disconnecting as opposed to VP shunts 9 -15 Overall, our data and literature review display that VGB shunts are a reasonable alternative to VP shunts, especially considering multiple shunt failures due to peritoneal infection or complication secondary to peritoneal adhesions

Next Steps and Future Opportunities A prospective study with closer follow-up of patients receiving VGB shunts could be implemented in order to better understand short-term complications and failure rates within the first year A comparative study looking at VP and VGB shunts as a first line treatment could be useful in understanding if these can be used earlier in the hydrocephalus treatment algorithm Creation of a national data bank or using data from a multi-center study to retrospectively examine VGB failure rates and longevity could be useful since data are limited at most single institutions

References 1. Wright, Z, Larrew, TW, Eskandari, R. Pediatric Hydrocephalus: Current State of Diagnosis and Treatment. Pediatrics in Review. 2016 Nov; 37(11): 478 -490. Available at https: //doi. org/10. 1542/pir. 20150134. Accessed on March 21, 2021. 2. Kinsman, SL, Johnston, MV. Congenital Anomalies of the Central Nervous System. Nelson Textbook of Pediatrics. 2020; 609: 3063 -3082. Accessed on March 21, 2021. 3. Jeng S, Gupta N, Wrensch M, Zhao S, Wu YW. Prevalence of congenital hydrocephalus in California, 1991 -2000. Pediatr Neurol. 2011; 45(2): 67– 71. doi: 10. 1016/j. pediatrneurol. 2011. 03. 009. Accessed on March 21, 2021. 4. Simon TD, Riva-Cambrin J, Srivastava R, Bratton SL, Dean JM, Kestle, JRW. Hydrocephalus Clinical Research Network. Hospital care for children with hydrocephalus in the United States: utilization, charges, comorbidities, and deaths. J Neurosurg Pediatr. 2008; 1(2): 131– 137. doi: 10. 3171/PED/2008/1/2/131. Accessed on March 21, 2021. 5. Koral K, Blackburn T, Bailey AA, Koral KM, Anderson J. Strengthening the argument for rapid brain MR imaging: estimation of reduction in lifetime attributable risk of developing fatal cancer in children with shunted hydrocephalus by instituting a rapid brain MR imaging protocol in lieu of head CT. AJNR Am J Neuroradiol. 2012; 33(10): 1851– 1854. doi: 10. 3174/ajnr. A 3076. Accessed on March 21, 2021. 6. Niederhauser BD, Mc. Donald RJ, Eckel LJ, et al. Retrospective review of rapid pediatric brain MR imaging at an academic institution including practice trends and factors affecting scan times. AJNR Am J Neuroradiol. 2013; 34(9): 1836– 1840. doi: 10. 3174/ajnr. A 3510. Accessed on March 21, 2021. 7. Simon TD, Hall M, Riva-Cambrin J, et al. Hydrocephalus Clinical Research Network. Infection rates following initial cerebrospinal fluid shunt placement across pediatric hospitals in the United States. J Neurosurg Pediatr. 2009; 4(2): 156– 165. doi: 10. 3171/2009. 3. PEDS 08215. Accessed on March 21, 2021. 8. Smith, GW, Moretz, WH, Pritchard, WL. Ventriculo-biliary shunt; a new treatment for hydrocephalus. Surg. Forum. 1958; 9: 701 -705. Accessed on March 21, 2021. 9. Novelli, PM, Reigel, DH. A closer look at the ventriculo-gallbladder shunt for the treatment of hydrocephalus. Pediatr Neurosurg. 1997 Apr; 26(4): 197 -9. doi: 10. 1159/000121191. Accessed on March 21, 2021. 10. West, KW, Turner, MK, Vane, DW, Boaz, J, Kalsbeck, J, Grodfeld, JL. Ventricular gallbladder shunts: an alternative procedure in hydrocephalus. J Pediatr Surg. 1987 Jul; 22(7): 609 -12. doi: 10. 1016/s 0022 -3468(87)80110 -0. Accessed on March 21, 2021. 11. Ketoff, JA, Klein, RL, Maukkassa, KF. Ventricular cholecystic shunts in children. J Pediatr Surg. 1997 Feb; 32(2): 181 -3. doi: 10. 1016/s 0022 -3468(97)90175 -5. Accessed on March 21, 2021. 12. Aldana, PR, James, HE, Postlethwait, RA. Ventriculogallbladder shunts in pediatric patients. Journal of Neurosurgery: Pediatrics. 2008; 1(4): 284 -287. Available at https: //thejns. org/pediatrics/view/journals/j-neurosurg-pediatr/1/4/article-p 284. xml. Accessed on March 21, 2021. 13. Stringel, G, Turner, M, Crase, T. Ventriculo-gallbladder shunts in children. Childs Nerv Syst. 1993 Sep; 9(6): 331 -3. doi: 10. 1007/BF 00302035. Accessed on March 21, 2021. 14. Rivero-Garvía M, Pancucci G, Morcillo J, Millán A, Márquez-Rivas J. Ventriculobiliary Shunts, Another Option. Pediatr Neurosurg. 2015; 50(3): 152 -6. doi: 10. 1159/000381030. Epub 2015 Apr 25. Accessed on March 21, 2021. 15. Pal, K, Jindal, V. Ventriculo cholecystic shunt in the management of hydrocephalus. Indian Pediatr. 2007 Jun; 44(6): 435 -7. Accessed on March 21, 2021.
- Slides: 11