Estrogens Progestins and Androgens Becky Worthylake bworthlsuhsc edu

Estrogens, Progestins and Androgens Becky Worthylake bworth@lsuhsc. edu

Outline • Overview • Estrogens – General • Estrogens & Modifiers – Therapeutic Formulations & Uses • Progestins – Therapeutic Formulations & Uses • Contraception • Androgens – General • Androgens – Uses & Therapeutic Formulations
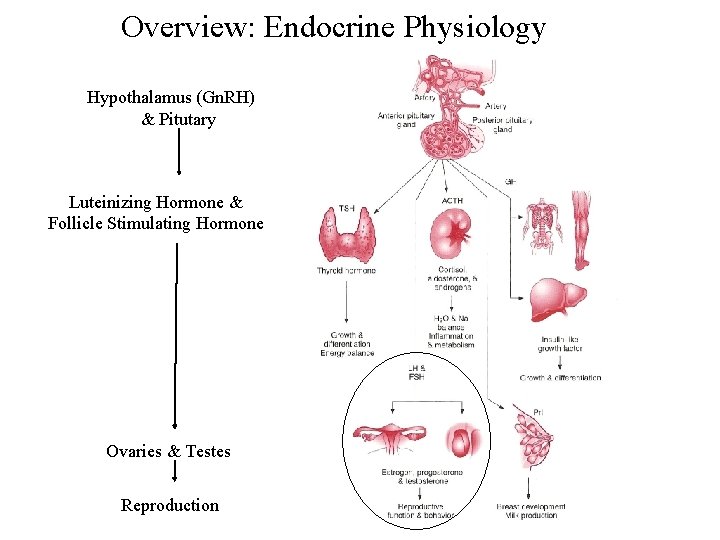
Overview: Endocrine Physiology Hypothalamus (Gn. RH) & Pitutary Luteinizing Hormone & Follicle Stimulating Hormone Ovaries & Testes Reproduction
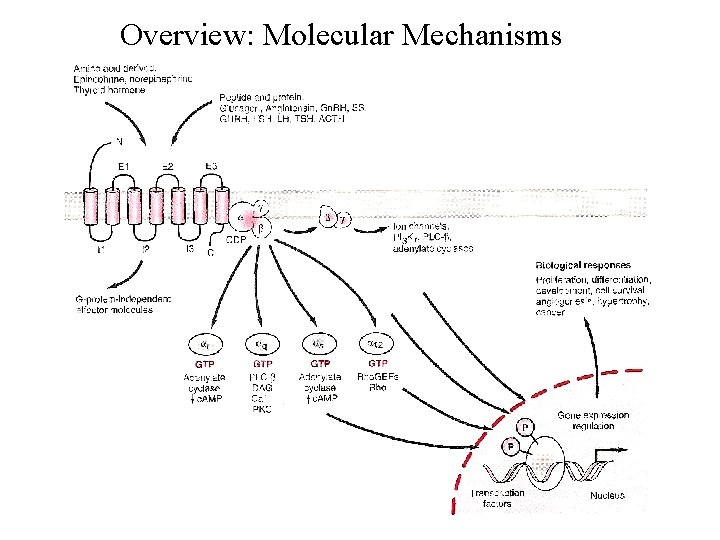
Overview: Molecular Mechanisms
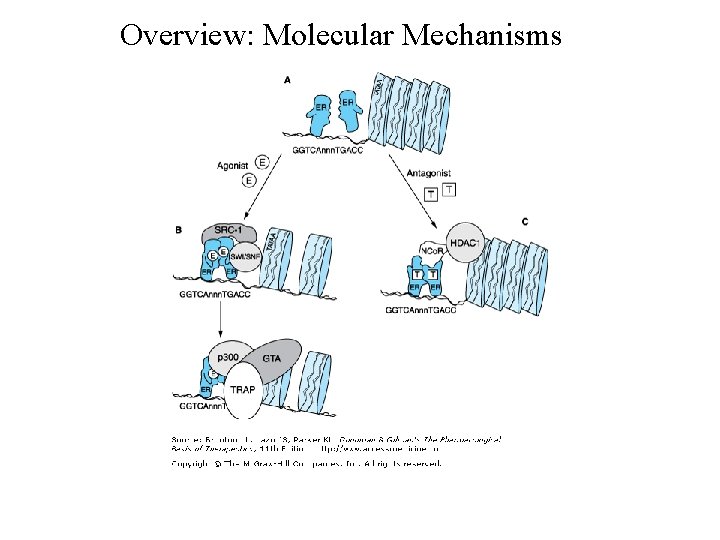
Overview: Molecular Mechanisms

Outline • Estrogens – General • Synthesis • Physiology • Regulation
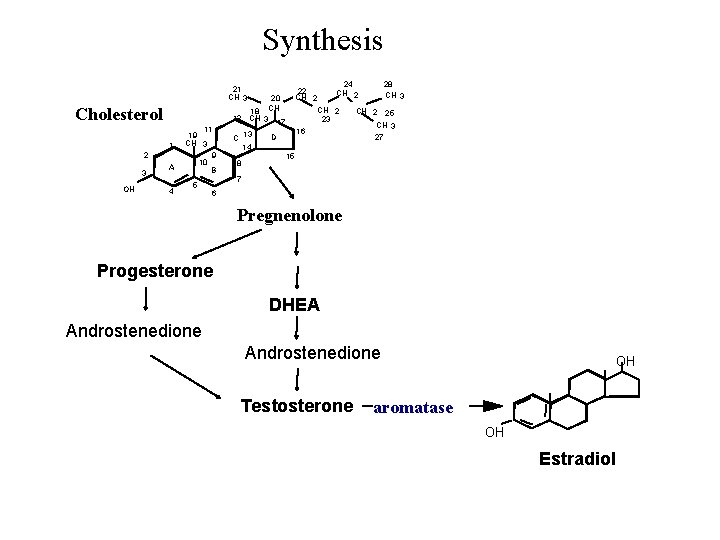
Synthesis 21 CH 3 Cholesterol 1 2 3 OH A 4 11 19 CH 3 9 10 B 5 20 18 CH 12 CH 3 17 13 C 14 8 24 CH 2 22 CH 2 23 16 D 28 CH 3 CH 2 25 CH 3 27 15 7 6 Pregnenolone Progesterone DHEA Androstenedione Testosterone OH aromatase OH Estradiol
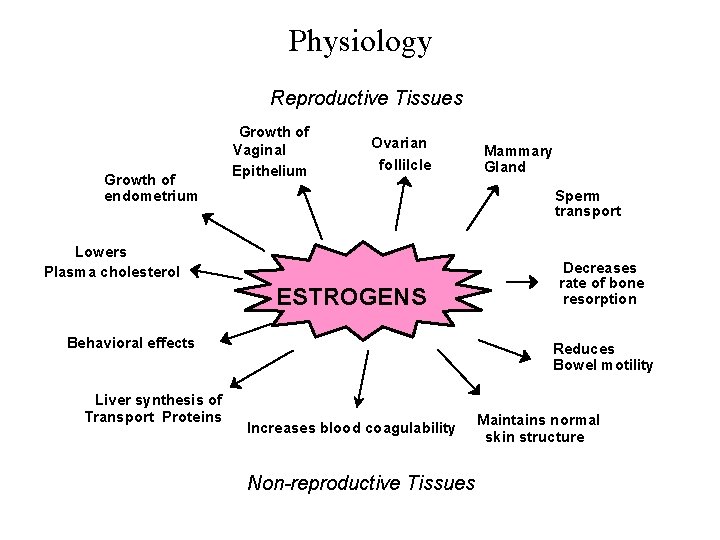
Physiology Reproductive Tissues Growth of endometrium Growth of Vaginal Epithelium Ovarian follilcle Sperm transport Lowers Plasma cholesterol ESTROGENS Behavioral effects Liver synthesis of Transport Proteins Mammary Gland Decreases rate of bone resorption Reduces Bowel motility Increases blood coagulability Non-reproductive Tissues Maintains normal skin structure
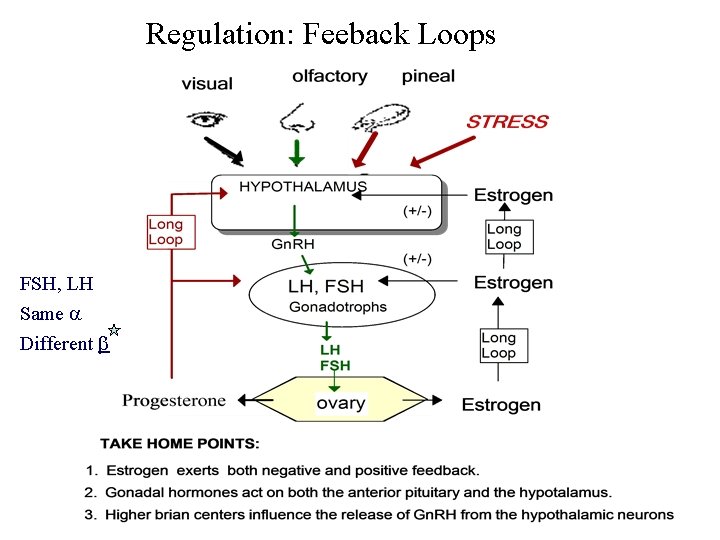
Regulation: Feeback Loops FSH, LH Same Different
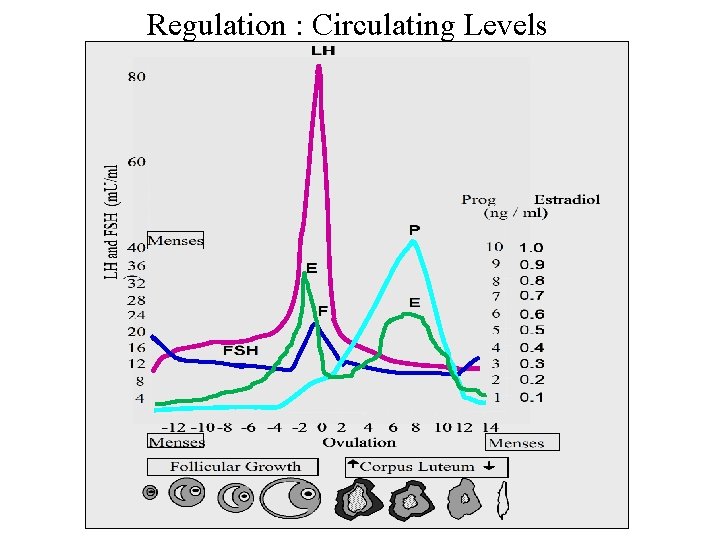
Regulation : Circulating Levels
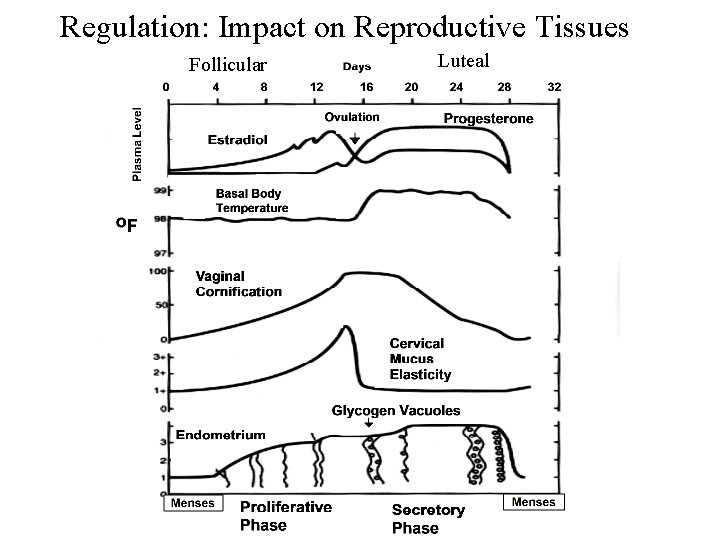
Regulation: Impact on Reproductive Tissues Follicular Luteal

Outline • Estrogens & Estrogen Modifiers – Therapeutic Formulations and Uses • Therapeutic Estrogens • SERMs (selective estrogen receptor modulators) • Estrogen Synthesis Inhibitors

Therapeutic Estrogens DRUG Estradiol COMMENTS Main estrogen in premenopausal women. Poor oral bioavailability Effective as a patch (ESTRADERM, ESTROGEL) Intramuscular delivery sustains release for weeks (DEPO ESTRADIOL) Topical administration with vaginal cream (ESTRING) Ethinylestradiol Semi-synthetic: commonly used on oral contraceptives Natural estrogen-main ingredient of conjugated Estrone Indications estrogens (PREMARIN) • Primary Hypogonadism • Postmenopausal Hormonal Therapy • Oral Contraceptives • Suppress ovulation in patients with intractable dysmenorrhea or hirsutism • Fertility treatments

Therapeutic Estrogens Cont’ Side effects Nausea, fluid retention, breakthrough bleeding, change in menstrual flow, breast tenderness. Adverse Effects: Thrombolytic complications; endometrial carcinoma; breast carcinoma; and hypertension. In men - feminization of genitalia & impotence. Contraindications: Pregnancy, incomplete bone growth, undiagnosed genital bleeding; stroke, thrombophlebitis, or thromboembolic disease. , heart disease. Women with family history of breast or uterine cancer (BRCA gene) Drug Interactions: efficacy of oral anticoagulants and hypoglycemic agents adverse effects of tricyclic antidepressants the effects of oxytocin on the uterus. St. John's wort may cause loss of contraceptive or hormonal-replacement efficacy of estrogens
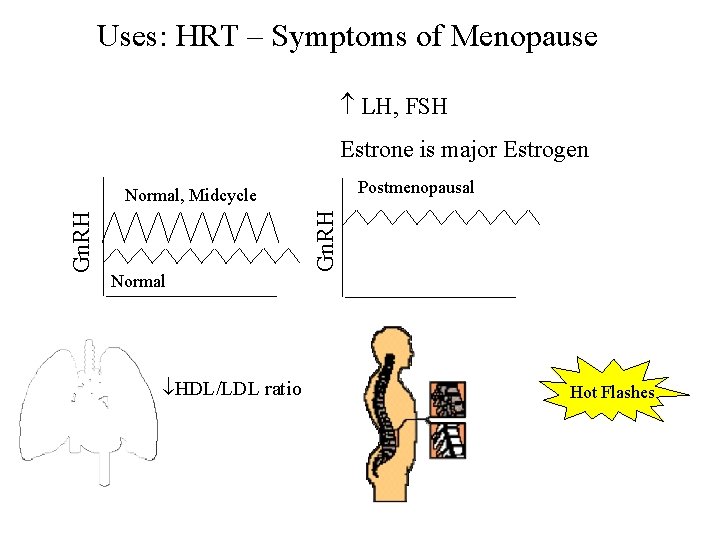
Uses: HRT – Symptoms of Menopause LH, FSH Estrone is major Estrogen Postmenopausal Normal HDL/LDL ratio Gn. RH Normal, Midcycle Hot Flashes
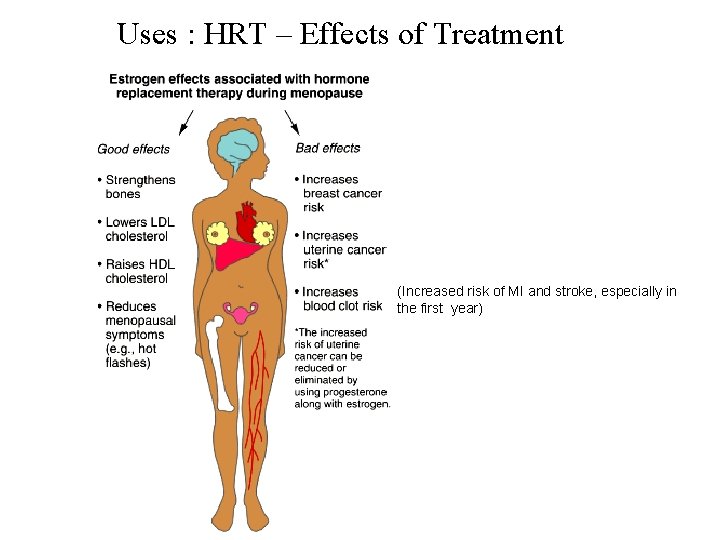
Uses : HRT – Effects of Treatment (Increased risk of MI and stroke, especially in the first year)

Uses: HRT - Formulations Early HRT used estrogen alone: increased risk of uterine (endometrial) cancer. As a result, addition of progestins is now used to limit endometrial hyperplasia Medroxyprogesterone (MPA) acetate is most commonly used • Various regimens are used: estrogen for 25 days with inclusion of MPA during last 10 -13 days of estrogen, 5 -6 days with no hormones • Combination formulations: PREMPRO (PREMARIN plus MPA) given at fixed dose daily; PREMPHASE (PREMARIN for 28 days and MPA for days 14 -28) • Newer combos of estrogens with progestins: FEM HRT (estradiol plus norethindrone acetate) ORTH PREFEST (estradiol plus norgestimate) • Vaginal creams (PREMARIN) or a ring device (ESTRING) can be used instead of oral doses. Reduces vaginal dryness, yeast infections and urinary tract infections.
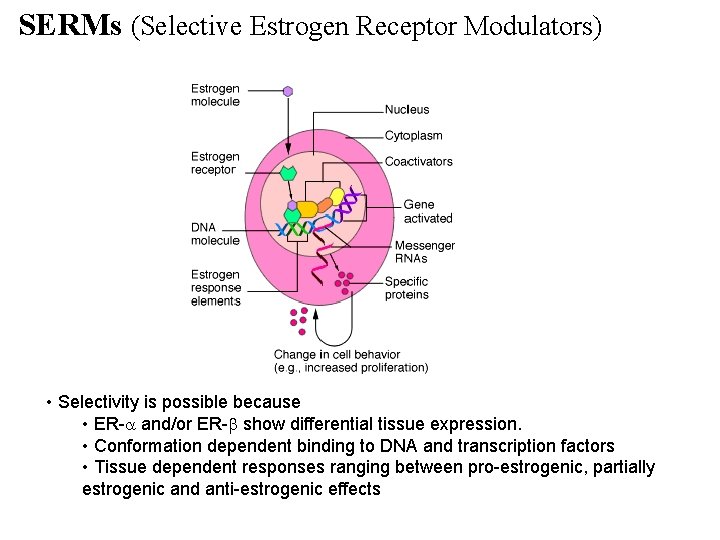
SERMs (Selective Estrogen Receptor Modulators) • Selectivity is possible because • ER- and/or ER- show differential tissue expression. • Conformation dependent binding to DNA and transcription factors • Tissue dependent responses ranging between pro-estrogenic, partially estrogenic and anti-estrogenic effects
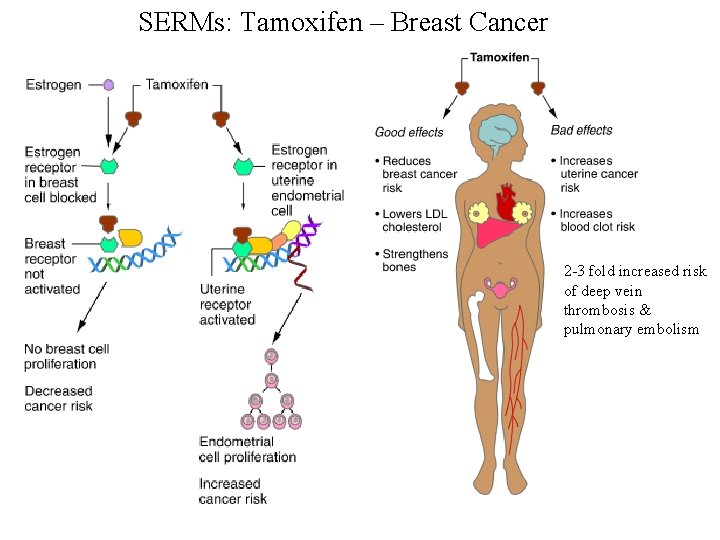
SERMs: Tamoxifen – Breast Cancer 2 -3 fold increased risk of deep vein thrombosis & pulmonary embolism

SERMs: Tamoxifen continued - Most effective in treatment of tumors that are ER-positive (50% response) or ER + PR positive (70 -80% response rates). Responses of ER-negative tumors is < 10%. - Adjuvant therapy with chemo or radiation in treatment - Preventative agent for women at high risk for breast cancer. -Resistance is usually developed in 5 years, which may, in part, reflect alterations in the ER receptors in the tumors.

SERMs: Other Raloxifene (EVISTA): - High affinity for both ER- and ER- -Treatment of osteoporosis in post-menopausal women. -Does not cause proliferation of the endometrium or breast tumor cells Side effects: 2 -3 fold risk of deep vein thrombosis and pulmonary embolism Interactions: Ampicillin absorption Raloxifene warfarin efficacy
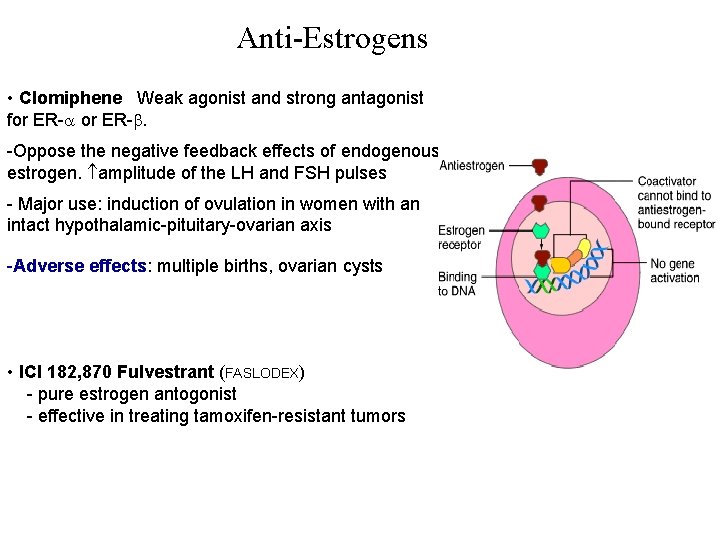
Anti-Estrogens • Clomiphene Weak agonist and strong antagonist for ER-. -Oppose the negative feedback effects of endogenous estrogen. amplitude of the LH and FSH pulses - Major use: induction of ovulation in women with an intact hypothalamic-pituitary-ovarian axis -Adverse effects: multiple births, ovarian cysts • ICI 182, 870 Fulvestrant (FASLODEX) - pure estrogen antogonist - effective in treating tamoxifen-resistant tumors

Estrogen Synthesis Inhibitors • Steroidal: exemestane (AROMASIN) • Non-steroidal: anastrozole (ARIMIDEX), letrozole (FEMARA) - Specifically block the local production of estrogens in hormonally-responsive tissues. - Second-line treatment for breast cancer in patients whom tamoxifen therapy is unsuccessful, but new studies rapidly proving its efficacy and promoting earlier use - Aromatase inhibitors do not have the bone protecting activity of tamoxifen, and adjuvant therapies to prevent bone loss are in trials

Outline • Progestins – Therapeutic Formulations & Uses • Therapeutic Progestins • anti-Progesterones

Progestins – Therapeutic Progesterone • Naturally occurring progesterone (low oral bioavailability) - Micronized particles suspended in oil and packaged in gelatin capsules (PROMETRIUM) - Vaginal gel (CRINONE) - Slow-release intrauterine device (PROGESTASERT) • 17 - -hydroxy-progesterone derivatives have substitutions at C 17 that slow hepatic metabolism : medroxyprogesterone (MPA) (PROVERA) • 19 -nor testosterone derivatives display primarily progestational rather than androgenic activity : norethindrone • Replacement of the 13 -methyl group of norethindrone with a 13 -ethyl substituent are more potent progestins and less androgenic: norgestrel, nomegestrol

Progestins continued Mechanism of Action: Interacts with PR to mimic the stimulatory affects of progesterone Physiological Target: Reproductive Tract - Decreases estrogen-driven endometrial proliferation - Establishment and maintenance of pregnancy Common Uses: - Oral contraceptives - HRT to limit estrogen’s effects on the endometrium - Uterine Bleeding disorders - Premature labor (decrease uterine contractions) - Stimulate Appetite in AIDS or cancer patients

Progestins: anti-Progesterones Mifepristone (RU 486) (mifeprex): PR antagonist Used in first trimester to terminate pregnancy (along with prostaglandins to increase uterine contractions) Post-coital contraceptive (prevent implantation) Investigational: induction of labor after fetal death and treatment of endometriosis. Adverse Effects: vaginal bleeding, abdominal pain and cramping Contraindicated in patients with vaginal bleeding, adrenal dysfunction or asthma (due to anti-glucocorticoid actions) Interactions: Decreases efficacy of anticoagulants. Inhibits hepatic metabolism by CYP 3 A 4 (eg. anti-retroviral protease inhibitors, calcium-channel blockers, carbamazepine)

Outline • Contraception • Therapeutic Estrogens & Progesterones • Oral Contraceptive Formulations • Emergency Contraception • Extended-Regimen Contraception • Mechanism of Action • Effects
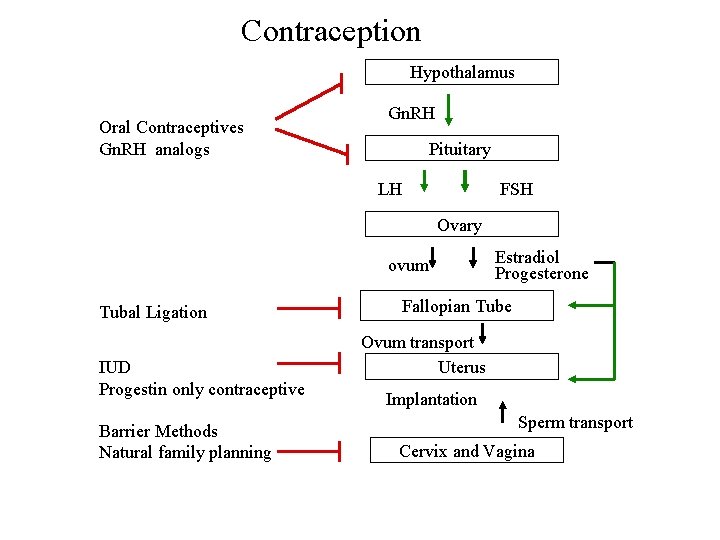
Contraception Hypothalamus Oral Contraceptives Gn. RH analogs Gn. RH Pituitary LH FSH Ovary ovum Tubal Ligation IUD Progestin only contraceptive Barrier Methods Natural family planning Estradiol Progesterone Fallopian Tube Ovum transport Uterus Implantation Sperm transport Cervix and Vagina

Oral Contraceptives: History • 1950: Pincus et al (progesterone prevents ovulation) • 1959: 1 st pill appeared in USA • 1960: mini pill (progesterone alone) • 1970: Introduction low dose or second generation of OCS • 1980: biphasic or triphasic regimens • 1990: 3 rd generation OCs e. g, norgestimate 0. 25 mg or desogestrel 0. 15 mg)
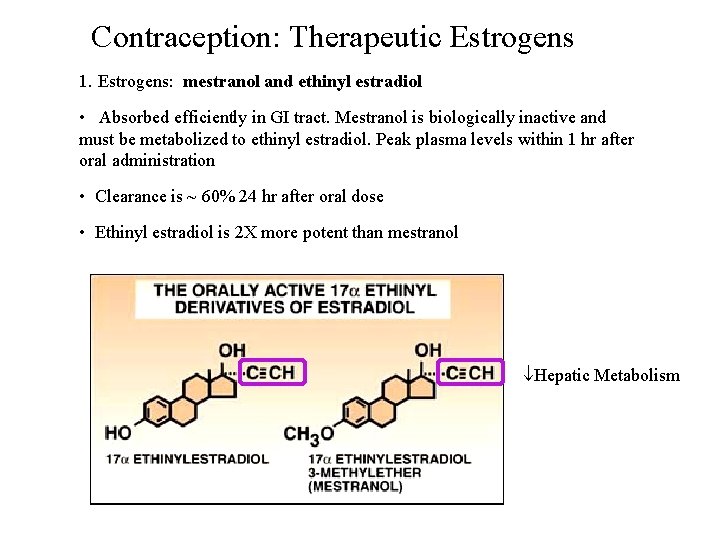
Contraception: Therapeutic Estrogens 1. Estrogens: mestranol and ethinyl estradiol • Absorbed efficiently in GI tract. Mestranol is biologically inactive and must be metabolized to ethinyl estradiol. Peak plasma levels within 1 hr after oral administration • Clearance is ~ 60% 24 hr after oral dose • Ethinyl estradiol is 2 X more potent than mestranol Hepatic Metabolism
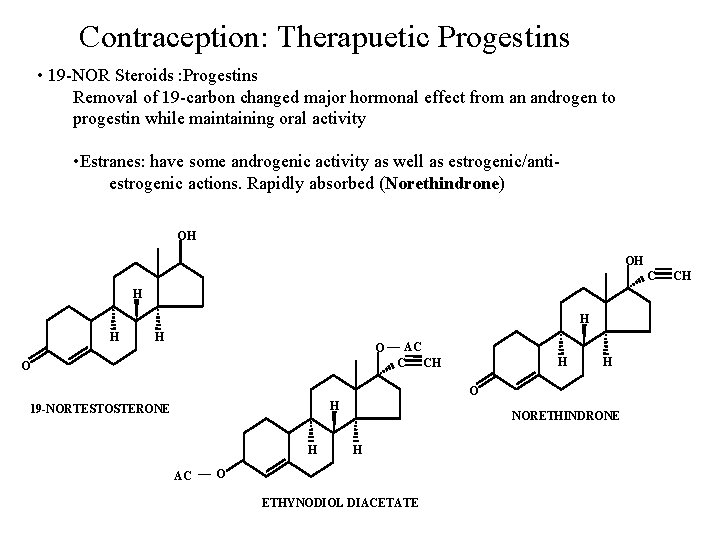
Contraception: Therapuetic Progestins • 19 -NOR Steroids : Progestins Removal of 19 -carbon changed major hormonal effect from an androgen to progestin while maintaining oral activity • Estranes: have some androgenic activity as well as estrogenic/antiestrogenic actions. Rapidly absorbed (Norethindrone) OH OH C H H O O AC C CH H H O H 19 -NORTESTOSTERONE H AC NORETHINDRONE H O ETHYNODIOL DIACETATE CH
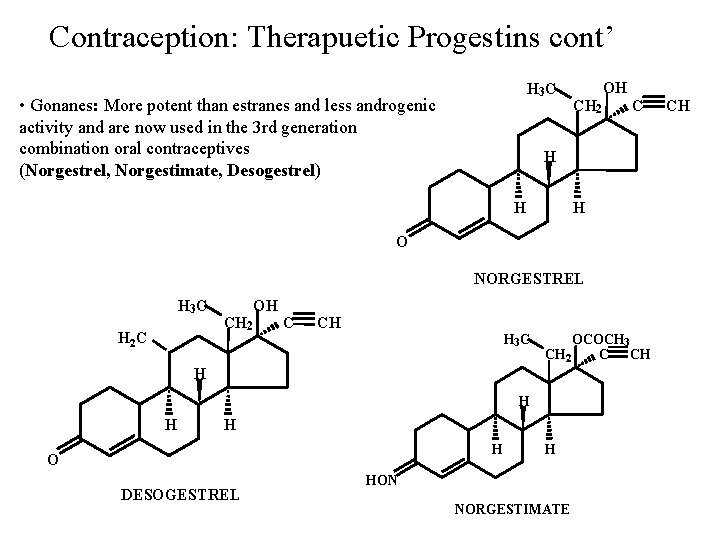
Contraception: Therapuetic Progestins cont’ H 3 C • Gonanes: More potent than estranes and less androgenic activity and are now used in the 3 rd generation combination oral contraceptives (Norgestrel, Norgestimate, Desogestrel) CH 2 OH C H H H O NORGESTREL H 3 C H 2 C CH 2 OH C CH H 3 C OCOCH 3 C CH CH 2 H H H O DESOGESTREL H HON NORGESTIMATE CH

Therapeutic Estrogen & Progestin Combinations • 1 st generation: products containing mestranol • Low dose OCs: products containing < 50 mcg ethinyl estradiol • 2 nd generation “Low-Dose” : products containing gonanes (levonorgestrel, norgestimate) and other members of norethindrone family and 20, 30, or 35 mcg ethinyl estradiol • 3 rd generation: desogestrel or gestodene (new progestins) with 20, 30, or 35 mcg ethinyl estradiol

Contraception: Formulations Monophasic: The concentrations of estrogens and progestins are fixed in the pill, which is taken for 21 days followed by 7 days of “hormone-free” pills. a. mestranol (50 µg) + norethindrone (1. 0 mg) (ORTHO-NOVUM 1/50, NORINYL 1+50) b. ethinyl estradiol (20 -30 µg) + a progestin (estranes or the gonanes, 0. 15 -1. 5 mg). Include ORTHONOVUM 1/35, NORDETTE, ORTHO-CEPT , LOESTRIN)

Contraception: Formulations Biphasics: • ethinyl estradiol (fixed concentration) + norethindrone (lower concentration in the first 7 -10 days and then higher concentration for the next 11 -14 days). (Include ORTHO-NOVUM 10/11, JENEST-28) • The rationale is to limit exposure to the higher concentration of the progestin.

Contraception: Formulations Triphasic: • Fixed concentration of ethinyl estradiol with 3 different concentrations of norethindrone (TRI-NORINYL ORTHO-NOVUM 7/7/7), • Fixed concentration of ethinyl estradiol with three concentrations of gonanes. (ORTHO-TRI-CYCLEN - norgestimate; TRI-LEVLEN, TRIPHASIL - levonorgestral ). • Rationale is to mimic the hormonal changes in the menstrual cycle

Contraception: Formulations Progestin Only: • Oral formulations of norethindrone (micronor) or levonorgestrel (ovrette) taken daily • Subdermal implants of levonorgestrel (norplant) for slow-release and longterm contraceptive actions (up to five years) • IM injections of medroxyprogesterone (depo-provera) that provides effective contraception for 3 months • IUD that releases low amounts of progesterone locally (progestasert).

Emergency Contraceptives • Drugs used for the prevention of pregnancy following unprotected intercourse or a known or suspected contraceptive failure. • Emergency hormone contraceptive regimens are highly effective and decrease the risk of pregnancy by 75 percent • To be effective these must be taken within 72 hours of intercourse • May also inhibit ovulation or fertilization depending on timing of administration Alteration of the endometrium, sperm penetration, and tubal motility are also affected. ESTABLISHED PREGNANCIES ARE NOT HARMED. • Two products are available: – Plan B: 0. 75 mg levonorgestrel – Preven: 0. 25 mg levonorgestrel and 0. 05 mg ethinyl estradiol (this product includes a pregnancy test kit)

Extended Regimen Contraception Levonorgestrel / ethinyl estradiol 0. 15 mg / 0. 03 mg And either placebo or ethinyl estradiol tablets 0. 01 mg tablets) Brand Names: Jolessa, Quasense, Seasonale, Seasonique 91 -day courses of tablets Advantages • Period once every 3 months • Period last about 3 days with decreased bleeding , Side Effects: Breakthrough bleeding and spotting Seasonique: incorporates low-dose estrogen rather than placebo tablets in an effort to limit bloating, hormonal fluctuations, and breakthrough bleeding.
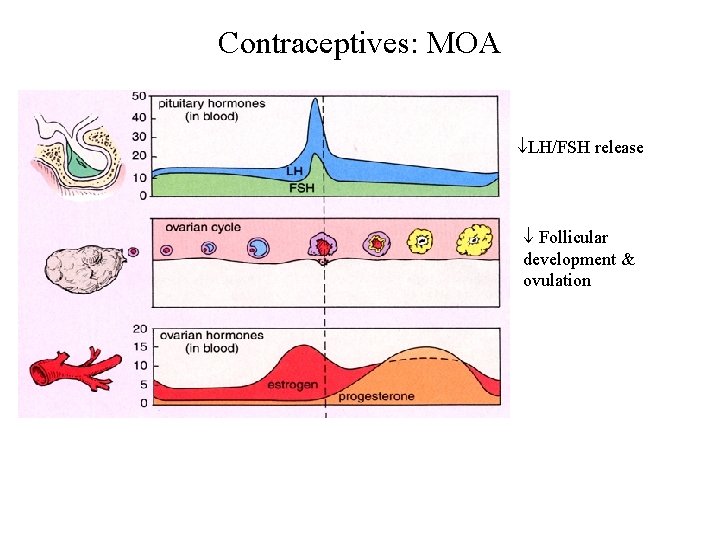
Contraceptives: MOA LH/FSH release Follicular development & ovulation
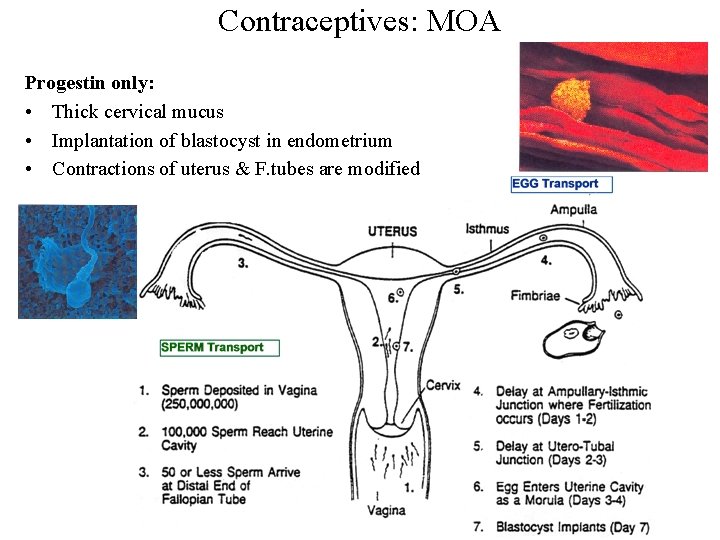
Contraceptives: MOA Progestin only: • Thick cervical mucus • Implantation of blastocyst in endometrium • Contractions of uterus & F. tubes are modified

Effects: Benefits Initiating Method • Start First day of next menstrual period • Some suggest starting on first Sunday following onset of menses – Usually avoids menstrual period on weekends – Most clinicians recommend backup for at least 2 cycles Other Beneficial effects 1. 2. 3. 4. 5. Decreases Dysmenorrhea Decreases benign breast and ovarian cysts Regulates cycle in anovulatory women Decreased blood loss during menstruation 50% reduction in ovarian and endometrial cancer.

Effects: Drug Interactions Drugs that disrupt liver metabolism and increase oral contraceptive metabolism - anti-seizure medications, St. John’s wort - antibiotics tetracycline and ampicillin - HIV protease inhibitors - Anti-tuberculosis drugs such as rifampin Oral contraceptives effect the activity of other drugs a. anticoagulants b. benzodiazepines, c. beta-blockers d. corticosteroids, and tricyclic antidepressants

Effects: Contraindications 1. Absolute a. History of thromboembolism, MI, stroke b. Impaired liver function c. Known or suspected breast cancer d. Undiagnosed abnormal vaginal bleeding e. Known or suspected pregnancy f. Smokers over age 35 (may use progestin-only) 2. Relative a. – Migraine headaches b. – Hypertension - ok if <35, or healthy, or BP controlled c. – Elective surgery: Discontinue 4 wks. prior to major surgery d. – Gallstones/ Cholecystitis e. – Epilepsy: anti-seizure meds may decrease effectiveness of OCP’s f. – Diabetes: small risk or worsening vascular disease.

Outline • Androgens – General • Synthesis • Regulation • Physiological Effects
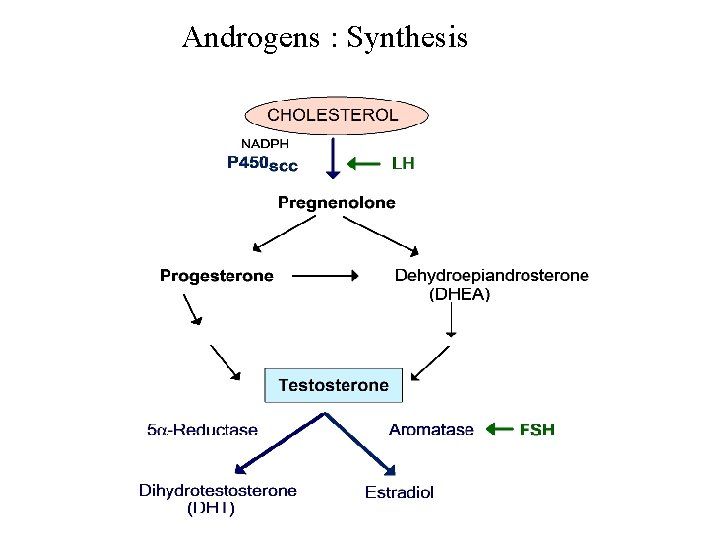
Androgens : Synthesis
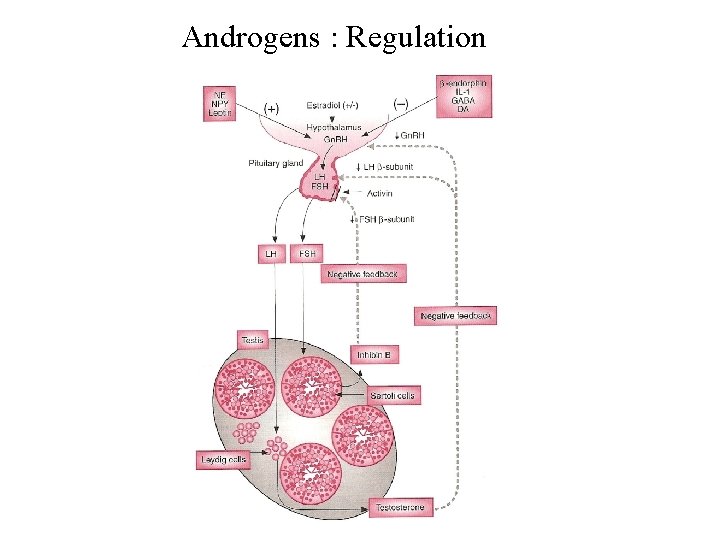
Androgens : Regulation
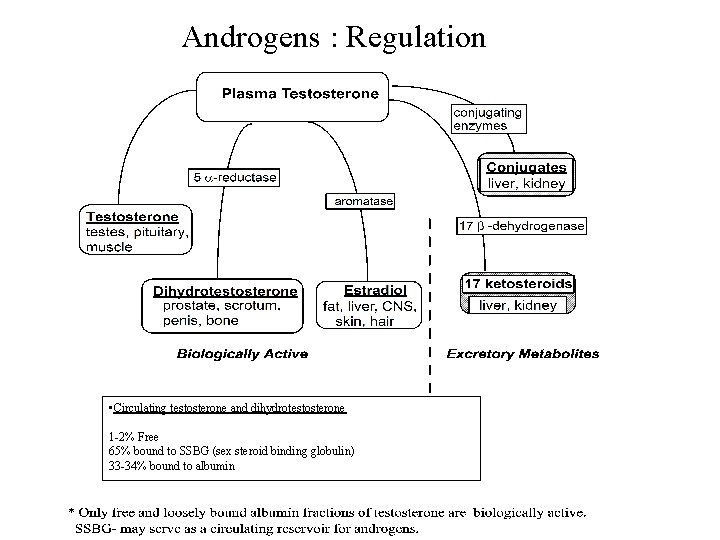
Androgens : Regulation • Circulating testosterone and dihydrotestosterone 1 -2% Free 65% bound to SSBG (sex steroid binding globulin) 33 -34% bound to albumin
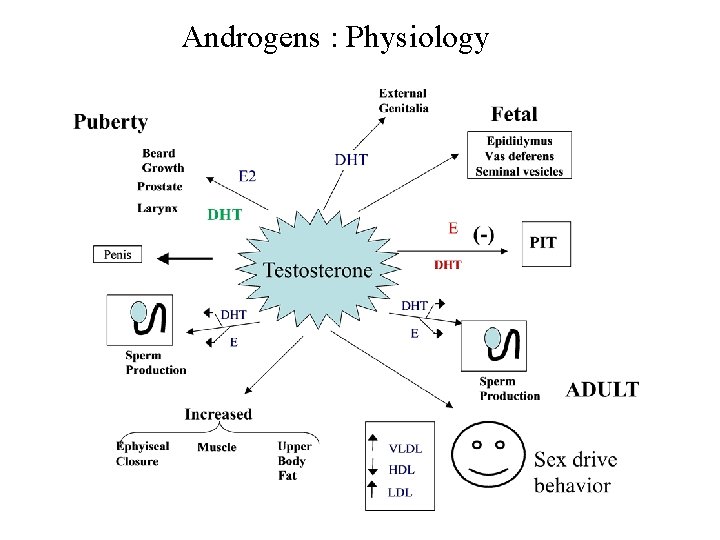
Androgens : Physiology

Outline • Androgens – Uses & Therapeutics • Treatable Conditions • Therapeutic Formulations of Testosterones and Androgens • Androgen Antagonists

Treatable Conditions A. Male hypogonadism: develop or maintain secondary sex characteristics B. Andropause C. Prostate Cancer D. Male Pattern Baldness

Condition: Adult Male Hypogonadism • • • Symptoms Decreased libido Erectile dysfunction Infertility Fatigue, weakness Depression, loss of motivation, irritability Vasomotor phenomena • • • Signs Decreased body hair Decreased muscle mass Small prostate and testes Gynecomastia Osteoporosis Anemia Treatment Transdermal testosterone esters Monitoring for both beneficial and deleterious effects required, age dependent

Condition: Andropause • Changes are slower and more subtle: progressive decline (total and free) in testosterone levels Leydig cell number and activity. • ~ 60% of healthy men over 65 have lower testosterone compared to 20 -35 year old men and may be related to impotence Treatment: • Pharmacological doses of testosterone in men muscle mass and muscle strength especially in combination with exercise. Also cognition and sense of well being. • Negative Effects: Lipid profiles ( LDL), prostate size, uninary symptoms • New Developments: “STRM” selctive androgen recepotor modulators: Goal is to have anabolic effect on muscle mass and anti-androgenic effect on the prostate
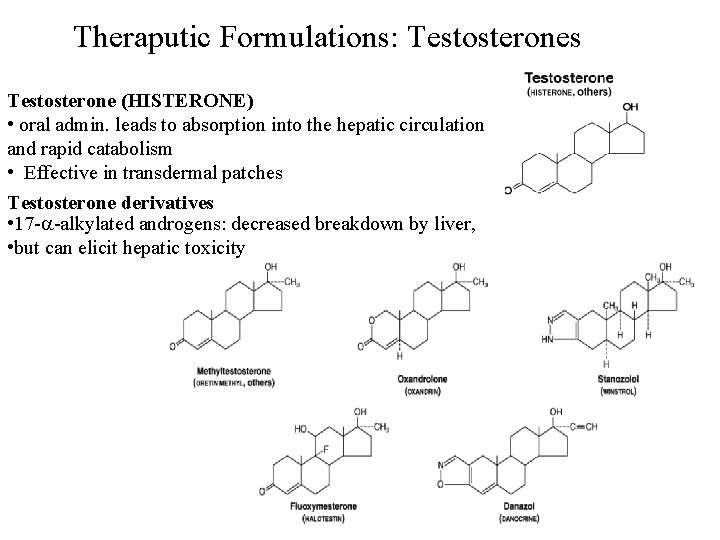
Theraputic Formulations: Testosterones Testosterone (HISTERONE) • oral admin. leads to absorption into the hepatic circulation and rapid catabolism • Effective in transdermal patches Testosterone derivatives • 17 - -alkylated androgens: decreased breakdown by liver, • but can elicit hepatic toxicity
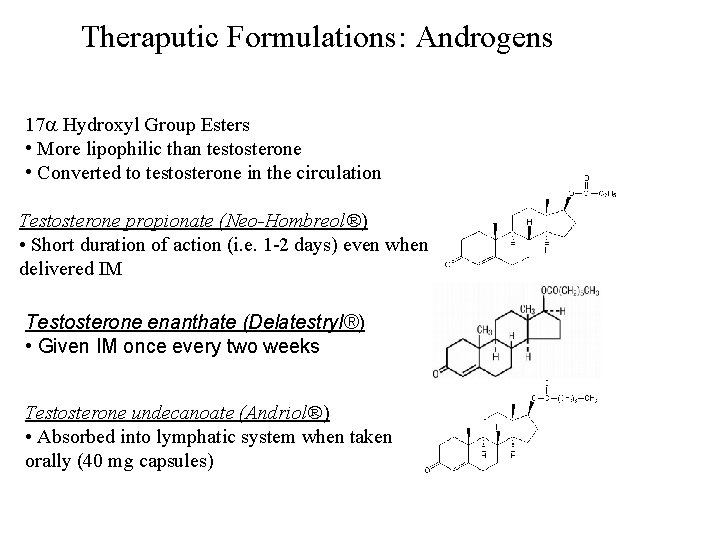
Theraputic Formulations: Androgens 17 Hydroxyl Group Esters • More lipophilic than testosterone • Converted to testosterone in the circulation Testosterone propionate (Neo-Hombreol®) • Short duration of action (i. e. 1 -2 days) even when delivered IM Testosterone enanthate (Delatestryl®) • Given IM once every two weeks Testosterone undecanoate (Andriol®) • Absorbed into lymphatic system when taken orally (40 mg capsules)
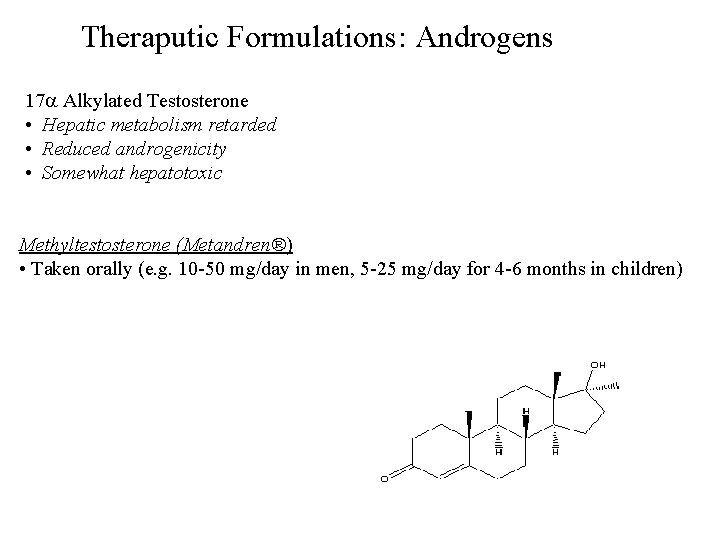
Theraputic Formulations: Androgens 17 Alkylated Testosterone • Hepatic metabolism retarded • Reduced androgenicity • Somewhat hepatotoxic Methyltestosterone (Metandren®) • Taken orally (e. g. 10 -50 mg/day in men, 5 -25 mg/day for 4 -6 months in children)

Theraputic Formulations: Side Effects Potential Side Effects of Excessive Androgen Treatment • Reduced spermatogenesis and fertility due to feedback inhibition of LH and FSH secretion from anterior pituitary • Acne, particularly in women due to androgen stimulation of sebaceous glands beneath skin • Virilization (including facial hair and hirsutism) in women and children • In older men, increased risk of benign prostate hyperplasia and prostate cancer • Hepatotoxicity (for 17 -alkylated androgens) Anabolic Steroid and Androgen Abuse in Sports 100 -200 x normal daily production in men

Androgen Antagonists Androgen Receptor antagonists Flutamide (EVLEXIN) and Bicalutamide (CASODEX). Bicalutamide has much less hepatoxicity Used in conjunction with Gn. RH analogs to treat metastatic prostate cancer Treat Hirsutism in women (due to hepatoxicity should not use for cosmetic purposes) 5 - -reductase inhibitors Finasteride (PROSCAR) used to treat benign prostatic hypertrophy and male patterned baldness (PROPECIA)
- Slides: 59